THE URINARY SYSTEM b III Physiology Urine IV
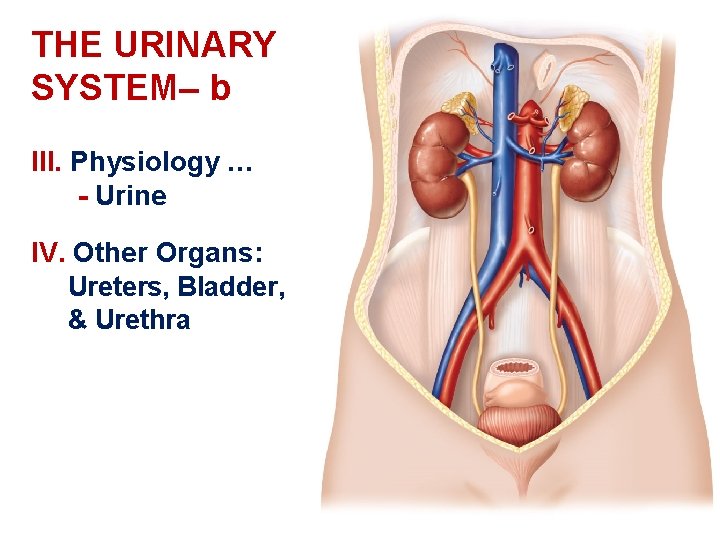
THE URINARY SYSTEM– b III. Physiology … - Urine IV. Other Organs: Ureters, Bladder, & Urethra
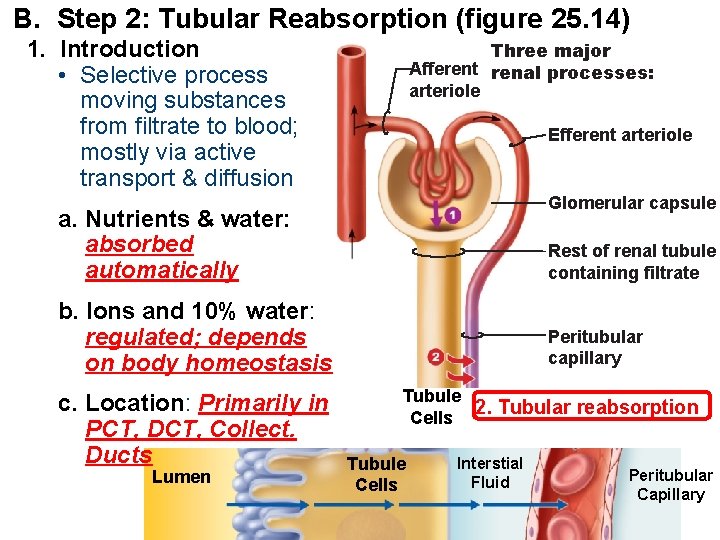
B. Step 2: Tubular Reabsorption (figure 25. 14) 1. Introduction • Selective process moving substances from filtrate to blood; mostly via active transport & diffusion Three major Afferent renal processes: arteriole Efferent arteriole Glomerular capsule a. Nutrients & water: absorbed automatically Rest of renal tubule containing filtrate b. Ions and 10% water: regulated; depends on body homeostasis c. Location: Primarily in PCT, DCT, Collect. Ducts Lumen Peritubular capillary Tubule 2. Tubular reabsorption Cells Tubule Cells Interstial Fluid Peritubular Capillary
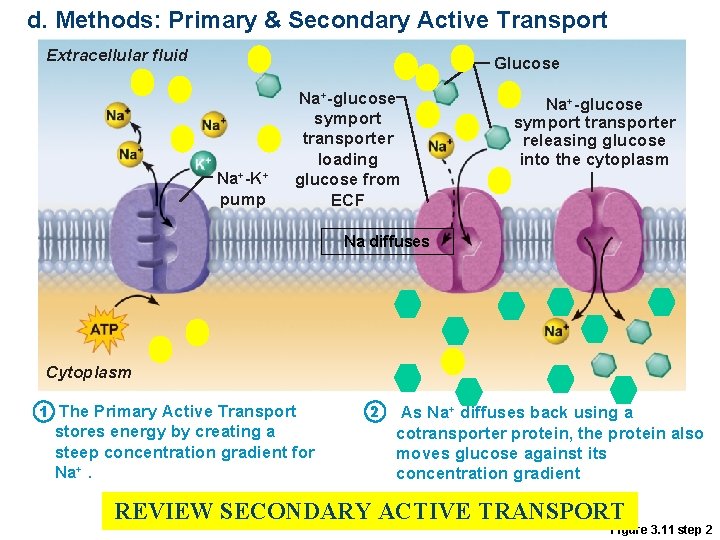
d. Methods: Primary & Secondary Active Transport Extracellular fluid Glucose Na+-K+ pump Na+-glucose symport transporter loading glucose from ECF Na+-glucose symport transporter releasing glucose into the cytoplasm Na diffuses Cytoplasm 1 The Primary Active Transport stores energy by creating a steep concentration gradient for Na+. 2 As Na+ diffuses back using a cotransporter protein, the protein also moves glucose against its concentration gradient REVIEW SECONDARY ACTIVE TRANSPORT Figure 3. 11 step 2
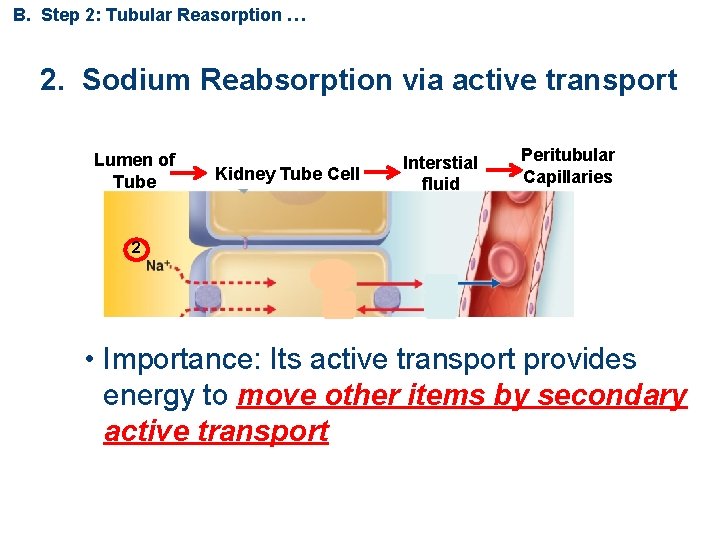
B. Step 2: Tubular Reasorption … 2. Sodium Reabsorption via active transport Lumen of Tube Kidney Tube Cell Interstial fluid Peritubular Capillaries 2 • Importance: Its active transport provides energy to move other items by secondary active transport

3. Reabsorption of Nutrients, Water, & ions Via Secondary Active Transport a. sodium diffuses in for step 2 and energy generated causes: b. Cotransport via Secondary Active Transport: Nutrients, Vitamins, some ions form Low to High • Then diffuse to peritubular capillaries 3 Lumen of Tube Kidney Tube Cell Peritubular Capillaries 2 3 Glucose Amino A. Vitamins Ions (some) • Transport Maximum (Tm) = maximum transport capacity due to Limited number of protein carriers/channels When saturated, excess is excreted in urine 1 sign of diabetes = glucose and ketones in urine
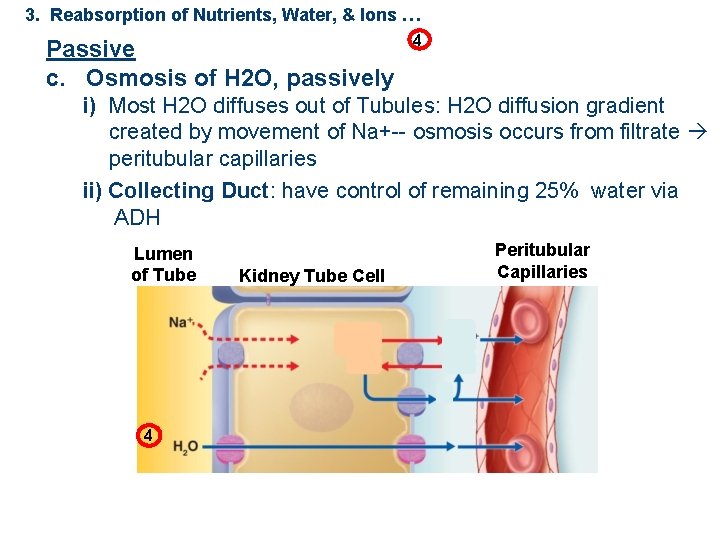
3. Reabsorption of Nutrients, Water, & Ions … Passive c. Osmosis of H 2 O, passively 4 i) Most H 2 O diffuses out of Tubules: H 2 O diffusion gradient created by movement of Na+-- osmosis occurs from filtrate peritubular capillaries ii) Collecting Duct: have control of remaining 25% water via ADH Lumen of Tube 4 Kidney Tube Cell Peritubular Capillaries
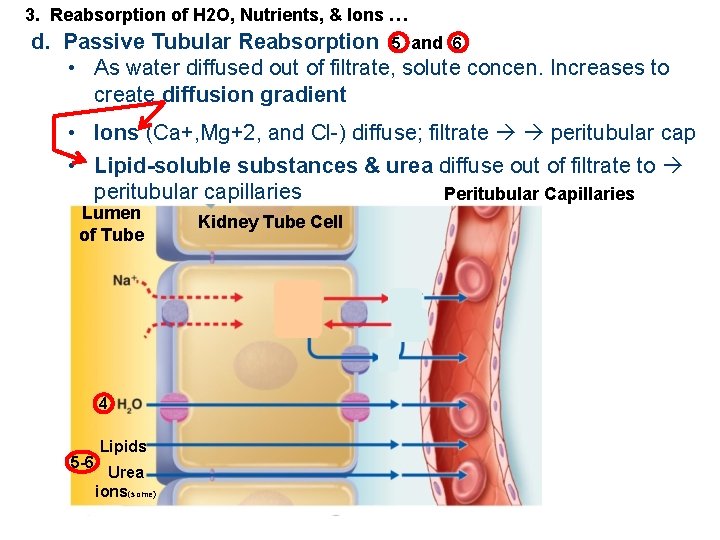
3. Reabsorption of H 2 O, Nutrients, & Ions … d. Passive Tubular Reabsorption 5 and 6 • As water diffused out of filtrate, solute concen. Increases to create diffusion gradient • Ions (Ca+, Mg+2, and Cl-) diffuse; filtrate peritubular cap • Lipid-soluble substances & urea diffuse out of filtrate to peritubular capillaries Peritubular Capillaries Lumen of Tube 4 5 -6 Lipids Urea ions(some) Kidney Tube Cell
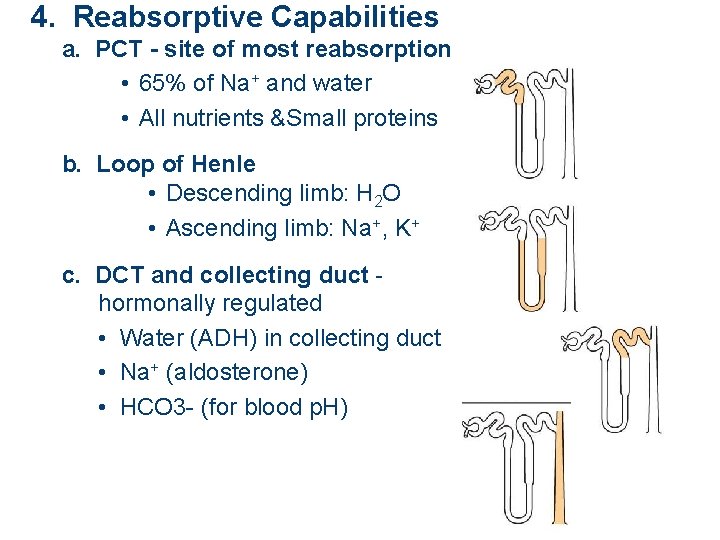
4. Reabsorptive Capabilities a. PCT - site of most reabsorption • 65% of Na+ and water • All nutrients &Small proteins b. Loop of Henle • Descending limb: H 2 O • Ascending limb: Na+, K+ c. DCT and collecting duct hormonally regulated • Water (ADH) in collecting duct • Na+ (aldosterone) • HCO 3 - (for blood p. H)
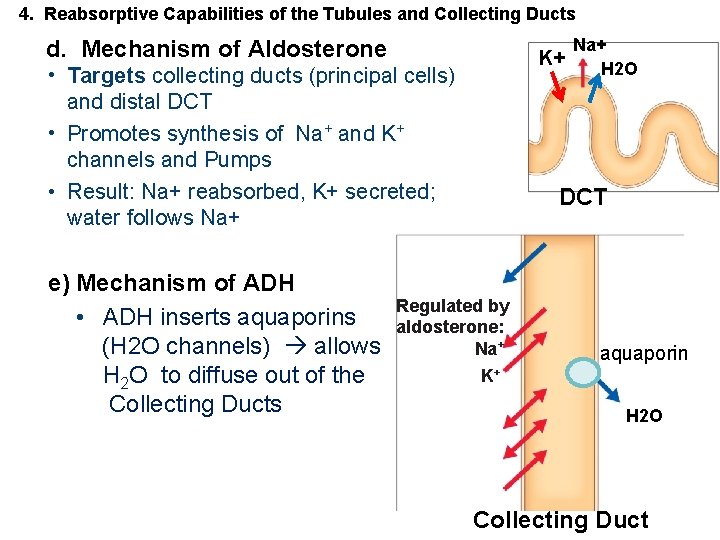
4. Reabsorptive Capabilities of the Tubules and Collecting Ducts Na+ K+ H 2 O d. Mechanism of Aldosterone • Targets collecting ducts (principal cells) and distal DCT • Promotes synthesis of Na+ and K+ channels and Pumps • Result: Na+ reabsorbed, K+ secreted; water follows Na+ DCT e) Mechanism of ADH Regulated by • ADH inserts aquaporins aldosterone: (H 2 O channels) allows triggers. Na+ K+ H 2 O to diffuse out of the Collecting Ducts aquaporin H 2 O Collecting Duct
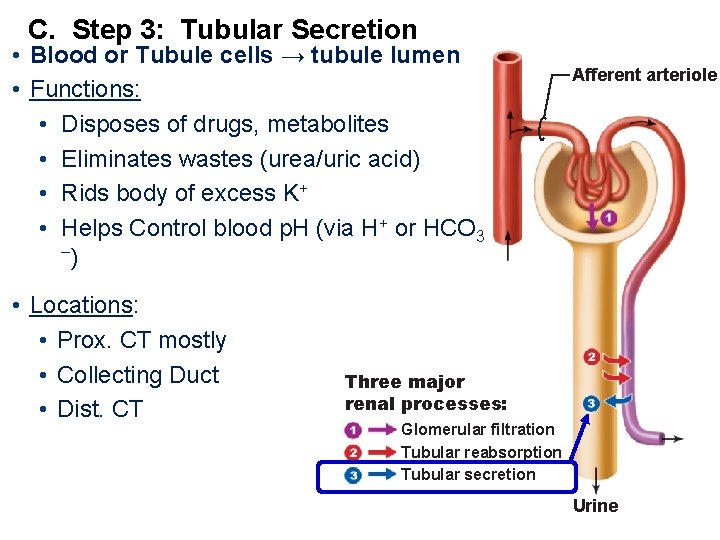
C. Step 3: Tubular Secretion • Blood or Tubule cells → tubule lumen • Functions: • Disposes of drugs, metabolites • Eliminates wastes (urea/uric acid) • Rids body of excess K+ • Helps Control blood p. H (via H+ or HCO 3 –) • Locations: • Prox. CT mostly • Collecting Duct • Dist. CT Afferent arteriole Three major renal processes: Glomerular filtration Tubular reabsorption Tubular secretion Urine

D. Regulation of Urine Concentration and Volume 1. Basic Concepts a. Kidney must maintain constant solute concentration: of body fluids = 300 m. Osmo b. How– Countercurrent mechanism: parallel portions of a tube connected by a hairpin turn maximum transfer of substances c. Loop of Henle ascending and descending limbs create Na. Cl/H 2 O gradient in interstitial fluid Cortex Medulla

2. Mechanism: Countercurrent in Loop and Vasa Recta i) Descending Limb • Permeable to H 2 O • Not to Na. Cl ii) Ascending Limb • Permeable to Na. Cl via active transport • Not to H 2 O iii) Vasa Recta maintains medulla gradient while removing water and solutes to blood. NET RESULT: filtrate more dilute at Dist CT (100) than interstial fluid & blood (300) Interstial fluid

3. Formation of Dilute or Concentrated Urine a) DILUTE URINE Active transport Passive transport • Filtrate is already dilute at top of DCT • Absence of ADH = no aquaporins • then collecting tubule impermeable to H 2 O • Medullary gradient not used Collecting duct Descending limb of loop of Henle DCT Cortex Na. CI H 2 O Outer medulla Na. CI H 2 O Urea Inner medulla (a) Absence of ADH Large volume of dilute urine
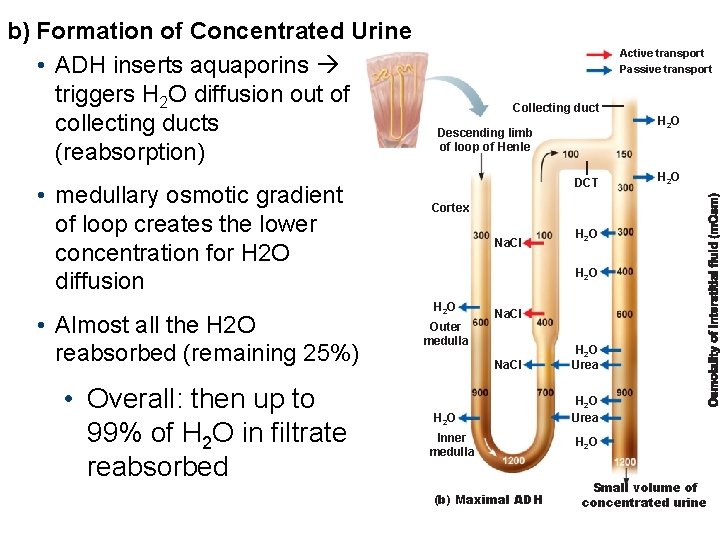
b) Formation of Concentrated Urine • ADH inserts aquaporins triggers H 2 O diffusion out of collecting ducts (reabsorption) • medullary osmotic gradient of loop creates the lower concentration for H 2 O diffusion • Almost all the H 2 O reabsorbed (remaining 25%) • Overall: then up to 99% of H 2 O in filtrate reabsorbed Active transport Passive transport Collecting duct Descending limb of loop of Henle DCT H 2 O Cortex Na. CI H 2 O Outer medulla Na. CI H 2 O Inner medulla (b) Maximal ADH H 2 O Urea H 2 O Small volume of concentrated urine
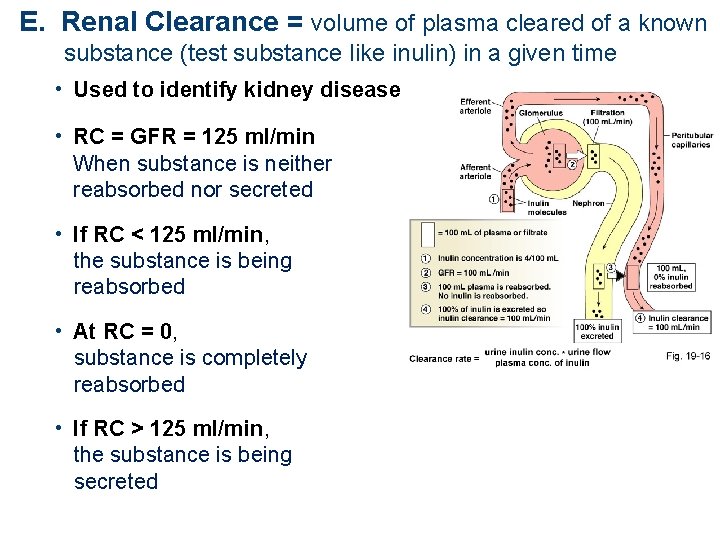
E. Renal Clearance = volume of plasma cleared of a known substance (test substance like inulin) in a given time • Used to identify kidney disease • RC = GFR = 125 ml/min When substance is neither reabsorbed nor secreted • If RC < 125 ml/min, the substance is being reabsorbed • At RC = 0, substance is completely reabsorbed • If RC > 125 ml/min, the substance is being secreted

III. Urine • Color • Odor • p. H • Specific Gravity • Chemical Composition • Water • Nitrogen Wastes: Urea, • Solutes: Na+, K+, phosphate, sulfate • Other Nitrogen Wastes: Uric Acid, Creatinine • Variable: Ca+2, Mg+2, Bi-carbonate • ABNORMAL SUBSTANCES
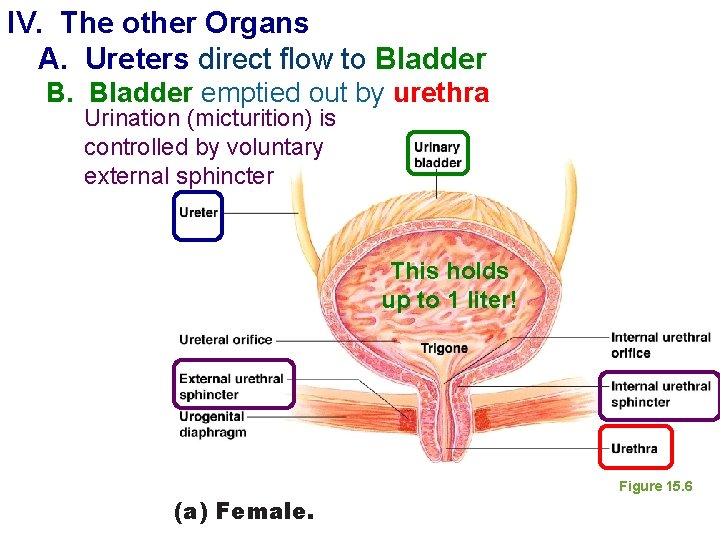
IV. The other Organs A. Ureters direct flow to Bladder B. Bladder emptied out by urethra Urination (micturition) is controlled by voluntary external sphincter This holds up to 1 liter! (a) Female. Figure 15. 6
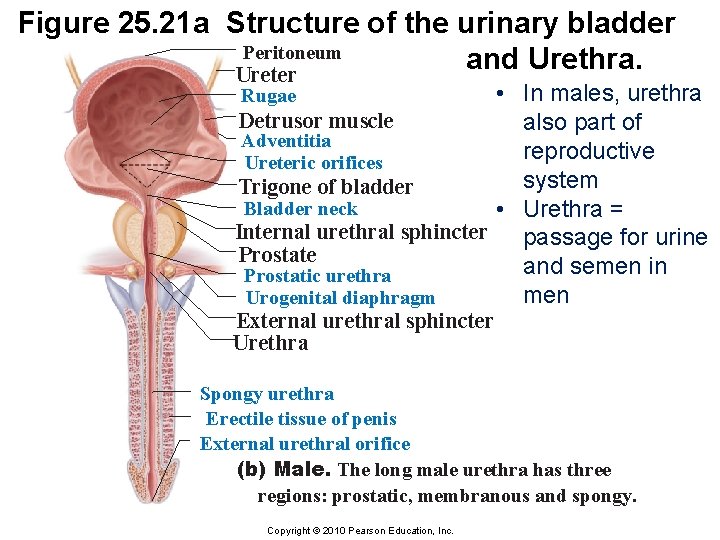
Figure 25. 21 a Structure of the urinary bladder Peritoneum and Urethra. Ureter • In males, urethra Detrusor muscle also part of Adventitia reproductive Ureteric orifices system Trigone of bladder Bladder neck • Urethra = Internal urethral sphincter passage for urine Prostate and semen in Prostatic urethra men Urogenital diaphragm Rugae External urethral sphincter Urethra Spongy urethra Erectile tissue of penis External urethral orifice (b) Male. The long male urethra has three regions: prostatic, membranous and spongy. Copyright © 2010 Pearson Education, Inc.

END OF PPT • Review Questions
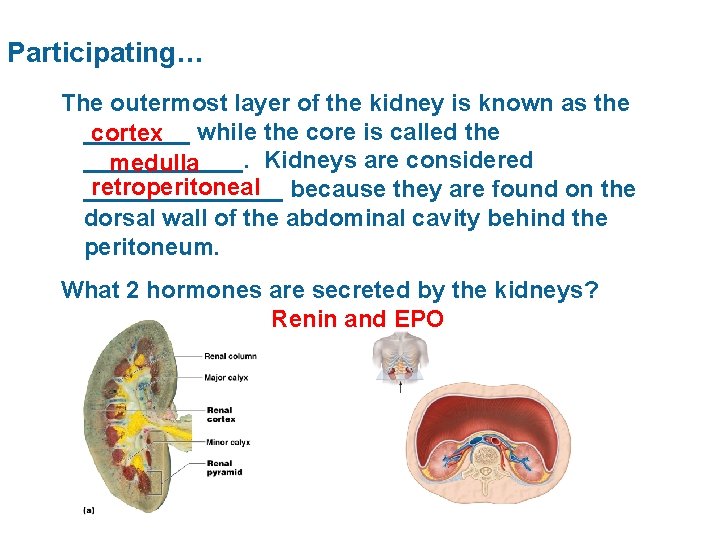
Participating… The outermost layer of the kidney is known as the ____ cortex while the core is called the ______. Kidneys are considered medulla retroperitoneal because they are found on the ________ dorsal wall of the abdominal cavity behind the peritoneum. What 2 hormones are secreted by the kidneys? Renin and EPO
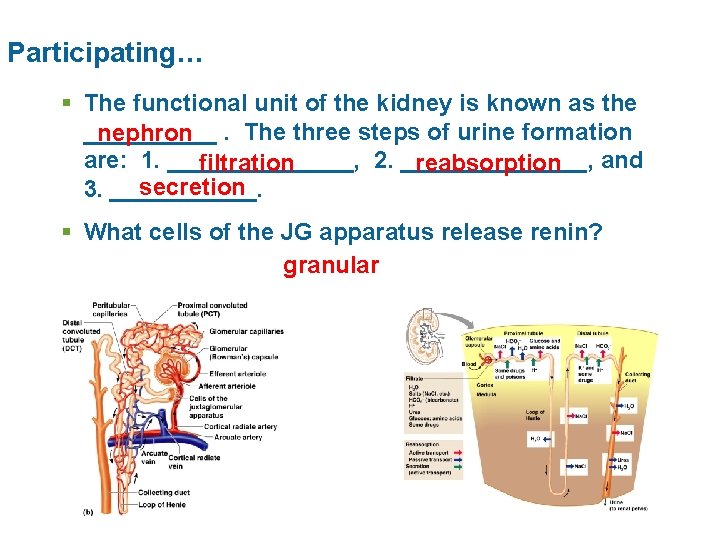
Participating… § The functional unit of the kidney is known as the _____ nephron. The three steps of urine formation are: 1. _______, 2. _______, and filtration reabsorption secretion 3. ______. § What cells of the JG apparatus release renin? granular

Participating… What are 3 things that trigger renin release by the granular cells? Very low b. p. ; low filtrate flow; sympathetic stimulation low Low levels of Na. Cl ions indicates ______ flow rates in the nephron and are detected by macula densa _______ cells of the J-G apparatus afferent which signal the _____ arteriole to dilate _____.
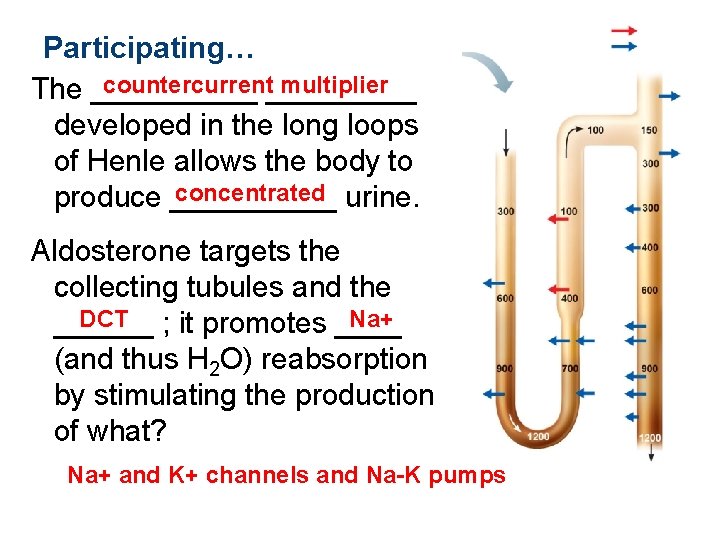
Participating… countercurrent_____ multiplier The _____ developed in the long loops of Henle allows the body to concentrated urine. produce _____ Aldosterone targets the collecting tubules and the DCT ; it promotes ____ Na+ ______ (and thus H 2 O) reabsorption by stimulating the production of what? Na+ and K+ channels and Na-K pumps
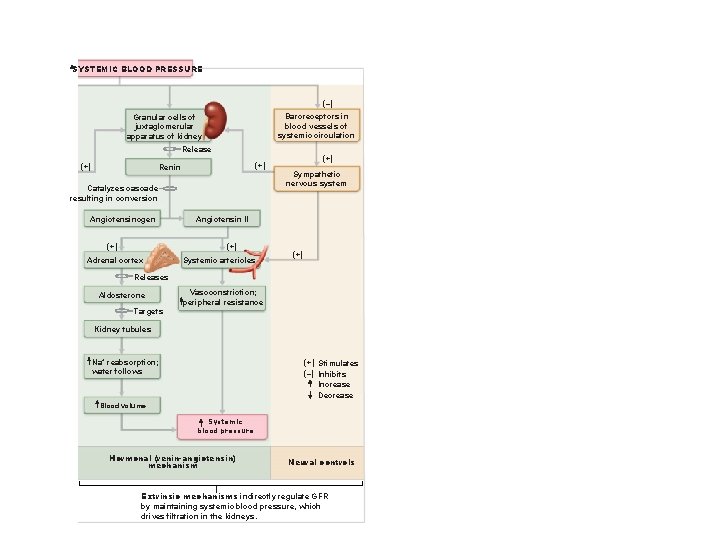
SYSTEMIC BLOOD PRESSURE (–) Baroreceptors in blood vessels of systemic circulation Granular cells of juxtaglomerular apparatus of kidney Release (+) Renin Catalyzes cascade resulting in conversion Angiotensinogen (+) Sympathetic nervous system Angiotensin II (+) Adrenal cortex (+) Systemic arterioles (+) Releases Aldosterone Targets Vasoconstriction; peripheral resistance Kidney tubules Na+ reabsorption; water follows (+) Stimulates (–) Inhibits Increase Decrease Blood volume Systemic blood pressure Hormonal (renin-angiotensin) mechanism Neural controls Extrinsic mechanisms indirectly regulate GFR by maintaining systemic blood pressure, which drives filtration in the kidneys.
- Slides: 24