The Rise of Antibiotic Resistant Bacteria By Ugiloy

The Rise of Antibiotic Resistant Bacteria By Ugiloy Hamrayeva, Farah Etienne, Ibeth Erazo DEN 1200 - E 601
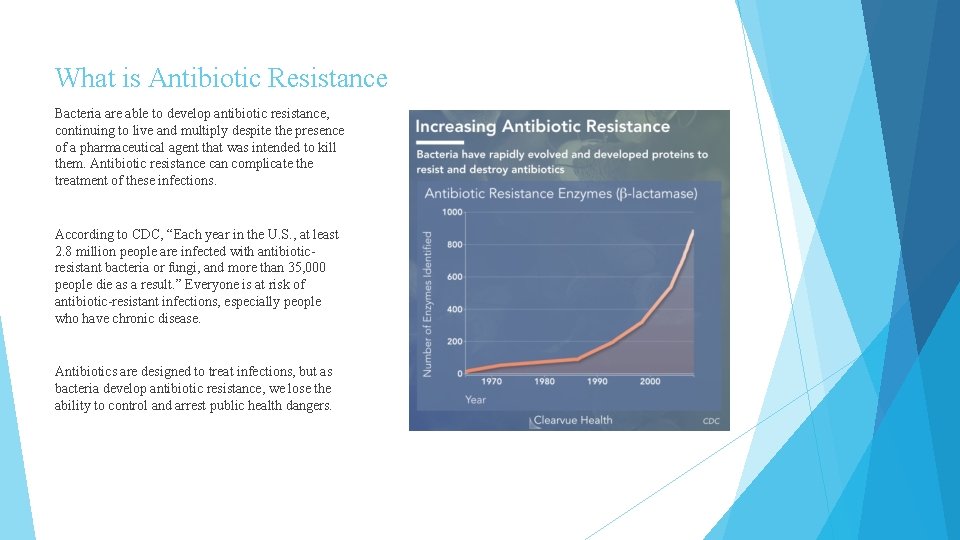
What is Antibiotic Resistance Bacteria are able to develop antibiotic resistance, continuing to live and multiply despite the presence of a pharmaceutical agent that was intended to kill them. Antibiotic resistance can complicate the treatment of these infections. According to CDC, “Each year in the U. S. , at least 2. 8 million people are infected with antibioticresistant bacteria or fungi, and more than 35, 000 people die as a result. ” Everyone is at risk of antibiotic-resistant infections, especially people who have chronic disease. Antibiotics are designed to treat infections, but as bacteria develop antibiotic resistance, we lose the ability to control and arrest public health dangers.

The Effect of Drug Resistant Bacteria in Oral Health Due to increased number of antibiotics prescribed in the dental setting, there is a rise of drug resistant bacteria that effects the oral health. The reasons behind the overprescribed medication might vary from patients’ request to dental professionals' lack of knowledge about the side effects of antibiotics. According to CDC, “appropriate antibiotic prescribing should be in accordance with evidence-based national and local clinical practice guidelines, when available. ” In accordance with these guidelines, it is vital to prescribe the proper amount of antibiotics only when necessary. This presentation will explore and analyze three scientific trials which are focused on therapeutic use of antibiotics and antimicrobial substances and its effect in oral health.
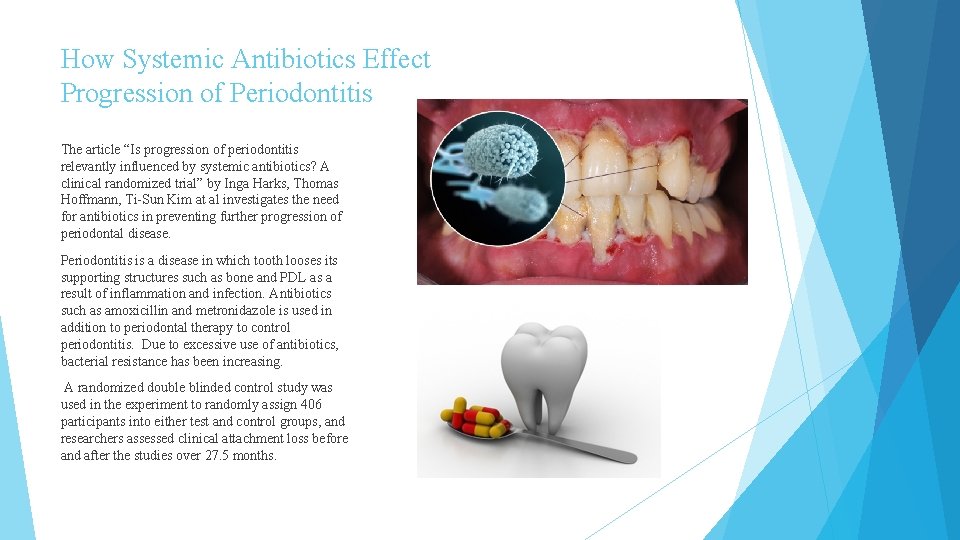
How Systemic Antibiotics Effect Progression of Periodontitis The article “Is progression of periodontitis relevantly influenced by systemic antibiotics? A clinical randomized trial” by Inga Harks, Thomas Hoffmann, Ti-Sun Kim at al investigates the need for antibiotics in preventing further progression of periodontal disease. Periodontitis is a disease in which tooth looses its supporting structures such as bone and PDL as a result of inflammation and infection. Antibiotics such as amoxicillin and metronidazole is used in addition to periodontal therapy to control periodontitis. Due to excessive use of antibiotics, bacterial resistance has been increasing. A randomized double blinded control study was used in the experiment to randomly assign 406 participants into either test and control groups, and researchers assessed clinical attachment loss before and after the studies over 27. 5 months.

The results of the Study Statistical analysis of the experiment reveals that the percentage of sites with attachment loss was 7. 8% in the control group and 5. 3% in the test group. Based on the statistical analysis of the experiment, further development of periodontal disease was prevented for both the test group (antibiotics) and the control group (placebo). The study revealed that mechanical removal of debris was effective in the prevention of clinical attachment loss regardless of the use of antibiotics.

Testing Bacteria for Antibiotic Sensitivity The major contributor to antibiotic resistance is the indiscriminate use of antibiotics. This includes using antibiotics that are ineffective at treating infections involving desensitized bacteria. For the article titled “Antibiotic sensitivity and resistance of bacteria from odontogenic maxillofacial abscesses”, Sang-Hoon Kang and Moon-Key Kim conducted a retrospective study in order to identify the antibiotic resistance of bacteria that are present in odontogenic abscesses. They collected pus specimens from 1, 772 patients with maxillofacial abscesses during an incision and drainage procedure. The bacteria were then cultured, identified (2, 489 strains in total, categorized as either gram-negative or grampositive), and exposed to 20 different antibiotics to test for sensitivity, resistance, and intermediate susceptibility.
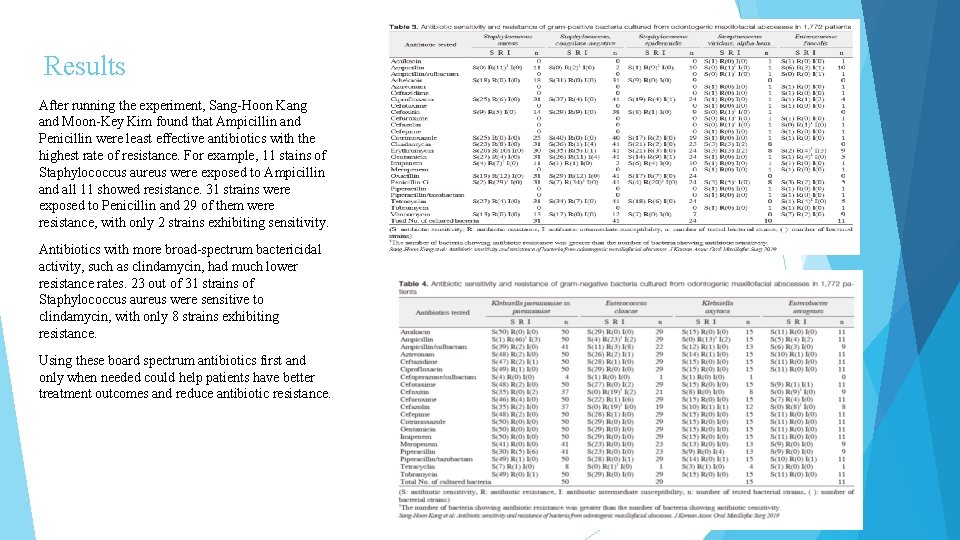
Results After running the experiment, Sang-Hoon Kang and Moon-Key Kim found that Ampicillin and Penicillin were least effective antibiotics with the highest rate of resistance. For example, 11 stains of Staphylococcus aureus were exposed to Ampicillin and all 11 showed resistance. 31 strains were exposed to Penicillin and 29 of them were resistance, with only 2 strains exhibiting sensitivity. Antibiotics with more broad-spectrum bactericidal activity, such as clindamycin, had much lower resistance rates. 23 out of 31 strains of Staphylococcus aureus were sensitive to clindamycin, with only 8 strains exhibiting resistance. Using these board spectrum antibiotics first and only when needed could help patients have better treatment outcomes and reduce antibiotic resistance.

DEVELOPMENT OF RESISTANCE TO ANTIMICROBIAL MOUTHRINSES In a RCT conducted by the School of Dental Medicine of the University of Basel - Switzerland title “DEVELOPTMENT OF RESISTANCE OF MUTANS STREPTOCOCCI AND PORPHYROMONAS GINGIVALIS TO CHLORHEXIDINE DIGLUCONATE AND AMINE FLUORIDE/STANNOUS FLUORIDE-CONTAINING MOUTHRINSES, IN VITRO” the following was analyzed. • Prevention and treatment of oral diseases focus primarily on the removal of the dental biofilm. • The treatment is frequently combined with the use of the antimicrobials chlorhexidine (CHX) and Am. F/Sn. F 2 in mouth rinses and toothpaste. • Products containing these antimicrobial substances have proven to reduce the need for antibiotic treatment. • Prolonged use of these antimicrobial substances might lead to the resistance of oral bacteria to their components in the long term. • Few studies have already reported that some oral pathogens can become resistant to antiseptics after exposure.
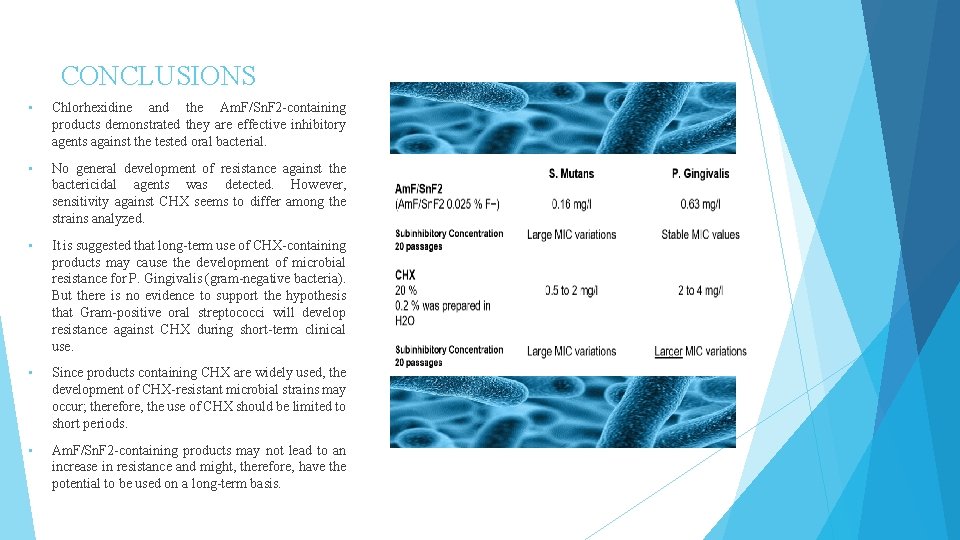
CONCLUSIONS • Chlorhexidine and the Am. F/Sn. F 2 -containing products demonstrated they are effective inhibitory agents against the tested oral bacterial. • No general development of resistance against the bactericidal agents was detected. However, sensitivity against CHX seems to differ among the strains analyzed. • It is suggested that long-term use of CHX-containing products may cause the development of microbial resistance for P. Gingivalis (gram-negative bacteria). But there is no evidence to support the hypothesis that Gram-positive oral streptococci will develop resistance against CHX during short-term clinical use. • Since products containing CHX are widely used, the development of CHX-resistant microbial strains may occur; therefore, the use of CHX should be limited to short periods. • Am. F/Sn. F 2 -containing products may not lead to an increase in resistance and might, therefore, have the potential to be used on a long-term basis.

'To Make a Long Story Short' • Antibiotic resistance and “superbugs” have become a pressing issue in the medical community in recent years. • Oral bacteria has the capacity to adapt and thrive under different treatments. • There is urgency for the control of antibiotic prescriptions in addition to therapeutic measures that are taken by therapist. • A new alert has risen because oral bacteria is showing also certain degree of resistance to habitual over the counter antimicrobial mouth rinses. • Individual risk assessments of the patient are important because they can give a better approach how each patient can react. • Patients should be informed about diverse effects of antibiotic treatments and its effect on the immune system.

The Role of the Dental Team • Since the guidelines for premedication have been changed to reduce the amount of antibiotics being prescribed, it is important for the dental team to be familiar with these kinds of research findings to help them understand why. • Although dental hygienists do not prescribe antibiotics, understanding the scientific literature can help them provide education to their patients. • These statistics will help dentists make better decisions about when antibiotic use is necessary and which antibiotics would be most effective. This will result in better outcomes for our patients.

As a future dental hygienist… • It is our role to investigate and research the effects of any drugs that can be used or prescribed during the treatment. Therefore, it is vital to be informed and educated on current studies. • It is important to have a better understanding of the long-term effects of antibiotics and common antimicrobial substances because it would give the capacity to detect success or failure of a given treatment since resistance could be developed at any stage. • It is our responsibility to educate and give instructions to the patients.

References • https: //www. cdc. gov/drugresistance/about. html. 10 February 2020. Document. 16 March 2020. • https: //www. ada. org/en/member-center/oral-health-topics/antibiotic-stewardship. 1 November 2019. Document. 16 March 2020. • Harks I, Koch R, Eickholz P, et al. Is progression of periodontitis relevantly influenced by systemic antibiotics? A clinical randomized trial. J Clin Periodontol. 2015; 42(9): 832– 842. doi: 10. 1111/jcpe. 12441 • Kulik, E. M. , Waltimo, T. , Weiger, R. et al. Development of resistance of mutans streptococci and Porphyromonas gingivalis to chlorhexidine digluconate and amine fluoride/stannous fluoride-containing mouthrinses, in vitro. Clin Oral Invest 19, 1547– 1553 (2015). • https: //www. unioncityoralsurgerygroup. com/are-antibiotics-necessary-for-oral-and-maxillofacial-surgery/ • https: //img. medscape. com/thumbnail_library/is_190722_gingivitis_bacteria_800 x 450. jpg • http: //viswajyothi. org/wp-content/uploads/2017/02/results. jpg • https: //healthcare-in-europe. com/media/story/22705/rect-01 -pilt-2. jpg • https: //blog. mattbierner. com/content/2015 -11 -22 -keyboard-bacterial-culture/bacteria-in-a-petri-dish-compressed. jpg • Sang-Hoon Kang et al: Antibiotic sensitivity and resistance of bacteria from odontogenic maxillofacial abscesses. J Korean Assoc Oral Maxillofac Surg 2019 Tables 3 and 4 • https: //www. clearvuehealth. com/images/antibiotic-resistance-research-statistics. 002. jpg • https: //dentalsave. com/wp-content/uploads/2017/03/prescription-drugs. jpg • https: //assets. speareducation. com/userfiles/Imtiaz/cover. jpg • Kang, Sang-Hoon, and Moon-Key Kim. “Antibiotic sensitivity and resistance of bacteria from odontogenic maxillofacial abscesses. ” Journal of the Korean Association of Oral and Maxillofacial Surgeons vol. 45, 6 (2019): 324 -331. doi: 10. 5125/jkaoms. 2019. 45. 6. 324
- Slides: 13