Third Trimester Bleeding Preterm labor and Premature rupture

Third Trimester Bleeding, Preterm labor, and Premature rupture of membranes Melissa Zahnd, APN, CNP, CDE Maternal Fetal Medicine

Third Trimester Bleeding

Definition • Bleeding/Spotting in pregnancy during the 3 rd Trimester-28 weeks and beyond

Etiologies • Placenta Previa • Placental Abruption • Vasa previa • Bloody show (PTL) • Cervicitis • Genital lacerations/Trauma • Foreign Body • Genital Lacerations/Trauma • Foreign Body • Cervical/Vaginal Cancer

Evaluation • VS • Labs (anemia/DIC) • KB • RH status • Fetal evaluation • US • Confirm placental location • Avoid digital exam

Placental Abruption • Placenta separates from uterine wall • 1: 100 births • 30% of cases (TTB) • 25% recurrence risk • Risk factors: Hypertension Cocaine use Abdominal trauma Sudden uterine decompression (PROM) • PROM • •
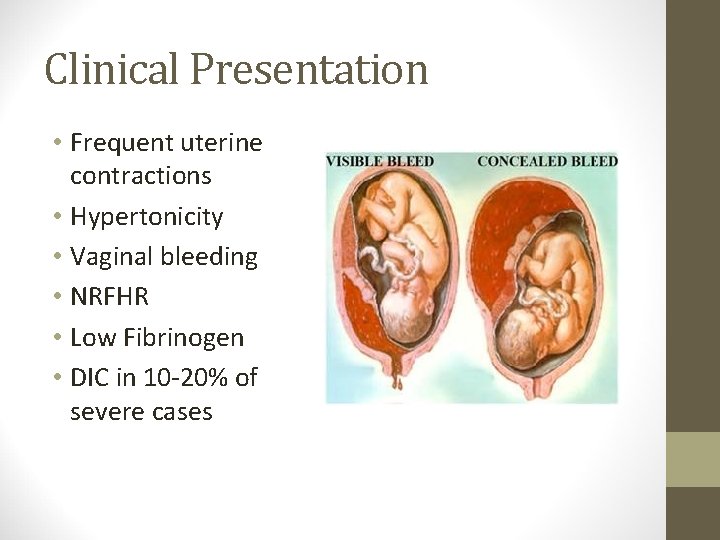
Clinical Presentation • Frequent uterine contractions • Hypertonicity • Vaginal bleeding • NRFHR • Low Fibrinogen • DIC in 10 -20% of severe cases
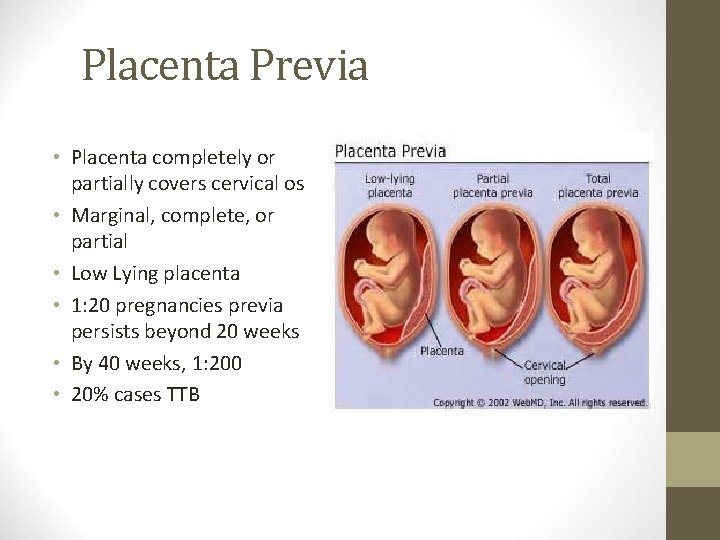
Placenta Previa • Placenta completely or partially covers cervical os • Marginal, complete, or partial • Low Lying placenta • 1: 20 pregnancies previa persists beyond 20 weeks • By 40 weeks, 1: 200 • 20% cases TTB

Risk factors • Prior C/S • History of myomectomy • D&C, repetitive • Multiples • Increased parity • AMA • Smoking

Symptoms • Painless vaginal bleeding • Vasa Previa • Fetal vessels of velamentous cord insertion covering os • Multiple gestations

Treatment • Delivery • Volume replacement • Monitor blood/coagulation • Indications for Transfusion • Acute blood loss 3050% • Chronic blood loss hgb <6, or <10 with comorbidities • Abnormal coagluation studies • • Fibrinogen <150 Prolonged PTT Platelets <20, 000 Platelets <50, 000 + C/S

Preterm Labor

Diagnosis • Regular contractions and cervical change-dilation, effacement, or both or initial presentation of regular contractions and cervical dilation of at least 2 cm between 20 weeks 0 days and 36 weeks 6 days.

Risk Factors • Prior History of PTB • African American • Low Pre-pregnancy BMI • Preterm contractions • PROM • Incompetent cervix • Short cx on US • Infections • Urinary • BV • Intra-Amniotic • Excessive uterine size • Uterine Distortion • Myomas • Septate, Didelphis • Placental abnormalities

Risk Factors • Maternal Smoking (PROM) • Substance abuse • Inflammation (oral) • Decidual hemorrhage • Pathologic uterine distention

Symptoms • Menstrual like cramps • Low, dull backache • Abdominal pressure • Pelvic Pressure • Abdominal cramping (w/wo diarrhea) • Increase or change in vaginal discharge • Uterine contractions • Sometimes painless

Evaluation • Fetal status • Maternal status • Rule out other possible etiologies • Labs • UA/Culture • Vaginal cultures/wet mount • Assessment of cervix • US • Fetal Fibronectin

Treatment • Underlying cause • Treat Infections • BV • Nifedipine • Terbutaline • Indomethacin • Steroids • Magnesium • NICU consult

Preterm Rupture of Membranes

Definition • Premature ROM: Amniorrhexis (SROM) Prior to the onset of labor at any gestation (PROM) • Preterm ROM: PROM prior to 37 weeks gestation • Use PPROM/PROM

Definitions • Latency Period: time interval between ROM and onset of labor • Expectant management: management of patients with the goal of prolonging gestation (“watchful waiting” until delivery indication arises)
Incidence-Preterm ROM • Complicates up to 3. 5% of all pregnancies • 30 -40% of Preterm births • PPROM ~25% cases of all PROM Garite (2007), Santaloya-Forgas et al. , (2007), Svigos, Robinson, et Vigneswaran, 2007)

Risk Factors • Chorioamnionitis • Vaginal infections • Cervical abnormalities • Vascular pathology (incl. abruptio) • Smoking • 1 st, 2 nd, 3 rd, or multiple trimester bleeding • Previous preterm delivery (PPROM) • AA ethnicity • Acquired or congenital connective tissue disorder • Nutritional deficiencies (Vit. C, copper, zinc)

The Patient • Vaginal discharge • Gush of fluid • Leaking of fluid • Oligo/Anhydramnios • Cramping • Contractions • Back pain

Diagnosis • Sterile Speculum exam (Pooling) • SSE-Free flow of fluid from cervical os • Nitrizine testing • Microscopic Fern testing • Fetal Fibronectin • Amni. Sure • Ultrasonography • Transabdominal Indigo dye injection

Why not do a digital vaginal exam? • Latency period • Infection
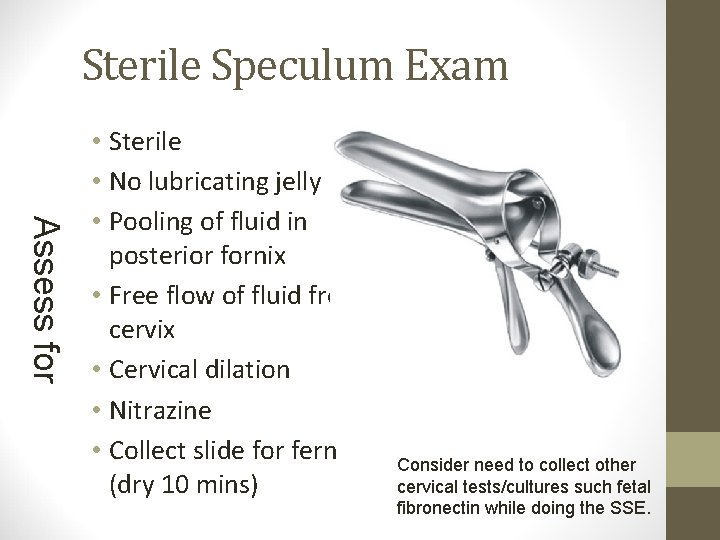
Sterile Speculum Exam Assess for • Sterile • No lubricating jelly • Pooling of fluid in posterior fornix • Free flow of fluid from cervix • Cervical dilation • Nitrazine • Collect slide for fern (dry 10 mins) Consider need to collect other cervical tests/cultures such fetal fibronectin while doing the SSE.

Nitrazine paper testing • Vaginal p. H (3. 5 -4. 5) • Turns blue in presence of alkaline Amniotic fluid • 93. 3% sensitivity • False positive (1 -17%) for urine, blood, semen, BV, Trichomonas
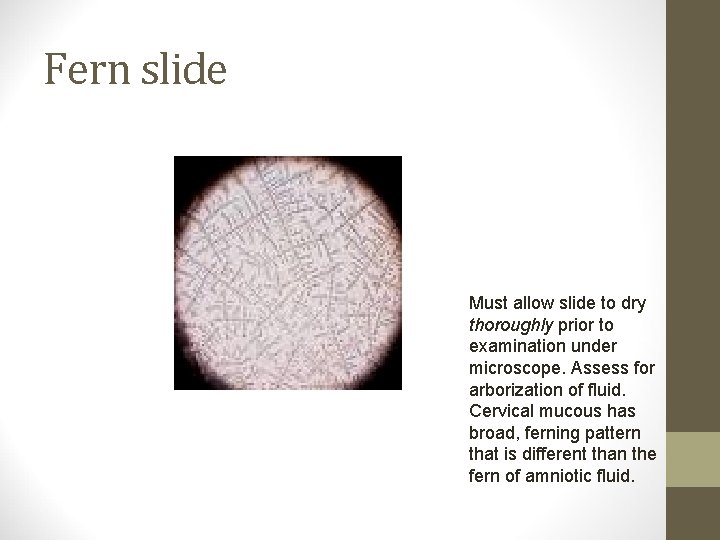
Fern slide Must allow slide to dry thoroughly prior to examination under microscope. Assess for arborization of fluid. Cervical mucous has broad, ferning pattern that is different than the fern of amniotic fluid.

Amni. Sure • • • Newer test Point of Care test Cost-up to $50 each Sensitivity-98. 7 -98. 9% Specificity-87. 5 -100% Awaiting further testing prior to recommendations
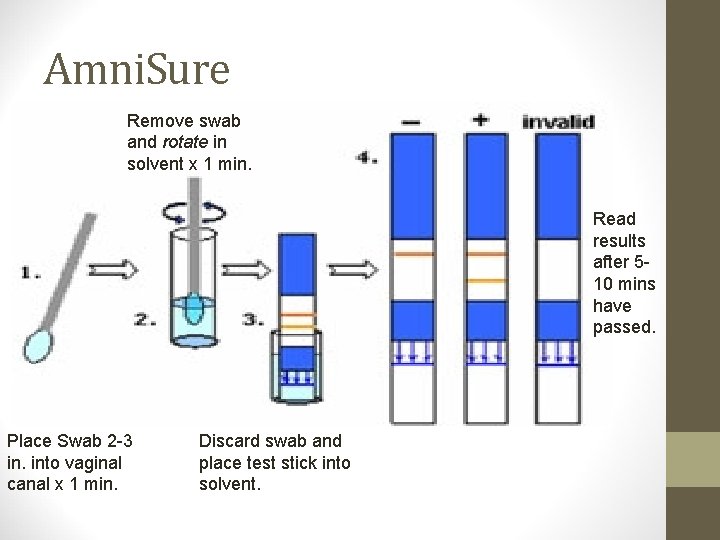
Amni. Sure Remove swab and rotate in solvent x 1 min. Read results after 510 mins have passed. Place Swab 2 -3 in. into vaginal canal x 1 min. Discard swab and place test stick into solvent.
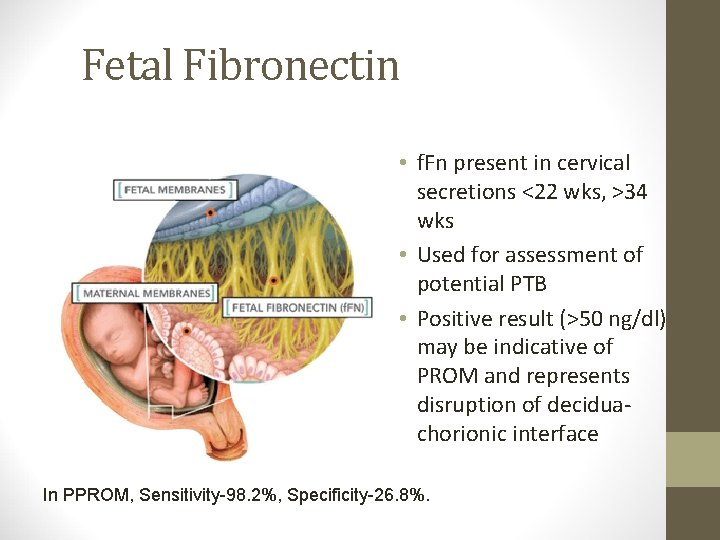
Fetal Fibronectin • f. Fn present in cervical secretions <22 wks, >34 wks • Used for assessment of potential PTB • Positive result (>50 ng/dl) may be indicative of PROM and represents disruption of deciduachorionic interface In PPROM, Sensitivity-98. 2%, Specificity-26. 8%.
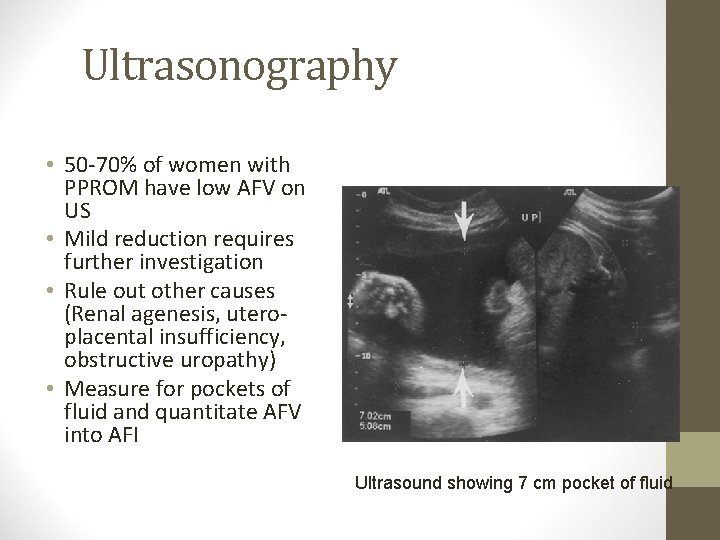
Ultrasonography • 50 -70% of women with PPROM have low AFV on US • Mild reduction requires further investigation • Rule out other causes (Renal agenesis, uteroplacental insufficiency, obstructive uropathy) • Measure for pockets of fluid and quantitate AFV into AFI Ultrasound showing 7 cm pocket of fluid
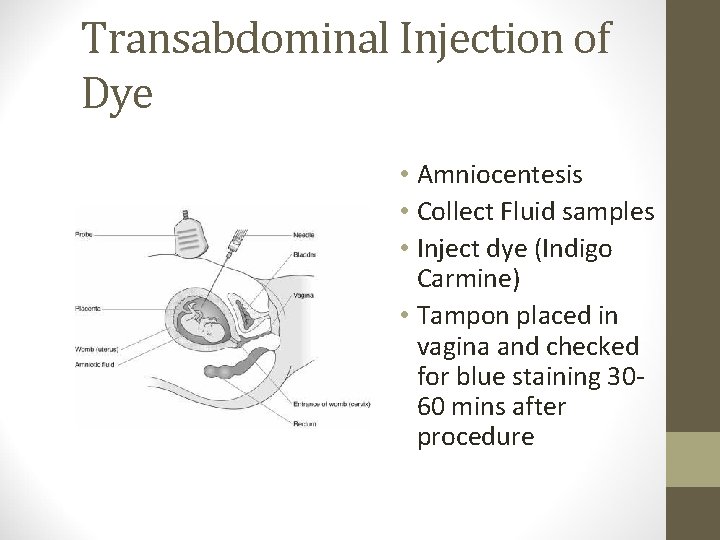
Transabdominal Injection of Dye • Amniocentesis • Collect Fluid samples • Inject dye (Indigo Carmine) • Tampon placed in vagina and checked for blue staining 3060 mins after procedure

How would I manage this patient? • Gestational age • Availability of NICU • Fetal presentation • FHR pattern • Active distress (maternal/fetal) • Is she in labor? • Cervical assessment
Delivery Indication • Maternal-Fetal Distress • Infection • Abruption • Cord Prolapse

Expectant Management • • Typical for GA 32 weeks or less (32 weeks, document FLM) Steroids Tocolysis if indicated for lung maturity Antibiotics (Ampicillin/EES-Azithro) Fetal Surveillance Majority Inpatient Observation Assess for Chorioamnionitis Goal: Mature Lung Profile, reduction of PTB risks!

Expectant Management Risks • Abruption • Chorioamnionitis • Cord Prolapse • Pulmonary Hypoplasia (<19 weeks PPROM • Skeletal Deformities • Endometritis (1/3) Benefits • Mature lung profile • Advancing GA (reducing risks associated with PTB)

Risks-Benefits Profile of Pre-term Birth Risks • Assoc. w/ PTB • NEC • IVH/CP • RDS • Cesarean Delivery • Endometritis (1/3) Benefits • Elimination of risks of expectant management

Outcomes • 1/3 develop intraamniotic infections, endometritis, or septicemia • Neonatal outcomes dependent on GA and indication for delivery

References • Duff, Patrick, MD. “Preterm premature rupture of membranes. ” Up. To. Date. Ed. Charles J Lockwood, MD and Vanessa A Barss, MD. 116. 27 June 2008 <http: //utdol. com>. • Garite, Thomas J, MD. “Premature Rupture of the Membranes. ” Clinics in Perinatalogy. N. p. : n. p. , n. d. 723 -736. • Hacker, and Moore. Essentials of Obstetrics and Gynecology. 4 th ed. N. p. : n. p. , 2004. • Santolaya-Forgas, Joaquin, et al. “Prelabor rupture of the membranes. ” Clinical Obstetrics-Handbook: The Fetus and Mother. By E Albert Reece and John Hobbins. N. p. : n. p. , 2007. 1130 -1173. • Svigos, John Micheal, Jeffrey S Robinson, and Rasniah Vigneswaran. “Prelabor Rupture of Membranes. ” High-Risk Pregnancy. N. p. : n. p. , n. d. 1321 -1330.
- Slides: 42