THROMBOSIS DEFINITION PROCESS OF FORMATION OF SOLID MASS

THROMBOSIS DEFINITION PROCESS OF FORMATION OF SOLID MASS IN CIRCULATION FROM THE CONSTITUENTS OF FLOWING BLOOD • THE MASS IS THROMBUS • THE DANGER BEINGISCHEMIC INJURY THROMBOEMBOLISM.
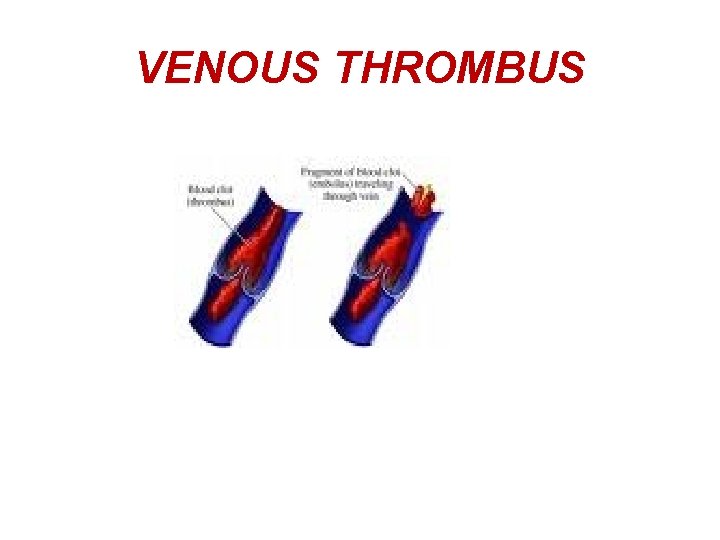
VENOUS THROMBUS
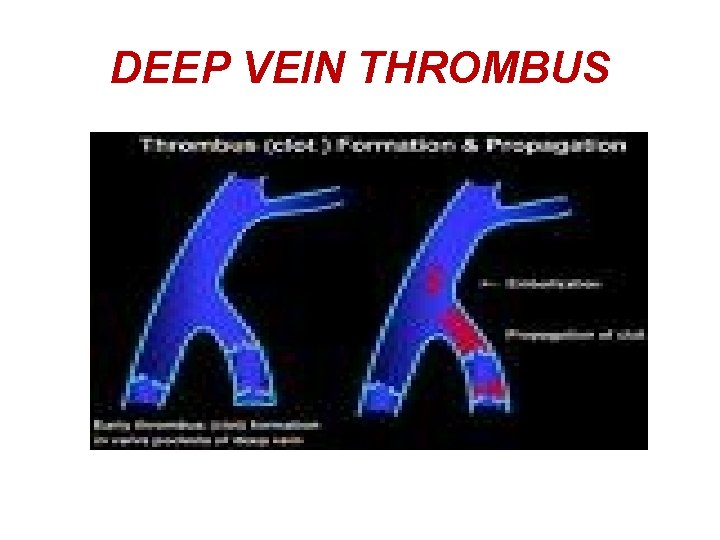
DEEP VEIN THROMBUS
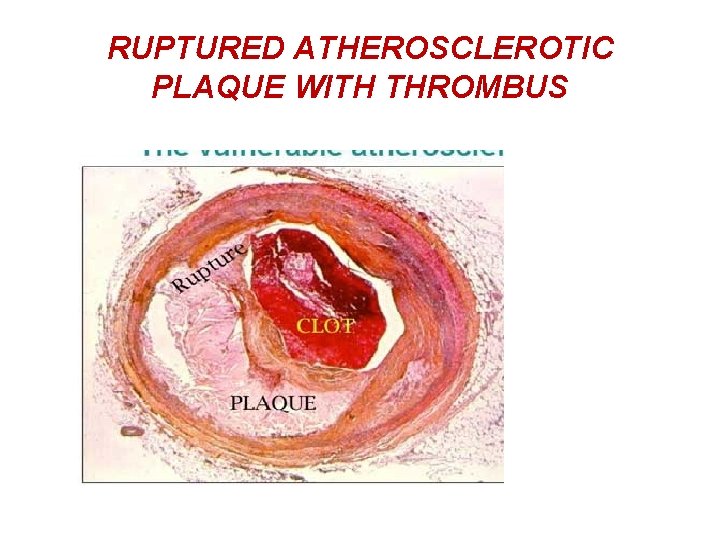
RUPTURED ATHEROSCLEROTIC PLAQUE WITH THROMBUS

FRESH THROMBUS

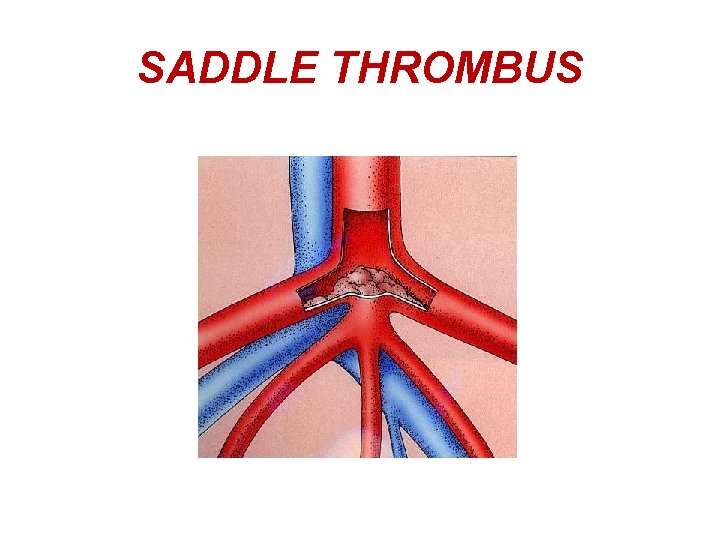
SADDLE THROMBUS
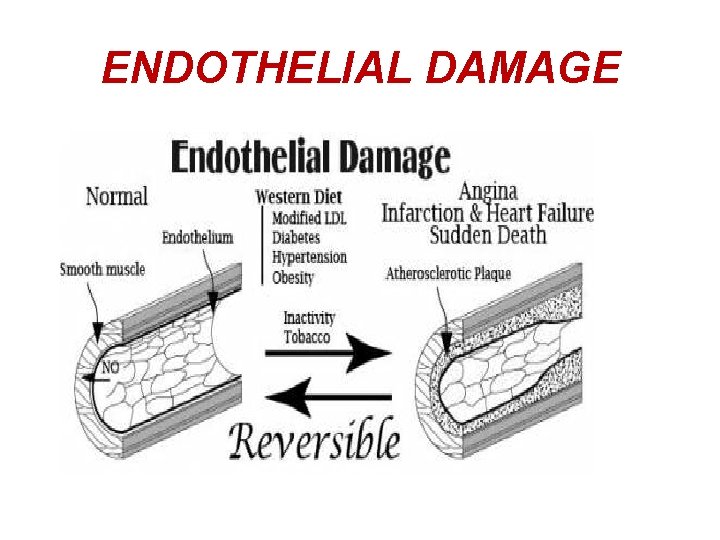
ENDOTHELIAL DAMAGE
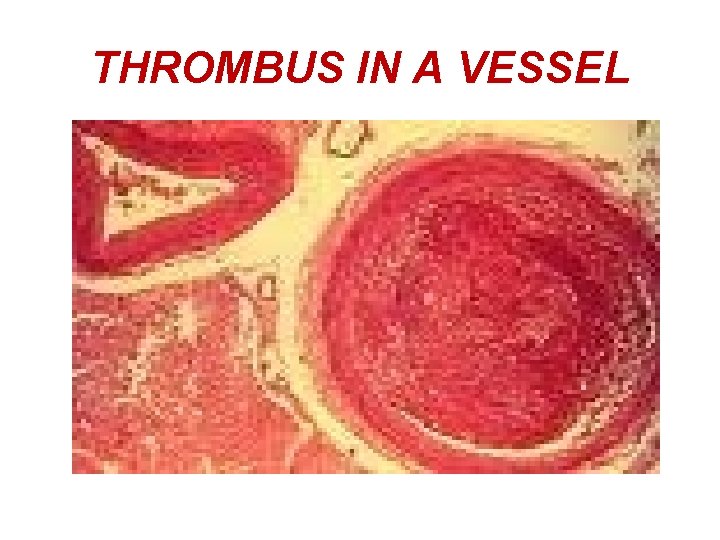
THROMBUS IN A VESSEL
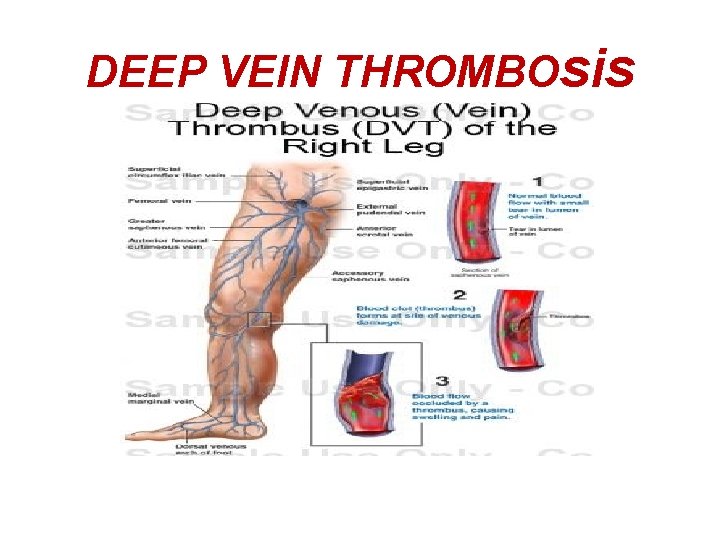
DEEP VEIN THROMBOsis

PATHOPHYSIOLOGY OF THROMBUS VIRCHOW’S TRIAD 1. ENDOTHELIAL INJURY 2. ALTERATION IN BLOOD FLOW 3. HYPERCOAGULABILITY OF THE BLOOD
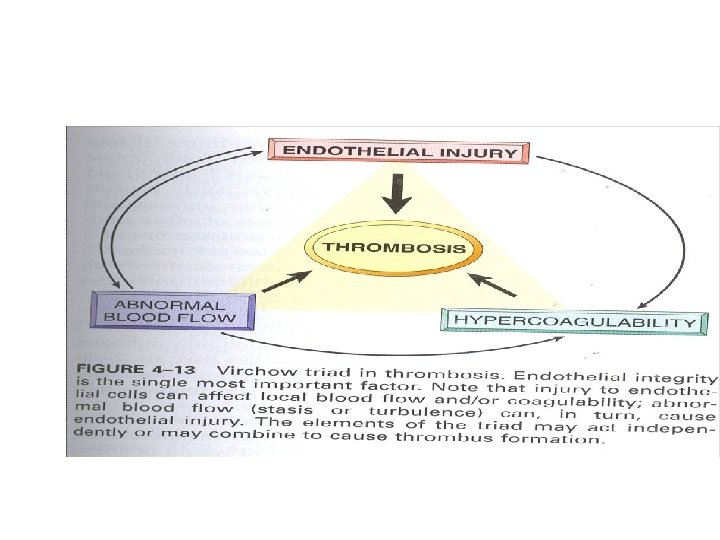

1. ENDOTHELIUM • INTACT ENDOTHELIUM HAS FOLLOWING FUNCTIONS 1. PROTECTS FLOWING BLOOD FROM THROMBOGENIC EFFECTS OF SUBENDOTHELIUM 2. ELABORATION OF ANTITHROMBOTIC FACTORSA. HEPARIN LIKE SUBSTANCE WHICH ACCELERATES THE FUNCTION OF ANTITHROMBIN III & INACTIVATES SOME COAGULATION FACTORS.

ENDOTHELIUM • B. THROMBOMODULIN –CONVERTS THROMBIN TO ACTIVATOR OF PROTEIN C, AN ANTICOAGULANT. • C. INHIBITORS OF PLATELET AGGREGATION SUCH AS ADPase, PGI 2 OR PROSTACYCLIN • D. PLASMINOGEN ACTIVATORFIBRINOLYTIC ACTIVITY

ENDOTHELIUM 3. RELEASE PROTHROMBOTIC FACTORS LIKE A. THROMBOPLASTIN OR TISSUE FACTOR

ENDOTHELIUM • B. von WILLEBRAND FACTOR-CAUSE ADHERENCE OF PLATELETS TO SUBENDOTHELIUM • C. PLATELET ACTIVATING FACTORACTIVATOR & AGGREGATOR OF PLATELETS • D. INHIBITOR OF PLASMINOGEN ACTIVATOR THAT SUPPRESSES FIBRINOLYSIS

ENDOTHELIAL INJURY • MAJOR CAUSE OF THROMBI OF HEART & ARTERIES IS ENDOTHELIAL INJURY • CLINICAL CONDITIONS WHERE ENDOTHELIAL INJURY IS SEEN A. MYOCARDIAL INFARCTION, B. MYOCARDITIS, C. CARDIAC SURGERY, D. PROSTHETIC VALVES

CAUSES OF ENDOTHELIAL INJURY E. ULCERATED PLAQUES, F. HAEMODYNAMIC STRESS IN HYPERTENSION, G. ARTERIAL DISEASES, H. DIABETES MELLITUS,

CAUSES OF ENDOTHELIAL INJURY I. ENDOGENOUS CHEMICAL AGENTS HYPERCHOLESTEROLAEMIA, ENDOTOIXINS, J. EXOGENOUS CHEMICAL AGENTSCIGARETTE SMOKE

2. PLATELETS PLAY A CENTRAL ROLE IN NORMAL HAEMOSTASIS ADHESION TO SUBENDOTHELIAL COLLAGEN Von WILLEBRANDS FACTOR IS REQUIRED FOR PLATELET ADHESION PLATELET ACTIVATIONPLATELET RELEASE REACTIONGRANULES ARE RELEASED

ROLE OF PLATELETS PLATELET AGGREGATION BY ADP FROM DENCE BODIES (PLATELET GRANULES) – TEMPORARY HAEMOSTATIC PLUG

3. COAGULATION SYSTEM 1. INTRINSIC PATHWAYCONTACT WITH ABNORMAL SURFACE - ACTIVATION OF F-12 & SEQUENTIAL INTERACTIONS OF FACTORS XI, IX, VIII & FINALLY F- X

3. COAGULATION SYSTEM 2. IN THE EXTRINSIC PATHWAY TISSUE DAMAGE-RELEASE OF TISSUE FACTOR OR THROMBOPLASTIN WHICH INTERACT WITH F – VII AND CALCIUM IONS – ACTIVATES FACTOR X

COAGULATION SYSTEM 3. COMMON PATHWAY-BEGINS WHERE BOTH INTRINSIC & EXTRINSIC PATHWAYS CONVERGE TO ACTIVATE FACTOR X WHICH FORMS COMPLEX WITH F - Va & PLATELET FACTOR 3 IN THE PRESENCE OF CALCIUM IONS.

COAGULATION SYSTEM • THIS COMPLEX ACTIVATES PROTHROMBIN (F-II) TO THROMBIN(FIIa)

REGULATORS OF COAGULATION SYSTEM • 1. PROTEASE INHIBITORS-ACT ON COAGULATION FACTORS & OPPOSE THE FORMATION OF THROMBIN PROTEASE INHIBITORS ARE - ANTITHROMBIN III, PROTEIN C, C 1 INACTIVATOR, α 1 -ANTITRYPSIN, α 2 -MACROGLOBULIN

REGULATORS OF COAGULATION SYSTEM 2. FIBRINOLYTIC SYSTEMPLASMINOGEN ACTIVATOR CONVERTS PLASMINOGEN TO PLASMIN A FIBRINOLYTIC ENZYME RELEASING FIBRIN SPLIT PRODUCTS.

2. HYPERCOAGULABILITY OF THE BLOOD 1. NEPHROTIC SYNDROME 2. ADVANCED CANCER 3. EXTENSIVE TRAUMA, BURNS, PUERPERIUM.

HYPERCOAGULABILITY OF THE BLOOD COAGULATION IS FAVOURED BY ADVANCED AGE, SMOKING, USE OF ORAL CONTRACEPTIVES & OBESITY.

HYPERCOAGULABILITY OF THE BLOOD HYPERCOAGULABILITY MAY BE a. DUE TO INCREASE COAGULATION FACTORS, b. INCREASE IN PLATELET COUNT

HYPERCOAGULABILITY OF THE BLOOD WITH INCREASE IN THEIR ADHESSIVENESS C. DECREASED LEVELS OF COAGULATION INHIBITORS SUCH AS ANTI -THROMBIN III, FIBRIN SPLIT PRODUCTS
3. ALTERATION OF BLOOD FLOW FORMATION OF ARTERIAL & CARDIAC THROMBI IS FACILITATED BY TURBULENCE IN BLOOD FLOW(NORMAL AXIAL FLOW IS DISTURBED) STASIS INITIATES THE VENOUS THROMBI EVEN WITHOUT ENDOTHELIAL INJURY.

TYPES OF THROMBI AND THEIR MORPHOLOGY • THROMBI OCCUR IN HEART, ARTERIES, VEINS & CAPILLARIES • ARTERIAL THROMBI PRODUCE ISCHEMIA & INFARCTION • CARDIAC & VENOUS THROMBI CAUSE EMBOLISM.

MORPHOLOGY OF THROMBI GROSS- VARIES IN SIZE, , SHAPE, COMPOSITION DEPENDING ON THE SITE OF ORIGIN

MORPHOLOGY OF THROMBI ARTERIAL THROMBI ARE WHITE & MURAL, ARE FIRM & PALE • VENOUS THROMBI - RED & OCCLUSIVE, SOFT & GELATINOUS

MORPHOLOGY OF THROMBI DEPENDS ON RATE OF FLOW OF BLOOD RAPID ARTERIAL & CARDIAC CIRCULATION - LINES OF ZAHNALTERNATE LAYERS OF LIGHT STAINING PLATELET AGGREGATES WITH FIBRIN & DARK STAINING LAYERS OF RED CELLS

LINES OF ZAHN-

LINES OF ZAHN-
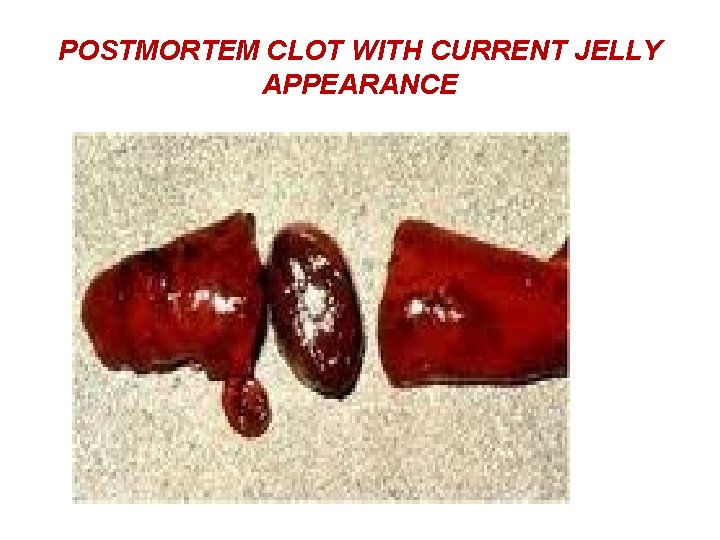
POSTMORTEM CLOT WITH CURRENT JELLY APPEARANCE

POSTMORTEM CLOT WITH CHICKEN FAT AND CURRENT JELLY APPEARANCE

MORPHOLOGY OF THROMBI • SLOW MOVING FLOW IN VEINS- RED THROMBIABUNDANT RED CELLS, LEUCOCYTES & PLATELETS TRAPPED IN FIBRIN MESHWORK.
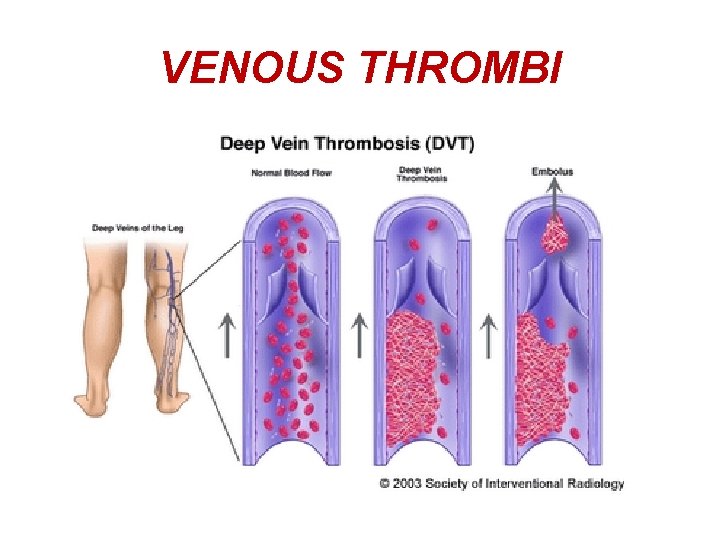
VENOUS THROMBI
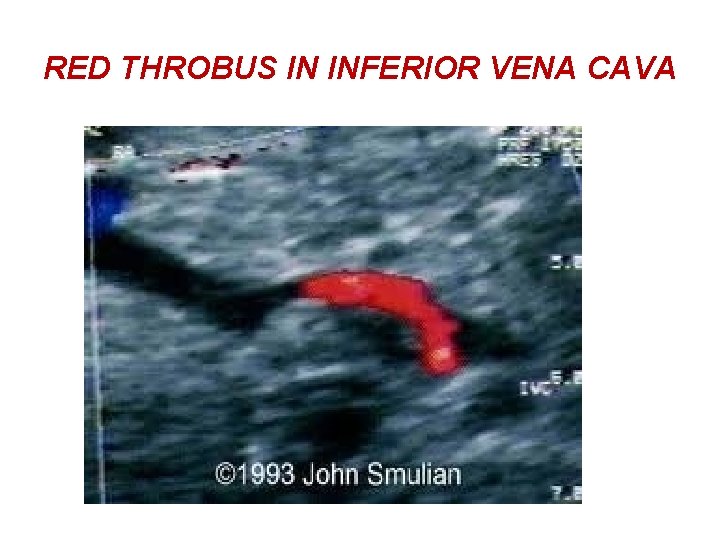
RED THROBUS IN INFERIOR VENA CAVA
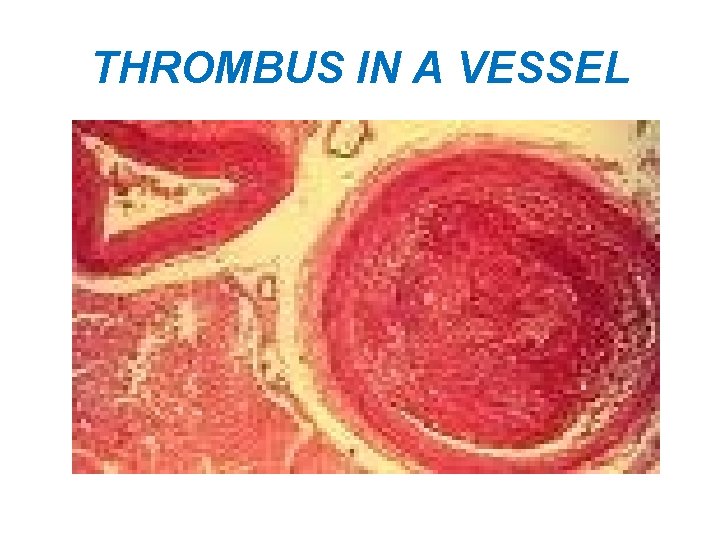
THROMBUS IN A VESSEL
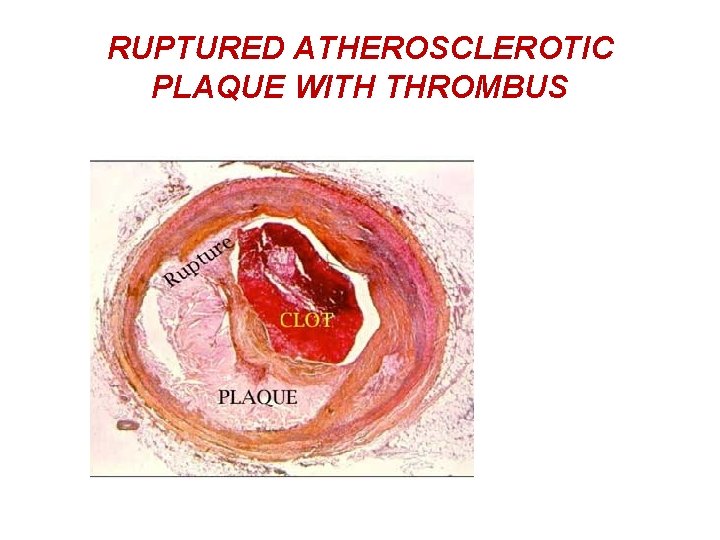
RUPTURED ATHEROSCLEROTIC PLAQUE WITH THROMBUS

ANTIMORTEM THROMBI & POSTMORTEM CLOTS • ANTIMORTEM THROMBI- GROSSDRY, GRANULAR, FIRM, FRIABLE, ADHERENT TO VESSEL WALL, MAY OR MAY NOT FIT THEIR VASCULAR CONTOURS, LINES OF ZAHNS PRESENT

ANTIMORTEM THROMBI & POSTMORTEM CLOTS • POSTMORTEM CLOT- GROSSLY GELATINOUS, SOFT, RUBBERY, NOT ATTACHED TO THE VESSEL WALL, TAKES THE SHAPE OF THE VESSEL WALL OR IT’S BIFURCATION, • THE SURFACE IS CHICKEN FAT YELLOW COVERING THE UNDERLYING RED CURRENT JELLY

FATE OF THROMBI 1. RESOLUTION- ACTIVATION OF FIBRINOLYTIC SYSTEM-RELEASE OF PLASMIN-DISSOLVE THROMBUS, PHAGOCYTES PHAGOCYTOSE THROMBUS , PROTEOLYTIC ENZYMES FROM LEUCOCYTES & ENDOTHELIUM DIGEST THE COAGULUM

FATE OF THROMBI • 2. ORGANISATION - CAPILLARIES GROW, FIBROBLASTS GROW TO PRODUCE GRANULATION TISSUECOLLAGENOUS TISSUE COVERED BY ENDOTHNELIUM- RECANALISATION HYALINISATION , CALCIFICATION TO FORM PHLEBOLITHS.
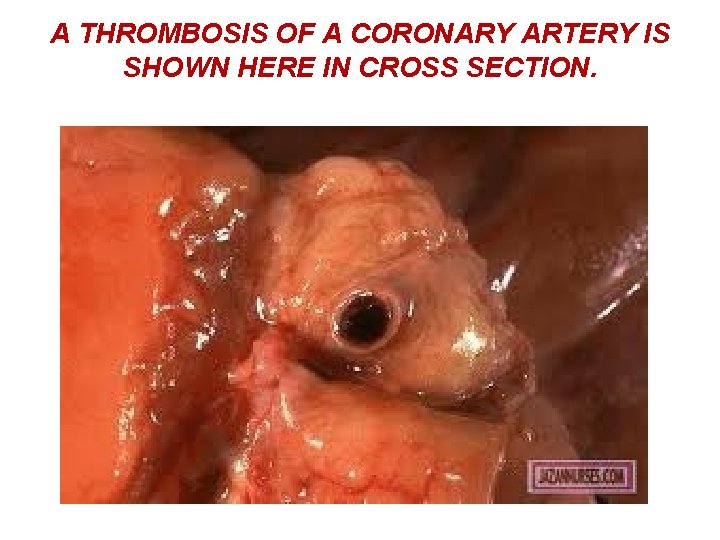
A THROMBOSIS OF A CORONARY ARTERY IS SHOWN HERE IN CROSS SECTION.
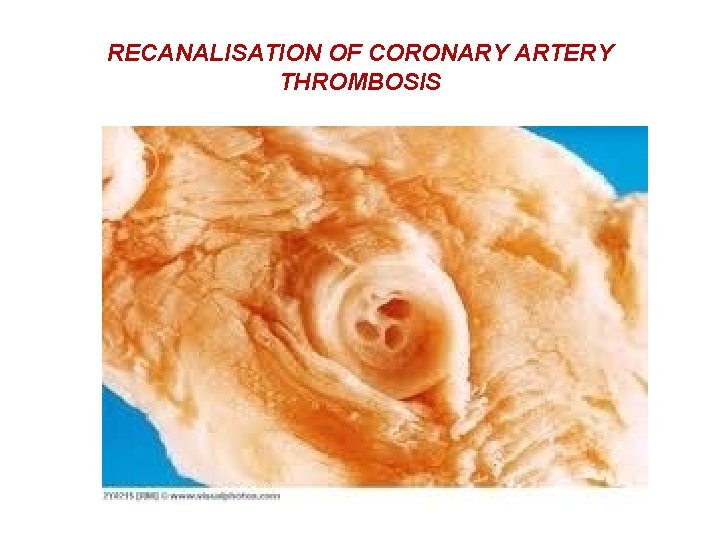
RECANALISATION OF CORONARY ARTERY THROMBOSIS

FATE OF THROMBUS 3. PROPAGATION- THROMBUS MAY ENLARGE IN SIZE DUE TO MORE & MORE DEPOSITION OF CONSTITUENTS OF BLOOD
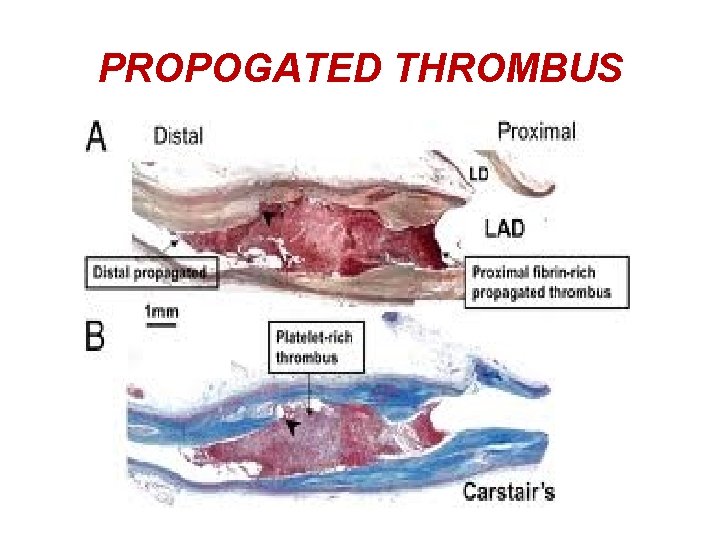
PROPOGATED THROMBUS

FATE OF THROMBUS MAY CAUSE OBSTRUCTION TO SOME IMPORTANT VESSEL 4. THROMBOEMBOLISMGET DETACHED FROM VESSEL WALL, RELEASED INTO BLOOD STREAM AS EMBOLI.
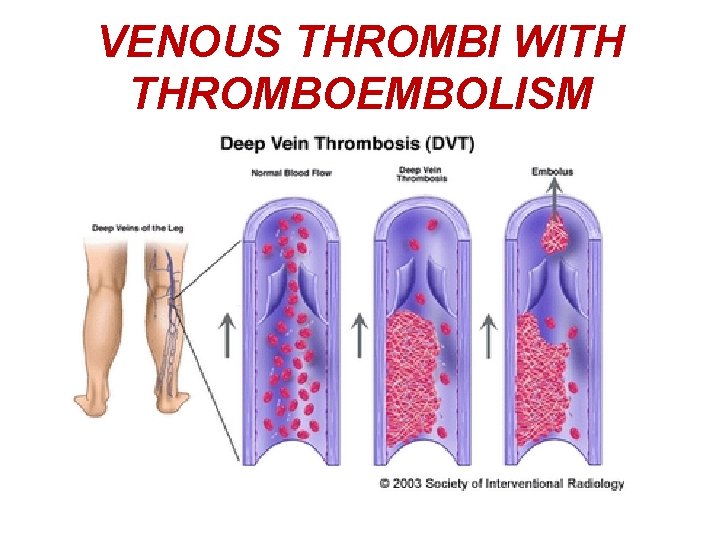
VENOUS THROMBI WITH THROMBOEMBOLISM

FACTORS PREDISPOSING TO THROMBOSIS • 1. GENETIC(PRIMARY) FACTORSa. DEFICIENCY OF ANTITHROMBIN, PROTEIN C OR S, b. DEFECTS IN FIBRINOLYSIS c. MUTATION IN FACTOR V

FACTORS PREDISPOSING TO THROMBOSIS • 2. ACQUIRED (SECONDARY ) FACTORSA - RISK FACTORSADVANCED AGE, PROLONGED BED REST, IMMOBILISATION, USE OF ORAL CONTRACEPTIVES, CIGARETTE SMOKING, TISSUE DAMAGE (TRAUMA, FRACTURE, BURNS)

FACTORS PREDISPOSING TO THROMBOSIS • CLINICAL CONDITIONS PREDISPOSING TO THROMBOSIS a. HEART DISEASES- MI, CHF, MITRAL STENOSIS, CARDIOMYOPATHY b. ATHEROSCLEROSIS,

FACTORS PREDISPOSING TO THROMBOSIS c. ANEURYSMS OF AORTA & OTHER VESSELS, VARICOSITIES OF LEG VEINS d. NEPHROTIC SYNDROME,

FACTORS PREDISPOSING TO THROMBOSIS f. DISSEMINATED CANCERS, g. LATE PREGNANCY & f. PUERPERIUM.

CLINICAL EFFECTS OF THROMBOSIS • DEPENDS ON SITE OF THROMBI, RAPIDITY OF FORMATION & NATURE OF THROMBI • 1. CARDIAC THROMBI- SUDDEN DEATH • 2. ARTERIAL THROMBI - INFARCTIONLEADING TO GANGRENE, SUDDEN DEATH IN CASE OF CORONARY ARTERY THROMBOSIS

CLINICAL EFFECTS OF THROMBOSIS • 3. VENOUS THROMBITHROMBOEMBOLISM, OEDEMA, POOR WOUND HEALING, SKIN ULCERS, PAINFUL THROMBOSED VEINS(THROMBOPHLEBITIS),

CLINICAL EFFECTS OF THROMBOSIS PAINFUL WHITE LEG (PHLEGMASIA ALBA DOLENS) DUE TO ILEOFEMORAL VENOUS THROMBOSIS IN POSTPARTUM CASES, THROMBOPHLEBITIS MIGRANS IN CANCER ( TROUSSEAU SIGN )

CLINICAL EFFECTS OF THROMBOSIS • 4. CAPILLARY THROMBI- MAY GIVE RISE TO DIC

DISSEMINATED INTRAVASCULAR COAGULATION DEFIBRINATION SYNDROME OR CONSUMPTION COAGULOPATHY IS A COMPLEX THROMBOHAEMORRHAGIC DISORDER (INTRAVASCULAR COAGULATION AND HAEMORRHAGE)

DISSEMINATED INTRAVASCULAR COAGULATION • ETIOLOGY 1. MASSIVE TISSUE INJURY- IN OBSTETRICAL SYNDROMESa. ABRUPTIO PLACENTAE,

DISSEMINATED INTRAVASCULAR COAGULATION b AMNIOTIC FLUID EMBOLISM, c. RETAINED DEAD FETUS, OTHER CONDITIONS LIKE MASSIVE TRAUMA, METASTATIC MALIGNANCIES, SURGERY

DIC • 2. INFECTIONS - ENDOTOXAEMIA, GRAM-NEGATIVE AND MENINGOCOCCAL SEPTICAEMIA, CERTAIN VIRAL INFECTIONS, MALARIA, ASPERGILLOSIS

DIC • 3. WIDESPREAD ENDOTHELIAL DAMAGEAORTIC ANEURYSM, HAEMOLYTIC URAEMIC SYNDROME, SEVERE BURNS, ACUTE GLOMERUONEPHRITIS

ETIOLOGY OF DIC 4. MISCELLANEOUS CAUSES LIKE SNAKE BITE , SHOCK, HEAT STROKE, ACUTE INTRAVASCULAR HAEMOLYSIS

PATHOGENESIS OF DIC -4 PHASES 1. ACTIVATION OF COAGULATIONETIOLOGIC FACTORS LISTED ABOVE INITIATE WIDESPREAD ACTIVATION OF COAGULATION PATHWAY BY RELEASE OF TISSUE FACTOR

PATHOGENESIS OF DIC-4 PHASES 2. THROMBOTIC PHASEENDOTHELIAL DAMAGE-PLATELET AGGREGATION AND ADHESION – DEPOSITION OF SMALL THROMBI AND EMBOLI THROUHOUT THE MICROVASCULATURE

DIC 4 PHASES 3. CONSUMPTION PHASE – CONSUMPTION OF COAGULATION FACTORS AND PLATELETS 4. SECONDARY FIBRINOLYSISPROTECTIVE MECHANISM AT THE SITE OF INTRAVASCULAR COAGULATION- FIBRIN SPLIT PRODUCTS

DIC CLINICAL FEATURES OF DIC 2 MAIN FEAURES OF DIC ARE 1. BLEEDING 2. ORGAN DAMAGE DUE TO ISCHEMIA 3. MICROANGIOPATHIC HAEMOLYTIC ANAEMIA 4. THROMBOSIS IN LARGER ARTERIES AND VEINS

LABORATORY INVESTIGATIONS IN DIC 1. PLATELET COUNT – LOW 2. PERIPHERAL SMEAR- FEATURES OF MICROANGIOPATHIC ANAEMIASCHISTOCYTES-DAMAGE TO RBCS CAUSED BY TRAPPING AND PASSAGE THROUGH THE FIBRIN THROMBI

LABORATORY FINDINGS IN DIC 3. PROTHROMBIN TIME , THROMBIN TIME, ACTIVATED PARTIAL THROMBOPLASTIN TIME ARE ALL PROLONGED

LABORATORY FINDINGS IN DIC 4. PLASMA FIBRINOGEN LEVELSREDUCED DUE TO CONSUMPTION COAGULOPATHY 5. FIBRIN DEGRADATION PRODUCTS - ARE RAISED DUE TO FIBRINOLYSIS
- Slides: 77