Thibodaux Using Six Sigma to Reduce Pressure Ulcers
Thibodaux Using Six Sigma to Reduce Pressure Ulcers Thibodaux Regional Medical Center Darcy Prejeant & Sheri Eschete August 20, 2007

What has contributed to our n Ongoing Leadership success? n Allocating Full Time Resources to PI n Involving Physicians n Having Process Owners Own Their Projects

Making a Commitment
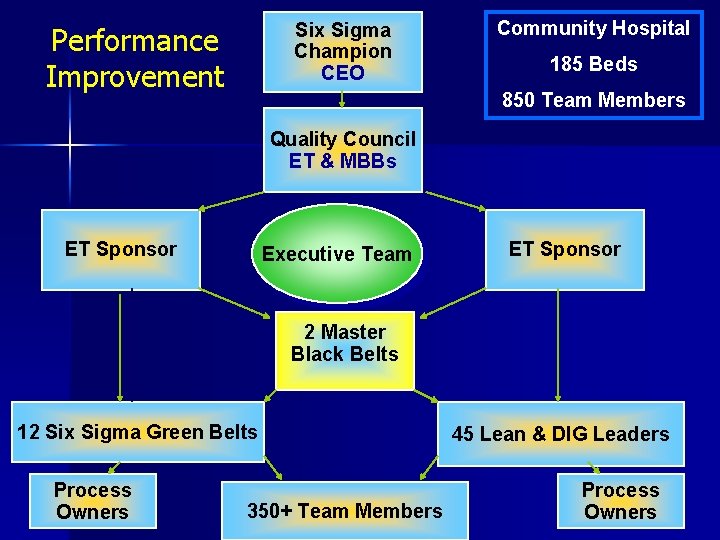
Six Sigma Champion CEO Performance Improvement Community Hospital 185 Beds 850 Team Members Quality Council ET & MBBs ET Sponsor Executive Team ET Sponsor 2 Master Black Belts 12 Six Sigma Green Belts Process Owners 350+ Team Members 45 Lean & DIG Leaders Process Owners

Master Black Belts n Keeping PI Alive – Train new Leaders – Organize projects – Assist in deploying projects – Serve as a resource – Assist Process Owner to monitor success – Report to Executive Team

Physician Paradigm Shift Physician Involvement n “TRMC administration has been doing it right… we need to learn from them. ” n This has opened the door to engage physicians

Process Owners Now Own Their Project n Has primary responsibility for the outcome of the process n Implement the solutions identified n Continue to monitor and evaluate results to achieve or exceed goal n Communicate continual progress to Master Black Belts n Give final report outs

“The Skin Savers” Title: Nosocomial Pressure Ulcers Pillar: Quality Project Description/Scope: § CQI data suggests an increase in nosocomial pressure ulcers on in-patient units (MS 2 & 3, ICU, SDU, and Rehab). § Includes in-patients with length of stay >72 hrs. Goal: Eliminate nosocomial Stage 3 and Stage 4 pressure ulcers and reduce Stage 2 pressure ulcers from 4. 0 to <1. 6 skin breaks/1000 patient days per quarter.
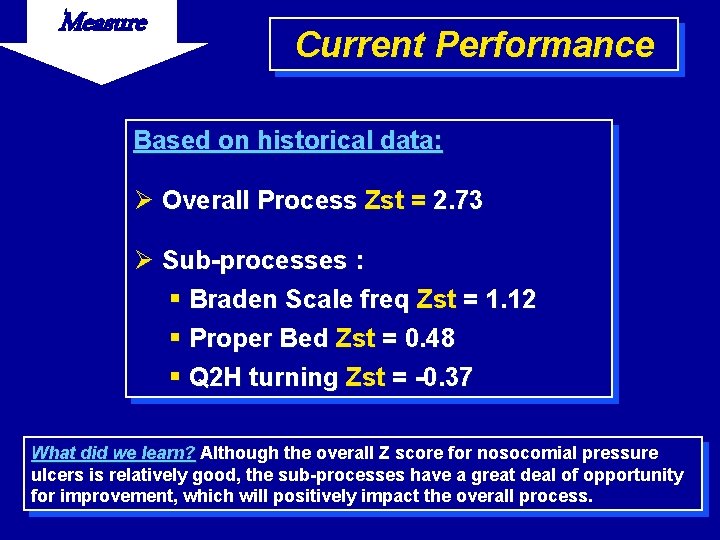

Measure Current Performance Based on historical data: Ø Overall Process Zst = 2. 73 Ø Sub-processes : § Braden Scale freq Zst = 1. 12 § Proper Bed Zst = 0. 48 § Q 2 H turning Zst = -0. 37 What did we learn? Although the overall Z score for nosocomial pressure ulcers is relatively good, the sub-processes have a great deal of opportunity for improvement, which will positively impact the overall process.

Measure Cause & Effect Diagram Braden Scale, Prevention & Treatment Protocols, and Daily skin assessments are the major factors affecting the current process.
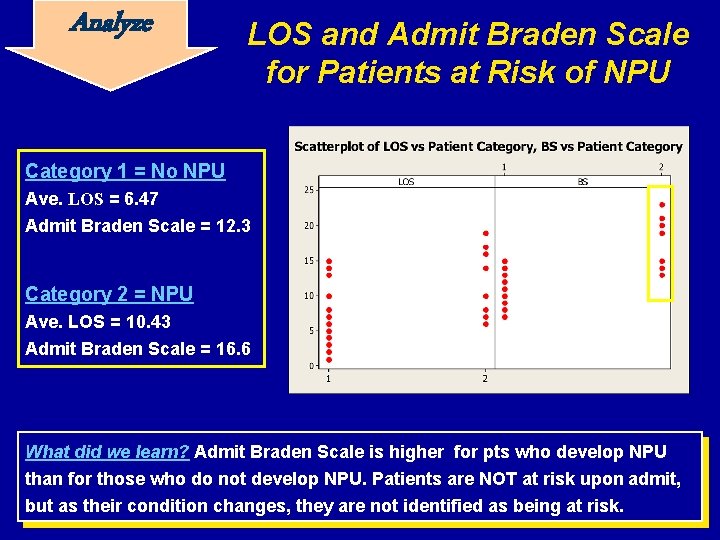
Analyze LOS and Admit Braden Scale for Patients at Risk of NPU Category 1 = No NPU Ave. LOS = 6. 47 Admit Braden Scale = 12. 3 Category 2 = NPU Ave. LOS = 10. 43 Admit Braden Scale = 16. 6 What did we learn? Admit Braden Scale is higher for pts who develop NPU than for those who do not develop NPU. Patients are NOT at risk upon admit, but as their condition changes, they are not identified as being at risk.
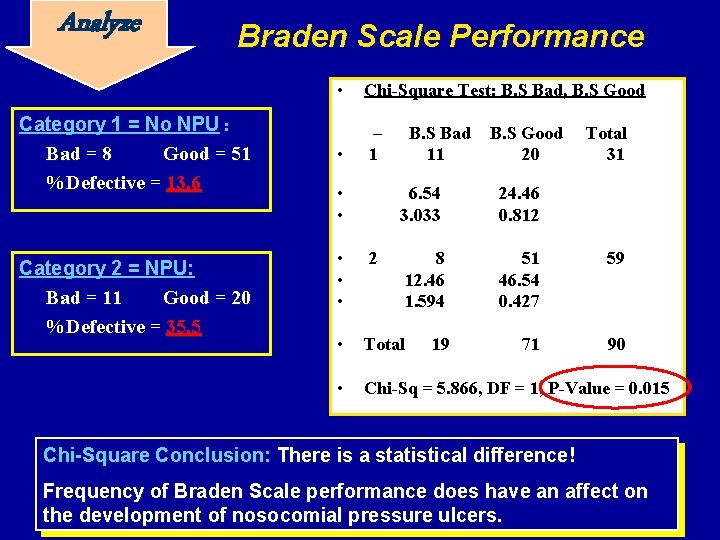
Analyze Braden Scale Performance Category 1 = No NPU : Bad = 8 Good = 51 %Defective = 13. 6 Category 2 = NPU: Bad = 11 Good = 20 %Defective = 35. 5 • Chi-Square Test: B. S Bad, B. S Good • – 1 • • B. S Bad 11 B. S Good 20 Total 31 6. 54 3. 033 24. 46 0. 812 8 12. 46 1. 594 51 46. 54 0. 427 59 71 90 • • • 2 • Total • Chi-Sq = 5. 866, DF = 1, P-Value = 0. 015 19 Chi-Square Conclusion: There is a statistical difference! Frequency of Braden Scale performance does have an affect on the development of nosocomial pressure ulcers.
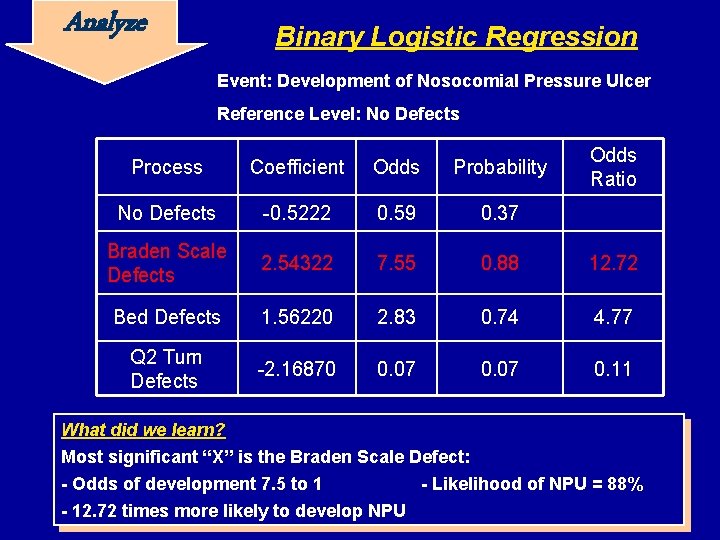
Analyze Binary Logistic Regression Event: Development of Nosocomial Pressure Ulcer Reference Level: No Defects Odds Ratio Process Coefficient Odds Probability No Defects -0. 5222 0. 59 0. 37 Braden Scale Defects 2. 54322 7. 55 0. 88 12. 72 Bed Defects 1. 56220 2. 83 0. 74 4. 77 Q 2 Turn Defects -2. 16870 0. 07 0. 11 What did we learn? Most significant “X” is the Braden Scale Defect: - Odds of development 7. 5 to 1 - 12. 72 times more likely to develop NPU - Likelihood of NPU = 88%

Improve Solutions Implemented • Braden Scale – Increased frequency of performance – Q 5 D – Added descriptions to BS assessment in HIS • Prevention/Treatment Protocol – Prompts added to HIS – Revised protocol to include more details – Task list for PCTs – Posted turning schedule • Education – Skin care covered in RN orientation by ET RN – Annual global competency on BS interpretation – ET RN accountability tracking tool for non-compliance
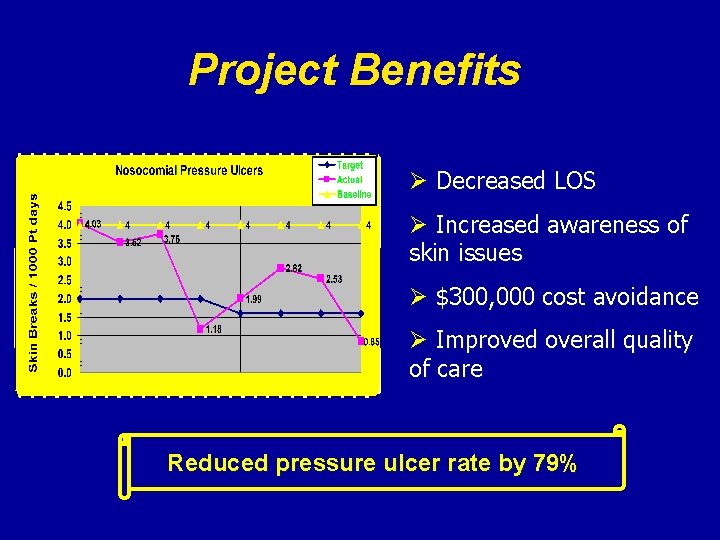
Project Benefits Ø Decreased LOS Ø Increased awareness of skin issues Ø $300, 000 cost avoidance Ø Improved overall quality of care Reduced pressure ulcer rate by 79%

Ongoing Efforts Led by Process Owner § § § New incontinence protocol New skin care product line New pressure ulcer staging system Complete pressure relief on heels Specialty beds on new unit Increased BS frequency – Q 3 D Continuous efforts on skin care issues are necessary for maintaining quality performance.

- Slides: 17