The Respiratory System Presented by Martin Ponciano LVN

The Respiratory System Presented by: Martin Ponciano, LVN, DSD, MS Based on Memmler’s The Human Body in Health and Disease, 11 th Edition

Phases of Respiration Process of obtaining oxygen from environment and delivering it to cells • Pulmonary ventilation • External exchange of gases • Internal exchange of gases
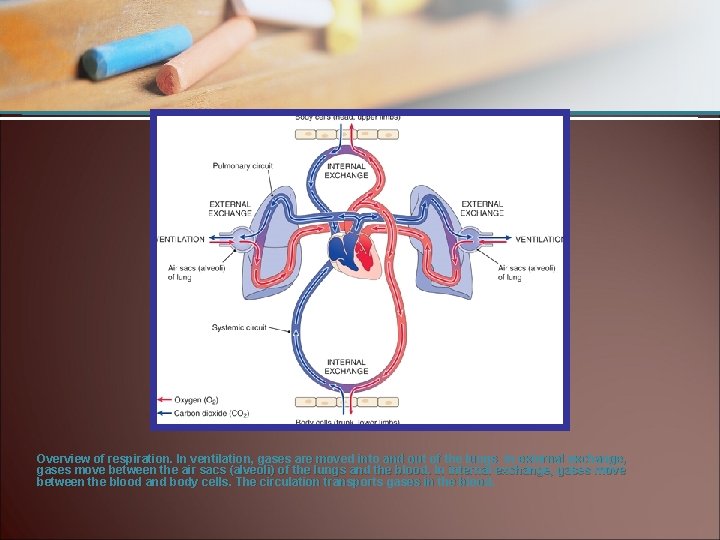
Overview of respiration. In ventilation, gases are moved into and out of the lungs. In external exchange, gases move between the air sacs (alveoli) of the lungs and the blood. In internal exchange, gases move between the blood and body cells. The circulation transports gases in the blood.

Checkpoint 18 -1: What are three phases of respiration?

The Respiratory System Conducts air into lungs • Nasal cavities • Pharynx • Larynx • Trachea (windpipe)
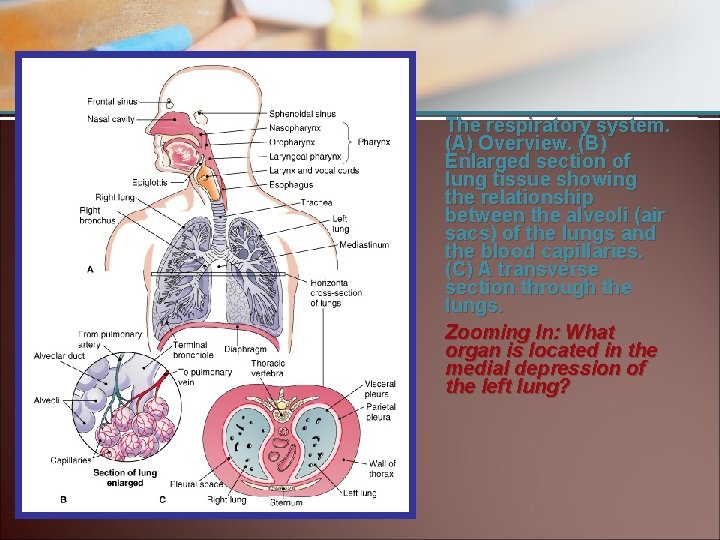
The respiratory system. (A) Overview. (B) Enlarged section of lung tissue showing the relationship between the alveoli (air sacs) of the lungs and the blood capillaries. (C) A transverse section through the lungs. Zooming In: What organ is located in the medial depression of the left lung?

Question: True or False? : The two gases involved in the external exchange of gases that takes place in the respiratory system are CO 2 and O 2.

Answer: True: The two gases involved in the external exchange of gases that takes place in the respiratory system are CO 2 and O 2.

The Nasal Cavities • Nostrils (nares) • Nasal cavities – Mucous membrane • Filters foreign bodies • Warms air • Moistens air – Conchae • Nasal septum • Sinuses
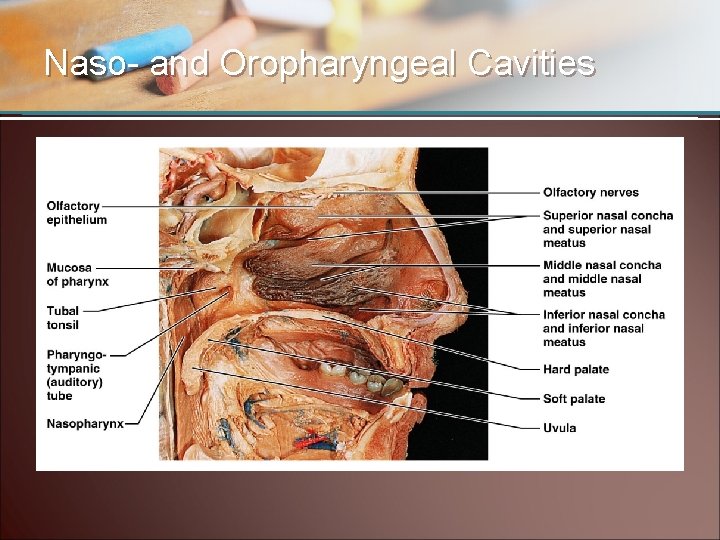
Naso- and Oropharyngeal Cavities

Checkpoint 18 -2: What happens to air as it passes over the nasal mucosa?

The Pharynx Throat (pharynx) carries air to respiratory tract and food to digestive system • Nasopharynx – Superior portion • Oropharynx – Middle portion • Laryngeal pharynx – Inferior portion

The Larynx (voice box) is located between the pharynx and trachea • Cartilage framework – Thyroid cartilage (Adam’s apple) • Vocal folds (vocal cords) – Used for speech • Glottis • Epiglottis
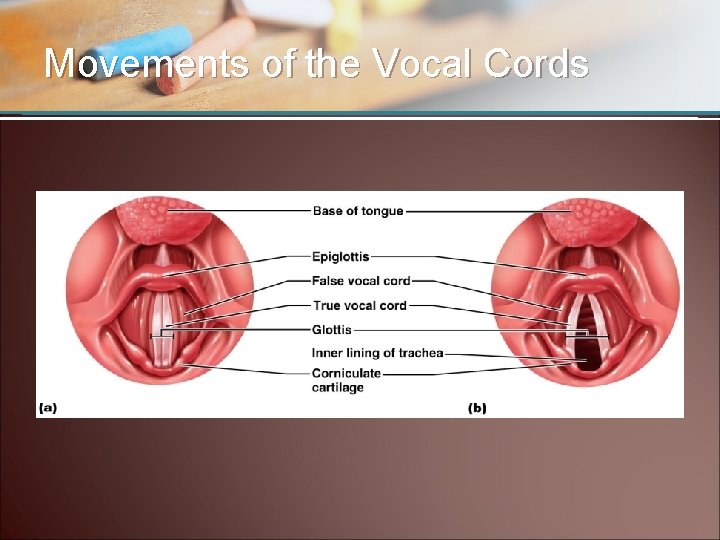
Movements of the Vocal Cords

The Trachea (wind pipe) conducts air between larynx and lungs • Framework of separate cartilages • Horseshoe shaped • Open at back for expansion during swallowing

Checkpoint 18 -3: What are the scientific names for the throat, voice box, and windpipe? Checkpoint 18 -4: What are three regions of the pharynx?

The Bronchi • Trachea divides into two primary bronchi that enter the lungs • Hilum • Epithelial tissue lining – Pseudostratified – Cilia
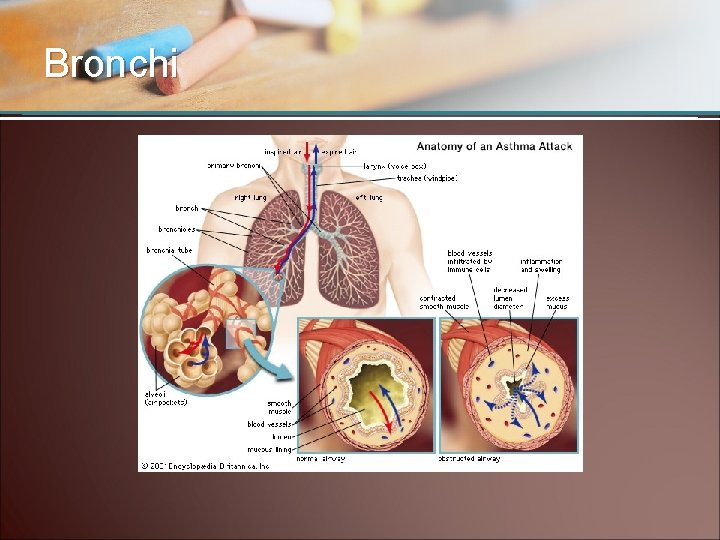
Bronchi

Checkpoint 18 -5: The cells that line the respiratory passageways help to keep impurities out of the lungs. What feature of these cells enables them to filter impurities and move fluids?

Question: The air-conducting passageways of the respiratory tract are lined with what type of tissue? a. stratified squamous epithelial b. pseudostratified epithelial c. squamous epithelial

Answer: b. pseudostratified epithelial

The Lungs • • • Mediastinum Lobes – Bronchial tree – Bronchioles Alveoli Diaphragm Pleura – Parietal pleura – Visceral pleura – Pleural space

Checkpoint 18 -6: In what structures does gas exchange occur in the lung? Checkpoint 18 -7: What is the name of the membrane that encloses the lung?

The Process of Respiration • Ventilation of lungs • Exchange of gases • Transport of gases in blood

Pulmonary Ventilation • Inhalation (inspiration) is active phase • Compliance • Exhalation (expiration) is passive phase • Lung capacity
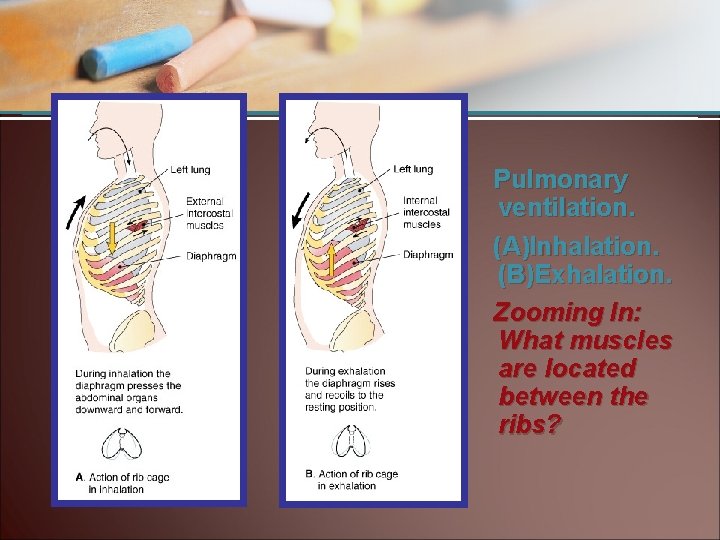
Pulmonary ventilation. (A)Inhalation. (B)Exhalation. Zooming In: What muscles are located between the ribs?
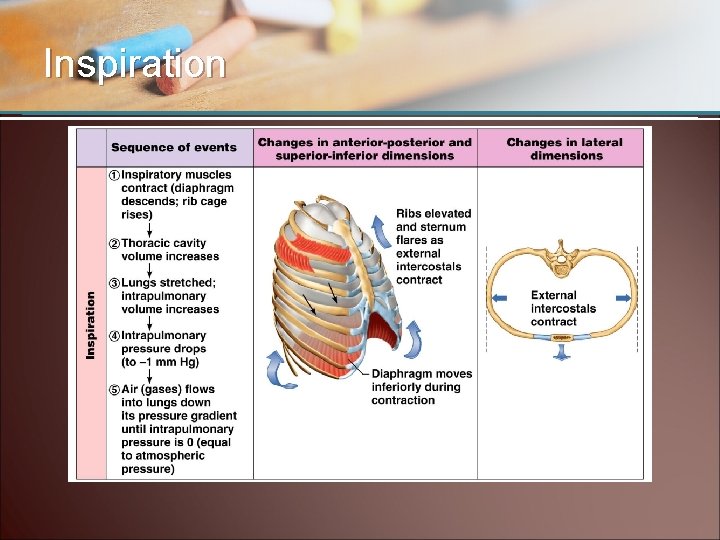
Inspiration
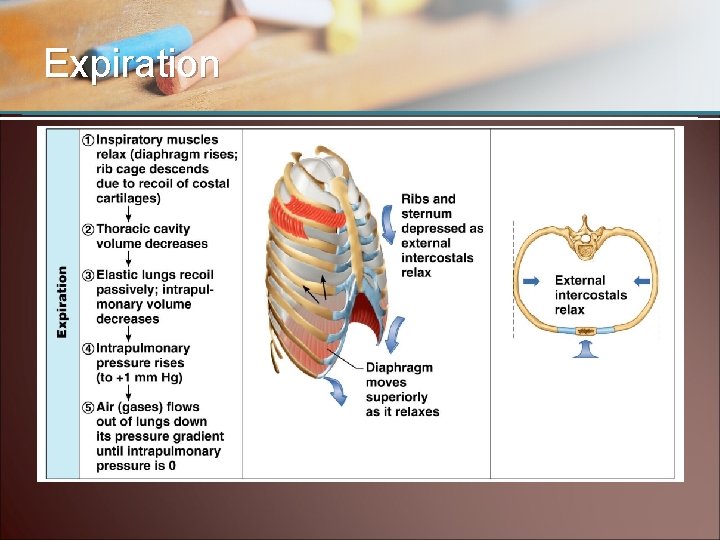
Expiration

Checkpoint 18 -8: What are the two phases of breathing? Which is active and which is passive?

Gas Exchange • Diffusion is movement of molecules from higher to lower concentration • External exchange – Gases move between alveoli and capillary blood • Internal exchange – Gases move between blood and tissues
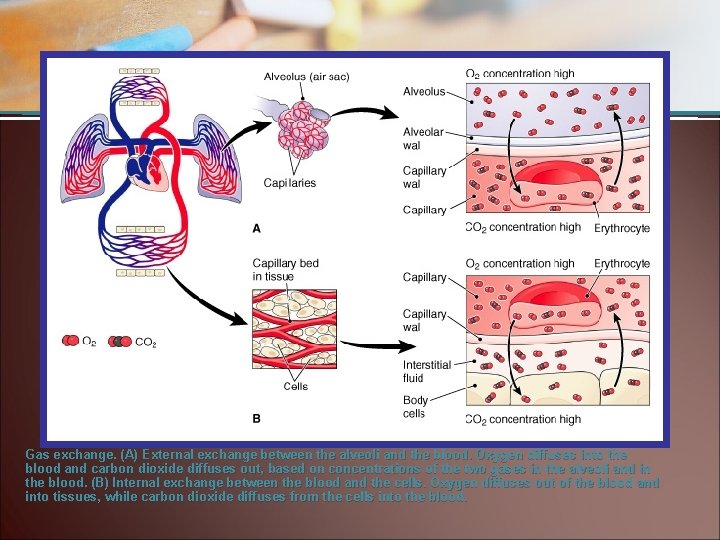
Gas exchange. (A) External exchange between the alveoli and the blood. Oxygen diffuses into the blood and carbon dioxide diffuses out, based on concentrations of the two gases in the alveoli and in the blood. (B) Internal exchange between the blood and the cells. Oxygen diffuses out of the blood and into tissues, while carbon dioxide diffuses from the cells into the blood.

Checkpoint 18 -9: Gases move between the alveoli and the blood by the process of diffusion. What is the definition of diffusion?

Transport of Oxygen • Most oxygen in capillary blood binds to hemoglobin • Oxygen must separate from hemoglobin to enter cells

Checkpoint 18 -10: What substance in red blood cells carries almost all of the oxygen in the blood?

Transport of Carbon Dioxide • 10% is dissolved in plasma and fluid in red blood cells • 15% is combined with protein of hemoglobin and plasma proteins • 75% dissolves in blood fluids and is converted to bicarbonate ion – First combines with water to form carbonic acid – Carbonic acid ionizes (separates) into hydrogen and bicarbonate ions – Carbonic anhydrase enzyme speeds conversion – Buffers blood to keep p. H steady

Checkpoint 18 -11: What is the main form in which carbon dioxide is carried in the blood?

Question: In what structure of the respiratory system does most gas exchange take place? a. bronchioles b. pleurae c. alveoli

Answer: c. alveoli

Regulation of Respiration Fundamental respiratory pattern • Controlled by central nervous system centers – Partly in medulla (main control center), partly in pons (modifies patterns set in the medulla) • Modified by receptors detecting changes in blood chemistry

Nervous Control • Control center is located in medulla and pons of brain stem • Motor nerve fibers extend into spinal cord • Fibers extend through phrenic nerve to diaphragm
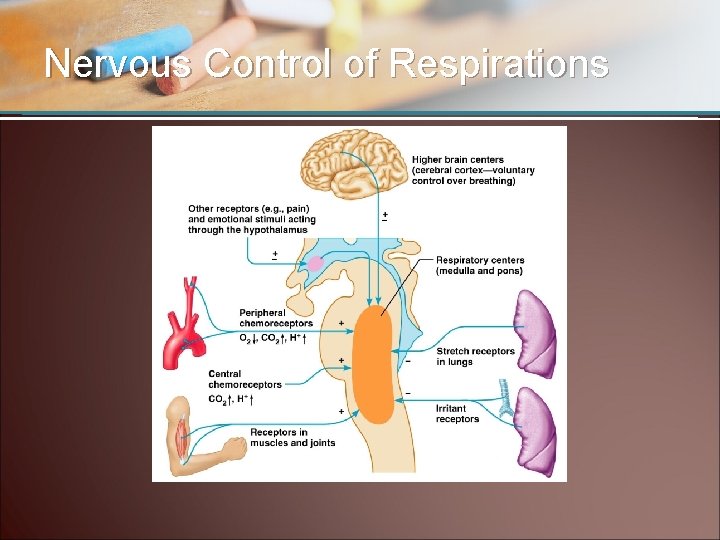
Nervous Control of Respirations

Checkpoint 18 -12: What part of the brain stem sets the basic pattern of respiration? Checkpoint 18 -13: What is the name of the motor nerve that controls the diaphragm?

Chemical Control • Central chemoreceptors – Located near medullary respiratory center – Respond to raised CO 2 level (hypercapnia) • Peripheral chemoreceptors – Located in neck and aortic arch – Respond to oxygen level considerably below normal

Checkpoint 18 -14: What gas is the main chemical controller of respiration?
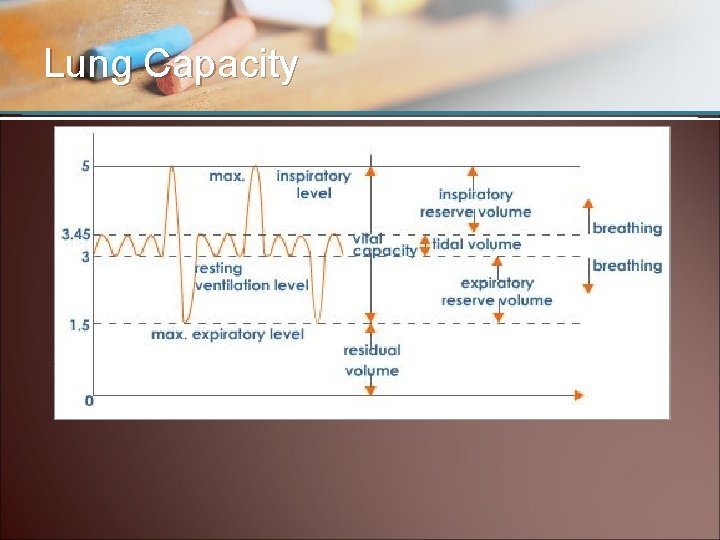
Lung Capacity

Abnormal Ventilation • Hyperventilation – High oxygen level and low CO 2 level (hypocapnia) – Increases blood p. H • Hypoventilation – Insufficient air in alveoli – Decreases blood p. H

Breathing Patterns • Measured in breaths per minute • Adults: 12 to 20 • Children: 20 to 40 • Infants: more than 40

• • Some Terms for Altered Breathing Hyperpnea Hypopnea Tachypnea Apnea Dyspnea Orthopnea Kussmaul respiration Cheyne-Stokes respiration

Breathing Patterns (cont. ) • • Eupnea: normal breathing Hyperpnea: deeper, more rapid breathing Hypopnea: slow, more shallow breathing Tachypnea: abnormally rapid rate of breathing – > 20 breaths per minute • Bradypnea: abnormally slow rate of breathing – <10 breaths per minute Dyspnea ◦ ◦ ◦ Aka SOB (shortness of breath) Difficult or labored breathing Usually one of the first symptoms of heart failure Apnea: spontaneous absence of respiration ◦ Sleep apnea syndromes Group of disorders Potentially fatal Breathing repeatedly stops during sleep Long enough to decrease significant amount of oxygen in blood Snoring may be a symptom

Breathing Patterns (cont. ) • Orthopnea: dyspnea that is relieved by sitting upright • Kussmaul respiration – deep, rapid respiration characteristic of acidosis • Cheyne-Stokes respiration – Pattern of alternating periods of hypopnea or apnea, followed by hyperpnea – Frequently seen in those who are dying

Question: What is the medical term for temporary cessation of breathing? a. dyspnea b. apnea c. hypopnea

Answer: b. apnea

Results of Inadequate Breathing: Lack of Oxygen Asphyxia ◦ ◦ Body cannot get need air to function Life-threatening Quick ↓ in O 2 levels ↑ in CO 2 levels Asphyxiation ◦ Aka suffocation ◦ Interruption of normal breathing resulting in asphyxia ◦ Can be caused by obstruction, drowning, smothering, choking, or inhaling gases (CO) instead of air

COPD Chronic obstructive pulmonary disease (COPD) ◦ Partial obstruction due to damage to bronchi ◦ Related to several lung disorders Ex. Chronic bronchitis & emphysema Respiratory function is impaired ◦ Reduce exchange of oxygen & carbon dioxide ◦ Traps air which may lead to over inflation of parts of lungs Patients have a history of: ◦ Smoking ◦ Dyspnea, where labored breathing occurs and gets progressively worse ◦ Coughing and frequent pulmonary infections COPD victims develop respiratory failure accompanied by hypoxemia, carbon dioxide retention, and respiratory acidosis

Disorders • Infection of the Respiratory System • Allergies • Environmental factors • Lung cancer

Disorders of the Nasal Cavities and Related Structures • Paranasal sinuses – Sinusitis – Polyps • Nasal septum – Deviated septum • Mucous membranes – Epistaxis

• Upper respiratory infection (URI) Infection • Common cold (acute coryza) • • • Respiratory syncytial virus (RSV) Croup Influenza Pneumonia – Bronchopneumonia – Lobar pneumonia – Pneumocystis pneumonia (PCP) Tuberculosis

Hay Fever and Asthma Hypersensitivity to allergens • Watery discharge from eyes and nose • Seasonal or chronic • Inflammation of airway tissues • Spasm in bronchial tubes

Chronic Obstructive Pulmonary Also called (COPD) chronic obstructive lung disease Disease • • • (COLD) Includes both chronic bronchitis and emphysema Normal air flow obstructed Reduced exchange of oxygen and carbon dioxide Air trapping and overinflation of lungs Dyspnea

Sudden Death Syndrome (SIDS) Also called. Infant crib death • Unexplained death • Seemingly healthy infant • Under 1 year old • Usually occurs in sleep

Checkpoint 18 -15: What does COPD mean and what two diseases are commonly involved in COPD?

Respiratory Syndrome Covers a range. Distress of inflammatory disorders(RDS) • Acute respiratory distress syndrome (ARDS) or shock lung – Usually appears in adults • Respiratory distress syndrome of the newborn – Formerly called hyaline membrane disease – Appears in premature newborns

Cancer • Lung cancer – Most common cause of cancer-related deaths – Most important cause is cigarette smoking • Cancer of larynx – Linked to cigarette smoking and alcohol consumption – High cure rate

Disorders Involving the Pleura • Pleurisy – Inflammation of pleura • Pneumothorax – Air in pleural space • Hemothorax – Blood in pleural space

Age andlose theelasticity, Respiratory Tract • Tissues become more rigid • Decreased compliance, lung capacity • Increased susceptibility to infection • Increased incidence of emphysema • Reduced capacity for exercise

Special Equipment for Respiratory Treatment • Bronchoscope • Oxygen therapy • Suction apparatus • Tracheostomy tube • Artificial respiration apparatuses

Question: What is the medical term for an accumulation of air in the pleural space? a. pneumothorax b. pleurisy c. atelectasis

Answer: a. pneumothorax

End of Presentation
- Slides: 70