The Skinny on Atopic Dermatitis Robyn Morrissette PAC

The Skinny on Atopic Dermatitis Robyn Morrissette, PA-C Division of Allergy and Immunology Pediatric Specialists of Virginia

No conflicts of interest to disclose.

Learning Objectives: 1. To understand how to recognize and diagnose atopic dermatitis 2. To learn the clinical presentation of atopic dermatitis 3. To review common treatments for atopic dermatitis 4. To review developing treatment for atopic dermatitis in the pediatric population 5. To review the association with food allergies.

• • • Case: Julia 7 month old female Referred to clinic by PMD for evaluation of a rash and to find the cause, concerned it is a food allergy Rash started around 3 mo and has worsened over last 3 months Started on the cheeks initially but is spreading to trunk Seems uncomfortable and itchy Has been told not to bathe every day as this will make the skin worse

• • • Case Report: Julia Mom has been moisturizing with Aveeno twice a day Given Hydrocortisone 2. 5% to use twice a day sparingly and only for 1 week. Medication worked but mom was nervous to use it again Rash seems to get worse if Julia is upset Rash seems worse if it is hot outside or if Julia is hot Seems to have difficulty sleeping when the rash is really bad


What is your diagnosis? What would you do?

What is Atopic Dermatitis? • Chronic pruritic inflammatory skin disease • Affects about 13% of children and about 7% of adults in the US alone • Also known as eczema • Often called the “itch that rashes”

What is Atopic Dermatitis? • Exact cause is unknown • Thought to be due to a “leaky” skin barrier • Do know there is an association with the Filaggrin gene and increased risk for AD • Also some link to substances that contain proteins called proteases – proteases break the link between the skin cells and make the skin barrier leaky

What is Atopic Dermatitis? • Sensitization to environmental allergens and food allergens commonly seen but is not a cause • Is an allergic spectrum disorder as patients with moderate to severe disease often have elevated serum Ig. E • About 70% patients have a positive family history of atopic diseases – Risk can increase to 3 -5 fold if both parents have atopic disease

Clinical Presentation of Atopic Dermatitis • Presentation varies widely • Childhood onset begins early in life – About 50% in first year – About 85% by age 5 • Can persist into adulthood in anywhere from 2050% of patients • Can have adult onset – Reported by about 26% of adult patients

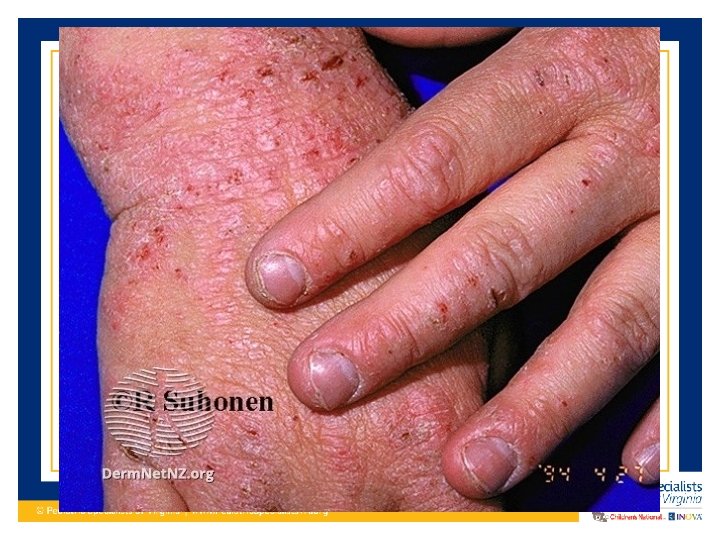
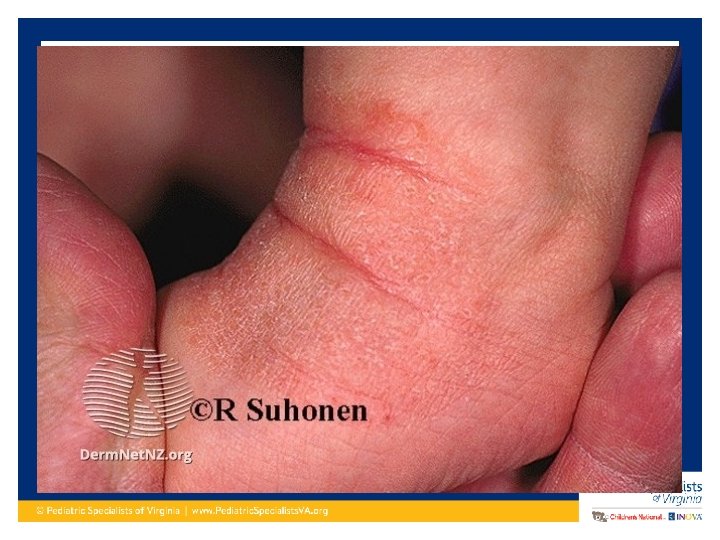
Clinical Presentation of Atopic Dermatitis • Dry skin and severe pruritis • Erythematous maculo-papular rash • Vesicles that can have exudate and crusting (acute flare) • Dry, scaly, excoriated patches (more chronic lesions) • Lichenification (chronic) • Hyper/hypo-pigmentation

Clinical Presentation of Atopic Dermatitis • • • Excoriations at various stages of healing Persistent fidgeting due to pruritis Irritability Insomnia due to pruritis at night Decreased concentration secondary to itching and being uncomfortable

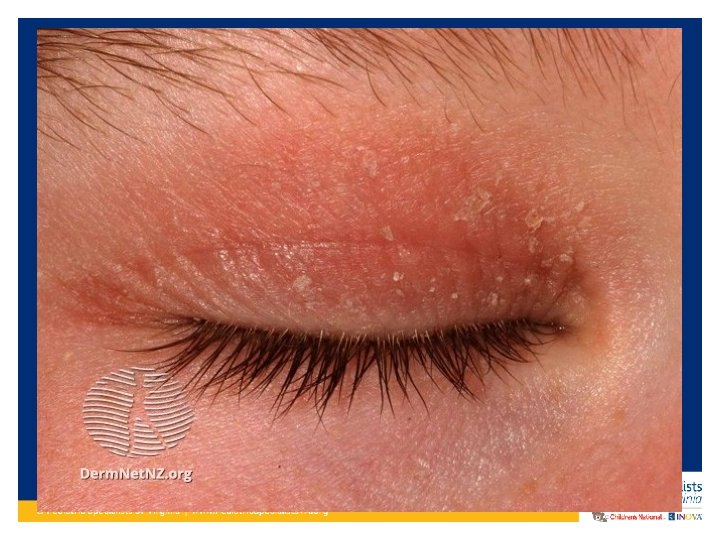
Clinical Presentation of Atopic Dermatitis • In infants to around age 2: Commonly starts on face and scalp. Sometimes on extensor surfaces. – Typically spares the genitalia/diaper area • Age 2 – teenager: Presents more on the flexor surfaces – Typical antecubital fossa and popliteal fossa presentation – Volar aspect wrists, ankles, neck • Adults: Continues on flexor surfaces and also on hands

Diagnosing Atopic Dermatitis • Clinical diagnosis based on history and presentation • Rule out other dermatologic conditions • Rule out rare immunodeficiency conditions such as hyper-Ig. E syndrome and Omenn syndrome – Eczema accompanied by other symptom such as failure to thrive, skin abscesses, cutaneous viral infection, chronic diarrhea – In adults need to rule psoriasis and cutaneous T-cell lymphoma
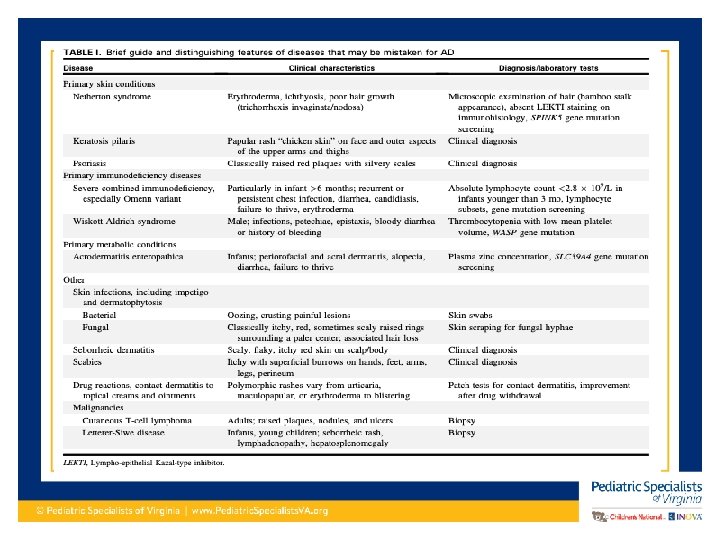
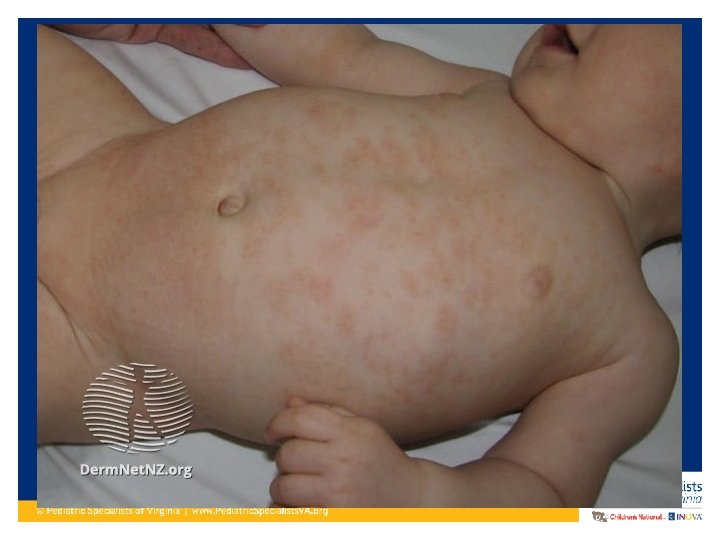
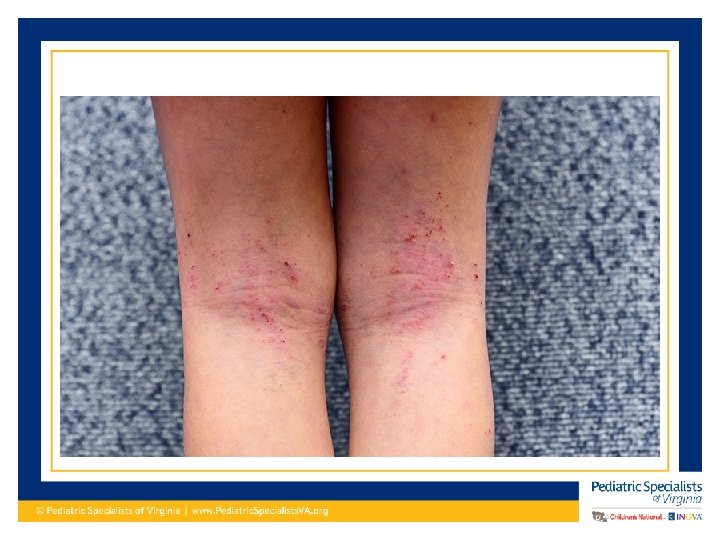
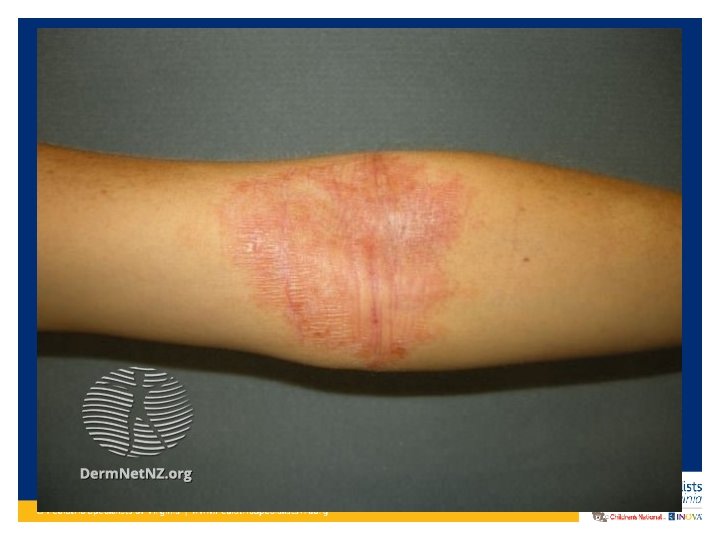

Diagnosing Atopic Dermatitis • Several sets of criteria have been developed • Hanifin-Rajka (H-R) criteria considered the gold standard • United Kingdom Working Party (UKWP) abridged version of H-R criteria, tends to work better for pediatric diagnosis • Not allergist/dermatologist use a diagnosing criteria


Treatments for Atopic Dermatitis

Treatments for Atopic Dermatitis • Accepted for publication June 26, 2019 • Includes newer topical medications like Crisaborole (Eucrisa)
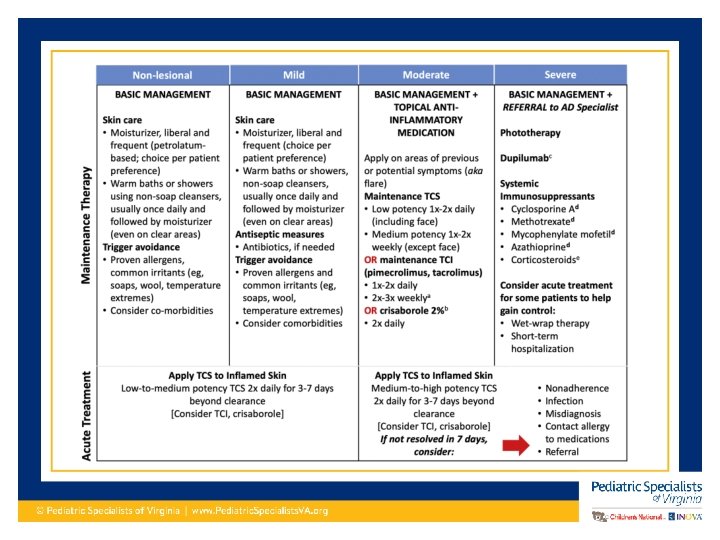

Treatments for Atopic Dermatitis • Treatment is daily given the chronicity of the disease • Multifaceted • Personalized to the patient and severity • Often requires review at follow up visits to ensure compliance

Treatments for Atopic Dermatitis • Atopic Derm myth #1: Baths make AD worse. • Every patient no matter severity gets daily care of basic management (bath and moisturizing) • Daily bath Soak and seal – 15 -20 minutes warm, clean water – Infants/small kids place wash cloth over areas not under water and continue to wet – Older kids can do shower – Soaps do not have to be done daily. If used, use at end and rinse immediately then out of bath. – Pat dry – Apply emollients (Aquaphor or Vaseline)

Treatments for Atopic Dermatitis • Recommend moisturizing in the morning and at bedtime after bath. • Should do at least 1 more time mid-day/afterschool • Can be done as needed • Infants – easy to tell parents to do with diaper changes • Older patients can use non-fragranced lotion (Cera. Ve, Aveeno, Cetaphil, Eucerin)

Treatments for Atopic Dermatitis • Avoidance of triggers (allergens and irritants) – – – Fragrances Wool Temperature extremes Foods Soaps/detergents

Treatments for Atopic Dermatitis • Topical Medications – Topical corticosteroids (Hydrocortisone, Triamcinolone, Desonide, etc) – Topical calcineurin inhibitors (pimecrolimus and tacrolimus) – Phosphodiesterase-4 inhibitor (Crisaborole) – Systemic immunosuppressants (Cyclosporine, Methotrexate) • Injectable medications – Dupilumab • Oral antihistamines

Treatments for Atopic Dermatitis Topical Steroids • Atopic Derm Myth #2: Use steroids sparingly and only for 7 days and no more. • Topical steroids applied twice a day to flare • Use a thick layer of the medication • Prefer ointment over creams/lotions • Use lowest potency that still controls the symptoms • Use until area clears then 2 -3 more days • Can use up to 14 days in a row before needing to take a break

Treatments for Atopic Dermatitis Topical Steroids • In some patients with severe atopic derm can do a daily preventive application of topical steroids – Typically done under supervision of Allergist or Dermatologist • Safe to use in infants • Side effect profile is mild if used appropriately – Side effect of topical steroids discoloration of the skin and thinning of the skin – Minimal absorption systemically if used appropriately

Treatments for Atopic Dermatitis • • • Topical Calcineurin inhibitor Includes Pimecrolimus and Tacrolimus Approved in use for patients age 2 years and older Popular for use on eyelid atopic dermatitis and hand dermatitis Can use up to 14 days in a row Side effect profile is mild if used appropriately – Most common side effect is redness initially at the application site improves with use – Can make you more photosensitive

Treatments for Atopic Dermatitis • • • Topical PDE 4 inhibitiors Crisaborole (brand name Eucrisa) Approved December 2016 Ages 2 and older Nonsteriodal topical ointment that inhibits PDE 4 (intracellular mediator of inflammation that degrades cyclic adenosine monophosphate) Can be applied anywhere except in the eyes, in the mouth, or vaginally

Treatments for Atopic Dermatitis Topical PDE 4 inhibitiors • Applied twice a day • No limitation in how long it can be used • Side effect profile is mild – Most common side effects include redness and pain at application – In our clinic majority of patients who come in on this medication have stopped if for these reasons
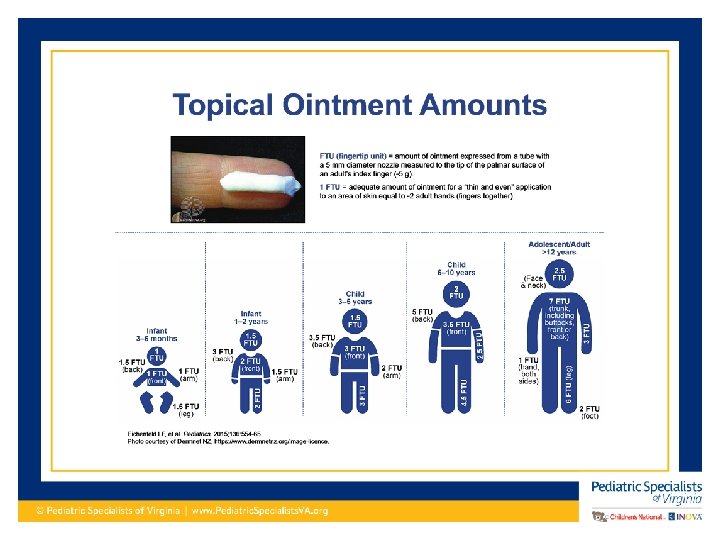


Treatments for Atopic Dermatitis Additional Therapies • Oral antihistamines to control itching – Cetirizine can be used as young as 6 months old – Hydroxyzine at bedtime to control itch and help sleep • Topical and oral antibiotics as needed for superinfection • Wet wrapping: Intense moisture therapy involving wrapping affected areas overnight for 5 nights – https: //www. nationaljewish. org/conditions/eczemaatopic-dermatitis/eczema-treatment/wet-wrap-therapy

Treatments for Atopic Dermatitis Additional Therapies • Biologics: – Newest medication approved for treatment of moderate -severe atopic dermatitis – Dupilumab (Brand name: Dupixent) • Monoclonal antibody that targets IL-4 receptor alpha-chain subunit common to IL-4 and IL-13 • Injectable medication • Reduction of pruritis • Reduction in symptoms of anxiety and depression • Improvement in quality of life • Approved for 12 years and older • Done under supervision of Allergist and/or Dermatologist

Treatments for Atopic Dermatitis Additional Therapies • • Bleach bathes Phototherapy Hospitalization for intense eczema care Systemic immunosuppressants

Atopic Dermatitis and Food Allergies • Commonly see patients with AD have food allergies but as discussed above it is not the cause • Can be at increased risk for food allergies • LEAP study – risk factors included severe eczema – Increased risk of peanut allergy if not introduced early • NIH study
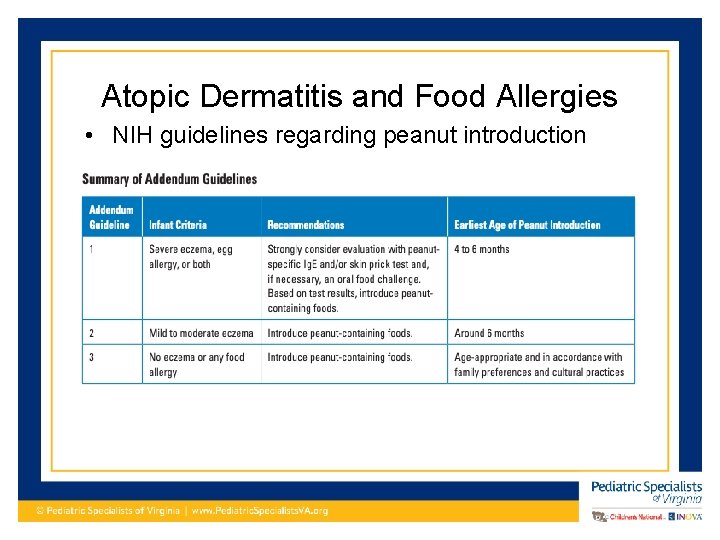
Atopic Dermatitis and Food Allergies • NIH guidelines regarding peanut introduction

Atopic Dermatitis and Food Allergies • Broad panel serum Ig. E or skin prick testing is not recommended in patients with eczema • Broad panel testing can lead to unnecessary food avoidances and potential development of food allergies due to avoidances • FARE blog post from December 2015 does a great job discussing research – http: //www. foodallergy. org/about-fare/blog/newresearch-on-food-allergies-and-atopic-dermatitis • History can help with difference between allergic reaction and food triggered eczema

Back to baby Julia… • Started daily eczema care plan including: – Daily bath – Frequent moisturizing with Vaseline or Aquaphor – Topical Desonide to face/neck flare ups and topical Triamcinolone to body flare ups – Cetirizine in the morning as needed for itching and Hydroxyzine at bedtime as needed for itching • Once the eczema was controlled addressed food allergy concerns – Skin testing negative to egg and peanut – Introduction at home

Questions? ?

Sources Fishbein, A, Silverberg, J, Wilson, E, Ong, P. Update on Atopic Dermatitis: Diagnosis, Severity Assesment, and Treatment Selection. The Journal of Allergy and Clinical Immunology: In Practice. https: //doi. org/10. 1016/j. jaip. 2019. 06. 044 Weston, W, Howe, William. Atopic dermatitis (eczema): Pathogenesis, clinical manifestations, and diagnosis. https: //www. uptodate. com/contents/atopic-dermatitis-eczemapathogenesis-clinical-manifestations Photos property of Dermnetnz. org

Sources Schneider, L, Tilles, S, Lio, P, et. al. Atopic Dermatitis: A Practice Paramater Update 2012 https: //www. aaaai. org/aaaai/media/Media. Library/PDF%20 doc uments/Practice%20 and%20 parameters/Atopic-Dermatitis 2013. pdf
- Slides: 49