Thromboembolic disease Thromboembolic disease remains the third leading

Thromboembolic disease • -Thromboembolic disease remains the third leading cause of direct maternal death • -The pregnant woman increased risk of developing venous thromboembolism (VTE) compared with the non-pregnant • which rises in the puerperium

Thromboprophylaxis in pregnancy • • Risk f a ct o r s f o r v e no us t hr o m bo e m bo lism Pre-existing factors – Previous VTE – Family history of VTE (e. g. deficiency of protein C or S, antithrombin deficiency, prothrombin gene variant, Factor V Leiden) – Known thrombophilia – Lupus anticoagulant – Medical co-morbidities (e. g. sickle cell disease, cardiac disease, proteinuria >3 g/day) – Age >35 years – Obesity (BMI >30 kg/m 2) – Parity >3 – Smoking – Intravenous drug user – Varicose veins

• • • Obstetric factors – Pre-eclampsia – Dehydration/hyperemesis gravidarum – Multiple pregnancy – Caesarean section or forceps delivery – Prolonged labour – Postpartum haemorrhage Transient factors – Systemic infection – Paraplegia or immobility – Recent surgical procedure – Ovarian hyper stimulation syndrome – Travel >4 hours • midwife should perform and document this risk assessment on the following occasions: • initial meeting with the woman (booking visit) • any hospital admission • following the birth of the baby.

• -If this assessment identifies women at risk of developing VTE, the midwife should promptly refer her to a consultant-led maternity unit with an expert in thrombosis in pregnancy • - The woman is likely to be commenced on subcutaneous injections of low molecular weight heparin (LMWH), as this does not cross the placental barrier with consequential effects on the fetus.

• -The midwife, or specialist nurse, should educate the woman in self-administration of the heparin, alerting her to carry a medical alert card containing such details with her at all times. • -The woman should be provided with a sharps bin for safe disposal of the injection devices. • -Gradient compression stockings or TED stockings are likely to be prescribed. Such stockings are available in two lengths, below the knee or thigh, and are designed to give a pressure gradient from the ankle to the knee or thigh that mimics the pumping action of the deep leg vein calf muscles, with the highest pressure being at the ankle.

• -It is important that the woman is measured correctly around the ankle and calf or thigh circumference depending upon the type of stocking prescribed • -Midwives should be trained in their use to be able to instruct the woman how to wear them correctly and monitor their use • -For hygiene purposes, stockings should be removed daily, but this should be no more than 30 minutes. • -The legs should be inspected and measured by the midwife every three days to detect any changes in size or tissue damage

• -The woman should be given advice about avoiding dehydration, ceasing smoking and eating a healthy diet. • - If the pregnant woman is expecting to travel long distances, especially by air, she will benefit by wearing loose fifing clothing and flight socks (TED stockings), drinking plenty of water, avoiding alcohol and remaining ambulant for as long as possible/performing leg exercises when at rest. • -During labour, the midwife should encourage mobility with regular changes of position and passive leg exercises when the woman is at rest.

• -It is important that hydration is maintained and regular observations are undertaken, including frequent examination of the woman's legs. • - If the woman has been prescribed LMWH in pregnancy, this should be omifed at the onset of contractions and regional anesthesia avoided within 12 hours of the last administered dose. • -There should be active management of the third stage of labour with the oxytoxic drug being administered IV. If

• -perineal suturing is required, the midwife should undertake this promptly to avoid the woman being in the lithotomy position for a prolonged time, as this further increases the risk for deep vein thrombosis (DVT). • - If surgery is necessary, intermifent calf compression will be required in theatre. • -The postnatal period presents further risk to the woman for both DVT and pulmonary embolism (PE), and early mobilization should be encouraged. • -Routine postnatal observations are important, especially respiration rate and the development of any leg swelling. • - If either condition is suspected the woman must be referred urgently to a haematologist, or if at home she must be readmitted to hospital.

Deep vein thrombosis • -A blood clot formed within a blood vessel is termed a thrombus, which can become detached and lodge in another blood vessel and partially or wholly occlude it. • -Virchow's triad ( • -In pregnancy, Virchow's triad is affected by the physiological changes to the hematological system • -Despite pregnancy presenting a state of hypervolaemia, by term hypercoagulability also develops to compensate for the demands of the forthcoming labour and maintenance of haemostasis.

• - In addition, there is relative venous stasis with a gradual 50% reduction in venous flow velocity, reaching its peak at 36 weeks and declining to pre-pregnancy values by 6 weeks following the baby's birth • -Furthermore, the physical effect of the gravid uterus exerts pressure on the pelvic veins and the inferior vena cava, increasing the woman's risk of developing a DVT in the veins of the calf, thigh and pelvis

• -In pregnancy, 90% of DVT occur in the leh leg compared with 55% in the non-pregnant woman due to compression of the leh iliac vein by the leh iliac artery in pregnancy • -The ileofemoral veins are the most common location, having 70% of pregnancy occurrences versus 9% in the non-pregnant woman, and are more likely to result in pulmonary embolism • -The complications of DVT are pulmonary embolism (PE) and post-thrombotic syndrome

• arising from damage to the venous valves that result in a backflow of blood, venous hypertension, oedema and tissue hypoxia. • -The midwife needs to be aware of the signs of DVT (listed below) as she may be the first person to identify this when undertaking an antenatal or postnatal examination on the woman:

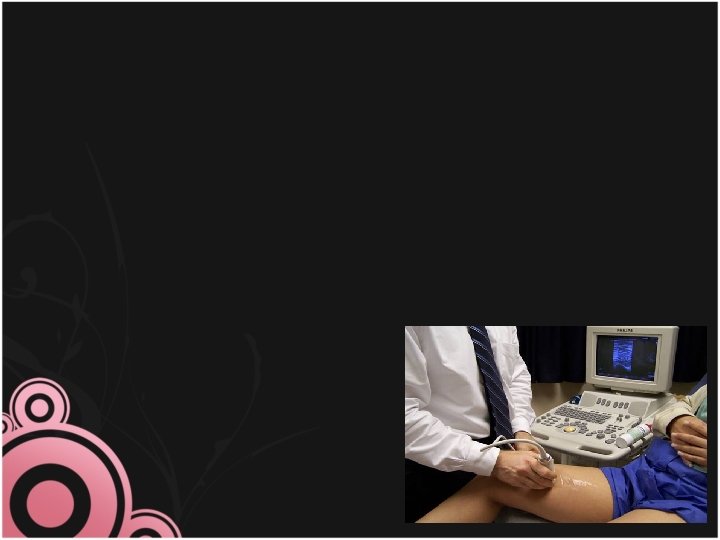
pain in the area of the clot swelling (usually one-sided) red discoloration difficulty in weight-bearing on the affected leg low grade pyrexia lower abdominal or back pain. -If the leg appears swollen a tape measure should be used to assess the circumference of both legs at the affected area for comparison. • - A DVT is potentially life threatening and the midwife must refer the woman immediately to hospital for medical examination, investigation and treatment. • •

• The classic diagnostic use of dorsiflexion of the foot (Homan's sign) is considered unreliable in pregnancy and the presence of severe lower back pain has greater significance • Medical investigations involve Doppler ultrasound and serum investigations might be performed; however, debate the usefulness of measuring D-dimers levels in pregnancy. Venography is generally avoided in pregnancy due to the small radiation risk to the fetus. • -Treatment of DVT in pregnancy is with LMWH administered 12 -hourly by subcutaneous injection to sustain the levels, and which should continue for at least 6 months aher the diagnosis. • -Gradient compression stockings should be prescribed and the woman taught how to put them on.

• -The woman will need to wear one on the affected leg for two years to reduce the risk of post-thrombotic syndrome Anticoagulation therapy should continue for at least 6 months aher the diagnosis (RCOG 2010 a). • -The woman should be seen by the anaesthetist prior to labour to discuss the risks that thromboembolic disorders have on the administration of regional/general anaesthesia. • - As soon as labour commences, heparin should be omifed and compression stockings should be worn. • - As regional anaesthesia carries a risk of spinal bleeding, this should be avoided within 12 hours of administration of heparin. • -Although general anaesthetic is itself a thrombotic risk, it may have to be considered for caesarean section.


• -The woman should be encouraged to remain mobile or undertake passive leg exercises and maintain hydration. • - An IVI should be sited, and drugs given IV instead of intramuscularly (IM). • - Prolonged use of the lithotomy position should be avoided, as this is a DVT risk. • - The third stage of labour should be actively managed with the oxytoxic drug being administered IV to prompt haemostasis. • - If perineal suturing is required, it should be undertaken promptly to limit the length of time the woman is in the lithotomy position • -The midwife should be aware that there is a 25 -fold increased risk of DVT and the • -potential for PE during the postnatal period.

• - As a consequence, the woman who has had a previous DVT is especially at high risk and thus the midwife is required to be particularly vigilant is assessing her condition, encouraging early ambulation and hydration. • - Heparin is recommenced as directed by the medical team. • - This is usually 2 hours aher a vaginal birth or longer if the woman had an epidural and/or caesarean section, and should continue until at least the 6 -week postnatal appointment, at which point a decision to change to warfarin may be made (. – • -Oestrogen-based contraceptive pills are contraindicated so depo-provera or barrier methods of contraception should be discussed with the woman and her partner.

Pulmonary embolism • -Pulmonary embolism (PE) occurs when a DVT detaches and becomes mobile, known as an embolus. • - A large embolus might lodge in the pulmonary artery and smaller ones can travel distally to small vessels in the lung periphery, where they may wholly or partially occlude the blood vessel • . Initially the lung tissue is ventilated but not perfused, producing intrapulmonary dead space, and there is impaired gaseous exchange • -Aher some hours, surfactant production by the affected lung ceases, the alveoli collapse and hypoxaemia results.

• - Pulmonary arterial pressure rises and there is a reduction in cardiac output. • -The area of the lung affected by the embolism may become infracted; however, in some instances, oxygenation of tissue continues to some extent from the bronchial circulation and airways.

• -In the case of a small embolism, there is likely to be dyspnoea, discomfort or pain in the chest, haemoptysis and low grade pyrexia, all of which can be misdiagnosed as a chest infection. Cardiovascular examination is usually normal • -A larger embolism that occludes a major vessel will result in a more acute presentation, because of sudden obstruction of the right ventricle and its outflow. There is severe central chest pain due to ischaemia, and pallor with sweating as shock develops. Tachycardia occurs and a gallop rhythm of the heart may be heard on examination.

• Hypotension develops as peripheral shutdown occurs. Syncope may result when cardiac output is suddenly reduced • -Admission to an intensive care unit is highly likely as there is a significant risk of death if treatment is delayed. • -Pulmonary embolism is a medical emergency and urgent referral to hospital is indicated.

• Diagnosis is made from a combination of clinical probability score and radiological imaging. Heparin, usually LWMH, is commenced at presentation with subsequent anticoagulation treatment and management in labour and the postnatal period being similar to that for a woman presenting with DVT

Disseminated intravascular coagulation (DIC) • -In DIC (also known as disseminated intravascular coagulopathy), damage to the endothelium (lining of blood vessel walls) arising from pre-eclampsia, placental abruption, major haemorrhage, embolism, intrauterine fetal death or retained placenta results in thromboplastins being released from the damaged cells, causing the extrinsic pathway to mount a coagulation cascade. • -Blood clofing occurs at the original site and then small clots (micro-thrombi) disperse throughout the rest of the vascular system. • -Large quantities of fibrinogen, thrombocytes (platelets) and clofing factors V and VIII are consumed.

• The micro-thrombi produced can occlude small blood vessels, resulting in ischaemia, hence some organ tissue dies and releases more thromboplastins and the cycle re-commences. • - All clofing factors and platelets are subsequently consumed and bleeding results. There is simultaneously widespread blood clofing and a clofing deficiency. Bleeding occurs, petechiae develop in the skin and, if untreated, major haemorrhage can result

- Slides: 30