The Urinary System By April Datu Angelique Delarazan

The Urinary System By: April Datu Angelique Delarazan
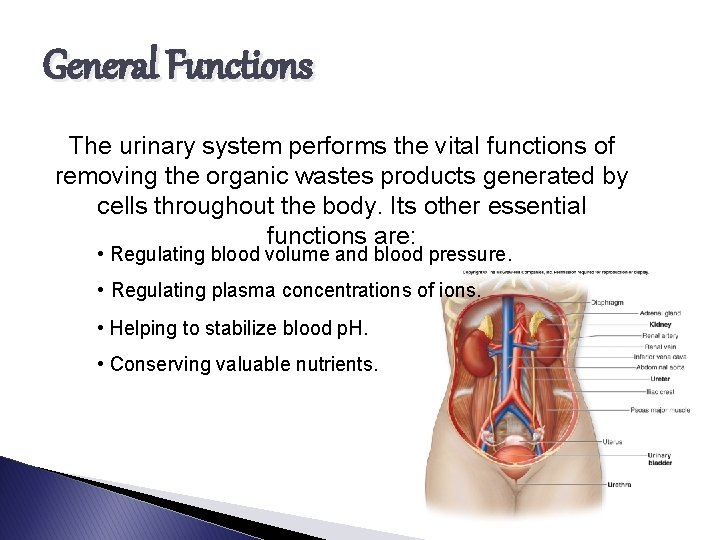
General Functions The urinary system performs the vital functions of removing the organic wastes products generated by cells throughout the body. Its other essential functions are: • Regulating blood volume and blood pressure. • Regulating plasma concentrations of ions. • Helping to stabilize blood p. H. • Conserving valuable nutrients.
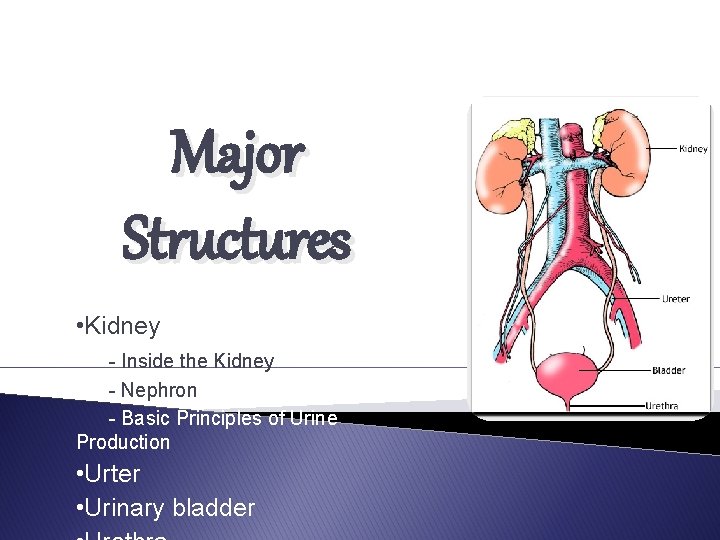
Major Structures • Kidney - Inside the Kidney - Nephron - Basic Principles of Urine Production • Urter • Urinary bladder
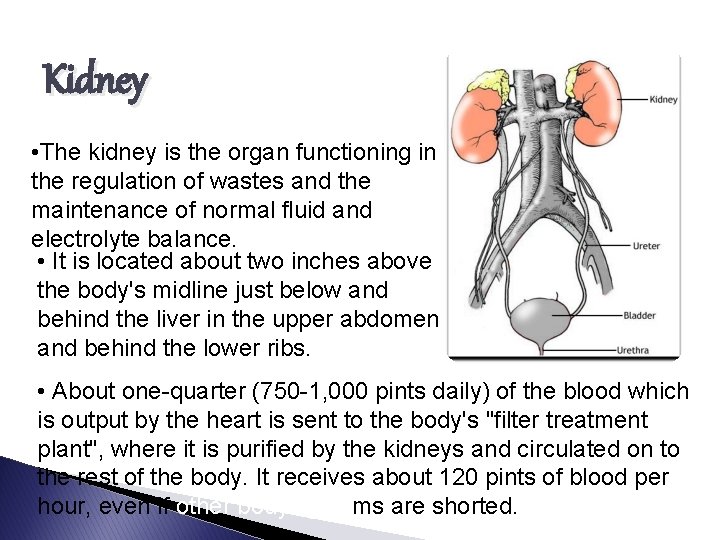
Kidney • The kidney is the organ functioning in the regulation of wastes and the maintenance of normal fluid and electrolyte balance. • It is located about two inches above the body's midline just below and behind the liver in the upper abdomen and behind the lower ribs. • About one-quarter (750 -1, 000 pints daily) of the blood which is output by the heart is sent to the body's "filter treatment plant", where it is purified by the kidneys and circulated on to the rest of the body. It receives about 120 pints of blood per hour, even if other body systems are shorted.
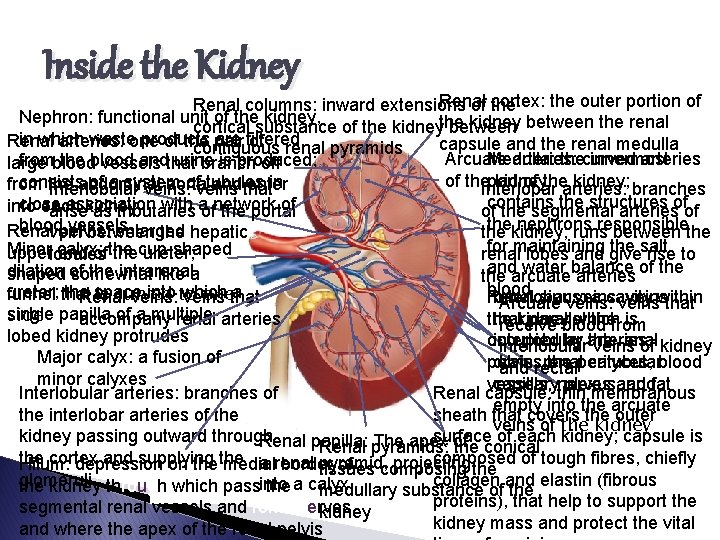
Inside the Kidney Renal cortex: the outer portion of Renal columns: inward extensions of the Nephron: functional unit of the kidney, kidney between the renal cortical substance of the kidneythe between in which wasteone products are filtered Renal arteries: of the pair of renal pyramids capsule and the renal medulla contiguous Arcuate Medulla: arteries: thecurved innermost arteries fromblood the blood andthat urine is produced; large vessels branch off of the. Interlobar part kidney of thearteries: kidney; branches consists of a system ofveins tubules in from the abdominal aorta and that enter Interlobular veins: the structures close association with aofnetwork of into each kidney arise as tributaries the portal ofcontains the segmental arteriesofof thekidney; nephrons responsible blood vessels Renal pelvis: enlarged vein between the hepatic the runs between the for maintaining the Minor calyx: upperlobules end ofthe thecup-shaped ureter; renal lobes and givesalt rise to andarcuate water balance dilation the intrarenal shaped of somewhat like a the arteries of the blood ureter; that the space into to which a funnel is curved onethat Renal veins: veins Renal Interlobar sinus: veins: a cavity veins within Arcuate veins: veins that single of a multipleside papilla accompany renal arteries the that kidney parallel which thefrom is receive blood lobed kidney protrudes occupied interlobular by arteries; the renal interlobular veins of kidney Major calyx: a fusion of pelvis, drains renal the peritubular calyces, blood and rectal minor calyxes vessels, capillarynerves plexus, andfat Interlobular arteries: branches of Renal capsule: thin membranous empty into the arcuate the interlobar arteries of the sheath that covers the outer veins of the kidney passing outward through surface of each kidney; capsule is Renal papilla: The apex of Renal pyramids: the conical the cortex and supplying composed of tough fibres, chiefly a renal pyramid, projecting Hilum: depression on the medial border of tissues composing the glomeruli. collagen and elastin (fibrous the kidney through which passinto the a calyx medullary substance of the proteins), that help to support the segmental renal vessels and renal nerves kidney mass and protect the vital and where the apex of the renal pelvis
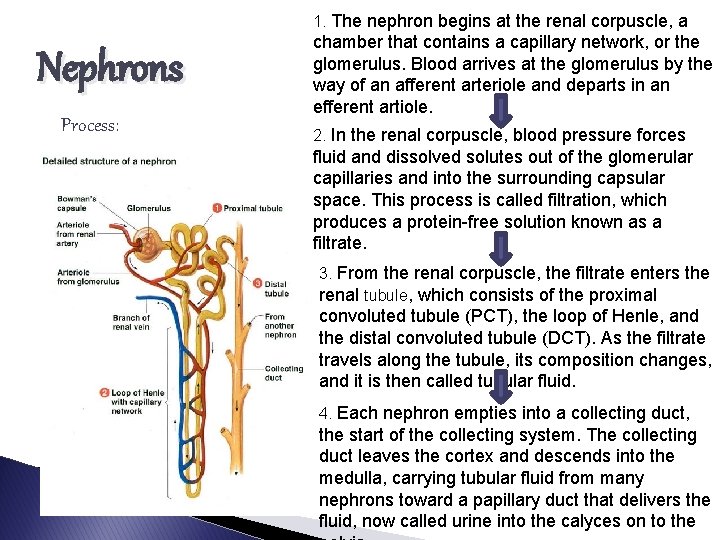
1. The nephron begins at the renal corpuscle, a Nephrons Process: chamber that contains a capillary network, or the glomerulus. Blood arrives at the glomerulus by the way of an afferent arteriole and departs in an efferent artiole. 2. In the renal corpuscle, blood pressure forces fluid and dissolved solutes out of the glomerular capillaries and into the surrounding capsular space. This process is called filtration, which produces a protein-free solution known as a filtrate. 3. From the renal corpuscle, the filtrate enters the renal tubule, which consists of the proximal convoluted tubule (PCT), the loop of Henle, and the distal convoluted tubule (DCT). As the filtrate travels along the tubule, its composition changes, and it is then called tubular fluid. 4. Each nephron empties into a collecting duct, the start of the collecting system. The collecting duct leaves the cortex and descends into the medulla, carrying tubular fluid from many nephrons toward a papillary duct that delivers the fluid, now called urine into the calyces on to the

Basic Principles of Urine Production The primary purpose of urine production is to maintain homeostasis by regulating the volume and compositing of the blood. This process involves the excretion of waste products. • Urea is the most abundant organic waste. • Creatinine is generated in skeletal muscle tissue through the breakdown of creatine phosphate, a highenergy compound that plays an important role in muscle contraction. • Uric acid is produced during the breakdown and recycling of RNA.

Basic Principles of Urine Production (continued) In the process of doing so, the kidneys ensure that the excreted urine does not contain organic substrates present in blood plasma. To accomplish these goals, the kidneys perform three distinct processes: • Secretion is • Reabsorption. • Filtration. In filtration, Reabsorption is the transport of solutes blood pressure forces removal of water and out of the peritubular water across the filtration solute molecules from capillaries, across the membrane in the renal the filtrate and their tubular epithelium, and corpuscle. Solute into the filtrate. This molecules small enough to reentry into the process is necessary circulation at the pass through the membrane are carried into peritubular capillaries. because filtration does not force all of the filtrate by the dissolved materials out surrounding molecules. of the blood.
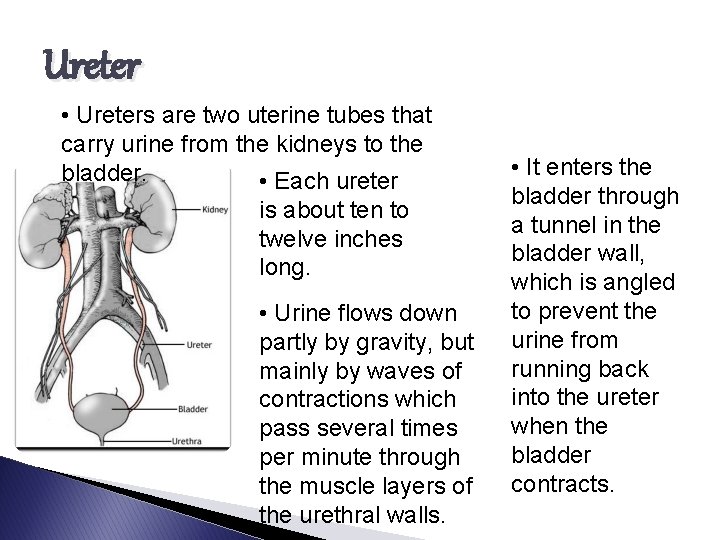
Ureter • Ureters are two uterine tubes that carry urine from the kidneys to the bladder. • Each ureter is about ten to twelve inches long. • Urine flows down partly by gravity, but mainly by waves of contractions which pass several times per minute through the muscle layers of the urethral walls. • It enters the bladder through a tunnel in the bladder wall, which is angled to prevent the urine from running back into the ureter when the bladder contracts.
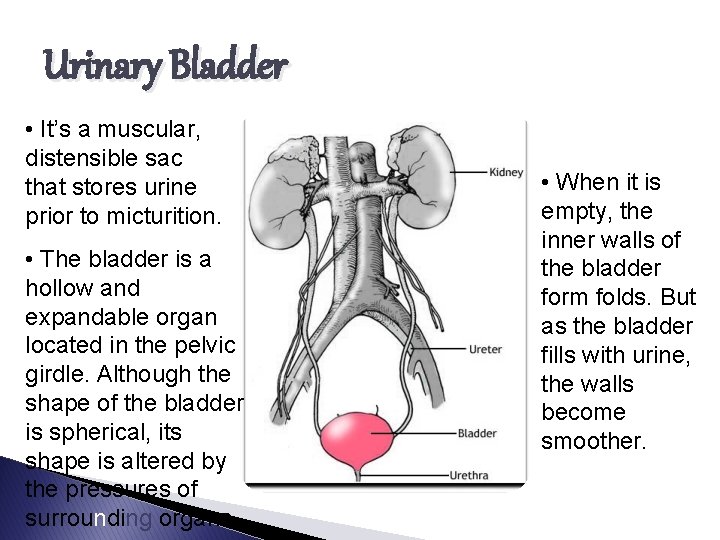
Urinary Bladder • It’s a muscular, distensible sac that stores urine prior to micturition. • The bladder is a hollow and expandable organ located in the pelvic girdle. Although the shape of the bladder is spherical, its shape is altered by the pressures of surrounding organs. • When it is empty, the inner walls of the bladder form folds. But as the bladder fills with urine, the walls become smoother.
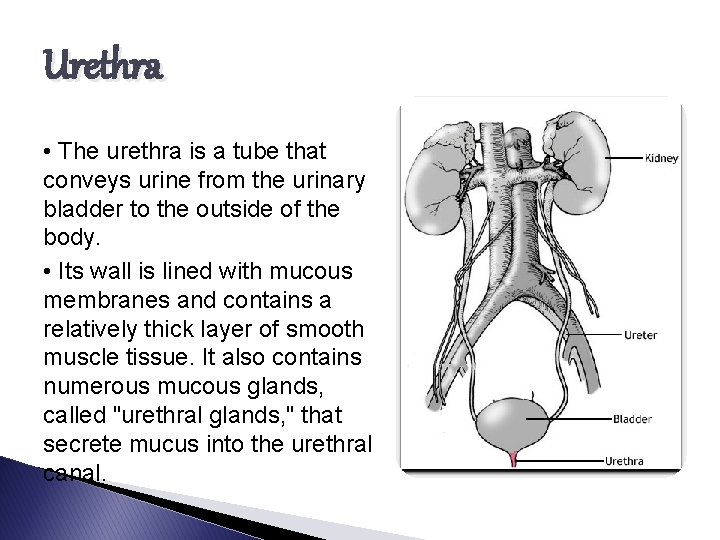
Urethra • The urethra is a tube that conveys urine from the urinary bladder to the outside of the body. • Its wall is lined with mucous membranes and contains a relatively thick layer of smooth muscle tissue. It also contains numerous mucous glands, called "urethral glands, " that secrete mucus into the urethral canal.

How It Works the kidneys, urine travels down two thin tubes called ureters to the bladder. Muscles in the ureter walls constantly tighten and relax to force urine downward away from the kidneys. 6. Nerves in the bladder tell you when it is time to urinate. The sensation to urinate becomes stronger as the bladder continues to fill and reaches its limit. At that point, nerves from the bladder send a message to the brain that the bladder is full, and the urge to empty the bladder intensifies. together with water and other waste substances, forms the urine as it in the passes through the nephrons and bloodstream to down the renal tubules of the kidneys. 5. Circular muscles called sphincters help keep urine 4. The urinary bladder from leaking. The swells into a round shape sphincter muscles close when it is full and gets tightly like a rubber band smaller when empty. around the opening of the bladder into the urethra. 1. Urea is carried 2. Urea, 3. From
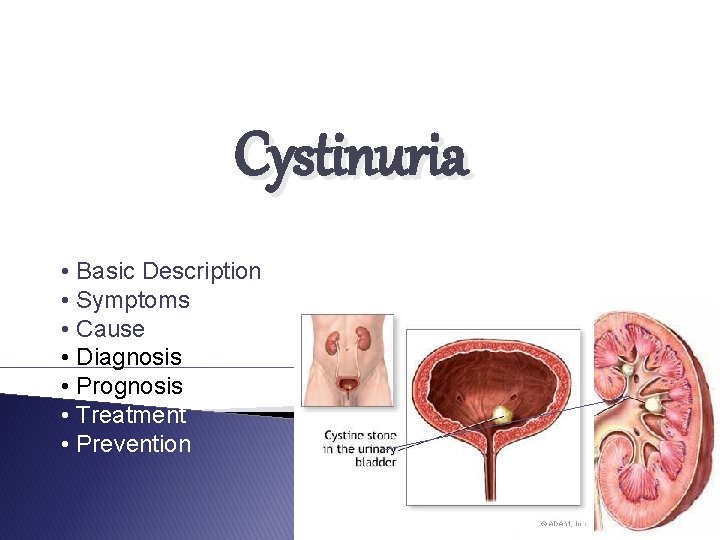
Cystinuria • Basic Description • Symptoms • Cause • Diagnosis • Prognosis • Treatment • Prevention
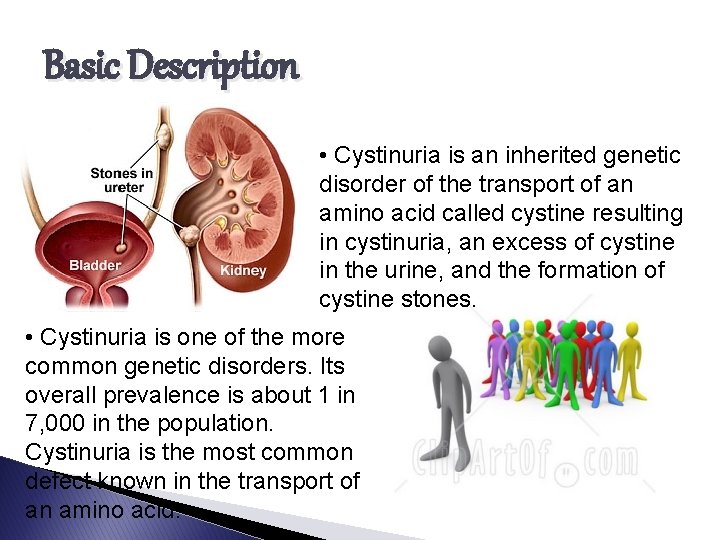
Basic Description • Cystinuria is an inherited genetic disorder of the transport of an amino acid called cystine resulting in cystinuria, an excess of cystine in the urine, and the formation of cystine stones. • Cystinuria is one of the more common genetic disorders. Its overall prevalence is about 1 in 7, 000 in the population. Cystinuria is the most common defect known in the transport of an amino acid.
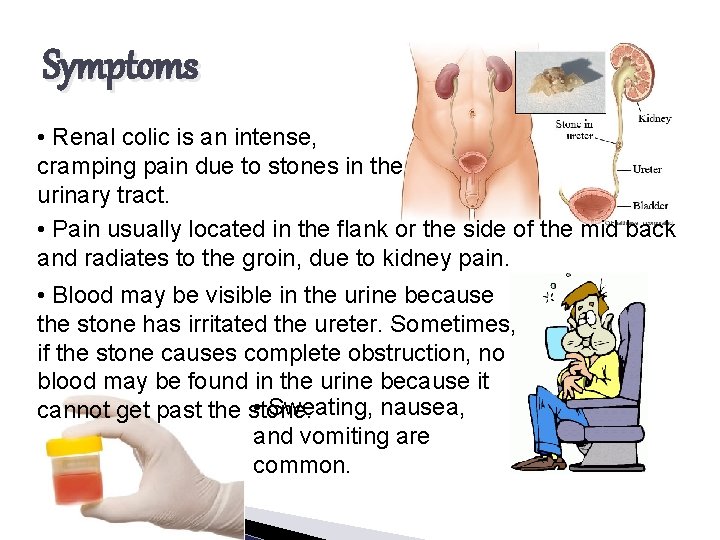
Symptoms • Renal colic is an intense, cramping pain due to stones in the urinary tract. • Pain usually located in the flank or the side of the mid back and radiates to the groin, due to kidney pain. • Blood may be visible in the urine because the stone has irritated the ureter. Sometimes, if the stone causes complete obstruction, no blood may be found in the urine because it • Sweating, nausea, cannot get past the stone. and vomiting are common.
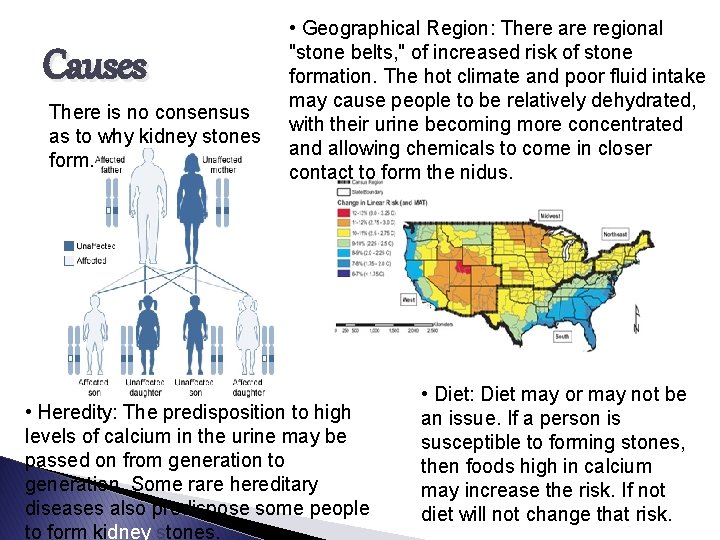
Causes There is no consensus as to why kidney stones form. • Geographical Region: There are regional "stone belts, " of increased risk of stone formation. The hot climate and poor fluid intake may cause people to be relatively dehydrated, with their urine becoming more concentrated and allowing chemicals to come in closer contact to form the nidus. • Heredity: The predisposition to high levels of calcium in the urine may be passed on from generation to generation. Some rare hereditary diseases also predispose some people to form kidney stones. • Diet: Diet may or may not be an issue. If a person is susceptible to forming stones, then foods high in calcium may increase the risk. If not diet will not change that risk.
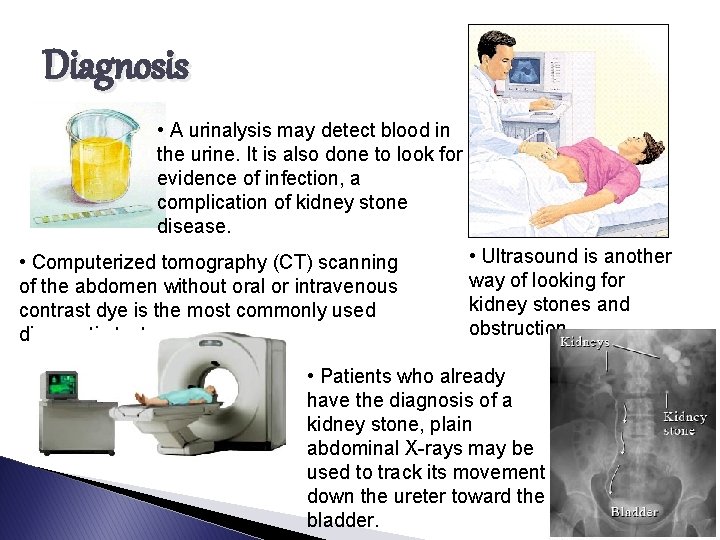
Diagnosis • A urinalysis may detect blood in the urine. It is also done to look for evidence of infection, a complication of kidney stone disease. • Computerized tomography (CT) scanning of the abdomen without oral or intravenous contrast dye is the most commonly used diagnostic test. • Ultrasound is another way of looking for kidney stones and obstruction. • Patients who already have the diagnosis of a kidney stone, plain abdominal X-rays may be used to track its movement down the ureter toward the bladder.

Prognosis • Cystinuria is a chronic, lifelong condition. Stones commonly return. However, the condition rarely results in kidney failure, and it does not affect other organs. “As many as 50% of patients who have had surgical treatment for a kidney stone will have another stone within five years if no medicines are used to treat — Dominic De Bellis, this condition. ” Ph. D
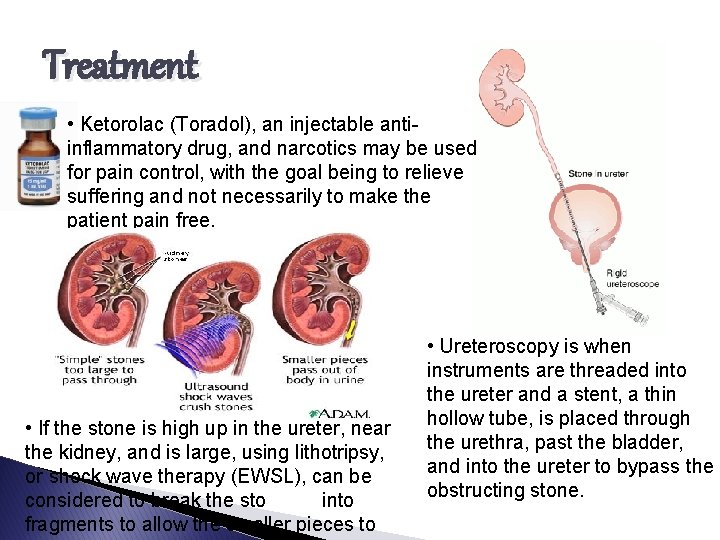
Treatment • Ketorolac (Toradol), an injectable antiinflammatory drug, and narcotics may be used for pain control, with the goal being to relieve suffering and not necessarily to make the patient pain free. • If the stone is high up in the ureter, near the kidney, and is large, using lithotripsy, or shock wave therapy (EWSL), can be considered to break the stone up into fragments to allow the smaller pieces to • Ureteroscopy is when instruments are threaded into the ureter and a stent, a thin hollow tube, is placed through the urethra, past the bladder, and into the ureter to bypass the obstructing stone.

Prevention • The risk of forming a stone can be minimized by avoiding dehydration. Keeping the urine dilute will not allow the chemical crystals to come out of solution and form the nidus of a stone. • Making certain that the urine remains clear and not concentrated will help minimize stone formation. • Medication may be prescribed for certain types of stones, and compliance with taking the medication is a must to reduce the risk of future episodes.

Bibliography • Martini, Frederic H. , and Bartholomew, Edwin F. . Essentials of Anatomy & Physiology. 4 th Ed. San Fransico, CA: Pearson Education, Inc. , 2007. • Campbell, Neil A. , Reece, Jane B. . AP* Edition Biology. 8 th Ed. San Fransico, CA: Pearson Benjamin Cummings, 2008. • “Your Urinary System and How It Works”. Niddk. August 2007. ‹http: //www. aresearchguide. com/12 biblio. html#c› • “Uriniary System”. Innerbody. 1993 -2010. ‹http: //www. innerbody. com/image/urinov. html › • “Cystinuria”. Medicinenet. 1996 -2010. ‹ http: //www. medicinenet. com/cystinuria/article. htm› • “Cystinura”. Wrong Diagnosis. 2010. ‹http: //www. wrongdiagnosis. com/c/cystinuria/intro. htm›

Thank you. The End
- Slides: 22