The Spondyloarthropathies Kathryn Dao MD Arthritis Center September

The Spondyloarthropathies Kathryn Dao, MD Arthritis Center September 15, 2005 Bio. Pharma

Objectives § Identify the different spondyloarthropathies § Beware of misconceptions § Know the clinical features § Be familiar with treatment options

What does the term “seronegative” mean when applied to the term seronegative spondyloarthropathy? a) Patients do not form antibodies b) Patients are negative for HLA-B 27 c) Patients are negative for RF d) Patients are negative for ANA

Spondyloarthropathies § Seronegative Spondyloarthropathy: a misnomer !! v thought to be variant of RA, hence “seronegative” § Definition: A group of inflammatory arthropathies that share distinctive clinical, radiographic and genetic features. These diagnoses include: v Ankylosing spondylitis v Reactive arthritis (Reiter's syndrome) v Psoriatic arthritis v Enteropathic arthritis (Crohns, Ulcerative colitis)

Family of Spondyloarthropathies Reactive Arthritis IBD Associated Arthritis Juvenile Spondylitis Psoriatic Arthritis SAPHO AS Undifferentiated Spondyloarthropathy Acute Ant. Uveitis
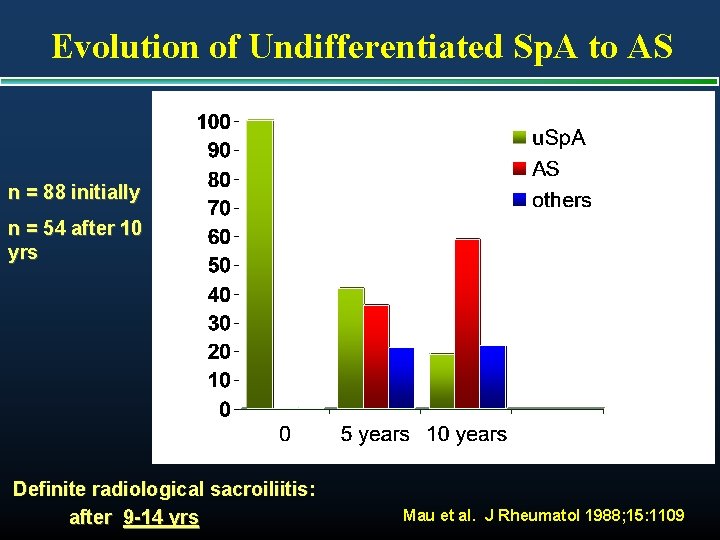
Evolution of Undifferentiated Sp. A to AS n = 88 initially n = 54 after 10 yrs Definite radiological sacroiliitis: after 9 -14 yrs Mau et al. J Rheumatol 1988; 15: 1109

Spondyloarthopathies (Sp. A) § Spondyloarthropathy: several criteria have been proposed § Key Features: v Inflammatory axial arthritis (sacroiliitis and spondylitis) v Peripheral arthritis (often asymmetric and oligoarticular) v Enthesitis v HLA-B 27 v XRay positivity evidence of erosions + hyperostosis (reactive bone) v Extra-axial, Extra-articular Features

Sp. A: Associated Extraarticular Features § Periarticular: Enthesitis, tendinitis, dactylitis (sausagedigit) § Ocular: Uveitis, Conjunctivitis § Gastrointestinal: Painless oral ulcerations, asymptomatic gut inflammation, symptomatic colitis § Genitourinary: urethritis, vaginitis, balanitis § Cardiac: Aortitis, valvular insufficiency, heart block § Cutaneous: keratoderma blennorrhagicum, psoriasis or nail lesions (onycholysis, dystrophy, pitting).
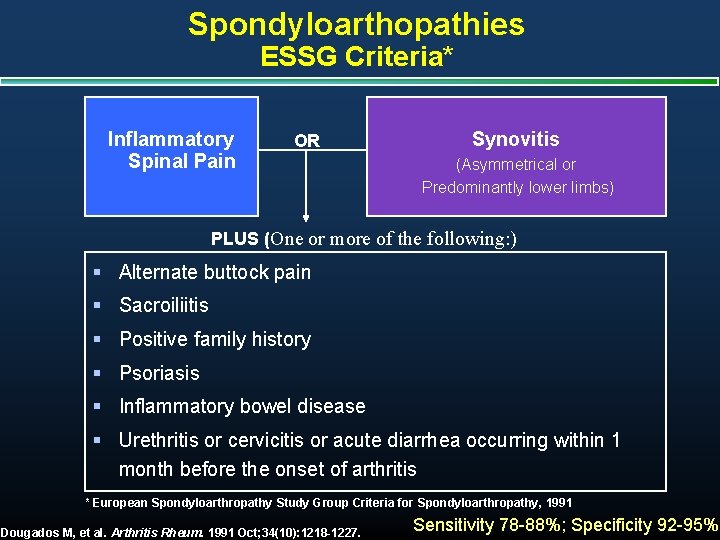
Spondyloarthopathies ESSG Criteria* Inflammatory Spinal Pain OR Synovitis (Asymmetrical or Predominantly lower limbs) PLUS (One or more of the following: ) § Alternate buttock pain § Sacroiliitis § Positive family history § Psoriasis § Inflammatory bowel disease § Urethritis or cervicitis or acute diarrhea occurring within 1 month before the onset of arthritis * European Spondyloarthropathy Study Group Criteria for Spondyloarthropathy, 1991 Dougados M, et al. Arthritis Rheum. 1991 Oct; 34(10): 1218 -1227. Sensitivity 78 -88%; Specificity 92 -95%

What is HLA-B 27? a) It is an antibody b) It is an MHC I molecule c) It is an MHC II molecule d) It is an antigen

HLA-B 27 § Class I MHC, important in antigen presentation CD 8 T cells § Associated with the spondyloarthropathies § HLA-B 27 is a normal gene found in 8% of Caucasians v 3 -4% of African-Americans, 1% of Orientals. § Risk developing AS in ANY HLA-B 27(+) person is only 1 -2%. § Over 95% of patients with ankylosing spondylitis are B 27+ § there is 20 -30% risk to 1 st degree relatives of AS patients § B 27 increases risk of SPONDYLITIS and UVEITIS BONUS: What evolutionary advantage does HLA-B 27 confer?
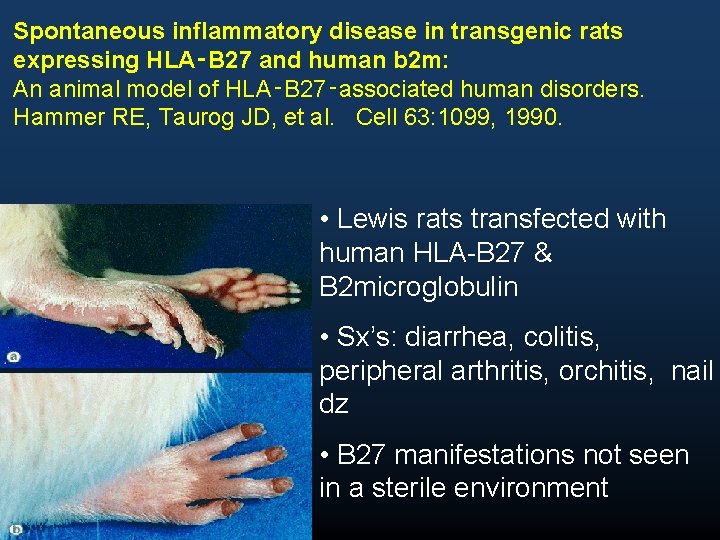
Spontaneous inflammatory disease in transgenic rats expressing HLA‑B 27 and human b 2 m: An animal model of HLA‑B 27‑associated human disorders. Hammer RE, Taurog JD, et al. Cell 63: 1099, 1990. • Lewis rats transfected with human HLA-B 27 & B 2 microglobulin • Sx’s: diarrhea, colitis, peripheral arthritis, orchitis, nail dz • B 27 manifestations not seen in a sterile environment

Clinical Associations with HLA-B 27 Khan MA. Ann Int Med 2002

Ankylosing Spondylitis
Ankylosing Spondylitis in USA

Unlike children, adults who are diagnosed with AS have SI joint involvement early in the disease (True/False)?

ANKYLOSING SPONDYLITIS § Inflammatory arthritis affects the axial spine: v starts in SI & ascends upwards to Cervical Spine § HLA-B 27+ > 90% Whites. AS occurs in 1 -2% of B 27+ persons (20% risk to 1 st degree relatives of AS pts) § More common in Caucasians than African-Americans § Male Predominant disease 5: 1 to 10: 1 § Females have less severe § Insidious disease onset between 16 -30 yrs. Rare after 45 yrs. § Juvenile spondylitis: males >9 yrs old
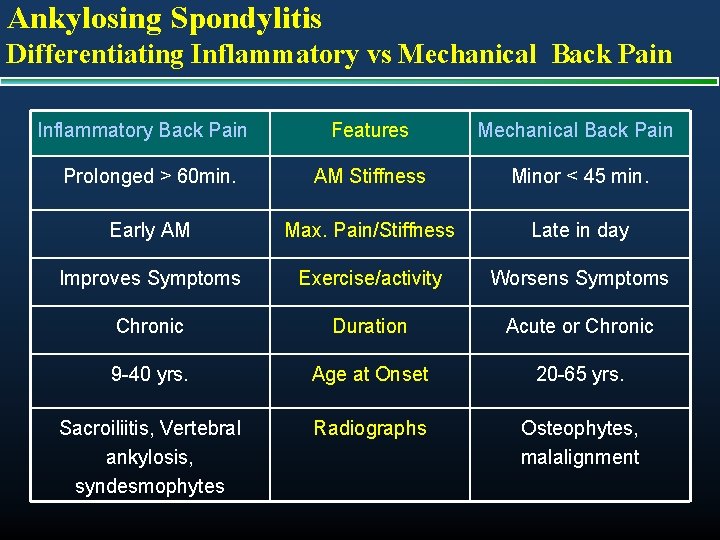
Ankylosing Spondylitis Differentiating Inflammatory vs Mechanical Back Pain Inflammatory Back Pain Features Mechanical Back Pain Prolonged > 60 min. AM Stiffness Minor < 45 min. Early AM Max. Pain/Stiffness Late in day Improves Symptoms Exercise/activity Worsens Symptoms Chronic Duration Acute or Chronic 9 -40 yrs. Age at Onset 20 -65 yrs. Sacroiliitis, Vertebral ankylosis, syndesmophytes Radiographs Osteophytes, malalignment
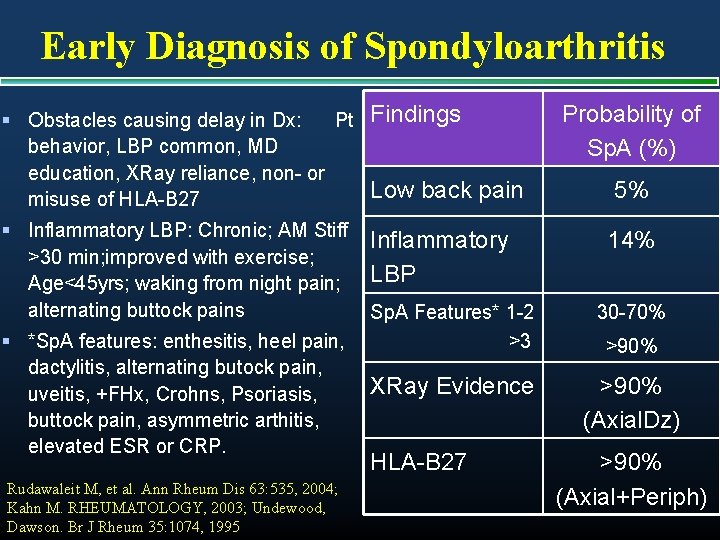
Early Diagnosis of Spondyloarthritis § Obstacles causing delay in Dx: Pt Findings behavior, LBP common, MD education, XRay reliance, non- or Low back pain misuse of HLA-B 27 § Inflammatory LBP: Chronic; AM Stiff >30 min; improved with exercise; Age<45 yrs; waking from night pain; alternating buttock pains § *Sp. A features: enthesitis, heel pain, dactylitis, alternating butock pain, uveitis, +FHx, Crohns, Psoriasis, buttock pain, asymmetric arthitis, elevated ESR or CRP. Rudawaleit M, et al. Ann Rheum Dis 63: 535, 2004; Kahn M. RHEUMATOLOGY, 2003; Undewood, Dawson. Br J Rheum 35: 1074, 1995 Inflammatory LBP Probability of Sp. A (%) 5% 14% Sp. A Features* 1 -2 >3 30 -70% XRay Evidence >90% (Axial. Dz) HLA-B 27 >90% (Axial+Periph)
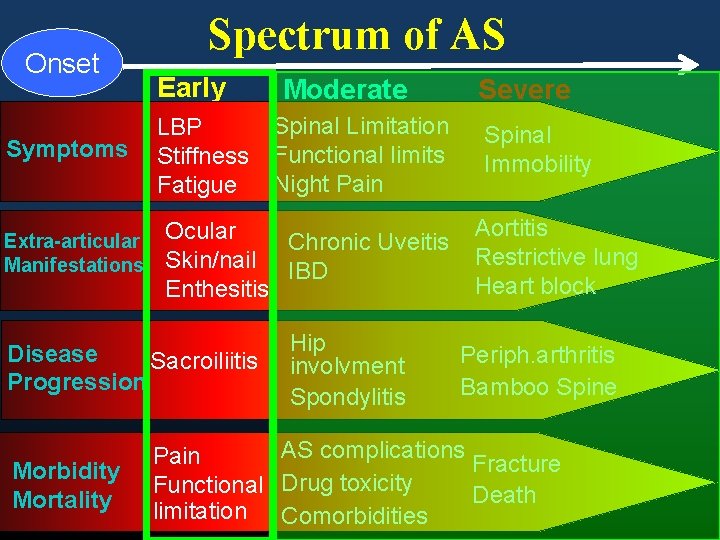
Onset Symptoms Extra-articular Manifestations Spectrum of AS Early LBP Stiffness Fatigue Spinal Limitation Functional limits Night Pain Ocular Chronic Uveitis Skin/nail IBD Enthesitis Disease Sacroiliitis Progression Morbidity Mortality Moderate Hip involvment Spondylitis Severe Spinal Immobility Aortitis Restrictive lung Heart block Periph. arthritis Bamboo Spine AS complications Pain Fracture Functional Drug toxicity Death limitation Comorbidities


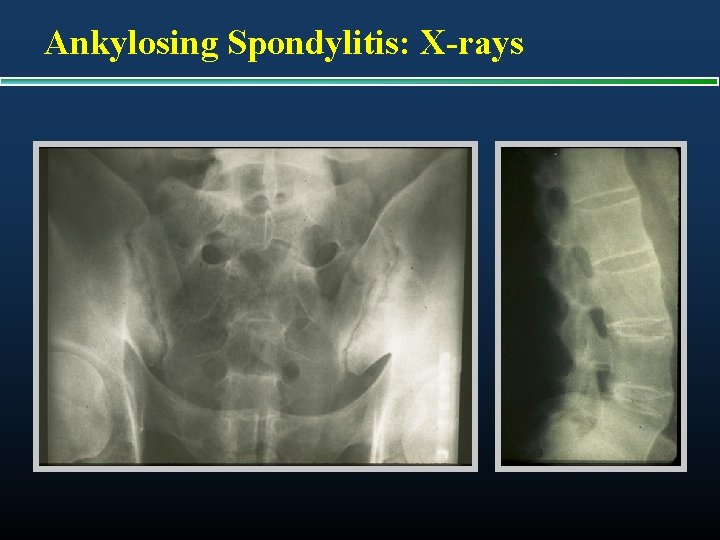
Ankylosing Spondylitis: X-rays
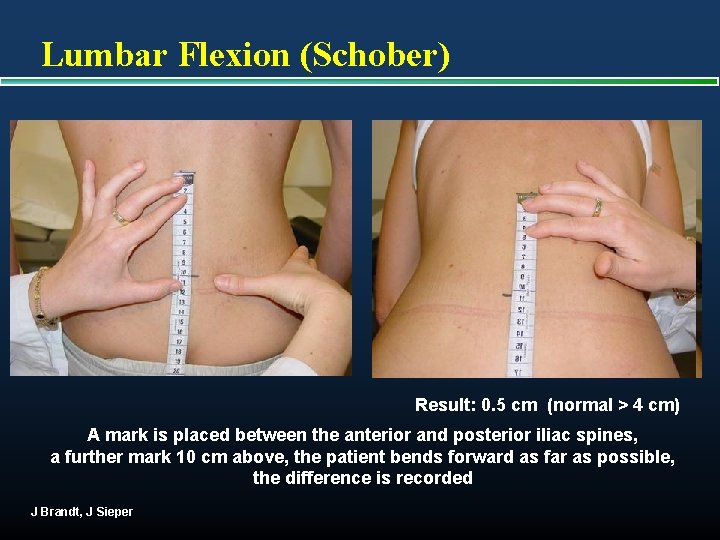
Lumbar Flexion (Schober) Result: 0. 5 cm (normal > 4 cm) A mark is placed between the anterior and posterior iliac spines, a further mark 10 cm above, the patient bends forward as far as possible, the difference is recorded J Brandt, J Sieper



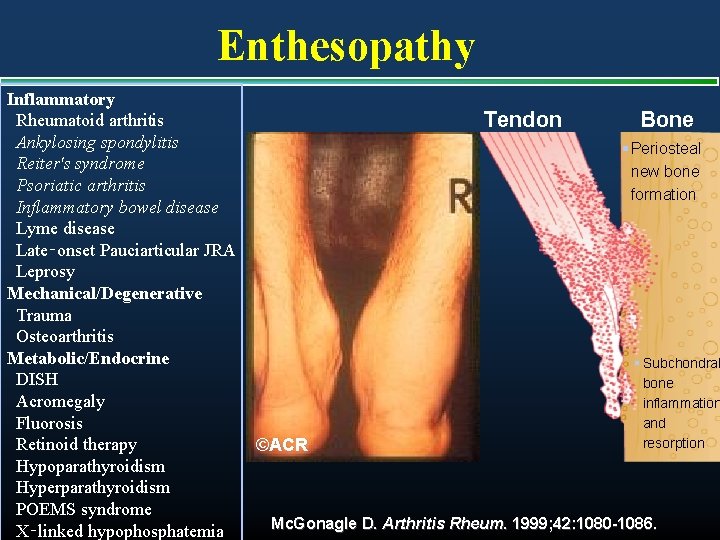
Enthesopathy Inflammatory Rheumatoid arthritis Ankylosing spondylitis Reiter's syndrome Psoriatic arthritis Inflammatory bowel disease Lyme disease Late‑onset Pauciarticular JRA Leprosy Mechanical/Degenerative Trauma Osteoarthritis Metabolic/Endocrine DISH Acromegaly Fluorosis Retinoid therapy Hypoparathyroidism Hyperparathyroidism POEMS syndrome X‑linked hypophosphatemia Tendon Bone § Periosteal new bone formation ©ACR § Subchondral bone inflammation and resorption Mc. Gonagle D. Arthritis Rheum. 1999; 42: 1080 -1086.

Severe Complications of AS § Spinal stiffness/ankylosis in kyphotic position § Spinal fractures (10 -20%) axial/T spine; incr 6 -8 fold § Severe uveitis (25 -40%) § Other organ involvement v Heart: AI, Heart Block v Lung: ILD, apical Fibrosis v kidney: amyloidosis, nephritis § Mortality: 1. 5 -4 fold increase Amyloidosis, spinal fractures, cardiovascular, gastrointestinal bleeding, pulmonary diseases, colon cancer, violence, alcohol

Reactive arthritis have been associated with all the following except: a) Chlamydia b) Ureaplasma c) Campylobacter d) Gonorrhea

REACTIVE ARTHRITIS § Acute inflammatory arthritis occuring 1 -3 weeks after infectious event (GU, GI, idiopathic) § TRIAD: arthritis + urethritis (vaginitis) + conjunctivitis (classic triad found in < one-third of pts) § Usually asymmetric oligoarticular + extraarticular Sxs v Arthritis recurrent in 15 -30%, more in chlamydial arthritis pts. § HLA-B 27+ in 75 -80% Caucasians § Post-venereal onset: more common Sex 5: 1 M: F § Post-dysenteric: less, equal M=F § Course: self limiting (< 6 mos), chronic, intermittent § Complications: Acute anterior uveitis 5%, carditis, fasciitis § Decreasing incidence in the HIV era (condom use)

Infectious Triggers for Reactive Arthritis COMMON PATHOGENS § Enteric Infections v. Shigella flexneri, serotype 2 a, 1 b v. Salmonella typhimurium, S. enteritidis v. Yersinia enterocololitica (serotypes 0: 3, 0: 8, 0: 9; SCANDINAVIA) v. Campylobacter jejuni § Urogenital Infections v. Chlamydia v trachomatis, C. pneumoniae Ureaplasma Urealyticum
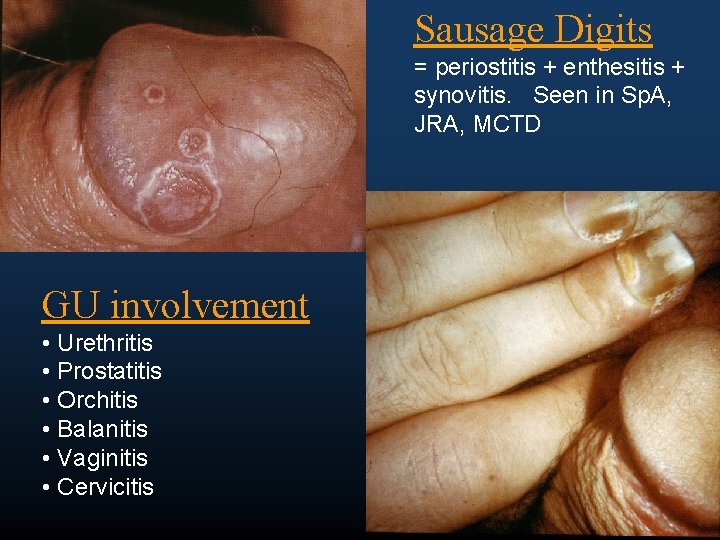
Sausage Digits = periostitis + enthesitis + synovitis. Seen in Sp. A, JRA, MCTD GU involvement • Urethritis • Prostatitis • Orchitis • Balanitis • Vaginitis • Cervicitis
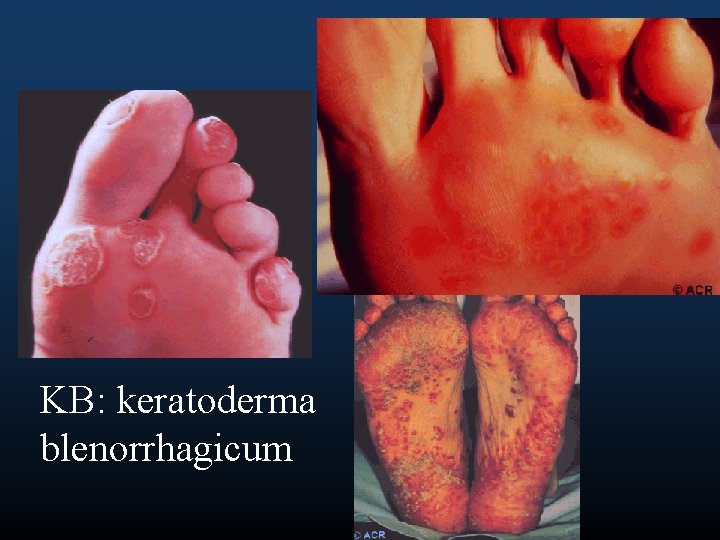
KB: keratoderma blenorrhagicum


Reactive Arthritis: Treatment • Antibotic TX (doxycycline, ciprofloxacin) x 3 mos indicated with proven Re. A • Abx do not affect outcome of Shigella, Salmonella infection Yli-Kertula, et al. ARD 62: 880, 2003 Laasila K, et al. ARD 62: 655, 2003 § 71 Re. A pts: RCT of Cipro 4 -7 yr § 1988 3 mos DBRCT showed 3 mos earlier lymecycline improved Re. A outcome: decrease duration of Chlamyda Re. A § 53 reassessed(26 cipro, 27 Placb § HLAB 27(+): 20 cipro, 25 placebo § 2003 F/U Study: 17/23 participated § Chronic Dz: 8%Cipro, 41%Placb § @ FU: 16 LBP, 10 peripheral arthritis § New Ank Sondy: 0 Cipro, 2 Plac § Sacroiliitis: § New Uveitis: 0 Cipro, 3 Placb v 1 unilateral Grade I § Conclude: 3 mos of Abx indicated in Re. A v 2 bilateral Grade II v 1 Grade IV § One AS, one chronic Sp. A § Chr. Abx doesn ‘t change outcome
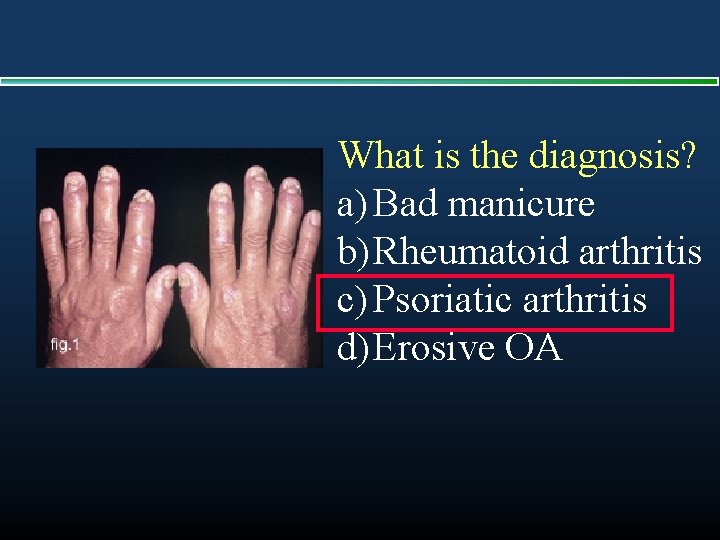
What is the diagnosis? a) Bad manicure b) Rheumatoid arthritis c) Psoriatic arthritis d) Erosive OA

PSORIATIC ARTHRITIS (Ps. A) § Chronic inflammatory arthropathy in setting of psoriasis § Etiology and genotype unclear § 1 -5% of US population has Psoriasis: 5 -42% of these develop psoriatic arthritis (skin usually precedes joints) v Frequency of Ps. A increases with disease severity and duration v Estimated 350 -400, 000 patients in USA § Nail changes: pitting, dystrophy, onycholysis § Course: chronic, destructive arthritis in 30 -50%

Classification of Psoriatic Arthritis Type Key Clinical Features Incidence Asymmetric polyarthritis or oligoarthritis Morning stiffness, DIP and PIP involvement, nail disease, 4 joints involved 40% Symmetric polyarthritis, RA-like distribution, but RF negative 25% Spondylitis Inflammatory low back pain, sacroilitis, axial involvement, 50% HLA-B 27+ 20% Distal interphalangeal joint disease Nail changes, often bilateral joint involvement 15% Arthritis mutilans Destructive form of arthritis, telescoping digits, joint lysis, typically in phalanges and metacarpals <5%



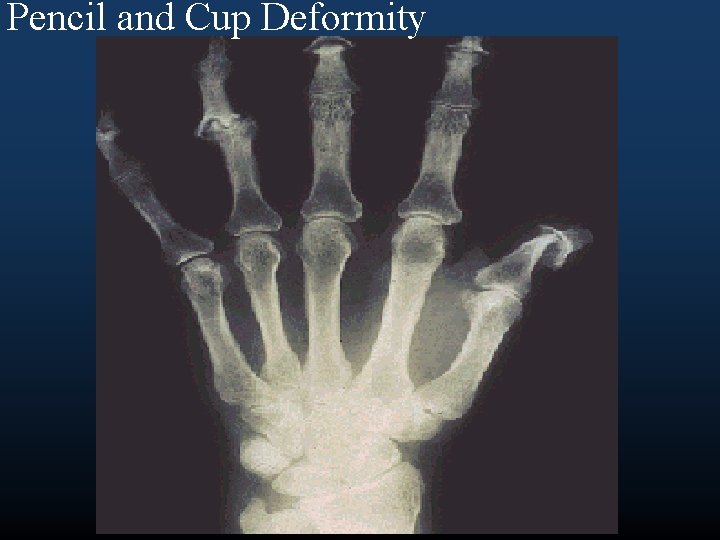
Pencil and Cup Deformity

In patients with inflammatory bowel disease and joint pains, the activity of the gut will parallel the activity of the… a) Peripheral joints b) Spine

ENTEROPATHIC ARTHRITIS § 5 -20% of IBD patients (Crohns disease or Ulcerative colitis) will develop inflammatory arthritis § Risk increases with extent of colonic dz and presence of other extraintestinal manifestations: abscesses, E. Nodosum uveitis, pyoderma gangrenosum § Gut disease may be asymptomatic for years § Subsets: v Asymmetric oligoarthritis (intermittent or chronic) v Seronegative RA-like polyarthritis 20% of IBD pts v Spondylitis 10 -15% (may be misdiagnosed as AS) § Peripheral arthritis parallels the gut! NOT THE SPINE!

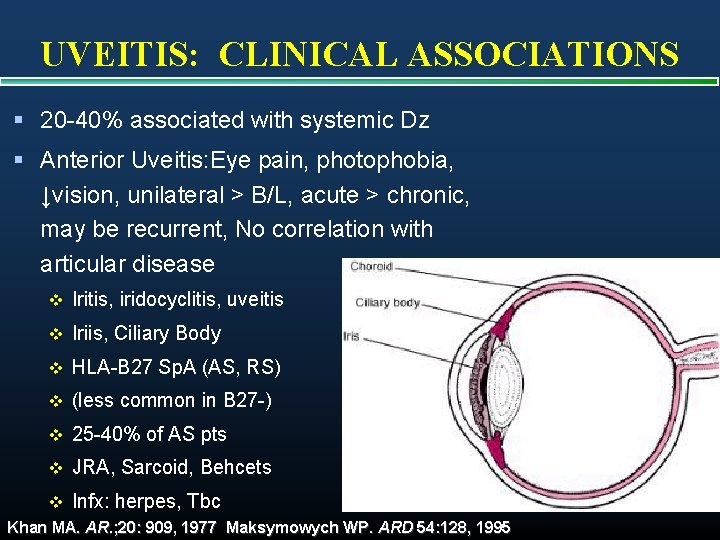
UVEITIS: CLINICAL ASSOCIATIONS § 20 -40% associated with systemic Dz § Anterior Uveitis: Eye pain, photophobia, ↓vision, unilateral > B/L, acute > chronic, may be recurrent, No correlation with articular disease v Iritis, iridocyclitis, uveitis v Iriis, Ciliary Body v HLA-B 27 Sp. A (AS, RS) v (less common in B 27 -) v 25 -40% of AS pts v JRA, Sarcoid, Behcets v Infx: herpes, Tbc Khan MA. AR. ; 20: 909, 1977 Maksymowych WP. ARD 54: 128, 1995

In a patient you suspect having a spondyloarthropathy (dactylitis, inflammatory back pain symptoms, and heel pain), what do you give to help them until they can see a rheumatologist? a) steroids b) methotrexate c) sulfasalazine d) NSAIDs

Sp. A: Therapeutic Options § Nonpharmacologic measures v Patient education, joint protection, maintenance of function and posture (Ankylosing Spondylitis Association, Arthritis Foundation) v Exercise, rest, physical therapy, diet, vocational counseling § Pharmacologic therapies: the Big Hurt v Analgesic agents: too little too late v NSAIDs - Mainstays of therapy (when disco was happening) v Corticosteroids - rarely used; rarely effective v DMARDs: (SSZ, MTX) who were we fooling? v Biologics: (anti-TNF therapies) are they for real?

NSAIDs § Effective: inflammatory back pain, spinal stiffness, peripheral arthritis, enthesopathy § No evidence that NSAIDs inhibit disease progression v ACR 2003 Wanders, vander Heijde: celecoxib Rx pts less progression § FDA-approved NSAIDs for AS: phenylbutazone Indomethacin, indomethacin-SR, enteric coated acetylsalicylic acid, naproxen, sulindac, diclofenac. § Anecdotal reports & few studies suggest that specific NSAIDs may be more effective: v phenylbutazone: v indomethacin: v diclofenac: limited availability: risk of agranulocytosis especially in long acting form. CNS Sx? as effective as Indocin, less toxic? LFTs!

NSAID Resistant AS/Sp. A § Consider DMARDs when: v Antiinflammatory v Progression v Active therapy is insufficient to control Sxs of inflammatory axial disease persisent polyarthritis v Uncontrolled extra-articular disease § But Which DMARD? v None shown to be effective at Axial disease v None FDA approved for AS, Sp. A v MTX indicated in psoriasis – not psoriatic arthritis – Hepatotoxicity Issues v Reliance on anecdotes and RA experience

Ineffective DMARDs § Gold - no proven benefit! v Intramuscular (aurothioglucose, aurothiomalate) v Auranofin 238 AS pts: no effect on Axial dz; but +effect on MD global, function v Primarily studied in psoriatic arthritis > AS > Reactive § Hydroxychloroquine v Controlled and uncontrolled trials in psoriatic arthritis, suggesting some efficacy. § Azathioprine: Uncontrolled and controlled trials in Re. A and psoriatic arthritis § MTX: no benefit in AS v Beneficial in psoriasis and psoriatic arthritis

Conclusion Spondyloarthropathies v. Inflammatory arthropathies v. Share genetic, clinical and radiologic features v. Ag driven immune response causing symptoms v. New therapies allow for more effective management of these diseases

Sulfasalazine in Sp. As: AS, Ps. A, and Re. A § 619 patients v Axial disease (n=187) v Peripheral v SSZ v 36 articular (n=432) 2 gr/day vs Placebo weeks § Results: v Axial – no SSZ response v Peripheral – favor SSZ (P=0. 0007) § SSZ effective for peripheral arthritis of Sp. As Clegg DO, et al. Arthritis Rheum. 1999; 42: 2325 -2329.

Rationale for TNF Therapy in Spondyloarthropathies § Sp. A Primary Pathology = Enthesitis v Mc. Gonagle D, etal. Curr Opin Rheum 11: 244, 1999 § Transgenic mice overexpressing TNF develop enthesitis and arthritis resembling AS w/ axial skeletal kyphosis & ankylosis with inflammatory & fibrotic change @ end plates, entheses v Crew MD, et al. J Interferon Cytokine Res. 18: 219, 1998 § Localization of TNF in Sacroiliac joints v Stone M, et al. Arthritis Rheum 2000 [abstract] § Osteoclasts and Synoviocytes in Ps. A express RANKL - Ritchlin C, et al. ACR 2001 § Therapeutic benefit of TNF inhibition in AS & Ps. A
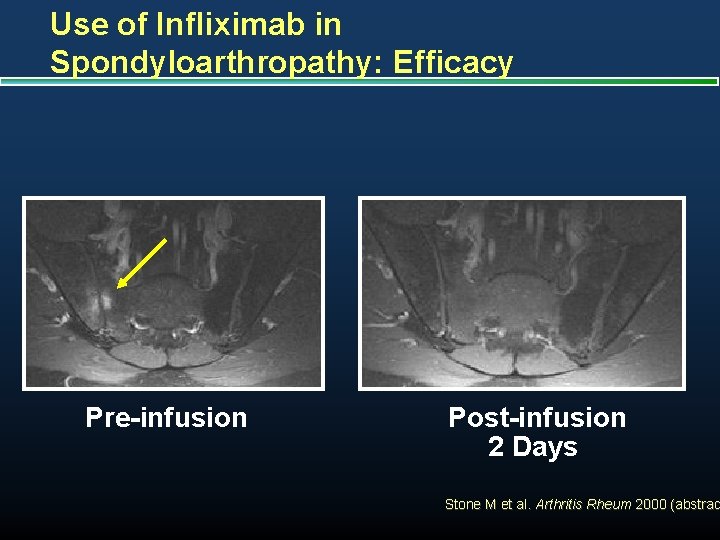
Use of Infliximab in Spondyloarthropathy: Efficacy Pre-infusion Post-infusion 2 Days Stone M et al. Arthritis Rheum 2000 (abstrac

BASDAI § The Bath Ankylosing Spondylitis Disease Activity Index (BASDAI) measures disease activity based on 6 selfadministered questions relating to: v Fatigue v Spinal pain v Peripheral arthritis v Enthesitis v Morning stiffness : 2 questions (meaned) Average 1 - 5/6; range 0 -10 Garrett S, et al. J Rheumatol. 1994; 21: 2286 -2291.

ASAS 20 Preliminary Response Criteria AS Improvement of 20% AND 10 units in at least 3 domains Patient global VAS Patient Pain VAS Function (BASFI) Stiffness (BASDAI) No worsening in remaining domain ASAS Partial Remission: < 20 in all 4 domains Anderson et al Arthritis Rheum 2001: 44: 1876 -886
- Slides: 58