Thoracolumbar fractures Special situations Presenters name Arial 24

Thoracolumbar fractures Special situations Presenter‘s name Arial 24 pt Meeting Arial 24 pt Presenter‘s title Arial 20 pt City, Month, Year Arial 20 pt

Learning outcomes • Identify sacral fractures and be able to assess stability and need for surgical intervention • Be aware of conditions such as ankylosing spondylitis and osteoporosis and how they may alter management of a given thoracolumbar injury

Special situations • Sacral fractures • Ankylosing spondylitis • Osteoporotic fractures
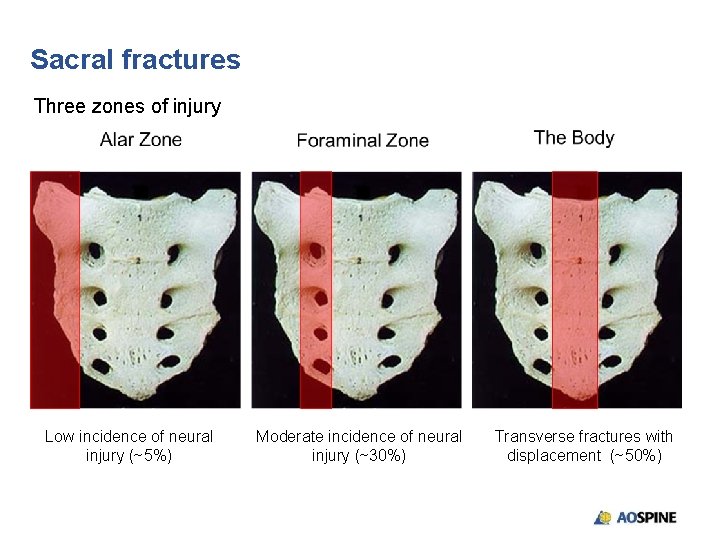
Sacral fractures Three zones of injury Low incidence of neural injury (~5%) Moderate incidence of neural injury (~30%) Transverse fractures with displacement (~50%)
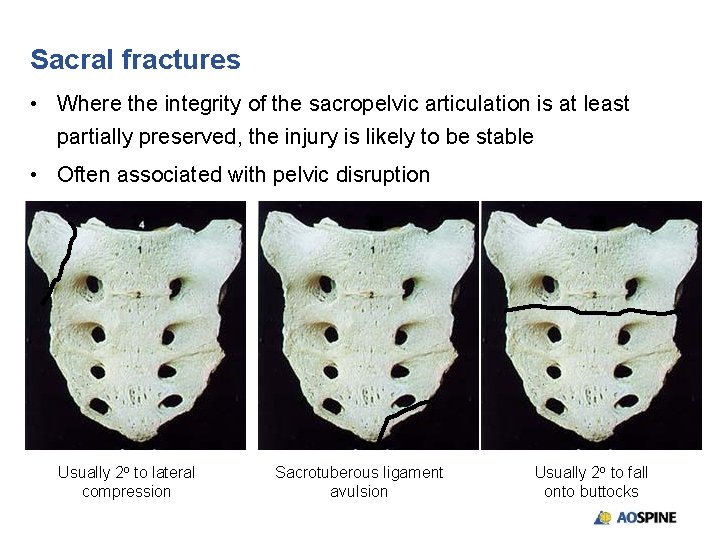
Sacral fractures • Where the integrity of the sacropelvic articulation is at least partially preserved, the injury is likely to be stable • Often associated with pelvic disruption Usually 2 o to lateral compression Sacrotuberous ligament avulsion Usually 2 o to fall onto buttocks
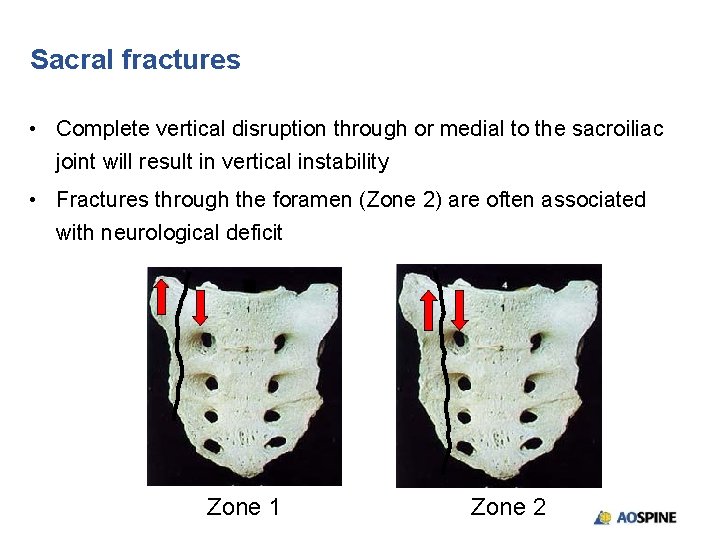
Sacral fractures • Complete vertical disruption through or medial to the sacroiliac joint will result in vertical instability • Fractures through the foramen (Zone 2) are often associated with neurological deficit Zone 1 Zone 2
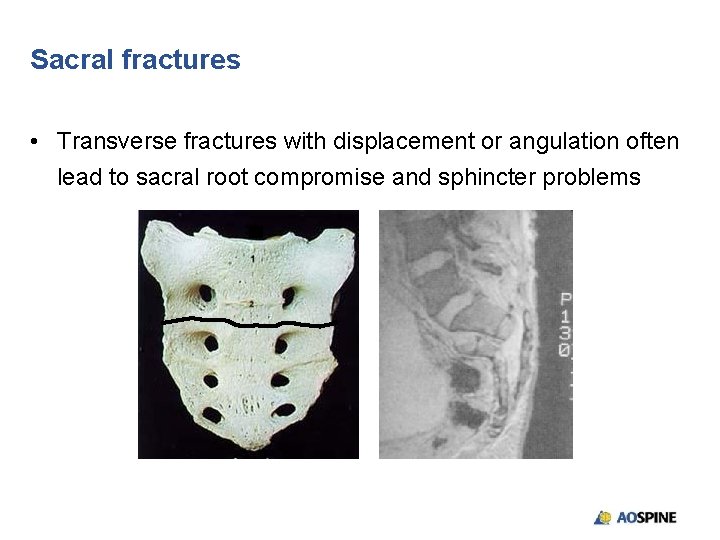
Sacral fractures • Transverse fractures with displacement or angulation often lead to sacral root compromise and sphincter problems

Take-home messages • Be aware of the possibility of sacral fractures • Often associated with pelvic disruption and require stabilization • Open reduction may be required to decompress sacral roots and ensure they are not caught in the fracture

Ankylosing spondylitis • Rigidity of spine creates a different biomechanical situation to that of the normal and mobile spine • Long lever arm results in issues similar to the management of long-bone fractures • Increased risk of neurological compromise, epidural hematoma and nonunion • Often extension injury due to fixed flexion deformity • 15– 20% delayed diagnosis • About half due to failure to diagnose at presentation • Remainder due to delayed presentation • ~ 70% present with neurological compromise
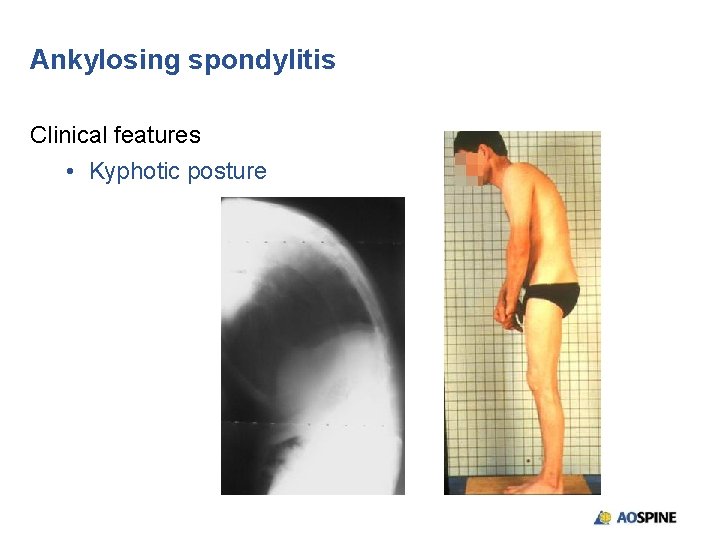
Ankylosing spondylitis Clinical features • Kyphotic posture
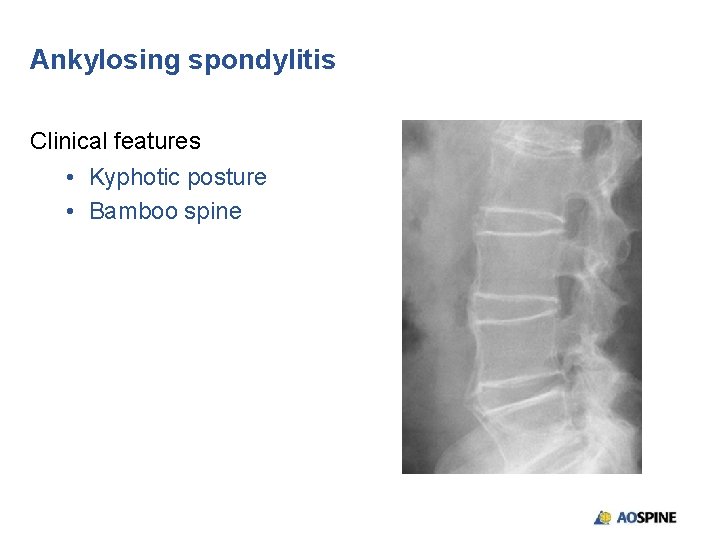
Ankylosing spondylitis Clinical features • Kyphotic posture • Bamboo spine
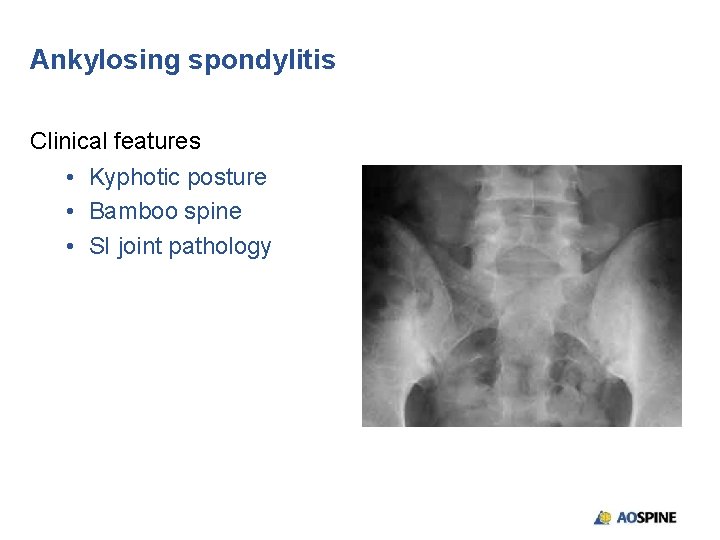
Ankylosing spondylitis Clinical features • Kyphotic posture • Bamboo spine • SI joint pathology

Ankylosing spondylitis • Flexed posture creates difficulties in nursing and stabilization • Often associated with osteopenia • High incidence of nonunion due to lever arm and difficulty maintaining alignment • Need to instrument long • Merit in AP approach, particularly in cervical spine, to improve posture and chance of achieving union

Ankylosing spondylitis Cervical spine • Often an extension injury • Beware of traction! • Requires stabilization • Placement of anterior graft helps improve sagittal balance • Requires anterior/posterior stabilization • Long construct to improve stability and chance of fusion
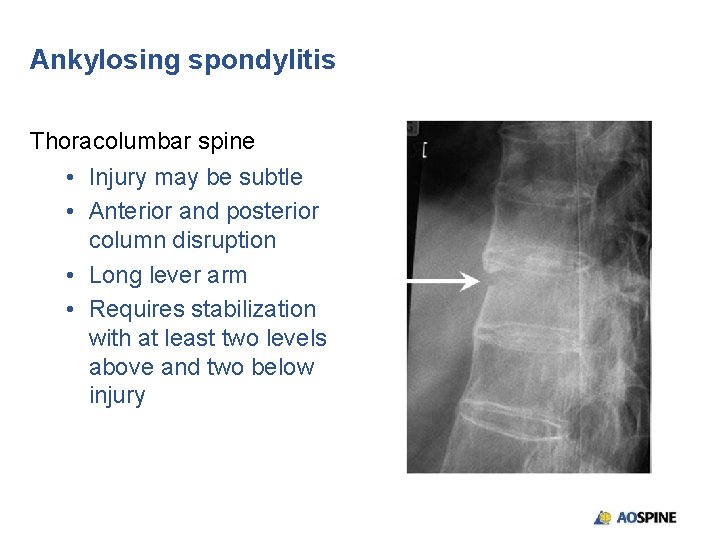
Ankylosing spondylitis Thoracolumbar spine • Injury may be subtle • Anterior and posterior column disruption • Long lever arm • Requires stabilization with at least two levels above and two below injury
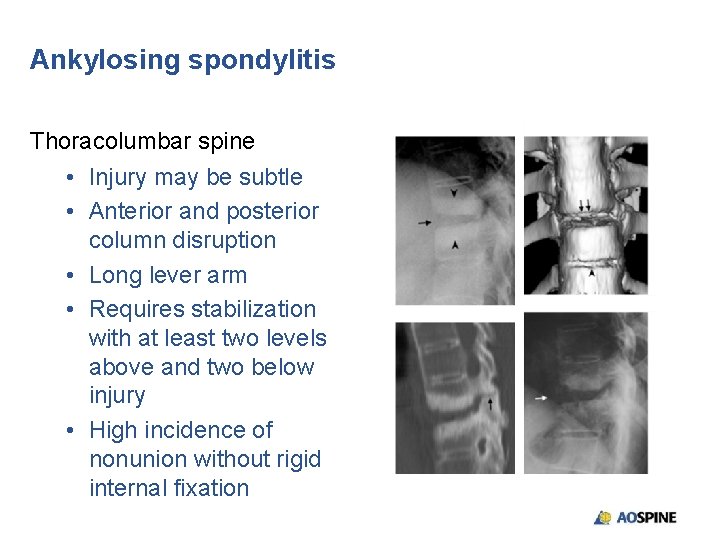
Ankylosing spondylitis Thoracolumbar spine • Injury may be subtle • Anterior and posterior column disruption • Long lever arm • Requires stabilization with at least two levels above and two below injury • High incidence of nonunion without rigid internal fixation

Take-home messages • Be aware of a spinal fracture in ankylosing spondylitis patients • Unless there are medical complications or comorbidities, stabilization is usually indicated • In the cervical spine, an anterior/posterior approach is often required • Instrument and fuse long in order to reduce the risk of instrumentation failure and nonunion

Osteoporosis • Associated with increased age • Progressive loss of vertebral height

Osteoporosis • Associated with increased age • Progressive loss of vertebral height • Leads to the development of senile kyphosis
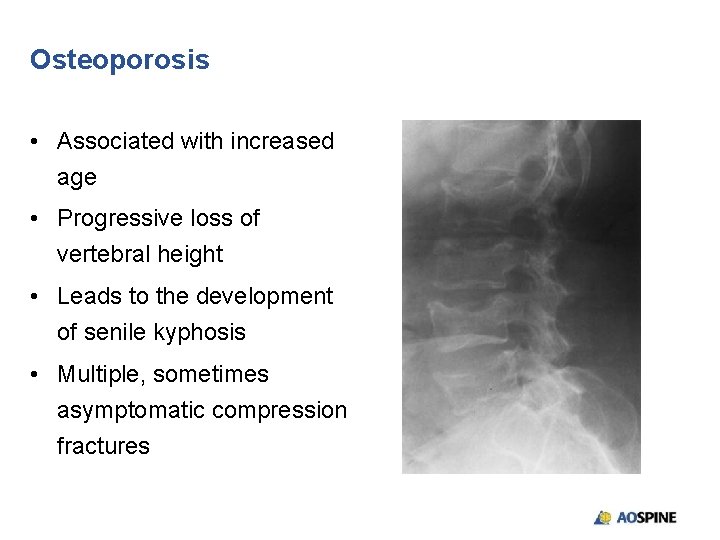
Osteoporosis • Associated with increased age • Progressive loss of vertebral height • Leads to the development of senile kyphosis • Multiple, sometimes asymptomatic compression fractures
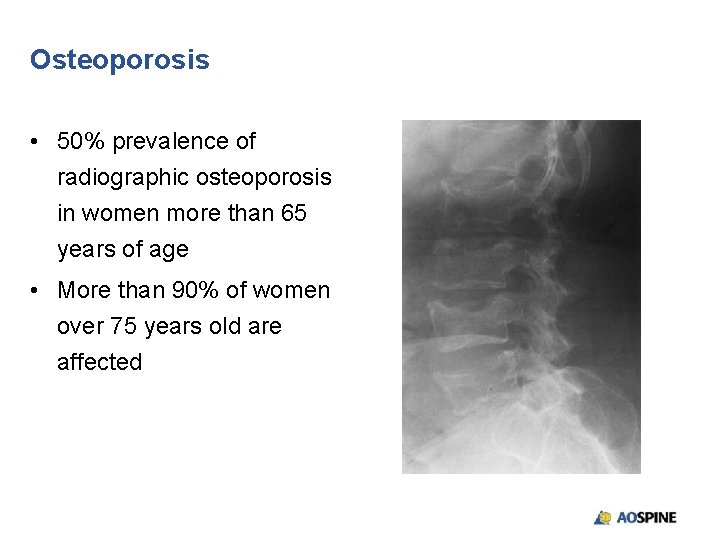
Osteoporosis • 50% prevalence of radiographic osteoporosis in women more than 65 years of age • More than 90% of women over 75 years old are affected
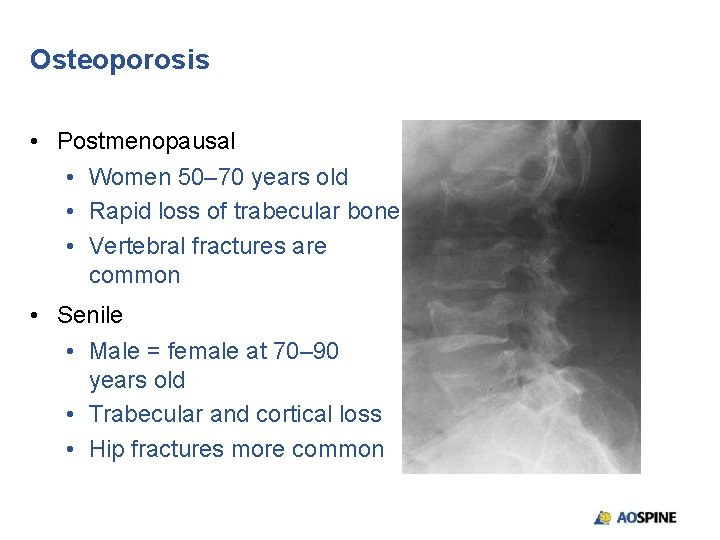
Osteoporosis • Postmenopausal • Women 50– 70 years old • Rapid loss of trabecular bone • Vertebral fractures are common • Senile • Male = female at 70– 90 years old • Trabecular and cortical loss • Hip fractures more common
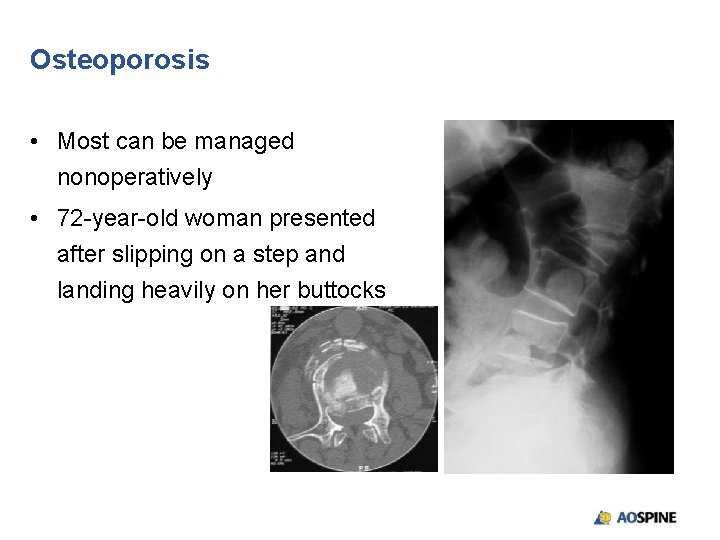
Osteoporosis • Most can be managed nonoperatively • 72 -year-old woman presented after slipping on a step and landing heavily on her buttocks
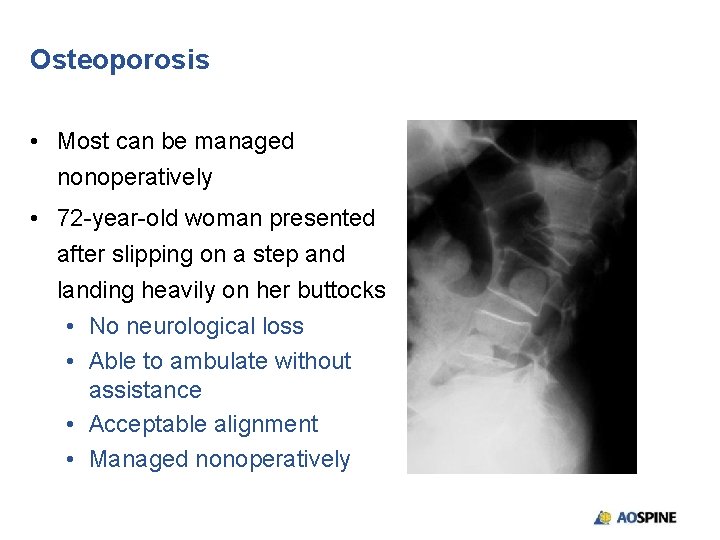
Osteoporosis • Most can be managed nonoperatively • 72 -year-old woman presented after slipping on a step and landing heavily on her buttocks • No neurological loss • Able to ambulate without assistance • Acceptable alignment • Managed nonoperatively
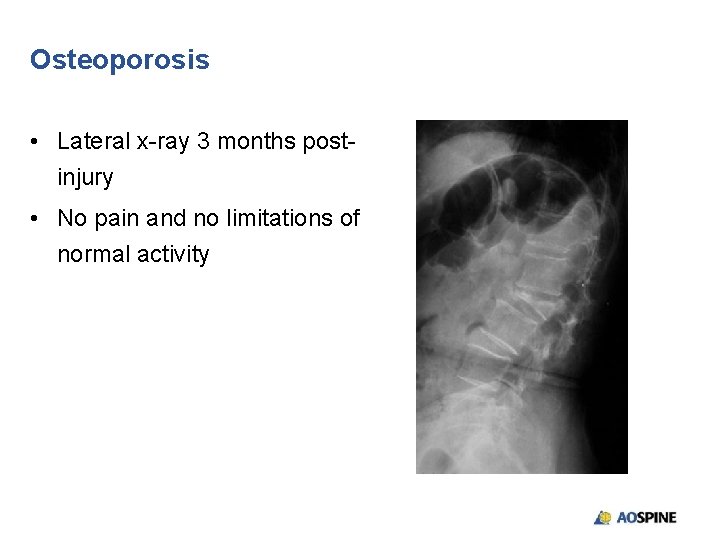
Osteoporosis • Lateral x-ray 3 months postinjury • No pain and no limitations of normal activity
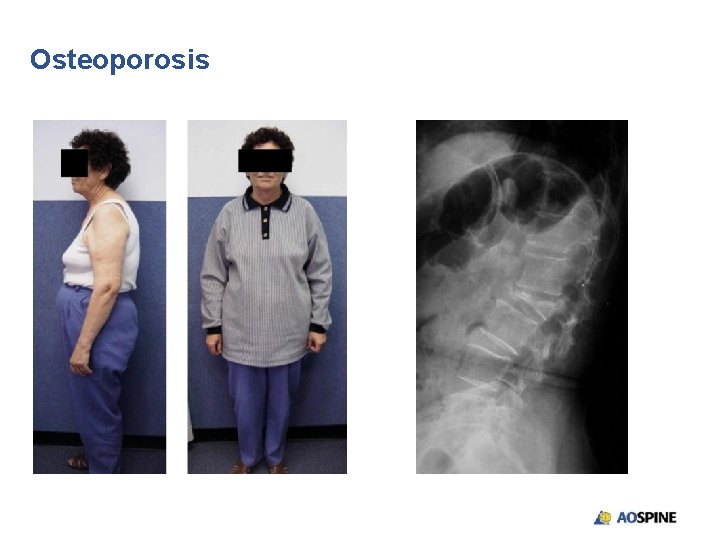
Osteoporosis

Osteoporosis • Where symptoms persist beyond 6 weeks, consider vetebroplasty
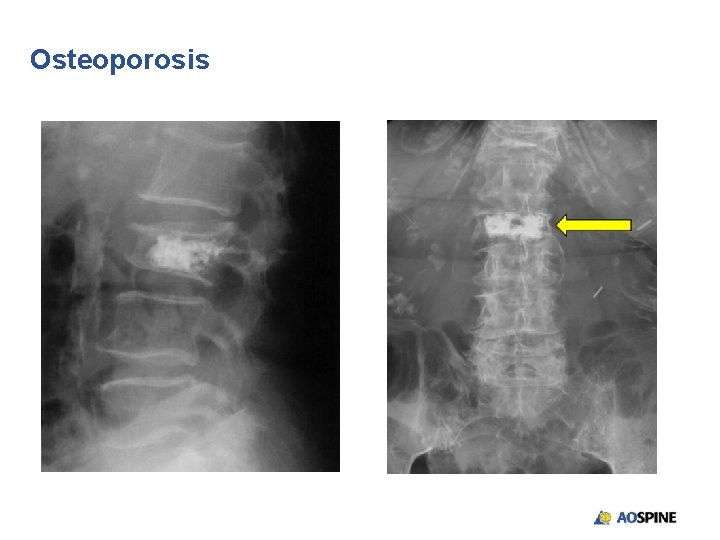
Osteoporosis
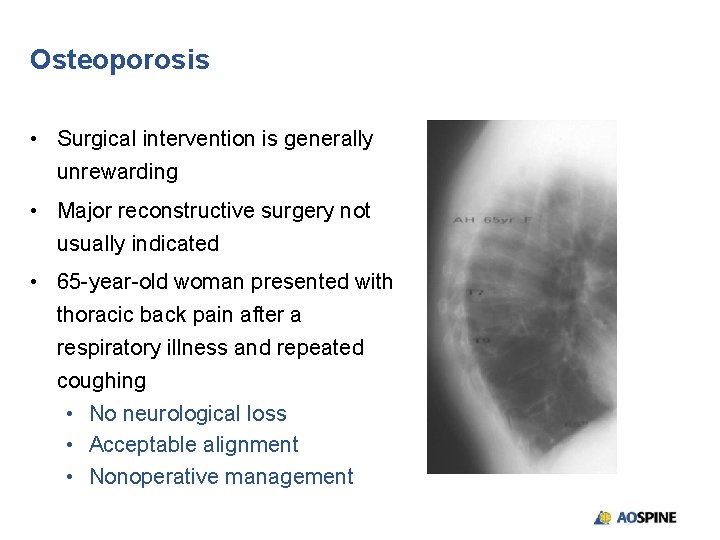
Osteoporosis • Surgical intervention is generally unrewarding • Major reconstructive surgery not usually indicated • 65 -year-old woman presented with thoracic back pain after a respiratory illness and repeated coughing • No neurological loss • Acceptable alignment • Nonoperative management
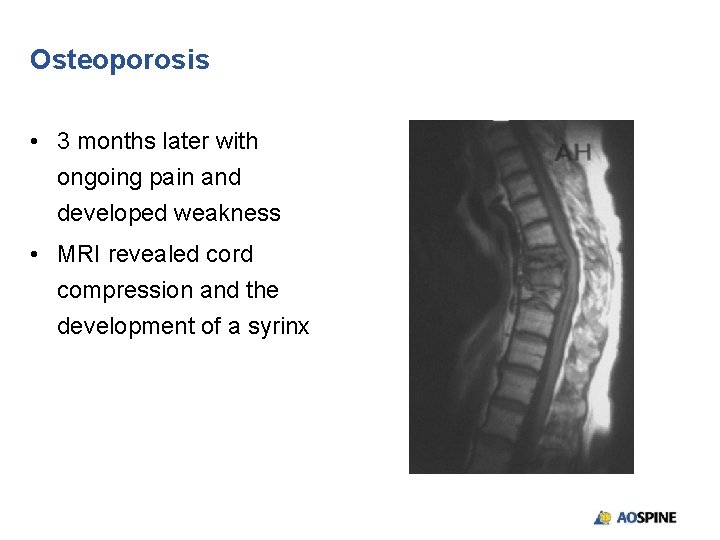
Osteoporosis • 3 months later with ongoing pain and developed weakness • MRI revealed cord compression and the development of a syrinx

Osteoporosis • Underwent surgical intervention • Good initial postoperative result • Good fixation above and below fractures
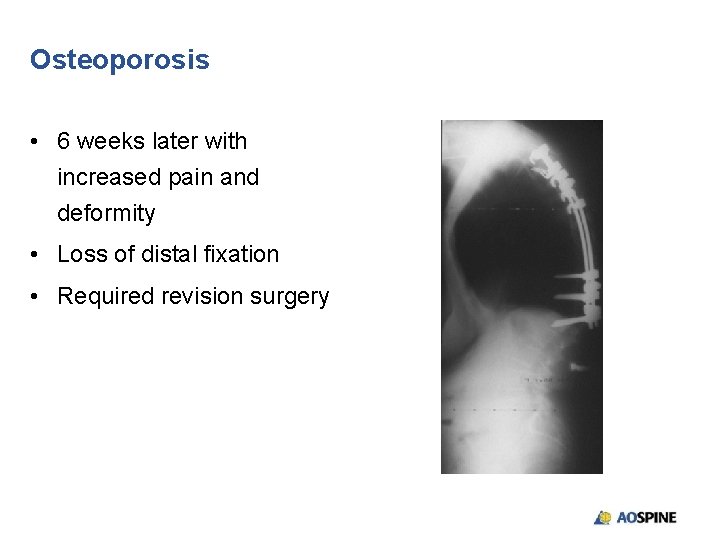
Osteoporosis • 6 weeks later with increased pain and deformity • Loss of distal fixation • Required revision surgery

Osteoporosis • 6 weeks later with increased pain and deformity • Loss of distal fixation • Required revision surgery • Extension of instrumentation

Take-home messages • Most can be managed nonoperatively • Consider vertebroplasty if symptoms persist beyond 6 weeks • If surgery is indicated: • Fuse long • Use cement to augment fixation • Use hooks to protect screws from pulling out • May require vertebroplasty at levels above and below instrumentation • May still not avoid junctional failure or compression fractures

Excellence in Spine
- Slides: 35