The Problem of Pain Approach to Abdominal Pain

The Problem of Pain Approach to Abdominal Pain Jason Phillips, MD

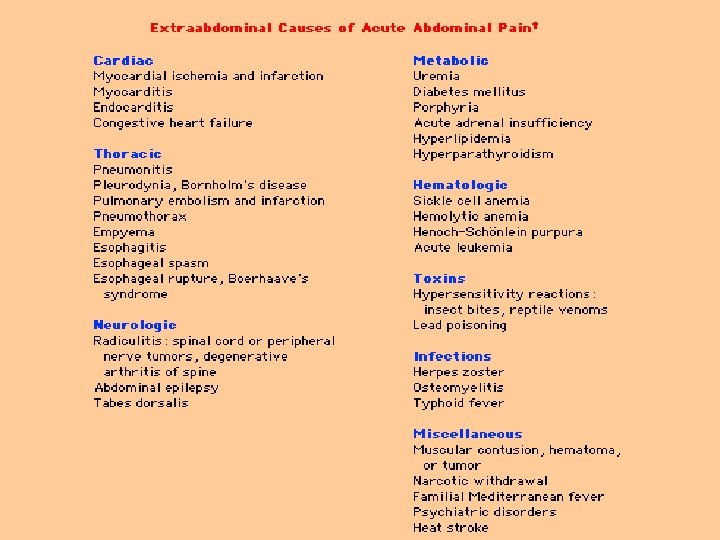

ER approach to abdominal pain Chief complaint: abd pain o Labs: CBC, chem, LFTs, lipase o CT abdomen o History o Possible PE

How do you approach a workup for abdominal pain What are the most likely possibilities? How do you organize your thoughts?

The Problem of Pain o Neurologic basis of pain n n Why is it difficult to localize? Why does the intensity of the pain vary? o General overview of approaching a patient with abdominal pain o Pain syndromes

Neurologic basis of abdominal pain o Pain receptors respond to n n Mechanical stimuli Chemical stimuli o Nociception mechanical receptors are located on serosa, within the mesentery, in the GI tract wall in the n n myenteric plexus (Auerbach plexus) submucosal plexus (Meissner plexus)

Neurologic basis of abdominal pain o Mucosal receptors respond to chemical stimuli o Substance P, serotonin, histamine, and prostaglandins o Chemical stimuli are released in response to inflammation or ischemia

Two basic problems with abdominal pain o Localization of visceral pain o Intensity of pain response

Localization of visceral pain o Visceral pain localizes to midline n n n Bilateral, symmetric innervation Afferent fibers celiac, superior mesenteric, or inferior mesenteric ganglion Localizes: epigastrium, periumbilical, and lower abdomen
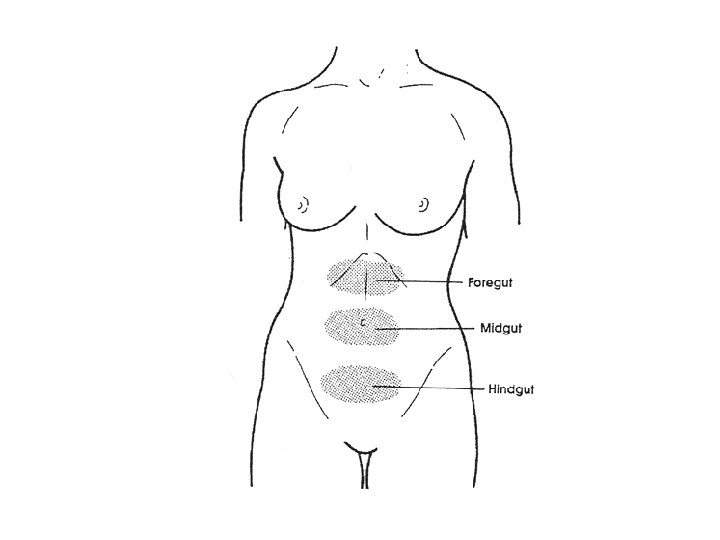

Localization of visceral pain o Exceptions to the bilateral rule o Gallbladder o Ascending and descending colon o Although bilaterally innervated, they have predominant ipsilateral innervation

Localization of visceral pain o Referred pain n Somatic fiber “cross-talk” Activate same spinothalamic pathways referred pain as the cutaneous dermatome sharing the same spinal cord level (Gallbladder – scapula) Results in aching pain with skin hyperalgesia and rigidity
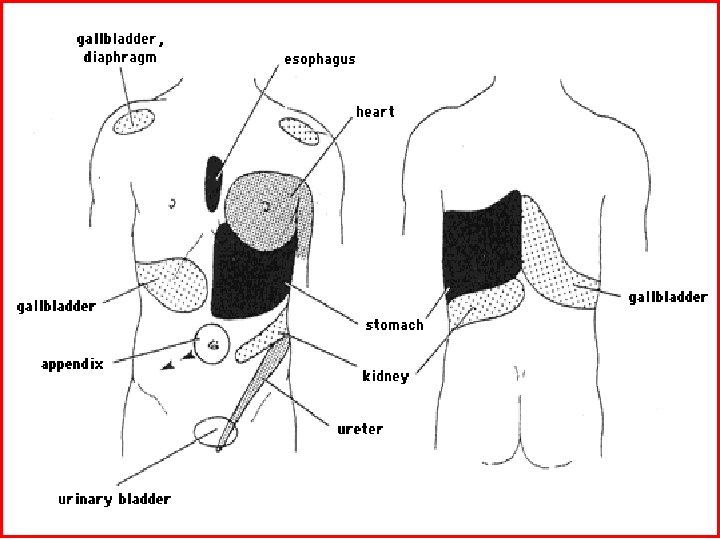

Intensity of pain response o Threshold for perceiving pain from visceral stimuli has marked individual variability o Balloon distension experiment in IBS

History o MOST IMPORTANT CLUE to the source of abdominal pain o Type of pain n Visceral = dull, aching, poorly localized Parietal = sharp, well localized Referred pain

History o General location n Generalized, RUQ, epigastric, LUQ, periumbilical, RLQ, LLQ, and ‘migratory’ n General region localizes organs/structures to include in the DDX n Radiation of pain (e. g. , acute pancreatitis)

History o Onset of pain n n Most gradual, steady crescendo (e. g. , cholecystitis) Abrupt, “ 10/10” – suggestive of perforation o Quality of pain n Colicky (comes and goes) – e. g. , gastroenteritis Steady – (e. g. , acute pancreatitis; biliary colic is a misnomer) Burning

History o Severity of pain n n Generally corresponds to severity of illness However, marked patient variability (“ 12/10 pain” is often functional or has functional overlay) o Aggravating or Relieving factors n n Eating (mesenteric ischemia vs PUD) Position changes (acute pancreatitis, peritonitis)

History o Associated symptoms n n n Nausea/vomiting Weight loss Changes in bowel habits

Physical exam: Acute abdomen or not? o General appearance and Vital signs o Abdominal exam n Auscultation p Bowel sounds present? p High pitched sounds of obstruction p Stethoscope palpation n Percussion p Tympany = distended bowel p Most humane test for rebound tenderness

Physical exam: Acute abdomen or not? o Palpation: n n n Acute abdomen or not? Peritoneal signs Rebound tenderness Mass? Hernia o Abdominal wall maneuvers n n Leg lift maneuvers (Carnett’s sign) Abdominal crunch

Further evaluation o Directed at pain syndromes o Labs o Imaging

Is the pain functional or not?

Functional abdominal pain o Can be difficult to distinguish from organic pain o Can only be labeled as functional when organic causes are excluded o Can superimpose on organic pain o Should not cause n Weight loss, Anemia, GI bleeding, Fever, Night sweats

Is it functional or not? o Clues that are suggestive of functional n Atypical history p RUQ that lasts 20 sec is not biliary colic p Dyspesia that worsens with a PPI n Overly dramatic descriptions of pain p “It feels like a knife stabbing me over and then something is pushing inside out” n Hyperbolic intensity p “ 11/10 exam epigastric pain” with a benign abd

Is it functional or not? o Clues that are suggestive of functional n Absence of nocturnal symptoms n Exacerbated by stress n Distractible exam n “Gut feeling”

Pain syndromes

Irritable Bowel Syndrome o Prevalence: 10 -15% of overall population o Only ~15% of patients seek medical care o 25 -50% of gastroenterology visits o Annual healthcare cost: $1. 7 billion

Irritable Bowel Syndrome ROME criteria: o 12 weeks or more of abdominal pain/discomfort in the last 12 months (does not have to be consecutive) o Two or more features: 1. 2. 3. Relieved with defecation Change in frequency of stool Change in appearance of stool

Irritable Bowel Syndrome 3 types of IBS patients o Constipation-predominant o Diarrhea-predominant o Alternating

Irritable Bowel Syndrome What is the normal range for frequency of bowel movements? Rule of 3 s: - Normal = Anywhere from 3 x per week to up to 3 x per day

Irritable Bowel Syndrome Pathophysiology Alterations in motility Visceral hyperalgesia Postinfectious IBS – lymphocytic infiltration of myenteric plexus?

Irritable Bowel Syndrome How do you prove its only IBS? Rome criteria positive for IBS o No alarm features and mild symptoms, reassurance and treatment of symptoms o Alarm features or severe symptoms, consider referral to GI

Upper abdominal pain o Biliary disease o Dyspepsia o Pancreatitis o Gastroparesis o Other

Upper abdominal pain: Biliary disease 1. 2. 3. n n n Most common location – epigastric NOT RUQ Steady onset; last hours (not minutes or seconds) Can radiate to right scapula Biliary colic Cholecystitis Acute cholangitis
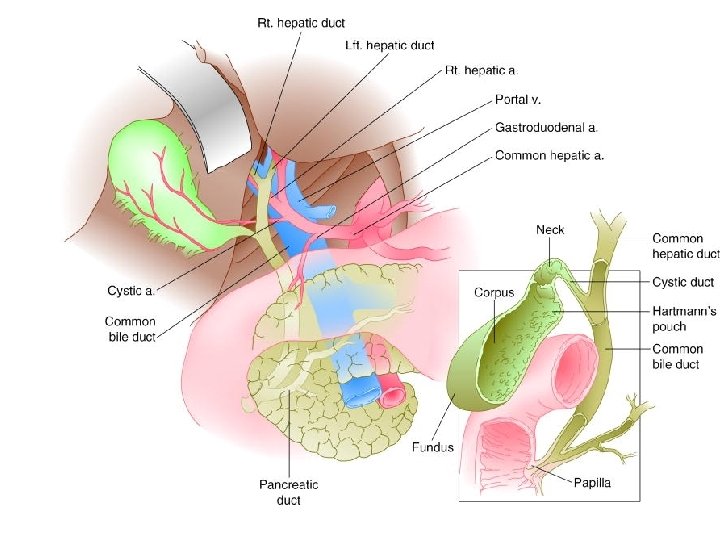
Upper abdominal pain: Biliary disease o Workup: n Labs: When are liver tests abnormal? Imaging: What is the most sensitive imaging study for biliary tract disease? n What are its limitations? n

Upper abdominal pain: Biliary disease o Labs: LFTs increase with choledocholithiasis (first transaminases, then AP/T Bili) o Ultrasound: Sensitivity Specificity n Cholecystitis 88% 89% p HIDA 97% 90% n Gallstones 84% 99% n Biliary dilation 55 -91% n Choledocholithiasis 50 vs 75% (nondilated vs dilated CBD)

Upper abdominal pain: Dyspepsia o Dyspepsia = “persistent or recurrent abdominal pain or discomfort in the upper abdomen. ” o Vague diagnosis that includes a long DDX


Upper abdominal pain: Dyspepsia o 80 -100% of ‘dyspepsia’ is a acid-related phenomenon or functional o Usually an outpatient problem o Peptic ulcer pain = epigastric, burning or hunger-like, worse between meals, relieved with food, nocturnal pain, associated nausea
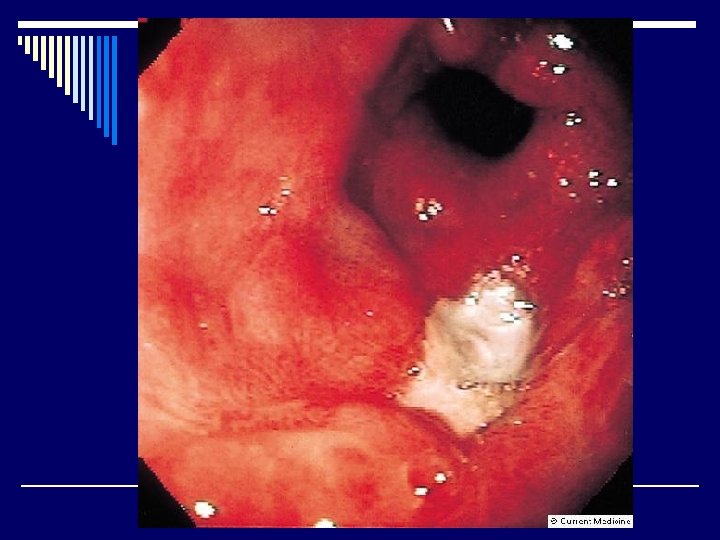
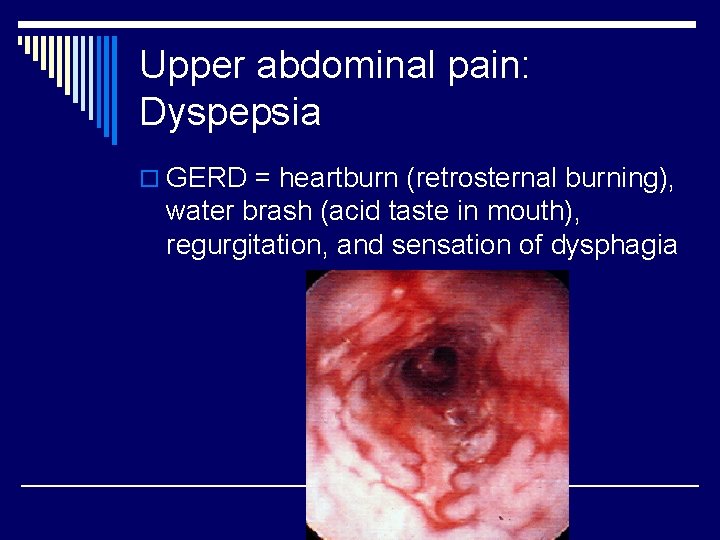
Upper abdominal pain: Dyspepsia o GERD = heartburn (retrosternal burning), water brash (acid taste in mouth), regurgitation, and sensation of dysphagia

Upper abdominal pain: Dyspepsia o Functional dyspepsia = same symptoms but no organic etiology can be found n n 12 weeks over last 12 months Not relieved with BM or associated with alterations in BMs (i. e. , NOT IBS)

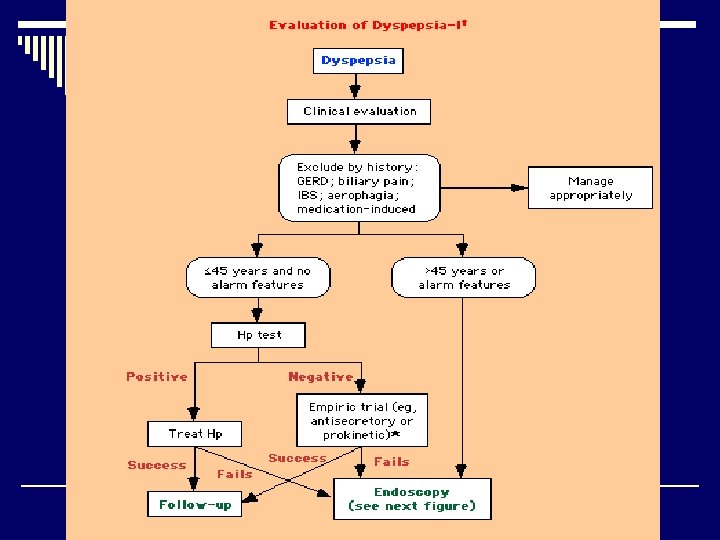
Upper abdominal pain: Dyspepsia o Best test? o 3 strategies n n n Empiric PPI H pylori – test and treat EGD

Gastroparesis o Often overlooked as a cause for epigastric pain o Gastroparesis symptoms n n Nausea 93% Abdominal pain 90% p Epigastric n n burning, vague, cramping Early satiety 86% Vomiting 68%

Gastroparesis o 60% report pain is worse after eating o 80% reports pain interrupted sleep o Vomiting food hours later o Look for important historical clues n Diabetes n Meds (narcotics, anticholinergics) n Recent viral gastroenteritis n CNS disease n Amyloid, scleroderma

Gastroparesis o Workup n EGD or UGI – rule out GOO n Gastric emptying scan

Upper abdominal pain: Pancreatitis o Acute Pancreatitis = acute epigastric pain that radiates to back, constant, severe, rapid onset within 1 hour, lasts days, associated nausea/vomiting, relieved with sitting forward; assoc restlessness o Rarely diffuse pain, RUQ, or LUQ

Upper abdominal pain: Pancreatitis Diagnosis is made when you have at least 2 of the 3 criteria: - Typical pancreatitic pain - Elevation in amylase and lipase - Abnormal imaging

Upper abdominal pain: Pancreatitis o Chronic pancreatitis = similar pain, less severe and onset 20 -30 minutes after a meal, can be episodic (early in disease course) or constant (late finding) o Associated malabsorption (pancreatic exocrine insufficiency) and diabetes (endocrine insufficiency) n Steatorrhea does not occur until 90% or more of pancreatic function is lost
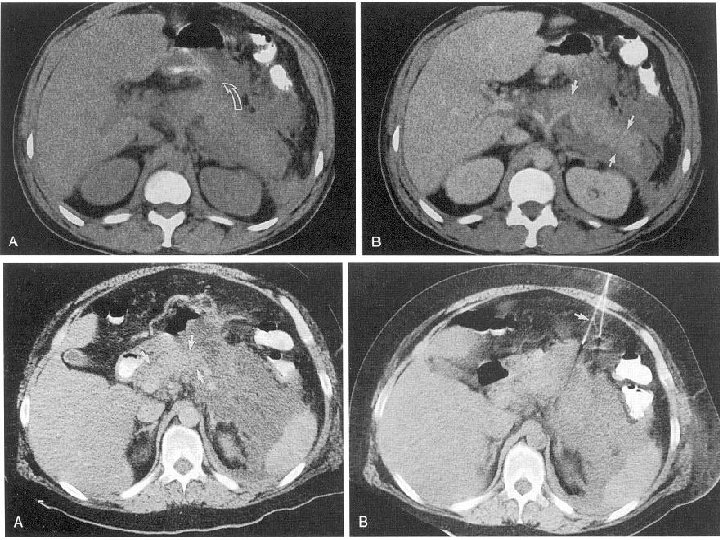

Upper abdominal pain: Other causes o Acute MI o Pneumonia o Splenic abscess or infarct

Lower abdominal pain o Appendicitis o Diverticular disease o IBS o Crohn’s disease o Hernia o Other

Lower abdominal pain o Appendicitis = begins as periumbilical pain that localizes to RLQ (Mc. Burney’s point) n n Initially visceral pain (superior mesenteric ganglion) RLQ when inflammation extends to peritoneal surface (parietal pain) o Pain evolves over hours o Exam: peritoneal irritation (rebound) + fever o Labs: Elevated WBC
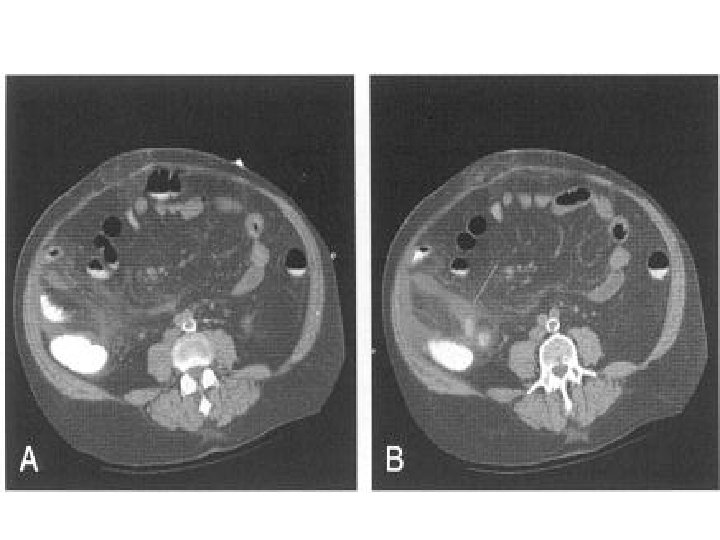

Lower abdominal pain o. Diverticulitis = usually LLQ abdominal pain n Constant w insidious onset Worsening over days Associated symptoms of fever and worsening constipation
Lower abdominal pain o Exam: spectrum of severity n n Mild LLQ tenderness Severe LLQ rebound o Labs: Elevated WBC o Imaging
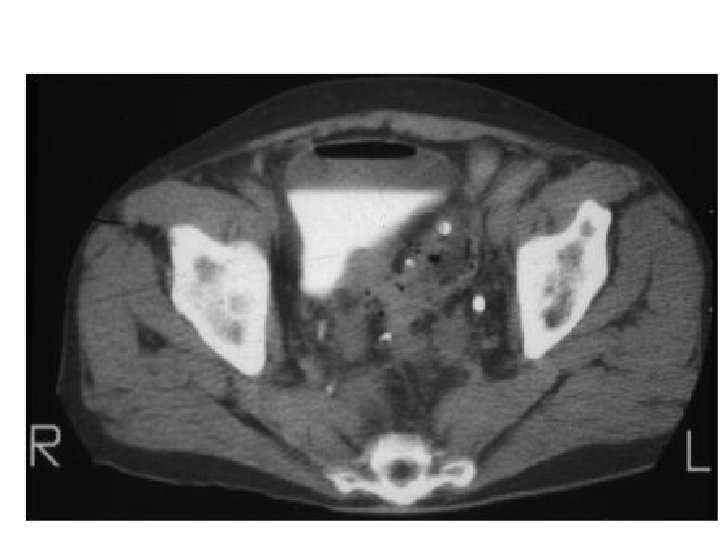

Lower abdominal pain o 70% of diverticulitis in Western countries in left sided. What group of patients usually have right sided diverticultitis (~75%)? o Do seeds cause diverticulitis and should they be avoided?

Lower abdominal pain o IBD can give lower abdominal pain with diarrhea, weight loss, hematochezia, fever n These clues are more obvious o However, 10% of patients with Crohn’s disease will NOT have diarrhea and can present with abdominal pain n n RLQ ileocecal CT, colonoscopy, SBFT

Lower abdominal pain o Hernia = weakness or disruption of the abdominal wall n n n Indirect: at the internal ring Direct: Hesselbach’s triangle Umbilical Epigastric Incisional

Lower abdominal pain o Groin hernias pain or dull pressure with lifting, straining, or increasing intrabdominal pressure; worse with prolonged standing and at end of day n Physical exam is crucial o Outright pain at rest is concerning for strangulation
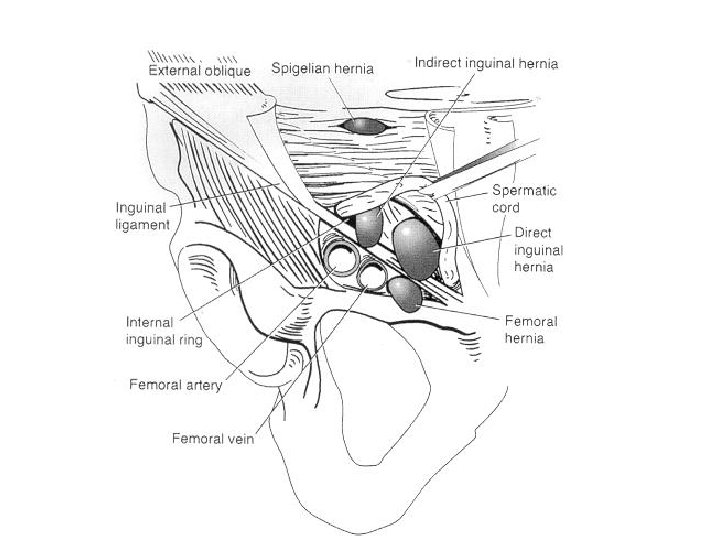

Lower abdominal pain o If in doubt, consult surgery for an opinion o If a hernia is bright red and impossible to reduce, call a surgeon immediately

Lower abdominal pain: Non-GI causes o Nephrolithiasis n n Colicky pain (spasms lasting 20 -60 mins) Site depends on location of stone (flank groin) UA: hematuria (neg in 20 -30% of cases) CT renal stone protocol

Lower abdominal pain: Non-GI causes o Pelvic inflammatory disease n n n Pelvic pain during menses or coitus Onset during of shortly after menses Bilateral Usually less than 2 weeks Exam critical: speculum and bimanual exam

Diffuse abdominal pain o Gastroenteritis o IBS o Obstruction o Mesenteric ischemia

Diffuse abdominal pain o Viral gastroenteritis = colicky abdominal cramps, watery diarrhea, and nausea/vomiting n n Incubation 24 -48 hours Symptoms begin with abdominal cramps and/or nausea most have vomiting and watery diarrhea Mild fever, myalgias Lasts 48 -72 hrs

Diffuse abdominal pain o Obstruction n Periumbilical pain with paroxysms of cramps occurring every 4 -5 minutes Abdominal distension Nausea Obstipation may be delayed up to 24 hours n History of abdominal surgery or malignancy n n n

Diffuse abdominal pain o Obstruction n Exam: distended appearance, tympanic, high pitched tinkle or large bowel sounds NGT decompression n Abdominal x-rays – supine and upright n
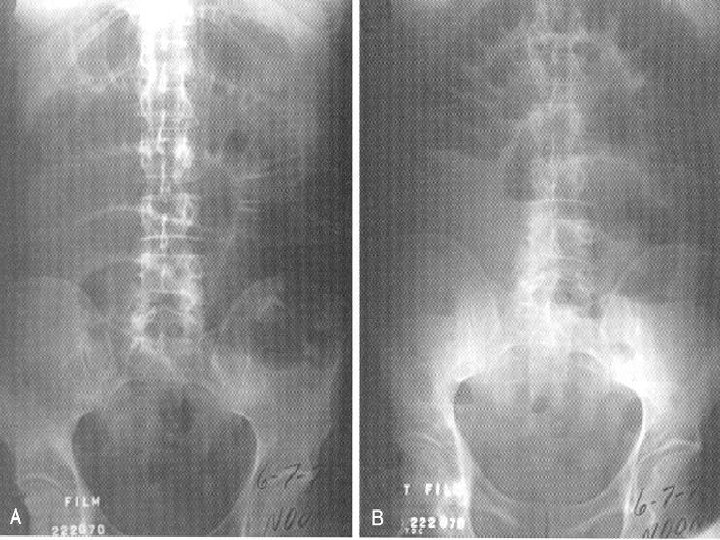

Ischemia o Acute mesenteric ischemia n n n Embolism Thrombosis Vasospasm o Chronic mesenteric ischemia n Intestinal angina o Can be difficult to diagnose

Acute mesenteric ischemia o Embolic sudden onset of severe, diffuse pain n Writhing in pain Abdominal exam feels benign - : pain out of proportion to exam” Be suspicious in the right patient: atrial fibrillation, mechanical heart valves, age

Acute mesenteric ischemia o Thrombotic and non-occlusive insidious onset of pain o Labs: nonspecific until late in the course o Imaging: mesenteric angiogram

Questions?
- Slides: 82