THE THYROID GLAND Thyroid cartilago Pyramidal lobe Left

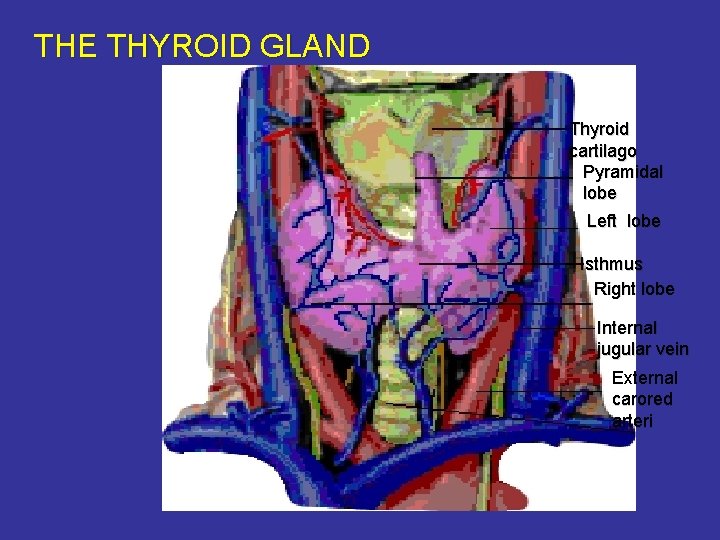
THE THYROID GLAND Thyroid cartilago Pyramidal lobe Left lobe Isthmus Right lobe Internal jugular vein External carored arteri
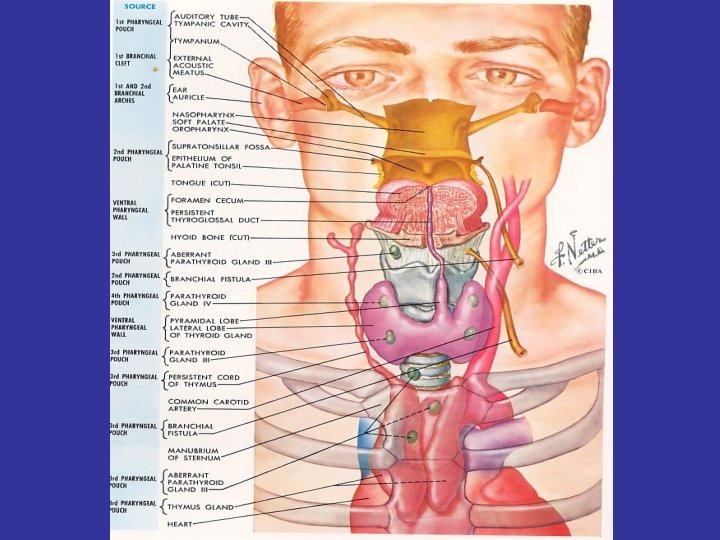

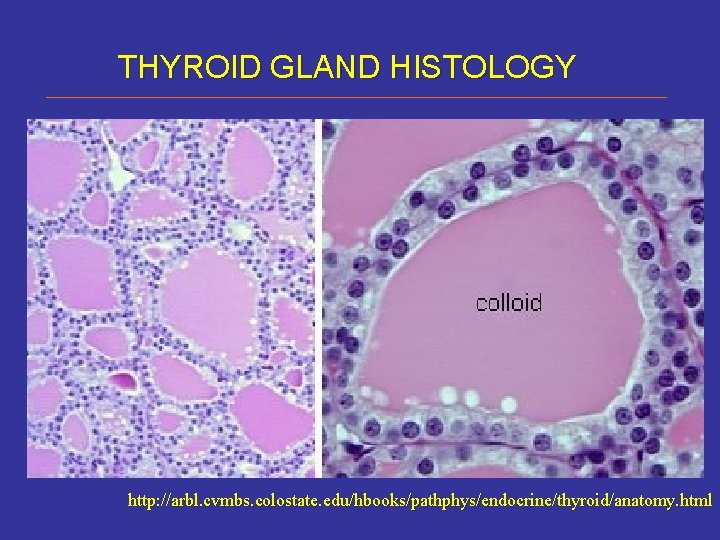
THYROID GLAND HISTOLOGY http: //arbl. cvmbs. colostate. edu/hbooks/pathphys/endocrine/thyroid/anatomy. html
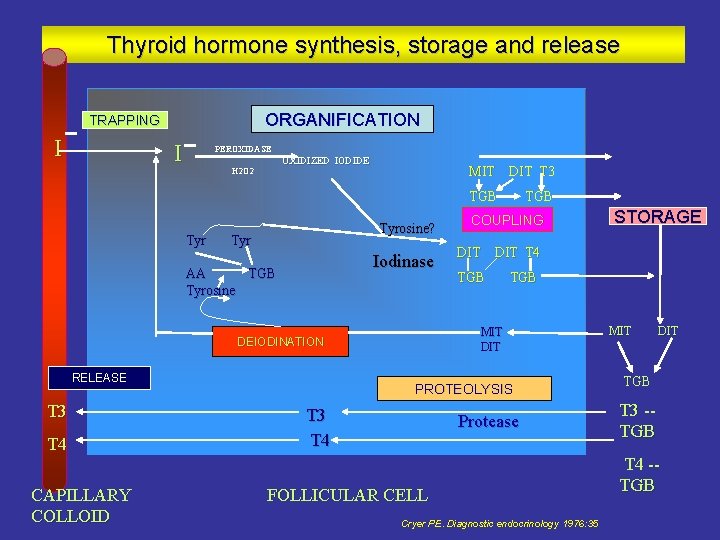
Thyroid hormone synthesis, storage and release ORGANIFICATION TRAPPING I I PEROXIDASE OXIDIZED IODIDE H 2 O 2 MIT DIT T 3 TGB Tyrosine? Tyr Iodinase AA TGB Tyrosine T 3 T 4 CAPILLARY COLLOID COUPLING TGB PROTEOLYSIS T 3 T 4 STORAGE DIT T 4 MIT DEIODINATION RELEASE TGB Protease FOLLICULAR CELL Cryer PE. Diagnostic endocrinology 1976: 35 MIT DIT TGB T 3 -TGB T 4 -TGB
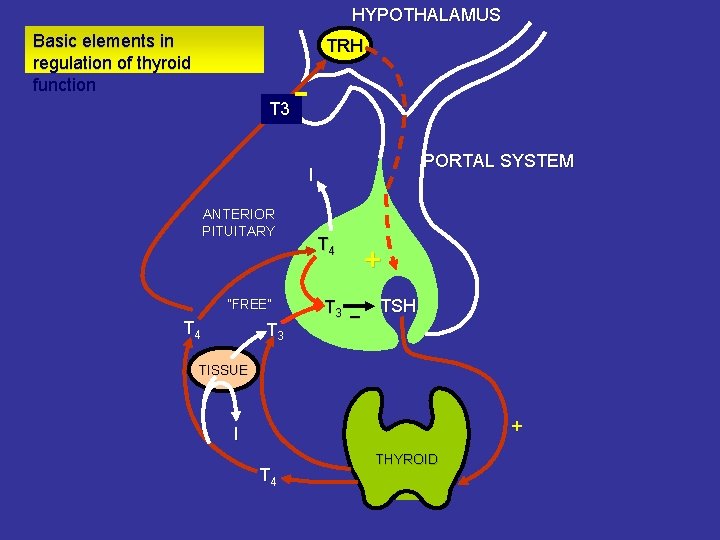
HYPOTHALAMUS Basic elements in regulation of thyroid function TRH T 3 PORTAL SYSTEM I ANTERIOR PITUITARY “FREE” T 4 T 3 _ + TSH TISSUE + I T 4 THYROID

Usually Complain thyroid disease • Thyroid enlargement which may be diffuse or nodular • Symptom of thyroid deficiency or Hypothyroidism • Symptoms of thyroid hormon excess, or Hyperthyroidism

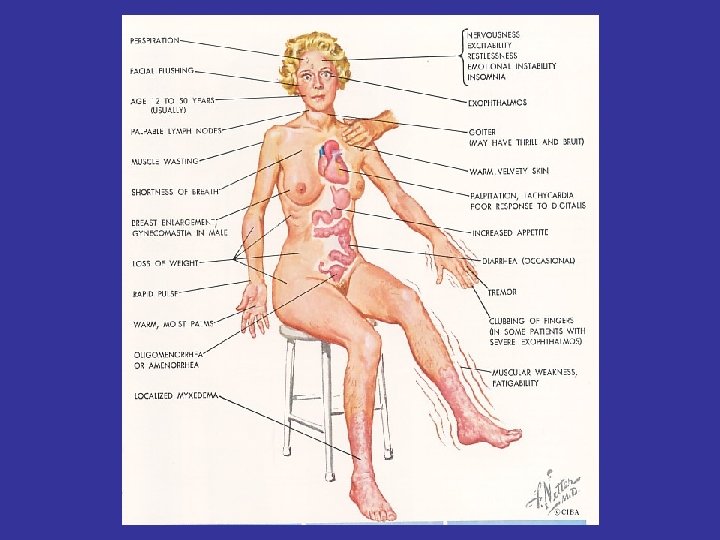
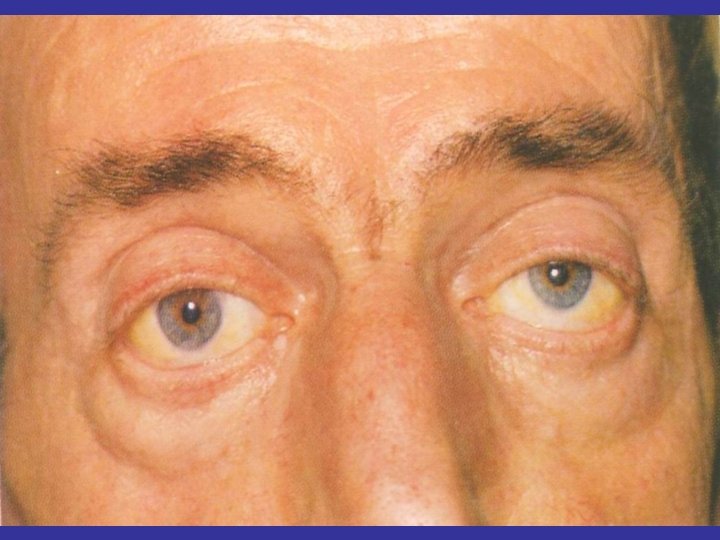
Usually Complain thyroid disease Complications of a Spesific form hyperthyroidism : Graves’ disease which may present which prominence of the eyes or exophthalmos and thickening of the skin over the lower legs (rare) or thyroid dermopathy

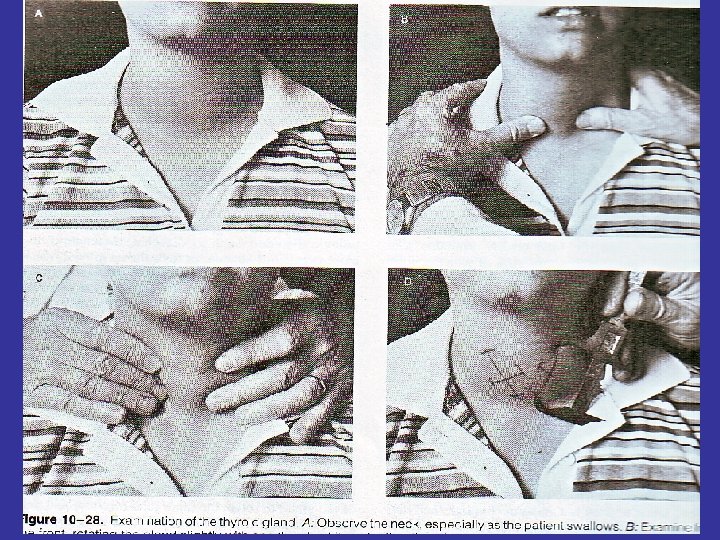
Physical Examination • Inspection : Good light coming from behind the examiner, The patient is instructed to swallow a sip of water, Observe the gland as it moves up and down. Enlargement and nodularity can often be noted.

Physical Examination • Palpate the gland from behind the patient with the middle threes fingers on each lobe while the patients swallows. Nodules can be measured in a similar way.

Physical Examination • On physical examination the normal thyroid gland about 2 cm in vertical dimension and about 1 cm in horizontal dimention above the isthmus • Enlarged thyroid gland is called Goiter • The generalized enlargement is termed diffuse goiter, irreguler or lumpy enlargement is called nodular goiter
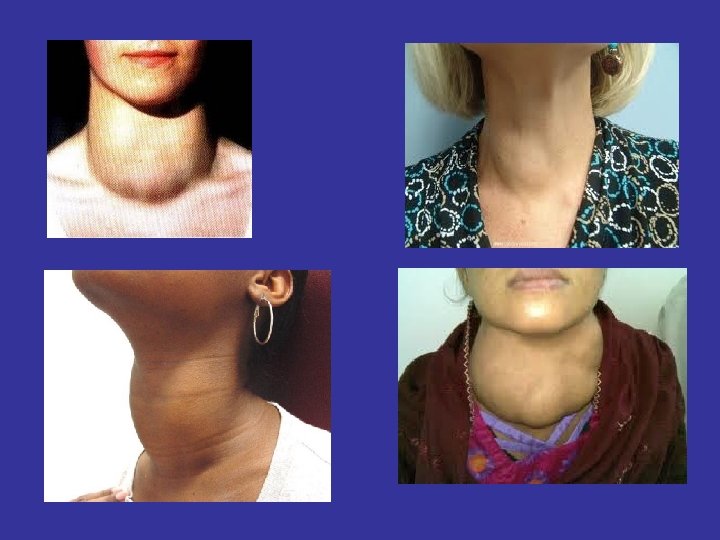
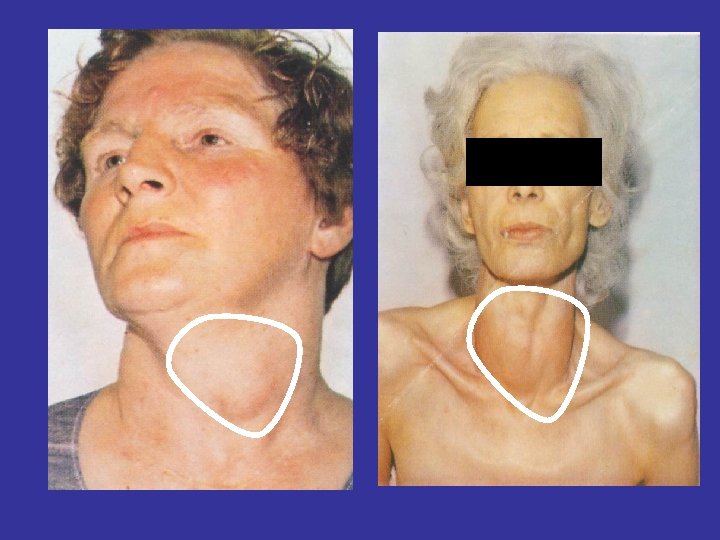

THYROID DISEASES HYPERTHYROIDISM HYPOTHYROIDISM THYROIDITIS THYROID NODUL
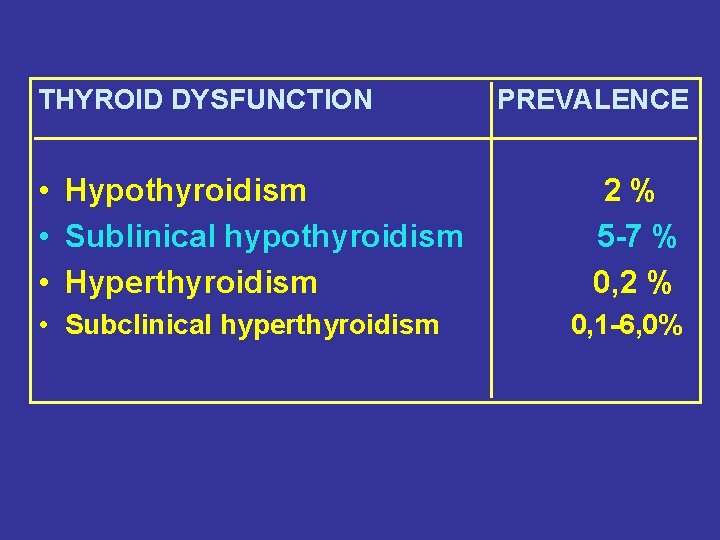
THYROID DYSFUNCTION • Hypothyroidism • Sublinical hypothyroidism • Hyperthyroidism • Subclinical hyperthyroidism PREVALENCE 2% 5 -7 % 0, 2 % 0, 1 -6, 0%

Hyperthyroidism & Thyrotoxicosis • Thyrotoxicosis is the clinical syndrome that results when tissues are exposed to high levels of circulating thyroid hormone. • Thyroxicosis is due to hyperactivity of the thyroid gland or hyperthyroidism • Occasionally, thyrotoxicosis may be due to other causes such us excessive ingestion of the thyroid hormone or excessive thyroid hormon from ectopis site

Conditions associated with thyrotoxicosis • • • Diffuse toxic goiter (Graves’ disease) Toxic adenoma (Plummer’s disease) Toxic multinodular goiter Subacute thyroiditis Hyperthyroid phase of Hashimoto’s thyroiditis • Thyrotoxicosis factitia • Rare: Ovarian struma, metastatic thyroid carcinoma, hydatiform mole

GRAVES’ DISEASE (DIFFUSE TOXIC GOITER) • GD is the most common form of thyrotoxicosis, may occur at any age, more commonly in females than in males (5 X) • The syndrome consist one or more of the following features: 1. THYROTOXICOSIS 2. GOITER 3. OPHTHALMOPATHY(Exophthalmos) 4. DERMOPATHY (Pretibial myxedema)

ETIOLOGY & PATHOGENESIS • GD is currently viewed as an autoimmun disease of unknown cause • Ther is a strong familial predisposition in that about 15%. 50% GD have circulating thyroid autoantibodies • Peak incidence 20 -40 -year • T-lymphocytes sensitized to antigen within thyroid gland stimulate B lymphocyte antibodies
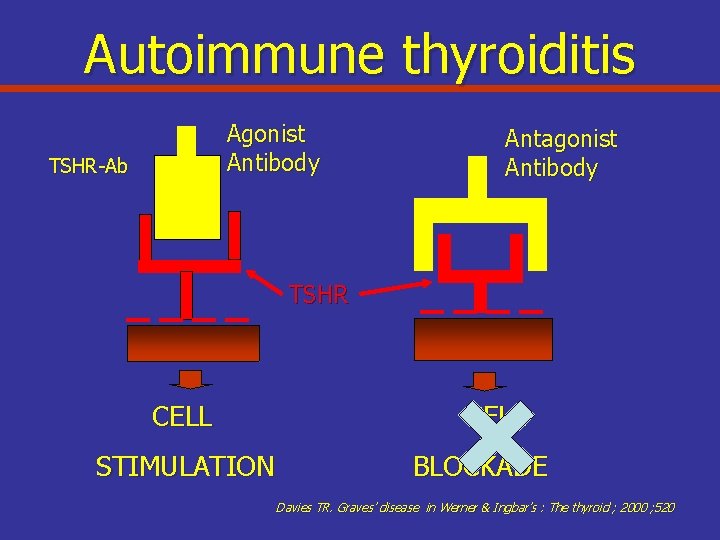
Autoimmune thyroiditis Agonist Antibody TSHR-Ab Antagonist Antibody TSHR CELL STIMULATION CELL BLOCKADE Davies TR. Graves’ disease in Werner & Ingbar’s : The thyroid ; 2000 ; 520

Clinical features Graves’s disease • Symptoms: in younger patients: palpitation, nervousness, easy fatigability, hyperkinesia, diarhhea, excessive sweating, intolerance to heat, weight loss, without loss appetite • Signs: Thyroid enlargement, exophthalmos, tachycardia, muscle weakness, tremor Older patients cardiovascular & myopatic predominate clinical manifestation palpitatation, dyspnea on exersice, tremor, nervousness, weight loss

Ophtamopathy Graves disease • Infitratif sympathetic overstimulation Lid retraction (Dalrymphe’s sign) Van Graves sign late palpebra sup Stellwat’s sign the wink eyes late Jefroy’s sign fold of forehead not see Mobius’sign convergention of the eyes late • Infiltratif autoimmune Exophthalmus, oculopathy congestif: cheimosis, conjunctivitis, periorbital edema Ulcerasi Cornea , neuritis optica, atrophi n opticus
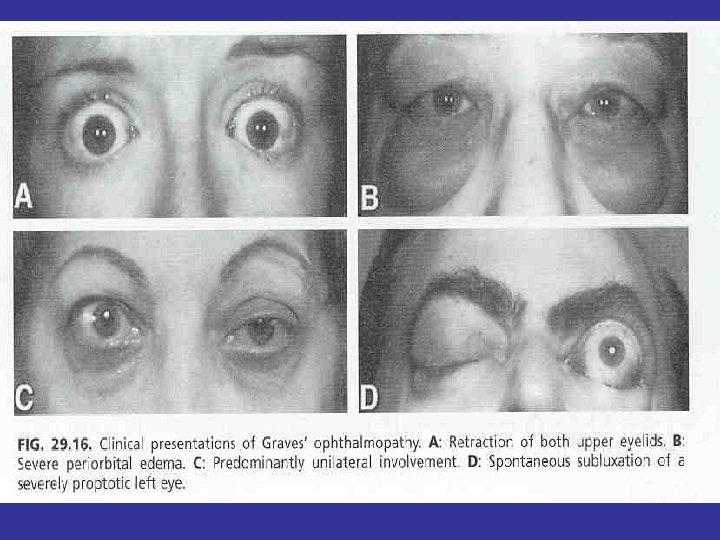
DISEASE SEVERITY Thyroid eye disease can be divided into MILD disease MODERATE disease SEVERE disease
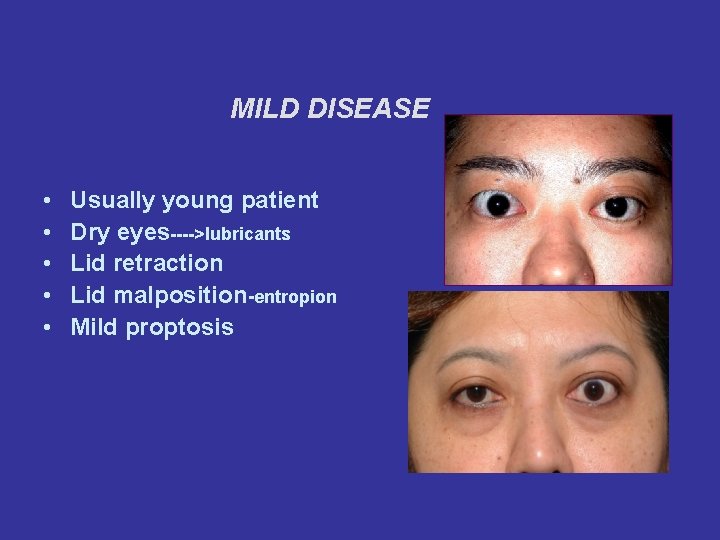
MILD DISEASE • • • Usually young patient Dry eyes---->lubricants Lid retraction Lid malposition-entropion Mild proptosis

MODERATE DISEASE Thyroid myopathy asymmetric involvement tends to involve vertical muscles in Asians
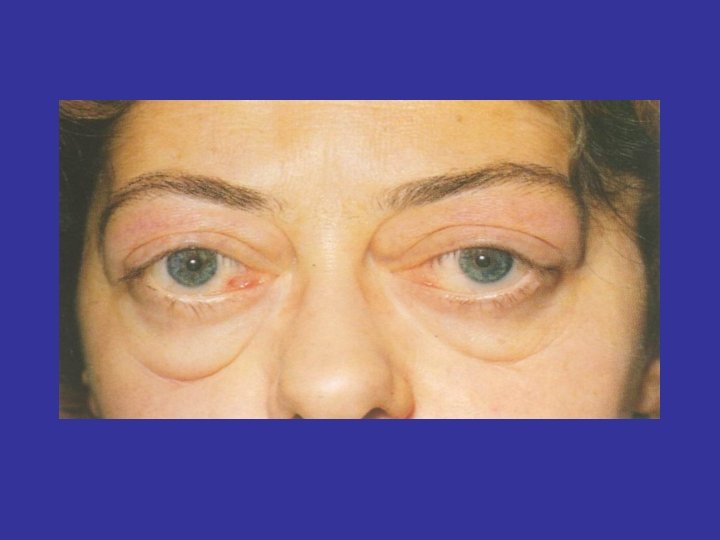
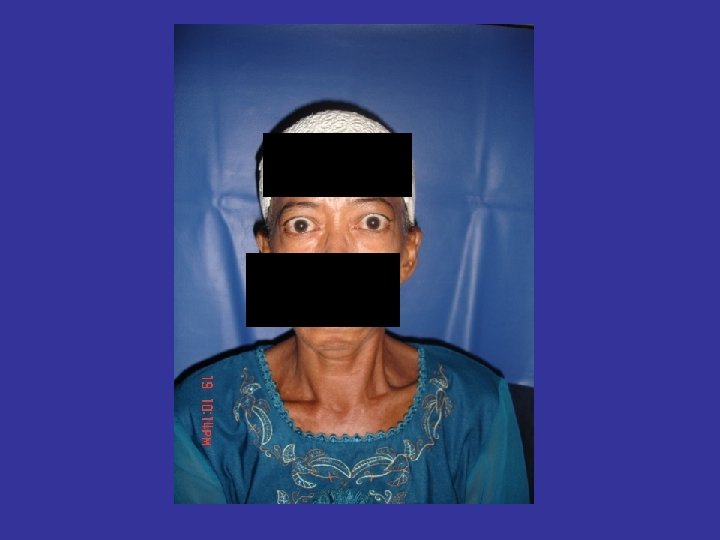
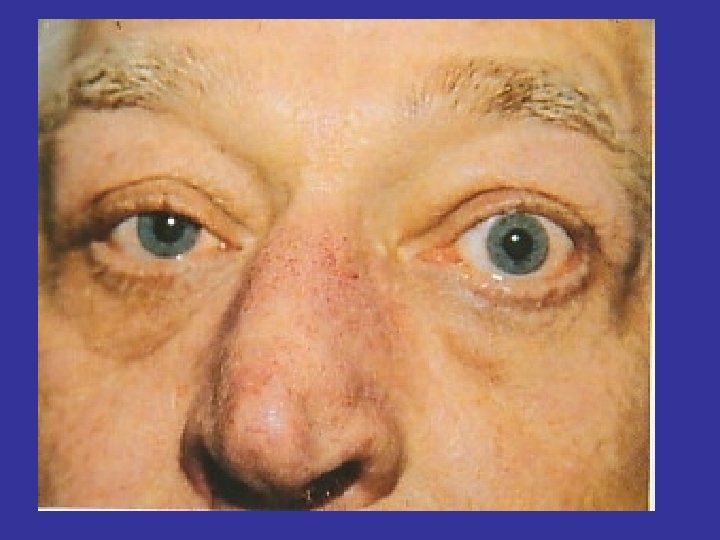
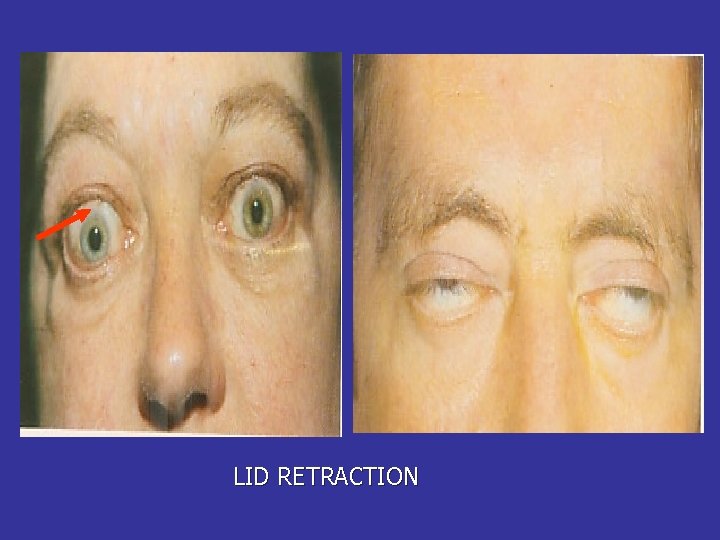
LID RETRACTION
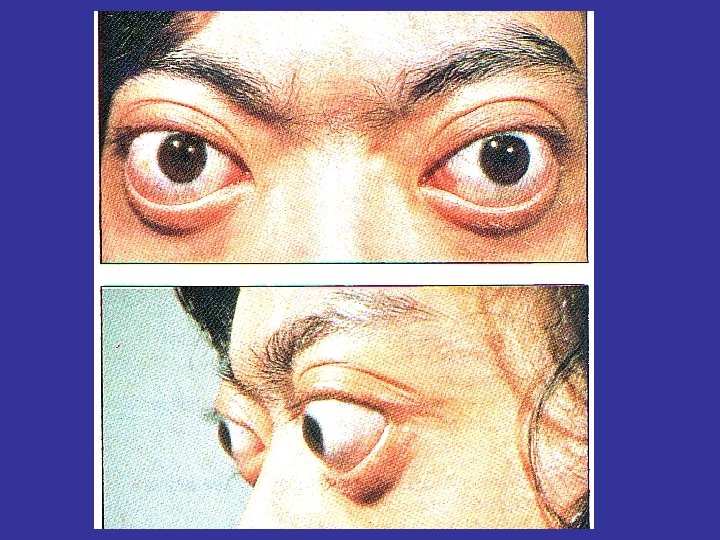
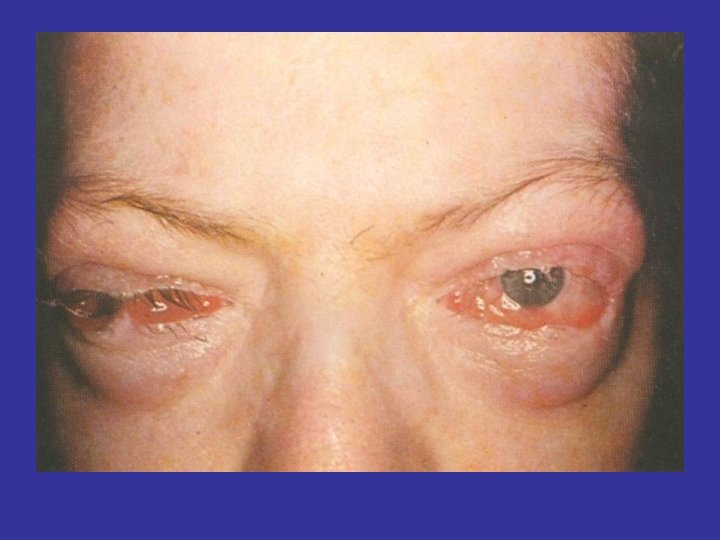
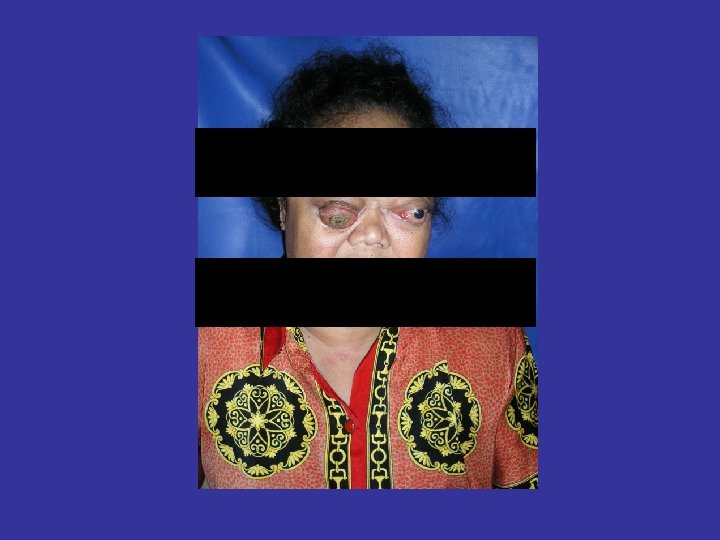
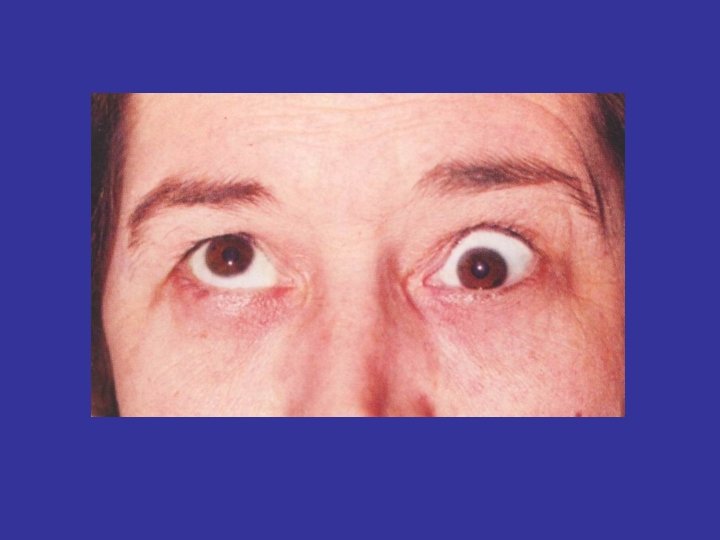

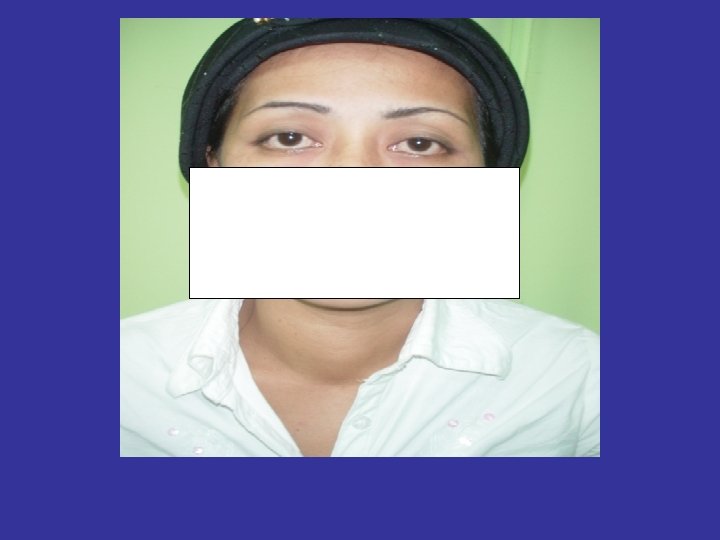

HERTEL EXOPHTHALMOMETER EXOPHTHALMOS : >18 MM
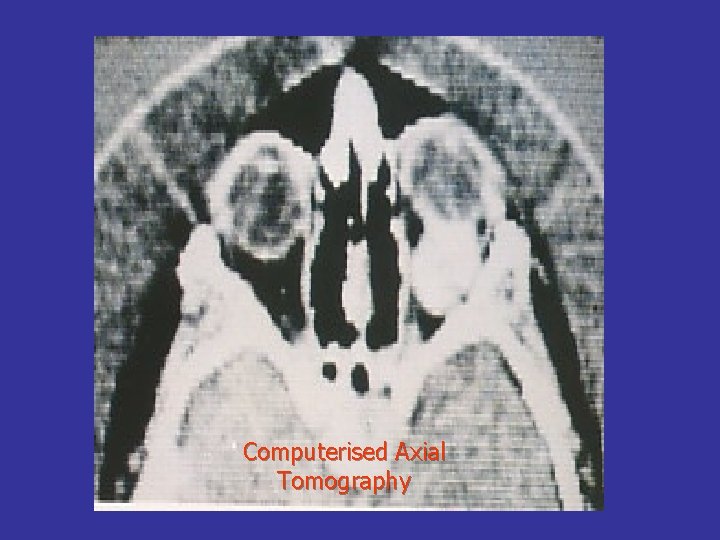
Computerised Axial Tomography

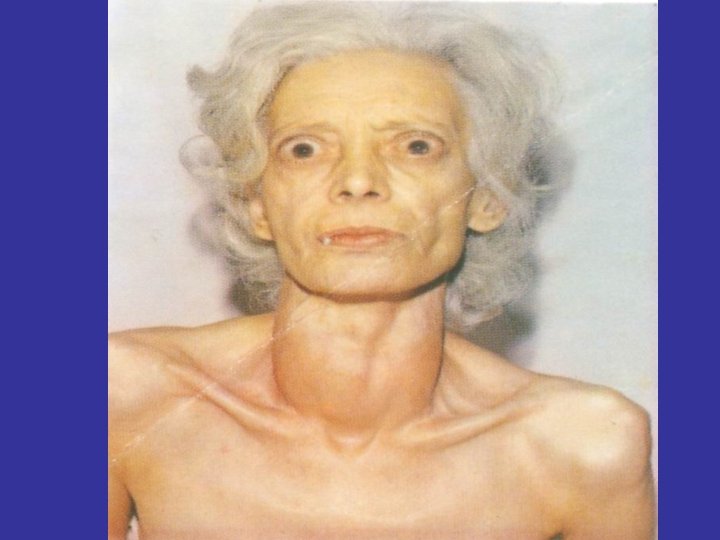
Thyroid Dermopathy • Thickening of the skin, over the lower tibia due to accumulation glycosaminglicans , rare (2 -3%) • TSH-R Ab high titer • Osteopathy in the metacarpal bones
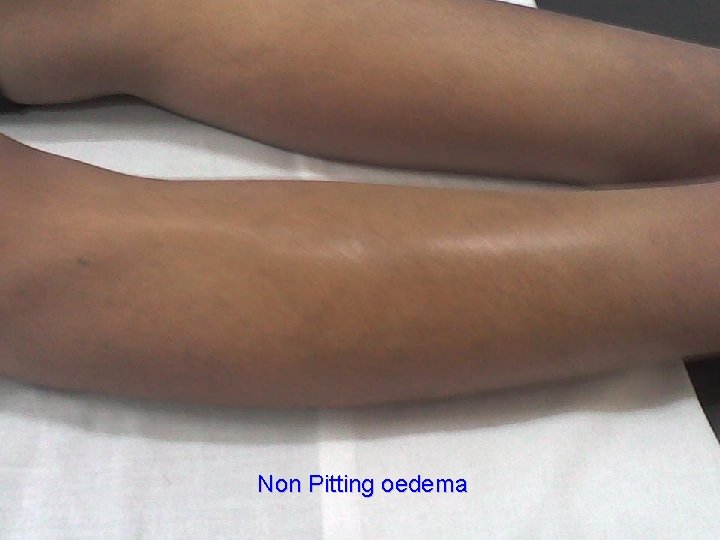
Non Pitting oedema
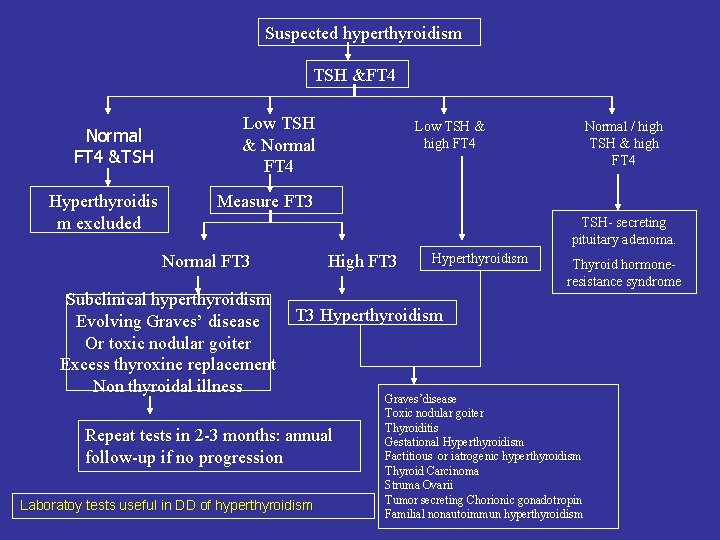
Suspected hyperthyroidism TSH &FT 4 Normal FT 4 &TSH Hyperthyroidis m excluded Low TSH & Normal FT 4 Low TSH & high FT 4 Normal / high TSH & high FT 4 Measure FT 3 TSH- secreting pituitary adenoma. Normal FT 3 Subclinical hyperthyroidism Evolving Graves’ disease Or toxic nodular goiter Excess thyroxine replacement Non thyroidal illness High FT 3 Hyperthyroidism Thyroid hormoneresistance syndrome T 3 Hyperthyroidism Repeat tests in 2 -3 months: annual follow-up if no progression Laboratoy tests useful in DD of hyperthyroidism Graves’disease Toxic nodular goiter Thyroiditis Gestational Hyperthyroidism Factitious or iatrogenic hyperthyroidism Thyroid Carcinoma Struma Ovarii Tumor secreting Chorionic gonadotropin Familial nonautoimmun hyperthyroidism

Atypical fashion Graves’ Disease • Thyrotoxic periodic paralysis: usually Asian males, sudden attack flacid paralysis, hypokalemia, usualy subsides spontaneously. Prevention: K+ supplement & Betablockers • Thyrocardiac disease: primarily with symptoms of heart involvement: refrsctory AF insensitif digoxin or high output heart failure, no evidence underlying heart disease (50%). Treatment of thyrotoxicosis cure

Atypical fashion Graves’ Disease • Apethetic hyperthyroidism: Older patients: weight loss, small goiter, slow AF, severe depression with none clinical features

Treatment modalities • Anti-thyroid • Surgery • I 131 radioactive

Treatment of Graves’ Disease 1. Antithyroid drug therapy: Young pts, small glands, mild disease Propylthiouracil, methimazole (6 m-15 mo), relaps 50 -60%. PTU inhibits the conversion T 4 T 3, effect more quickly compare to methimazole Methimazole - longer duration, single dose Therapy 3 -6 months tapering dose and combination levothyroxin 0. 1 mg/d 12 -24 months Allergic reaction (rash), agranulocytosis, jaundice, liver failure

Treatment of Graves’ diseae • Surgical treatment Subtotal thyroidectomy treatment of choice for very large glands, or multinodular goiter, prepared wth anti thyroid drug (about 6 months) Complication : Hypothyroidism, recurent laryngeal nerve injury
Treatment of Graves’ disease • Radioactive iodine therapy USA Na. I 131 I euthyroid over 612 weeks Complication: hypothyroidism

Treatment of Graves’ disease • Other medical measures: Beta-adrenergic blocking agents Propranolol 10 -40 mg every 6 hours, multivitamin supplements, phenobarbital as sedative + to lower T 4 levels Cholestyramine, 4 gr orally 3 X daily lower T 4

Complication of Graves’ Disease Thyrotoxic crisis (thyroid storm) Acute exacerbation symptoms thyrotoxicosis. May be mild & febrile until life threatning. Etiology : after thyroid surgery in patients who has been inadequatlely prepared, RAI 131, parturition in adequately controlled thyrotoxicosis or stressfull illnes.

• Thyrotoxic crisis(thyroid “storm”): Clinical manifestation: Fever, Sweating, flushing, tachycardia / AF, heart failure, agitation, delirium, coma, jaundice, nausea, vomiting and diarrhea. 75% death………….

Treatment of Thyrotoxic crisis (“thyroid storm”) • Prophiltriourasil (PTU): 4 x 300 mg atau • Neomercazole 6 x 20 mg. • Yodium : Sodium yodida IV 1 mg/12 jam, atau lugol 5% 3 x 10 tts /hr • Propranolol (Inderal): IV 1 -5 mg/6 jam, atau tab 4 x 60 -80 mg/hr via sonde lambung • Kortikosteroid: Dexamethason 2 mg/6 jam • Antibiotik dianjurkan jika infeksi sebagai pencetus.

- Slides: 62