Thoracic Anaesthesia One Lung Ventilation OLV By Asremzee
Thoracic Anaesthesia & One Lung Ventilation (OLV) By Asremzee Ab Razak

Indications for Thoracic Surgery Lung related surgery n n n Lobectomy, pneumonectomy Drainage of empyema Closure of bronchopleural fistula Cardiac surgery Aortic surgery Resection of thymus, retrosternal thyroid or other mediastinal tumours. Oesophagectomy (thoracoabdominal approach) Trauma Surgery n n Repair of rupture airways or pulmonary vessels Lung resection Diagnostic Procedures: n Thoracoscopy, mediastinoscopy

Probs a/w Thoracic Surgery Preoperative assessment n n Patient may have CVS and Respiratory impairments Patient with carcinoma of esophagus may be cachexic, malnourished, and have electrolytes abnormalities.

Probs a/w Thoracic Surgery Nature of Surgery n Most of the surgical procedures are major cases with significant physiological changes, massive blood loss and long operating time.

Probs a/w Thoracic Surgery Requirement of anaesthesia n Insertion of Double Lumen Tube (DLT) and management of one lung ventilation (OLV), including management if hypoxaemia occurs during OLV

Anaesthetic Management Preoperative Assessment n n Emphasis on CVS and RESPIRATORY systems Consultation may Involving; cardiologist, respiratory physician if indicated. Pre-op test for suitability of pt for pneumonectomy, lobectomy mostly usually done by thoracic surgeon. Endocrinophaties (rare) may be seen in pt with Ca of Bronchus; eg: w Myasthenic Syndrome (Eaton Lambert Syndrome) w Ectopic hormone secretion eg. ACTH, PTH w Patient with myasthenia gravis for thymomectomy

Preoperative Preparation Cessation of smoking Optimizing medical condition Nutrition especially for Ca of esophagus n TPN to improve pt preoperatively Treatment of any lung Infection (A/B) Bronchodilators during peri-operative period Chest physiotherapy and breathing exersices: n n Postural drainage Physiotherapy & suction Deep breathing & coughing exercises Incentive spirometry

Preoperative Preparation (cont) Prophylactic digilization; Controversial. n n To reduce the incidence of Supraventricular arrhytmias & post pneumonectomy edema Now limited use w (doubt of effectiveness) w Problems of toxcity perioperatively These measures are extremely useful and have been shown to reduce perioperative morbidity and mortality.

Investigations Baseline FBC Renal profile, RBS ECG, CXR More detailed tests; n ECHO, Stress test (if indicated) Baseline ABG Lung Function Test

Premedication Depends on general status of the patient. IM narcotic analgesic better than oral sedation in Ca of esophagus d/t uncertain drug absorption from GIT. Omit premedication in cachexic, malnourished patient

Intra. Operative Management Monitoring Checklist to be established before commencing anaesthesia; n n n n ECG Blood Pressure (NIBP / IBP intra arterial) CVP Pulse oxymetry Capnography Urine Output (CBD in Situ) Temperature (Probe In Situ) Peripheral Nerve Stimulator

One Lung Ventilation (OLV) It is a method for lung separation To facilitate ventilatory management under certain conditions. Mainly used in thoracic surgery Cause significant physiological change d/t V/Q mismatch

Indication of OLV

Absolute Indication of OLV 1. Isolation of each lung to prevent contamination of a healthy lung a. Infection (abscess, infected cyst) b. Massive hemorrhage 2. Control of distribution of ventilation to only one lung a. Bronchopleural fistula b. Bronchopleural cutaneous fistula c. Unilateral cyst or bullae d. Major bronchial disruption or trauma 3. Unilateral lung lavage 4. Video assisted thoracoscopic surgery

Relative Indication of OLV 1. Surgical exposure—high priority a. Thoracic aortic aneurysm b. Pneumonectomy c. Upper lobectomy 2. Surgical exposure—low priority a. Esophageal surgery b. Middle and lower lobectomy c. Thoracoscopy under general anesthesia d. Thoracic spine procedures 3. Post removal of totally occluding chronic unilateral pulmonary emboli
Other Indication of OLV A. Patient related: confine infection or bleeding to one n n lung, separate ventilation to each lung (bronchopulmonary fistula, tracheobronchial disruption, large lung cyst or bulla), severe hypoxemia due to unilateral lung disease. B. Procedure related: repair of thoracic aortic n n n aneurysm, lung resection (pneumonectomy, lobectomy, segmental resection), thoracoscopy, esophageal surgery, single lung transplantation, anterior approach to the thoracic spine, bronchoalveolar lavage.
Positioning of patient in thoracic surgery Most of the time in lateral decubitus position with dependent lung below. n n d/t most lung resection done vie posterior approach. Nondependent lung above. Proper positioning is crucial to avoid injury and facilitate surgical exposure n n n Lower arm is flexed Upper arm extended in front of the head pulling the scapula way from the operative field. 2 Pillows- between arms and legs. Axillary roll beneath dependent axilla – avoid injury to brachial plexus. Pressure is avoided to the eyes and dependent ear
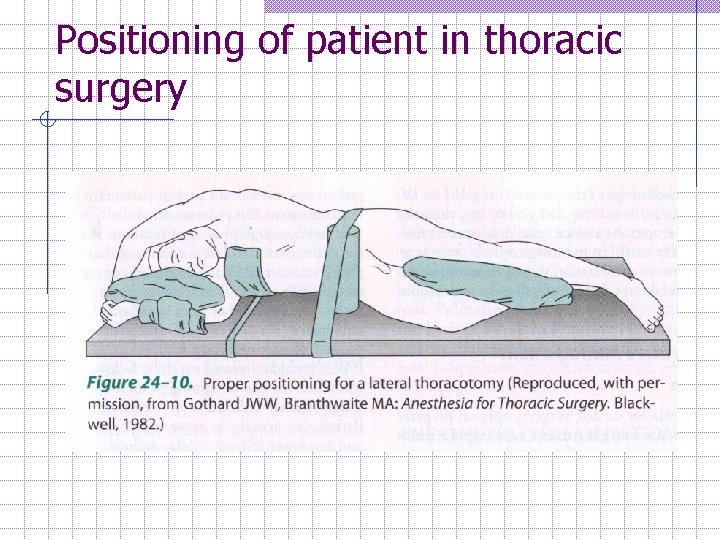
Positioning of patient in thoracic surgery

Several Terms to Know Shunting n n A process whereby desaturated, mixed venous blood from R heart return to the L heart without being saturated with Oxygen in the lungs. Overall effect – to Decrease (dilute) arterial O 2 content (a. k. a. R to L Shunts) w In absence of pulmonary congestion it do not produce hypoxaemia n Types of shunting w Absolute – Anatomic Shunts (V/Q = 0) w Relative – in area og lung with low but finite V/Q ratio w Can be partially corected by Fi. O 2 (not for Absolute shunt)

Several Terms to Know Venous Admixture n n The amount of Mixed Venous Blood that would have to be mixed with pulmonary end capillary blood to account for the difference in O 2 tension between arterial and pulmonary end capillary blood. Qt x Ca. O 2 = (Qs x Cv. O 2) + (Qc x Cc. O 2)
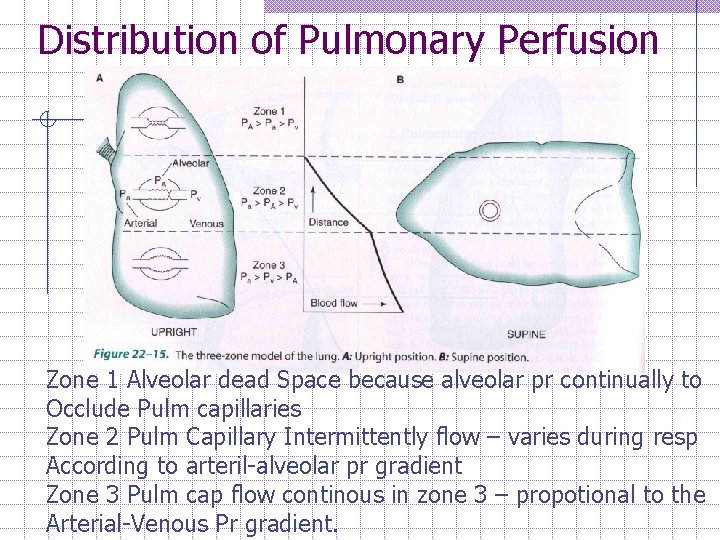
Distribution of Pulmonary Perfusion Zone 1 Alveolar dead Space because alveolar pr continually to Occlude Pulm capillaries Zone 2 Pulm Capillary Intermittently flow – varies during resp According to arteril-alveolar pr gradient Zone 3 Pulm cap flow continous in zone 3 – propotional to the Arterial-Venous Pr gradient.
Ventilation/Perfusion (V/Q) Ratio Normal n n Alveolar ventilation ~ 4 L/min Pulm capillary perfusion ~ 5 L/min V/Q = ~0. 8 Ranges from 0 (no ventilation) to infinite (no perfusion) – intrapulmonary Shunt

Physiology of the Lateral Decubitus Position. Ventilation and blood flow of the lungs in lateral decubitus position is different than in upright position. These variables will now be considered as they pertain to the lateral decubitus position under six circumstances that are encountered during thoracic surgery.

Physiology of the Lateral Decubitus Position. 6 circumstances that are encountered during thoracic surgery. 1. 2. 3. 4. 5. 6. LATERAL POSITION, AWAKE, BREATHING SPONTANEOUSLY, CHEST CLOSED. LATERAL POSITION, AWAKE, BREATHING SPONTANEOUSLY, CHEST OPEN. LATERAL POSITION, ANESTHESIZED, BREATHING SPONTANEOUSLY, CHEST CLOSED. LATERAL POSITION, ANESTHESIZED, BREATHING SPONTANEOUSLY, CHEST OPEN. LATERAL POSITION, ANESTHESIZED, PARALYZED, CHEST OPEN. ONE LUNG VENTILATION, ANESTHESIZED, PARALYZED, CHEST OPEN.
1) LATERAL POSITION, AWAKE, BREATHING SPONTANEOUSLY, CHEST CLOSED. Distribution of blood flow and ventilation is similar to that in the upright position but turned by 90 degrees. Blood flow and ventilation to the dependent lung are significantly greater than to the nondependent lung. Good V®/Q® matching at the level of the dependent lung results in adequate oxygenation in the awake patient breathing spontaneously.

1) LATERAL POSITION, AWAKE, BREATHING SPONTANEOUSLY, CHEST CLOSED. 2 important concepts in this situation. 1. perfusion is gravity dependent, the vertical hydrostatic gradient is smaller in the lateral than in the upright position; therefore, zone 1 is usually less extended. 2. In regard to ventilation, the dependent hemidiaphragm is pushed higher into the chest by the abdominal contents compared with the nondependent lung hemidiaphragm.
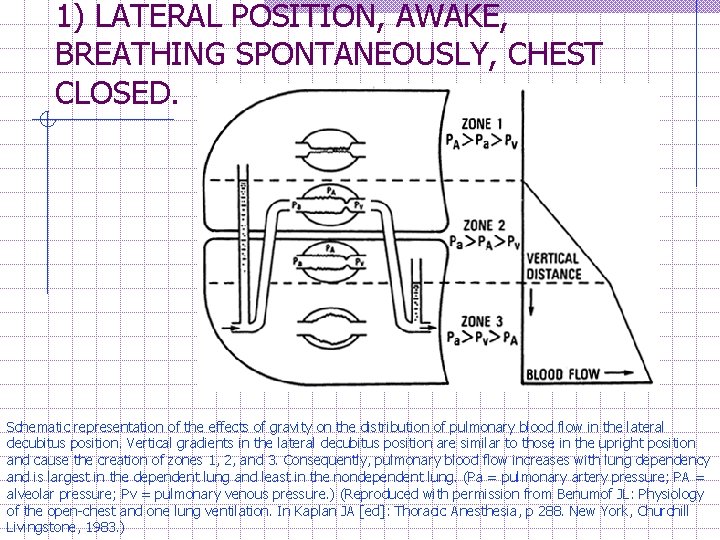
1) LATERAL POSITION, AWAKE, BREATHING SPONTANEOUSLY, CHEST CLOSED. Schematic representation of the effects of gravity on the distribution of pulmonary blood flow in the lateral decubitus position. Vertical gradients in the lateral decubitus position are similar to those in the upright position and cause the creation of zones 1, 2, and 3. Consequently, pulmonary blood flow increases with lung dependency and is largest in the dependent lung and least in the nondependent lung. (Pa = pulmonary artery pressure; PA = alveolar pressure; Pv = pulmonary venous pressure. ) (Reproduced with permission from Benumof JL: Physiology of the open-chest and one lung ventilation. In Kaplan JA [ed]: Thoracic Anesthesia, p 288. New York, Churchill Livingstone, 1983. )

1) LATERAL POSITION, AWAKE, BREATHING SPONTANEOUSLY, CHEST CLOSED. During spontaneous ventilation, the conserved ability of the dependent diaphragm to contract results in an adequate distribution of VT to the dependent lung. Because most of the perfusion is to the dependent lung, the V®/Q® matching in this position is maintained similar to that in the upright position.

2) LATERAL POSITION, AWAKE, BREATHING SPONTANEOUSLY, CHEST OPEN. Controlled positive-pressure ventilation is the most common way to provide adequate ventilation and ensure gas exchange in an open chest situation. Thoracoscopy is performed using intercostal blocks with the patient breathing spontaneously to allow proper lung examination. n The thoracoscope provides an adequate seal of the open chest to prevent a “free” openchest situation.

2) LATERAL POSITION, AWAKE, BREATHING SPONTANEOUSLY, CHEST OPEN. 2 complications can arise from the patient breathing spontaneously with an open chest. 1. Mediastinal shift, usually occurring during inspiration The negative pressure in the intact hemithorax, compared with the less negative pressure of the open hemithorax, can cause the mediastinum to move vertically downward and push into the dependent hemithorax. w The mediastinal shift can create circulatory and reflex changes that may result in a clinical picture similar to that of shock and respiratory distress. w Depending on the severity of the distress, the patient needs to be tracheally intubated immediately, with initiation of positive-pressure ventilation, and the anesthesiologist must be prepared to intubate in this position without disturbing the surgical field.

2) LATERAL POSITION, AWAKE, BREATHING SPONTANEOUSLY, CHEST OPEN. Schematic representation of mediastinal shift in the spontaneously breathing, openchested patient in the lateral decubitus position. During inspiration, negative pressure in the intact hemithorax causes the mediastinum to move downward. During expiration, relative positive pressure in the intact hemithorax causes the mediastinum to move upward. (Reproduced with permission from Tarhan S, Moffitt EA: Principles of thoracic anesthesia. Surg Clin North Am 53: 813, 1973. )
2) LATERAL POSITION, AWAKE, BREATHING SPONTANEOUSLY, CHEST OPEN. 2. Paradoxical breathing. w During inspiration, the relatively negative pressure in the intact hemithorax compared with atmospheric pressure in the open hemithorax can cause movement of air from the nondependent into the dependent lung. w The opposite occurs during expiration. w This gas movement reversal from one lung to the other represents wasted ventilation and can compromise the adequacy of gas exchange. w Increased by a large thoracotomy or by an increase in airways resistance in the dependent lung. w Positive-pressure ventilation or adequate sealing of the open chest eliminates paradoxical breathing.

2) LATERAL POSITION, AWAKE, BREATHING SPONTANEOUSLY, CHEST OPEN. Schematic representation of paradoxical respiration in the spontaneously breathing, openchested patient in the lateral decubitus position. During inspiration, movement of gas from the exposed lung into the intact lung and movement of air from the environment into the open hemithorax cause collapse of the exposed lung. During expiration, the reverse occurs, and the exposed lung expands. (Reproduced with permission from Tarhan S, Moffitt EA: Principles of thoracic anesthesia. Surg Clin North Am 53: 813, 1973. )

3) LATERAL POSITION, ANESTHESIZED, BREATHING SPONTANEOUSLY, CHEST CLOSED. The induction of general anesthesia does not cause significant change distribution of blood flow but has change the distribution of ventilation. Most of the VT enters the nondependent lung, and this results in a significant V®/Q® mismatch. GA causes a reduction in the volumes of both lungs secondary to a reduction in FRC. Any reduction in volume in the dependent lung is of a greater magnitude than that in the nondependent lung for several reasons. n n cephalad displacement of the dependent diaphragm by the abdominal contents is more pronounced and is increased by paralysis. mediastinal structures pressing on the dependent lung or positioning of the dependent side of the operating table prevents the lung from expanding properly.

3) LATERAL POSITION, ANESTHESIZED, BREATHING SPONTANEOUSLY, CHEST CLOSED. Above factor change lungs to a lower volume on the S-shaped volume– pressure curve. n n nondependent lung moves to a steeper position on the compliance curve and receives most of the VT. dependent lung is on the flat (noncompliant) part of the curve.
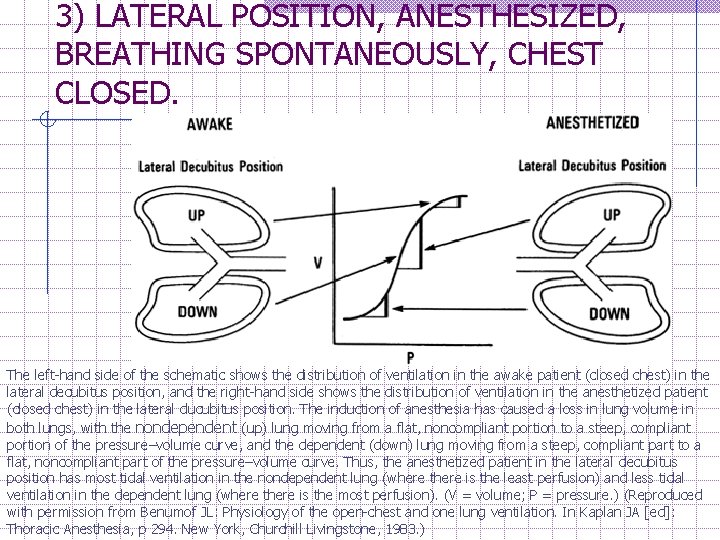
3) LATERAL POSITION, ANESTHESIZED, BREATHING SPONTANEOUSLY, CHEST CLOSED. The left-hand side of the schematic shows the distribution of ventilation in the awake patient (closed chest) in the lateral decubitus position, and the right-hand side shows the distribution of ventilation in the anesthetized patient (closed chest) in the lateral ducubitus position. The induction of anesthesia has caused a loss in lung volume in both lungs, with the nondependent (up) lung moving from a flat, noncompliant portion to a steep, compliant portion of the pressure–volume curve, and the dependent (down) lung moving from a steep, compliant part to a flat, noncompliant part of the pressure–volume curve. Thus, the anesthetized patient in the lateral decubitus position has most tidal ventilation in the nondependent lung (where there is the least perfusion) and less tidal ventilation in the dependent lung (where there is the most perfusion). (V = volume; P = pressure. ) (Reproduced with permission from Benumof JL: Physiology of the open-chest and one lung ventilation. In Kaplan JA [ed]: Thoracic Anesthesia, p 294. New York, Churchill Livingstone, 1983. )

4) LATERAL POSITION, ANESTHESIZED, BREATHING SPONTANEOUSLY, CHEST OPEN. Opening the chest has little impact on the distribution of perfusion. upper lung - no longer restricted by the chest wall & free to expand further increase in V®/Q® mismatch as the nondependent lung is preferentially ventilated owing to a now increased compliance.

5) LATERAL POSITION, ANESTHESIZED, PARALYZED, CHEST OPEN. paralysis and positive-pressure ventilation, n n n diaphragmatic displacement is maximal over the nondependent lung, least amount of resistance to diaphragmatic movement caused by the abdominal contents. This further compromises the ventilation to the dependent lung and increases the V®/Q® mismatch.
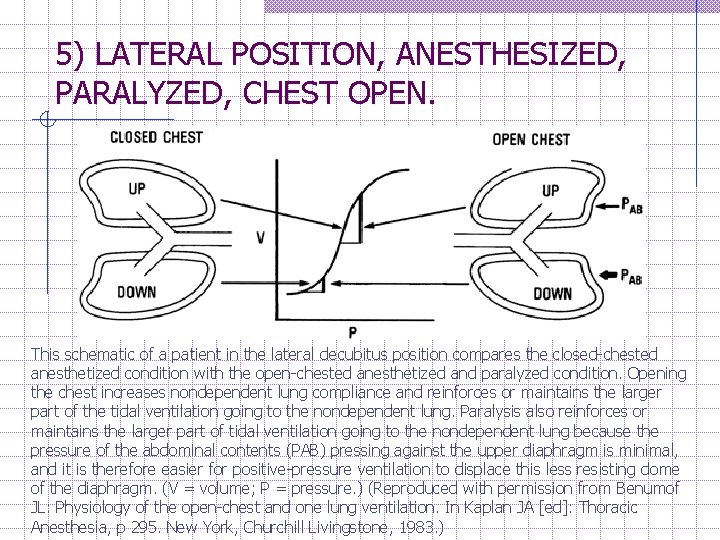
5) LATERAL POSITION, ANESTHESIZED, PARALYZED, CHEST OPEN. This schematic of a patient in the lateral decubitus position compares the closed-chested anesthetized condition with the open-chested anesthetized and paralyzed condition. Opening the chest increases nondependent lung compliance and reinforces or maintains the larger part of the tidal ventilation going to the nondependent lung. Paralysis also reinforces or maintains the larger part of tidal ventilation going to the nondependent lung because the pressure of the abdominal contents (PAB) pressing against the upper diaphragm is minimal, and it is therefore easier for positive-pressure ventilation to displace this less resisting dome of the diaphragm. (V = volume; P = pressure. ) (Reproduced with permission from Benumof JL: Physiology of the open-chest and one lung ventilation. In Kaplan JA [ed]: Thoracic Anesthesia, p 295. New York, Churchill Livingstone, 1983. )

SHUNTING IN TWO LUNG VENTILATION, LATERAL POSITION. During two-lung ventilation in the lateral position, n n mean blood flow to the nondependent lung is assumed to be 40% of cardiac output, 60% of cardiac output goes to the dependent lung. Normally, venous admixture (shunt) in the lateral position is 10% of cardiac output and is equally divided as 5% in each lung. Average percentage of cardiac output participating in gas exchange is 35% in the nondependent lung and 55% in the dependent lung.
6) ONE LUNG VENTILATION, ANESTHESIZED, PARALYZED, CHEST OPEN. Creates an obligatory right-to-left transpulmonary shunt through the nonventilated, nondependent lung because the V®/Q® ratio of that lung is zero. n In theory, additional 35% should be added to the total shunt during one-lung ventilation. Assuming active HPV, blood flow to the nondependent hypoxic lung will be reduced by 50% and therefore is (35/2) = 17. 5%. To this must be added 5%, which is the obligatory shunt through the nondependent lung. n shunt through the nondependent lung is therefore 22. 5% Together with the 5% shunt in the dependent lung, total shunt during one-lung ventilation is 22. 5% + 5 = 27. 5%. This results in a Pa. O 2 of approximately 150 mm Hg (FIO 2 = 1. 0).
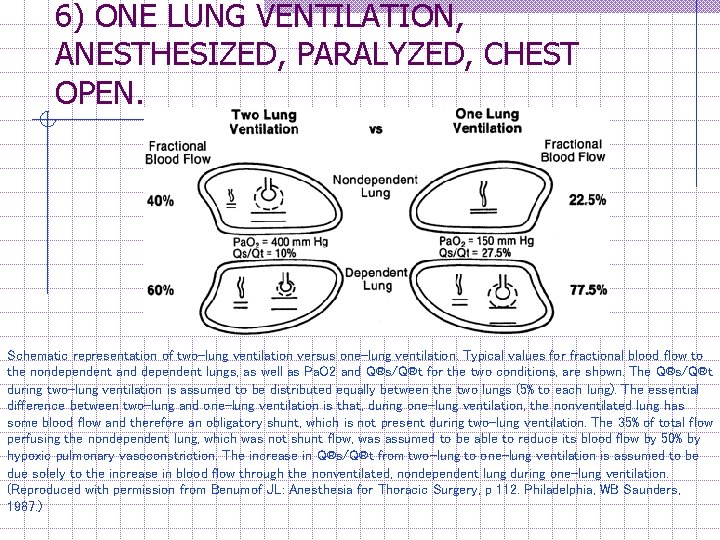
6) ONE LUNG VENTILATION, ANESTHESIZED, PARALYZED, CHEST OPEN. Schematic representation of two-lung ventilation versus one-lung ventilation. Typical values for fractional blood flow to the nondependent and dependent lungs, as well as Pa. O 2 and Q®s/Q®t for the two conditions, are shown. The Q®s/Q®t during two-lung ventilation is assumed to be distributed equally between the two lungs (5% to each lung). The essential difference between two-lung and one-lung ventilation is that, during one-lung ventilation, the nonventilated lung has some blood flow and therefore an obligatory shunt, which is not present during two-lung ventilation. The 35% of total flow perfusing the nondependent lung, which was not shunt flow, was assumed to be able to reduce its blood flow by 50% by hypoxic pulmonary vasoconstriction. The increase in Q®s/Q®t from two-lung to one-lung ventilation is assumed to be due solely to the increase in blood flow through the nonventilated, nondependent lung during one-lung ventilation. (Reproduced with permission from Benumof JL: Anesthesia for Thoracic Surgery, p 112. Philadelphia, WB Saunders, 1987. )
6) ONE LUNG VENTILATION, ANESTHESIZED, PARALYZED, CHEST OPEN. 72. 5% of the perfusion is directed to the dependent lung during one-lung ventilation, the matching of ventilation in this lung is important for adequate gas exchange. The dependent lung is no longer on the steep (compliant) portion of the volume–pressure curve because of reduced lung volume and FRC. There are several reasons for the reduction in FRC; n n n general anesthesia, paralysis, pressure from abdominal contents, compression by the weight of mediastinal structures, suboptimal positioning on the operating table. Other considerations that impair optimal ventilation to the dependent lung; n n n absorption atelectasis, accumulation of secretions, formation of a fluid transudate in the dependent lung. All of these create a low V®/Q® ratio and a large P(A-a)O 2 gradient.

Physiology of OLV A. One lung anesthesia results in a large ventilation perfusion mismatch, secondary to a large right to left intrapulmonary shunt (20 30%).

Physiology of OLV (cont) B. Factors known to inhibit hypoxic pulmonary vasoconstriction include (worsen Rt to Lt Shunt): (1)very high or very low pulmonary artery pressures; (2)hypocapnia; (3)vasodilators; n GTN, Nitroprusside, (B adrenergic agonist)Dobutamine & Salbutamol (4)high or low mixed venous oxygen; (5)pulmonary infection; (6)volatile anesthetics.

Physiology of OLV (cont) C. Factors that decrease blood flow to the ventilated lung: n n high mean airway pressure (high PEEP, hyperventilation, or high peak inspiratory pressures). vasoconstrictors Low FIO 2 intrinsic PEEP(inadequate expiratory times).

Physiology of OLV (cont) D. Carbon dioxide elimination is usually not affected by one lung anesthesia provided minute ventilation is unchanged & preexistin CO 2 retention was not present while ventilating 2 lungs n Arterial CO 2 tension is usually not appreciably altered

Physiology of OLV (cont) Role of hypoxic vasoconstriction in preserving Pa. O 2 (in dogs). Assumptions are shown in insert. Lung is ventilated with Fi. O 2 = 1. 0, while increasing portions of lung are subjected to hypoxia or atelectasis. In the absence of hypoxic pulmonary vasoconstriction, the expected Pa. O 2 would follow the broken line, whereas in the presence of an active hypoxic pulmonary vasoconstriction response, observed Pa. O 2 is maintained close to the solid line. (Pa. O 2 = alveolar PO 2; Pa. O 2 = arterial PO 2. )(Adapted with permission from Marshall BE, Marshall C, Benumof JL et al: Hypoxic pulmonary vasoconstriction in dogs: Effects of lung segment size and alveolar oxygen tension. J Appl Physiol 51: 1543, 1981. )

Methods for separating the lungs Bronchial blockers Fogarty catheter (Arterial Embolectomy Catheter) Endobronchial intubation Univent tube. Double Lumen ET tubes (Carlens and Roberts-Shaw), Bronchocath (PVC)

Bronchial blocker Inflatable devices that are passed alongside or through a single lumen endotracheal tube to selectively occlude a bronchial orifice. An inflatable catheter (Fogarty embolectomy catheter)can be used as a bronchial blocker in conjunction with a regular endotracheal tube (inside or alongside); a guidewire in the catheter is used to facilitate placement. n n Used in the past in children undergoing bronchopulmonary lavage. Inflation of the cuff at the distal end - block ventilation to that lung.

Bronchial Blocker The lumen of the blocker permits suctioning of the airway distal to the catheter tip. Depending on the clinical circumstance, oxygen can be insufflated through the catheter lumen. A conventional endotracheal tube is then placed in the trachea. Bronchial blockers are rarely used in current practice.

Bronchial Blocker (Pro & Cons) Advantages n n Reusable bronchial blocker For selective ventilation in children < 12 y/o. Disadvantages n n n Use a bronchoscope to place the catheter (need skills) Tend to dislodge during manipulation - with disastrous consequences. Blocker balloon requires a high distending pressure, -easily slips out of the bronchus into the trachea, obstructing ventilation and losing the seal between the two lungs.

Fogarty Catheter Achieves the same effect in an adult Similar to bronchial blocker but use of a Fogarty catheter designed for embolectomy procedures. Best performed under direct vision with the aid of a fiberoptic bronchoscope. A conventional ET tube is then placed alongside the catheter after withdrawing the bronchoscope.

Fogarty Catheter Alternatively, the bronchial blocker may be inserted through the lumen of a standard tracheal tube, n n if the rubber diaphragm in a swivel connector is first perforated for passage of the blocker. The swivel connector is then placed between the tracheal tube and the Y piece of the breathing circuit. A fiberscope can be inserted through the lumen of the tracheal tube to facilitate positioning of the blocker under direct vision.

Endobronchial intubation

Univent tube A Single lumen Endotracheal tube with a built in side channel for a retractable bronchial blocker. After intubation of the trachea, the movable blocker is advanced and positioned into the desired mainstem bronchus with the aid of a fiberoptic bronchoscope, then it is inflated. Once the balloon is inflated, the blocked lung can be vented to the atmosphere and allowed to collapse.
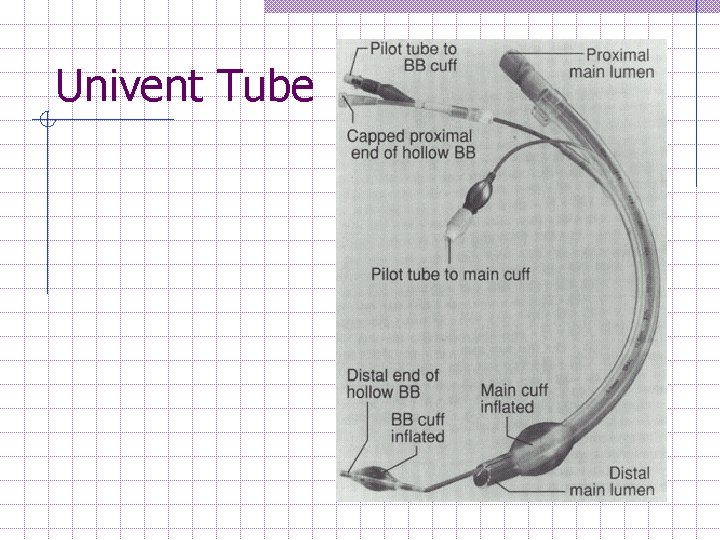
Univent Tube

Univent Tube(Pro & Cons) Advantages n n n Stabilized by the cuff of the ET tube. bronchial blocker is housed in a small channel bored in the endotracheal tube wall. May be ideal for cases in which changing tubes (e. g. , from single- to double-lumen) may be difficult (e. g. , mediastinoscopy followed by thoracotomy), or in cases of bilateral lung transplantion. Disadvantages n n Requires bronchoscopy to actually direct the placement of the blocker. (skills) Correct positioning of the blocker may be difficult to achieve or maintain.

Double Lumen ET tubes (DLT) (Carlens & Roberts-Shaw) Most widely used means of achieving lung separation and one-lung ventilation. Several different types of DLT, n n Carlens (with carinal hook) Robert-Shaw (without carinal hook) w Red Rubber n Bronchocath PVC (similar to Robert Shaw)
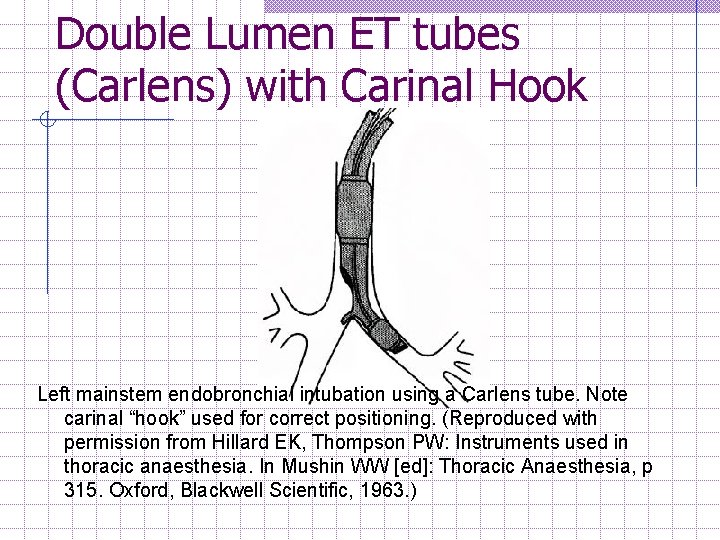
Double Lumen ET tubes (Carlens) with Carinal Hook Left mainstem endobronchial intubation using a Carlens tube. Note carinal “hook” used for correct positioning. (Reproduced with permission from Hillard EK, Thompson PW: Instruments used in thoracic anaesthesia. In Mushin WW [ed]: Thoracic Anaesthesia, p 315. Oxford, Blackwell Scientific, 1963. )

DLT main features Essentially similar in design in that two catheters are bonded together. n 2 Curves: Oropharyngeal, bronchial; n 2 Lumens w 1 st lumen is long enough to reach a mainstem bronchus. w 2 nd lumen ends with an opening in the trachea.

DLT main features Essentially similar in design in that two catheters are bonded together. n 2 Cuffs (bronchial (1 -3 mls), Tracheal (5 -7 mls) w Lung separation is achieved by inflation of two cuffs, the proximal tracheal cuff and the distal bronchial cuff located in the mainstem bronchus. n 2 Sides: Right, Left; w For Right sided DLT have additional ventition slot at bronchial cuff for ventilating the Right Upper Lobe (because the right mainstem bronchus is too short to accommodate both the right lumen tip and a right bronchial cuff).
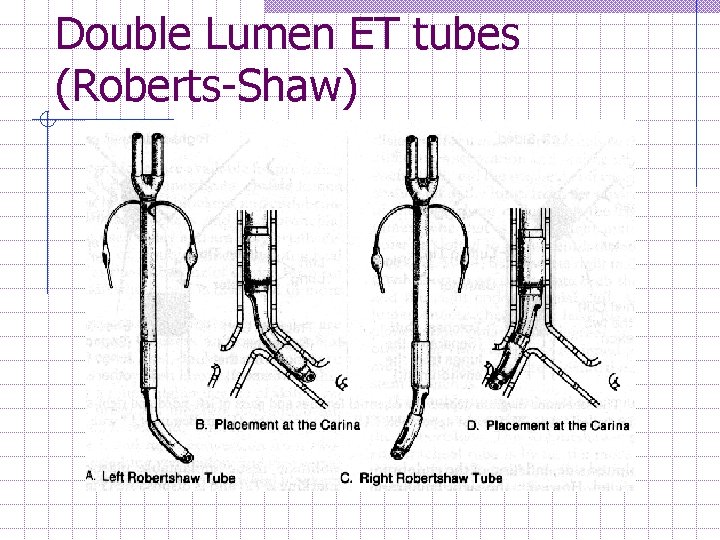
Double Lumen ET tubes (Roberts-Shaw)

Double Lumen ET tubes (Roberts-Shaw) Lt and Rt-sided forms without a carinal hook, (easier insertion) D-shaped, large-diameter lumina w Allow easy suctioning + low resistance to gas flow w Fixed curvature to facilitate proper positioning + reduce the possibility of kinking. Original Red rubber tubes three sizes: (S, M, L) n n For our local population size S & M are used S for Female, M for Males

Double Lumen ET tubes (Roberts-Shaw PVC) Clear PVC Robert Shaw = Bronchocath Disposable. Sizes n n French sizes 35, 37, 39, and 41. Size 28 for pediatric cases. Design n The right-sided endobronchial tube is designed to minimize occlusion of the right upper lobe. w The right endobronchial cuff is doughnut shaped and allows the right upper lobe ventilation slot to ride over the right upper lobe orifice.

Double Lumen ET tubes (Roberts-Shaw PVC) sizes Size ranges from 28 41 Fr. n n Left sided Robertshaw types are the most common used The choice or size of DLT is usually basedon the patients height (37 Fr most common for women) (39 Fr most common for men) Patient height Tube size Depth of insertion n 136 164 cm 37 Fr 27 cm 165 179 cm 39 Fr 29 cm 180 194 cm 41 Fr 31 cm

DLTs (Roberts-Shaw) types Original Red rubber vs Clear, PVC (Bronchocath) n n n Reusable tubes Less cost Although the red rubber tubes may be more difficult to insert, they are less likely to dislocate during patient positioning and surgical manipulation. Durable tracheal cuff rubs against the patient's upper teeth. If these teeth are prominent and sharp, as compared with the thicker-walled cuffs of the red rubber tubes. Can withstand repeated sterilization. n n n Disposable More Expansive Easy to insert, positioning and to dislocate. the thin-walled tracheal cuffs of the disposable tubes are much more likely to tear If Wrong size of tube is used (insertion is attempted) - tube cannot be reused because sterility is compromised

DLTs (Roberts-Shaw) types Original Red rubber vs Clear, PVC (Bronchocath) n n No color differentiation of endobronchial cuffs Radiolucent, no radioopaque line. Red/yellow color tube – gas exchange not visible. Foreign body reaction not suitable for long term used. n n n easy recognition of the blue colored endobronchial cuff when FOB is used. confirmation of position on CXR (radioopaque lines) Clear PVC easy for cont observation of tidal gas exchange and of respiratory moisture. Suitable for use in long-term ventilation in the intensive care unit (a high-volume lowpressure cuff. ) Tubes of choice nowadays for lung separation and OLV.

Choices of DLT Left Sided – mostly used n n Because of probs with proper positioning of Right sided DLT in ensuring that Rt upper lobe is well ventilated (more difficult) If clamping of Lt main bronchus is necessary (Lt Pneumonectomy) w DLT cuffs are deflated and withdrawn in the trachea w Tracheal Cuffs reinflated so that both lument ventilating the Right lung. Left Sided DLT contraindicated only if; n Left main bronchus stenosed, distorted or infiltrated by tumour.

Size of DLT Correct SIZE for patient is Very Important Too Small n n fail to provide adequate lung isolation Will require large endobronchial volume or pressure that could damage the bronchus Too LARGE n Can rupture the trachea or bronchus It is important to test for leaks around the bronchus n The bronchial cuff should be inflated to the minimal Volume that provide lung isolation. w (Minimal Leaking Technique)

Positioning of DLT Steps for insertion A. Preliminary steps; n prepare and check tube lubricate tube Established patient monitors. Pre Oxygenate patient for 3 – 5 minutes Induce with I/v Fentanyl, STP, Scoline

Positioning of DLT Steps for insertion B. Intubation; 1. 2. 3. 4. 5. Laryngoscopy is performed once pt is adequately anesthesized. insert tube with distal concave curvature tip facing anteriorly. remove stylet once through the vocal cords rotate tube 90 degrees (in direction of desired lung) advancement of tube ceases when resistance is encountered. Average lip line is 29 + 2 cm.

Positioning of DLT Steps for insertion B. Intubation; 6. 7. 8. If a carinal hook is present (carlens DLT), must watch hook go through cords to avoid trauma to them. insert tube with distal concave curvature facing anteriorly, and remove stylet once through the vocal cords. (As step 2 – 3) Then in step 4, rotate 180 degrees (so distal concavity faces posteriorly and hook is anterior). Once hook is past cords, rotate so that distal concavity is pointed right or left as desired. Connect to the breathing circuits.

Positioning of DLT

Placement checking of DLT Cuff inflation and checking for placement by auscultation Checking tube placement with the fiberoptic bronchoscope

Placement checking of DLT C. Checking by Auscultation 1. Inflate tracheal cuff (high volume, lowpressure, capacity 20 m. L max)- expect equal lung ventilation (same as regular ETT). w w 2. 3. Both lungs should expands and BS should equal bilaterally. This indicates the DLT is in the trachea not in esophagus. If BBS not equal, probably too far down (tracheal lumen opening is at carina or even endobronchial). Withdrawal by 2 -3 cm fixes this. Inflate bronchial cuff and ventilate. w w Both lungs should expand & BS should equal Bilaterally This indicate the bronchial cuff is not over inflated as to occlude the bronchial lumen.

Placement checking of DLT C. Checking by Auscultation (cont) 4. Disconnect the tracheal tube (Rt tube of Lt DLT) and clamp the right side w w 5. Disconnect the bronchial tube (left tube in the Lt. Sided DLT) & Clamp the Left Side. w n Only the left lung should expand Listen to the disconnected tube to detect air leak Only the right lung should expand. Note: if Lung isolation needs to be achieved urgently to prevent soiling of the unaffected lung (eg. Empyema of Bleeding into the lung) the Bronchial cuff should be inflated FIRST before the above steps are taken.

Placement checking of DLT Cuff inflation and checking for placement by auscultation

Placement checking of DLT C. Checking by Auscultation (Minimal Leaking Technique) 1. 2. Inflate tracheal cuff (high volume, lowpressure, capacity 20 m. L max)- expect equal lung ventilation (same as regular ETT). If BBS not equal, probably too far down (tracheal lumen opening is at carina or even endobronchial). Withdrawal by 2 -3 cm fixes this. Clamp the right side (marked "tracheal" for leftsided tube) and remove cap from the right connector. Expect some left sided ventilation through bronchial lumen, and some air leak past bronchial cuff, which is not yet inflated.

Placement checking of DLT C. Checking by Auscultation (Minimal Leaking Technique) 3. 4. 5. Slowly inflate bronchial cuff until minimal or no leak is heard at uncapped right connector. Go slow- it only requires 1 -3 cc of gas and bronchial rupture is a risk (using this minimal-leak technique guards against this). Remove the clamp and replace the cap on the right. Check that both lungs are ventilated. This ensures that the bronchial cuff is not partially or completely obstructing the contralateral hemithorax. Selectively clamp each side, and expect visible chest movement and audible breath sounds only on the right when left is clamped, and vice versa.

Placement checking of DLT C. Checking by Auscultation Note: w w w if PIP is 20 cm water with two-lung ventilation, it should not exceed 40 cm water with OLV If separation is absolutely critical (bronchopulmonary lavage), check using an underwater seal. With deflated bronchial cuff, air escapes around it when the bronchial side is ventilated, and this can be heard as it exits the tracheal lumen. If the tracheal lumen is connected to a tube which is led underwater, gas can be seen to bubble up out of the tube. Place the end of the tube 50 cm below the surface of the water, and inflate/position until no leak is obtained to ensure absolute lung separation.
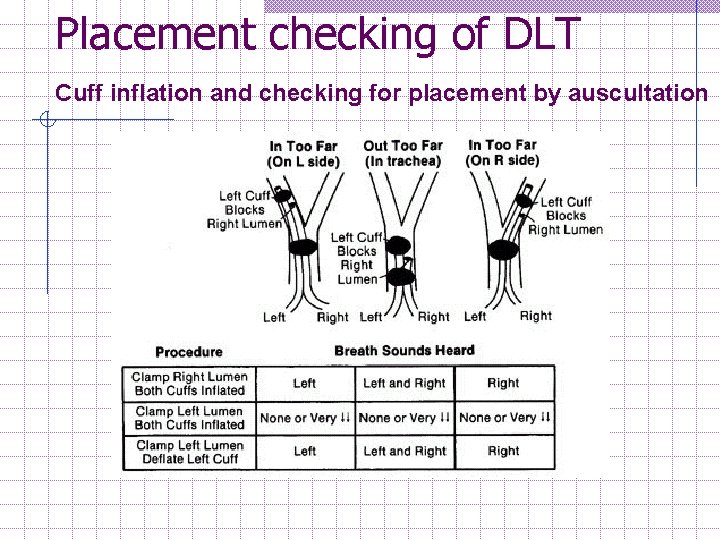
Placement checking of DLT Cuff inflation and checking for placement by auscultation

Several possibilities of DLT malposition: 1. The bronchial lumen enters the wrong side. Consequences; wrong lung collapse, inadequate separation, increased PIP, instability of the DLT, tracheal or bronchial laceration, obstruction of RUL bronchus by left sided tube bronchial cuff. 2. Too far down. BS will not be heard on contralateral side since tracheal lumen may be endobronchial.

Several possibilities of DLT malposition: (cont) 3. Too shallow. BS good bilateral through bronchial lumen, inaudible through tracheal lumen (inflated bronchial cuff obstructs gas flow through tracheal lumen). Deflate cuff(s) and rotate/advance bronchial tube into desired side.

Several possibilities of DLT malposition: (cont) 4. R sided tube may obstruct RUL bronchus. Mean distance from carina to origin of RUL bronchus is 2. 5 cm. Margin of error is small therefore R sided DLTs are harder to position accurately and keep in place during positioning and surgical manipulation. Normally choose a tube with the bronchial lumen on the non operated (dependent) side. properly positioned left sided DLT can be used for operations on either hemithorax. During L pneumonectomy, it may be withdrawn when the surgeon needs to clamp and suture the L main bronchial stump.

Several possibilities of DLT malposition: 5. LUL bronchus (mean distance 5 cm from carina) may occasionally be obstructed by L DLT bronchial cuff. 6. Bronchial cuff herniation may obstruct ventilation on its own side, or herniate over the carina and obstruct contralateral ventilation. 7. Rare complication is Tracheal rupture w use minimal-leak technique to inflate tracheal cuff Bronchial rupture (don't over-inflate, be sure positioned correctly, avoid intraoperative dislocation [if absolute separation of the lungs not needed, deflate during repositioning]).

Placement checking of DLT Checking tube placement with the fiberoptic bronchoscope (FOB) D. Confirmation of DLT position n n Proper positioning is best performed with fibreoptic bronchoscope (FOB) The FOB is passed down the trachea lumen first. w Clear straight-ahead view of the carina w The left tube going to the left side w Upper surface of the left endobronchial cuff just below the carina. n n The FOB the is passed to bronchial lumen to determine whethere is any cuff herniation partially occluding the endobronchial lumen. The DLT is reposition if necessary.

Placement checking of DLT Checking tube placement with the fiberoptic bronchoscope Several situations exist where auscultation is impossible n n (patient is prepped and draped), or when they do not provide reliable information (preexisting lung disease so that BS are not very audible, or if the tube is only slightly malpositioned). The double-lumen tube's precise position can be most reliably determined with the fiberoptic bronchoscope. Smith, Hirsch & Ehrenwerth (Anesth Analg 1986; 65: S 1) n showed that in patients with double-lumen tubes whose position seemed appropriate to ausculation, 48% had some degree of malposition. So always check position with fiberoptic.
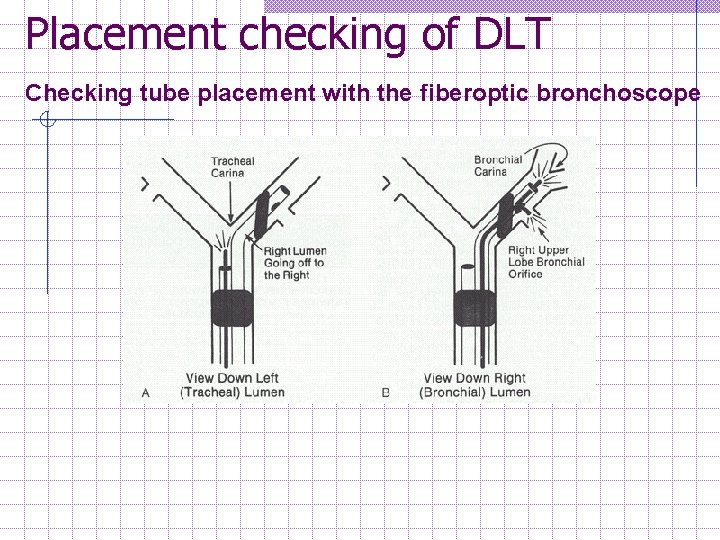
Placement checking of DLT Checking tube placement with the fiberoptic bronchoscope
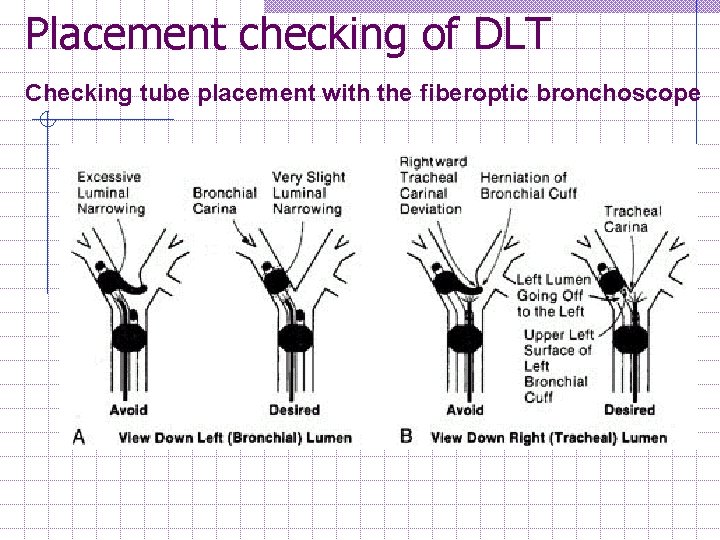
Placement checking of DLT Checking tube placement with the fiberoptic bronchoscope

After Position Checking & Confirmation by FOB The DLT is Anchored and securely tapes. Recheck by means of auscultation and /or Fibre. Optic Bronchoscope after positioning patient laterally.

Contraindications of doublelumen tubes Carinal or proximal bronchial mainstem lesions Full stomach Small patients Difficult upper airway anatomy Critically ill (ie can't break PEEP)

Complications of double-lumen tubes Traumatic larnygitis Tracheobronchial tree disruption especially overinflated bronchial cuff.

Management of OLV 1. Maintain two-lung ventilation until pleura is opened (or as long as possible) w Because the OLV have greatest risk of hypoxaemia. 2. Vent settings for the dependent lung on OLV: FIO 2 1. 0 VT 10 m. L/kg n n n If peak Airway Pr rise excessively >30 cm H 20 Tv have to be reduce to 6 -10 ml/kg & RR to maintain same Minute Ventilation Closed Sp. O 2 monitoring is Mandatory RR adjustred to desired p. ETCO 2 (~3040 mm. Hg) PEEP 0 -5 cm H 2 O to the dependent lung

Management of OLV (cont) 3. Check ABG baseline (room air) and 15 -20 min after instituting OLV. n FIO 2 can continue to decrease for 45 minutes after OLV instituted. 4. If severe hypoxemia occurs: w w Ruled out the possible cause disconnection, circuit, malfunctioning of unidirectional valves, etc. Increase Fi. O 2 to 1. 0 (if not done yet) supplement anaesthesia with narcotic analgesic & volatile agent Check position of DLT n n w By auscultation of dependent lung and if any adv sound. Direct visualisation with FOB (if available) Suction DLT to clear secretion Rule out cuff probs by inflating and deflating the cuff. Check hemodynamic status n n Correct hypovolaemia and hypotension if present. Sent ABG

Management of OLV (cont) 4. If severe hypoxemia occurs (cont); w Non-dependent lung CPAP 5 -10 cm. H 2 O, the single most effective intervention. Add CPAP 10 cm water after a non-dependent lung inflation. (require separete O 2 source and Pr Gauge to determine the amount of CPAP applied. ) w The diagram shows a commercially-available CPAP setup. The same thing can be achieved with a Mapleson D pediatric circuit and an auxiliary oxygen flowmeter. (During thoracoscopy, CPAP is usually not possible as it obstructs the surgeon. ) w Apply PEEP to Dependent lung start with 5 cm. H 2 O can be increase to 10 cm. H 2 O if CVS status no compromised.
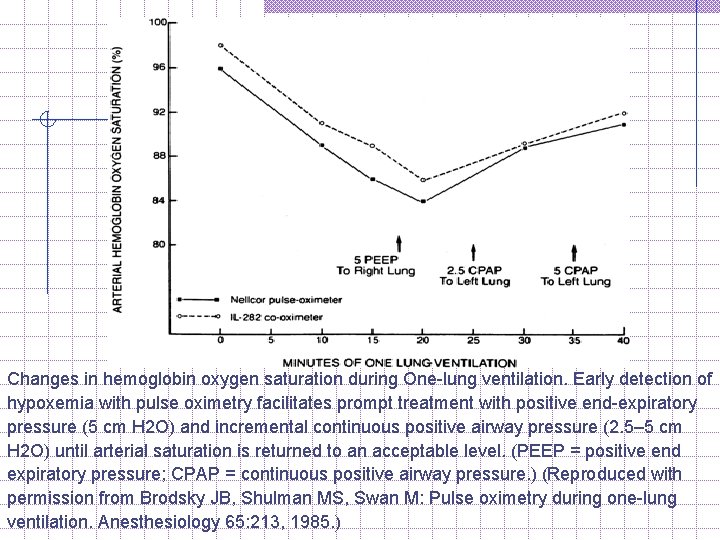
Changes in hemoglobin oxygen saturation during One lung ventilation. Early detection of hypoxemia with pulse oximetry facilitates prompt treatment with positive end expiratory pressure (5 cm H 2 O) and incremental continuous positive airway pressure (2. 5– 5 cm H 2 O) until arterial saturation is returned to an acceptable level. (PEEP = positive end expiratory pressure; CPAP = continuous positive airway pressure. ) (Reproduced with permission from Brodsky JB, Shulman MS, Swan M: Pulse oximetry during one lung ventilation. Anesthesiology 65: 213, 1985. )

Management of OLV (cont) 4. If severe hypoxemia occurs (cont); w Recheck patient; s oxygenation and haemodynamic parameters. n n n Inform surgeon if pt oxygenation not good Resume 2 lungs ventilation till Sp. O 2 improve Intermittent two-lung ventilation w Clamp pulmonary artery ASAP (if pneumonectomy) n Eliminates the shunting of blood to non ventilated lung causing hypoxaemia.

Management of OLV (cont) If hypoxemia occurs…. (cont) Consistent effective measures n n n Periodic inflation of collapse lung wih O 2 Early ligation or clamping of the ipsilateral Pulm. Art. (during Pneumonectory) 5 -10 cm H 2 O of CPAP to the collapse lung; most effective when there is partial reexpansion of the lung (can interfere the surgery). Marginally effective measures; n n n 5 – 10 cm. H 2 O of PEEP to the ventilated lung Continous insufflation of O 2 into the collapse lung Changing the Tv and RR

Management of OLV (cont) If persistent hypoxemia …. (cont) n n Require reexpansion of collapse lung Endobronchial tube / blocker can change with positioning & surgical manipulation or traction w n Frequent suction of both lumen is essential. w n Repeat FOB through the tracheal lumen can quickly exclude this problem. If Blood present in the airway, instillation of 3 – 5 ml Sod Bicarb. May help facilitate the removal of clots. Pneumothorax on the dependent, ventilated side should also be considered – like to occur following extensive mediastinal dissection or with high peak insp pr.
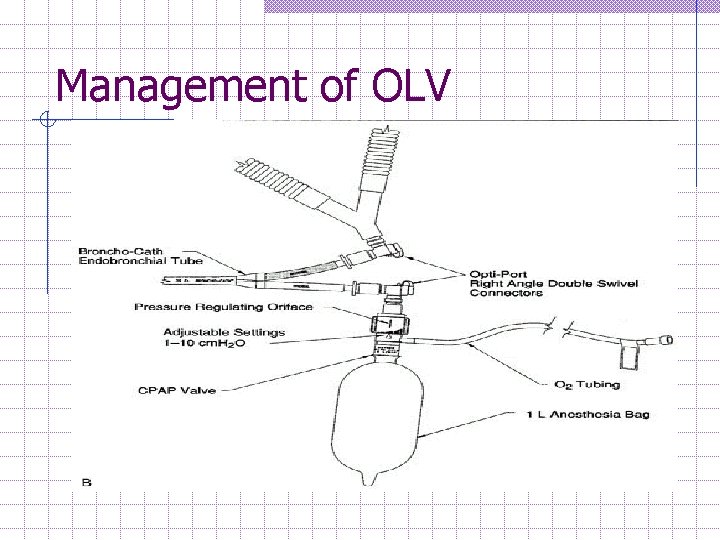
Management of OLV
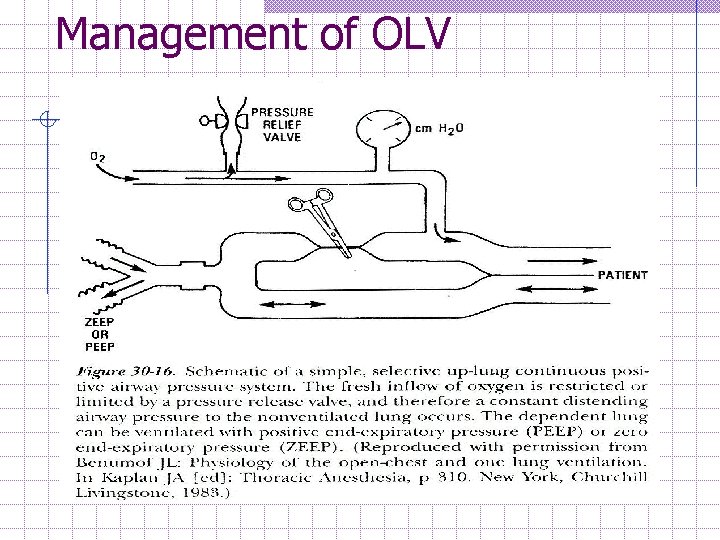
Management of OLV

Post Operative Management ICU Admission at least overnight n n Ventilatory support / not ? decision Close monitoring Post op analgesia Care of drainage (intercostal) n Post pneumonectomy drainage – depends on surgeon (controversial!) Post pneumonectomy pulmonary Edema Early Active Chest Physiotherapy, BE, Early ambulation

Post Operative Management ICU Admission at least overnight n Ventilatory support / not depends on; w Perioperative status of patient w Length & extent of OP w Any Intraop Complication w Patient recovery characteristic

Post Operative Management ICU Admission at least overnight n Closed monitoring in ICU w CVS; BP, CVP, Pulse w RESP; adequate ventilation, ABG w Temperature; Radiant warmer, blanket w Fluid balance: Urine output w Serum electrolytes w Hb, HCT, to be tranfuse if HCT <30% w CXR w 12 leads ECG

Post Operative Management Post op analgesia w IV inf. narcotics analgesic eg. morphine w Thoracic epidural inf. 0. 1% Bupivacaine +2 ug/ml fentanyl w PCA w S/C morphine w Intercostal block under direct vision at chest closure w Interpleural block at the end of surgery; w Wound infiltration of the skin

Post Operative Management Care of drainage (intercostal) n Make sure drain functioning and patent w Confirm drainage position by CXR n Note amount & nature of fluids drained out w To Inform surgeon if fluid consist of large amt of fresh blood n Post pneumonectomy instercostal drainage insertion – w depends on surgeon (controversial!) w Suctioning intercostal drain is contraindicated n Tracheal position is checked before extubation, w Injection / aspiration of air to the operated side to keep mediastinum in midline or slightly to the operated side.

Post Operative Management Post pneumonectomy pulmonary Edema n n n n 2 - 4% of cases more frequent in r pneumonectomy Sx begin 48 -72 hr after OP CXR 1 st detected before onset of Sx Mortality rate is high >50% Histologically similar to ARDS Multifactorial causes Patient should be fluid restricted w Total positive fluid balance not more than 20 ml/kg in 1 st 24 hr – diuretic may be given

Post Operative Management Post pneumonectomy pulmonary Edema n Multifactorial causes w Fluid overload w Abnormal lymphatic drainage w Increase capillary permeability w Right ventricular dysfunction (some of the mech proposed

Post Operative Management Watch out of other Complications; n RESP insufficiency – w sputum retention Atelectesis, Resp distress / failure n CVS insufficiency – w Hypotension, dysrrhytmias, pericarditis, cardiac failure w MI, heart herniation through open pericardium into pleural cavity Haemorrhage n Empyema n

Post Operative Management Watch out of other Complications; n Excessive fluid accumulation in chest cavity post pneumonectomy causes w hypovolaemia, resp distress, mediastinal shift Post pneumonectomy bronchopleural fistula d/t dehiscence of bronchial stump n Others n w Renal failure, pulmonary infarction, w spinal cord ischaemia, paraplegia

THANK YOU

1. 2. 3. 4. 5. 6. References C. Y. Lee. Manual Of Anaesthesia for Medical Officers. : 253 -255, 1996 G. Edward Morgan, Jr. , Maged S. Mikhail, Michael J. Murray. Clinical Anaesthesiology 3 rd Edition. : 528 -539, 2002. Lippincot’s Interactive Anaesthesia Library On CD-ROM V. 3. 0: James B. Eissenkraft, Edmond Cohen, & Steven M. Neustein; Anesthesia For Thoracic Surgery. : Chapter 30 Slinger P, et al. Arterial oxygenation during one-lung ventilation. A comparison of enflurane and isoflurane. Anesthesiology 82(4): 940946, 1995. ANESTHESIA FOR LUNG RESECTION Article from Department of Anesthesia and Critical Care, at The University of Chicago. July 24, 1996 P. Allan Klock, M. D. , Michael O'Connor, M. D. ANE 551 Advanced Principles (Rev Summer 2004) Anesthesia For Thoracic Surgery. UNIVERSITY OF DETROIT MERCY GRADUATE PROGRAM OF NURSE ANESTHESIOLOGY
- Slides: 113