THE RESPIRATORY SYSTEM OXYGENATION Lisa B Flatt RN
THE RESPIRATORY SYSTEM & OXYGENATION Lisa B. Flatt, RN, MSN, CHPN

Anatomy & Physiology Nose Pharynx Larynx Tracheobronchial Tree Right & Left Bronchus Bronchioles Alveoli Lungs Cilia Diaphragm Pleural Cavity

Breathe Deeply……. . The pharynx is the passageway for _air_into the lungs and _food __into the __esophagus_. The left lung has __2___lobes. The right lung has __3____lobes. The smallest structure in the lungs is the _alveoli_. The _alveoli__is the gas-exchange unit. What warms air _cilia____ and in conjunction with mucus traps dust, allergens, particles…

The Alveoli What and how they do it…. . Are encased in parchment thin capillary filled sacks O 2 & CO 2 are exchanged by diffusion (movement of particles from area of higher to lower concentration) Out into the body…… O 2 combines with hemoglobin (goes to the tissue as oxyhemoglobin) CO 2 is exhaled after the venous system returns oxygen depleted blood to the lungs

The Need to Breathe The goal is to move air in and out of the lungs You need physics and gas pressures and must equalize the pressure inside and out Breathing is automatic Breathe in and diaphragm goes __down__ so the pressure inside your chest is __greater_than outside. Need for oxygen & to get rid of excess CO 2

What would cause an increased demand for oxygen? Name some disease states __stress, anxiety_____ ___anemia, lung diseases_____ Name some illnesses ____infection, sepsis_____ ____fever_____ What about others? Pg. 57 ___activity_____ ___age related, shape you’re in!_____

Lung function, capacity and elasticity are measured by: Tidal volume-amt. you breath in and breath out Vital capacity-maximum amt. of air you breath out after the maximum amt of air you breath in Total lung capacity-max amt of air in lungs after max inspiratory effort Residual volume-amt of air left in lungs after forced exhalation Expiratory reserve volume-amt of air forcefully exhaled after normal TV exhalation Inspiratory reserve volume-amt of air forcefully inhaled after your normal TV Pulmonary Function Test (PFT) – measures all of above, tells us about overall lung function and if they are congruent with functioning

Disease States Asthma Sudden Infant Death Syndrome Emphysema COPD Posture : kyphosis Cancer Bronchitis

Smoking…… What does it do to our bodies Cilia – decreased motility, get stuck to the sides Mucus – gross colors, sticky and thick, increased and cough it up Air exchange – poor, decreased, deprives the body

Fun facts…. Narcotics effect on breathing___suppress, no effect/increase in O 2 usage: Morphine, suppresses respiration, decreases the myocardial consumption of oxygen___ Lung cancer and predisposing occupations ___asbestosis, construction, radiation______ ___farmers, agriculture, chemical exposure______ ___coal mining, second hand smoke, smokers_____ Physical conditions that can affect oxygenation ___activity, breathing patterns______ ___body habitus, stress, illness______ ___age, pain, crying-depression/psychological state______

Respirations Normal rate adults: _12 -20 bpm___infants: _30 -60? ? ___ Rapid rate is called_tachypnea______ Reasons: __spesis, pain, fever, activity, metabolic acidosis_____________ Decreased rate is called___bradypnea_______ Reasons: __medication, brain injury, psychological state, metabolic states___ Excessive amount of air in lungs__hyperventilation___ Inadequate amount of air in lungs_hypoventilation___ Difficult or labored breathing__dyspnea____

Respirations cont’d Labored or difficult breathing __dyspnea_______ Must sit upright to breath___orthopnea_____ Apnea is _not breathing__________ Breathing pattern with periods of apnea lasting __10 -60 sec. is called___cheyne-stokes__ Gasping breathing associated with diabetes__kussmaul’s___
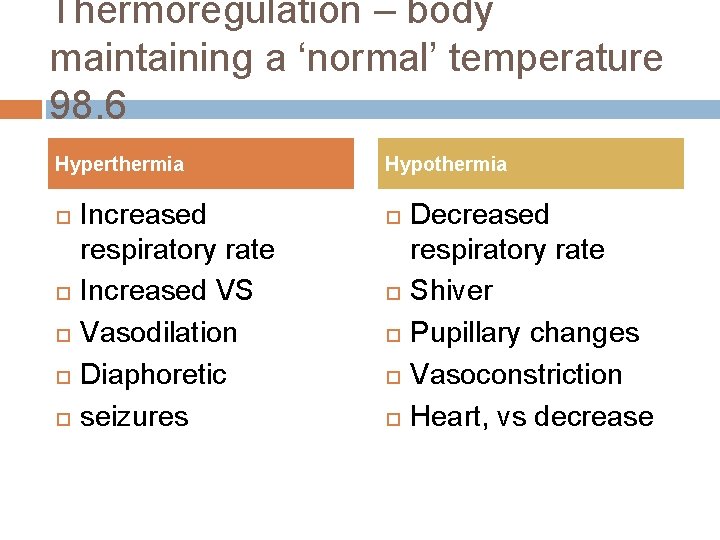
Thermoregulation – body maintaining a ‘normal’ temperature 98. 6 Hyperthermia Increased respiratory rate Increased VS Vasodilation Diaphoretic seizures Hypothermia Decreased respiratory rate Shiver Pupillary changes Vasoconstriction Heart, vs decrease
Hemoglobin Contains and carrier iron Low hgb treated with __iron____Side effects of Iron: constipation, dk stools, GI upset______ Hgb can be decreased from __CO poisoning, hemorrhage, GIB_____

How do the following affect breathing? Age – lung capacity decreases as you age Sex – men have increased lungs/bigger chests Cigar/cigarette smoking – decrease lung compliance, damage structures Cultural/spiritual or religious background – peace pipes, smoking, incense

More…… And More………. Activity – good, increases lung capacity and compliance Diet – healthy, iron Body weight - appropriate Height - OK Aerobic exercise – increase respiratory rate, air exchange and burning calories Stress – (like aerobic exercise!), bad stuff

…. . And More…… Environmental Factors - toxins Altitudes- higher thinner air, less O 2 Ventilation of space – air movement, clean Occupations – breathing in harmful substances Air temperature and humidity – hot and cold, painful, humid - stuffy Alternative and Holistic therapies – hypnosis, etc…

3 Areas of Altered Respiratory Function Movement of air in or out of the lungs (altered O 2 intake and supply) Diffusion of O 2 and CO 2 (between alveoli and pulmonary capillaries) Transport of O 2 and CO 2 (altered cellular demand for O 2)

Movement of air in or out of the lungs (altered O 2 intake and supply) Oxygen intake needs exceed what they can take in – blockage (nasal) Tumor, food, mucus, anything….

Diffusion of O 2 and CO 2 (between alveoli and pulmonary capillaries) Diffusion is movement of particles from an area of higher concentration to lower concentration Anemia, BMT failures, lung diseases

Transport of O 2 and CO 2 (altered cellular demand for O 2) More hgb=greater O 2 capacity Sepsis, fever, exercise

Oxygen Safety No smoking No flames No fires Tripping over stuff, like tubing and cannisters Humidifier with NS – keeps nasal mucosa moist

Oxygen delivery methods BVM – bag valve mask Ventilator – endotracheal tube Nasal cannula – 2 -6 L Face Mask – varying amounts of oxygen Nonrebreather mask – 100% - 2/3 on inspiration – completely collapses? = breath CO 2 Face tent – rarely used Transtracheal oxygen – O 2 via trach CPAP Bi. PAP

Oxygen saturation – amount/percent of O 2 in RBC – used by pulse ox Fi. O 2 – fracional concentration of oxygen

Blood Products Plasma – volume expander, clotting factors RBC – H/H and iron IVIG – intravenous immune globulins Platelets- clotting Cryoprecipitate – clotting factors / frozen product from plasma Albumin – promotes intravascular fluid absorption Prolastin – for alpha-one antitrypsin disease (enzyme deficiency)

S/S Transfusion Reaction Chills Fever Headache Backache Hematuria Clammy SOB

Others… Circulatory overload – vein distention, cough, crackles, tachycardia, HTN – go slow, titrate up and check VS!

Nursing Promotions Percussion Postural drainage Nasopharyngeal suctioning Incentive Spirometer Coughing and deep breathing Medications Pursed lip breathing – fish face Hydration Pulmonary toileting

Medications Bronchodilators Expectorants Antitussives Some cardiac drugs can be used to increase respiration and oxygens: NTG, calcium channel blockers, etc. . See page 71

Blood gases See handout I gave you!

Care Plan
- Slides: 31