THE URINARY SYSTEM Functions 1 Remove nitrogenous wastes























- Slides: 52

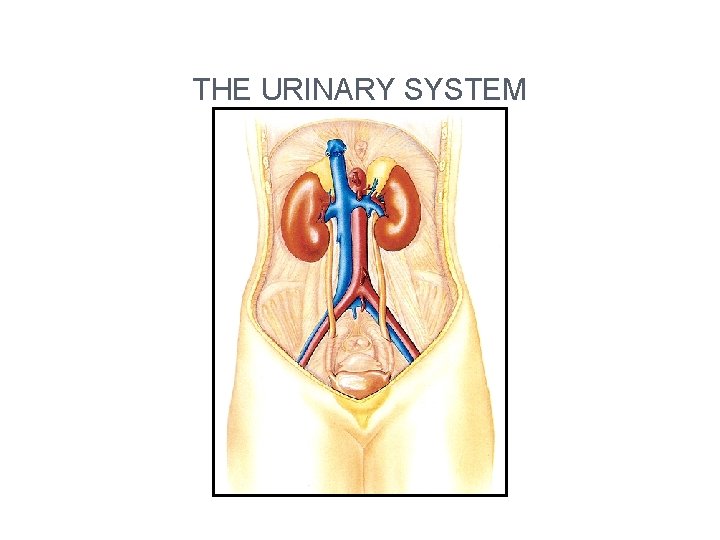
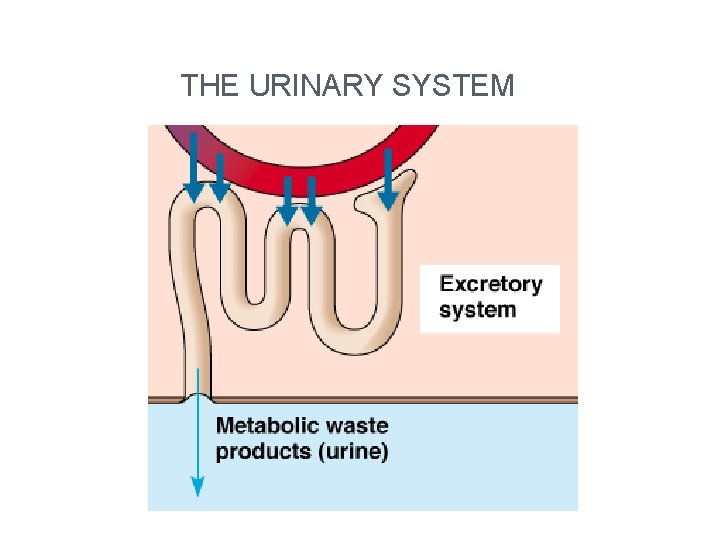
THE URINARY SYSTEM

Functions 1. Remove nitrogenous wastes 2. Maintain electrolyte, acid-base, and fluid balance of blood 3. Homeostatic organ system 4. Acts as blood filter 5. Release hormones: calcitriol & erythropoietin

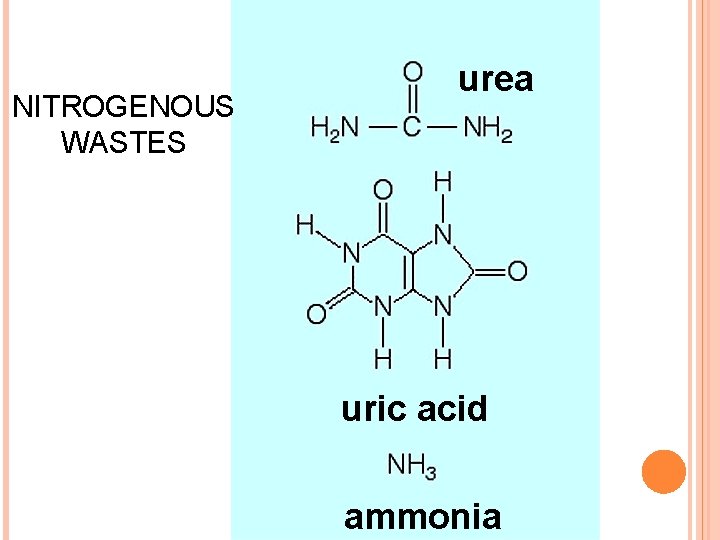
NITROGENOUS WASTES urea uric acid ammonia


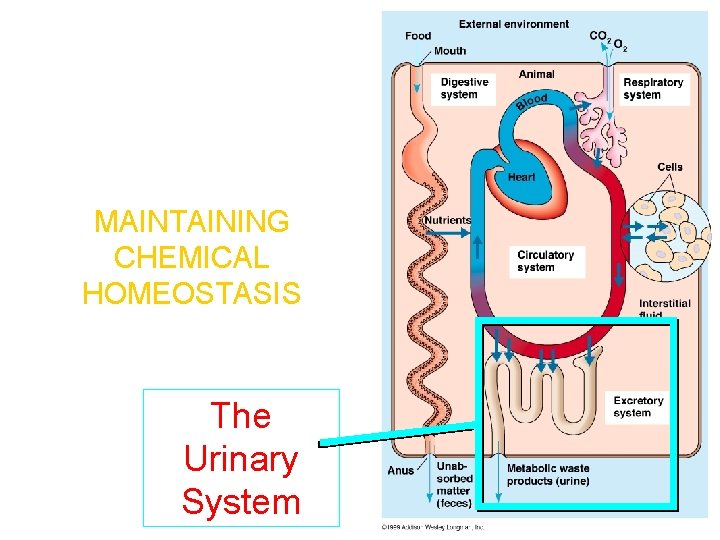
MAINTAINING CHEMICAL HOMEOSTASIS The Urinary System

THE URINARY SYSTEM

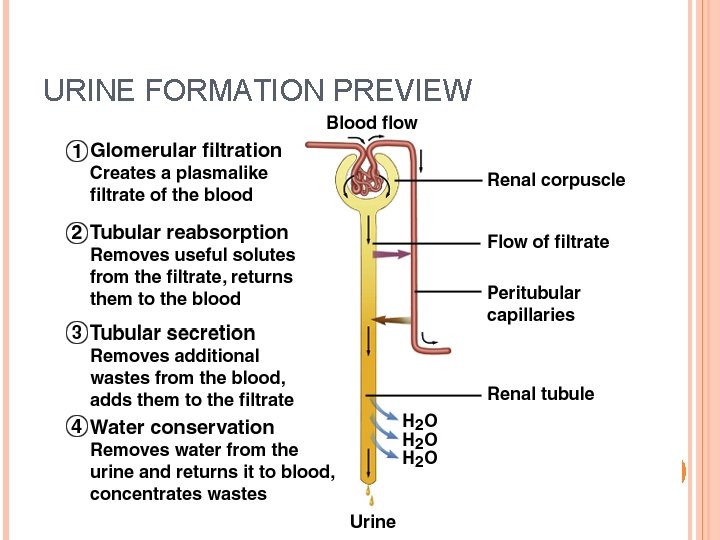
URINE FORMATION PREVIEW

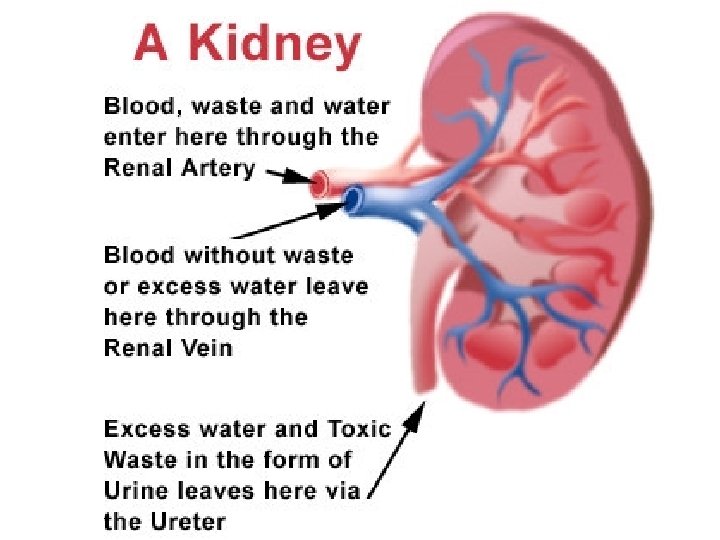
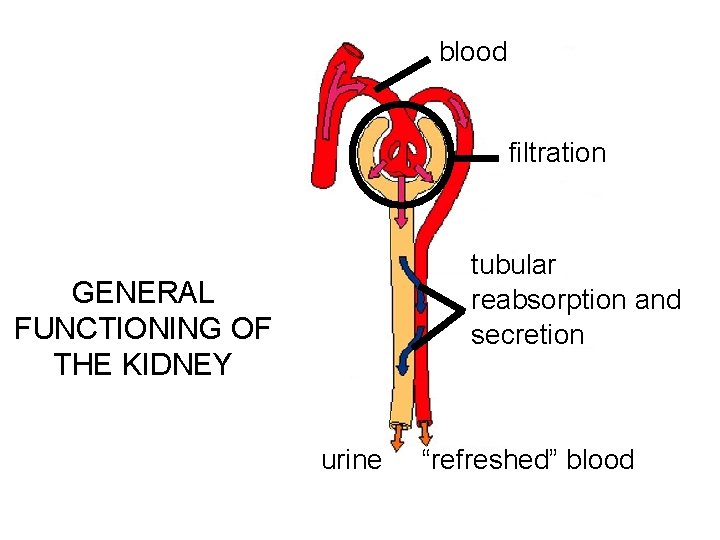
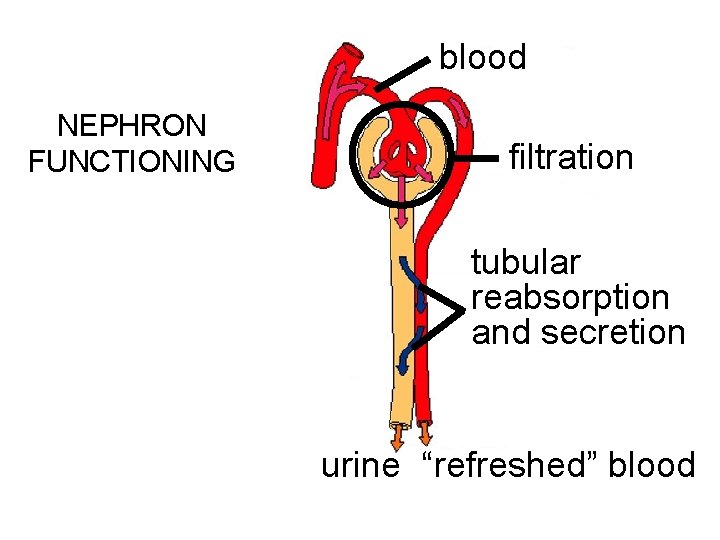
blood filtration tubular reabsorption and secretion GENERAL FUNCTIONING OF THE KIDNEY urine “refreshed” blood

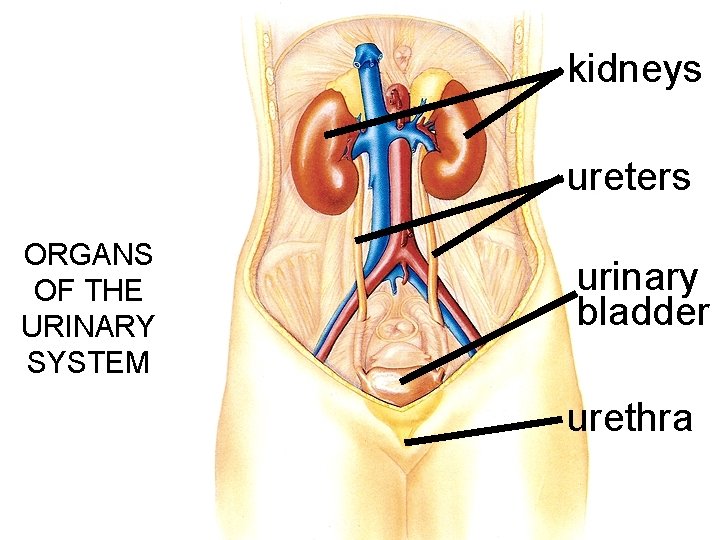
kidneys ureters ORGANS OF THE URINARY SYSTEM urinary bladder urethra

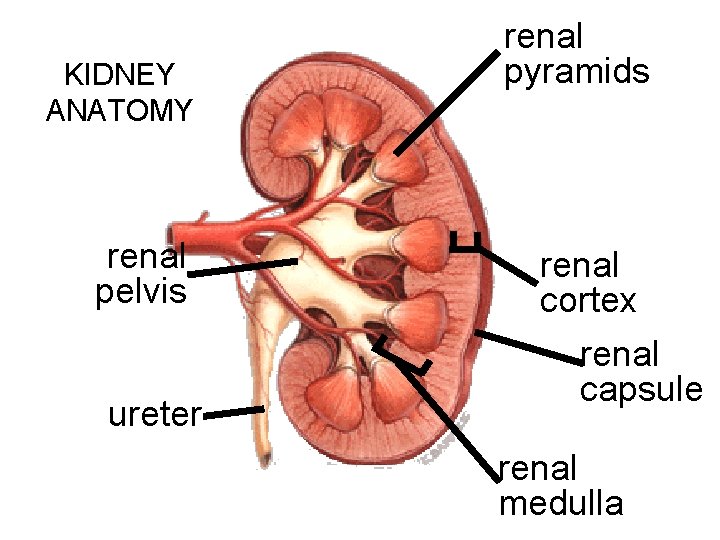
KIDNEY ANATOMY renal pelvis ureter renal pyramids renal cortex renal capsule renal medulla

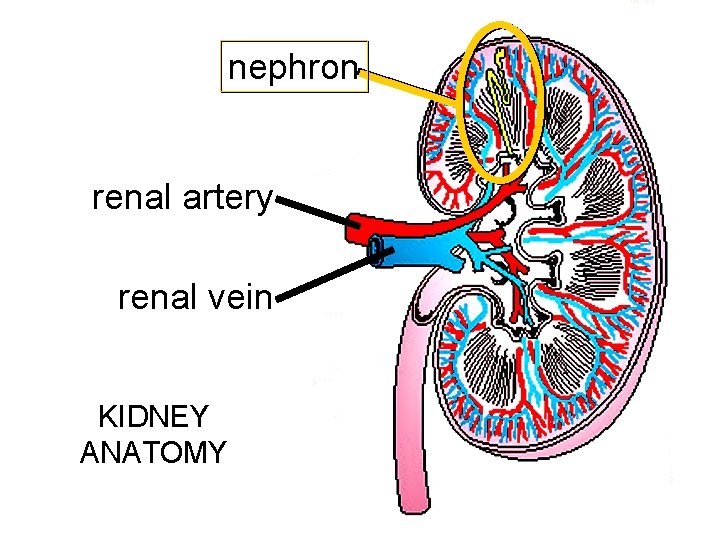
nephron renal artery renal vein KIDNEY ANATOMY

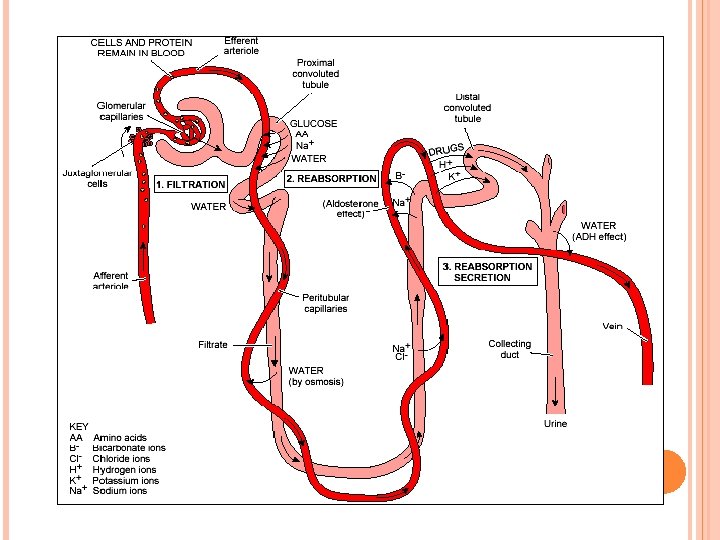
blood NEPHRON FUNCTIONING filtration tubular reabsorption and secretion urine “refreshed” blood

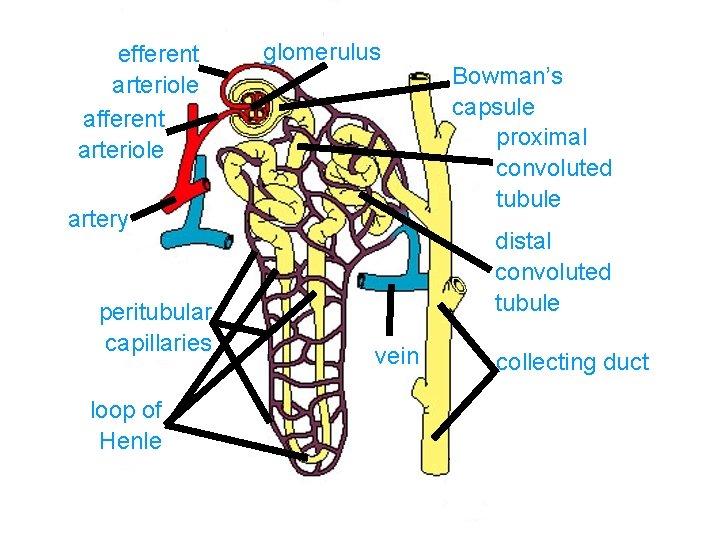
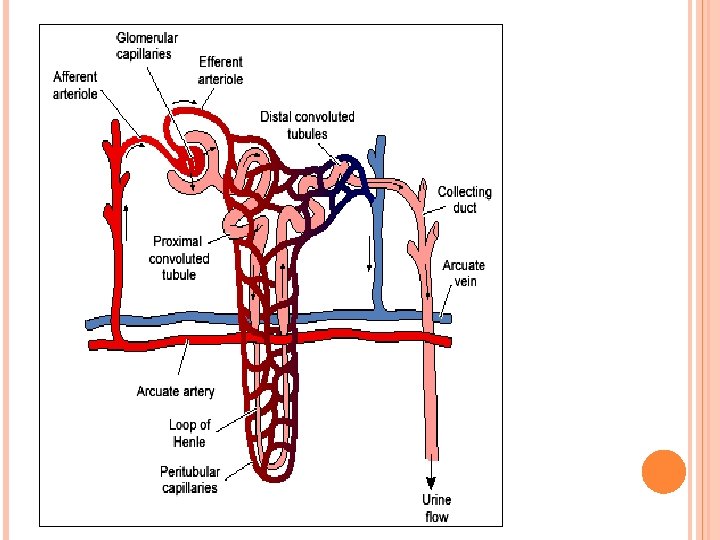
efferent arteriole afferent arteriole glomerulus artery peritubular capillaries loop of Henle Bowman’s capsule proximal convoluted tubule distal convoluted tubule vein collecting duct



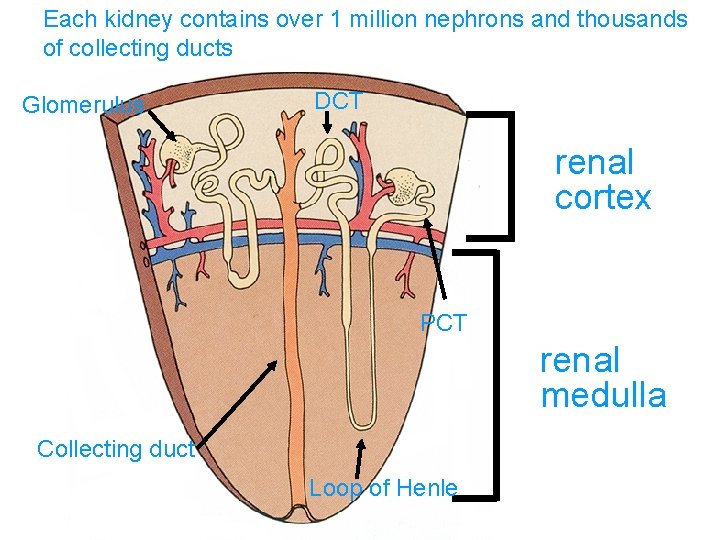
Each kidney contains over 1 million nephrons and thousands of collecting ducts Glomerulus DCT renal cortex PCT renal medulla Collecting duct Loop of Henle

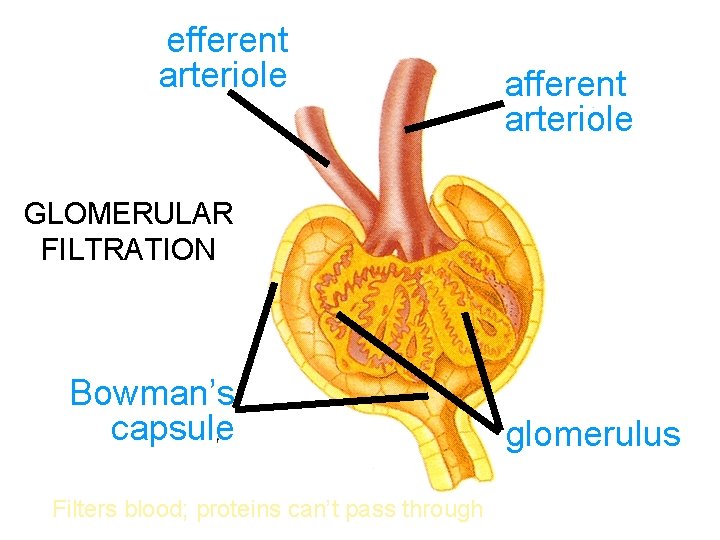
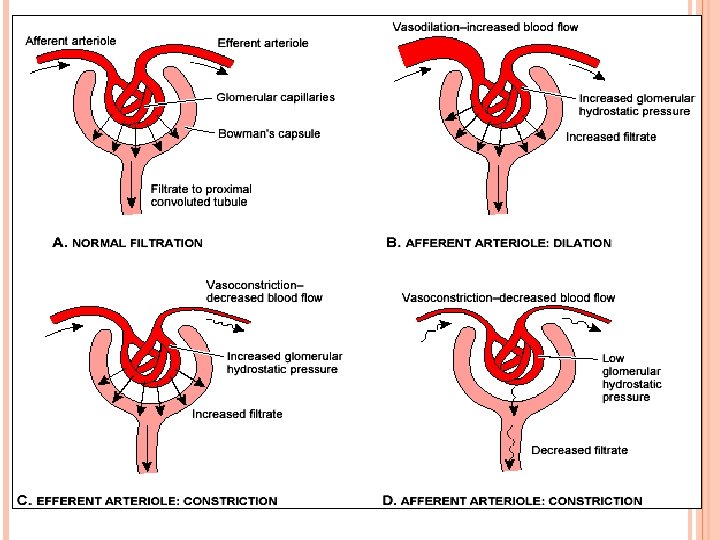
efferent arteriole afferent arteriole GLOMERULAR FILTRATION Bowman’s capsule Filters blood; proteins can’t pass through glomerulus


COMPOSITION OF GLOMERULAR FILTRATE • • Water Small Soluble Organic Molecules • Mineral Ions

PROXIMAL CONVOLUTED TUBULE Reabsorbs: water, glucose, amino acids, and sodium. • • 65% of Na+ is reabsorbed 65% of H 2 O is reabsorbed 90% of filtered bicarbonate (HCO 3 -) 50% of Cl- and K+

LOOP OF HENLE Creates a gradient of increasing sodium ion concentration towards the end of the loop within the interstitial fluid of the renal pyramid. • 25% Na+ is reabsorbed in the loop • 15% water is reabsorbed in the loop • 40% K is reabsorbed in the loop

DISTAL CONVOLUTED TUBULE Under the influence of the hormone aldosterone, reabsorbs sodium and secretes potassium. Also regulates p. H by secreting hydrogen ion when p. H of the plasma is low. • only 10% of the filtered Na. Cl and 20% of water remains

COLLECTING DUCT Allows for the osmotic reabsorption of water. ADH (antidiuretic hormone)- makes collecting ducts more permeable to water- produce concentrated urine

Urine Water- 95% Nitrogenous waste: • urea • uric acid • creatinine Ions: • sodium • potassium • sulfate • phosphate From the original 1800 g Na. Cl, only 10 g appears in the urine

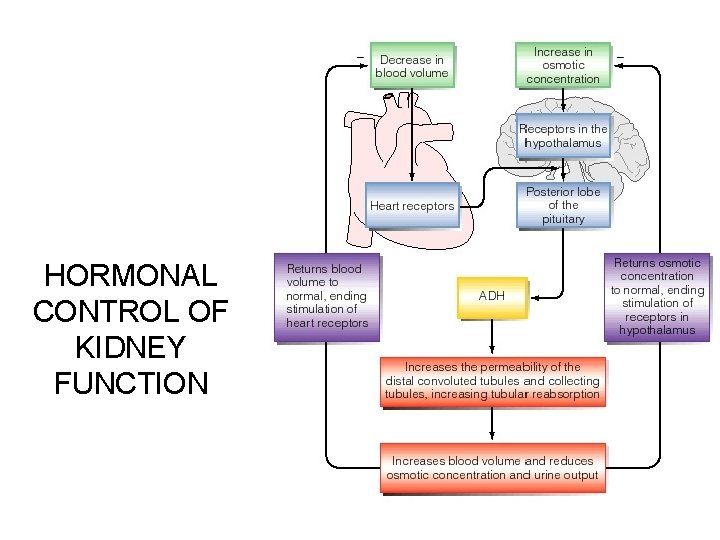
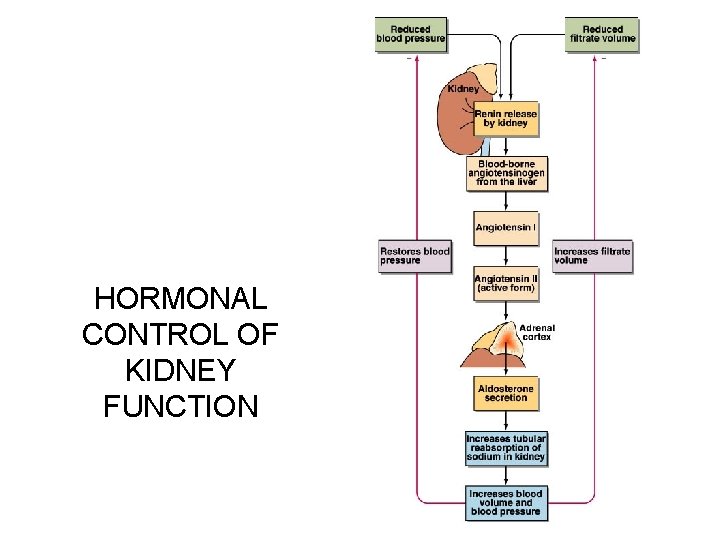
HORMONAL CONTROL OF KIDNEY FUNCTION

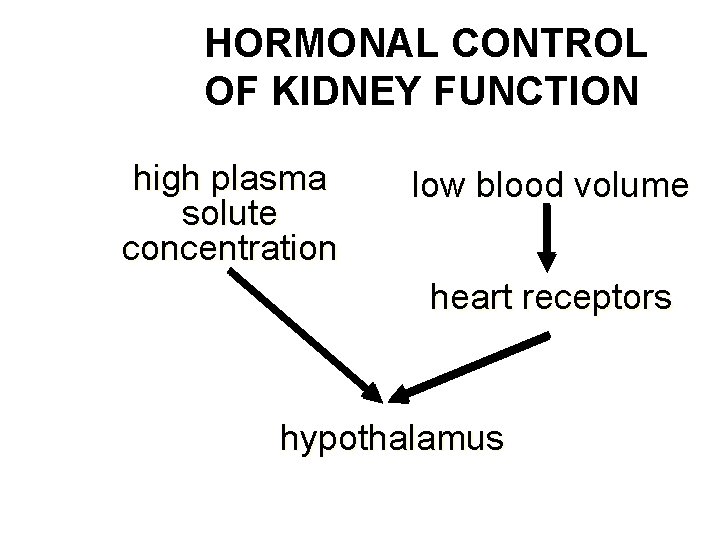
HORMONAL CONTROL OF KIDNEY FUNCTION high plasma solute concentration low blood volume heart receptors hypothalamus

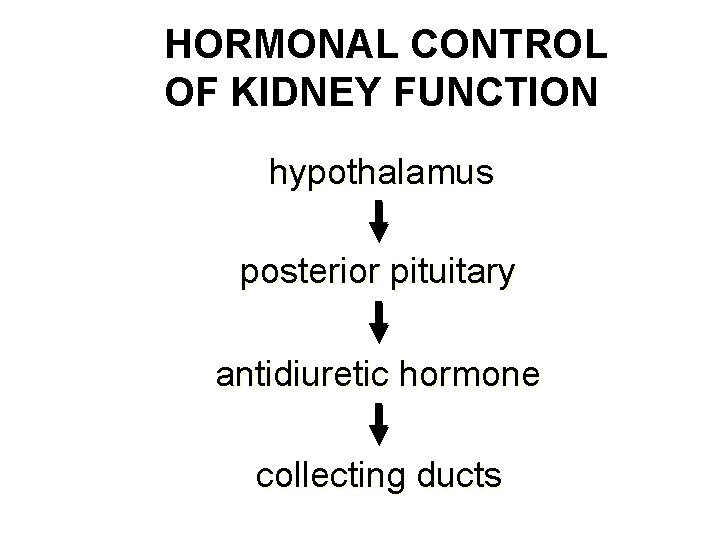
HORMONAL CONTROL OF KIDNEY FUNCTION hypothalamus posterior pituitary antidiuretic hormone collecting ducts

HORMONAL CONTROL OF KIDNEY FUNCTION

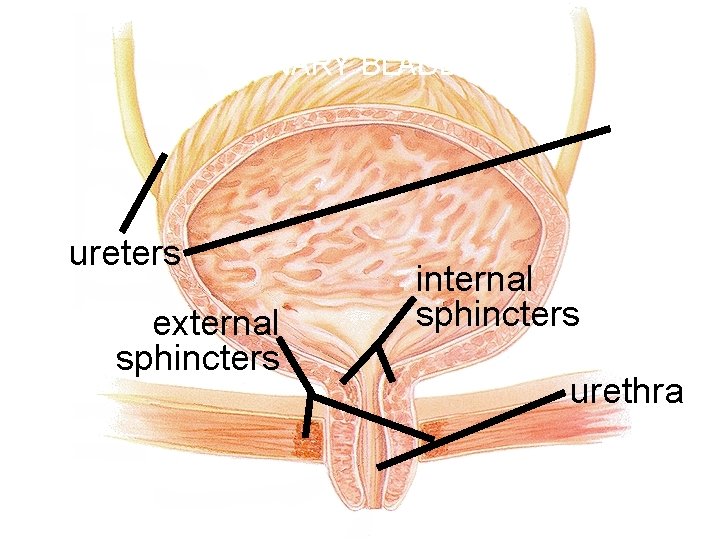
URINARY BLADDER ureters external sphincters internal sphincters urethra

Bladder 1. Mucosa (transitional epithelium) 2. Muscular layer (detrusor muscle): 3 layers of smooth muscle 3. Fibrous adventia

Sphincter Muscles on Bladder Internal urethral sphincter: • Smooth muscle • Involuntary control • More superiorly located External Urethral sphincter: • Skeletal muscle • Voluntary control • Posteriorly located

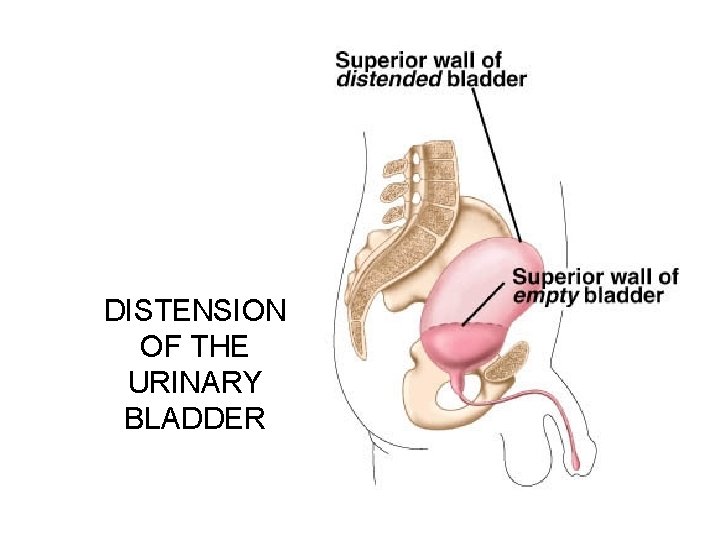
Diuresis (Micturition) When bladder fills with 200 ml of urine, stretch receptors transmit impulses to the CNS and produce a reflex contraction of the bladder (PNS)

DISTENSION OF THE URINARY BLADDER

Urinalysis characteristics: • smell- ammonia-like • p. H- 4. 5 -8, ave 6. 0 • specific gravity– more than 1. 0; ~1. 001 -1. 003 • color- affected by what we eat: salty foods, vitamins

Color- pigment is urochrome Yellow color due to metabolic breakdown of hemoglobin (by bile or bile pigments) Beets or rhubarb- might give a urine pink or smoky color Vitamins- vitamin C- bright yellow Infection- cloudy

Specific Gravity Water: s. g. = 1 g/liter; Urine: s. g. ~ 1. 001 to 1. 030 Pyelonephritus- urine has high s. g. ; form kidney stones Diabetes insipidus- urine has low s. g. ; drinks excessive water; injury or tumor in pituitary

Abnormal Constitutes of Urine Glucose- when present in urine condition called glycosuria (nonpathological) [glucose not normally found in urine] Indicative of: • Excessive carbohydrate intake • Stress • Diabetes mellitus

Abnormal Constitutes of Urine Albumin-abnormal in urine; it’s a very large molecule, too large to pass through glomerular membrane > abnormal increase in permeability of membrane Albuminuria- nonpathological conditionsexcessive exertion, pregnancy, overabundant protein intake-- leads to physiologic albuminuria Pathological condition- kidney trauma due to blows, heavy metals, bacterial toxin

Abnormal Constitutes of Urine Ketone bodies- normal in urine but in small amts Ketonuria- find during starvation, using fat stores Ketonuria is couples w/a finding of glycosuria-- which is usually diagnosed as diabetes mellitus RBC-hematuria Hemoglobinuria- due to fragmentation or hemolysis of RBC; conditions: hemolytic anemia, transfusion reaction, burns or renal disease

Abnormal Constitutes of Urine Bile pigments. Bilirubinuria (bile pigment in urine)- liver pathology such as hepatitis or cirrhosis WBCPyuria- urinary tract infection; indicates inflammation of urinary tract Casts- hardened cell fragments, cylindrical, flushed out of urinary tract WBC casts- pyelonephritus RBC casts- glomerulonephritus Fatty casts- renal damage

URINARY TRACT DISORDERS OVERALL OUTLINE Incontinence & retention UTI’s Inflammatory disorders Nephrotic syndrome Urinary tract obstruction Stones Hydronephrosis Tumors Renal cell carcinoma Bladder cancer Congenital disorders Polycystic kidneys Wilm’s tumor (nephroblastoma) Renal failure Acute Chronic Dialysis

INCONTINENCE, RETENTION, & CATHETERS Urinary Incontinence Loss of voluntary control of bladder Frequently called “neurogenic bladder” Many causes Enuresis = involuntary control after age 4 or 5 Types: Stress Urge Overflow Urinary retention Called “residual urine” Causes : Anatomical defects Neurogenic defects Treated with “catheterization”

Urinary Tract Infections Urethritis; Cystitis; Pyelonephritis Etiology Ascending infection ----- women > men Prostatic hypertrophy with urinary retention Incomplete emptying of bladder with urinary stasis Blood borne pathogens Pathophysiology of UTI’s Dysuria, urgency, & nocturia Systemically get fever & malaise CVA tenderness in pyelonephritis

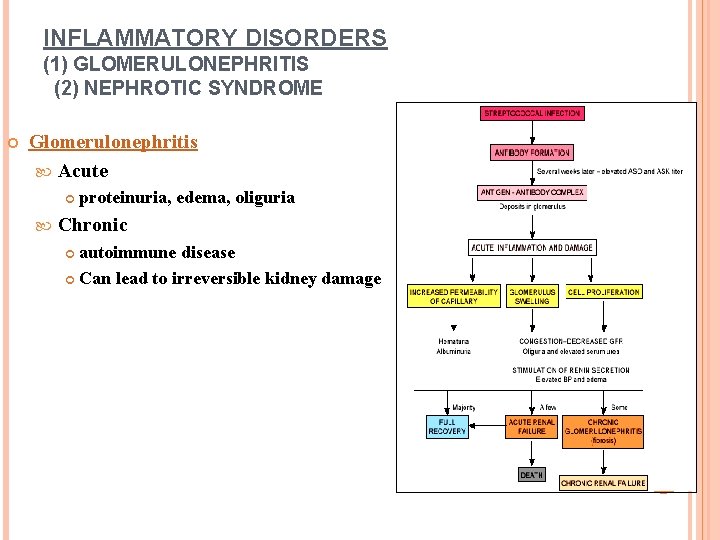
INFLAMMATORY DISORDERS (1) GLOMERULONEPHRITIS (2) NEPHROTIC SYNDROME Glomerulonephritis Acute proteinuria, edema, oliguria Chronic autoimmune disease Can lead to irreversible kidney damage

• Nephrotic Syndrome – Glomerular disorder where one loses the capacity to retain protein, especially albumin – Symptoms – severe edema (anasarca) * can get skin breakdown since impaired arterial flow – proteinuria – hypoalbuminemia – oliguria – Etiol: » Toxic agents (lead, mercury) » Toxic drugs (aminoglycosides) » Diseases (diabetes, lupus » Key = any significant problem with the glomerulus can lead to nephrotic syndrome

OBSTRUCTIVE DISORDERS Renal Calculi (kidney stones) Causes: Calcium, Uric acid, Urine crystals Symptoms: renal colic, N&V, chills, fever Risk factors: prolong dehydration, prolong immobilization, infection Treatment: surgery, lithotripsy Anomalies Strictures Kinks Ptosis Pelvic kidney Tumors Note that primary symptom = hematuria Renal Cell Ca = most common, unilateral, adeno Ca from tubular epithelium See picture Bladder Ca = usually from transitional epithelium Neurogenic bladder

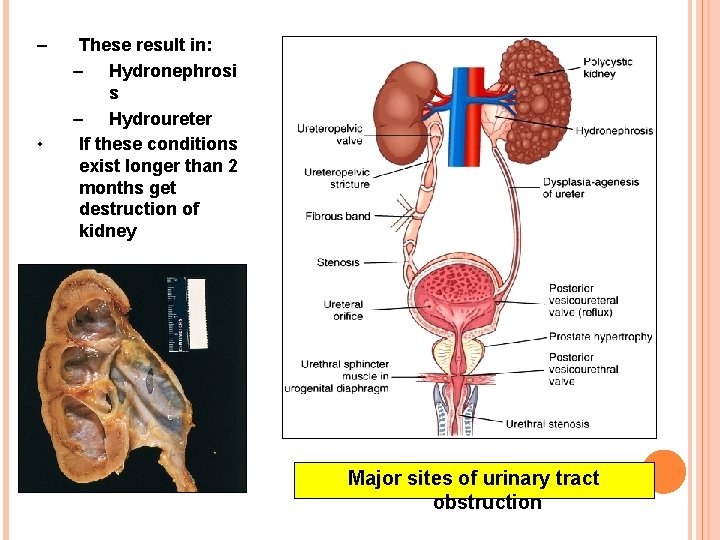
– • These result in: – Hydronephrosi s – Hydroureter If these conditions exist longer than 2 months get destruction of kidney Major sites of urinary tract obstruction

Congenital Diseases • Vesicoureteral reflux • Due to ectopic insertion of ureter into bladder. If far away from trigone, do not get adequate compression of ureter when voiding & get reflux • Incidence: 1/1000 • If one gets it each sibling(to be) has 50% incidence • Girls> boys; 10: 1 ratio • Ectopic kidney • • May get kinking of ureter • Usually in pelvis • Asymptomatic Renal agenesis • Usually unilateral & left kidney • 2 types: (1) occurs randomly (2) genetic • Asymptomatic • Remaining kidney becomes large since compensatory hypertrophy

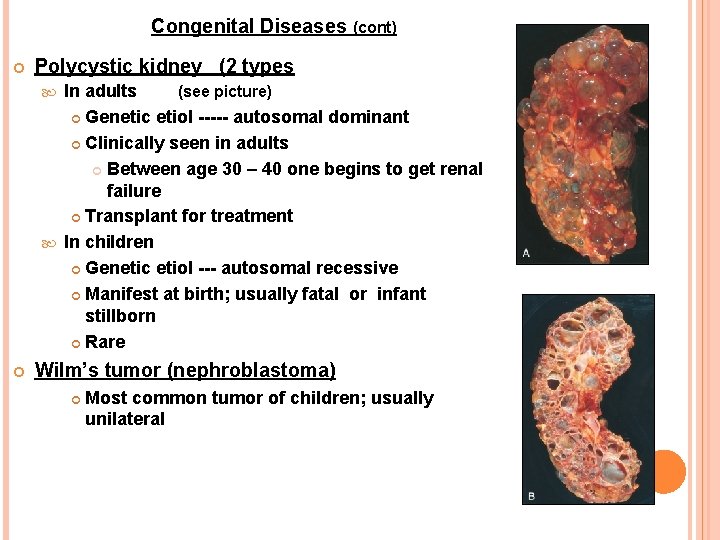
Congenital Diseases (cont) Polycystic kidney (2 types In adults (see picture) Genetic etiol ----- autosomal dominant Clinically seen in adults Between age 30 – 40 one begins to get renal failure Transplant for treatment In children Genetic etiol --- autosomal recessive Manifest at birth; usually fatal or infant stillborn Rare Wilm’s tumor (nephroblastoma) Most common tumor of children; usually unilateral

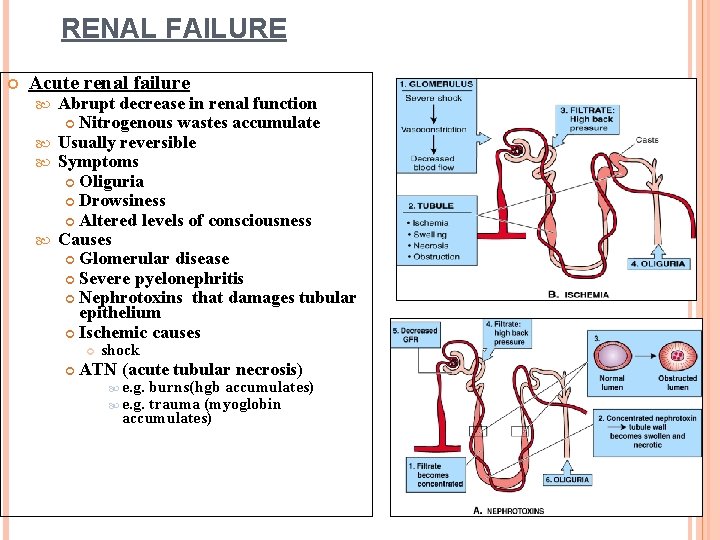
RENAL FAILURE Acute renal failure Abrupt decrease in renal function Nitrogenous wastes accumulate Usually reversible Symptoms Oliguria Drowsiness Altered levels of consciousness Causes Glomerular disease Severe pyelonephritis Nephrotoxins that damages tubular epithelium Ischemic causes shock ATN (acute tubular necrosis) e. g. burns(hgb accumulates) e. g. trauma (myoglobin accumulates)

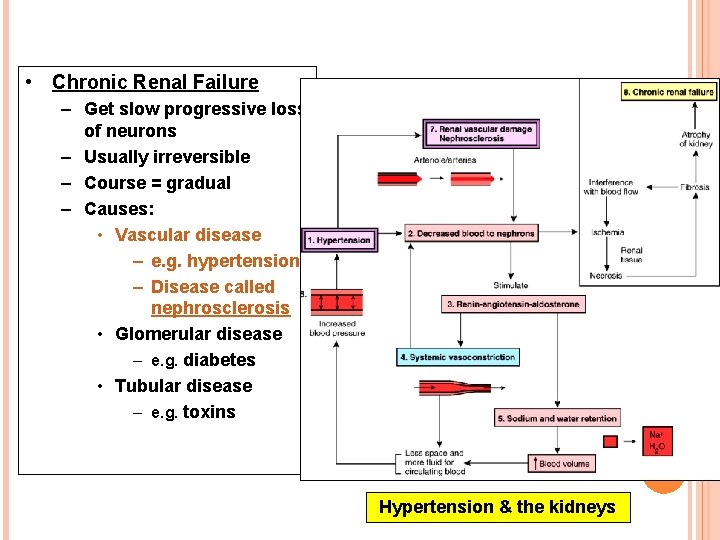
• Chronic Renal Failure – Get slow progressive loss of neurons – Usually irreversible – Course = gradual – Causes: • Vascular disease – e. g. hypertension – Disease called nephrosclerosis • Glomerular disease – e. g. diabetes • Tubular disease – e. g. toxins Hypertension & the kidneys

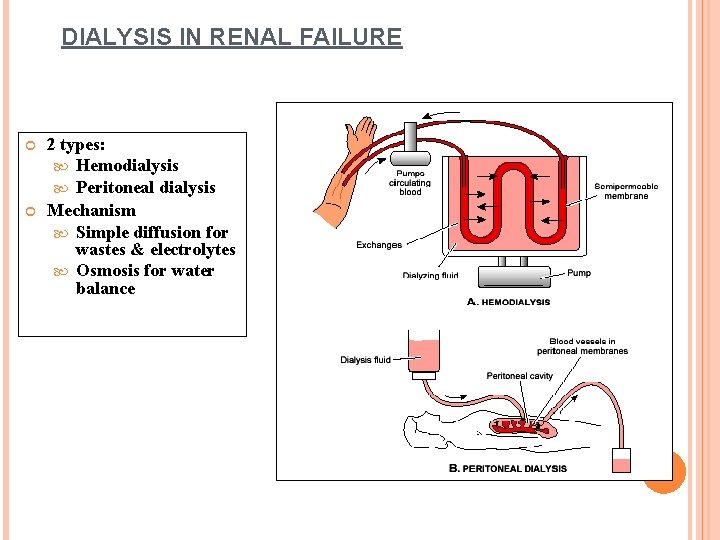
DIALYSIS IN RENAL FAILURE 2 types: Hemodialysis Peritoneal dialysis Mechanism Simple diffusion for wastes & electrolytes Osmosis for water balance