The TeachBack Project A Hospital Based Multidisciplinary Project

The Teach-Back Project: A Hospital Based Multidisciplinary Project to Improve Teaching with Patients and Families April 15 th, 2015 Cori Gibson, MSN, RN, CNL Carol Klingbeil, MS, RN, CPNP-PC Laurie Newton, DNP, RN, CPNP

Disclosure Statement • There are no relevant financial relationships related to this presentation. • There is no sponsorship/commercial support of this presentation. • The content being presented will be fair, well-balanced and evidence-based.

Learning Objectives • Identify disciplines that can benefit from learning health literacy teaching strategies. • Describe a brief educational intervention that was effective at improving knowledge and use of health literacy focused communication strategies. • Evaluate evidence of both initial improvement and subsequent sustainability over time after a brief educational intervention.

Background and Significance • Health Literacy – “The degree to which individuals have the capacity to obtain, process, and understand basic health information and services needed to make appropriate health decisions. ”* – Low health literacy is associated with poor health outcomes. • Higher rates of hospitalization & ED use • Prolonged recovery time from illnesses • Illness complications *Healthy People 2010

Background and Significance • Many patients/families leave medical encounters with a poor understanding of their illness and treatment plan. • Several studies back this: – 40 -80% of information provided by practitioners was forgotten immediately after visit. – Only about 50% of information given by health care providers was retained.

Background and Significance • This becomes even more complicated in pediatrics. – Healthcare workers are responsible for addressing both the parents’ and children's literacy skills. – Growing evidence that health status and access to care in children may be linked to the parent’s level of health literacy.

Background and Significance • As health care providers, we often expect patients to ask us questions if they don’t understand… – This is not always the case. • Strategies to help improve communication with patients: – Slow down – Use plain language – Show or draw pictures – Limit information – Use the “teach-back” technique

Background & Significance • Teach-back – Asking the parent and/or child to repeat back what they understood in their own words, and clarify information as needed – Process is highlighted by Joint Commission and National Quality Forum as one of its 30 practices for improving patient safety

Why is Teach-Back so Powerful? 9

Emily’s Story

Juan’s Story

A Parent’s Perspective • Kelly’s video

Purpose • To examine the impact of a brief educational intervention for multidisciplinary staff on health literacy and the use of teach-back
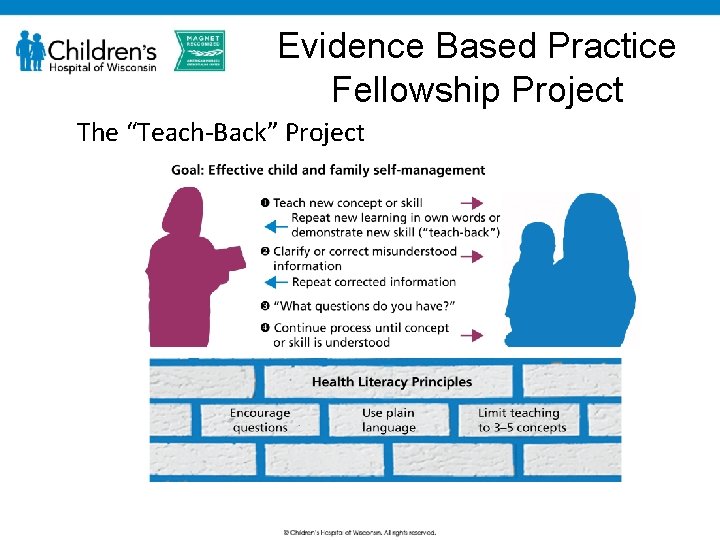
Evidence Based Practice Fellowship Project The “Teach-Back” Project

Sample and Setting • Over 300 healthcare team members – Nurses (acute care, emergency room, surgical) – Dieticians – Respiratory care practitioners – Occupational and Physical therapists • Children’s Hospital of Wisconsin and Children’s Hospital of Wisconsin - Surgicenter

Methods Descriptive pre/post test design • Pre-survey (Survey Monkey®) – Self evaluation of prior knowledge on health literacy and teach-back

Methods • Educational intervention – 30 minute instructor led sessions • Goals: – Raise awareness of prevalence and impact of low health literacy – Educate on use of key strategies to improve communication and safety – Encourage staff to incorporate use of teach-back into everyday practice

Renee’s Story • Video

Methods • Post survey (Survey Monkey®) – 2 months after session • One year sustainability(follow-up) survey (Survey Monkey®) – Nurses (subset of inpatient units) – Dieticians, respiratory care practitioners, and therapists
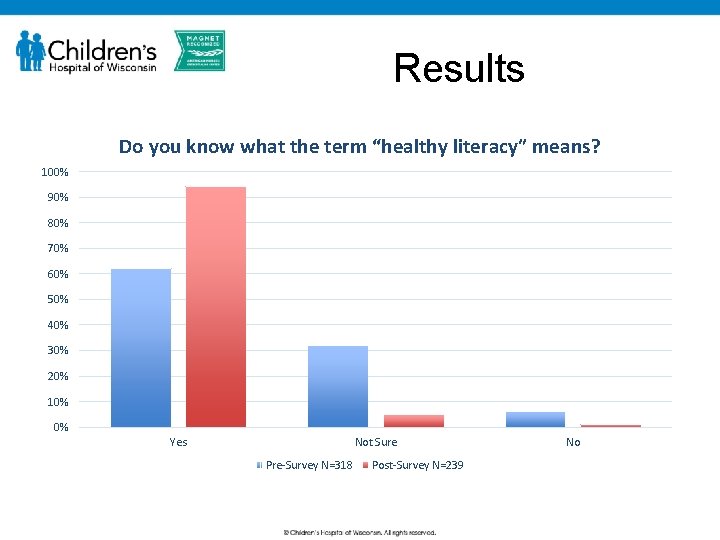
Results Do you know what the term “healthy literacy” means? 100% 90% 80% 70% 60% 50% 40% 30% 20% 10% 0% Yes Not Sure Pre-Survey N=318 Post-Survey N=239 No
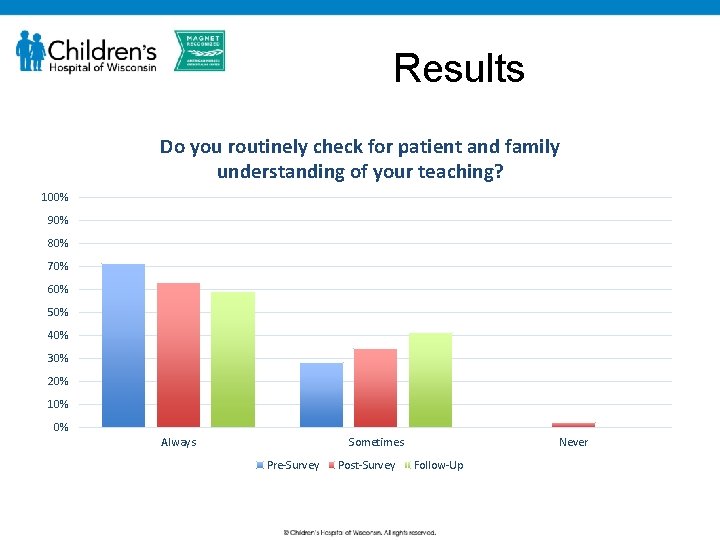
Results Do you routinely check for patient and family understanding of your teaching? 100% 90% 80% 70% 60% 50% 40% 30% 20% 10% 0% Always Sometimes Pre-Survey Post-Survey Never Follow-Up
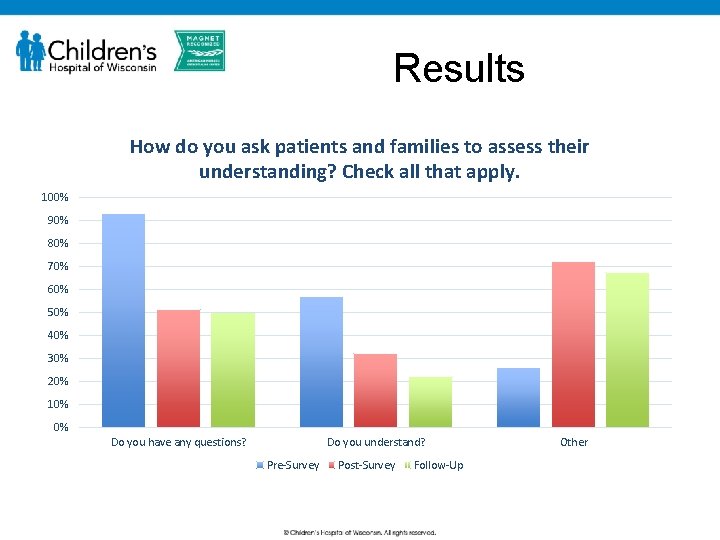
Results How do you ask patients and families to assess their understanding? Check all that apply. 100% 90% 80% 70% 60% 50% 40% 30% 20% 10% 0% Do you have any questions? Do you understand? Pre-Survey Post-Survey Follow-Up Other
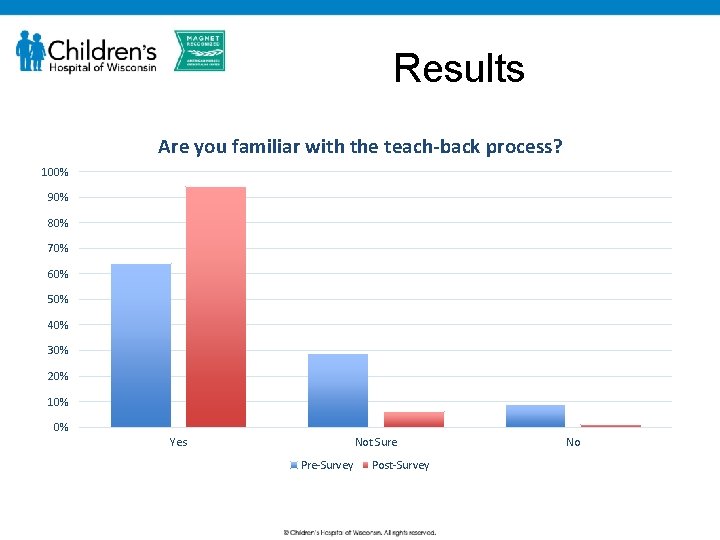
Results Are you familiar with the teach-back process? 100% 90% 80% 70% 60% 50% 40% 30% 20% 10% 0% Yes Not Sure Pre-Survey Post-Survey No
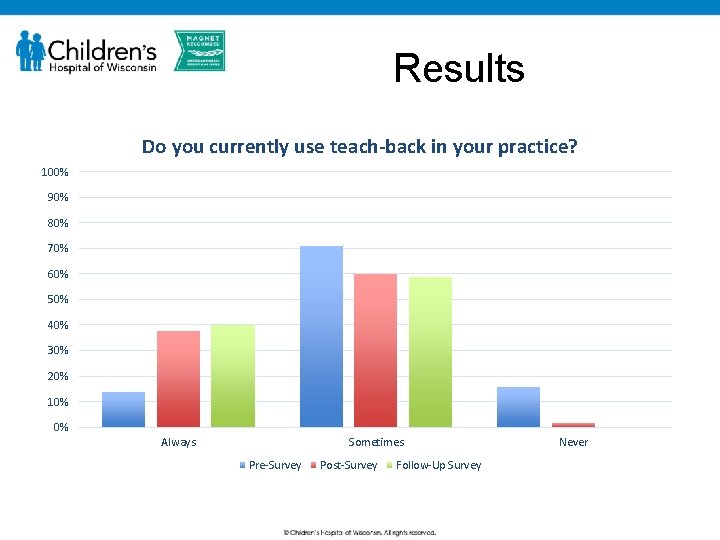
Results Do you currently use teach-back in your practice? 100% 90% 80% 70% 60% 50% 40% 30% 20% 10% 0% Always Sometimes Pre-Survey Post-Survey Follow-Up Survey Never
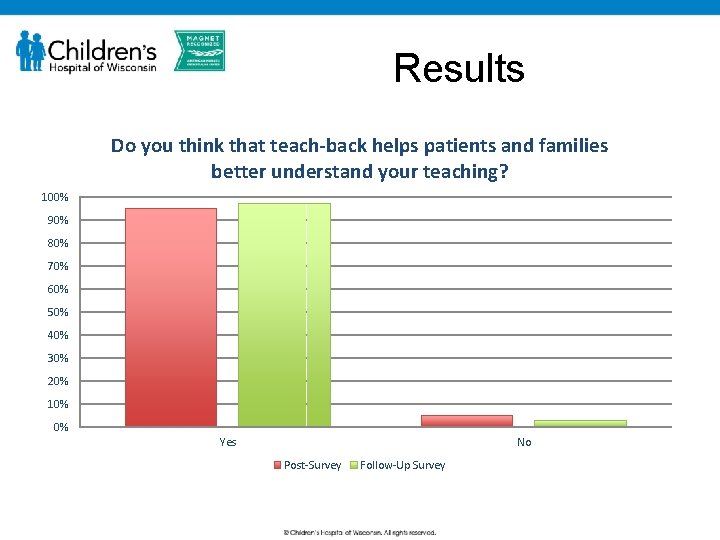
Results Do you think that teach-back helps patients and families better understand your teaching? 100% 90% 80% 70% 60% 50% 40% 30% 20% 10% 0% Yes No Post-Survey Follow-Up Survey
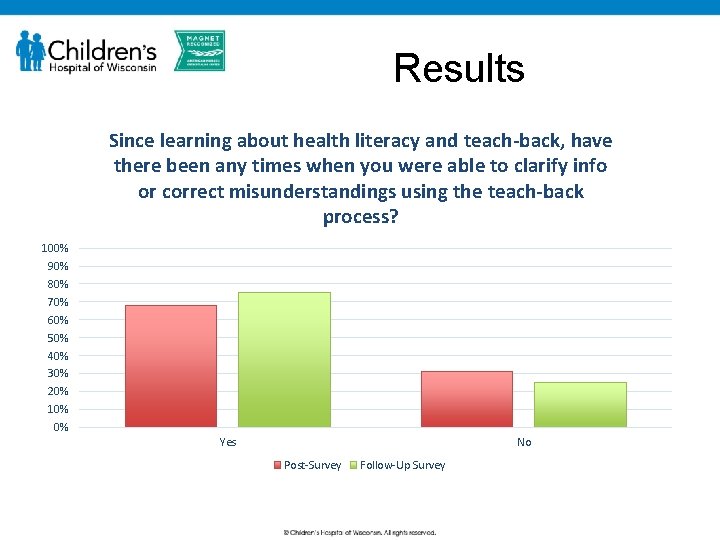
Results Since learning about health literacy and teach-back, have there been any times when you were able to clarify info or correct misunderstandings using the teach-back process? 100% 90% 80% 70% 60% 50% 40% 30% 20% 10% 0% Yes No Post-Survey Follow-Up Survey
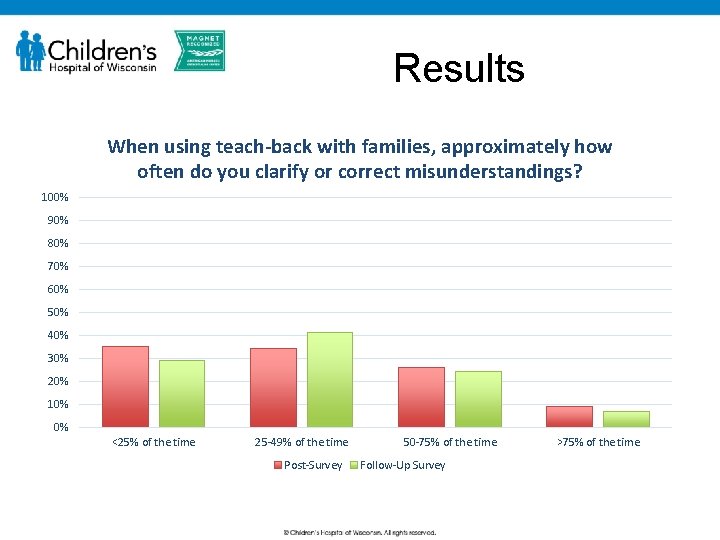
Results When using teach-back with families, approximately how often do you clarify or correct misunderstandings? 100% 90% 80% 70% 60% 50% 40% 30% 20% 10% 0% <25% of the time 25 -49% of the time Post-Survey 50 -75% of the time Follow-Up Survey >75% of the time

Results • Question: When do you feel it’s necessary/important to use teach- back? – When I don’t think they understand – With medications and treatments – With signs and symptoms to call for
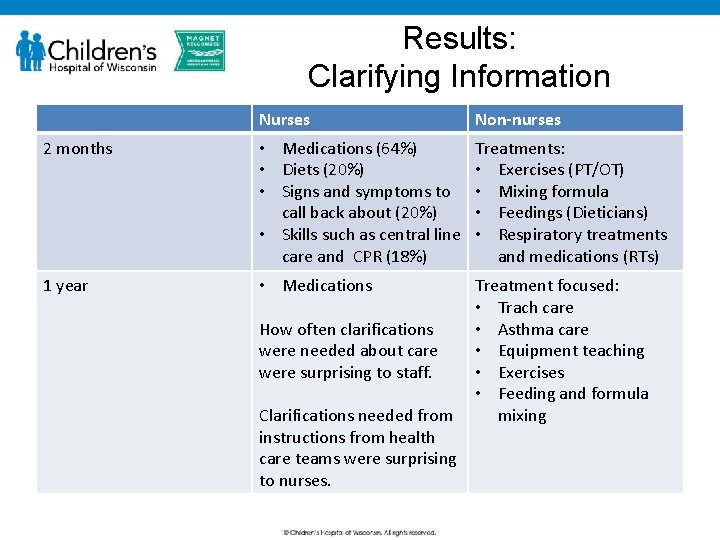

Results: Clarifying Information Nurses Non-nurses 2 months • Medications (64%) • Diets (20%) • Signs and symptoms to call back about (20%) • Skills such as central line care and CPR (18%) Treatments: • Exercises (PT/OT) • Mixing formula • Feedings (Dieticians) • Respiratory treatments and medications (RTs) 1 year • Medications Treatment focused: • Trach care • Asthma care • Equipment teaching • Exercises • Feeding and formula mixing How often clarifications were needed about care were surprising to staff. Clarifications needed from instructions from health care teams were surprising to nurses.

Quotes • Asthma albuterol inhaler, mom was using it every 4 hours & prn instead of q 4 hours prn. She was doing this for 3 years!!! • Family of a toddler with a head injury told the Dr. that they understood when to call and follow-up. I asked what they were told and what they knew, many questions surfaced and many things were not understood. • I am often surprised at how many times the reiteration is wrong, so we go through it again. • I have been able to catch many misunderstandings about when you give home meds using teach back.
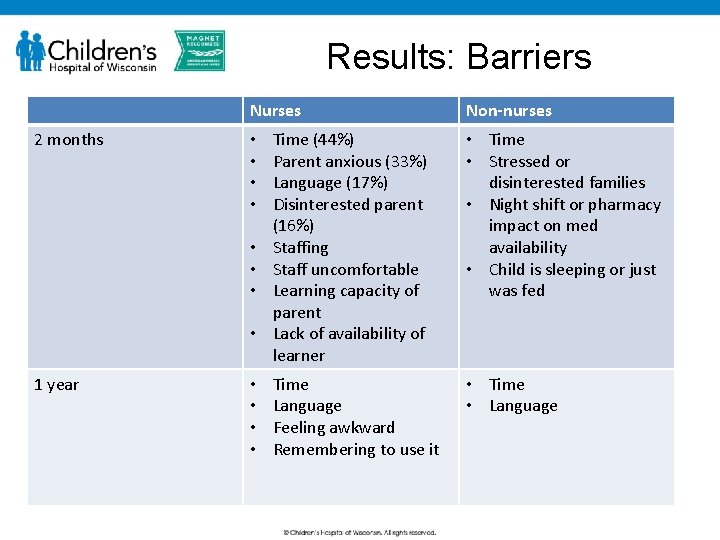
Results: Barriers Nurses 2 months • • 1 year • • Non-nurses Time (44%) Parent anxious (33%) Language (17%) Disinterested parent (16%) Staffing Staff uncomfortable Learning capacity of parent Lack of availability of learner • Time • Stressed or disinterested families • Night shift or pharmacy impact on med availability • Child is sleeping or just was fed Time Language Feeling awkward Remembering to use it • Time • Language

Quotes • Feels cumbersome, takes time and I feel like I’m quizzing them. • Parents are in a huge rush to leave and just want to get out of here. So they kind of listen but kind of don’t. • A lot have chronically ill children and maybe feel as though they already are competent in caring for them. They get defensive when you try to review it with them. • Still feeling awkward. • Need to remember to use.

Results: Other Comments Nurses and non-nurses 2 months • • 1 year Good openers are helpful and scripting helpful Hearing good catches are important Helpful intervention Universal tool to assess health literacy on admission is needed Improved medication print out with family friendly language Staffing adjustments especially in areas with rapid turnover Recognition of the problem and that many families are overwhelmed with information • Comments made at this point were positive over all at the strength of the intervention. • Several said they needed more time to feel comfortable with teachback. • Still wanted assessment tool for reading and health literacy.

Quotes • I have become aware of how complicated the words are that I am using when teaching that are unneeded. • I think it made me realize that many people say they understand do not. • Helpful intervention. • I believe it’s the only way to teach families. • Simple powerful tool. • Are we teaching this to residents?

Conclusions • • Coaching is needed over time. Prompts are helpful. Scripting is supportive and appreciated. Time must be given and prioritized for discharge and teaching. • Start early with teaching. • Discharge safety needs to be an organizational priority. • Language barriers need to be addressed.

Sharing Time • What stories do you have to share? • What improvements can be made in your practice given what you learned today?

What Questions Do You Have?

Resources • Always Use Teach-back! Toolkit available at: http: //www. teachbacktraining. org/ • AHRQ Health Literacy Universal Precautions Toolkit available at: http: //www. ahrq. gov/professionals/quality-patient-safety/qualityresources/tools/literacy-toolkit/index. html • Plain Language Thesaurus for Health Communications available at: https: //depts. washington. edu/respcare/public/info/Plain_Language_T hesaurus_for_Health_Communications. pdf • Ask Me 3 for Clear Health Communication from the National Patient Safety Foundation available at: http: //www. npsf. org/? page=askme 3 • Health Literacy Missouri – resources available at: http: //www. healthliteracymissouri. org/ • Center for Disease Control health literacy resources available at: www. cdc. gov/healthliteracy/

References • • Attwood, C. A. (2008). Health literacy…Do your patients really understand? American Academy of Ambulatory Care Nurses: Viewpoint, 3 -5. Betz, C. L. , Meeske, K. , Ruccione, K. , Smith, K. , & Chang, N. (2008). Health literacy: A pediatric nursing concern. Pediatric Nursing, 34(3), 231 -239. Kemp, E. C. , Floyd, M. R. , Mc. Cord-Duncan, E. , & Lang, F. (2008). Patients prefer the method of “tell back-collaborative inquiry” to assess understanding of medical information. Journal of the American Board of Family Medicine, 21(1), 24 -30. Levetown, M. (2008). Communicating with children and families: From everyday interactions to skill in conveying distressing information. Pediatrics, 121(5), e 1441 -1460. Nair, E. L. & Cienkowski, K. M. (2010). The impact of health literacy on patient understanding of counseling and education materials. International Journal of Audiology, 49, 71 -75. National Quality Forum. (n. d. ). Improving patient safety through informed consent for patents with limited health literacy. Retrieved from www. qualityforum. org. Scotten, M. (2015). Parental health literacy and its impact on patient care. Primary Care Clinical Office Practice, 42, 1 -16. Squellati, R. (2010). Health literacy: Understanding basic health information. Creative Nursing, 16(3), 110 -114).
- Slides: 39