The Respiratory System Paediatrics OSCE Revision Elizabeth Evans

The Respiratory System Paediatrics OSCE Revision Elizabeth Evans

Plan ¡What could come up in the OSCE ¡Respiratory examination ¡Respiratory conditions

Key Points ¡Likely to be one examination from: CV/Resp/GI ¡May have a station with images or recordings ¡May have a history ¡Mostly normal children ¡Know a little about everything: Vivas are v. short ¡Easiest way to get marks: Be nice to the child!

What could come up? Most respiratory disease in children presents acutely, thus unlikely to appear in the OSCE: History: -Normal -Asthma -CF -Hyperexpanded chest from asthma -Infection

Respiratory Examination ¡Inspection- increased work of breathing ¡Hands- cyanosis, clubbing (CF or CHD) ¡RR and HR – remember changes with age ¡Face- central cyanosis ¡Avoid trachea in children – indicate to examiner ¡Chest shape ¡Palpation- apex beat and chest expansion ¡Percussion- do not go straight for this on the chest! ¡Auscultate

Dyspnoea in a child ¡Nasal flaring ¡Subcostal and intercostal recession ¡Expiratory grunting ¡Difficulty feeding ¡Added sounds eg expiratory wheeze

CONDITIONS
Respiratory infections ¡URTI: common cold ¡LRTI: pneumonia sore throat bronchiolitis otitis media whooping cough croup diptheria acute epiglottitis

Croup ¡ Viral laryngotracheobronchitis (parainfluenza virus) ¡ 6 months – 6 years (peak in 2 nd year) ¡ URTI symptoms (coryza/fever) for 2 days before onset of a characteristic barking cough and stridor (subglottic oedema) lasting around 3 days ¡ Most improve spontaneously within 24 h ¡ 1 in 10 require hospitalisation: under 12 months, severe illness or signs of respiratory failure ¡ Single dose of dexamethasone or nebulised budesonide is beneficial ¡ Nebulised adrenaline provides transient improvement (reduces oedema) and is used in more severe cases to enable time for transfer to ITU

Acute epiglottitis ¡ Life-threatening emergency ¡ Haemophilus influenza type B (Hib immunisation has caused reduction) ¡ 1 - 6 years ¡ Rapid onset, intensely painful throat, febrile child, unable to swallow and reluctant to speak. Sat upright with open mouth drooling saliva. ¡ Resus room, call ENT and anaesthetist ¡ Do not examine throat! ¡ Secure airway, then take bloods for culture and commence IV cefuroxime ¡ Rifampicin for household contacts
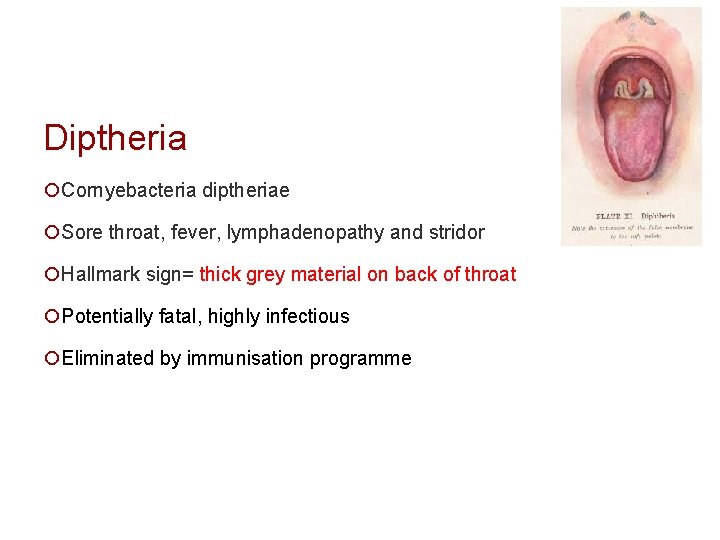
Diptheria ¡Cornyebacteria diptheriae ¡Sore throat, fever, lymphadenopathy and stridor ¡Hallmark sign= thick grey material on back of throat ¡Potentially fatal, highly infectious ¡Eliminated by immunisation programme
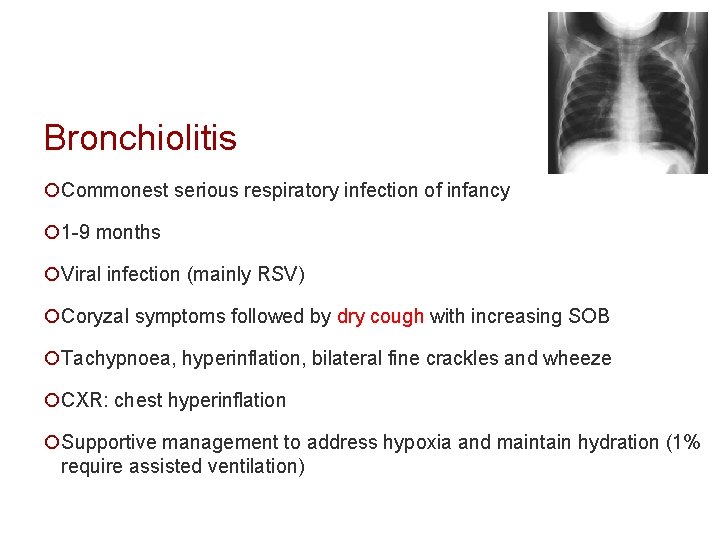
Bronchiolitis ¡Commonest serious respiratory infection of infancy ¡ 1 -9 months ¡Viral infection (mainly RSV) ¡Coryzal symptoms followed by dry cough with increasing SOB ¡Tachypnoea, hyperinflation, bilateral fine crackles and wheeze ¡CXR: chest hyperinflation ¡Supportive management to address hypoxia and maintain hydration (1% require assisted ventilation)

Whooping cough ¡Bordetella pertussis (highly contagious) ¡Spread by droplet infection ¡Characteristic inspiratory whoop (may be absent in infants) ¡During paroxysms of coughing the child may go blue and vomit ¡May persist for 3 months ¡Culture organism from nasal swab ¡Erythromycin reduces infectivity but does not shorten duration of symptoms

Asthma ¡Most common chronic respiratory disorder of childhood- 10% ¡Clinical diagnosis usually based on history and examination ¡If >5 able to demonstrate diurnal variation in PEFR ¡Wheeze= whistling noise made by the chest

¡History: ¡Examination Nocturnal cough Usually normal between attacks Intermittent symptoms In chronic severe asthma: Triggers -hyperexpansion Exercise tolerance Atopy FH of asthma Parental smoking -pectus carinatum -Harrison sulcus

Asthma Treatment ¡ Aim- asymptomatic with no exacerbations ¡ Educate child and parents on avoidance of triggers, importance of regular therapy and correct inhaler technique ¡ Stepwise approach: British Guidelines for Asthma Management: Step 1: Inhaled SABA Step 2: Low dose inhaled steroids (if requiring 3 xday SABA) Step 3: Add LABA or leukotriene antagonist Step 4: Increase inhaled steroid. Oral Theophylline. Leukotriene antagonist. Step 5: Alternate day oral steroids.
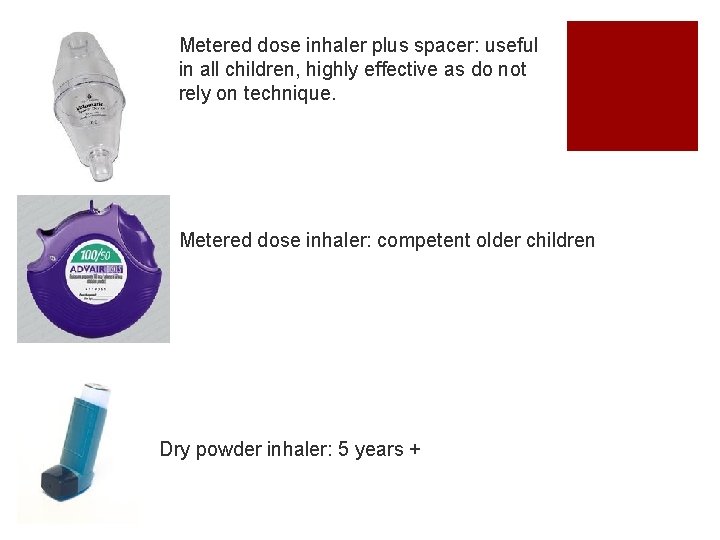
Metered dose inhaler plus spacer: useful in all children, highly effective as do not rely on technique. Metered dose inhaler: competent older children Dry powder inhaler: 5 years +

Cystic Fibrosis ¡ Autosomal recessive disease affecting 1 in 2500 ¡ Mutation in CFTR protein resulting in defective chloride channel, increased viscosity of secretions in respiratory tract and pancreas ¡ Consider in any child with recurrent chest infection or failure to thrive ¡ Repeated infections lead to bronchial wall damage and abscesses ¡ Deficiency of pancreatic enzymes results in malabsorption and steatorrhoea ¡ Diagnosis: screening performed as part of Guthrie test. Gold standard diagnostic test is the sweat test. Genetic testing also useful to confirm diagnosis.

CF Examination General: small for age, Creon supplements or insulin around bed Peripheral: finger clubbing Airway: nasal polyps, hyperinflated chest, crackles GI: scar from meconium ileus operation

CF Management ¡MDT approach ¡Respiratory: physio, aggressive treatment of lung infections ¡Nutritional: high calorie diet, vitamin ADEK, Creon (pancreatic enzyme supplements) ¡Severe lung disease may be considered for lung transplantation

Thank you
- Slides: 21