The Urinary System Differences bw Children and Adults

The Urinary System Differences b/w Children and Adults Nephrotic Syndrome Anthony Ly, Khanh. Ly Luong, Thai Nguyen, Thao Tran, Vy Tran

Primary functions Maintain body homeostatic • Regulating blood pressure, blood volume, osmolarity and composition of extra cellular fluid • Produce hormone such as : renin, calcitrol and erythropoietin • Regulating plasma ion concentrations • Acid-base balance

Primary Functions Continued Filter blood Detoxify superoxides, free radicals, and drugs. Excretion • Removal of organic waste products from body fluids such as: urea, uric acid, creatine, creatinine, ammonia Elimination waste products through urine
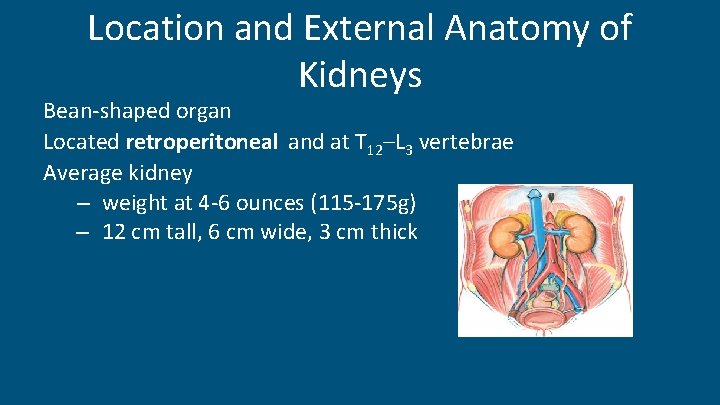
Location and External Anatomy of Kidneys Bean-shaped organ Located retroperitoneal and at T 12–L 3 vertebrae Average kidney – weight at 4 -6 ounces (115 -175 g) – 12 cm tall, 6 cm wide, 3 cm thick

Hilus – Located on concave surface – renal nerves and blood vessels enter and exit Renal capsule : thin layer cover the kidney – serve as protector and shock absorber • The renal parenchyma is divided into an outer cortex and inner medulla
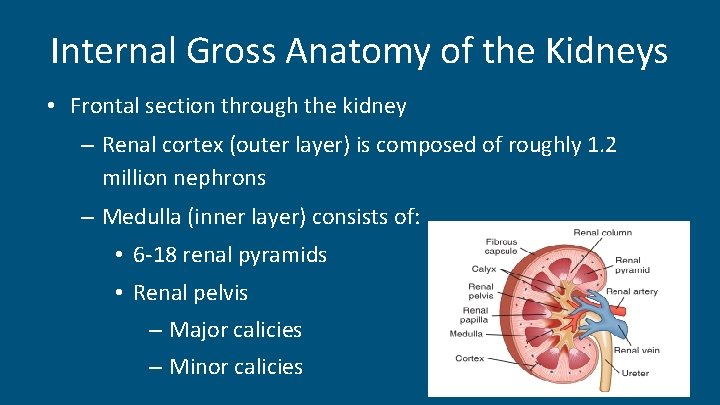
Internal Gross Anatomy of the Kidneys • Frontal section through the kidney – Renal cortex (outer layer) is composed of roughly 1. 2 million nephrons – Medulla (inner layer) consists of: • 6 -18 renal pyramids • Renal pelvis – Major calicies – Minor calicies
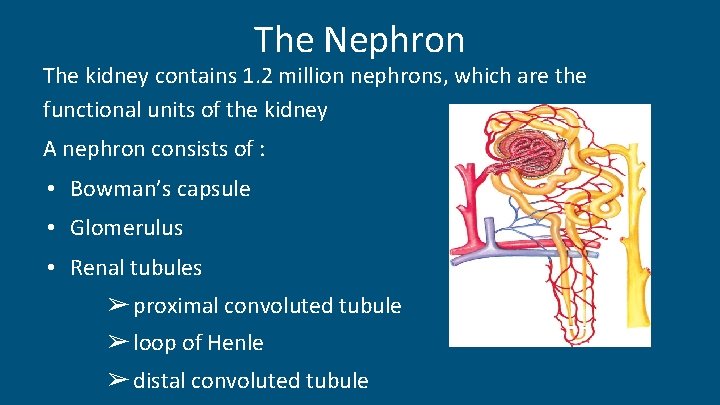
The Nephron The kidney contains 1. 2 million nephrons, which are the functional units of the kidney A nephron consists of : • Bowman’s capsule • Glomerulus • Renal tubules ➢ proximal convoluted tubule ➢ loop of Henle ➢ distal convoluted tubule

Summary of Nephron Function Each segment of nephron and collecting system contribute – Glomerulus – Proximal convoluted tubule (PCT) – Loop of Henle • Descending limb • Thick ascending limb – Distal convoluted tubule (DCT) and collecting ducts Concentrated urine produced after considerable modification of filtrate

Glomerulus • Selective filtration • Glomerular Filtration Rate (GFR) is the amount of filtrate formed per minute by the two kidneys combined. • • GFR is about 125 ml/min (on average) equivalent 180 L/day. 99% of the filtrate is reabsorbed, so that only 1 -2 L of urine per day is excreted.

Proximal convoluted tubule • Actively reabsorbs of 80% nutrients, plasma proteins electrolytes, water, glucose, HCO 3 - and amino acids from filtrate • Secretion: H+ and creatinine

Loop of Henle • Reabsorption: – Sodium in ascending loop – Water in descending loop – Concentration of filtrate

Distal convoluted tubule • Actively secretes ions (potassium, hydrogen iron), ammonia, toxins, and drugs • Reabsorbs water (regulate by ADH) and HCO 3 • Regulation of Ca 2+, PO 4 - (by parathyroid hormone), Na+, K+ (by aldosterone)

Collecting duct • Reabsorption of water (ADH required) • Collecting tubules receive urine from distal convoluted tubules

In summary Urinary System- The Nephron

Differences between children and adults -Kidney begins to develop within the 1 st weeks of embryonic life. - Completed at the end of the 1 st year after birth - Nephrons reach their full complement by birth - Kidneys continue to grow in size until body growth is complete in adolescence
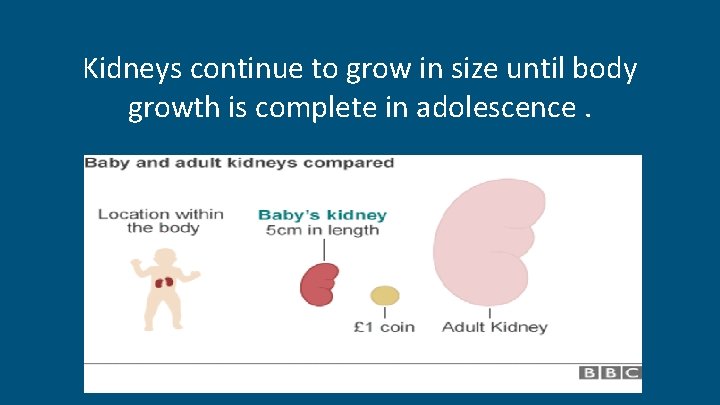
Kidneys continue to grow in size until body growth is complete in adolescence.
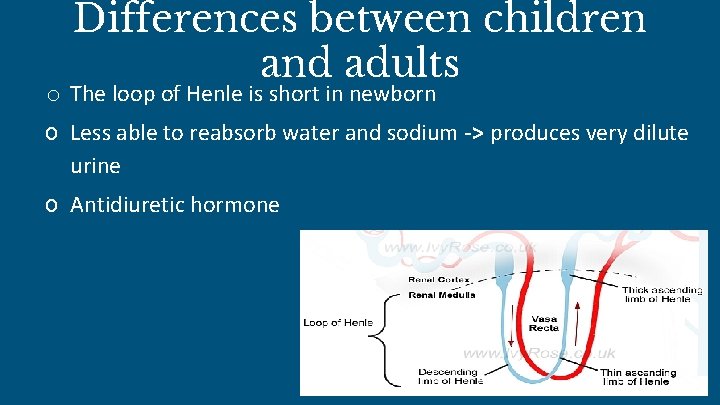
Differences between children and adults o The loop of Henle is short in newborn o Less able to reabsorb water and sodium -> produces very dilute urine o Antidiuretic hormone
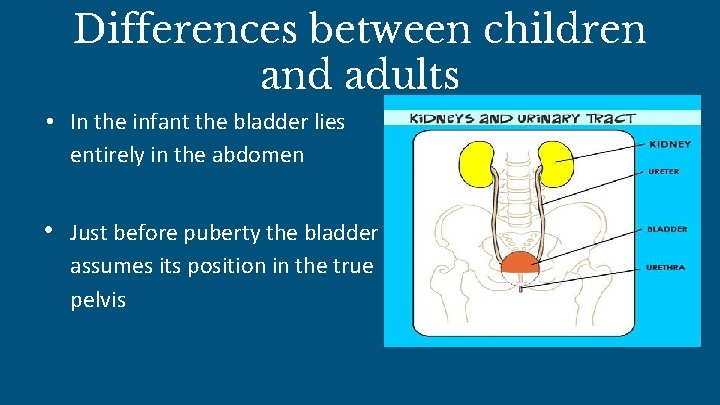
Differences between children and adults • In the infant the bladder lies entirely in the abdomen • Just before puberty the bladder assumes its position in the true pelvis

Differences between children and adults • Renal function in early infancy: • Glomerular filtration & absorption are low • Do not reach adult values until 1 -2 years of age -> inability to excrete excess water & solutes

Renal function in early infancy • Urea synthesis & excretion are slower - Retain large amount of nitrogen & electrolytes • Hydrogen ion excretion, acid secretion & bicarbonate levels are lower - Newborn is prone to develop severe metabolic acidosis • Kidneys are less able to adapt to sodium deficiencies & excesses - Prone to dehydration & fluid overload

Renal function in early infancy • During infancy the bladder is emptied spontaneously • Gain control of detrusor & sphincter function by 4 years of age

Clinical Manifestations - The presenting complaints and their significance vary with ages

Laboratory Tests • Blood studies & routine urinalysis • GFR • Creatinine • BUN, urine specific gravity, protein, glucose, ketones

Nursing Care Management • Assessment • Observe any manifestations • Weight, intake & output, and blood pressure • Preparing children & parents for test, urine collection & blood specimen • Assist with more complex diagnostic tests: - Radiography, cystoscopy

Nephrotic Syndrome - Glomerular disorders -> Increased glomerular permeability to plasma protein -> massive urinary protein loss. - Massive proteinuria , hypoalbuminemia, hyperlipidemia, & edema
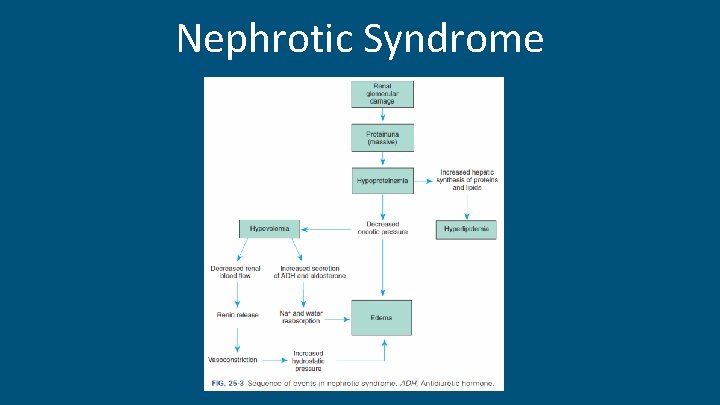
Nephrotic Syndrome
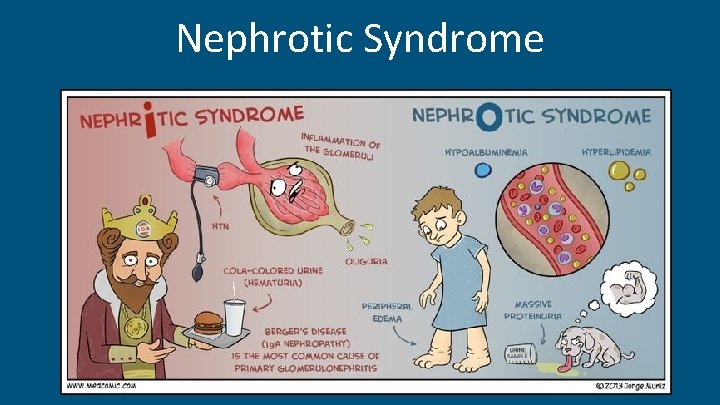
Nephrotic Syndrome

Etiology • Primary glomerular disease - Glomerulonephritis - Inherited - Autoimmune • External causes - Infection - Neoplasm - Drugs

Types of Nephrotic Syndrome • Minimal Change Nephrotic Syndrome (MCNS) - 80% of cases in preschool children - Cause is unknown - Precipitating factor: viral upper respiratory tract infection

Types of Nephrotic Syndrome • Secondary Nephrotic Syndrome - Related to glomerular damage ( acute or chronic glomerulonephritis) - Result of toxicity to drugs - Major presenting symptoms of renal dz in pedi pts with AIDS

Types of Nephrotic Syndrome • Congenital Nephrotic Syndrome - Autosomal recessive gene - Small for gestational age - If the infant does not receive dialysis or a successful kidney transplant, death in the 1 st year or 2 is possible

Diagnostic Evaluation • H& P manifestations • Urinalysis: massive proteinuria, hyaline casts, high specific gravity • Blood studies: hypoalbuminemia, hyperlipidemia, high platelet count • Renal biopsy – glomerular status & type of nephrotic syndrome

Manifestations • Puffiness of face, eyes, abdomen, genitalia and extremities • Apparent on arising in morining, subside during the day • Massive protein in urine • Hypertension • Hyperlipidemia • Hypoalbuminemia • Labs: Albumin, Total Protein, Calcium , Cholesterol

Therapeutic Management • • Relieve edema: ACE inhibitor, diuretics Diet: low- moderate protein, low sodium High cholesterol: lovastatin Prednisone: Inflammation ( prime therapeutic agents) - Initial episode should be at least 3 months - Complications: infection, growth retardation, obesity, HTN, GI bleeding, hyperglycemia - MCNS relapse 1 to 3 x per year • Immunosuppressant therapy

Nursing Management • Major Nursing Intervention: edema - Assess by weighing daily, I&Os, - Measuring abdominal girth - Frequent small meals - Skin care - Teaching

Nursing Diagnostic ?

Nursing Diagnostic • Risk for infection • Impaired skin integrity • Imbalance nutrition

Self Assessment What electrolyte imbalances do you expect when a patient has kidney failure? Select all that apply A) K B) mg C) ca D) hco 3

Answer ABCD

Self Assessment Development of the kidney begins within the ________ of embryonic life but is not completed until about the end of ________.

Answer - First weeks ; 1 st year after birth

Self Assessment Hydrogen ion excretion is _______, acid secretion is _____ for the first year of life, and plasma bicarbonate levels are ______. Because of these inadequacies of the kidney and because of less efficient of blood buffers, the newborn is more prone to develop severe ________.
Answer - Reduced, lower. Metabolic acidosis

Self Assessment What procedure involves the insertion rigid or flexible tubed instrument through the urethra to examine the urinary bladder, obtain biopsies of the tumors, or other growth, and remove polyps? a. Renal transplantation b. Cystoscopy c. Lithotripsy d. Nephrolithotomy e. Catheterization

Answer Cystoscopy

Self Assessment The edema that occurs in nephrotic syndrome is due to: A. Increased hydrostatic pressure caused by sodium retention B. Decreased aldosterone secretion from adrenal insufficiency C. Increased fluid retention caused by decreased glomerular filtration D. Decreased colloidal osmotic pressure caused by loss of serum albumin

Answer D. Decreased colloidal osmotic pressure caused by loss of serum albumin

References Hockenberry, M. J. & Wilson, D. (2015). Wong’s Nursing Care of Infants and Children (10 th Ed. ). St. Louis: Mosby/Elsevie Lewis, S. L. , Dirksen S. R. , Keitkemper M. M. , &Bucher, L. (2014). Medical-Surgical Nursing: Assessment and Management of Clinical Problems (9 th Ed. ). St. Louis, MO: Mosby
- Slides: 48