Thrombosis Dr Aarathi Rau Hemostasis Normal hemostasis the

Thrombosis Dr Aarathi Rau

Hemostasis • Normal hemostasis: the end result of a set of well regulated processes that accomplish • fluid blood in the normal blood vessel • Rapid & localized hemostatic plug at the site of vessel injury.

Normal hemostasis • Arteriolar constriction • Exposure of extracellualar matrix (ECM) beneath the endothelium • Adherence of platelets to form platelet plug • Activation of platelets & degranulation (ADP, thrombin, thromboxane A 2) • Tissue factor (from injury) stimulate coagulation cascade • Fibrin clot & platelets form secondary hemostatic plug • Limit size of clot by fibrinolysis
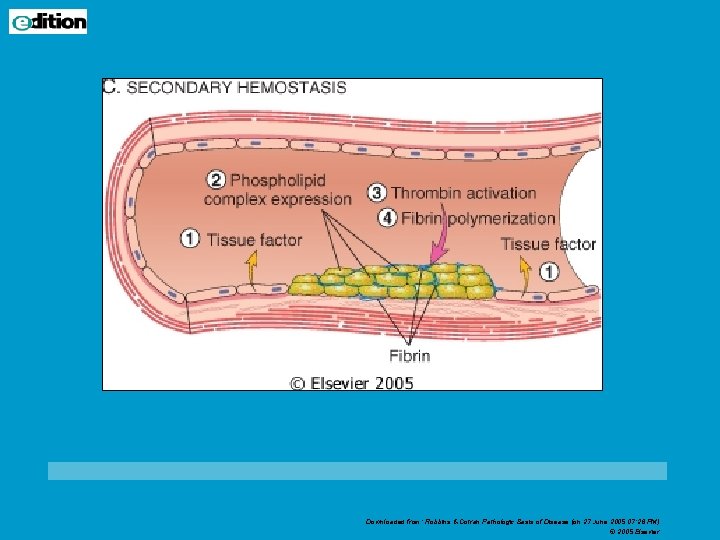
Downloaded from: Robbins & Cotran Pathologic Basis of Disease (on 27 June 2005 07: 26 PM) © 2005 Elsevier

Thrombosis • Definition: the pathological process characterized by intravascular clotting in a living person. • Thrombus: intravascular clot • Formed from the constituents of blood • Occurs in an uninjured vessel or after relatively minor injury.

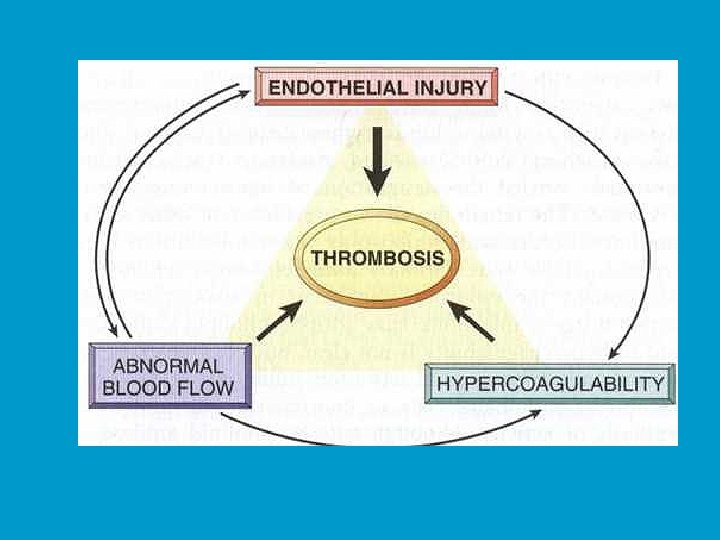
Virchows triad • Endothelial injury • Stasis or abnormal blood flow • hypercoagulability

Endothelium • PROTHROMBOTIC • ANTITHROMBOTIC • v. WF---platelet adherence • Antiplatelet: NO , PGI 2 – vasodilators block platelet adherence & aggregation • Thromboplastin • PAF------fibrin formation • Anti coagulant • Thrombomodulin • Antithrombin III-interferes with clotting • inhibitors pf Plasminogen activator ( PA I)--depresses fibrinolysis • Tissue type Plasminogen activator (t PA) promotes fibrin lysis

Causes of endothelial injury • • Hemodynaminc injury e. g. hypertension Atherosclerosis Inflammation (thrombophlebitis) Autoimmune diseases e. g. Polyarteritis nodosa (PAN) • Metabolic: hyperlipidemia, homocystinemia • Trauma • Infections
Altered blood flow • Turbulent flow (disruption of normal laminar flow)- arterial • stasis (venous) • Platelets & WBC’s in contact with endothelial cells


Effects of altered blood flow • Activation of endothelial cells so that procoagulant > anticoagulant • Prevent removal of platelets and • Prevent fresh anticoagulants from blood reaching endothelium • Stasis-dilated veins • Mechanical damage of endothelium

Altered composition of blood • Hypercoagulability • Heriditary: deficiency of Protein C/S, Factor V Leiden, Antithrombin III (AT III) • Hyperhomocystinemia (acquired or congential ) • Acquired • tissue damage - thromboplastin • Tumour, bacteria, smoking • Autoimmune : SLE, PAN • Antiphospholipid antibodies

Formation of a thrombus • Virchows triad predisposes • Platelets adhering to site of endothelial injury • Fibrin • RBC’s +Fibrin+Platelets • Lines of Zahn • Propogation

Morphology of thrombus • Lines of Zahn platelets+ fibrin alternating with fibrin + RBC’s+ platelets • Attached to vessel wall • Friable along the lines of Zahn • Moulded to blood vessel

Site of Thrombi • Arterial -Coronary, cerebral, femoral • Site of endothelial injury (AS), turbulence (bifurcation) • Venous • Lower extremities(90%)-superficial /deep veins of legs • Ovarian, periuterine, portal hepatic vein in sites of stasis

Site of Thrombi (cont. ) • Cardiac (usual mural) – ventricles: site of endothelial injury, MI, dilated cardiomyopathy – atria: occur in sites of stasis, Atrial Fibrillation • Heart Valves (vegetations) – infective endocarditis – non-bacterial thrombotic endocarditis – Verrucous (Libman-Sacks )endocarditis
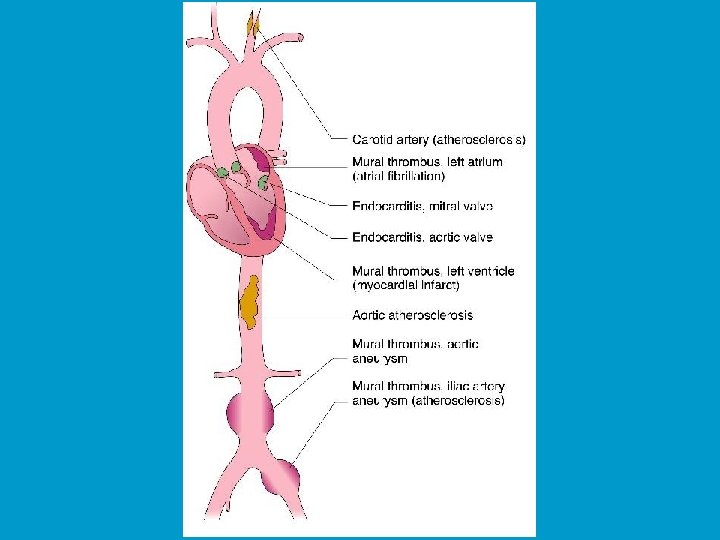

Mural Thrombi Downloaded from: Robbins & Cotran Pathologic Basis of Disease (on 27 June 2005 07: 26 PM) © 2005 Elsevier
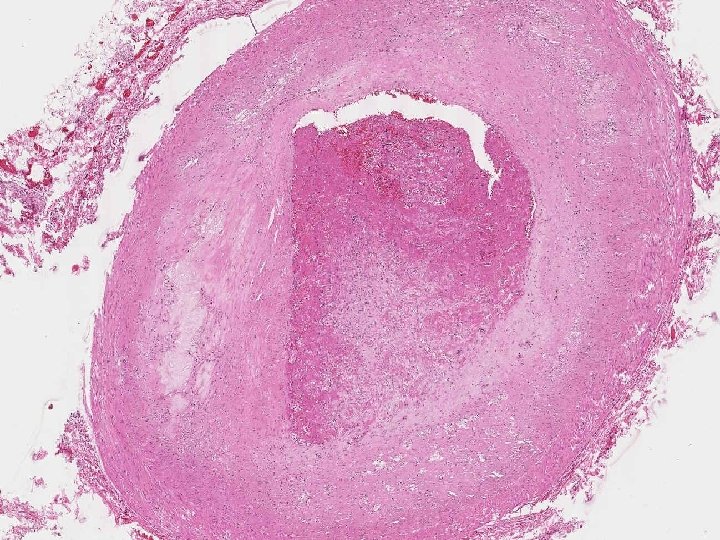
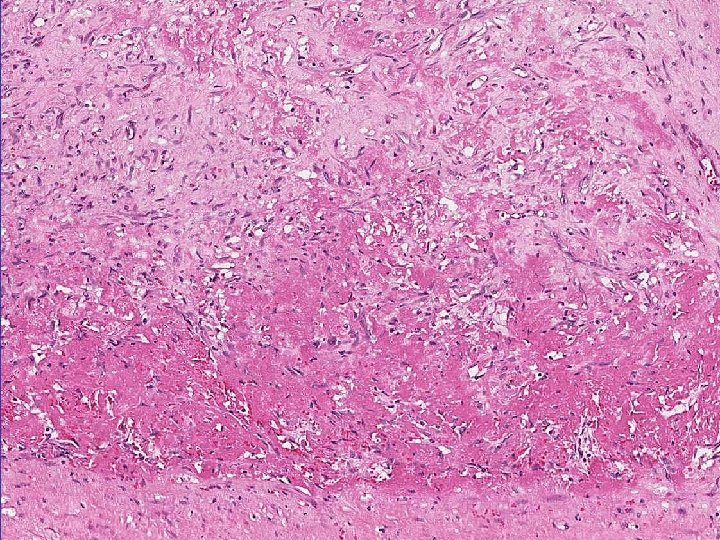

Arterial Vs Venous thrombus • Arterial –lines of Zahn more prominent paler in colour usually occlusive, retrograde propagation • Venous –less prominent lines of Zahn red/ darker in colour(like clotted blood) Invariably occlusive, propagate in direction of blood flow/towards the heart • Post mortem clot: not friable, not attached to blood vessel, currant jelly, chicken fat

Fate of /Outcome of thrombus • Dissolution-fibrinolysis of RECENT thrombi • Propagation-grow downstream • Embolization-detach& travel elsewhere in circulation • Organization-granulation tissue grows into the thrombus • Recanalization-blood vessels fuse into larger channels allowing resumption of blood flow.
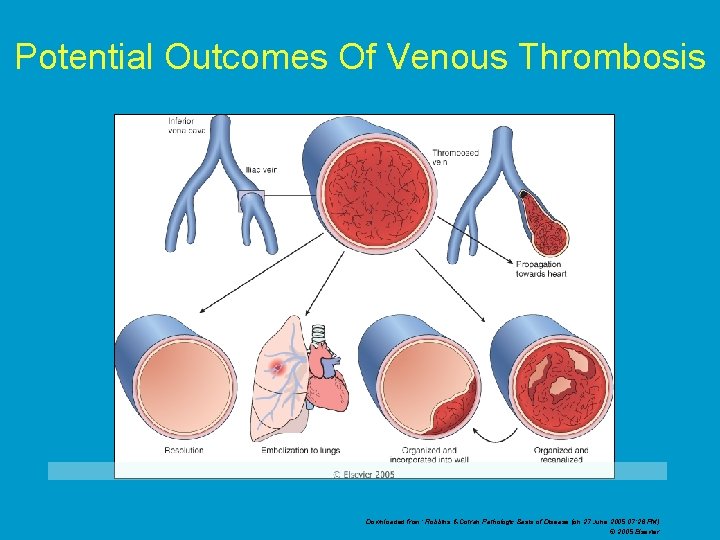
Potential Outcomes Of Venous Thrombosis Downloaded from: Robbins & Cotran Pathologic Basis of Disease (on 27 June 2005 07: 26 PM) © 2005 Elsevier

Common causes of thrombosis • T –Tissue damage • H- Heriditary -deficiency of Protein. C/S, Factor V Leiden, Antithrombin III • R- Rest • O –Obstetric • M- Malignancy (Trosseau syndrome ) • B- Blood flow disturbances • I- Immune mechanisms SLE, Antipholspolipid Ab, PAN

Clinical importance of thrombi • Cause obstruction of arteries and veins • Possible source of emboli

Clinical complications • • Arterial & cardiac thrombosis-Infarction, CAD Systemic Embolization Venous obstruction –Oedema, DVT Pulmonary Emboli Infection –secondary infection, mycotic aneurysm Inflammation of vessel wall –thrombophlebitis Trosseau syndrome-migratory thrombophlebitis associated with internal malignancy due to procoagulant substances.

MCQ’s • In which of the following conditions are lines of Zahn seen? • Post mortem clot • Primary platelet clot • Corraline thrombus • Clot in sample bottle

• In which of the following conditions are lines of Zahn seen? • Post mortem clot • Primary platelet clot • Corraline thrombus √ • Clot in sample bottle

• Which is the earliest step in the formation of a thrombus? • Formation of fibrin • Adherence of platelets to vascular sub endothelium • Activation of clotting factor VII • Trapping of RBC’s

• Which is the earliest step in the formation of a thrombus? • Formation of fibrin • Adherence of platelets to vascular sub endothelium √ • Activation of clotting factor VII • Trapping of RBC’s

SHORT ANSWER QUESTIONS • • Fate of a thrombus Virchows triad Predisposing factors for thrombosis Difference between post-mortem clot and thrombus

CLINICAL IMPORTANCE • Major cause of morbidity and mortality

- Slides: 35