The Referral Is the Key 18 weeks Referral












- Slides: 31

The Referral Is the Key 18 weeks Referral to Treatment standard Tracey Gillies National Clinical Lead for 18 weeks Service Redesign and Transformation Improvement and Support Team, SGHD

18 Weeks Referral to Treatment Time “ a whole journey waiting time target of 18 weeks from general practitioner referral to treatment …. by December 2011” Cabinet Secretary for Health and Wellbeing, Scottish Parliament – Official Report, 28 th June 2007. “… how should the new waiting time target be defined in order to maximise its potential for improving the quality of patient care? ” Better Health, Better Care, August 2007


Current view of many clinicians Speed of access Quality

Dimensions of Quality

What do patients want? How can we improve patients’ experience • Develop One Stop Clinics • Reduce sequential testing (where possible) • Develop robust pre-operative assessment processes • Develop strong discharge planning processes

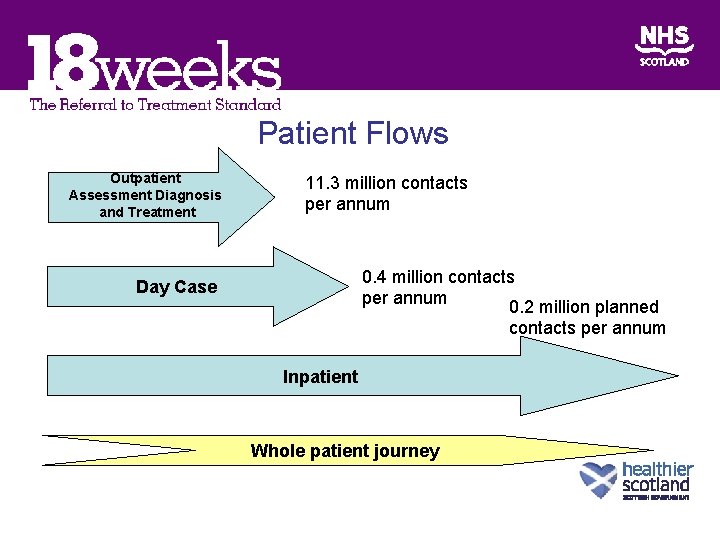
Patient Flows Outpatient Assessment Diagnosis and Treatment 11. 3 million contacts per annum 0. 4 million contacts per annum 0. 2 million planned Day Case contacts per annum Inpatient Whole patient journey

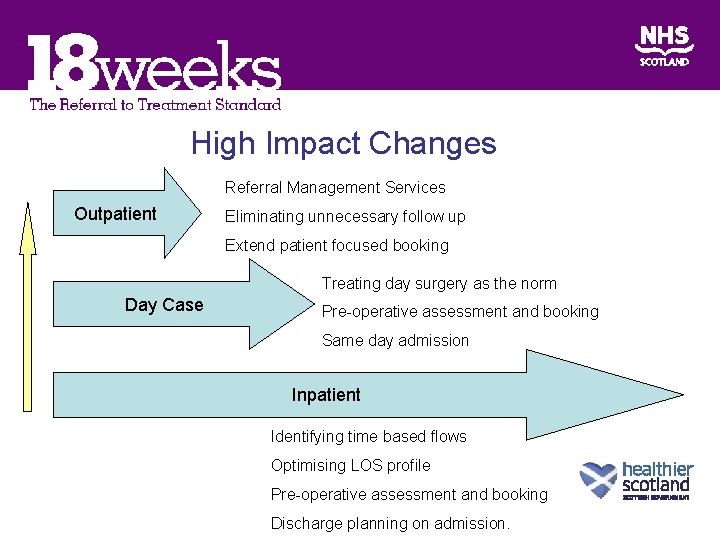
High Impact Changes Referral Management Services Outpatient Eliminating unnecessary follow up Extend patient focused booking Treating day surgery as the norm Day Case Pre-operative assessment and booking Same day admission Inpatient Identifying time based flows Optimising LOS profile Pre-operative assessment and booking Discharge planning on admission.

Patient Flows Outpatient Assessment Diagnosis and Treatment = Day Case In patient = 0. 4 million contacts per annum 0. 2 million planned contacts per annum 11. 3 million contacts per annum

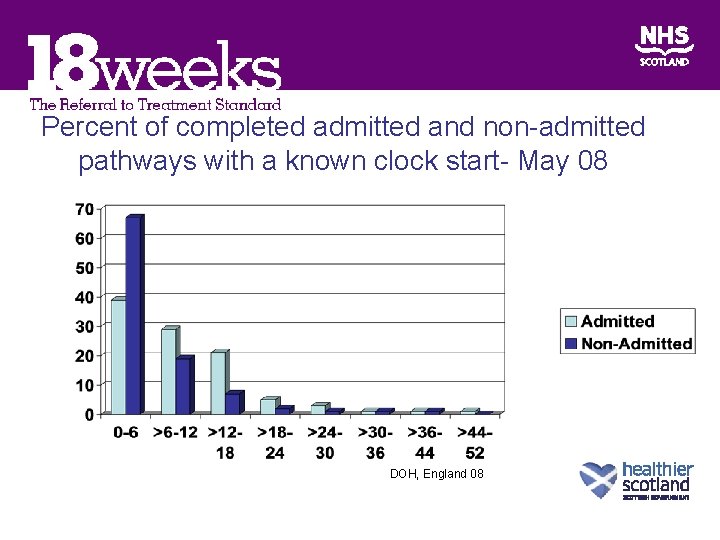
Percent of completed admitted and non-admitted pathways with a known clock start- May 08 DOH, England 08

Focus on 5 Simple Changes Patient Pathway Improve referral and diagnostic pathways Treat day surgery as the norm Actively manage admissions to hospital Actively manage discharge and length of stay Actively manage follow ups

Improve patient flow - develop and manage patient pathways Reduce variation develop protocoldriven care Utilise and Optimise Improve Understand develop the administrative materials manage demand skills of the processes management and capacity workforce (remove carve out, reduce the number of queues) Improve access, diagnostic and assessment process Actively manage admission to hospital Treat day surgery as the norm Actively manage discharge and length of stay Actively manage follow up

Building on previous experience and best practice

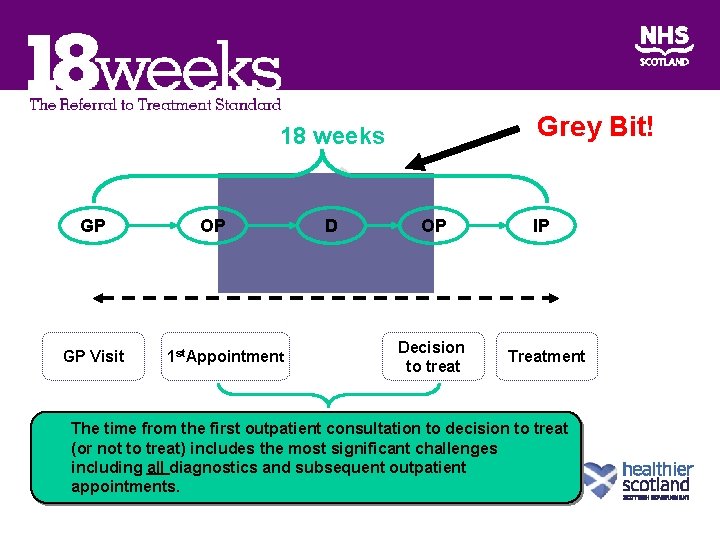
Grey Bit! 18 weeks GP GP Visit OP 1 st. Appointment D OP Decision to treat IP Treatment The time from the first outpatient consultation to decision to treat (or not to treat) includes the most significant challenges including all diagnostics and subsequent outpatient appointments.

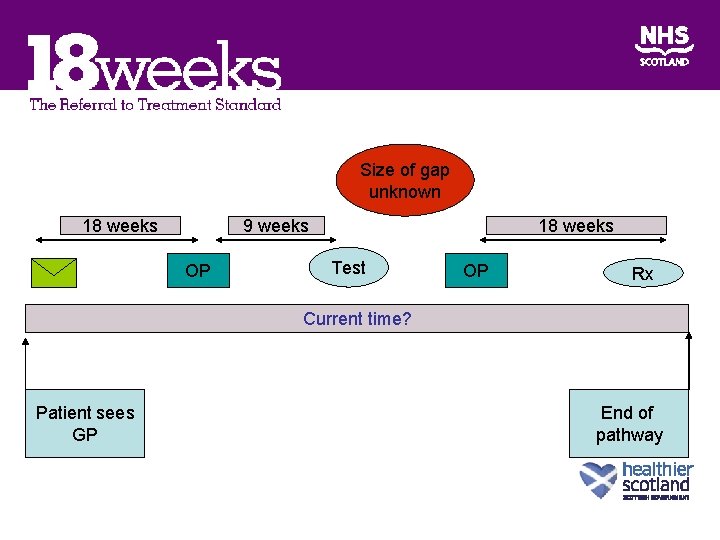
Size of gap unknown 18 weeks 9 weeks OP 18 weeks Test OP Rx Current time? Patient sees GP End of pathway


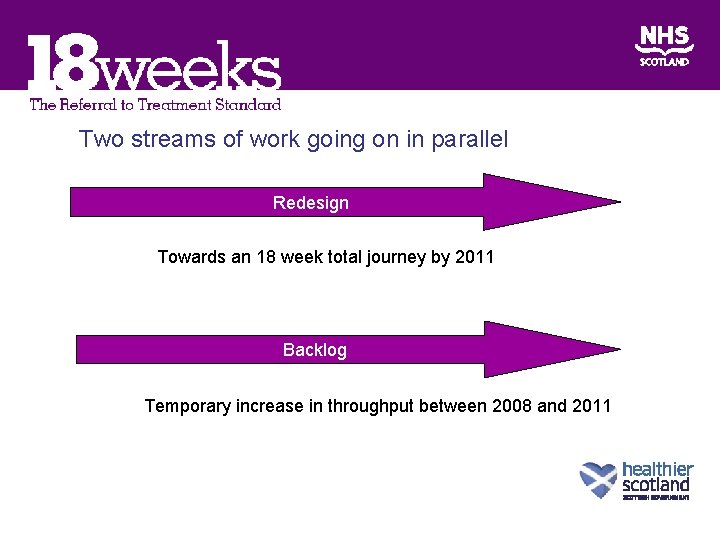
Two streams of work going on in parallel Redesign Towards an 18 week total journey by 2011 Backlog Temporary increase in throughput between 2008 and 2011

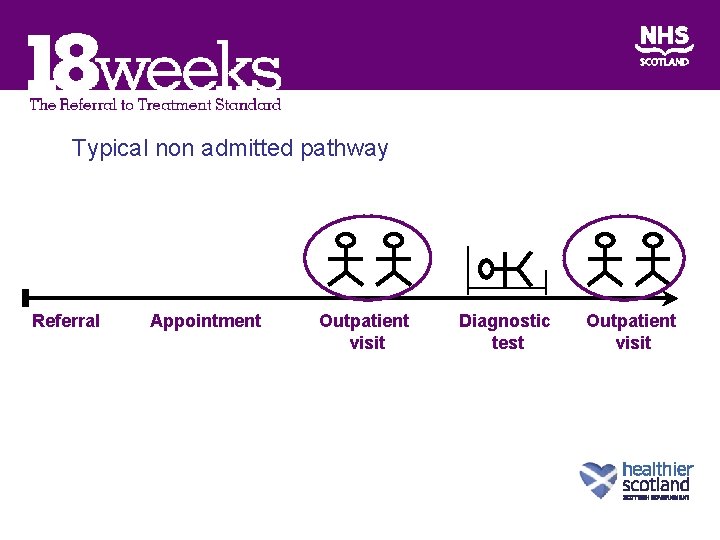
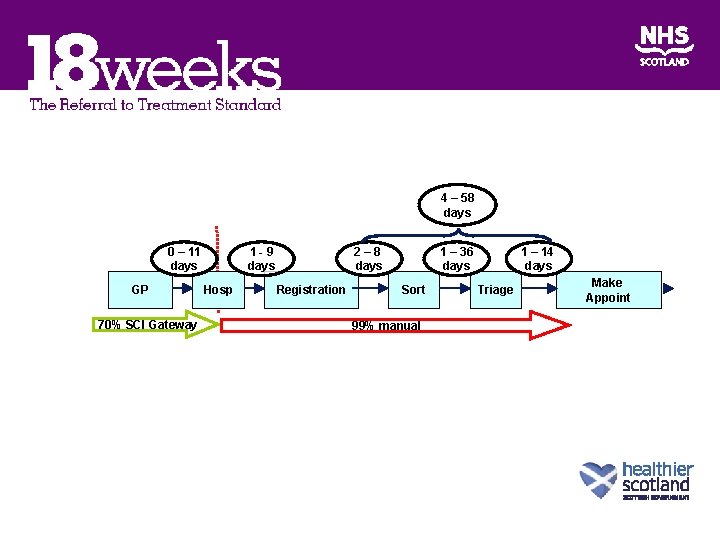
Typical non admitted pathway Referral Appointment Outpatient visit Diagnostic test Outpatient visit

4 – 58 days 0 – 11 days GP 70% SCI Gateway 1 -9 days Hosp 2– 8 days Registration 1 – 36 days Sort 99% manual 1 – 14 days Triage Make Appoint

What exactly do we mean by e triage? • Deal with referral electronically • Attribute clinical priority/destination/PFB queue • Make this information available to referrer Role of e triage in referral management • • Reduction in waste Right referral to right place/person Benefits for referrer- transparency of process Improve demand capacity work

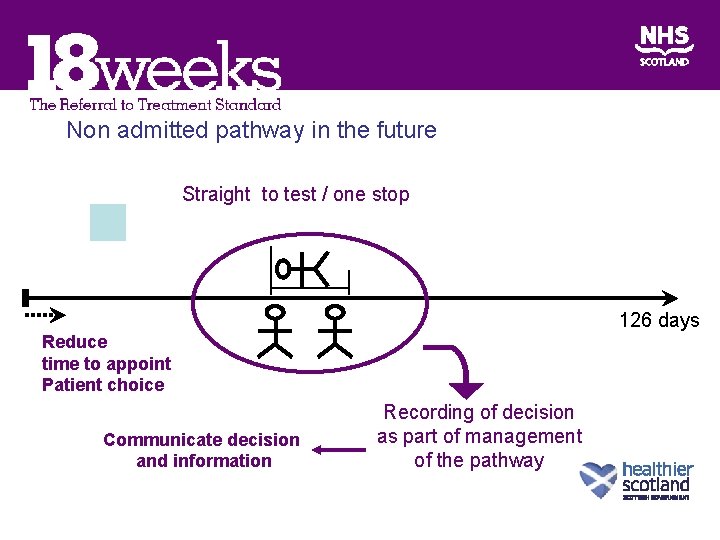
Non admitted pathway in the future Straight to test / one stop 126 days Reduce time to appoint Patient choice Communicate decision and information Recording of decision as part of management of the pathway

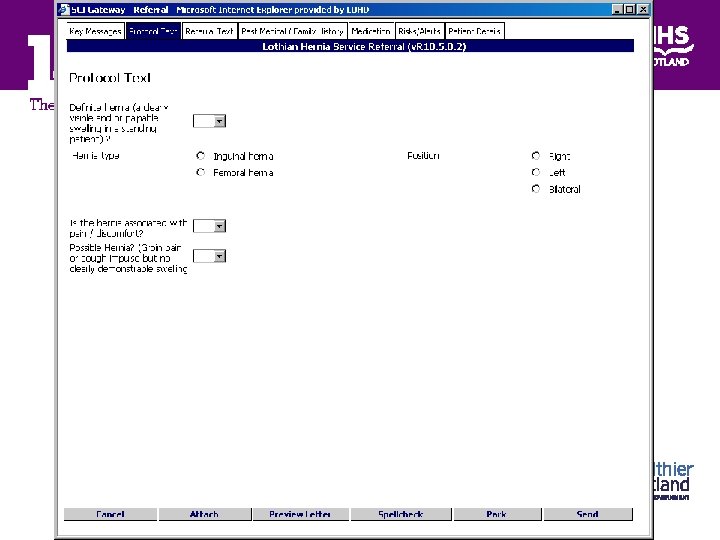
Is the purpose of the referral clear? Are there useful referral protocols in place? What information does the patient have or need? Is the timescale appropriate?


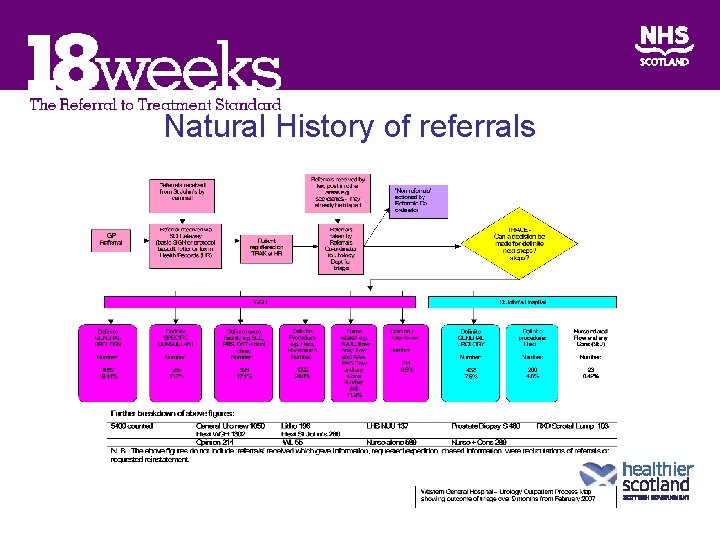
Natural History of referrals

Online Knowledge service • • Joint development between NES and 18 weeks Owned at board level Local pathways, linked to available evidence Patient area



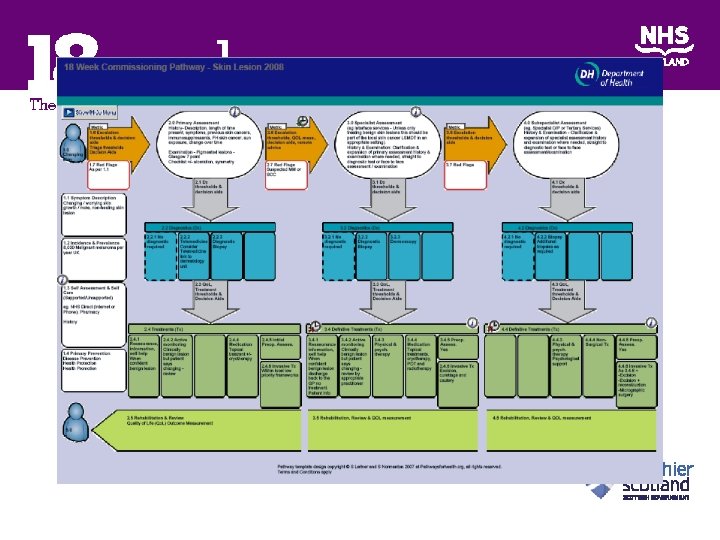
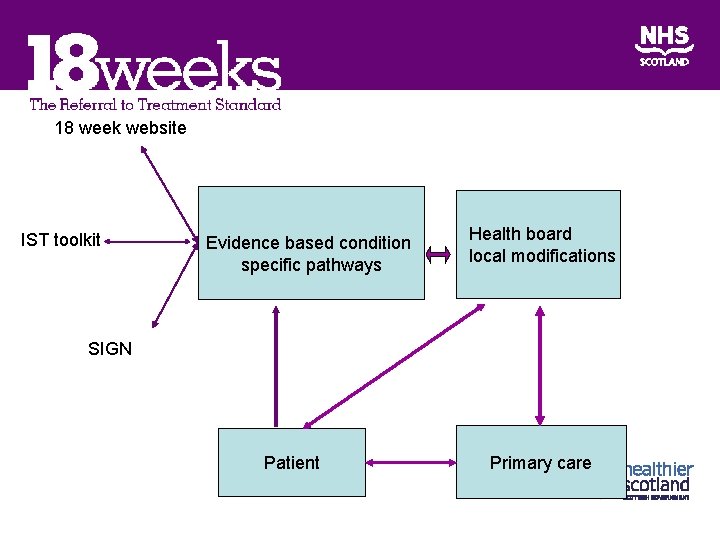
18 week website IST toolkit Evidence based condition specific pathways Health board local modifications SIGN Patient Primary care

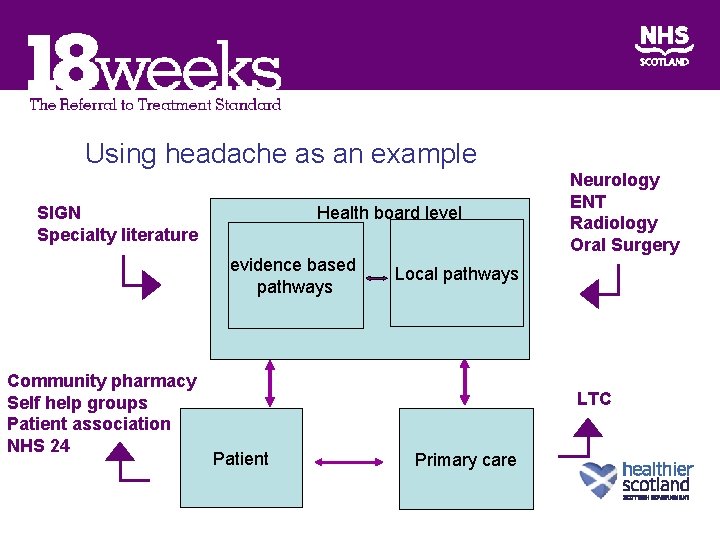
Using headache as an example SIGN Specialty literature Health board level evidence based pathways Community pharmacy Self help groups Patient association NHS 24 Neurology ENT Radiology Oral Surgery Local pathways LTC Patient Primary care

Advantages • Management of patient expectation • Pace of change between now and 2011 rapid and difficult to maintain communication • Dissemination of information • Up to each board to use as much as wished • Addresses in part the mutuality and shifting the balance of care agenda • Needs to be “living “ not once only
