Thrombophilia A pediatric perspective Craig Dobson MD CPT

Thrombophilia A pediatric perspective. Craig Dobson, MD CPT, MC, USAR NCC Pediatrics Residency Program

Definitions l Unexpected tendency to form clots under inappropriate circumstances. l Family history of vascular disease under age 50. Incl. MI, CVA or DVT.

Case l 9 yo male at presents for eval for psych admission to CNMC for acute psychosis. l Disorganized behavior, non-communicative except occasional screaming fits. l Associated symptoms headache, high fevers, occasional watery stools. l Head CT with contrast notes lateral venous sinus thrombosis. But why?

Epidemiology l Venous thrombosis lifetime prevalence 510% of total population. l Highest incidence in neonatal and postpubertal. l Neonates 5/100 k. l Teens incidence 23/100 k.

Neonatal Presentation Typically in-utero or within first 48 hrs of life. l Catheter thrombosis. l – Still requires evaluation. l Renal vein thrombosis – Flank mass on exam – Thrombocytopenia, HTN, hematuria. Seizures from CVA or lesion on head U/S. l Neonatal Purpura Fulminans l – Homozygous Protein C or S def.

Adolescent Presentation l DVT l CVA l Asymptomatic, suspected through FHx. l Important to screen to avoid sudden death early in adulthood.
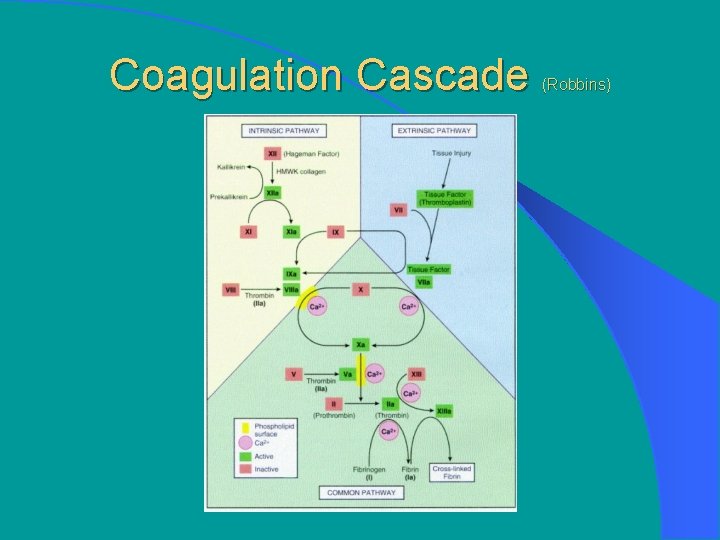
Coagulation Cascade (Robbins)
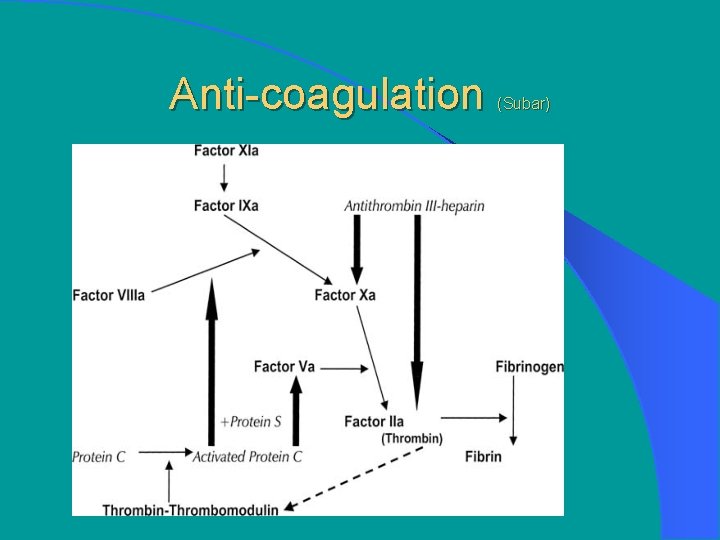
Anti-coagulation (Subar)
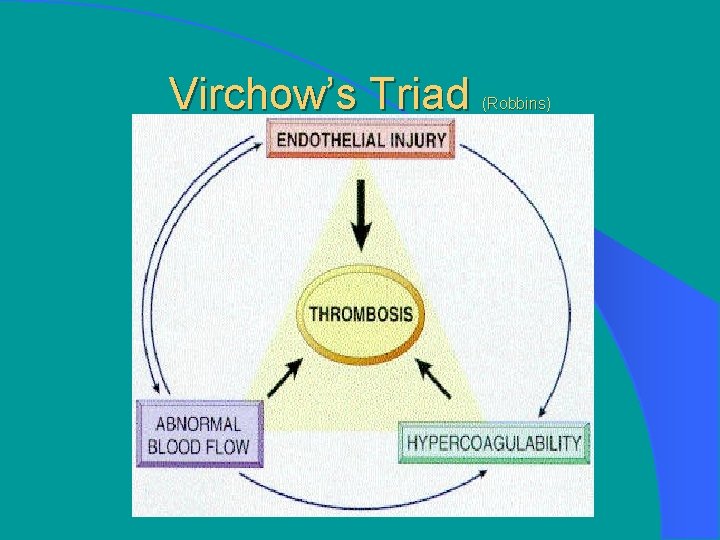
Virchow’s Triad (Robbins)

Work Up l l l l PT/PTT, Mixing studies if elev PTT. CBC ATIII, Protein C&S (total and free) Factor V Leiden Homocysteine level or MTHFR gene mutation Prothrombin G 20210 A gene mutation Anti-phospholipid Abs Lipoprotein a

Etiology/Genetic l Excessive factor VIII (11/100 whites) l Factor V Leiden (8/100 whites) l Prothrombin excess (2/100 whites) l Antithrombin III def. (1/5000)

Etiology/Genetic l Sickle cell disease (1/400 blacks) l Protein C deficiency (1/500) l Protein S deficiency l Rare conditions: Def in fibrinolysis, congenital HUS, pro-coagulant platelets.

Etiology/Acquired l Platelets and RBCs – Polycythemia/thrombocythemia – TTP, HUS l Excess Thrombin – Factor V Leiden – Lupus anticoagulant/ anti-cardiolipin – Incr tissue factor (infection/trauma/malignancy)

Etiology/Acquired l Def thrombin regulation – ATIII deficiency (renal failure) – Hepatic synthetic dysfunction. – Auto-antibodies – DIC l Medications – OCPs – Heparin – L-asp (really hepatic synth. )

Etiologies/Acquired l Homocysteinemia – Smoking – Sedentary lifestyle – Coffee – Diet (low folate, B 6 or B 12)

Therapies/Heparin l Mechanism: catalysis of AT. l Neonates have lower AT levels. l Monitoring: a. PTT l Problems – a. PTT levels based on adult therapeutic studies. – Even in adults, therapeutic a. PTT may not suggest clinically sufficient anti-coag.

Therapies/Heparin l Recommended dose 75 U/kg loading. l Maintenance drip dose varies: – Infants <1 yr of age 28 U/kg/hr – Children > 1 yr 20 U/kg/hr l Side effects (besides bleeding): – Heparin induced thrombocytopenia – Osteoporosis

Therapies/ LMWH l Low Molecular Weight Heparin l Less monitoring needed, more predictable blood levels, less osteoporosis. l Increase dose needed for age <2 mo (0. 75 mg Q 12). >2 mo (0. 5 mg) l Monitor anti-factor Xa levels. – In children you need to monitor , unlike adults. – Peak is 2 -6 hrs after injection SQ.

Therapies/Oral-anticoagulants l Increases vitamin-K dependent proteins (II, VII, IX, X) plus Proteins C & S. l Newborns have reduced levels of vitamin-K dependent proteins. (Shot at birth helps. ) l Vitamin K added to formulas. l Minimal in breastmilk.

Therapies/Oral Anticoagulants l Monitor INR 2 -3. l Problem: requires stable diet. Impossible in 2 yr old. l Some recommend INR 1. 5 -2. 5. l Large difference in required dose: – Infants 0. 32 mg/kg/d – Teens 0. 09 mg/kg/d

Case Revised l Etiology thought originally to be erosive mastoiditis due to fluid in mastoid near lateral venous sinus. l Mastoidectomy performed, culture negative transudate. l Further testing by GI, revealed pt with early presentation of Crohn’s disease.

References Manco-Johnson, M & Nuss, R. Advances in Pediatrics, Chp 12, Vol 48. 2001. ) l Monagle, et al. Antithrombotic Therapy in Children. Chest. 119 (1), 2001. l Cotran: Robbins Pathologic Basis of Disease, 1999 (all images). l Subar M - Clin Geriatr Med - 01 -Feb-2001; 17(1): 57 -70, vi Van Cott, E. Coagulation disorders and treatment strategies: laboratory evaluation of hypercoagulable states. Hematology/oncology Clinics of North Amer. V 12 (6), 1998. l
- Slides: 22