Therapeutic Advances for Type 2 Diabetes Mellitus Meredith

Therapeutic Advances for Type 2 Diabetes Mellitus Meredith Hawkins, MD Diabetes Research Center Albert Einstein College of Medicine

Evidence that Improving Glycemic Control Reduces Complications DCCT Kumamoto UKPDS 9 7% 8 7% Retinopathy 76% 69% 17 -21% Nephropathy 54% 70% 24 -33% Neuropathy 60% - - Macrovascular disease 41%* - 16%* Hb. A 1 c * not statistically significant
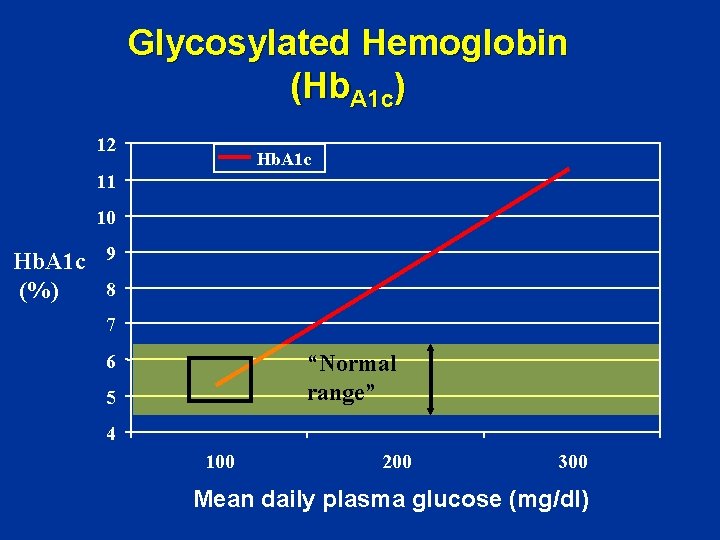
Glycosylated Hemoglobin (Hb. A 1 c) 12 Hb. A 1 c 11 10 Hb. A 1 c 9 8 (%) 7 “Normal range” 6 5 4 100 200 300 Mean daily plasma glucose (mg/dl)

Diet and Exercise are the Cornerstones of Diabetes Management!!

Long-term Success Stories: 1. Self-monitoring: Diet: record food intake daily, limit certain foods or food quantity Weight: check body weight 1 x/wk 2. Lower calorie, fat intake 3. Eat breakfast daily 4. Regular physical activity: 2500– 3000 kcal/wk (eg, walk 4 miles/d) 5. Behavior strategies: eg. Cognitive restructuring, spiritual
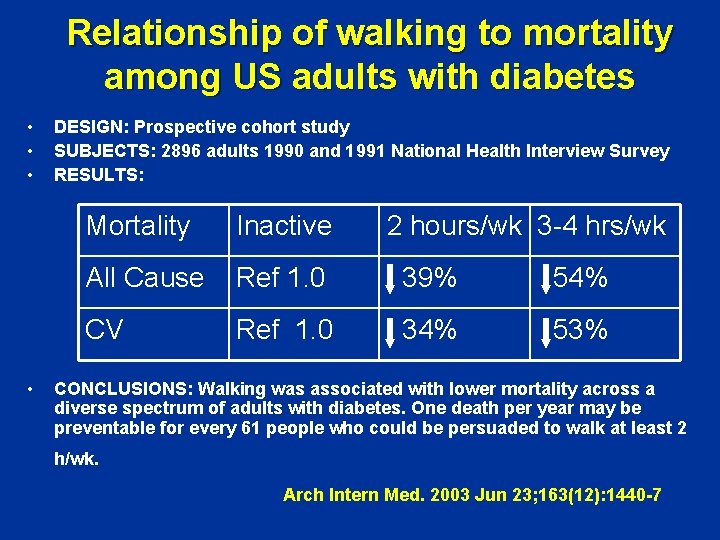
Relationship of walking to mortality among US adults with diabetes • • DESIGN: Prospective cohort study SUBJECTS: 2896 adults 1990 and 1991 National Health Interview Survey RESULTS: Mortality Inactive 2 hours/wk 3 -4 hrs/wk All Cause Ref 1. 0 39% 54% CV Ref 1. 0 34% 53% CONCLUSIONS: Walking was associated with lower mortality across a diverse spectrum of adults with diabetes. One death per year may be preventable for every 61 people who could be persuaded to walk at least 2 h/wk. Arch Intern Med. 2003 Jun 23; 163(12): 1440 -7
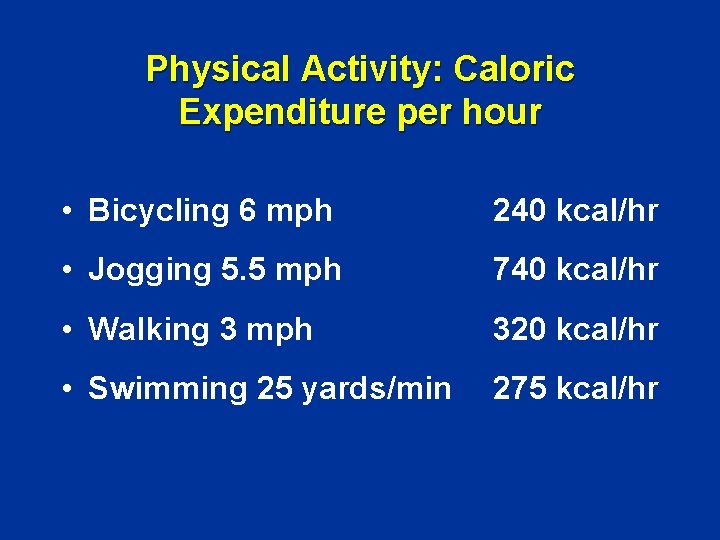
Physical Activity: Caloric Expenditure per hour • Bicycling 6 mph 240 kcal/hr • Jogging 5. 5 mph 740 kcal/hr • Walking 3 mph 320 kcal/hr • Swimming 25 yards/min 275 kcal/hr
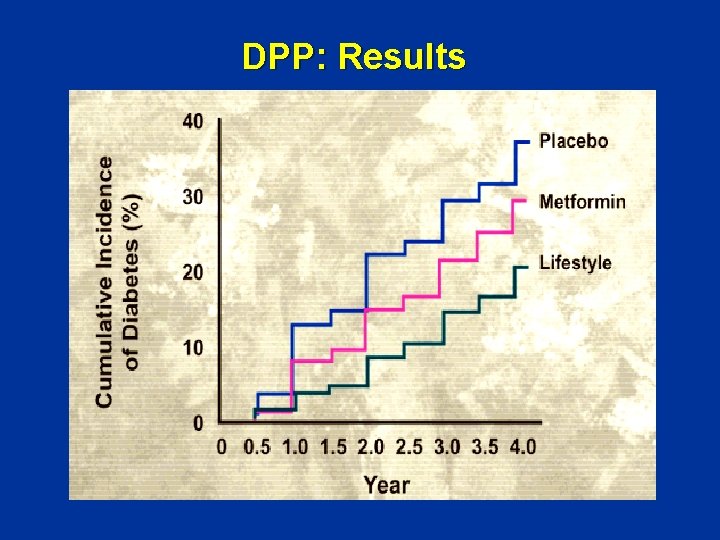
DPP: Results
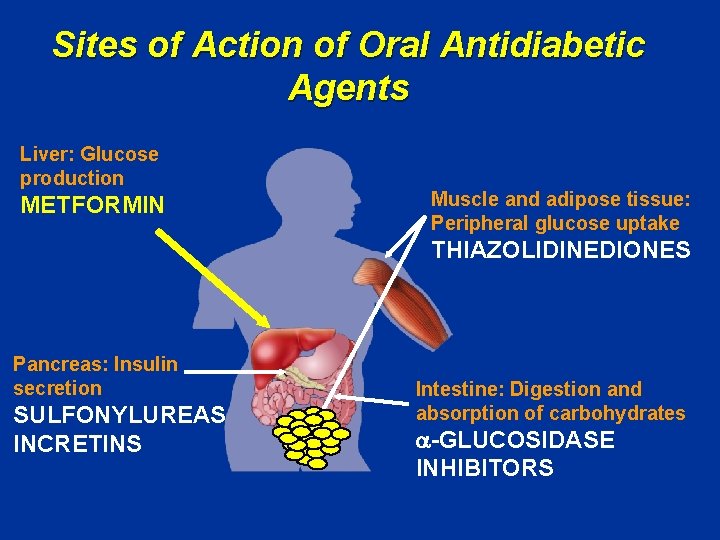
Sites of Action of Oral Antidiabetic Agents Liver: Glucose production METFORMIN Muscle and adipose tissue: Peripheral glucose uptake THIAZOLIDINEDIONES Pancreas: Insulin secretion SULFONYLUREAS INCRETINS Intestine: Digestion and absorption of carbohydrates -GLUCOSIDASE INHIBITORS

Metformin Advantages • Improves insulin resistance • Low risk of hypoglycemia • Effective in > 80% of patients • Advantageous lipid effects • Long record of relative safety • Favorable effects on weight • Decreased macrovascular complications (UKPDS) • Prevents Diabetes (DPP) Disadvantages • Contraindicated in organ failure • Lactic acidosis (1: 30 -90, 000) • Slow titration • GI side effects.
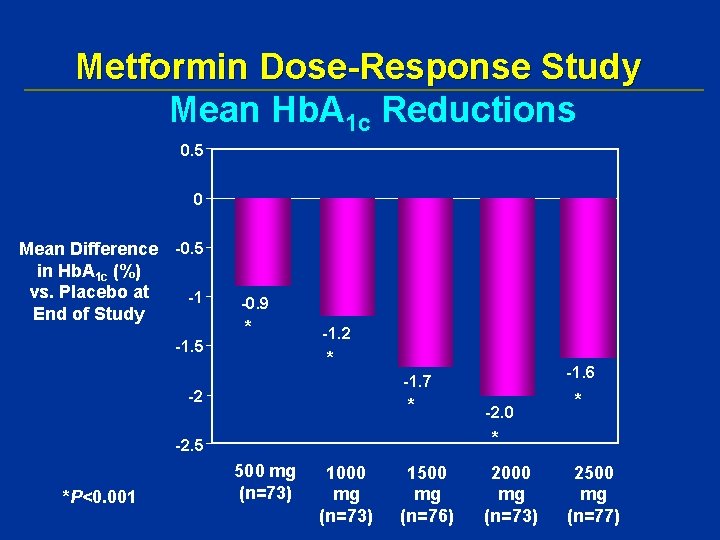
Metformin Dose-Response Study Mean Hb. A 1 c Reductions 0. 5 0 Mean Difference -0. 5 in Hb. A 1 c (%) vs. Placebo at -1 End of Study -1. 5 -0. 9 * -1. 2 * -2. 0 * * -2. 5 *P<0. 001 -1. 6 -1. 7 500 mg (n=73) 1000 mg (n=73) 1500 mg (n=76) 2000 mg (n=73) 2500 mg (n=77)

% Risk Reduction UKPDS: Effects of Intensive (Metformin) Treatment* † § ¶ ‡ Any Diabetes. Related Endpoint Diabetes. Related Mortality * Compared with conventional treatment; † P=0. 0023; ‡ P=0. 017; §P=0. 011; ¶ P=0. 01 All-Cause Mortality MI American Diabetes Association. Diabetes Care. 1999; 22(suppl 1): S 27 -S 31. UK Prospective Diabetes Study (UKPDS) Group. Lancet. 1998; 352: 854 -865.
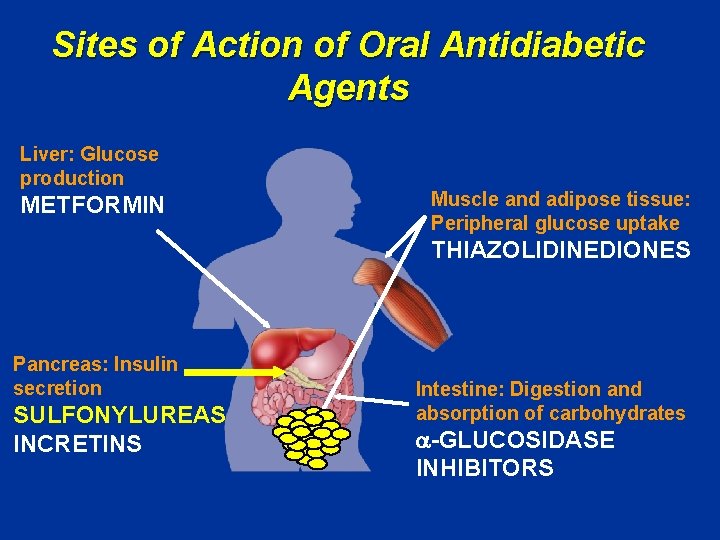
Sites of Action of Oral Antidiabetic Agents Liver: Glucose production METFORMIN Muscle and adipose tissue: Peripheral glucose uptake THIAZOLIDINEDIONES Pancreas: Insulin secretion SULFONYLUREAS INCRETINS Intestine: Digestion and absorption of carbohydrates -GLUCOSIDASE INHIBITORS
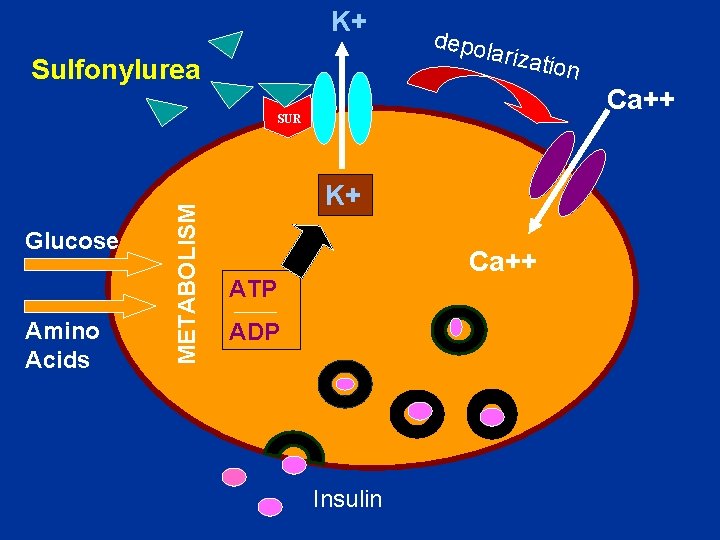
K+ Sulfonylurea depo lariza Ca++ Amino Acids METABOLISM SUR Glucose tion K+ Ca++ ATP ADP Insulin

Sulfonylureas Advantages Disadvantages • Improves insulin secretion • Long history of use • Once-daily dosing • Dose flexibility • Effective • Fast response • Well tolerated • Low cost • Weight gain • Hypoglycemia • Caution in the elderly and with organ failure • Hyperinsulinemia • Drug interactions • No response (20%) or response lost over time • Increased risk of cardiovascular disease ?
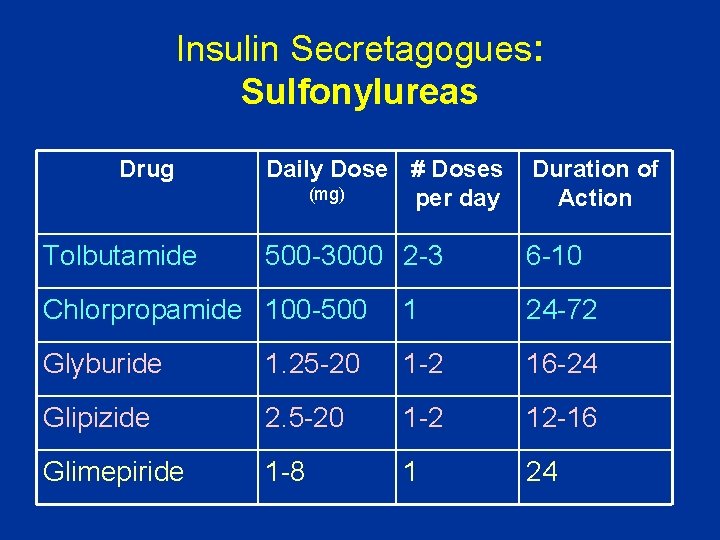
Insulin Secretagogues: Sulfonylureas Drug Tolbutamide Daily Dose # Doses (mg) per day Duration of Action 500 -3000 2 -3 6 -10 Chlorpropamide 100 -500 1 24 -72 Glyburide 1. 25 -20 1 -2 16 -24 Glipizide 2. 5 -20 1 -2 12 -16 Glimepiride 1 -8 1 24
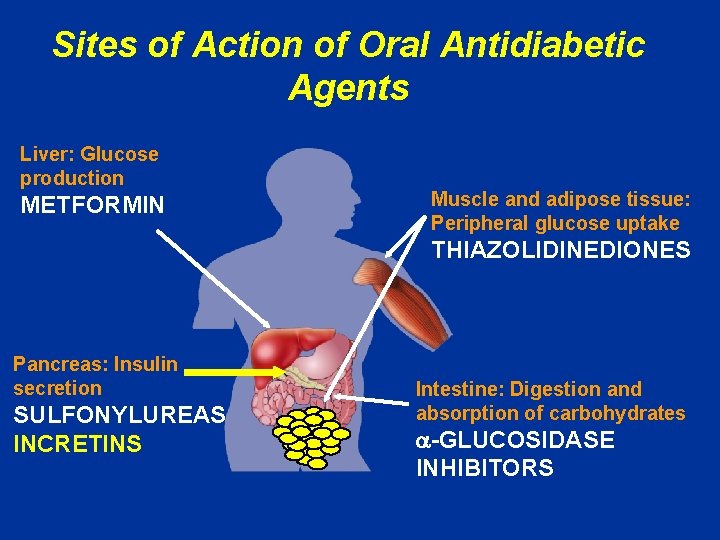
Sites of Action of Oral Antidiabetic Agents Liver: Glucose production METFORMIN Muscle and adipose tissue: Peripheral glucose uptake THIAZOLIDINEDIONES Pancreas: Insulin secretion SULFONYLUREAS INCRETINS Intestine: Digestion and absorption of carbohydrates -GLUCOSIDASE INHIBITORS

Insulin and Glucagon in Normal Glucose Tolerance Glucagon -Cells + HGO Glucose -Cells Insulin HGO= hepatic glucose output Adapted from Unger RH. Metabolism. 1974; 23: 581. + Glucose uptake
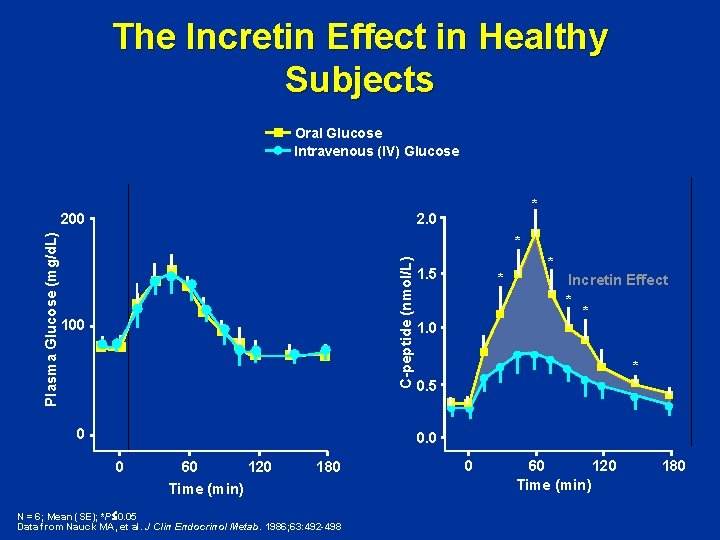
The Incretin Effect in Healthy Subjects Oral Glucose Intravenous (IV) Glucose * 2. 0 * C-peptide (nmol/L) Plasma Glucose (mg/d. L) 200 100 0 1. 5 * 1. 0 * Incretin Effect * * * 0. 5 0. 0 0 60 120 180 Time (min) N = 6; Mean (SE); *P 0. 05 Data from Nauck MA, et al. J Clin Endocrinol Metab. 1986; 63: 492 -498 0 60 120 Time (min) 180
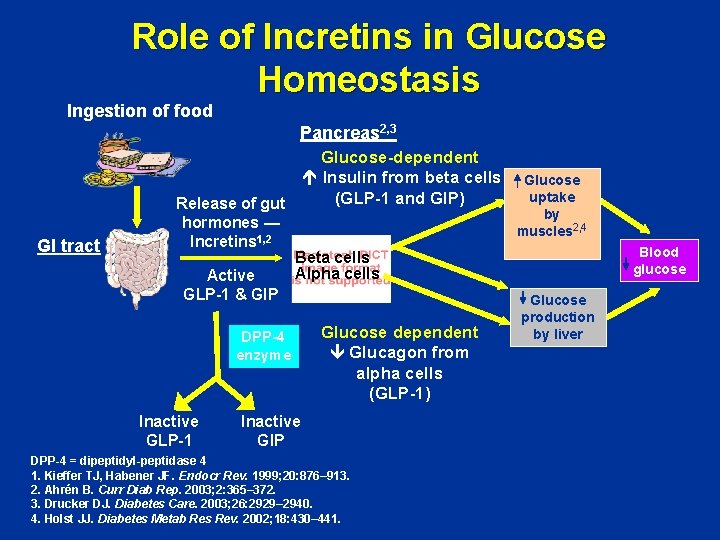
Role of Incretins in Glucose Homeostasis Ingestion of food Pancreas 2, 3 GI tract Release of gut hormones — Incretins 1, 2 Active GLP-1 & GIP Glucose-dependent Insulin from beta cells (GLP-1 and GIP) Blood glucose Beta cells Alpha cells DPP-4 enzyme Inactive GLP-1 Glucose uptake by muscles 2, 4 Glucose dependent Glucagon from alpha cells (GLP-1) Inactive GIP DPP-4 = dipeptidyl-peptidase 4 1. Kieffer TJ, Habener JF. Endocr Rev. 1999; 20: 876– 913. 2. Ahrén B. Curr Diab Rep. 2003; 2: 365– 372. 3. Drucker DJ. Diabetes Care. 2003; 26: 2929– 2940. 4. Holst JJ. Diabetes Metab Res Rev. 2002; 18: 430– 441. Glucose production by liver
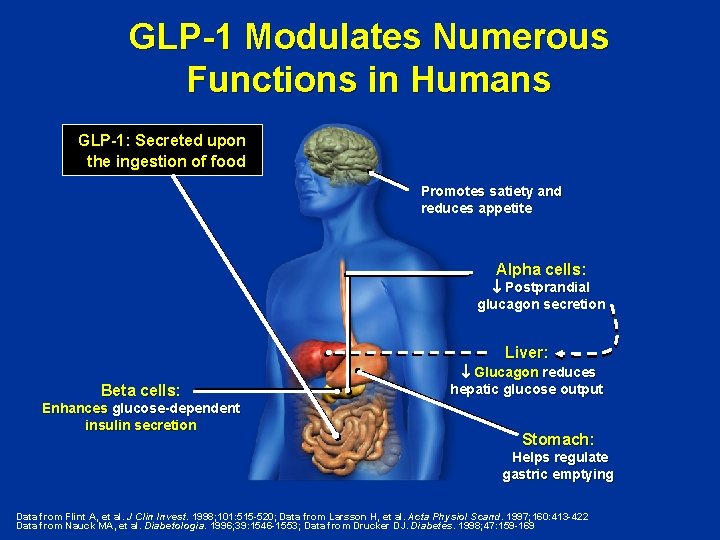
GLP-1 Modulates Numerous Functions in Humans GLP-1: Secreted upon the ingestion of food Promotes satiety and reduces appetite Alpha cells: Postprandial glucagon secretion Liver: Beta cells: Enhances glucose-dependent insulin secretion Glucagon reduces hepatic glucose output Stomach: Helps regulate gastric emptying Data from Flint A, et al. J Clin Invest. 1998; 101: 515 -520; Data from Larsson H, et al. Acta Physiol Scand. 1997; 160: 413 -422 Data from Nauck MA, et al. Diabetologia. 1996; 39: 1546 -1553; Data from Drucker DJ. Diabetes. 1998; 47: 159 -169

Incretins eg. GLP-1, Exenatide (Byetta), DPP-IV inhibitors (Januvia) Advantages Disadvantages • Promote satiety • Weight loss (Byetta) • Improve postprandial insulin secretion • Reduce glucagon levels • Delayed nutrient absorption • • • Duration (GLP-1) Nausea Other GI side effects Require injection Lack of long-term safety data • Cost
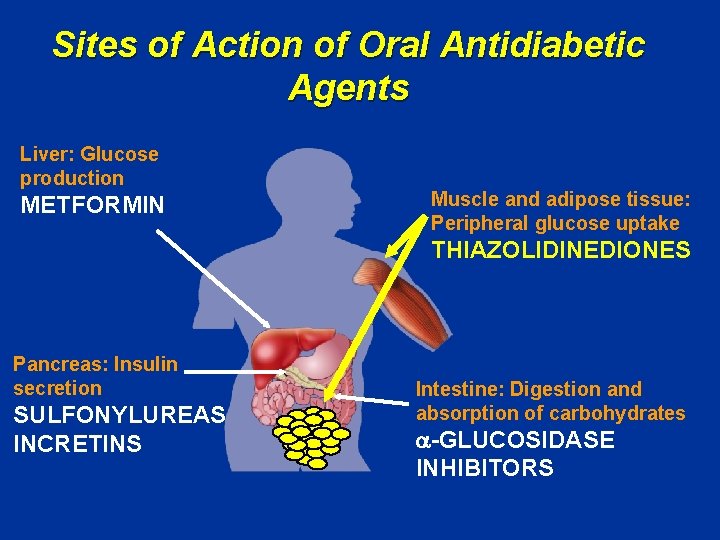
Sites of Action of Oral Antidiabetic Agents Liver: Glucose production METFORMIN Muscle and adipose tissue: Peripheral glucose uptake THIAZOLIDINEDIONES Pancreas: Insulin secretion SULFONYLUREAS INCRETINS Intestine: Digestion and absorption of carbohydrates -GLUCOSIDASE INHIBITORS
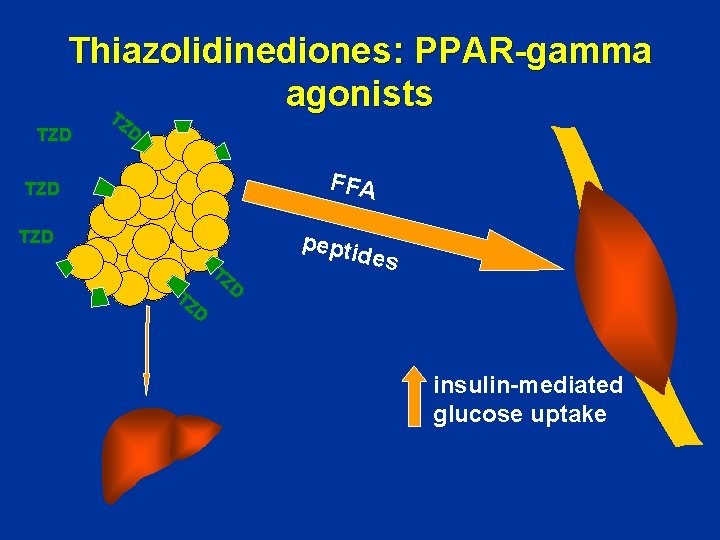
Thiazolidinediones: PPAR-gamma agonists T TZD ZD FFA TZD TZ D pepti des insulin-mediated glucose uptake

Thiazolidinediones Advantages Disadvantages • Target insulin resistance • +/- lipid profile • Use in renal insufficiency • Preserve b-cell function • Prevent progression from IGT to type 2 diabetes • • • Hepatotoxicity Weight gain Fluid retention Congestive Heart Failure Delayed onset of action Lack of long-term safety data • Cost • Cardiovascular outcomes? ? ?

Currently Available TZDs Agent Dosage Range Pioglitazone 15– 45 mg once daily Rosiglitazone 4– 8 mg daily (in 1 or 2 doses) + Hepatic metabolism Renal and liver excretion
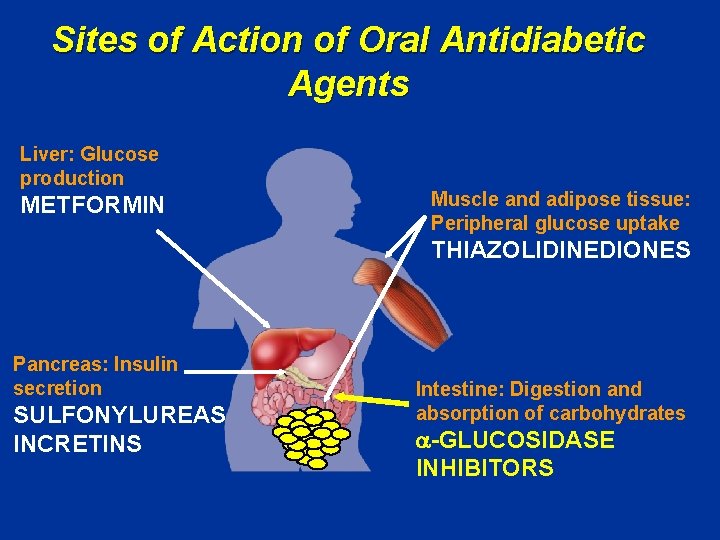
Sites of Action of Oral Antidiabetic Agents Liver: Glucose production METFORMIN Muscle and adipose tissue: Peripheral glucose uptake THIAZOLIDINEDIONES Pancreas: Insulin secretion SULFONYLUREAS INCRETINS Intestine: Digestion and absorption of carbohydrates -GLUCOSIDASE INHIBITORS
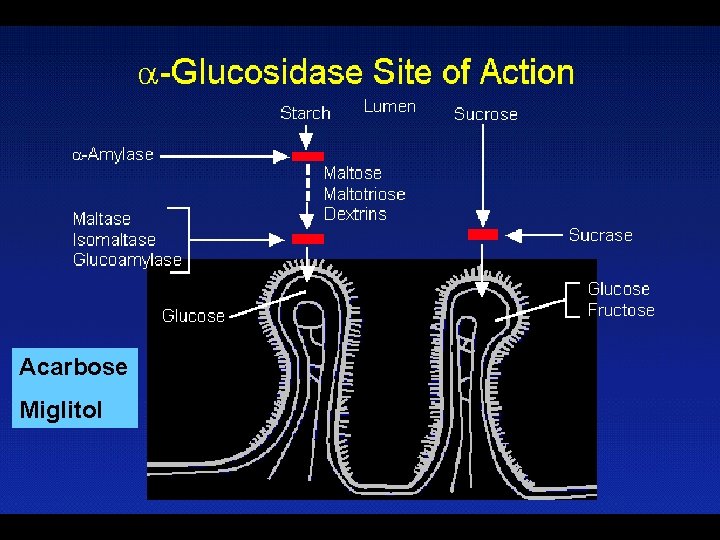
Acarbose Miglitol

-Glucosidase Inhibitors Advantages • Long history of use • Good safety profile • No weight gain • Mild stool softening • No substantial systemic drug-drug interaction • Good adjunctive therapy Disadvantages • Require highcarbohydrate diet • Most be taken before every meal • Modest efficacy • Flatulence and GI side effects • Elevated LFT’s have been reported
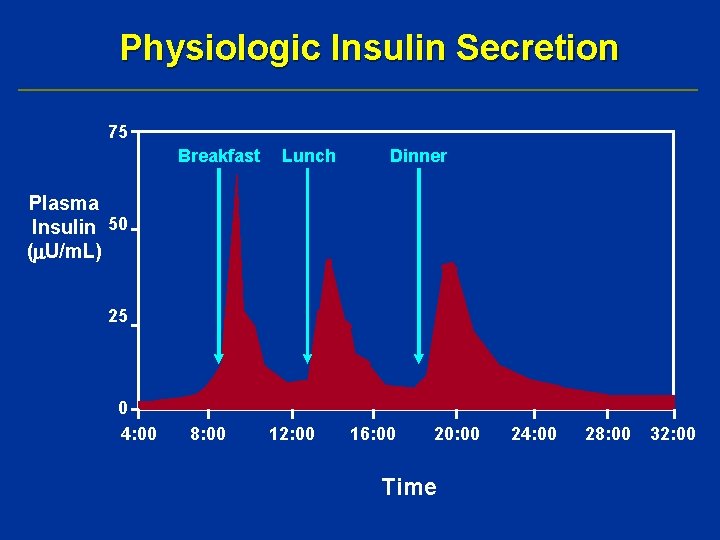
Physiologic Insulin Secretion 75 Breakfast Lunch Dinner Plasma Insulin 50 ( U/m. L) 25 0 4: 00 8: 00 12: 00 16: 00 20: 00 Time 24: 00 28: 00 32: 00

Insulin Preparations • These preparations target insulin-sensitive tissue to increase glucose uptake and decrease hepatic glucose production Rapid-Acting – Insulin lispro (analogue) – Insulin aspart (analogue) – Insulin glulisine (analogue) Short-Acting – Regular (soluble) Intermediate-Acting – NPH (isophane) – Lente (insulin zinc suspension) Long-Acting – Ultralente (no longer on market) – Insulin glargine and detemir (analogue)*
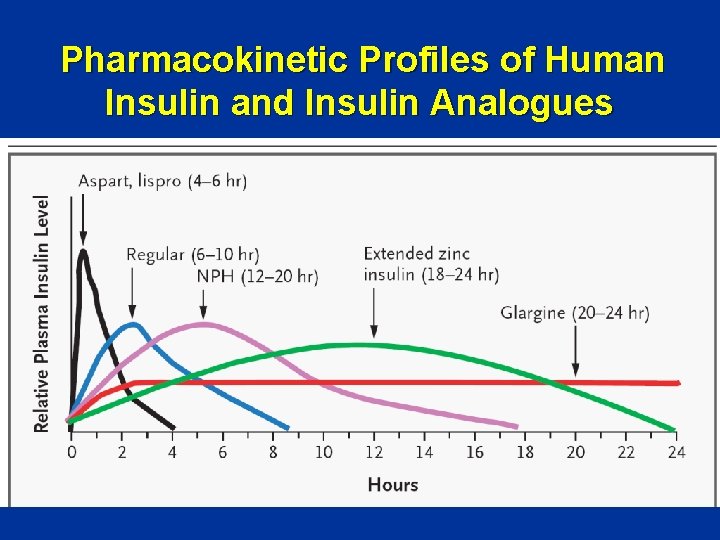
Pharmacokinetic Profiles of Human Insulin and Insulin Analogues
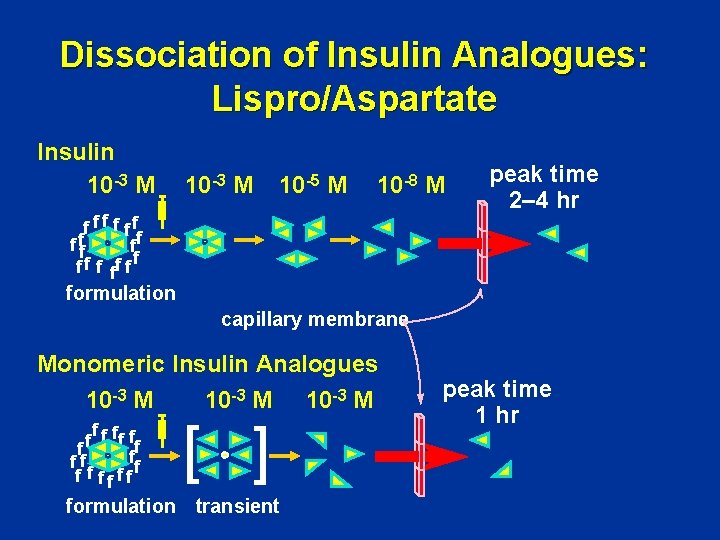
Dissociation of Insulin Analogues: Lispro/Aspartate Insulin 10 -3 M 10 -5 M 10 -8 M f f ff ff f f peak time 2– 4 hr formulation capillary membrane Monomeric Insulin Analogues 10 -3 M ff f f ff fff [ ] formulation transient peak time 1 hr
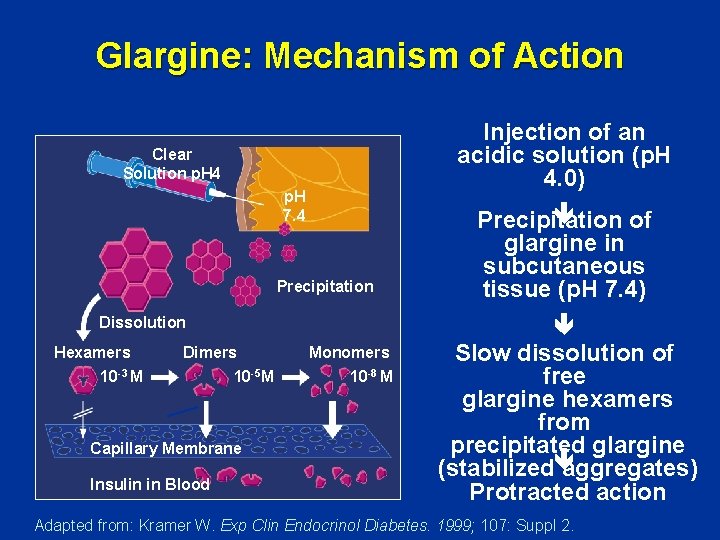
Glargine: Mechanism of Action Injection of an acidic solution (p. H 4. 0) Clear Solution p. H 4 p. H 7. 4 Precipitation Dissolution Hexamers 10 -3 M Dimers 10 -5 M Capillary Membrane Insulin in Blood Monomers 10 -8 M Precipitation of glargine in subcutaneous tissue (p. H 7. 4) Slow dissolution of free glargine hexamers from precipitated glargine (stabilized aggregates) Protracted action Adapted from: Kramer W. Exp Clin Endocrinol Diabetes. 1999; 107: Suppl 2.
Insulin Effect Basal-Bolus Insulin: Insulin Glargine at HS and Mealtime Lispro or Aspart B L Insulin lispro or aspart D HS Insulin glargine

Starting Basal Insulin: Type 2 DM • Continue oral agent(s) at same dosage (d/c TZD) • Add single, evening insulin dose (around 10 U)* – NPH (bedtime) • Treat to target fasting glucose (usually 80 -120 mg/d. L) • Increase insulin dose weekly as needed – Increase 4 U if FBG >140 mg/d. L – Increase 2 U if FBG = 120 to 140 mg/d. L • Next step: add short-acting insulin before meals * It will usually take 40 -60 units to get to target 5 -18

ADA Treatment Guidelines 2007

Cost of pharmacological therapy for Type 2 DM for glucose control
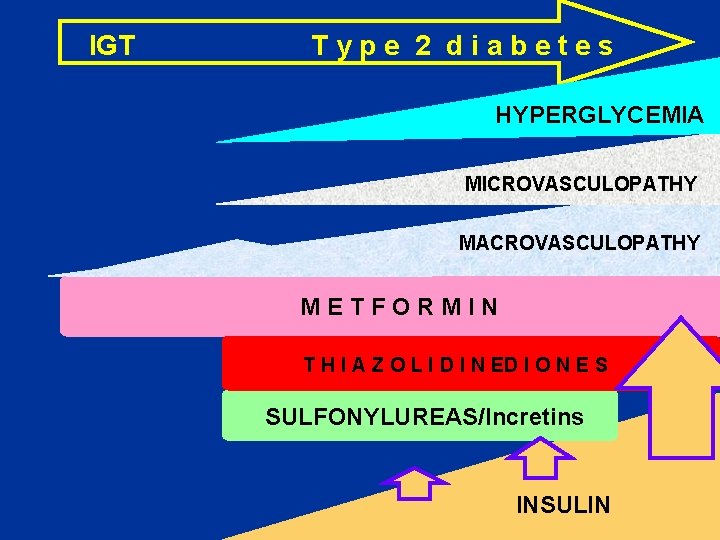
IGT Type 2 diabetes HYPERGLYCEMIA MICROVASCULOPATHY MACROVASCULOPATHY METFORMIN T H I A Z O L I D I N ED I O N E S SULFONYLUREAS/Incretins INSULIN
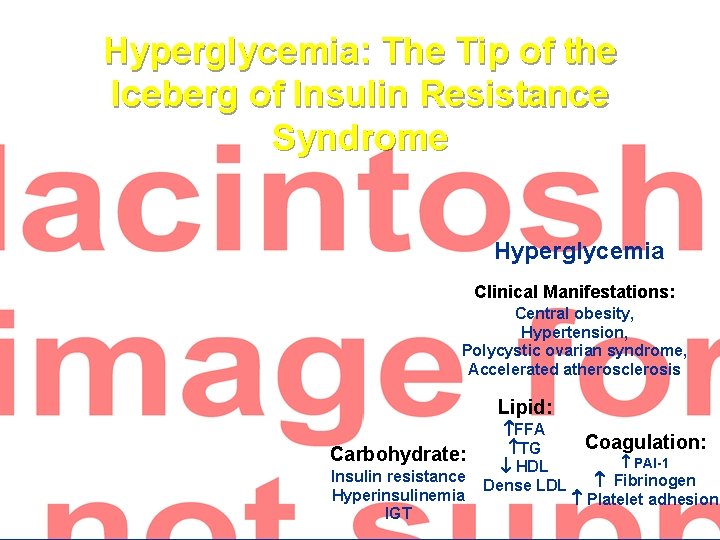
Hyperglycemia: The Tip of the Iceberg of Insulin Resistance Syndrome Hyperglycemia Clinical Manifestations: Central obesity, Hypertension, Polycystic ovarian syndrome, Accelerated atherosclerosis Lipid: Carbohydrate: Insulin resistance Hyperinsulinemia IGT FFA TG HDL Dense LDL Coagulation: PAI-1 Fibrinogen Platelet adhesion

Goal Recommendations in Type 2 Diabetes Goal Average preprandial glucose (mg/d. L) 90– 130 Average postprandial glucose (mg/d. L) <180 Hb. A 1 c (%) <7 LDL-Cholesterol (mg/d. L) <100 Triglycerides (mg/d. L) <150 HDL-Cholesterol (mg/d. L) >40 Blood pressure (mm Hg) <130/80 American Diabetes Association: Clinical Practice Recommendations. Diabetes Care Vol. 30, Suppl. 1, 2007
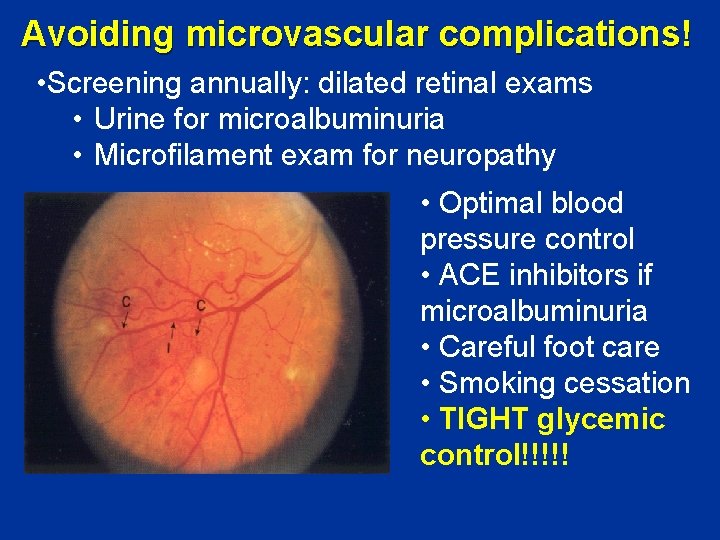
Avoiding microvascular complications! • Screening annually: dilated retinal exams • Urine for microalbuminuria • Microfilament exam for neuropathy • Optimal blood pressure control • ACE inhibitors if microalbuminuria • Careful foot care • Smoking cessation • TIGHT glycemic control!!!!!
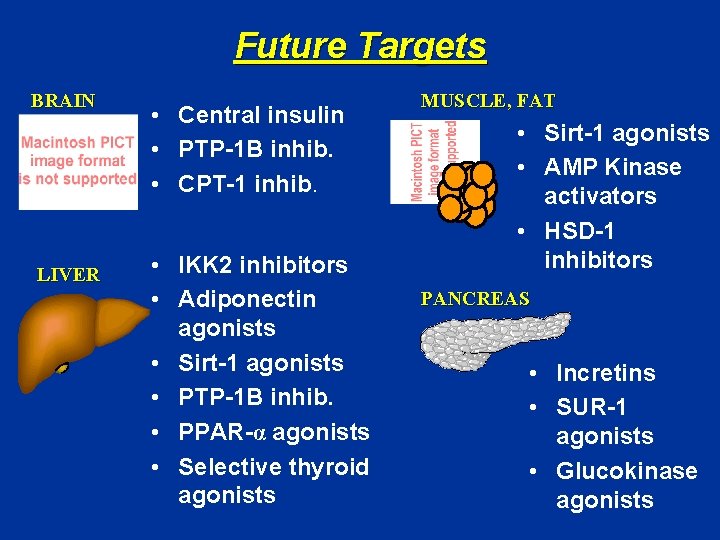
Future Targets BRAIN LIVER • Central insulin • PTP-1 B inhib. • CPT-1 inhib. • IKK 2 inhibitors • Adiponectin agonists • Sirt-1 agonists • PTP-1 B inhib. • PPAR-α agonists • Selective thyroid agonists MUSCLE, FAT • Sirt-1 agonists • AMP Kinase activators • HSD-1 inhibitors PANCREAS • Incretins • SUR-1 agonists • Glucokinase agonists
- Slides: 43