Thoracolumbar Spine Injury at CT Sameer B Raniga

Thoracolumbar Spine Injury at CT Sameer B. Raniga, MD, FRCR 1 Mathew R. Skalski, DC, DACBR 2 Anand Kirwadi, MBBS, MRCS, FRCR 3 Venugopal K. Menon, MCh, MS 4 Faisal H. Al-Azri, MD, FRCPS 1 Sajid Butt, MBBS, FRCR 5 1 Department 2 Department 3 Department 4 Department 5 Department of Radiology, Sultan Qaboos University Hospital, Muscat, Oman of Radiology, Keck School of Medicine, University of Southern California, Calif of Radiology, Manchester Royal Infirmary, Manchester, England of Spine Surgery, Khoula Hospital, Muscat, Oman of Radiology, Royal National Orthopaedic Hospital, Stanmore, England Disclaimer: None of the authors have any conflict of interest or financial gain to disclose. Presented as an education exhibit at the 2015 RSNA Annual Meeting Corresponding author: Sameer Raniga, MD, FRCR Sultan Qaboos University Hospital, PO Box 38, PC 123, Al Khoud, Muscat, Oman E-mail: sameerraniga@yahoo. com

Introduction Thoracolumbar (TL) spine trauma computed tomography (CT) is frequently encountered by radiologists in emergency settings. The majority of spine traumas are caused by road traffic accidents. Approximately three-fourths of all spinal fractures involve the TL spine, which is associated with spinal cord injury, long-term pain, and diminished quality of life. Accurate and early diagnosis of spine fracture is essential, as missing or misdiagnosing a spine fracture can result in an increased incidence of neurologic deficits and can potentially lead to an unstable spine. Abbreviations: ALL = anterior longitudinal ligament PLC = posterior ligamentous complex PLL = posterior longitudinal ligament TL = thoracolumbar

Learning Objectives After reviewing this presentation, the reader will be able to: List appropriate imaging strategies in TL spine trauma. Identify the surgically relevant anatomy. List the four patterns of injury morphology on CT images—fracturedislocation, flexion-distraction, burst, and compression. Discuss CT characteristics, pearls, and pitfalls of each of the four patterns of spine injuries with its implications in surgical decision making. Recognize commonly missed injuries and how to find them. Create a surgically relevant radiologic report by using a CT spine trauma checklist.

Content Organization Imaging strategies: who, what, and how? Review the surgically relevant TL spine anatomy CT checklist—systematic search pattern Injury morphologic patterns 1) Fracture-dislocation 2) Flexion-distraction 3) Burst 4) Compression CT criteria, pearls, and pitfalls to diagnose each pattern, with emphasis on management, are explained. Look-alike and fracture mimics Please click on icon for annotation and description of images.
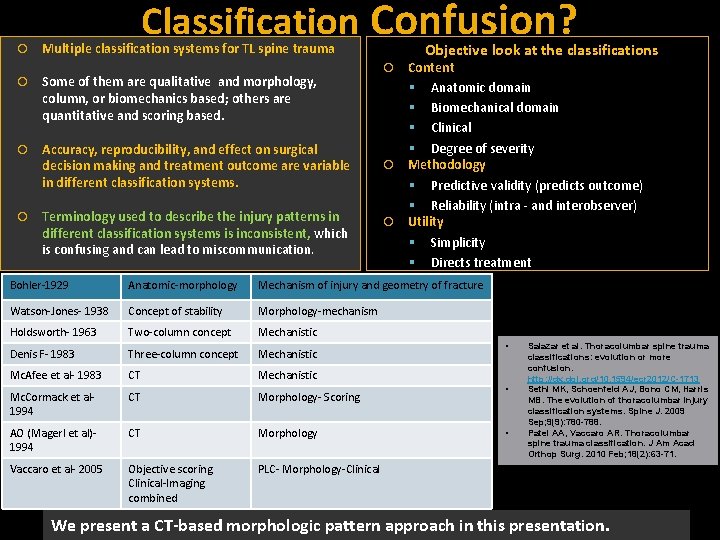

Classification Confusion? Some of them are qualitative and morphology, column, or biomechanics based; others are quantitative and scoring based. Accuracy, reproducibility, and effect on surgical decision making and treatment outcome are variable in different classification systems. Objective look at the classifications Multiple classification systems for TL spine trauma Terminology used to describe the injury patterns in different classification systems is inconsistent, which is confusing and can lead to miscommunication. Content Anatomic domain Biomechanical domain Clinical Degree of severity Methodology Predictive validity (predicts outcome) Reliability (intra - and interobserver) Utility Simplicity Directs treatment Bohler-1929 Anatomic-morphology Mechanism of injury and geometry of fracture Watson-Jones- 1938 Concept of stability Morphology-mechanism Holdsworth- 1963 Two-column concept Mechanistic Denis F- 1983 Three-column concept Mechanistic Mc. Afee et al- 1983 CT Mechanistic Mc. Cormack et al 1994 CT Morphology- Scoring AO (Magerl et al)1994 CT Morphology Vaccaro et al- 2005 Objective scoring Clinical-Imaging combined PLC- Morphology-Clinical • • • Salazar et al. Thoracolumbar spine trauma classifications: evolution or more confusion. http: //dx. doi. org/10. 1594/ecr 2012/C-1713 Sethi MK, Schoenfeld AJ, Bono CM, Harris MB. The evolution of thoracolumbar injury classification systems. Spine J. 2009 Sep; 9(9): 780 -788. Patel AA, Vaccaro AR. Thoracolumbar spine trauma classification. J Am Acad Orthop Surg. 2010 Feb; 18(2): 63 -71. We present a CT-based morphologic pattern approach in this presentation.
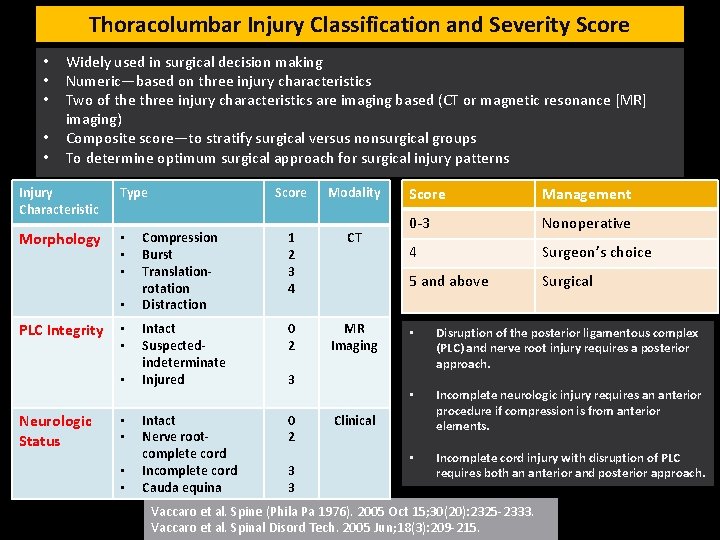
Thoracolumbar Injury Classification and Severity Score • • • Widely used in surgical decision making Numeric—based on three injury characteristics Two of the three injury characteristics are imaging based (CT or magnetic resonance [MR] imaging) Composite score—to stratify surgical versus nonsurgical groups To determine optimum surgical approach for surgical injury patterns Injury Characteristic Type Morphology • • PLC Integrity • • • Neurologic Status • • Score Modality Compression Burst Translationrotation Distraction 1 2 3 4 CT Intact Suspectedindeterminate Injured 0 2 MR Imaging Intact Nerve rootcomplete cord Incomplete cord Cauda equina 0 2 3 3 3 Score Management 0 -3 Nonoperative 4 Surgeon’s choice 5 and above Surgical • Disruption of the posterior ligamentous complex (PLC) and nerve root injury requires a posterior approach. • Incomplete neurologic injury requires an anterior procedure if compression is from anterior elements. • Incomplete cord injury with disruption of PLC requires both an anterior and posterior approach. Clinical Vaccaro et al. Spine (Phila Pa 1976). 2005 Oct 15; 30(20): 2325 -2333. Vaccaro et al. Spinal Disord Tech. 2005 Jun; 18(3): 209 -215.

Imaging Strategies: Who Should Undergo Multidetector CT? Recommendations for appropriate imaging in the evaluation of TL spine trauma are less definitive than those for the cervical spine. High-energy injury Symptoms • • • • Falls from substantial height (>10 feet) Motor vehicle crash with or without ejection Pedestrian struck by motorist Assault A concomitant cervical spine fracture is considered to have a high-energy mechanism of injury. Back pain or midline tenderness Local signs of TL injury Abnormal neurologic signs Cervical spine fracture Glasgow Coma Scale less than 15 Major distracting injury Alcohol or drug intoxication www. imagingpathways. health. wa. gov. au Diaz JJ Jr, Cullinane DC, Altman DT, Bokhari F, Cheng JS, Como J, et al. Practice management guidelines for the screening of thoracolumbar spine fracture. J Trauma. 2007; 63(3): 709 -718. Hsu JM, Joseph T, Ellis AM. Thoracolumbar fracture in blunt trauma patients: guidelines for diagnosis and imaging. Injury. 2003; 34(6): 426 -433. • Fractures found in any level of the spine Screen the whole spine (15%-20% discontinuous fractures) • Thorax, abdomen, and pelvis CT—Reconstruct spine

Imaging Strategies How? Which modality? Radiographs—Low-risk patients and children (multidetector CT for problem solving) Multidetector CT—High-risk patients, polytrauma, head injury Neurologic deficit—Multidetector CT and MR imaging Screening TL spine MR imaging— Not indicated in the absence of neurologic deficit when multidetector CT result is normal. ▪ American College of Radiology Appropriateness Criteria Dedicated multidetector CT of spine Reconstructed thorax, abdomen, and pelvis CT images may be used instead of primary spine imaging. Multidetector CT protocol Contiguous 0. 625 -mm axial volumetric acquisition Axial, sagittal, and coronal nonenhanced images in bone algorithm (2 -mm contiguous sections) Axial and sagittal images in soft -tissue algorithm (2 -mm contiguous sections)
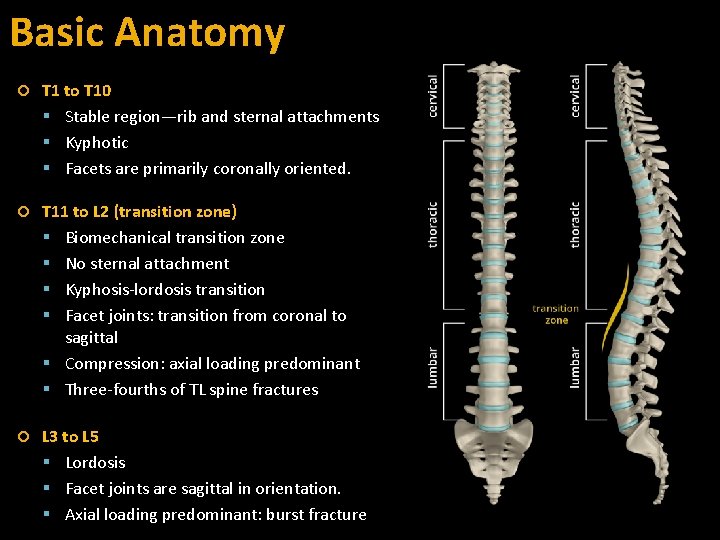
Basic Anatomy T 1 to T 10 Stable region—rib and sternal attachments Kyphotic Facets are primarily coronally oriented. T 11 to L 2 (transition zone) Biomechanical transition zone No sternal attachment Kyphosis-lordosis transition Facet joints: transition from coronal to sagittal Compression: axial loading predominant Three-fourths of TL spine fractures L 3 to L 5 Lordosis Facet joints are sagittal in orientation. Axial loading predominant: burst fracture
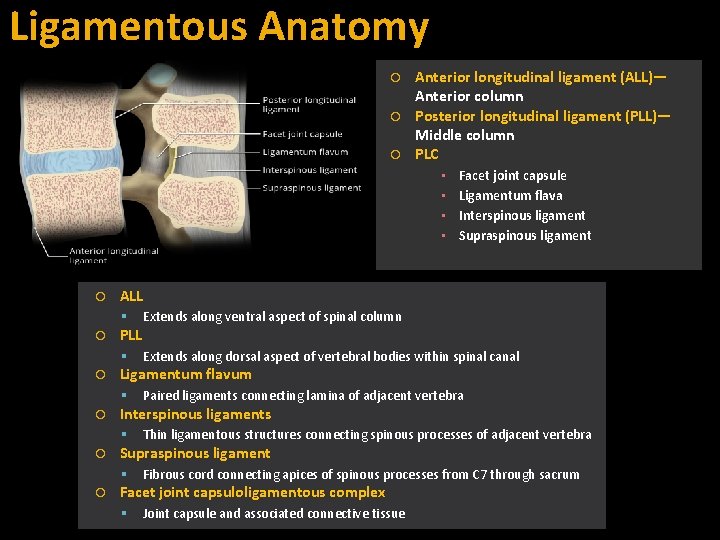
Ligamentous Anatomy Anterior longitudinal ligament (ALL)— Anterior column Posterior longitudinal ligament (PLL)— Middle column PLC ▪ ▪ ALL Paired ligaments connecting lamina of adjacent vertebra Thin ligamentous structures connecting spinous processes of adjacent vertebra Supraspinous ligament Extends along dorsal aspect of vertebral bodies within spinal canal Interspinous ligaments Extends along ventral aspect of spinal column Ligamentum flavum Facet joint capsule Ligamentum flava Interspinous ligament Supraspinous ligament Fibrous cord connecting apices of spinous processes from C 7 through sacrum Facet joint capsuloligamentous complex Joint capsule and associated connective tissue
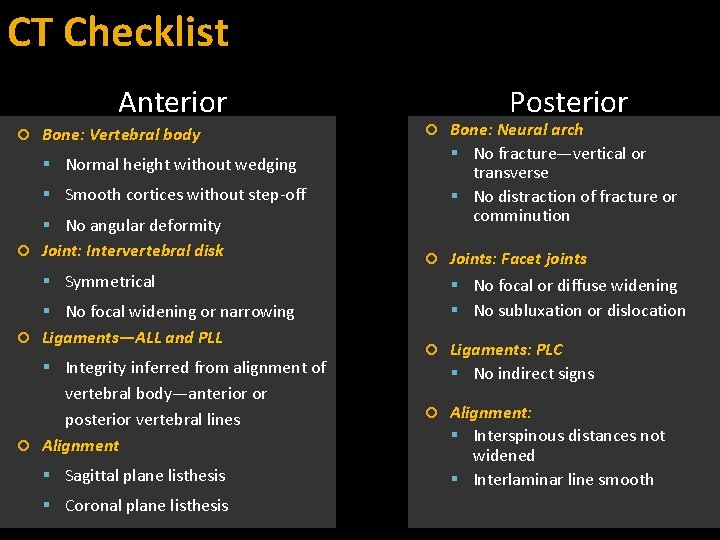
CT Checklist Anterior Bone: Vertebral body Posterior Bone: Neural arch No fracture—vertical or transverse No distraction of fracture or comminution Joints: Facet joints Normal height without wedging Smooth cortices without step-off No angular deformity Joint: Intervertebral disk Symmetrical No focal or diffuse widening No subluxation or dislocation No focal widening or narrowing Ligaments—ALL and PLL Integrity inferred from alignment of vertebral body—anterior or posterior vertebral lines Alignment Sagittal plane listhesis Coronal plane listhesis Ligaments: PLC No indirect signs Alignment: Interspinous distances not widened Interlaminar line smooth
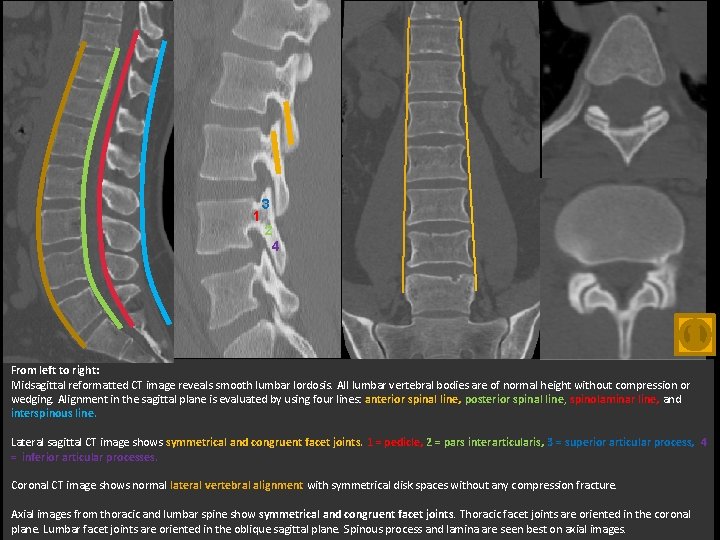
1 3 2 4 From left to right: Midsagittal reformatted CT image reveals smooth lumbar lordosis. All lumbar vertebral bodies are of normal height without compression or wedging. Alignment in the sagittal plane is evaluated by using four lines: anterior spinal line, posterior spinal line, spinolaminar line, and interspinous line. Lateral sagittal CT image shows symmetrical and congruent facet joints. 1 = pedicle, 2 = pars interarticularis, 3 = superior articular process, 4 = inferior articular processes. Coronal CT image shows normal lateral vertebral alignment with symmetrical disk spaces without any compression fracture. Axial images from thoracic and lumbar spine show symmetrical and congruent facet joints. Thoracic facet joints are oriented in the coronal plane. Lumbar facet joints are oriented in the oblique sagittal plane. Spinous process and lamina are seen best on axial images.
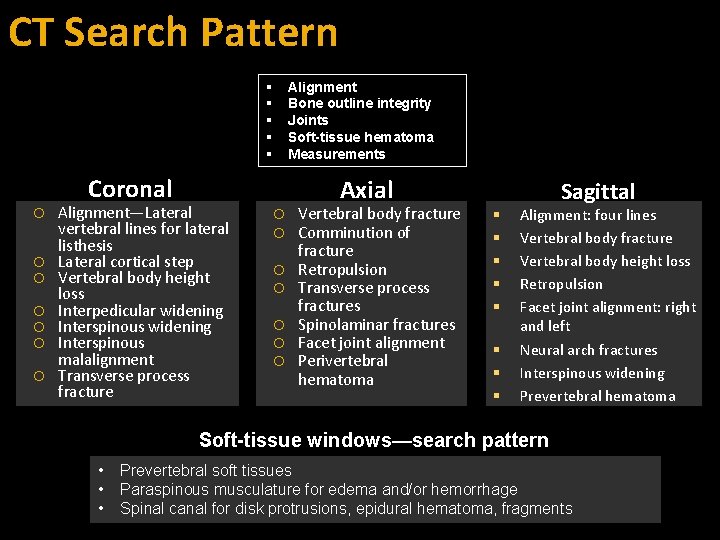
CT Search Pattern Alignment Bone outline integrity Joints Soft-tissue hematoma Measurements Coronal Alignment—Lateral vertebral lines for lateral listhesis Lateral cortical step Vertebral body height loss Interpedicular widening Interspinous malalignment Transverse process fracture Axial Vertebral body fracture Comminution of fracture Retropulsion Transverse process fractures Spinolaminar fractures Facet joint alignment Perivertebral hematoma Sagittal Alignment: four lines Vertebral body fracture Vertebral body height loss Retropulsion Facet joint alignment: right and left Neural arch fractures Interspinous widening Prevertebral hematoma Soft-tissue windows—search pattern • • • Prevertebral soft tissues Paraspinous musculature for edema and/or hemorrhage Spinal canal for disk protrusions, epidural hematoma, fragments
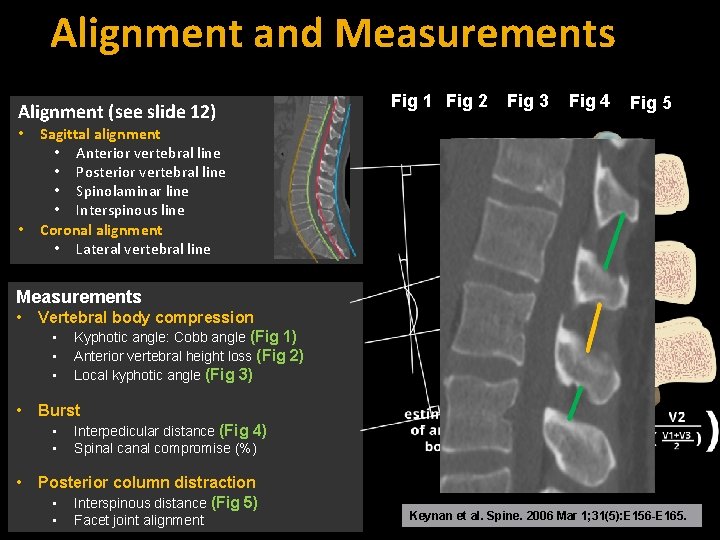
Alignment and Measurements Alignment (see slide 12) • • Fig 1 Fig 2 Fig 3 Fig 4 Fig 5 Sagittal alignment • Anterior vertebral line • Posterior vertebral line • Spinolaminar line • Interspinous line Coronal alignment • Lateral vertebral line Measurements • Vertebral body compression • Kyphotic angle: Cobb angle (Fig 1) • Anterior vertebral height loss (Fig 2) • Local kyphotic angle (Fig 3) • Burst • • • Interpedicular distance (Fig 4) Spinal canal compromise (%) Posterior column distraction • Interspinous distance (Fig 5) • Facet joint alignment Keynan et al. Spine. 2006 Mar 1; 31(5): E 156 -E 165.
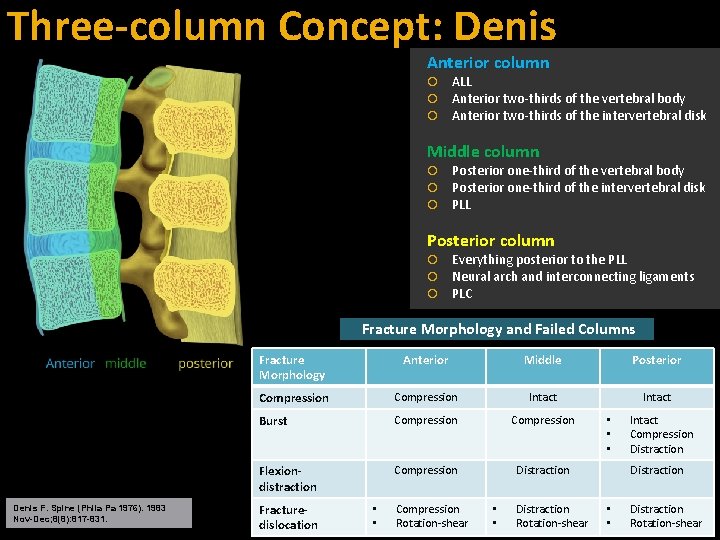
Three-column Concept: Denis Anterior column ALL Anterior two-thirds of the vertebral body Anterior two-thirds of the intervertebral disk Middle column Posterior one-third of the vertebral body Posterior one-third of the intervertebral disk PLL Posterior column Everything posterior to the PLL Neural arch and interconnecting ligaments PLC Fracture Morphology and Failed Columns Denis F. Spine (Phila Pa 1976). 1983 Nov-Dec; 8(8): 817 -831. Fracture Morphology Anterior Middle Posterior Compression Intact Burst Compression Flexiondistraction Compression Distraction Fracturedislocation • • Compression Rotation-shear • • Distraction Rotation-shear • • • Intact Compression Distraction • • Distraction Rotation-shear
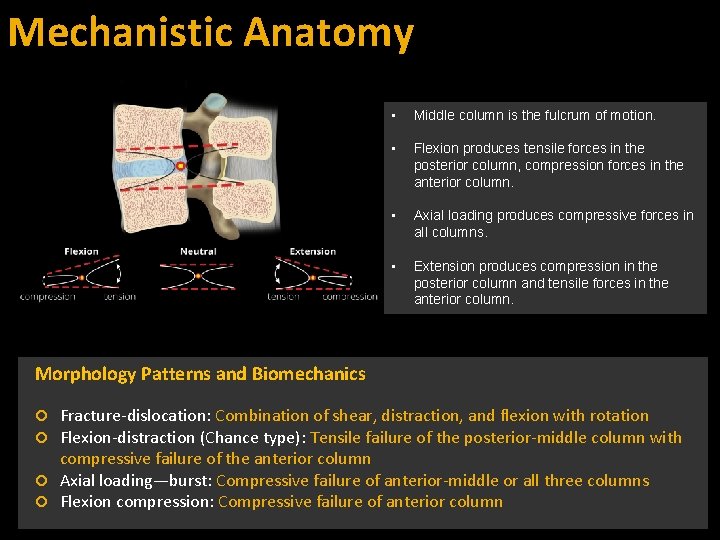
Mechanistic Anatomy • Middle column is the fulcrum of motion. • Flexion produces tensile forces in the posterior column, compression forces in the anterior column. • Axial loading produces compressive forces in all columns. • Extension produces compression in the posterior column and tensile forces in the anterior column. Morphology Patterns and Biomechanics Fracture-dislocation: Combination of shear, distraction, and flexion with rotation Flexion-distraction (Chance type): Tensile failure of the posterior-middle column with compressive failure of the anterior column Axial loading—burst: Compressive failure of anterior-middle or all three columns Flexion compression: Compressive failure of anterior column
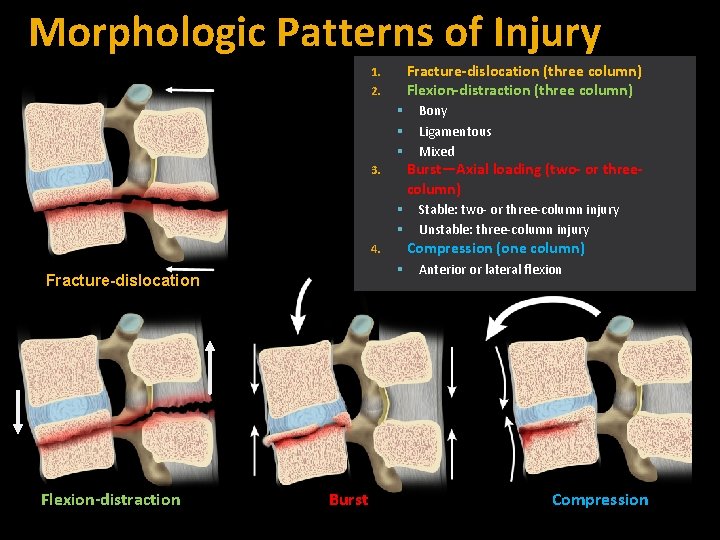
Morphologic Patterns of Injury Fracture-dislocation (three column) Flexion-distraction (three column) 1. 2. Burst—Axial loading (two- or threecolumn) 3. Flexion-distraction Burst Stable: two- or three-column injury Unstable: three-column injury Compression (one column) 4. Fracture-dislocation Bony Ligamentous Mixed Anterior or lateral flexion Compression
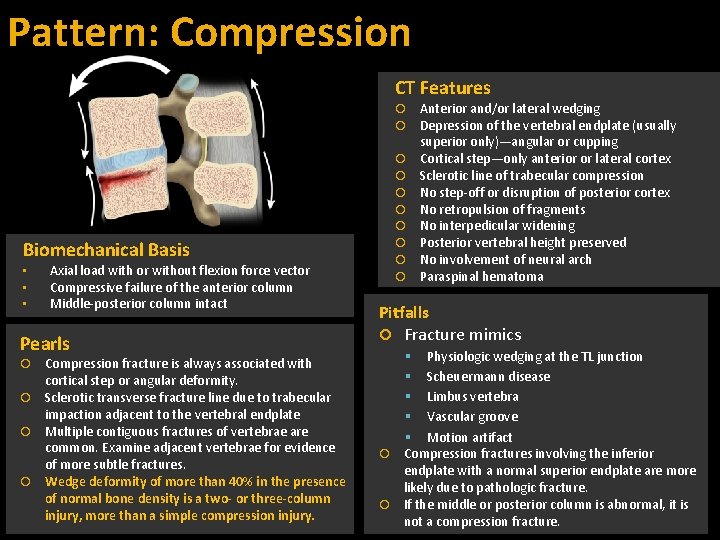
Pattern: Compression CT Features Anterior and/or lateral wedging Depression of the vertebral endplate (usually superior only)—angular or cupping Cortical step—only anterior or lateral cortex Sclerotic line of trabecular compression No step-off or disruption of posterior cortex No retropulsion of fragments No interpedicular widening Posterior vertebral height preserved No involvement of neural arch Paraspinal hematoma Biomechanical Basis • • • Axial load with or without flexion force vector Compressive failure of the anterior column Middle-posterior column intact Pearls Compression fracture is always associated with cortical step or angular deformity. Sclerotic transverse fracture line due to trabecular impaction adjacent to the vertebral endplate Multiple contiguous fractures of vertebrae are common. Examine adjacent vertebrae for evidence of more subtle fractures. Wedge deformity of more than 40% in the presence of normal bone density is a two- or three-column injury, more than a simple compression injury. Pitfalls Fracture mimics Physiologic wedging at the TL junction Scheuermann disease Limbus vertebra Vascular groove Motion artifact Compression fractures involving the inferior endplate with a normal superior endplate are more likely due to pathologic fracture. If the middle or posterior column is abnormal, it is not a compression fracture.
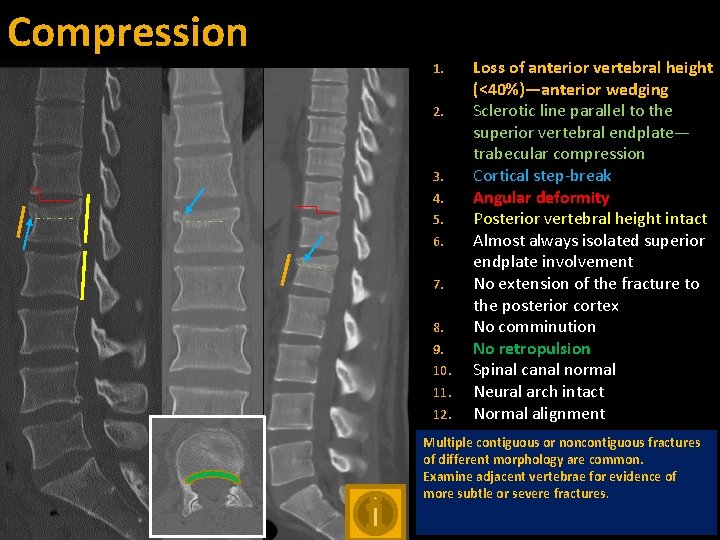
Compression 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. 11. 12. Loss of anterior vertebral height (<40%)—anterior wedging Sclerotic line parallel to the superior vertebral endplate— trabecular compression Cortical step-break Angular deformity Posterior vertebral height intact Almost always isolated superior endplate involvement No extension of the fracture to the posterior cortex No comminution No retropulsion Spinal canal normal Neural arch intact Normal alignment Multiple contiguous or noncontiguous fractures of different morphology are common. Examine adjacent vertebrae for evidence of more subtle or severe fractures.
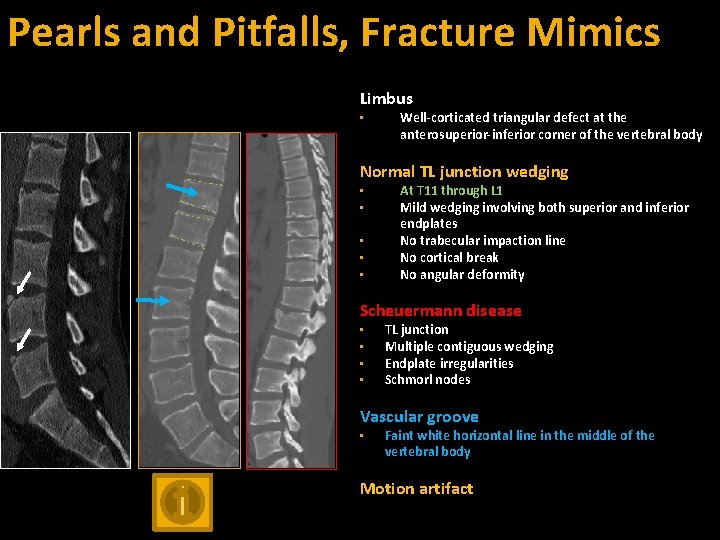
Pearls and Pitfalls, Fracture Mimics Limbus • Well-corticated triangular defect at the anterosuperior-inferior corner of the vertebral body Normal TL junction wedging • • • At T 11 through L 1 Mild wedging involving both superior and inferior endplates No trabecular impaction line No cortical break No angular deformity Scheuermann disease • • TL junction Multiple contiguous wedging Endplate irregularities Schmorl nodes Vascular groove • Faint white horizontal line in the middle of the vertebral body Motion artifact
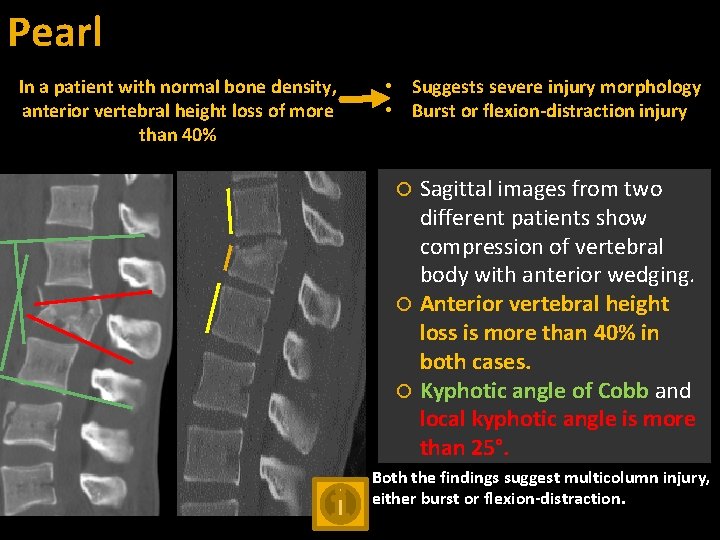
Pearl In a patient with normal bone density, anterior vertebral height loss of more than 40% • Suggests severe injury morphology • Burst or flexion-distraction injury Sagittal images from two different patients show compression of vertebral body with anterior wedging. Anterior vertebral height loss is more than 40% in both cases. Kyphotic angle of Cobb and local kyphotic angle is more than 25°. Both the findings suggest multicolumn injury, either burst or flexion-distraction.
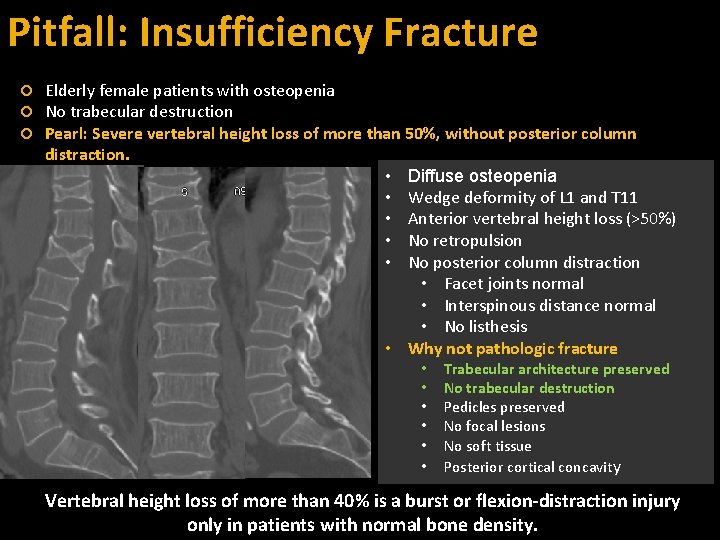
Pitfall: Insufficiency Fracture Elderly female patients with osteopenia No trabecular destruction Pearl: Severe vertebral height loss of more than 50%, without posterior column distraction. • Diffuse osteopenia • Wedge deformity of L 1 and T 11 • Anterior vertebral height loss (>50%) • No retropulsion • No posterior column distraction • Facet joints normal • Interspinous distance normal • No listhesis • Why not pathologic fracture • • • Trabecular architecture preserved No trabecular destruction Pedicles preserved No focal lesions No soft tissue Posterior cortical concavity Vertebral height loss of more than 40% is a burst or flexion-distraction injury only in patients with normal bone density.
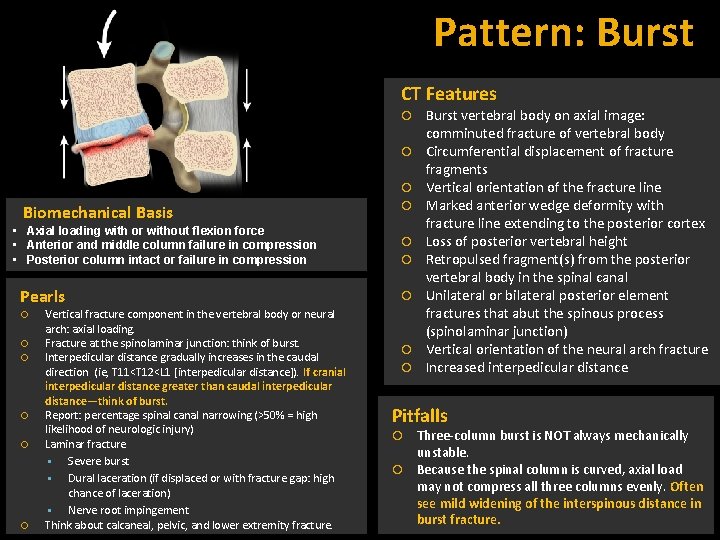
Pattern: Burst CT Features Biomechanical Basis • Axial loading with or without flexion force • Anterior and middle column failure in compression • Posterior column intact or failure in compression Pearls Vertical fracture component in the vertebral body or neural arch: axial loading. Fracture at the spinolaminar junction: think of burst. Interpedicular distance gradually increases in the caudal direction (ie, T 11<T 12<L 1 [interpedicular distance]). If cranial interpedicular distance greater than caudal interpedicular distance—think of burst. Report: percentage spinal canal narrowing (>50% = high likelihood of neurologic injury) Laminar fracture Severe burst Dural laceration (if displaced or with fracture gap: high chance of laceration) Nerve root impingement Think about calcaneal, pelvic, and lower extremity fracture. Burst vertebral body on axial image: comminuted fracture of vertebral body Circumferential displacement of fracture fragments Vertical orientation of the fracture line Marked anterior wedge deformity with fracture line extending to the posterior cortex Loss of posterior vertebral height Retropulsed fragment(s) from the posterior vertebral body in the spinal canal Unilateral or bilateral posterior element fractures that abut the spinous process (spinolaminar junction) Vertical orientation of the neural arch fracture Increased interpedicular distance Pitfalls Three-column burst is NOT always mechanically unstable. Because the spinal column is curved, axial load may not compress all three columns evenly. Often see mild widening of the interspinous distance in burst fracture.
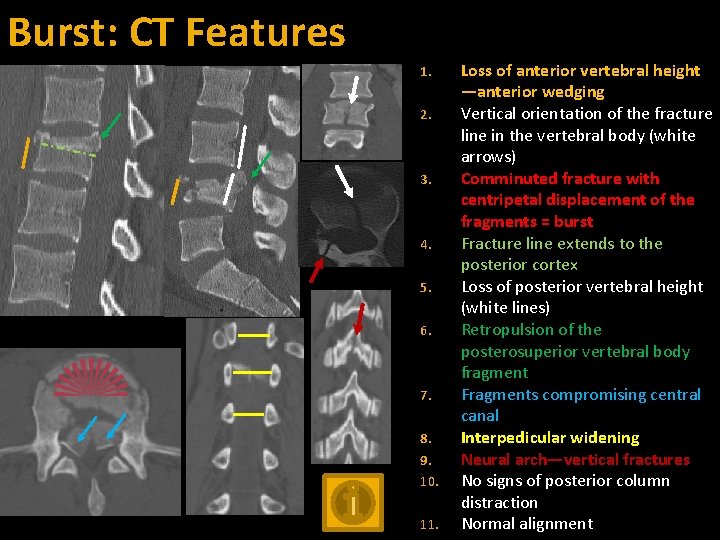
Burst: CT Features 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. 11. Loss of anterior vertebral height —anterior wedging Vertical orientation of the fracture line in the vertebral body (white arrows) Comminuted fracture with centripetal displacement of the fragments = burst Fracture line extends to the posterior cortex Loss of posterior vertebral height (white lines) Retropulsion of the posterosuperior vertebral body fragment Fragments compromising central canal Interpedicular widening Neural arch—vertical fractures No signs of posterior column distraction Normal alignment
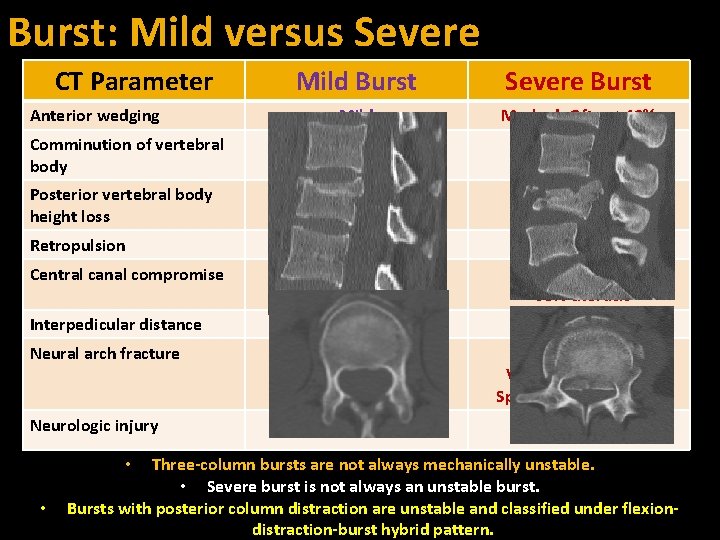
Burst: Mild versus Severe CT Parameter Mild Burst Severe Burst Anterior wedging Mild Marked- Often >40% Comminution of vertebral body Mild Severe Posterior vertebral body height loss Mild Severe Minimal Marked Mild >50% lumbar >30% thoracic Interpedicular distance Normal Widened Neural arch fracture Absent Often present Vertical orientation Spinolaminar junction None or mild Often significant Retropulsion Central canal compromise Neurologic injury Three-column bursts are not always mechanically unstable. • Severe burst is not always an unstable burst. Bursts with posterior column distraction are unstable and classified under flexiondistraction-burst hybrid pattern. • •
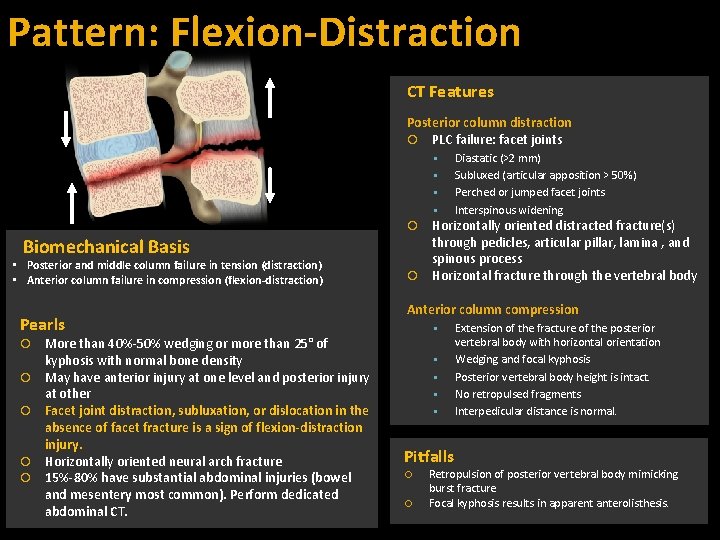
Pattern: Flexion-Distraction CT Features Posterior column distraction PLC failure: facet joints Biomechanical Basis • Posterior and middle column failure in tension (distraction) • Anterior column failure in compression (flexion-distraction) Pearls More than 40%-50% wedging or more than 25° of kyphosis with normal bone density May have anterior injury at one level and posterior injury at other Facet joint distraction, subluxation, or dislocation in the absence of facet fracture is a sign of flexion-distraction injury. Horizontally oriented neural arch fracture 15%-80% have substantial abdominal injuries (bowel and mesentery most common). Perform dedicated abdominal CT. Diastatic (>2 mm) Subluxed (articular apposition > 50%) Perched or jumped facet joints Interspinous widening Horizontally oriented distracted fracture(s) through pedicles, articular pillar, lamina , and spinous process Horizontal fracture through the vertebral body Anterior column compression Pitfalls Extension of the fracture of the posterior vertebral body with horizontal orientation Wedging and focal kyphosis Posterior vertebral body height is intact. No retropulsed fragments Interpedicular distance is normal. Retropulsion of posterior vertebral body mimicking burst fracture Focal kyphosis results in apparent anterolisthesis.
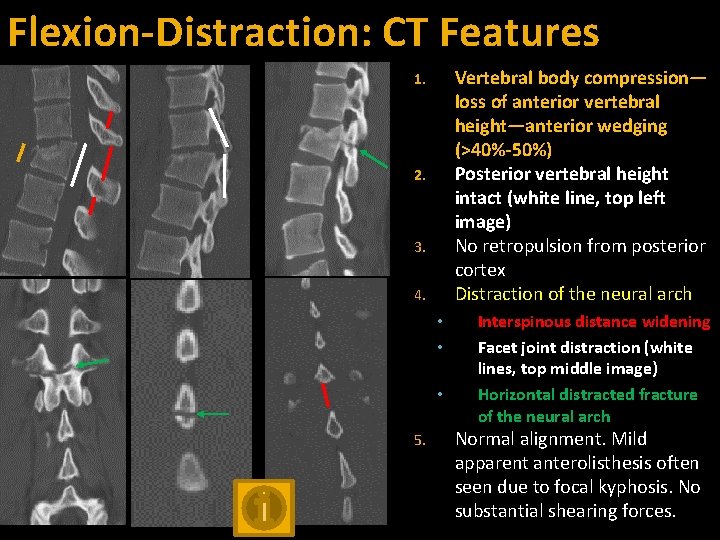
Flexion-Distraction: CT Features Vertebral body compression— loss of anterior vertebral height—anterior wedging (>40%-50%) Posterior vertebral height intact (white line, top left image) No retropulsion from posterior cortex Distraction of the neural arch 1. 2. 3. 4. • • • 5. Interspinous distance widening Facet joint distraction (white lines, top middle image) Horizontal distracted fracture of the neural arch Normal alignment. Mild apparent anterolisthesis often seen due to focal kyphosis. No substantial shearing forces.
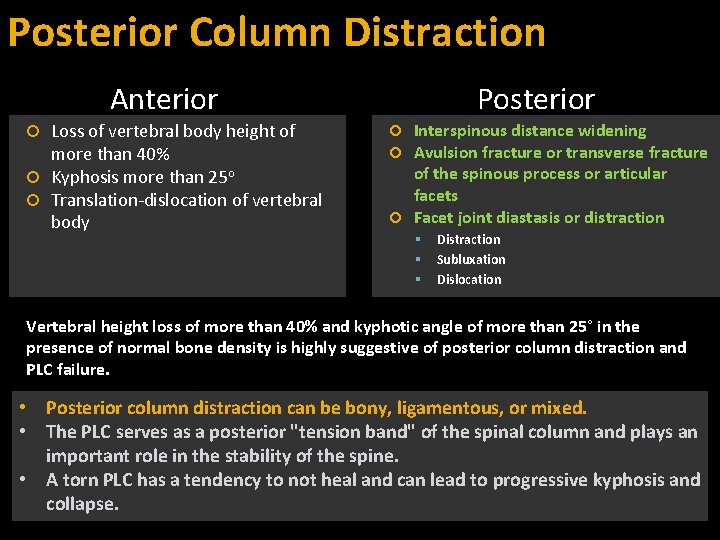

Posterior Column Distraction Anterior Loss of vertebral body height of more than 40% Kyphosis more than 25 o Translation-dislocation of vertebral body Posterior Interspinous distance widening Avulsion fracture or transverse fracture of the spinous process or articular facets Facet joint diastasis or distraction Distraction Subluxation Dislocation Vertebral height loss of more than 40% and kyphotic angle of more than 25° in the presence of normal bone density is highly suggestive of posterior column distraction and PLC failure. • Posterior column distraction can be bony, ligamentous, or mixed. • The PLC serves as a posterior "tension band" of the spinal column and plays an important role in the stability of the spine. • A torn PLC has a tendency to not heal and can lead to progressive kyphosis and collapse.
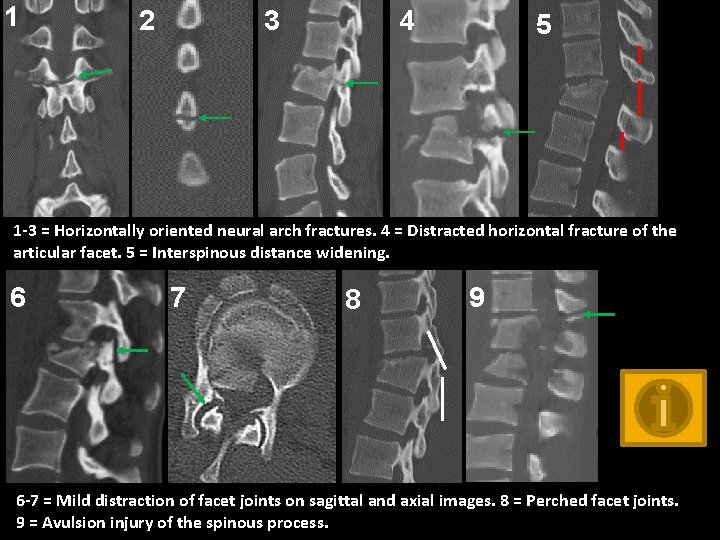
1 2 4 3 5 1 -3 = Horizontally oriented neural arch fractures. 4 = Distracted horizontal fracture of the articular facet. 5 = Interspinous distance widening. 6 7 8 9 6 -7 = Mild distraction of facet joints on sagittal and axial images. 8 = Perched facet joints. 9 = Avulsion injury of the spinous process.
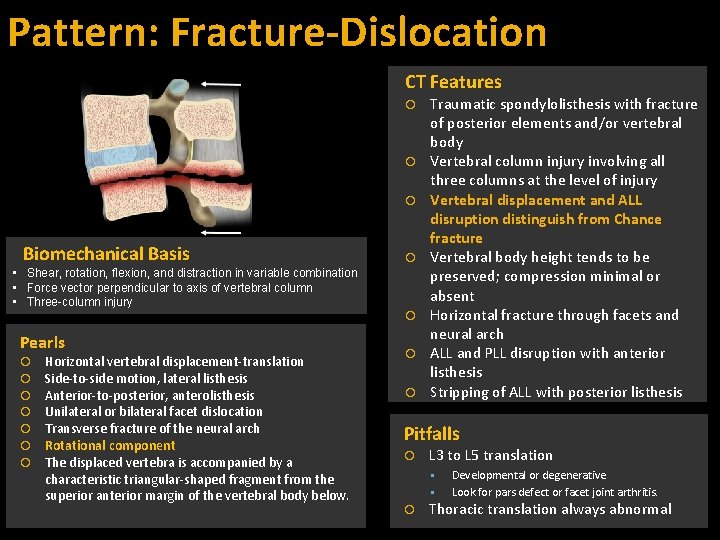
Pattern: Fracture-Dislocation CT Features Biomechanical Basis • Shear, rotation, flexion, and distraction in variable combination • Force vector perpendicular to axis of vertebral column • Three-column injury Pearls Horizontal vertebral displacement-translation Side-to-side motion, lateral listhesis Anterior-to-posterior, anterolisthesis Unilateral or bilateral facet dislocation Transverse fracture of the neural arch Rotational component The displaced vertebra is accompanied by a characteristic triangular-shaped fragment from the superior anterior margin of the vertebral body below. Traumatic spondylolisthesis with fracture of posterior elements and/or vertebral body Vertebral column injury involving all three columns at the level of injury Vertebral displacement and ALL disruption distinguish from Chance fracture Vertebral body height tends to be preserved; compression minimal or absent Horizontal fracture through facets and neural arch ALL and PLL disruption with anterior listhesis Stripping of ALL with posterior listhesis Pitfalls L 3 to L 5 translation Developmental or degenerative Look for pars defect or facet joint arthritis. Thoracic translation always abnormal
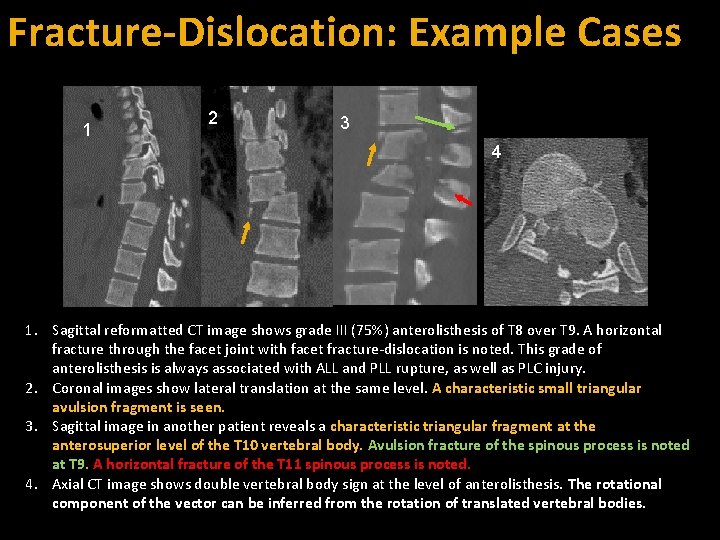
Fracture-Dislocation: Example Cases 1 2 3 4 1. Sagittal reformatted CT image shows grade III (75%) anterolisthesis of T 8 over T 9. A horizontal fracture through the facet joint with facet fracture-dislocation is noted. This grade of anterolisthesis is always associated with ALL and PLL rupture, as well as PLC injury. 2. Coronal images show lateral translation at the same level. A characteristic small triangular avulsion fragment is seen. 3. Sagittal image in another patient reveals a characteristic triangular fragment at the anterosuperior level of the T 10 vertebral body. Avulsion fracture of the spinous process is noted at T 9. A horizontal fracture of the T 11 spinous process is noted. 4. Axial CT image shows double vertebral body sign at the level of anterolisthesis. The rotational component of the vector can be inferred from the rotation of translated vertebral bodies.
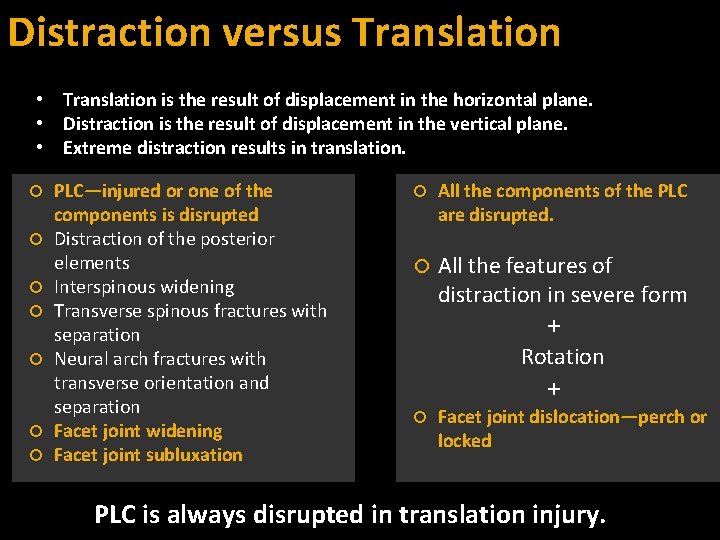
Distraction versus Translation • Translation is the result of displacement in the horizontal plane. • Distraction is the result of displacement in the vertical plane. • Extreme distraction results in translation. PLC—injured or one of the components is disrupted Distraction of the posterior elements Interspinous widening Transverse spinous fractures with separation Neural arch fractures with transverse orientation and separation Facet joint widening Facet joint subluxation All the components of the PLC are disrupted. All the features of distraction in severe form + Rotation + Facet joint dislocation—perch or locked PLC is always disrupted in translation injury.
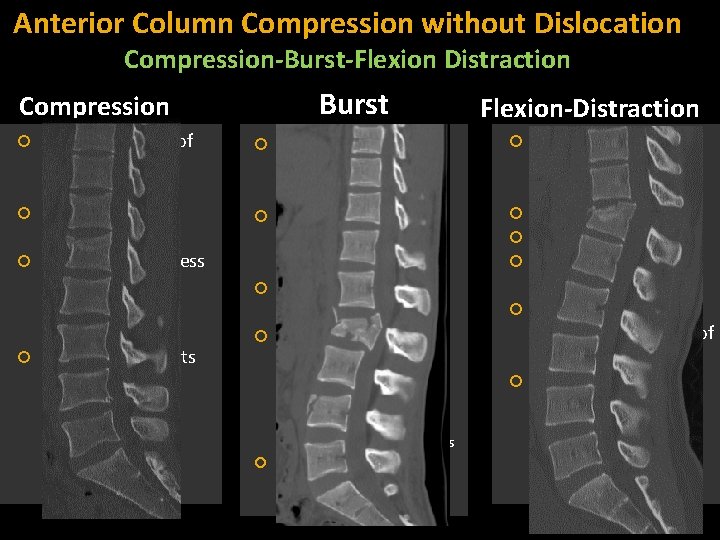
Anterior Column Compression without Dislocation Compression-Burst-Flexion Distraction Burst Compression Posterior cortex of vertebral body is intact Posterior height normal Loss of height is less than 40% in the absence of osteopenia Posterior elements normal More than 40% anterior vertebral height loss Vertical fracture line in sagittal or coronal plane Posterior vertebral body height loss Retropulsion Flexion-Distraction Bulge—sagittal Axial—Loss of smooth arc of cortical bone between the medial surfaces of the pedicles Posterior element vertical fractures More than 40%-50% anterior vertebral height loss No comminution No retropulsion Horizontal posterior element fracture Distracted or separated fractures of posterior elements PLC failure
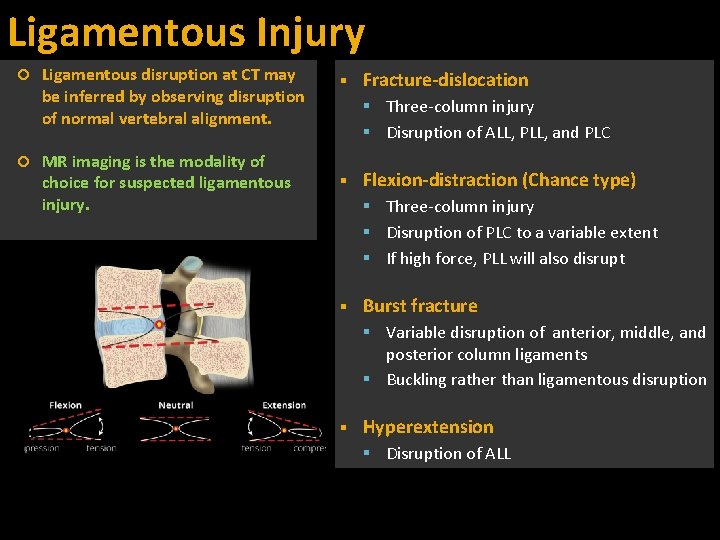
Ligamentous Injury Ligamentous disruption at CT may be inferred by observing disruption of normal vertebral alignment. MR imaging is the modality of choice for suspected ligamentous injury. Fracture-dislocation Three-column injury Disruption of ALL, PLL, and PLC Flexion-distraction (Chance type) Three-column injury Disruption of PLC to a variable extent If high force, PLL will also disrupt Burst fracture Variable disruption of anterior, middle, and posterior column ligaments Buckling rather than ligamentous disruption Hyperextension Disruption of ALL
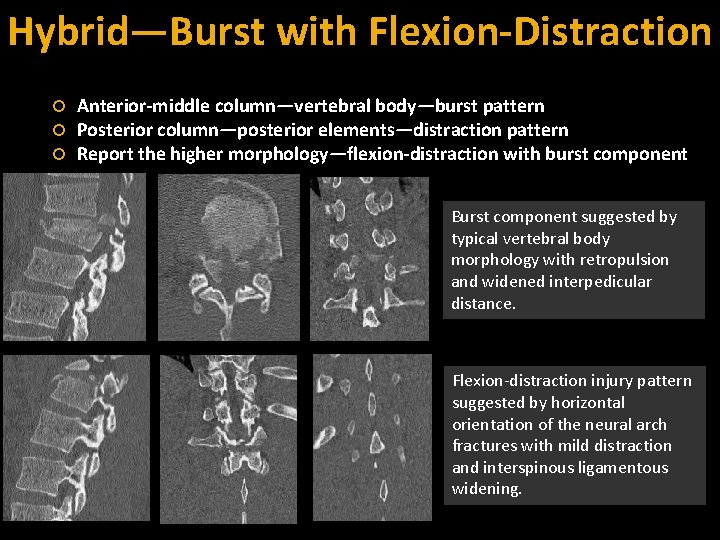
Hybrid—Burst with Flexion-Distraction Anterior-middle column—vertebral body—burst pattern Posterior column—posterior elements—distraction pattern Report the higher morphology—flexion-distraction with burst component Burst component suggested by typical vertebral body morphology with retropulsion and widened interpedicular distance. Flexion-distraction injury pattern suggested by horizontal orientation of the neural arch fractures with mild distraction and interspinous ligamentous widening.
Surgical Indications Stability Assessment of spine stability or instability is based on imaging and clinical information. Neurologic Involvement With any type of fracture pattern Symptoms of cord/neural compression It’s best to report injury extent and patterns without pronouncing the spine definitively stable or unstable on the basis of imaging findings alone. Mechanical Instability To restore stability Report the involvement of the individual columns and total number of columns in the report. Presence of three-column injury is not always mechanically unstable. In burst fracture, all the columns may fail in compression, which is a biomechanically stable injury. Flexion-distraction and fracturedislocation morphology are always mechanically unstable. Clinical Instability—Failure of stress testing Severe pain More than 25° kyphosis Focal neurologic signs Surgical Approach • Disruption of the PLC and nerve root injury requires a posterior approach. • Incomplete neurologic injury requires an anterior procedure if compression is from anterior elements. • Incomplete cord injury with disruption of PLC requires both an anterior and posterior approach.

How to Not Miss a Fracture Alignment Sagittal Coronal Bones—Vertebral body and neural arch Vertebral body—loss of height and fracture Neural arch—fracture Joints and ligaments Facet joint—fracture, subluxation, or dislocation Ligaments—PLC Spinal canal Bony fragment Canal compromise Spinal canal hematoma Periosseous soft tissue

What to Include in a Surgically Relevant Report Morphology pattern One of the four patterns—dislocation, distraction, burst, or simple compression Combination of patterns—report in descending order of severity (eg, burst and chance —write in the report “Chance with burst”) Traumatic anterolisthesis—grade it. Flexion-distraction—describe it. Anterior column compression Approximate anterior vertebral body height loss Kyphotic angle of Cobb Extension of the fracture line to the posterior vertebral cortex Posterior vertebral body height loss Retropulsed fragment from the posterior vertebral body Approximate compromise of the central spinal canal in percentage Posterior column distraction Present or absent—describe individual components Carefully look at the entire spine for contiguous and discontinuous fractures.

References Denis F. The three column spine and its significance in the classification of acute thoracolumbar spinal injuries. Spine (Phila Pa 1976). 1983; Nov-Dec; 8(8): 817 -831. Diagnostic imaging pathways. Government of Western Australia. http: //www. imagingpathways. health. wa. gov. au/. Diaz JJ Jr, Cullinane DC, Altman DT, et al. Practice management guidelines for the screening of thoracolumbar spine fracture. EAST Practice Management Guideline Committee. J Trauma. 2007 Sep; 63(3): 709 -718. Hsu JM, Joseph T, Ellis AM. Thoracolumbar fracture in blunt trauma patients: guidelines for diagnosis and imaging. Injury. 2003; 34(6): 426 -433. Kenyan O, Fisher CG, Vaccaro A, et al. Radiographic measurement parameters in thoracolumbar fractures: a systematic review and consensus statement of the Spine Trauma Study Group. Spine 2006; 31(5): E 156–E 165. Patel AA, Vaccaro AR. Thoracolumbar spine trauma classification. J Am Acad Orthop Surg. 2010 Feb; 18(2): 63 -71. Rogers LE and West OC. Thoracolumbar spine trauma. In Imaging skeletal trauma. 4 th edition. Saunders, 2014; 90 -127. Salazar JP, Halaburda Berni J, Torrents C, Casas L. Thoracolumbar spine trauma classifications: evolution or more confusion. Presented at 2012 ECR. http: //dx. doi. org/10. 1594/ecr 2012/C-1713. Sethi MK, Schoenfeld AJ, Bono CM, Harris MB. The evolution of thoracolumbar injury classification systems. Spine J. 2009 Sep; 9(9): 780 -788. Vaccaro AR, Lehman RA Jr, Hurlbert RJ, et al. A new classification of thoracolumbar injuries: the importance of injury morphology, the integrity of the posterior ligamentous complex, and neurologic status. Spine (Phila Pa 1976). 2005 Oct 15; 30(20): 2325 -2333. Vaccaro AR, Zeiller SC, Hulbert RJ, et al. The thoracolumbar injury severity score: a proposed treatment algorithm. J Spinal Disord Tech. 2005 Jun; 18(3): 209 -215.

Suggested Readings Davis JM, Beall DP, Lastine C, Sweet C, Wolff J, Wu D. Chance fracture of the upper thoracic spine. AJR Am J Roentgenol. 2004 Nov; 183(5): 1475 -1478. Diaz JJ Jr, Cullinane DC, Altman DT, et al. Practice management guidelines for the screening of thoracolumbar spine fracture. EAST Practice Management Guideline Committee. J Trauma. 2007 Sep; 63(3): 709 -718. Groves CJ, Cassar-Pullicino VN, Tins BJ, Tyrrell PN, Mc. Call IW. Chance-type flexion-distraction injuries in the thoracolumbar spine: MR imaging characteristics. Radiology 2005 Aug; 236(2): 601 -608. Harris JH Jr, Harris WH. The radiology of emergency medicine. 4 th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2000. pp. 276– 282. Kenyan O, Fisher CG, Vaccaro A, et al. Radiographic measurement parameters in thoracolumbar fractures: a systematic review and consensus statement of the Spine Trauma Study Group. Spine 2006; 31(5): E 156–E 165. Khurana B, Sheehan SE, Sodickson A, Bono CM, Harris MB. Traumatic thoracolumbar spine injuries: what the spine surgeon wants to know. Radio. Graphics. 2013 Nov-Dec; 33(7): 2031 -2046.

Suggested Readings Mohanty SP, Bhat NS, Abraham R, Ishwara Keerthi C. Neurological deficit and canal compromise in thoracolumbar and lumbar burst fractures. J Orthop Surg (Hong Kong) 2008; 16(1): 20– 23. Reid AB, Letts RM, Black GB. Pediatric Chance fractures: association with intraabdominal injuries and seatbelt use. J Trauma 1990; 30: 384– 391. Rogers LE and West OC. Thoracolumbar spine trauma. In Imaging skeletal trauma. 4 th edition. Saunders, 2014; 90 -127. Sethi MK, Schoenfeld AJ, Bono CM, Harris MB. The evolution of thoracolumbar injury classification systems. Spine J. 2009 Sep; 9(9): 780 -788. Vaccaro AR, Lehman RA Jr, Hurlbert RJ, et al. A new classification of thoracolumbar injuries: the importance of injury morphology, the integrity of the posterior ligamentous complex, and neurologic status. Spine (Phila Pa 1976). 2005 Oct 15; 30(20): 2325 -2333. Vaccaro AR, Zeiller SC, Hulbert RJ, et al. The thoracolumbar injury severity score: a proposed treatment algorithm. J Spinal Disord Tech. 2005 Jun; 18(3): 209 -215. Wood KB, Li W, Lebl DS, Ploumis A. Management of thoracolumbar spine fractures. Spine J. 2014; 14: 145– 164.
- Slides: 41