The Use of Placental Blood on Admission to
The Use of Placental Blood on Admission to the NICU Copyright Monet Nicole Birthing Stories Denver, CO Audrey Nervig DNP, NNP Lori Rubarth, Ph. D, APRN, NNP-BC Creighton University

Disclosure • The author declares that she has no relevant or material financial interests that relate to the evidence based practice implementation described in this presentation

Background / Significance • Phlebotomy = Poor patient Outcomes • Pain 7, 8, 12, 18 • Blood Loss 1 • Anemia 19 • Early Blood Transfusion 4, 19 • Intraventricular Hemorrhage (IVH) 4 • Historical Misconceptions 5, 9, 16 • False results • Correlates with maternal labs • Not feasible or sustainable

Purpose • To implement and assess the feasibility and efficacy of drawing initial laboratory specimens for all infants upon admission to the NICU from the otherwise discarded placenta, eliminating the need for heel lance, venous sticks, and arterial draws. • Doctorate of Nursing Practice Project

Supporting Research Evidence • Correlation 2, 3, 9, 10, 11, 15, 16 • Complete Blood Count with Differential • Blood Culture • Feasibility and Sustainability 1, 5 • Benefits of Placental Draws 1, 5 • Higher Hemoglobin • Decreased Blood Transfusion • Elimination or Decrease in Severity of IVH

Setting and Sample • Midwest Level III 35 bed NICU • All infants admitted to NICU will have initial phlebotomy drawn from placenta • Evaluate infants < 1500 grams pre- and postimplementation • Non eligible infants: • Admitted to NICU from outside hospital or newborn nursery • Placental abruption • Cord blood banking • RN unable to draw useable specimen from placenta

Implementation 1. CBC with differential Comparison (N=20) 2. Trained NICU staff RNs to draw placental blood 3. Policy and Practice Change 4. Retrospective Chart Review 5. Analysis and Interpretation
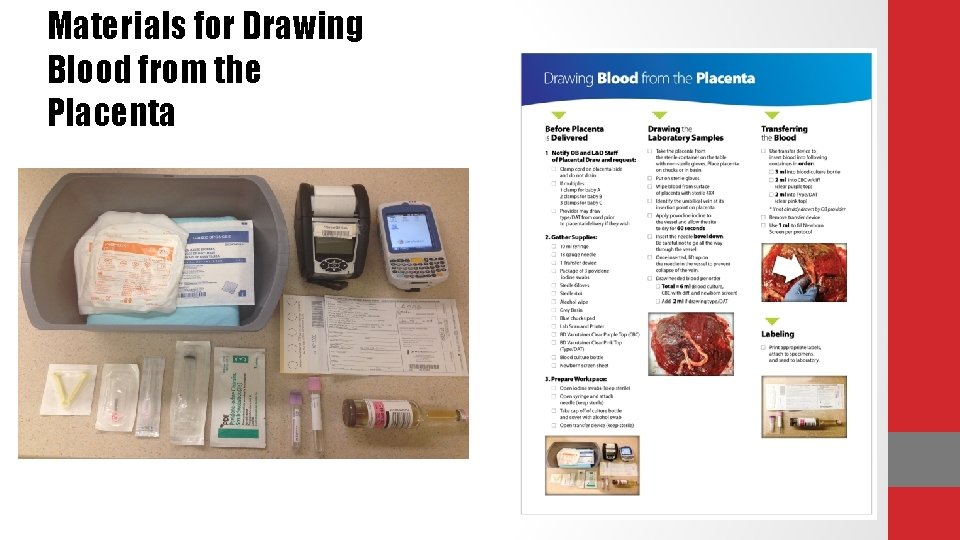
Materials for Drawing Blood from the Placenta
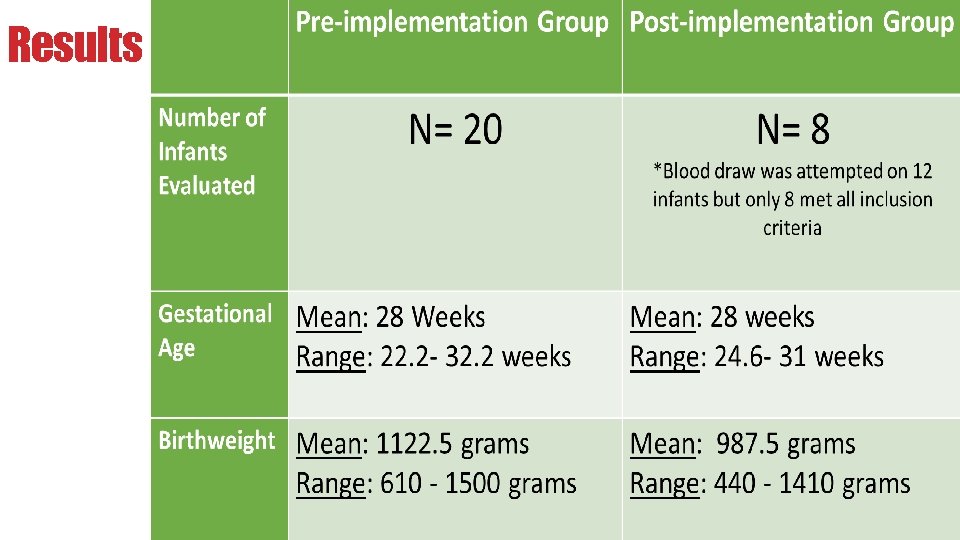
Results
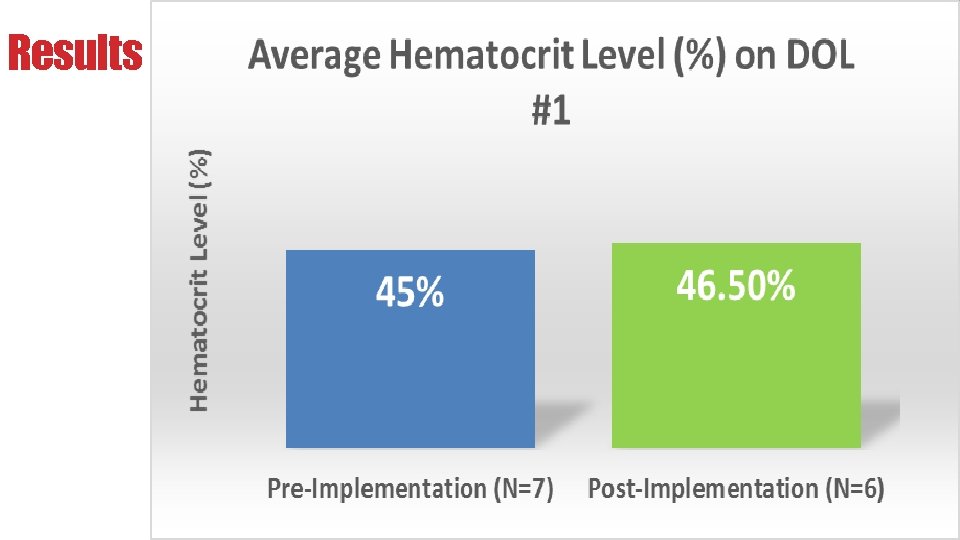
Results

Results
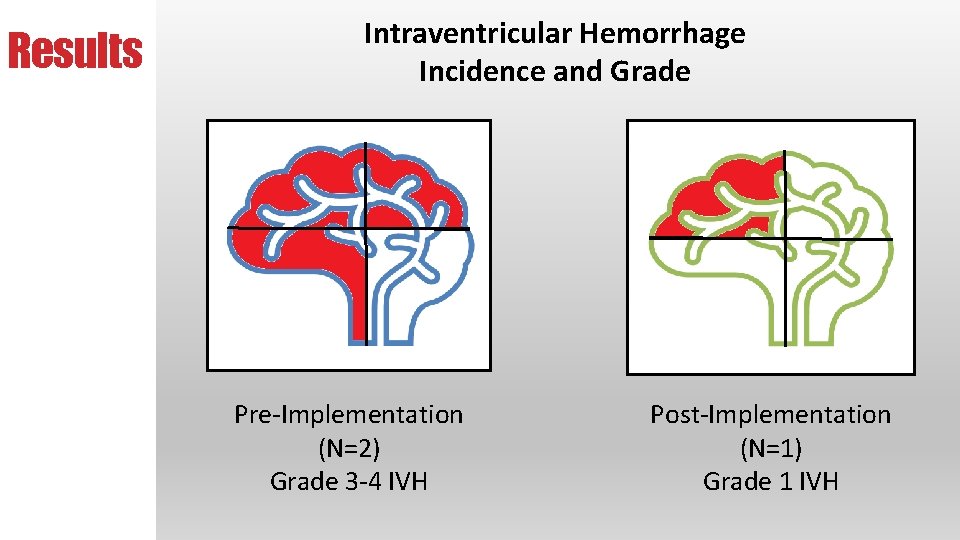
Results Intraventricular Hemorrhage Intraventricular Incidence and Grade Hemorrhage Pre-Implementation (N=2) Grade 3 -4 IVH Post-Implementation (N=1) Grade 1 IVH

Results Intraventricular Feasibility and Sustainability Hemorrhage • Placental Blood Draw Success Rate (N=12) • 56% for CBCs • 75% for Blood Cultures • No contaminated specimens • Genetic Screening (Karyotype and Microarray) • Incorporated into standard of practice • RN Staff • No increased cost to the unit

Limitations and Opportunities • EBP implementation project, could not control for variables • Resistance to change • Learned skill

Further Outcome Evaluations • Continued evaluation • Process Improvement • Development of RN skill expertise • Newborn Metabolic Screening • Standardized reference range for CBC indices drawn from placental blood

Take Home Message • Drawing admission lab specimens from the placenta for VLBW infants • May increase hematocrit levels • May delay early blood transfusions • May decrease incidence and/or severity of IVH • Is a feasible and sustainable procedure • Has additional clinical benefits • Additional Evaluation is needed

Acknowledgements • Lori Rubarth, Ph. D, APRN-NP, NNP-BC • Brenda Wallingford, DNP, APRN-NP, NNP-BC • Molly Schlegel, DNP, APRN-NP, NNP-BC • Tracy Meyers, RN, BSN • Terrance Zach, M. D. • John Schmidt, M. D. • Harold Kaftan, M. D. • Brenda Horton, MT(ASCP) • Craig Stacey, MBA, MT(ASCP) • RN Staff of CHI Health Bergan Mercy Medical Center • Tom Rubarth, Graphic Design

References 1. Baer, V. L. , Lambert, D. K. , Carroll, P. D. , Gerday, E. , & Christensen, R. D. (2013). Using umbilical cord blood for the initial blood tests of VLBW neonates results in higher hemoglobin and fewer RBC transfusions. Journal of Perinatology, 33, 363365. doi: 10. 1038/jp. 2012. 127 2. Beeram, M. R. , Loughran, C. , Cipriani, C. , Govande, V. (2012). Utilization of umbilical cord blood for the evaluation of group b streptococcal Sepsis Screening. Clinical Pediatrics, 51(5), 447 -453. doi: 10. 1177/0009922811431882 3. Carroll, P. D. , Nankervis, C. A. , Iams, J. , & Kelleher, K. (2012). Umbilical cord blood as a replacement source for admission complete blood count in premature infants. Journal of Perinatology, 32, 97 -102. doi: 10. 1038/jp. 2011. 60 4. Christensen, R. D. (2012). Associations between “early” red blood cell transfusion and severe intraventricular hemorrhage, and between “late” red blood cell transfusion and necrotizing enterocolitis. Seminars in Perinatology, 36, 283 -289. doi: 10. 1053/j. semperi. 2012. 04. 009 5. Christensen, R. D. , Lambert, D. K. , Baer, V. L. , Montgomery, D. P. , Barney, C. K. , Coulter, D. M. , …Bennett, S. T. (2011). Postponing or eliminating red blood cell transfusions of very low birth weight neonates by obtaining all baseline laboratory blood tests from otherwise discarded fetal blood in the placenta. Transfusion, 51, 253 -258. doi: 10. 111/j. 1537 -2995. 2010. 02827. x 6. Costakos, D. T. , Walden, J. , Rinzel, M. T. , & Dahlen, L. (2009). Painless blood testing to prevent neonatal sepsis. Wisconsin Medical Journal, 108(6), 321 -322. Retrieved from: http: //web. b. ebscohost. com. cuhsl. creighton. edu/ehost/detail? vid=16&sid=edcaf 8 ae-2285 -4020 -b 59 ad 9 b 1 a 169294 d%40 sessionmgr 112&hid=103&bdata=Jn. Npd. GU 9 ZWhvc 3 Qtb. Gl 2 ZQ%3 d%3 d#db=mdc&AN=19813501 7. Grunau, R. E. (2013). Neonatal pain in very preterm infants: Long-term effects on brain, neurodevelopment, and pain reactivity. Rambam Maimonides Medical Journal, 4(4). doi: 10. 5041/RMMJ. 10132. 8. Grunau, R. E. , Holsti, L. , Haley, D. W. , Oberlander, T. , Weinberg, J. Solimano, A. , . . . Yu, W. (2005). Neonatal procedural pain exposure predicts lower cortisol and behavioral reactivity in preterm infants in the NICU. Pain, 113(3), 293 -300. Retrieved from: http: //www. ncbi. nlm. nih. gov/pmc/articles/PMC 1447527/pdf/nihms-4619. pdf 9. Hansen, A. , Forbes, P. , & Buck, R. (2005). Potential substitution of cord blood for infant blood in the neonatal sepsis evaluation. Biology of the Neonate, 88, 12 -18. doi: 10. 1159/000083946 10. Herson, V. C. , Block, C. , Mc. Laughlin, J. C. , Tetreault, J. , Eisenfeld, L. I. , & Krause, P. J. (1998). Placental blood sampling: an aid to the diagnosis of neonatal sepsis. The Journal of Perinatology, 18(2), 135 -137.

References 11. Kalathia, M. B. , Shingala, P. A. , Parmar, P. N. , Parikh, Y. N. , & Kalathia, I. M. (2013). Study of umbilical cord blood culture in diagnosis of early-onset sepsis among newborns with high-risk factors. Journal of Clinical Neonatology, 2(4), 169 -172. doi: 10. 4103/2249 -4847 -123092 12. Knaepen, L. , Patijn, J. , van Kleef, M. , Mulder, M. , Tibboel, D. , & Joosten, E. A. J. (2012). Neonatal repetitive needle pricking: Plasticity of the spinal nociceptive circuit and extended postoperative pain in later life. Developmental Neurobiology, 73(1), 85 -97. doi: 10. 11002/dneu. 22047 13. Levine, M. E. (1973). Introduction to clinical nursing. Philadelphia, PA: FA Davis Company 14. Mefford, L. C. (2004). A theory of health promotion for preterm infants based on Levine’s conservation model of nursing. Nursing Science Quarterly, 17(3), 260 -266. doi: 10. 1177/0894318404266327 15. Polin, J. I. , Knox, I. , Baumgart, S. , Campman, E. , Mennuti, M. T. , & Polin, R. A. (1981). Use of umbilical cord blood culture for detection of neonatal bacteremia. Obstetrics and Gynecology, 57(2), 233 -237. Retrieved from: http: //journals. lww. com/greenjournal/Abstract/1981/02000/Use_of_Umbilical_Cord_Blood_Culture_for_Detection. 18. aspx 16. Qaiser, D. H. , Sandila, M. P. , Omair, A. , & Ghori, G. M. (2013). Correlation of routine haematological parameters between normal maternal blood and the cord blood of healthy newborns in selected hospitals of Karachi. Journal of the College of Physicians and Surgeons of Pakistan, 23(2), 128 -131. Retrieved from: http: //web. b. ebscohost. com. cuhsl. creighton. edu/ehost/detail? vid=16&sid=edcaf 8 ae-2285 -4020 -b 59 a d 9 b 1 a 169294 d%40 sessionmgr 112&hid=103&bdata=Jn. Npd. GU 9 ZWhvc 3 Qtb. Gl 2 ZQ%3 d%3 d#db=mdc&AN=23374517 17. Rotshenker-Olshinka, K. , Shinwell, E. S. , Juster-Reicher, A. , Rosin, I. , & Flidel-Rimon, O. (2014). Comparison of hematologic indices and markers of infection in umbilical cord blood and neonatal blood. Journal of Maternal-Fetal & Neonatal Medicine, 27(6), 625 -628. doi: 10. 3109/14767058. 2013. 825597 18. Walker, S. (2013). Neonatal pain. Pediatric Anesthesia, 24, 39 -48. Retrieved from: http: //web. a. ebscohost. com. cuhsl. creighton. edu/ehost/detail? sid=3 e 3 b 405 a-4 f 35 -4 a 96 b 399434 ac 765 f 571%40 sessionmgr 4003&vid=7&hid=4101 19. Widness, J. A. (2000). Pathophysiology, diagnosis, and prevention of neonatal anemia. Neo. Reviews, 1(4), e 61 -e 68. doi: 10. 1542/neo/1 -4 -

Questions? Copyright Emma Jean Photography Brisbane, Queensland, Australia

Additional Slides for Questions Copyright Emma Jean Photography Brisbane, Queensland, Australia

Correlation – Research Evidence • Blood Culture • • Copyright Emma Jean Photography Brisbane, Queensland, Australia Low contamination rate 2, Low false positive rate, 9, 15 High specificity, sensitivity, and positive predictive value 11 Detects more pathogens than peripheral samples 10, 11 • CBC with Differential • • • Moderate to high statistically significant correlation between WBC 3, 9 High correlation between I: T ratios No statistical difference in false positives 3, 9 A significant high correlation for Hct and Hgb 3, 9 and High correlation for platelets 9 • Overall infant values are independent of maternal values 16
- Slides: 22