Thoracolumbar Fractures Sami Al Eissa MD Consultant Orthopedic

Thoraco-lumbar Fractures Sami Al Eissa, MD Consultant Orthopedic & Spine Surgery

Epidemiology • United State – 150000 to 160000 vertebral column fracture/ year. • 10000 -12000 spine cord injury – 15000 major thoraco-lumbar fracture/ year • 4700 – 5000 significant neurological deficit • Saudi Arabia – No national statistic exist – In one trauma center in Riyadh; • Over 100 patients admitted yearly with major T/L fracture from MVA only
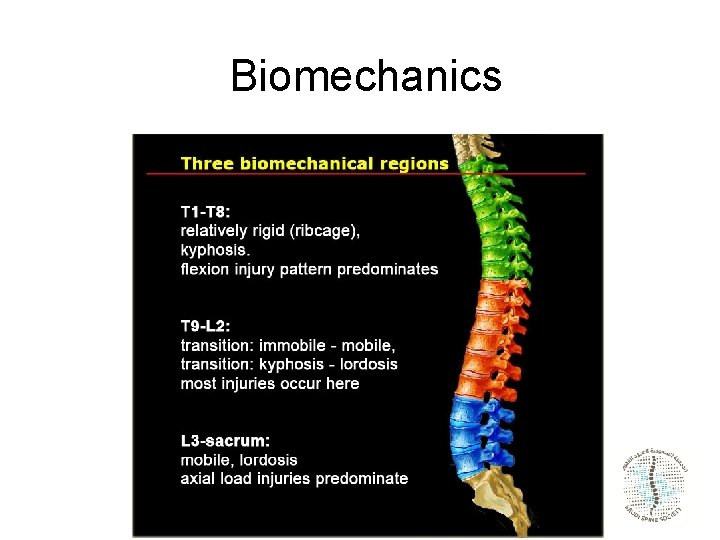
Biomechanics
Biomechanics T 2 – T 9 • Shielded by; – Paraspinal musculature – Sternum & Rigid thoracic rib stiffness – Coronal alignment of facet joint » Resist flexion / Extension » Minimal resistance to torsion – Physiological kyphosis compression/ flexion injuries

Biomechanics • T 11 – L 1; Transition zone between Kyphotic immobile segment & Lordotic mobile segment –Predispose to injury by rotational and shearing forces • Rib are not present • Facet have not re-oriented completely 60% of TL fractures occur at this junction
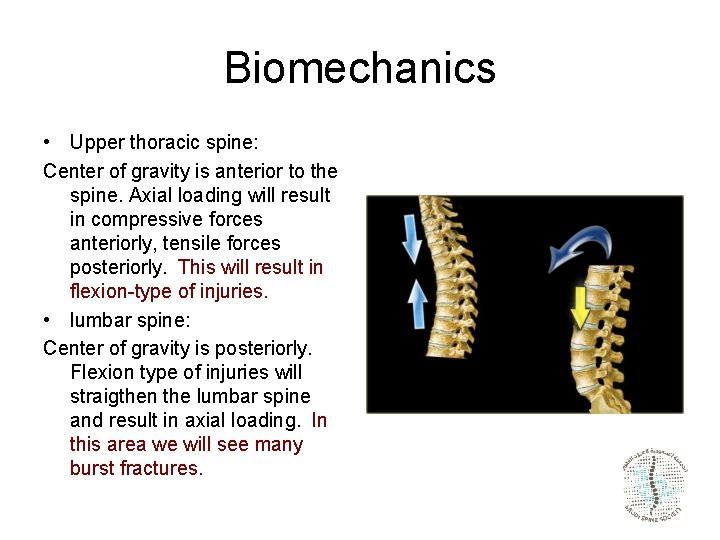
Biomechanics • Upper thoracic spine: Center of gravity is anterior to the spine. Axial loading will result in compressive forces anteriorly, tensile forces posteriorly. This will result in flexion-type of injuries. • lumbar spine: Center of gravity is posteriorly. Flexion type of injuries will straigthen the lumbar spine and result in axial loading. In this area we will see many burst fractures.
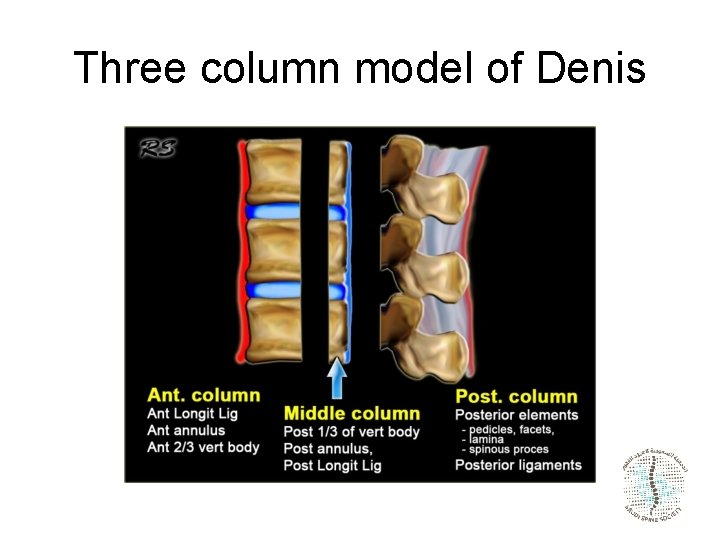
Three column model of Denis
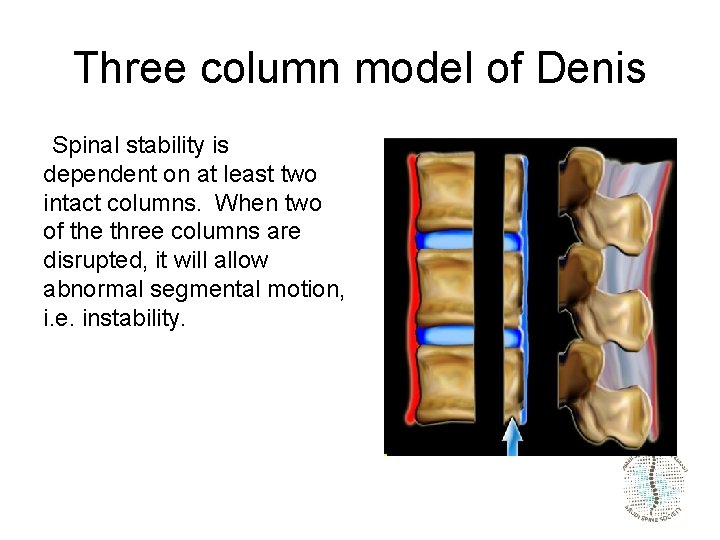
Three column model of Denis Spinal stability is dependent on at least two intact columns. When two of the three columns are disrupted, it will allow abnormal segmental motion, i. e. instability.

Thoracolumbar fractures • 75% to 90% of spinal fractures occur in the thoracic and lumbar spine • Most of these occurring at thoracolumbar junction (T 10 L 2). • Little consensus regarding injury classification and management. • Treatment varies widely, from bracing to circumferential fusion, based on geographical, institutional, and surgeon preferences rather than on scientific evidence.

General guidelines • Stability • Neurological compromise • Deformity

How can we decide?
Conservative Brace or no brace How can not decide? Posterior approach Surgery Bed rest Anterior approach How many levels?
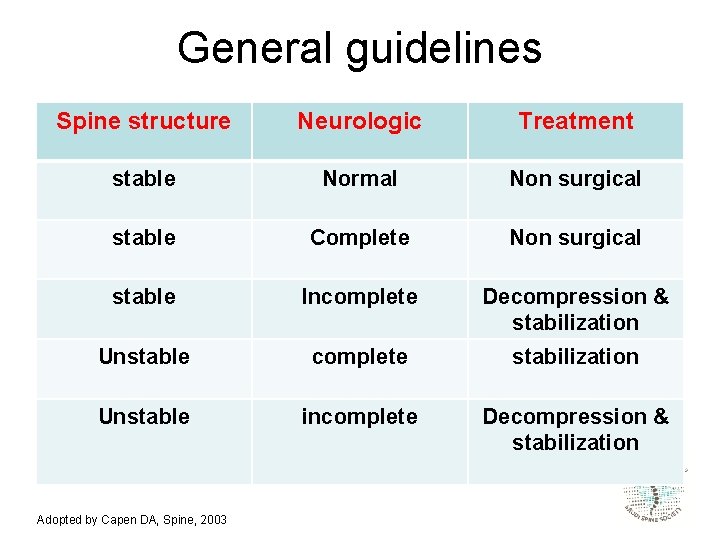
General guidelines Spine structure Neurologic Treatment stable Normal Non surgical stable Complete Non surgical stable Incomplete Decompression & stabilization Unstable complete stabilization Unstable incomplete Decompression & stabilization Adopted by Capen DA, Spine, 2003

Classification • Many systems are convoluted, with an impractical number of variables. Others are too simple, lacking sufficient detail to provide clinically relevant information. lack of a widely accepted classification system
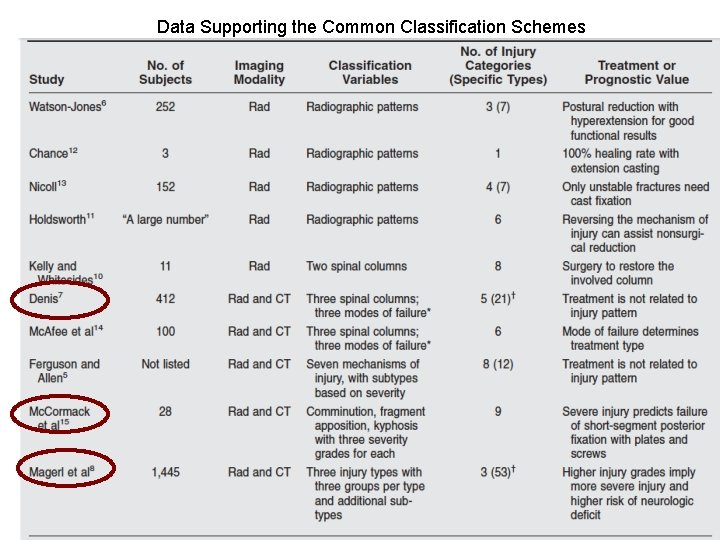
Data Supporting the Common Classification Schemes

Classification • Several classification systems • Most commonly used are – Denis classification system – Load sharing classification described by Mc. Comack – AO classification system
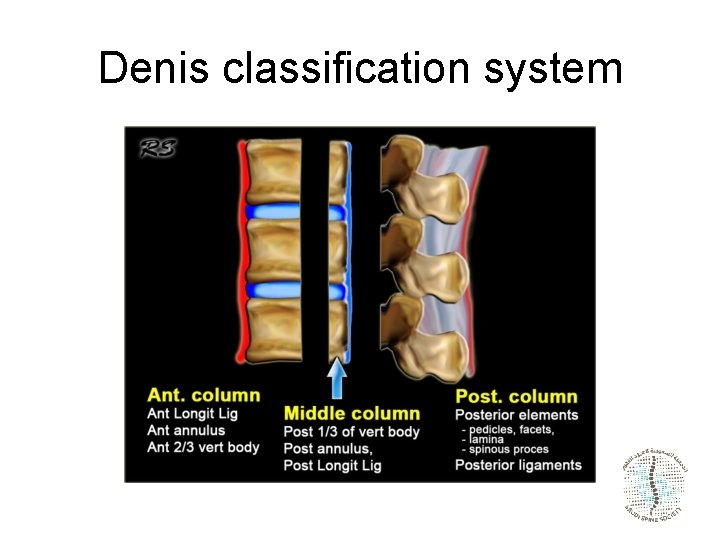
Denis classification system
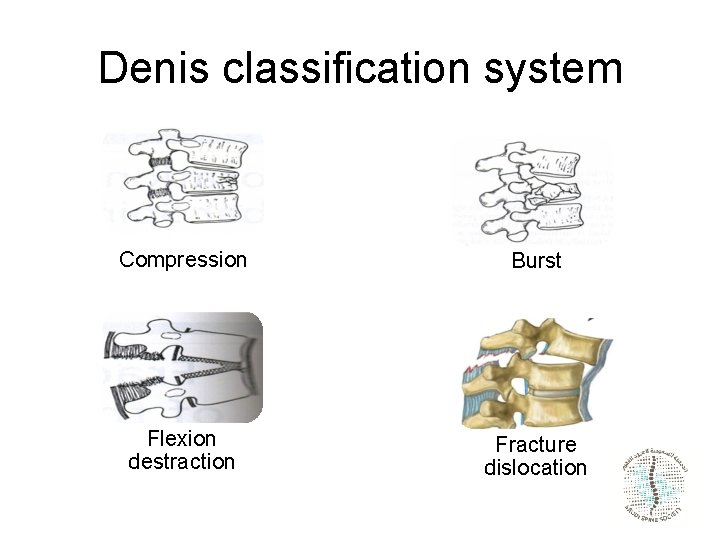
Denis classification system Compression Burst Flexion destraction Fracture dislocation

Denis classification system • Not sufficiently detailed to account for all fracture types • Does not provide prognostic information for the neurological status of does not adequately aid surgical decision making.

AO classification • Simple Morphology • Neurological Injury • Modefiers

AO Classification
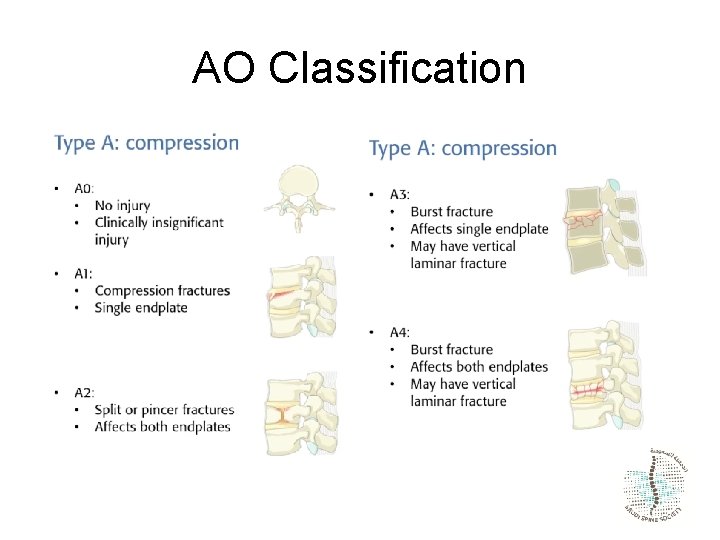
AO Classification
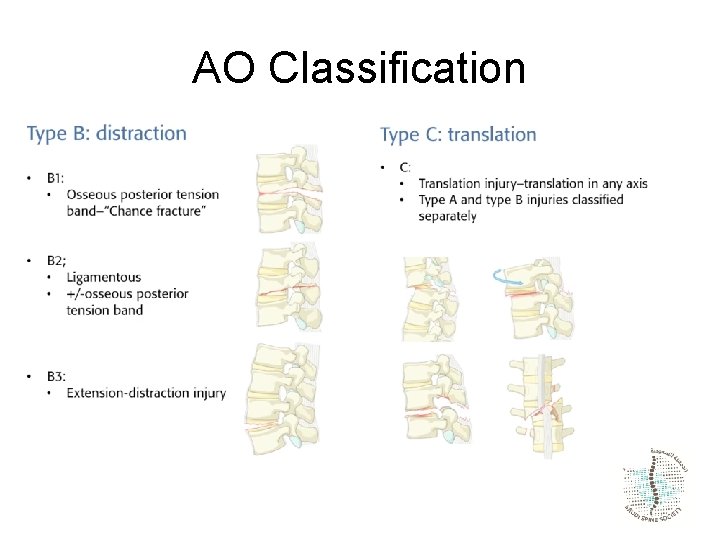
AO Classification
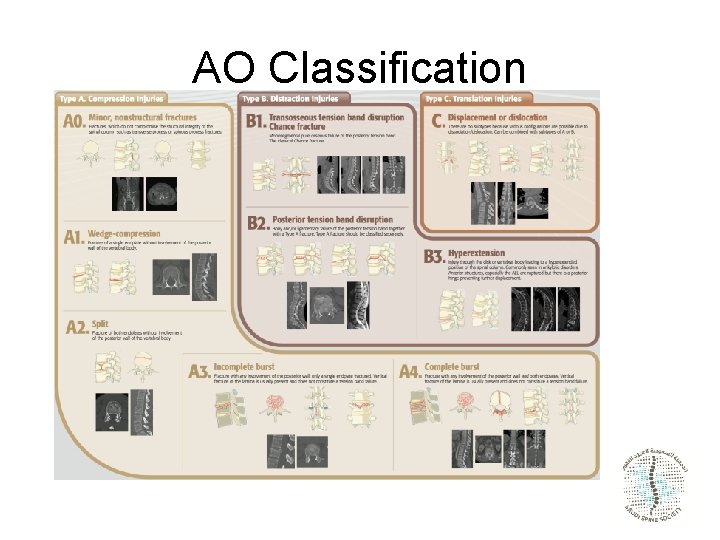
AO Classification
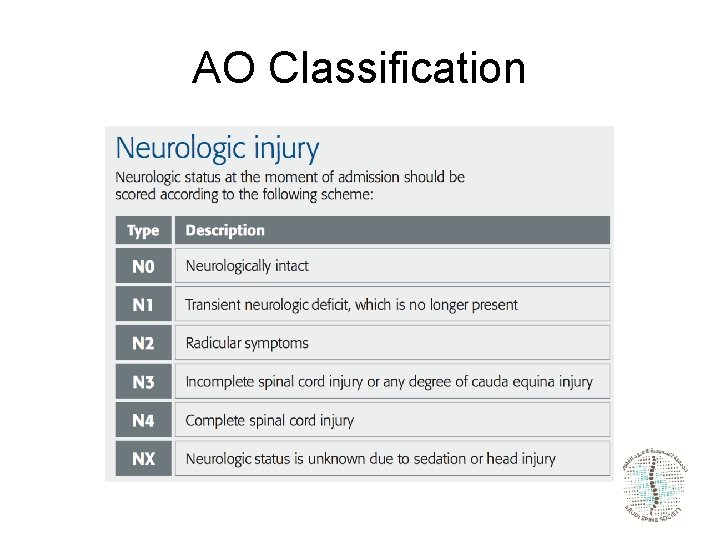
AO Classification

AO classification
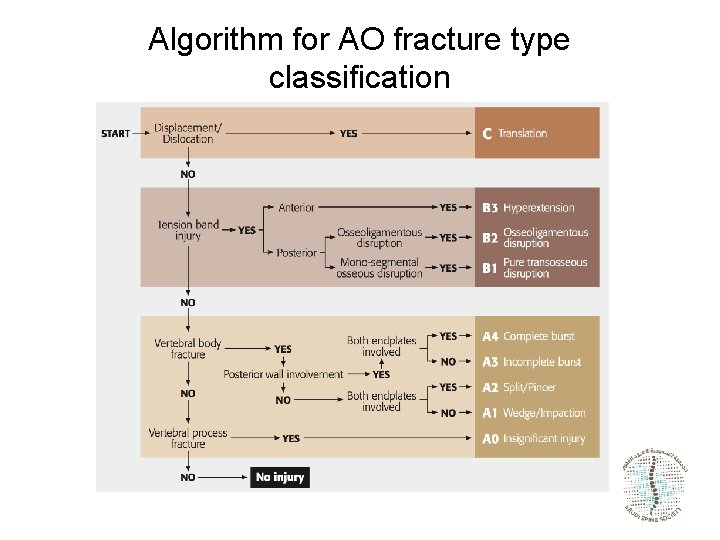
Algorithm for AO fracture type classification

Thoracolumbar Injury Classification and Severity Score • Introduced by the Spine Trauma Study Group in 2005 • The TLICS is the first system to incorporate the neurologic status of the patient
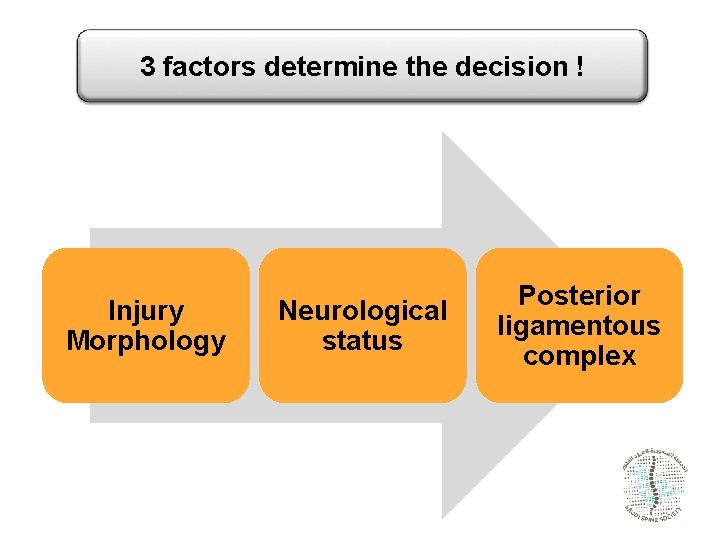
3 factors determine the decision ! Injury Morphology Neurological status Posterior ligamentous complex
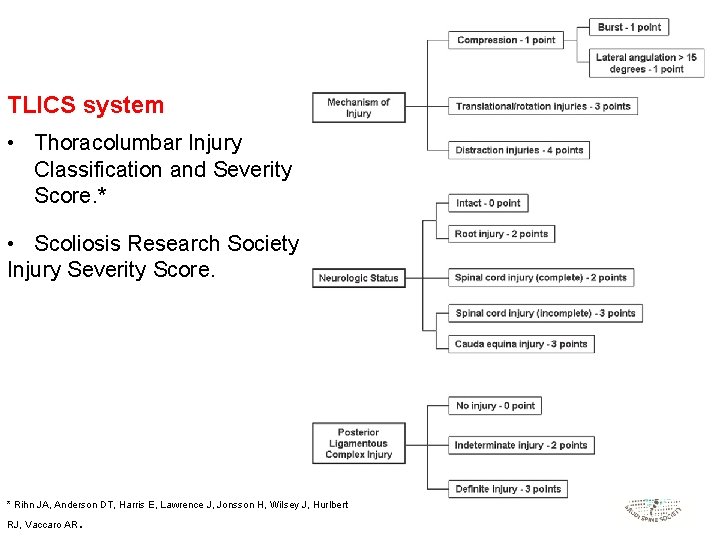
TLICS system • Thoracolumbar Injury Classification and Severity Score. * • Scoliosis Research Society Injury Severity Score. * Rihn JA, Anderson DT, Harris E, Lawrence J, Jonsson H, Wilsey J, Hurlbert . RJ, Vaccaro AR
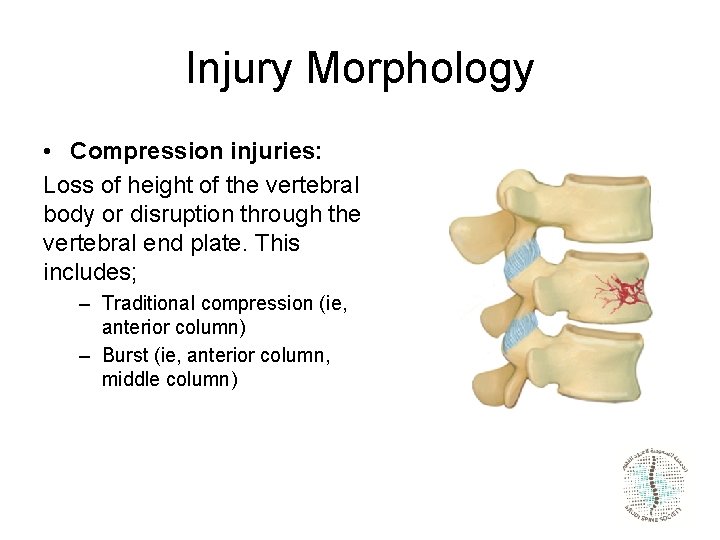
Injury Morphology • Compression injuries: Loss of height of the vertebral body or disruption through the vertebral end plate. This includes; – Traditional compression (ie, anterior column) – Burst (ie, anterior column, middle column)
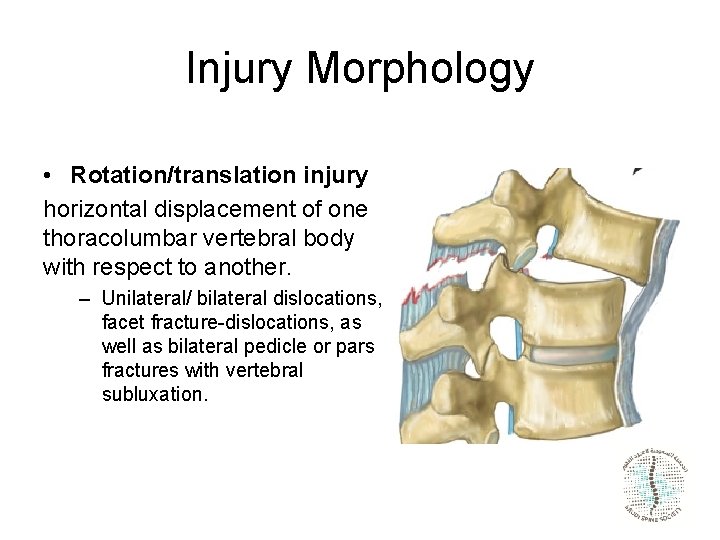
Injury Morphology • Rotation/translation injury horizontal displacement of one thoracolumbar vertebral body with respect to another. – Unilateral/ bilateral dislocations, facet fracture-dislocations, as well as bilateral pedicle or pars fractures with vertebral subluxation.
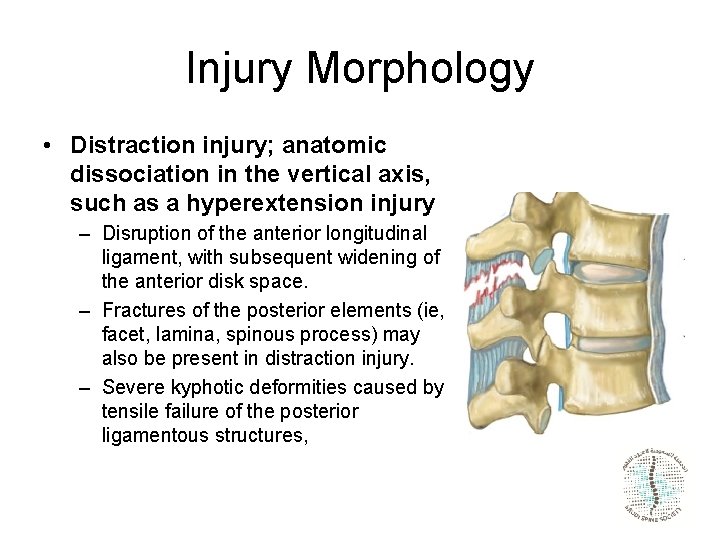
Injury Morphology • Distraction injury; anatomic dissociation in the vertical axis, such as a hyperextension injury – Disruption of the anterior longitudinal ligament, with subsequent widening of the anterior disk space. – Fractures of the posterior elements (ie, facet, lamina, spinous process) may also be present in distraction injury. – Severe kyphotic deformities caused by tensile failure of the posterior ligamentous structures,
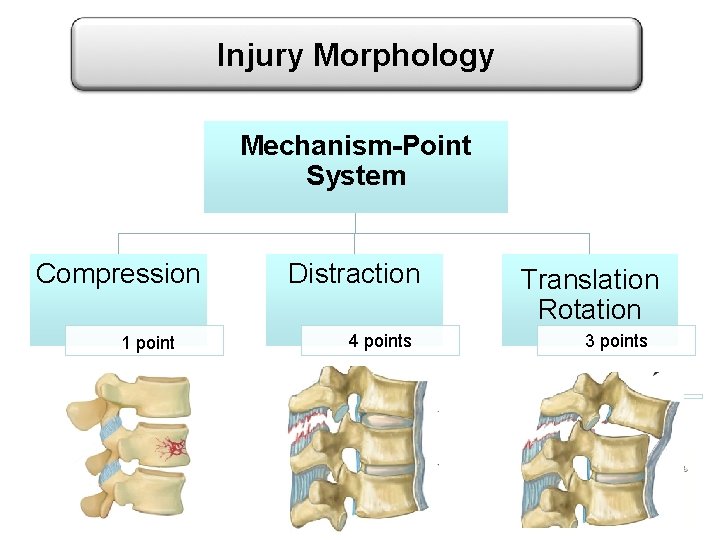
Injury Morphology Mechanism-Point System Compression 1 point Distraction 4 points Translation Rotation 3 points

Neurologic status • Described in increasing order of urgency: neurologically – Intact – Nerve root injury – Complete (motor and sensory) spinal cord or cauda equina injury – Incomplete (motor or sensory) spinal cord or cauda equina injury.
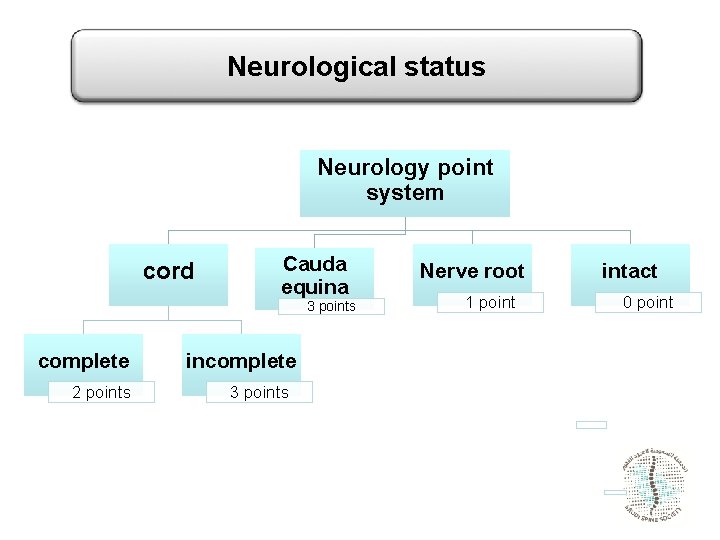
Neurological status Neurology point system cord Cauda equina 3 points complete 2 points incomplete 3 points Nerve root 1 point intact 0 point

Posterior Ligamentous Complex Integrity • Anatomic structures of the PLC include the supraspinous ligament, interspinous ligament, ligamentum flavum, and facet joint capsules. • plays a critical role in protecting the spine and spinal cord against excessive flexion, rotation, translation, and distraction. Once disrupted, the ligamentous structures demonstrate poor healing ability

Posterior Ligamentous Complex Integrity • Categorized – Intact, Indeterminate, and Disrupted. • Assessment based on – – Clinical exam Plain radiographs CT scans magnetic resonance Widening of the interspinous space or of the facet joints, empty facet joints, facet perch or subluxation, Dislocation of the spine
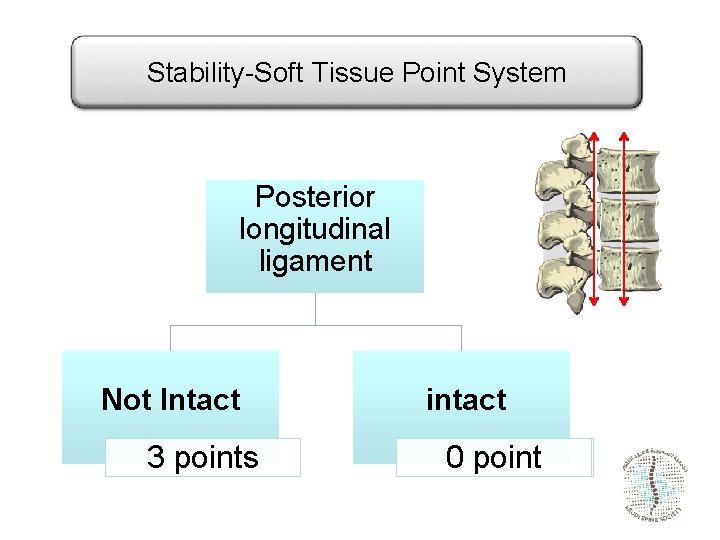
Stability-Soft Tissue Point System Posterior longitudinal ligament Not Intact 3 points intact 0 point
Next Step - Direct TX Assign Points Conservative Surgery


Treatment • Fractures with 4 points or less = non operative. • Fractures with 5 points or more = surgery
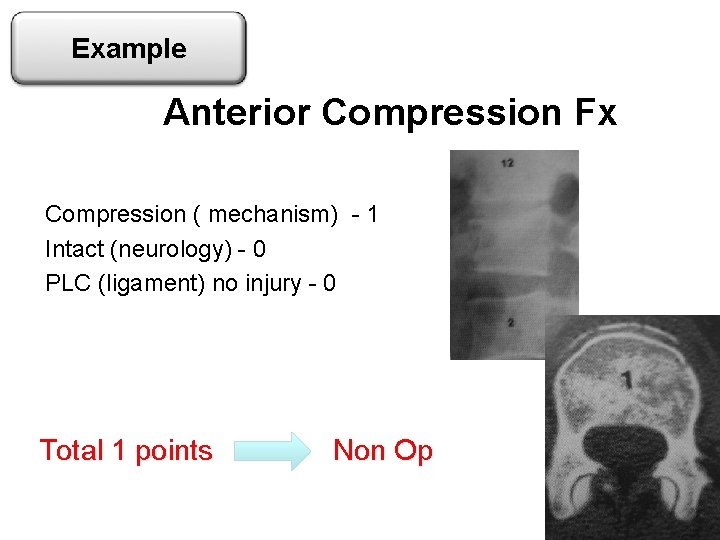
Example Anterior Compression Fx Compression ( mechanism) - 1 Intact (neurology) - 0 PLC (ligament) no injury - 0 Total 1 points Non Op
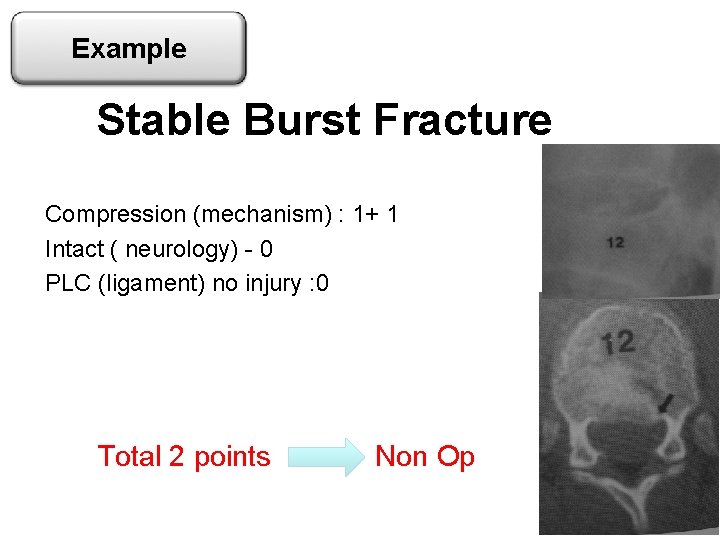
Example Stable Burst Fracture Compression (mechanism) : 1+ 1 Intact ( neurology) - 0 PLC (ligament) no injury : 0 Total 2 points Non Op
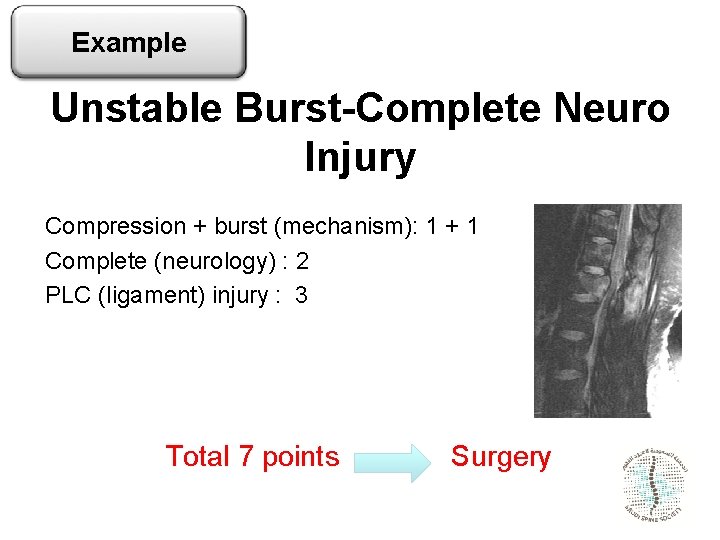
Example Unstable Burst-Complete Neuro Injury Compression + burst (mechanism): 1 + 1 Complete (neurology) : 2 PLC (ligament) injury : 3 Total 7 points Surgery
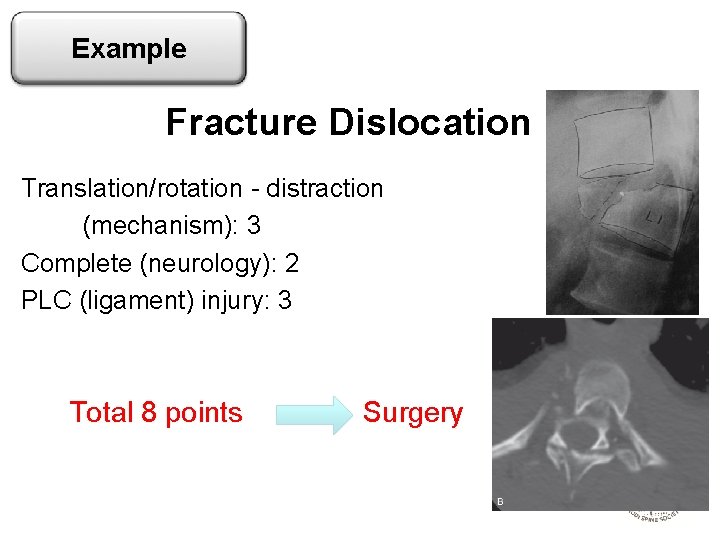
Example Fracture Dislocation Translation/rotation - distraction (mechanism): 3 Complete (neurology): 2 PLC (ligament) injury: 3 Total 8 points Surgery
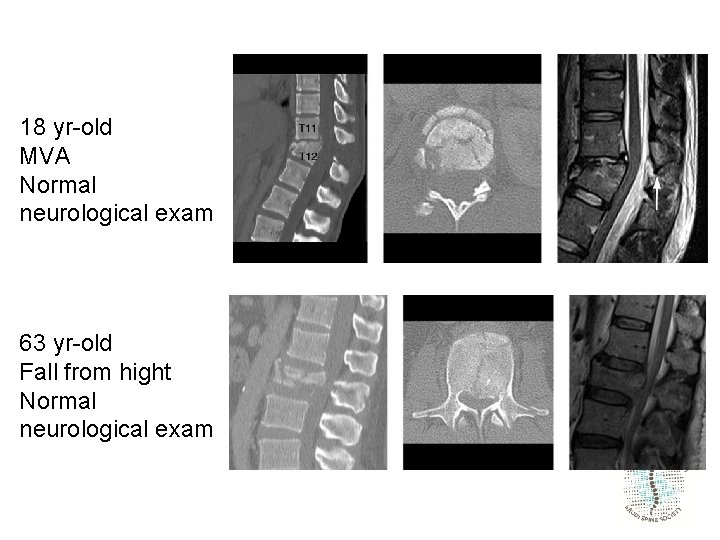
18 yr-old MVA Normal neurological exam 63 yr-old Fall from hight Normal neurological exam


Limitation of TLICS system

• Not for pediatric population • For acute injuries • cannot be applied to; – – – Symptomatic epidural hematoma Spinal cord injury without radiographic abnormalities posttraumatic deformity Iatrogenic spinal instability Pathologic fractures associated with tumor or infection.

• TLICS is a reliable system for assessing fractures of the thoracic and lumbar spine when used by experts. • the posterior ligamentous complex subcomponent score was the least reliable component.

Timing of surgery • Remain unclear. • Lack of class one evidence, no standard guidelines.

Timing of surgery • Preclinical studies suggest that early surgical decompression of the spinal cord is important in mitigating secondary injury. • The completeness of SCI injury seems to be the key prognostic factor • To date …. there is no robust evidence to suggest that early surgical intervention in t. SCI is superior. • Surgical decompression performed before 24 h post injury has the potential to result in superior motor recovery in comparison with late surgery performed at or after 24 h post injury
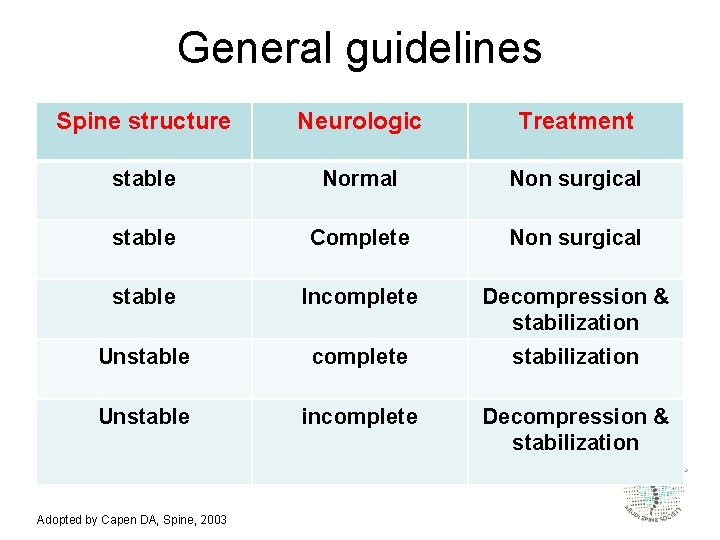
General guidelines Spine structure Neurologic Treatment stable Normal Non surgical stable Complete Non surgical stable Incomplete Decompression & stabilization Unstable complete stabilization Unstable incomplete Decompression & stabilization Adopted by Capen DA, Spine, 2003

Conclusion • Have a clear understanding to nature of the fracture and it’s consequences. Stability, deformity, and neurological picture will remain the main factors determining the surgical decision
- Slides: 55