Thick Thin Blood Smear Blood Examination The most

Thick & Thin Blood Smear

Blood Examination • The most commonly used technique for blood examination is stained blood films. • Geimsa stain is usually used to stain the films. • Delafild’s haematoxylin stain is used for microfilariae. • Either thick or thin films may be used depending on the circumstances. • The thick film is more sensitive in detecting parasite and also saves time in examination. • The thin film technique cause very little distortion of the parasite, and permits species identification when it may not be possible in thick films, but many fields must be examined to detect parasite when they are few in number. Raed Z. Ahmed, Medical Parasitology Lab. , 2012

Continue ……… • Therefore, both thick and thin films must always be prepared when searching for plasmodia and trypanosomes. • If a precise identification can not be made from thick film, the thin film will be available. • Thick films should be used when searching for microfilariae. • The most economical use of slides is achieved by making a combination thick and thin slide. • However, combination films must dry thoroughly 8 -10 hrs. to overnight before they can be satisfactorily stained. • Slides for malaria should be stained in the same day. Raed Z. Ahmed, Medical Parasitology Lab. , 2012

Continue ……… • The thin films will dry quickly and can be stained as soon as they are dry, and examine for parasites. • If parasites are not seen in the thin film, stain the thick film using Field’s stain, and examine for parasites. • Direct wet mounts of fresh whole blood (or centrifuged blood) are usually used for detection of microfilariae and trypanosomes, this only gives evidence of infection and stained films are necessary for confirmation of species present. • In areas where malaria, trypanosomes, and/or microfilariae may all present, both wet and stained films should be prepared and examined. • If neither trypanosomes nor microfilariae occur in region, only stained smears need to be made for detection of plasmodia. Raed Z. Ahmed, Medical Parasitology Lab. , 2012

Examination of Thick & Thin blood smear • For optimum staining, the thick and thin films should be made on separate slides and different concentrations used for staining. • When it’s done good quality staining of thick film is of primary importance, best results are obtained if the blood smear have dried overnight. • Fixation of thin blood film done by adding 3 drops of methanol, or dipping it in a container of methanol for few seconds, with prolonged fixation it may be difficult to demonstrate Schuffner’s dots and Maurer’s dots. • To permit dehemoglobinization, thick film should not be fixed; therefore avoid exposure to methanol or methanol vapor Raed Z. Ahmed, Medical Parasitology Lab. , 2012

Reading of Thick Film • Focus on film with 10 x objective and search for microfilariae. They are easily detected with 10 x objective. • If microfilariae are present, switch to oil- immersion objective and identify the species. • Also, look for malaria parasites with oil- immersion objective, at least 100 fields should be examined. • Microscopy of thick film should reveal the following features: 1. The background should be clean, free from debris, with a pale mottled- gray color derived from the lysed erythrocytes. 2. Leukocyte nuclei are stained a deep, rich purple. 3. Malaria parasite are well defined with deep- red chromatin and pale purplish blue cytoplasm. Raed Z. Ahmed, Medical Parasitology Lab. , 2012

Reading of Thin Film • Focus with the 10 x objective on the thin terminal end of the film where the RBCs are in one layer, put oil drop on the slide and switch to the oilimmersion objective. • When examining fro malaria parasites and trypanosomes, at least 200 fields should be examined. • Microscopy of thin film should reveal the following features: 1. The background should be clean and free from debris; erythrocytes are stained a pale greyish pink. 2. Neutrophil leukocytes have deep purple nuclei and well defined granules. 3. Malaria parasite are well defined with deep- red chromatin and pale purplish blue cytoplasm. 4. Like plasmodia, the cytoplasm of trypanosomes stain blue, the nucleus and kinetoplast stain red or purple. Raed Z. Ahmed, Medical Parasitology Lab. , 2012

Identification of malarial parasites • In thin films, look at the appearance of the parasite and the appearance of the RBCs containing the parasites. 1. The appearance of the parasites 2. The appearance of the RBC containing the parasites: § Size: Is the parasitized cell the same size as the blood cell without parasite or Is it enlarged? § Stippling: Is the RBC filled with pink or red staining dots? • Schuffner’s stippling in the “ghost” of the erythrocyte can some times be seen at the edges of the film and indicate infection with Plasmodium vivax or P. ovale, . • Maurer’s dots show as stippling in erythrocytes containing the larger ring forms of Plasmodium falciparum. Raed Z. Ahmed, Medical Parasitology Lab. , 2012
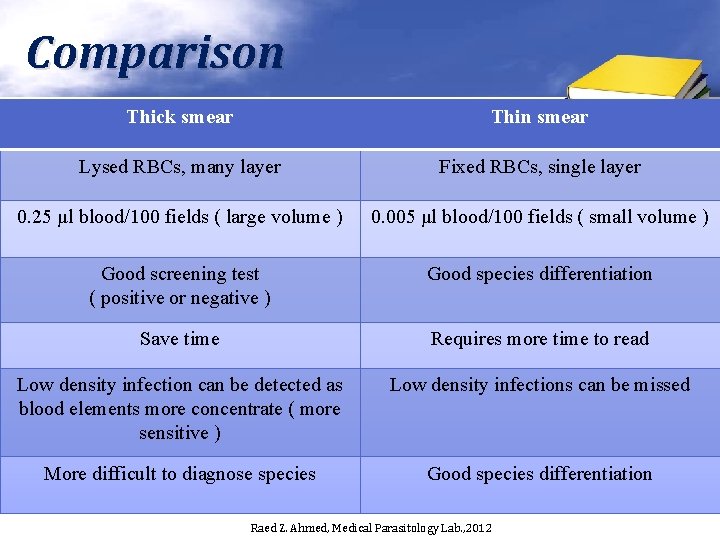

Comparison Thick smear Thin smear Lysed RBCs, many layer Fixed RBCs, single layer 0. 25 μl blood/100 fields ( large volume ) 0. 005 μl blood/100 fields ( small volume ) Good screening test ( positive or negative ) Good species differentiation Save time Requires more time to read Low density infection can be detected as blood elements more concentrate ( more sensitive ) Low density infections can be missed More difficult to diagnose species Good species differentiation Raed Z. Ahmed, Medical Parasitology Lab. , 2012

Blood Parasites Raed Z. Ahmed, Medical Parasitology Lab. , 2012
Blood Protozoa Microfilariae Trypanosoma Plasmodium falciparum Blood Parasite Leishmania Plasmodium vivax Plasmodium ovale Plasmodium malariae Raed Z. Ahmed, Medical Parasitology Lab. , 2012

Blood Parasites Trypanosoma spp. Raed Z. Ahmed, Medical Parasitology Lab. , 2012
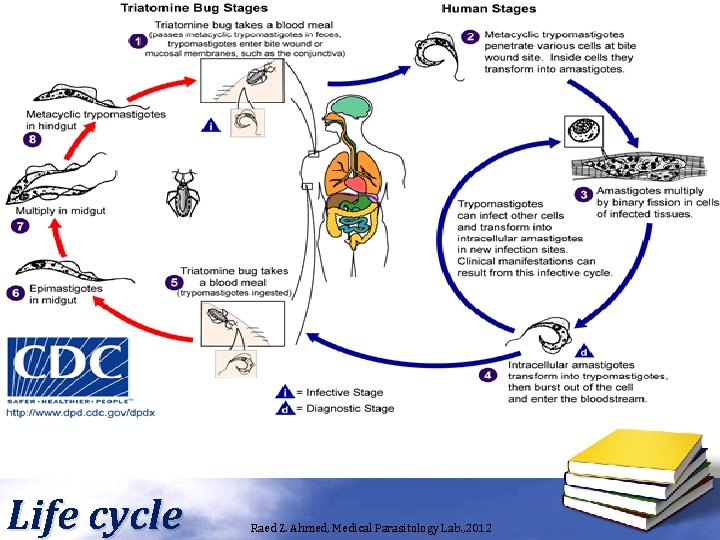
Life cycle Raed Z. Ahmed, Medical Parasitology Lab. , 2012

Trypanosoma spp. • Trypanosoma cruci (Americans) cause Chaga’s disease. • Trypanosoma bruci (Africans) cause sleeping sickness disease. • Trypanosoma have many stages: – Amastigote, Promastigote, Epimastigote and Trypomastigote. • Reservoir host: mammalian animal. • Intermediate host: Tse tse fly (Glossina spp. ) • Definitive host: Human. • Infective stage: Metacyclic trypomastigote. • Diagnostic stage: Trypomastigote. Raed Z. Ahmed, Medical Parasitology Lab. , 2012
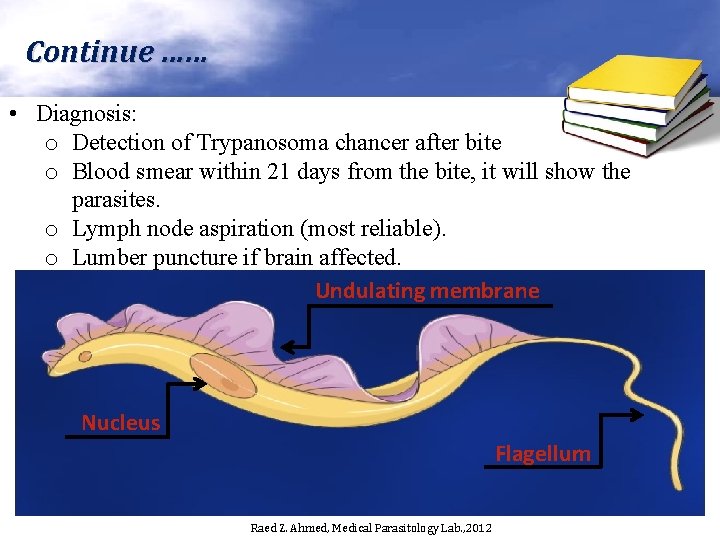
Continue …… • Diagnosis: o Detection of Trypanosoma chancer after bite o Blood smear within 21 days from the bite, it will show the parasites. o Lymph node aspiration (most reliable). o Lumber puncture if brain affected. Undulating membrane Nucleus Flagellum Raed Z. Ahmed, Medical Parasitology Lab. , 2012
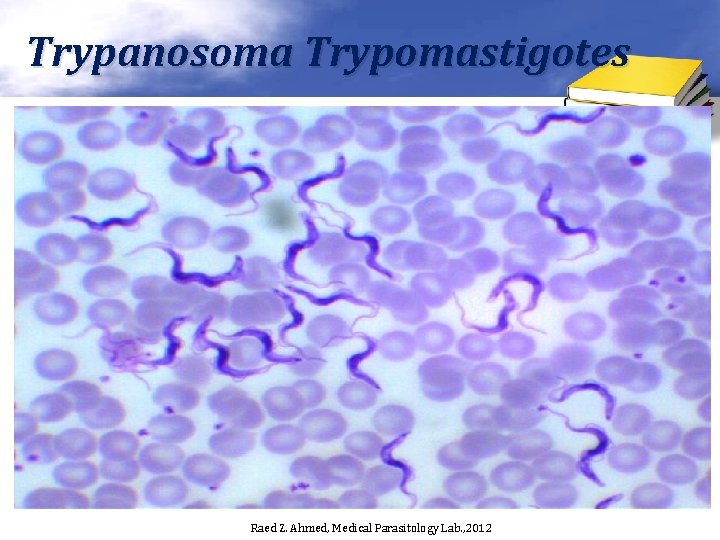
Trypanosoma Trypomastigotes Raed Z. Ahmed, Medical Parasitology Lab. , 2012

Blood Parasites Leishmania spp. Raed Z. Ahmed, Medical Parasitology Lab. , 2012
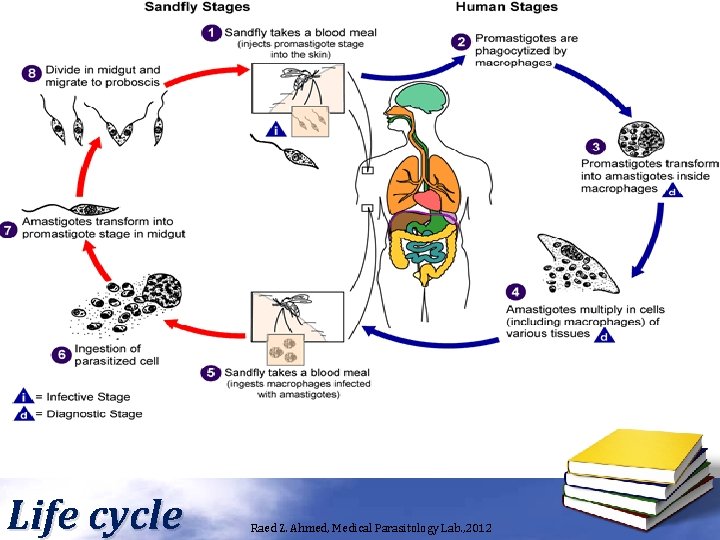
Life cycle Raed Z. Ahmed, Medical Parasitology Lab. , 2012

Leishmania spp. • There is many species affect man: – Leishmania tropica : cause skin lesion ( cutaneous ) – Leishmania braziliense : cause muco-cutaneous lesion. – Leishmania donovani : cause visceral lesion. • Leishmania have two stages: – Amastigote (Leishmania stage), in man (reticuloendothelial cell). – Promastigote (Leptomonas stage), the infective stage and present in the lumen gut of the sand fly. • Reservoir host: dogs and rodents. • Intermediate host: Sand fly (Phlebotomus). • Definitive host: Human. Raed Z. Ahmed, Medical Parasitology Lab. , 2012
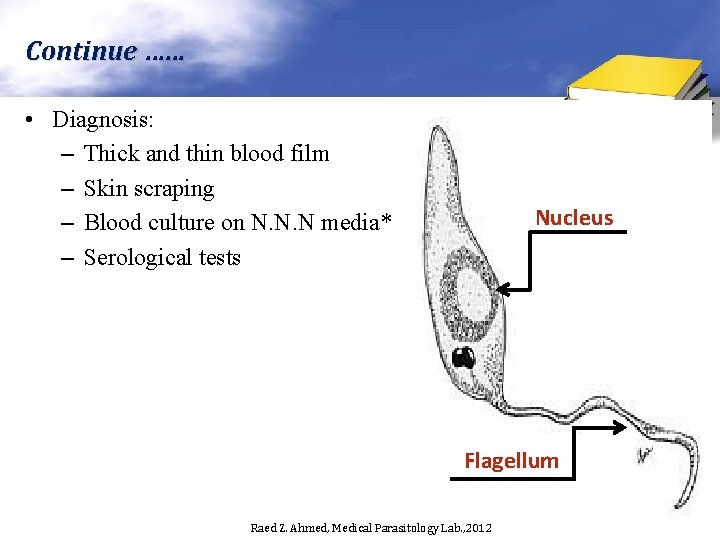
Continue …… • Diagnosis: – Thick and thin blood film – Skin scraping – Blood culture on N. N. N media* – Serological tests Nucleus Flagellum Raed Z. Ahmed, Medical Parasitology Lab. , 2012
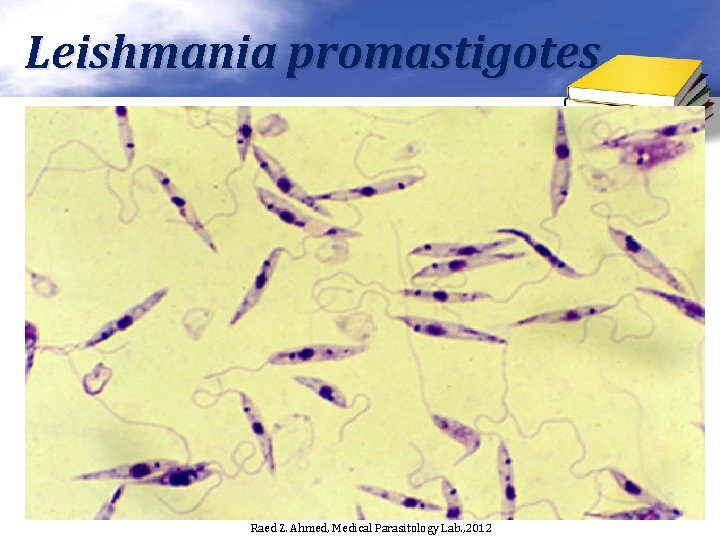
Leishmania promastigotes Raed Z. Ahmed, Medical Parasitology Lab. , 2012

Blood Parasites Plasmodium spp. Raed Z. Ahmed, Medical Parasitology Lab. , 2012
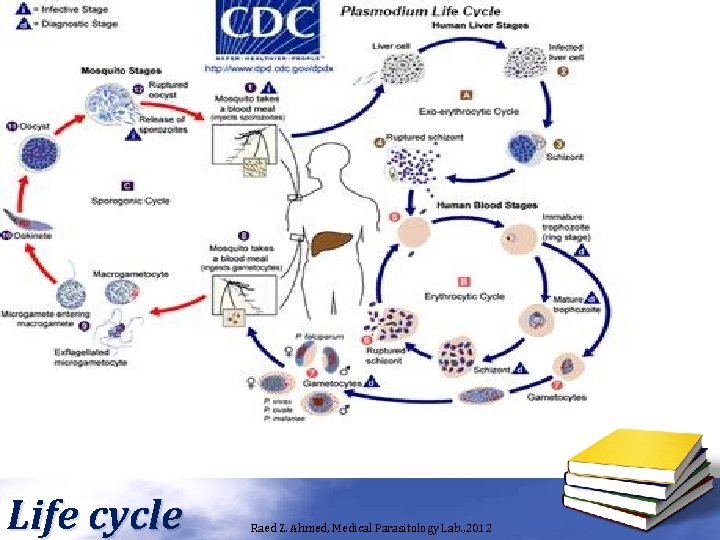
Life cycle Raed Z. Ahmed, Medical Parasitology Lab. , 2012

Plasmodium spp. • Four species of Plasmodium are the causative agent of malaria, these are: – P. vivax, P. malariae, P. falciparum, and P. ovale. • Intermediate host: Human. • Definitive host: Anopheles mosquitoes. • Plasmodium spp. have 4 stages: – Ring form (young trophozoite. ) – Late ( old ) trophozoite – Schizonts – Gametocyte. • Infective stage: Sporozoites. • Diagnosis: – Thick and stained thin blood film to detect parasites. Raed Z. Ahmed, Medical Parasitology Lab. , 2012
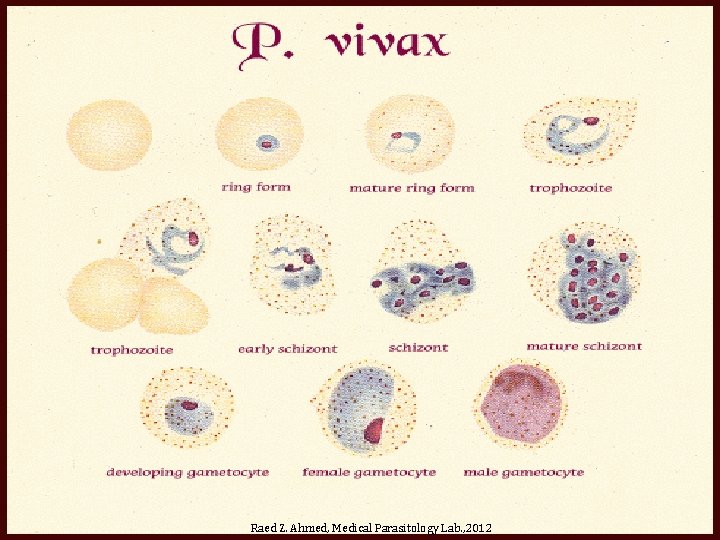
Raed Z. Ahmed, Medical Parasitology Lab. , 2012
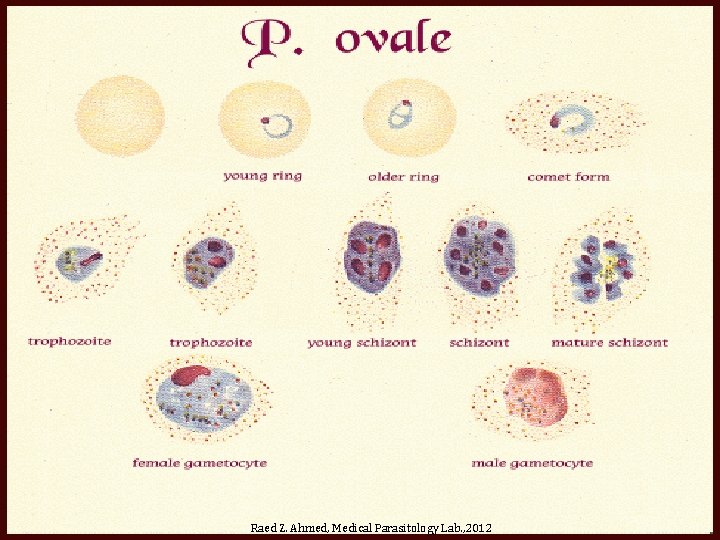
Raed Z. Ahmed, Medical Parasitology Lab. , 2012
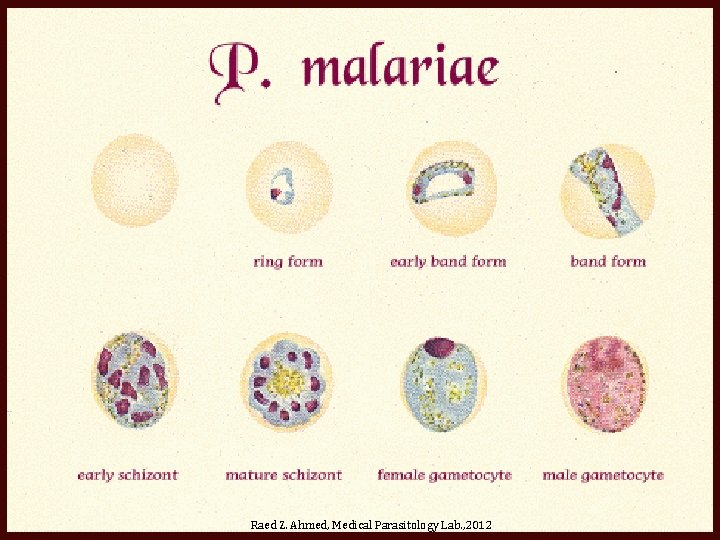
Raed Z. Ahmed, Medical Parasitology Lab. , 2012
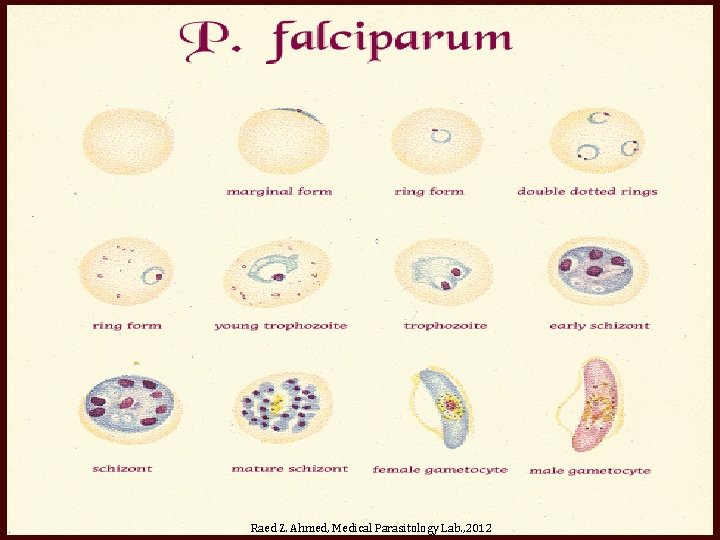
Raed Z. Ahmed, Medical Parasitology Lab. , 2012
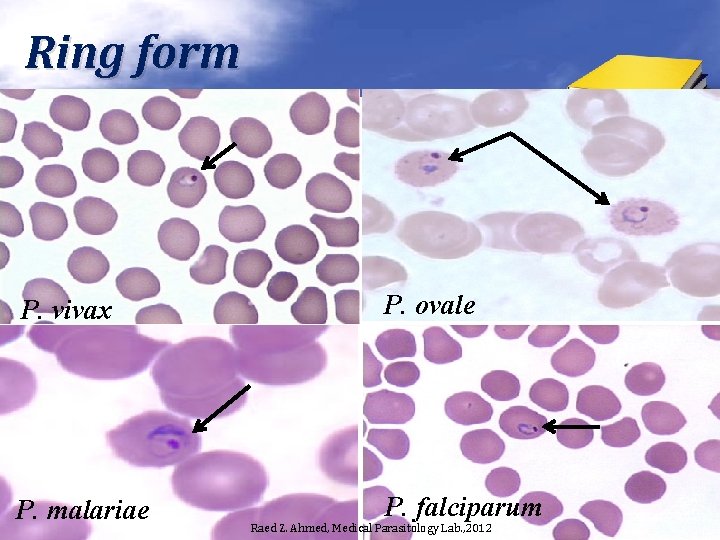
Ring form P. vivax P. ovale P. malariae P. falciparum Raed Z. Ahmed, Medical Parasitology Lab. , 2012
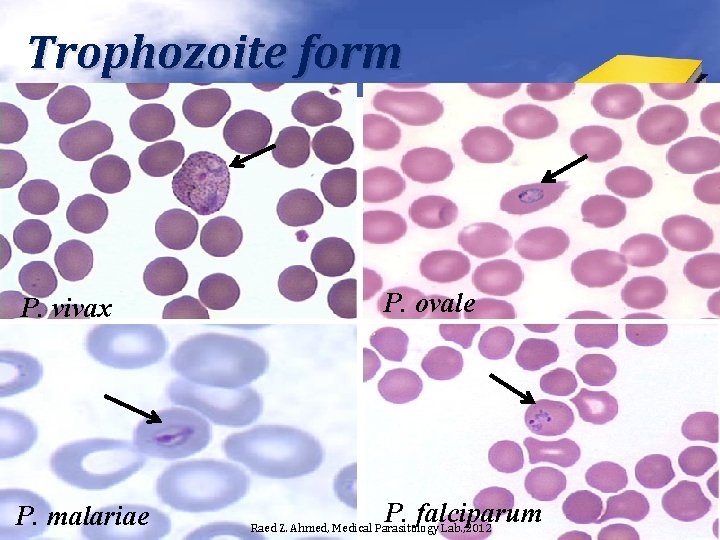
Trophozoite form P. vivax P. malariae P. ovale P. falciparum Raed Z. Ahmed, Medical Parasitology Lab. , 2012
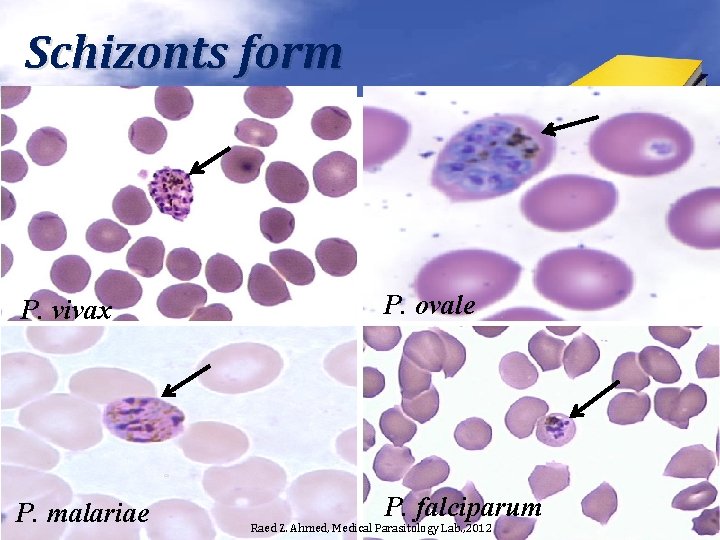
Schizonts form P. vivax P. ovale P. malariae P. falciparum Raed Z. Ahmed, Medical Parasitology Lab. , 2012
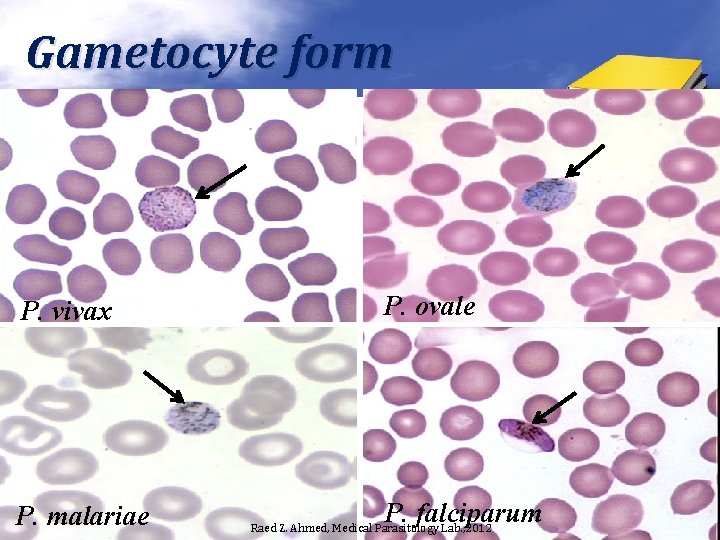
Gametocyte form P. vivax P. malariae P. ovale P. falciparum Raed Z. Ahmed, Medical Parasitology Lab. , 2012
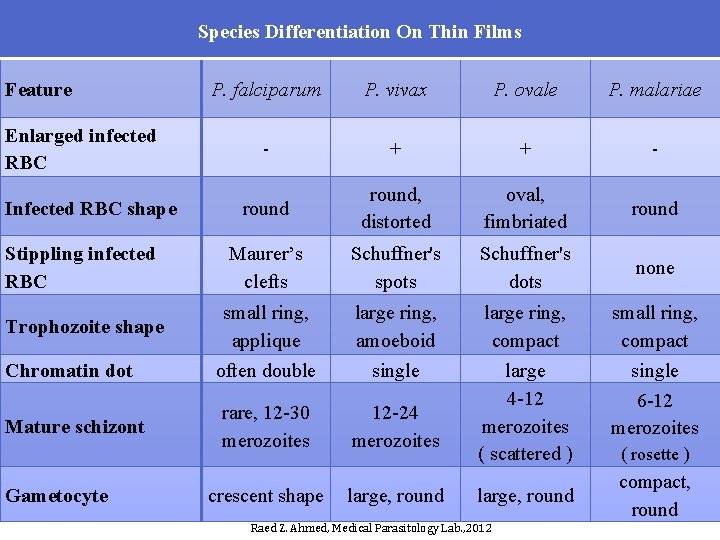
Species Differentiation On Thin Films Feature P. falciparum P. vivax P. ovale P. malariae - + + - round, distorted oval, fimbriated round Stippling infected RBC Maurer’s clefts Schuffner's spots Schuffner's dots none Trophozoite shape small ring, applique large ring, amoeboid large ring, compact small ring, compact often double single rare, 12 -30 merozoites 12 -24 merozoites large 4 -12 merozoites ( scattered ) single 6 -12 merozoites crescent shape large, round Enlarged infected RBC Infected RBC shape Chromatin dot Mature schizont Gametocyte large, round Raed Z. Ahmed, Medical Parasitology Lab. , 2012 ( rosette ) compact, round
- Slides: 33