The PNS Afferent Nervous System two kinds of






















- Slides: 103

The PNS: Afferent Nervous System • two kinds of pathways: • 1. Somatic: sensory/afferent information from skeletal muscles, joints, tendons, skin • part of the somatosensory system • receptors are scattered at the body surface • touch, vibration, itch, tickle, temperature, pain & proprioception • processed in the somatosensory cortex • receptors can also become specialized = Special senses

The PNS: Afferent Nervous System • 2. Visceral: sensory information from the internal viscera • receptors are scattered throughout the organs • e. g. blood pressure, body fluid concentration, respiratory gas concentration • this information is critical form determining the appropriate efferent output to maintain homeostasis

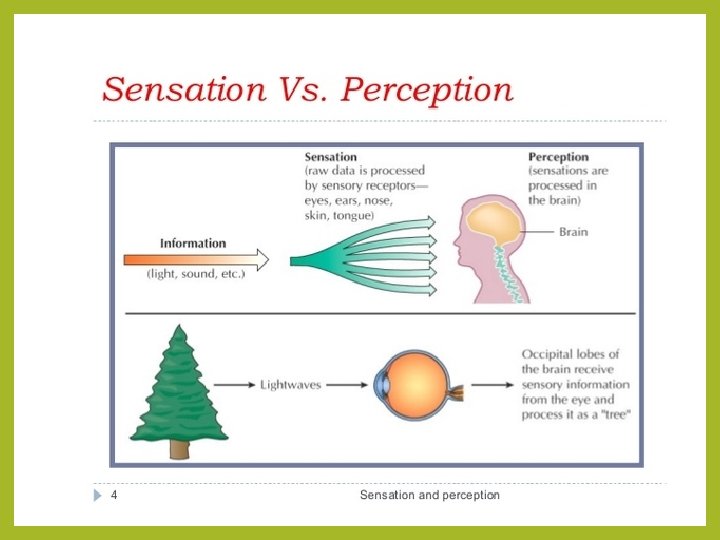
Perception & Sensation • Sensation: response to environment via generation of nerve impulses • before nerve impulse is generated - sensory receptors integrate or sum up the incoming signals • nerve impulses then sent via ascending tracts in spinal cord to the brain • several types of integration: one type is adaptation - decrease in response to a stimulus • role of the thalamus? ? (gatekeeper? ? ) • Perception: our conscious interpretation of the external world • occurs upon arrival of nerve impulse at cerebral cortex • created by the brain based on information it receives from sensory receptors • interpretation of sensation


Sensation • each type of sensation = sensory modality • one type of neuron carries only one type of modality • modalities can be grouped into two classes: • 1. general senses – includes both the somatic and visceral senses • tactile (touch, pressure), thermal, pain, itch, vibration and proprioception • 2. special senses: sight, sound, hearing, taste

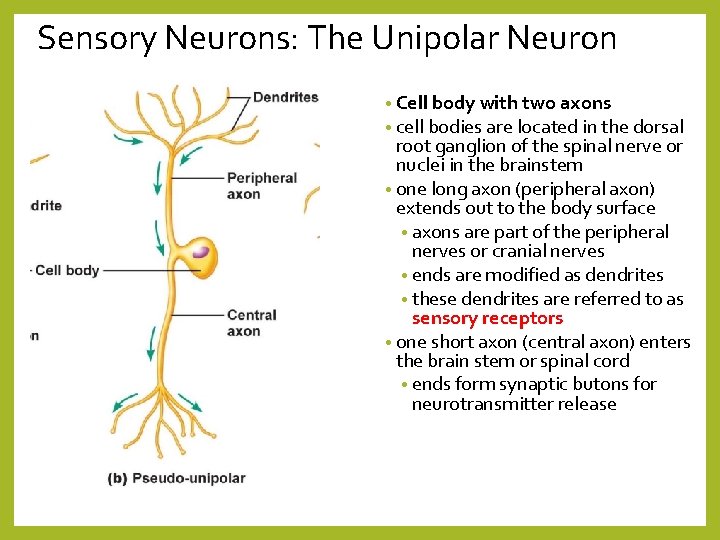
Sensory Neurons: The Unipolar Neuron • Cell body with two axons • cell bodies are located in the dorsal root ganglion of the spinal nerve or nuclei in the brainstem • one long axon (peripheral axon) extends out to the body surface • axons are part of the peripheral nerves or cranial nerves • ends are modified as dendrites • these dendrites are referred to as sensory receptors • one short axon (central axon) enters the brain stem or spinal cord • ends form synaptic butons for neurotransmitter release

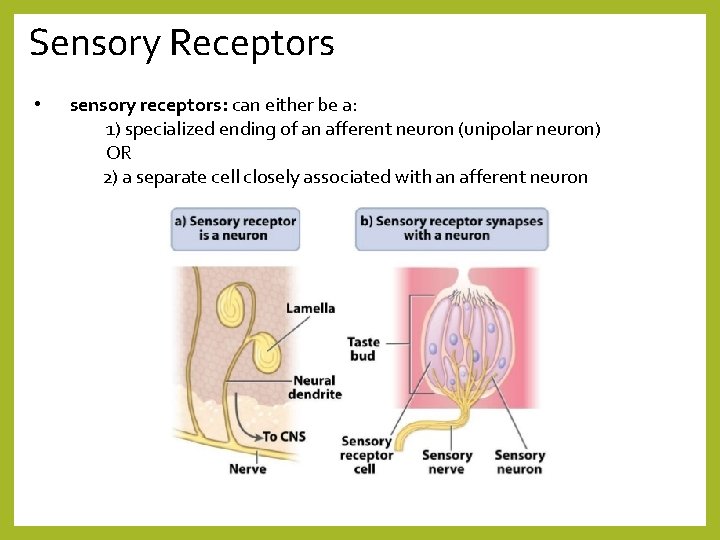
Sensory Receptors • sensory receptors: can either be a: 1) specialized ending of an afferent neuron (unipolar neuron) OR 2) a separate cell closely associated with an afferent neuron

Sensory Receptors • 1. 2. 3. can classify a sensory receptor based on: their microscopic features their location the stimulus that triggers the action potential

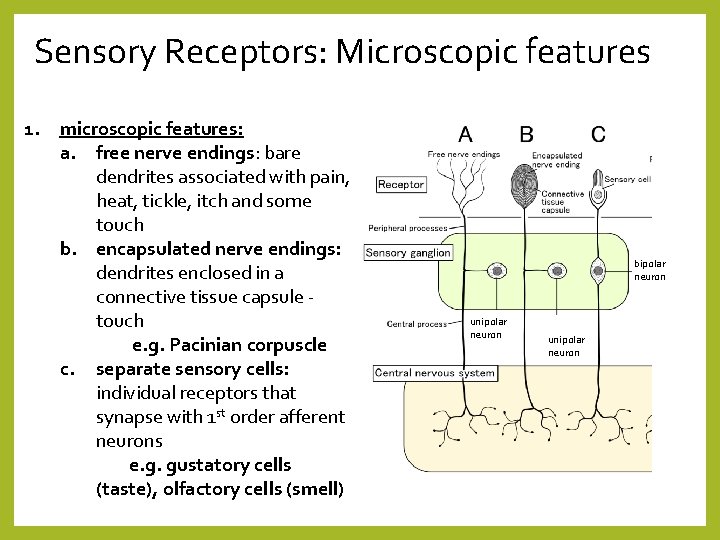
Sensory Receptors: Microscopic features 1. microscopic features: a. free nerve endings: bare dendrites associated with pain, heat, tickle, itch and some touch b. encapsulated nerve endings: dendrites enclosed in a connective tissue capsule touch e. g. Pacinian corpuscle c. separate sensory cells: individual receptors that synapse with 1 st order afferent neurons e. g. gustatory cells (taste), olfactory cells (smell) bipolar neuron unipolar neuron

Sensory Receptors: Location • 2. receptor location: a. exteroceptors: located at or near the body surface - responds to information coming in from the environment (taste, touch, smell, vision, pressure, heat and pain) b. interoceptors: located in blood vessels, visceral organs and the nervous system - provide information about internal environment c. proprioceptors: located in inner ear, skeletal muscle and jointsprovides information about position of limbs and head

Sensory Receptors: Stimulus • 3. type of stimulus: 1. Chemoreceptors (separate cells) 2. Mechanoreceptors (free nerve endings, encapsulated) 3. Nociceptors/pain receptors (free nerve endings) 4. Thermoreceptors (encapsulated) 5. Photoreceptors (separate cells) 6. Osmoreceptors

Sensation Mechanism • 1. stimulation of the sensory receptor (dendrites of neuron) • stimulus alters the permeability of the sensory neuron’s plasma membrane to ions • 2. transduction of the stimulus • increased influx of Na+ ions depolarization (i. e. graded receptor potential) • bigger the stimulus = stronger the graded potential threshold • 3. generation of the nerve impulse • increase in graded potential past threshold -> Action Potential • AP propagates toward the CNS • 4. integration of the sensory input • receipt of sensory information by a particular region in the CNS • integration of sensation perception

SENSORY PATHWAYS

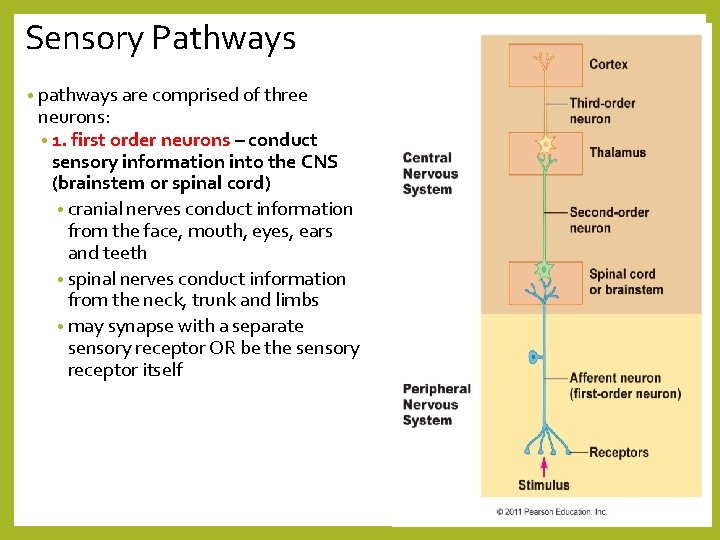
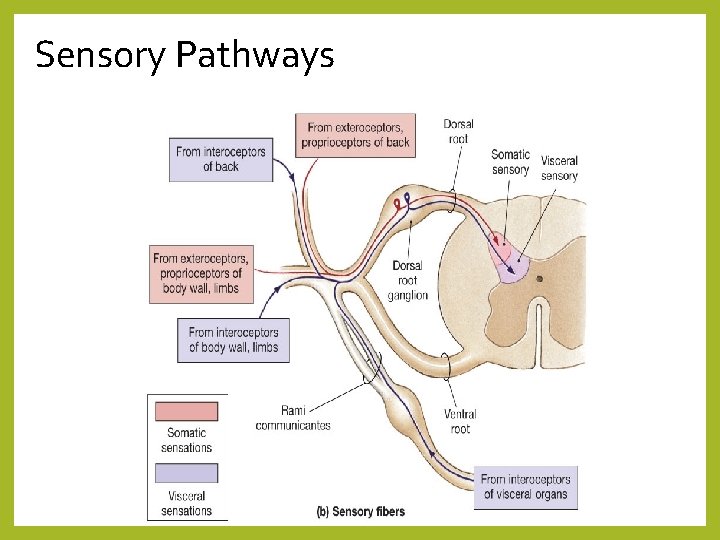
Sensory Pathways • pathways are comprised of three neurons: • 1. first order neurons – conduct sensory information into the CNS (brainstem or spinal cord) • cranial nerves conduct information from the face, mouth, eyes, ears and teeth • spinal nerves conduct information from the neck, trunk and limbs • may synapse with a separate sensory receptor OR be the sensory receptor itself

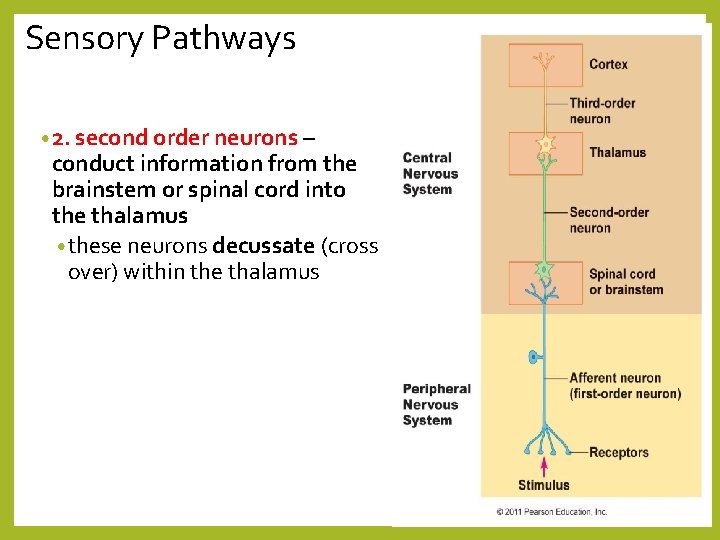
Sensory Pathways • 2. second order neurons – conduct information from the brainstem or spinal cord into the thalamus • these neurons decussate (cross over) within the thalamus

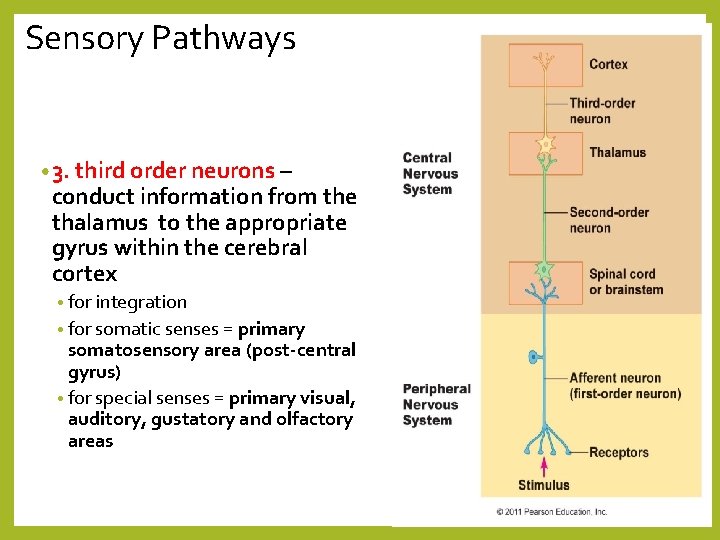
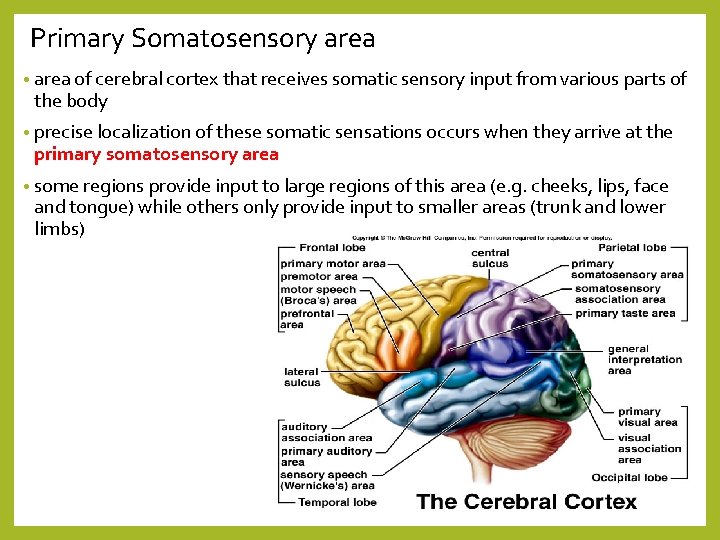
Sensory Pathways • 3. third order neurons – conduct information from the thalamus to the appropriate gyrus within the cerebral cortex • for integration • for somatic senses = primary somatosensory area (post-central gyrus) • for special senses = primary visual, auditory, gustatory and olfactory areas

Sensory Pathways

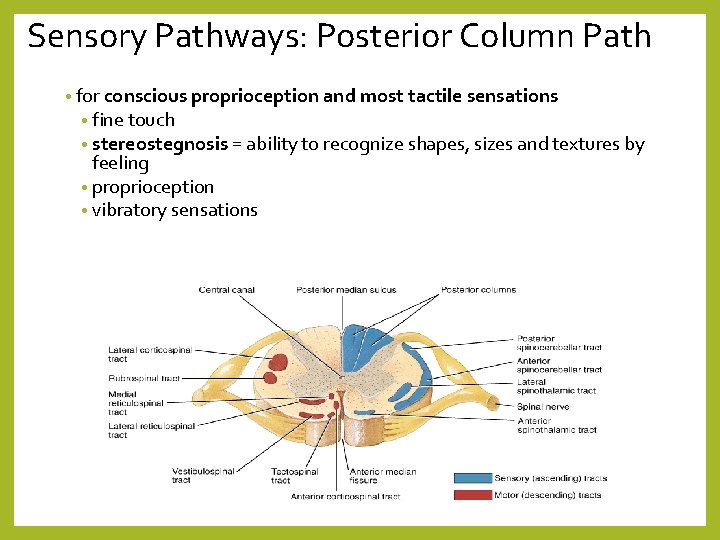
Sensory Pathways: Posterior Column Path • for conscious proprioception and most tactile sensations • fine touch • stereostegnosis = ability to recognize shapes, sizes and textures by feeling • proprioception • vibratory sensations

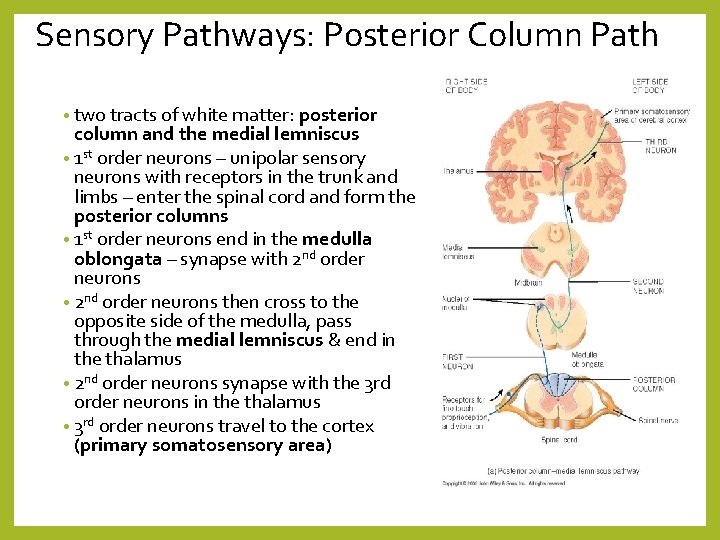
Sensory Pathways: Posterior Column Path • two tracts of white matter: posterior column and the medial lemniscus • 1 st order neurons – unipolar sensory neurons with receptors in the trunk and limbs – enter the spinal cord and form the posterior columns • 1 st order neurons end in the medulla oblongata – synapse with 2 nd order neurons • 2 nd order neurons then cross to the opposite side of the medulla, pass through the medial lemniscus & end in the thalamus • 2 nd order neurons synapse with the 3 rd order neurons in the thalamus • 3 rd order neurons travel to the cortex (primary somatosensory area)

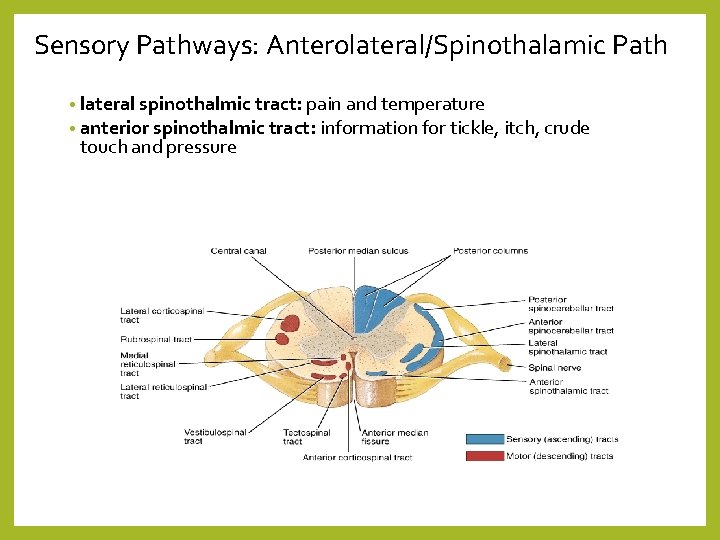
Sensory Pathways: Anterolateral/Spinothalamic Path • lateral spinothalmic tract: pain and temperature • anterior spinothalmic tract: information for tickle, itch, crude touch and pressure

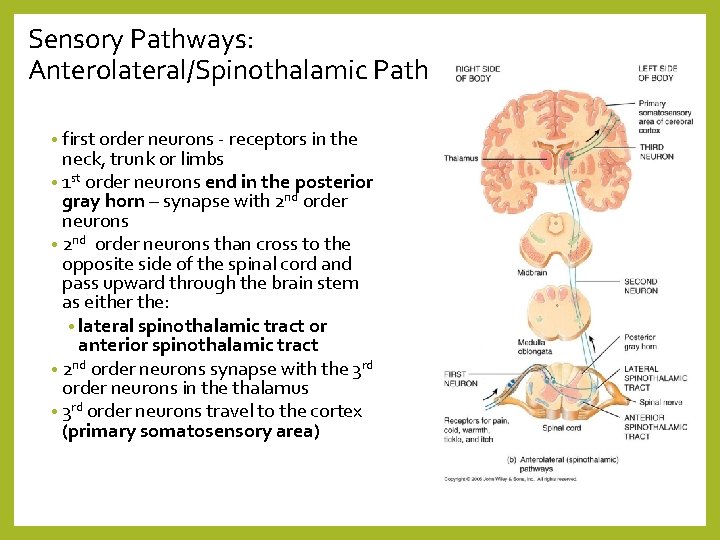
Sensory Pathways: Anterolateral/Spinothalamic Path • first order neurons - receptors in the neck, trunk or limbs • 1 st order neurons end in the posterior gray horn – synapse with 2 nd order neurons • 2 nd order neurons than cross to the opposite side of the spinal cord and pass upward through the brain stem as either the: • lateral spinothalamic tract or anterior spinothalamic tract • 2 nd order neurons synapse with the 3 rd order neurons in the thalamus • 3 rd order neurons travel to the cortex (primary somatosensory area)

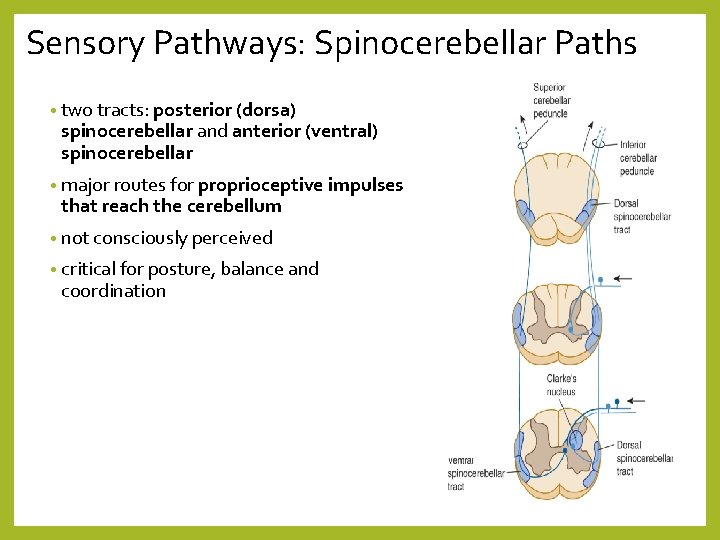
Sensory Pathways: Spinocerebellar Paths • two tracts: posterior (dorsa) spinocerebellar and anterior (ventral) spinocerebellar • major routes for proprioceptive impulses that reach the cerebellum • not consciously perceived • critical for posture, balance and coordination

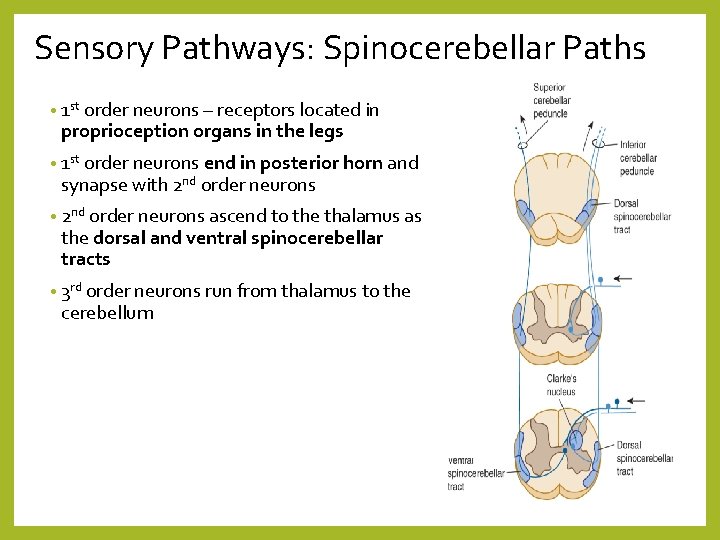
Sensory Pathways: Spinocerebellar Paths • 1 st order neurons – receptors located in proprioception organs in the legs • 1 st order neurons end in posterior horn and synapse with 2 nd order neurons • 2 nd order neurons ascend to the thalamus as the dorsal and ventral spinocerebellar tracts • 3 rd order neurons run from thalamus to the cerebellum

Primary Somatosensory area • area of cerebral cortex that receives somatic sensory input from various parts of the body • precise localization of these somatic sensations occurs when they arrive at the primary somatosensory area • some regions provide input to large regions of this area (e. g. cheeks, lips, face and tongue) while others only provide input to smaller areas (trunk and lower limbs)

GENERAL SENSES Proprioception & Touch

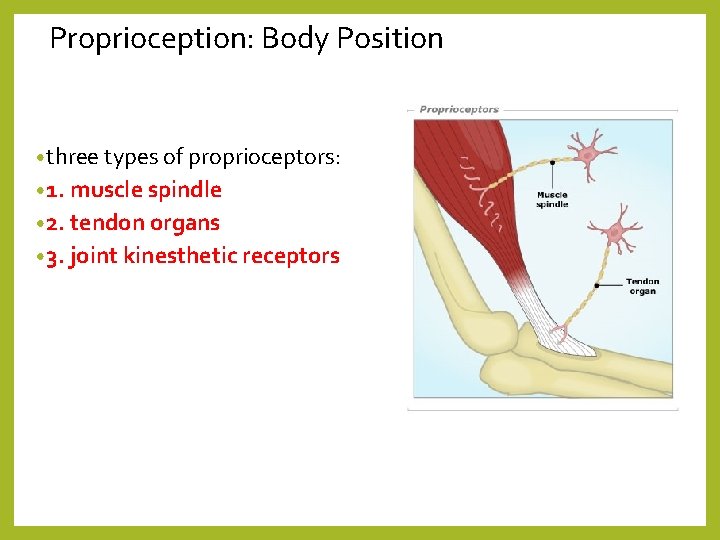
Proprioception: Body position • proprioception: perception of body position and speed • differs from exteroception (perception of outside world) and interception (perception of internal condition of organs, pain, hunger) • detected by mechanoreceptors known as proprioceptors • proprioceptors are located in skeletal muscles, joints, tendons and the inner ear • allow us to estimate weight and to determine how much muscular effort is needed for a specific muscular task

Proprioception: Body Position • three types of proprioceptors: • 1. muscle spindle • 2. tendon organs • 3. joint kinesthetic receptors

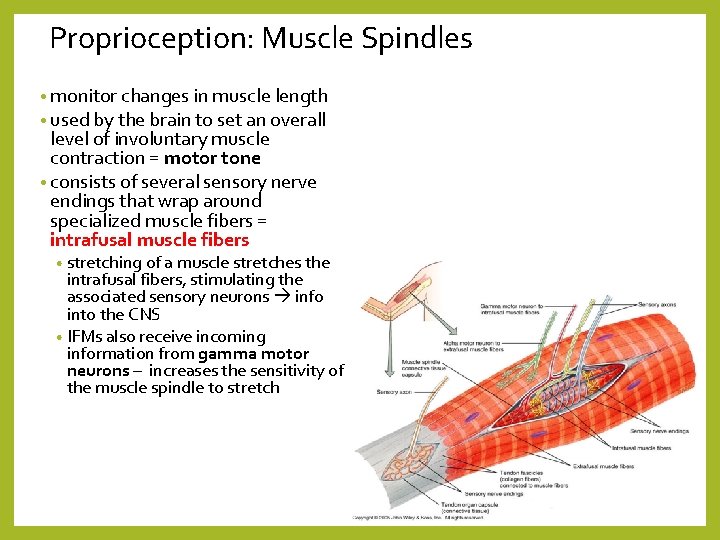
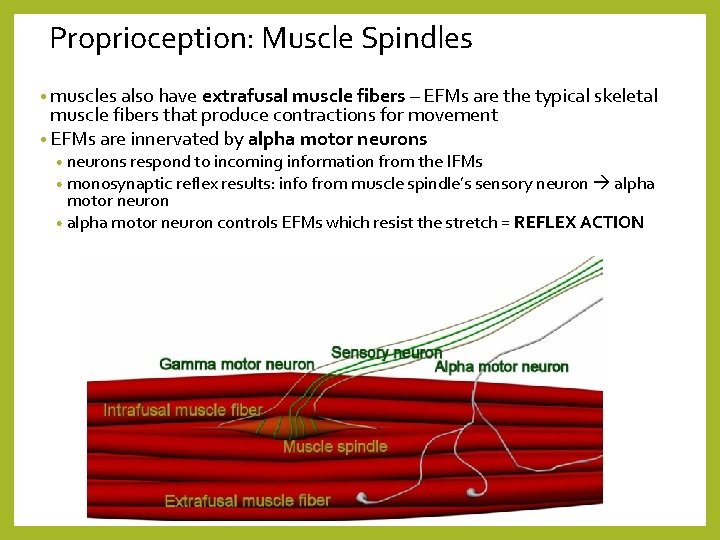
Proprioception: Muscle Spindles • monitor changes in muscle length • used by the brain to set an overall level of involuntary muscle contraction = motor tone • consists of several sensory nerve endings that wrap around specialized muscle fibers = intrafusal muscle fibers • stretching of a muscle stretches the intrafusal fibers, stimulating the associated sensory neurons info into the CNS • IFMs also receive incoming information from gamma motor neurons – increases the sensitivity of the muscle spindle to stretch

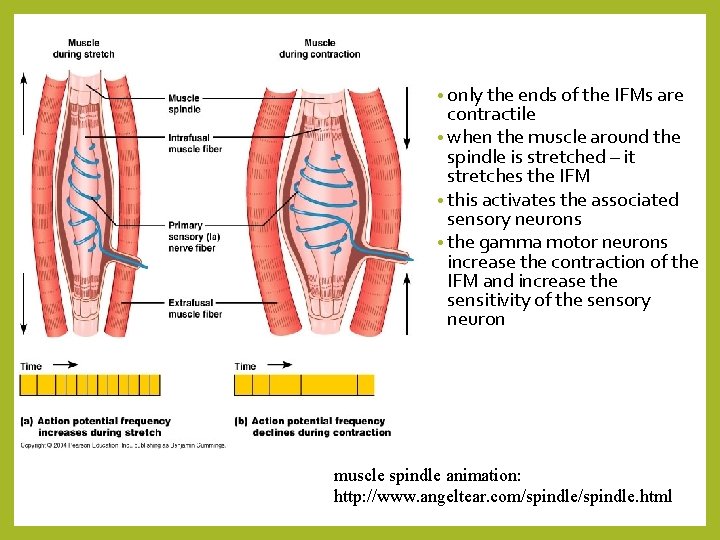
• only the ends of the IFMs are contractile • when the muscle around the spindle is stretched – it stretches the IFM • this activates the associated sensory neurons • the gamma motor neurons increase the contraction of the IFM and increase the sensitivity of the sensory neuron muscle spindle animation: http: //www. angeltear. com/spindle. html

Proprioception: Muscle Spindles • muscles also have extrafusal muscle fibers – EFMs are the typical skeletal muscle fibers that produce contractions for movement • EFMs are innervated by alpha motor neurons • neurons respond to incoming information from the IFMs • monosynaptic reflex results: info from muscle spindle’s sensory neuron alpha motor neuron • alpha motor neuron controls EFMs which resist the stretch = REFLEX ACTION

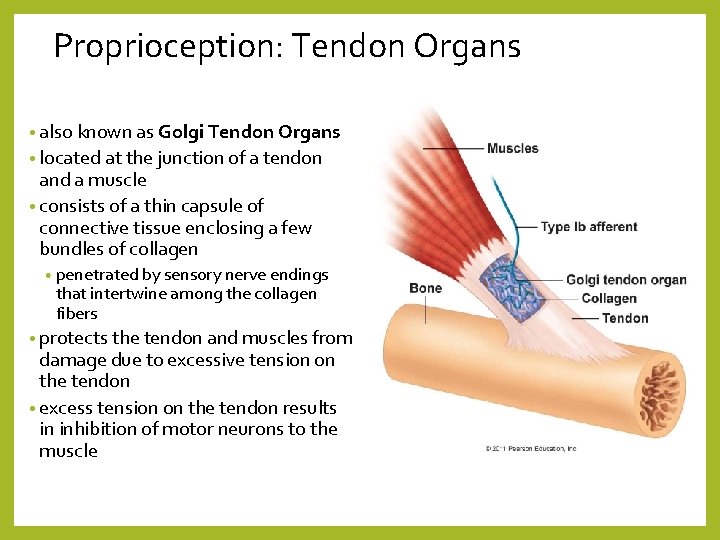
Proprioception: Tendon Organs • also known as Golgi Tendon Organs • located at the junction of a tendon and a muscle • consists of a thin capsule of connective tissue enclosing a few bundles of collagen • penetrated by sensory nerve endings that intertwine among the collagen fibers • protects the tendon and muscles from damage due to excessive tension on the tendon • excess tension on the tendon results in inhibition of motor neurons to the muscle

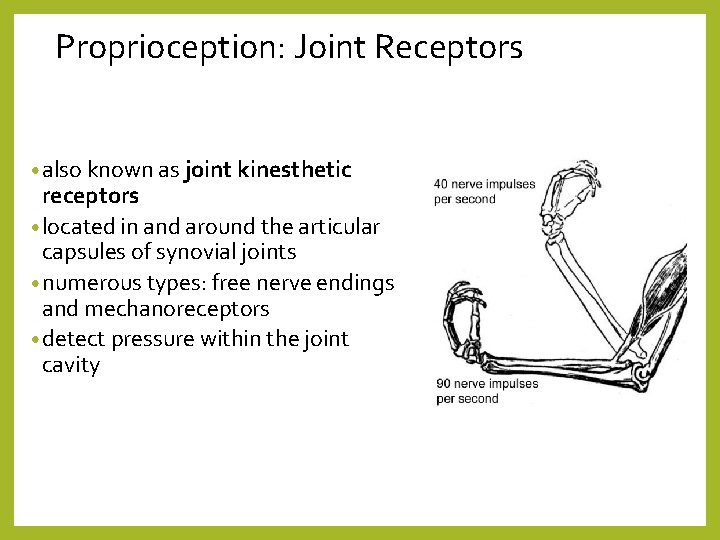
Proprioception: Joint Receptors • also known as joint kinesthetic receptors • located in and around the articular capsules of synovial joints • numerous types: free nerve endings and mechanoreceptors • detect pressure within the joint cavity

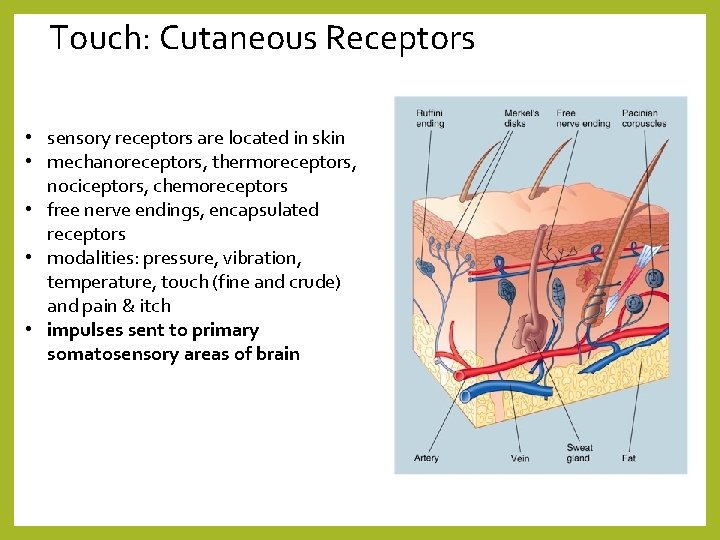
Touch: Cutaneous Receptors • sensory receptors are located in skin • mechanoreceptors, thermoreceptors, nociceptors, chemoreceptors • free nerve endings, encapsulated receptors • modalities: pressure, vibration, temperature, touch (fine and crude) and pain & itch • impulses sent to primary somatosensory areas of brain

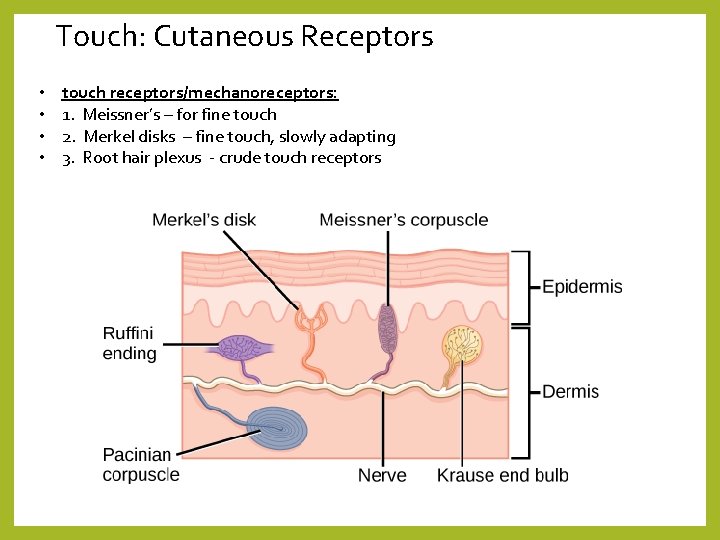
Touch: Cutaneous Receptors • • touch receptors/mechanoreceptors: 1. Meissner’s – for fine touch 2. Merkel disks – fine touch, slowly adapting 3. Root hair plexus - crude touch receptors

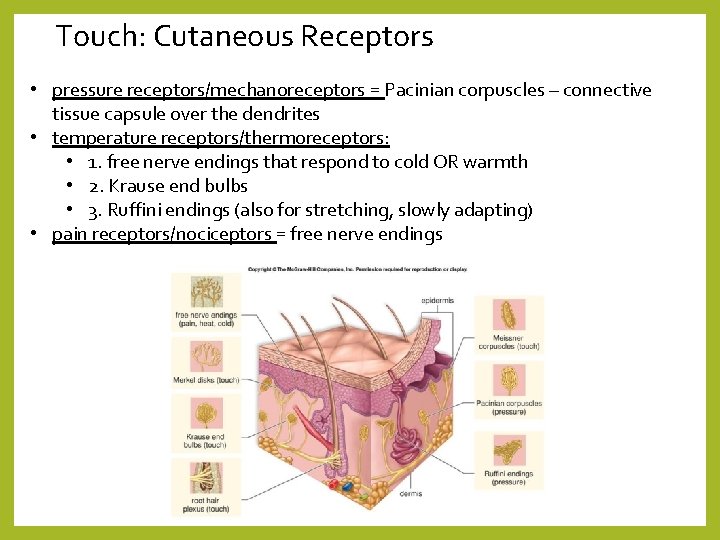
Touch: Cutaneous Receptors • pressure receptors/mechanoreceptors = Pacinian corpuscles – connective tissue capsule over the dendrites • temperature receptors/thermoreceptors: • 1. free nerve endings that respond to cold OR warmth • 2. Krause end bulbs • 3. Ruffini endings (also for stretching, slowly adapting) • pain receptors/nociceptors = free nerve endings

SPECIAL SENSES Sight, Sound, Taste, Smell

Taste: Chemoreceptors fungiform • taste requires dissolving of substances & their binding to sensory receptors • sensory receptors are located in taste buds: salty, sweet, bitter and sour • 10, 000 taste buds found on tongue, soft palate & larynx • found associated with projections called papillae • 1. fungiform • 2. circumvallate • 3. foliate • (4. filiform – no taste buds; for texture) filiform fungiform foliate

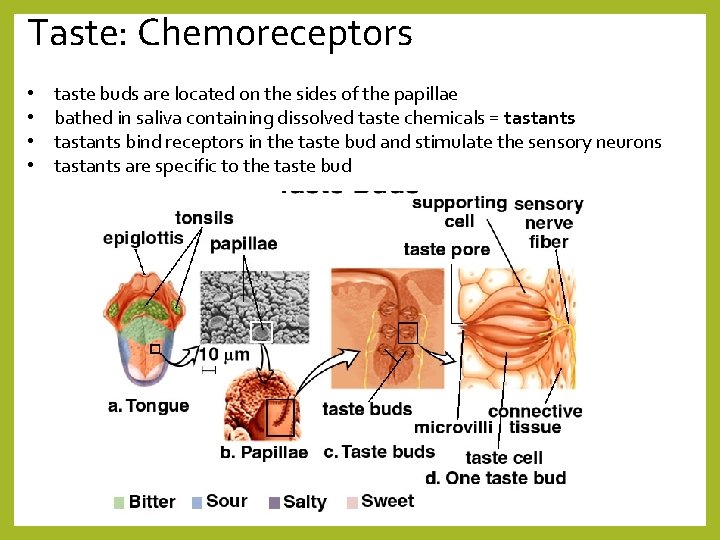
Taste: Chemoreceptors • • taste buds are located on the sides of the papillae bathed in saliva containing dissolved taste chemicals = tastants bind receptors in the taste bud and stimulate the sensory neurons tastants are specific to the taste bud

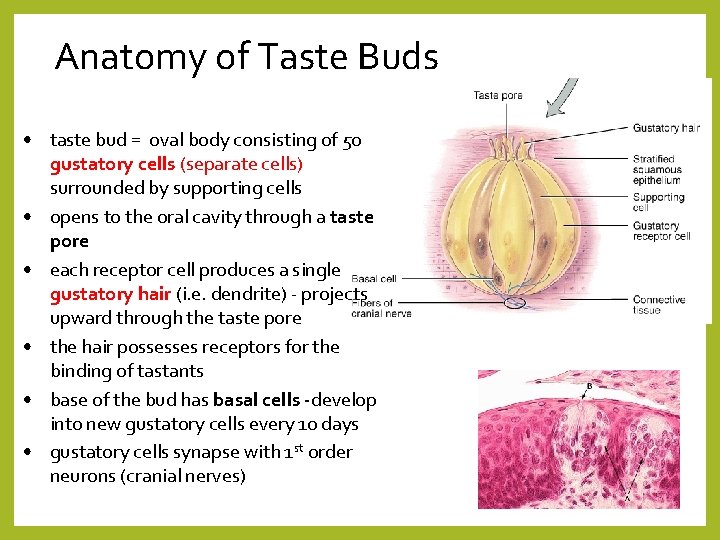
Anatomy of Taste Buds • taste bud = oval body consisting of 50 gustatory cells (separate cells) surrounded by supporting cells • opens to the oral cavity through a taste pore • each receptor cell produces a single gustatory hair (i. e. dendrite) - projects upward through the taste pore • the hair possesses receptors for the binding of tastants • base of the bud has basal cells -develop into new gustatory cells every 10 days • gustatory cells synapse with 1 st order neurons (cranial nerves)

Physiology of Taste • receptor-ligand interaction – ligand is the tastant and the receptor is the gustatory cell • tastant binding leads to a change in the receptor potential – action potential • release of neurotransmitters from the taste cell – binds to and stimulates the first order neuron (cranial nerves VII, IX and X) • complete adaptation in 1 to 5 minutes • thresholds for tastes vary among the 4 primary tastes – most sensitive to bitter (poisons) – least sensitive to salty and sweet

Physiology of Taste • mechanism is distinct for different tastants – e. g. salty foods – Na+ enters the gustatory cell via ligand-gated channels depolarization & release of NTs (direct method) – BUT other tastants do NOT enter the cell but bind to G protein coupled receptors in the plasma membrane - trigger the production of a second messenger which than causes a depolarization and action potential (indirect method)

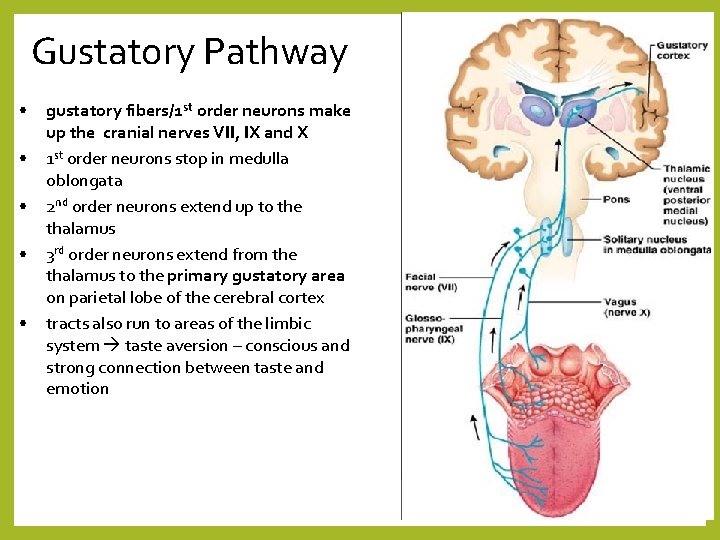
Gustatory Pathway • • • gustatory fibers/1 st order neurons make up the cranial nerves VII, IX and X 1 st order neurons stop in medulla oblongata 2 nd order neurons extend up to the thalamus 3 rd order neurons extend from the thalamus to the primary gustatory area on parietal lobe of the cerebral cortex tracts also run to areas of the limbic system taste aversion – conscious and strong connection between taste and emotion

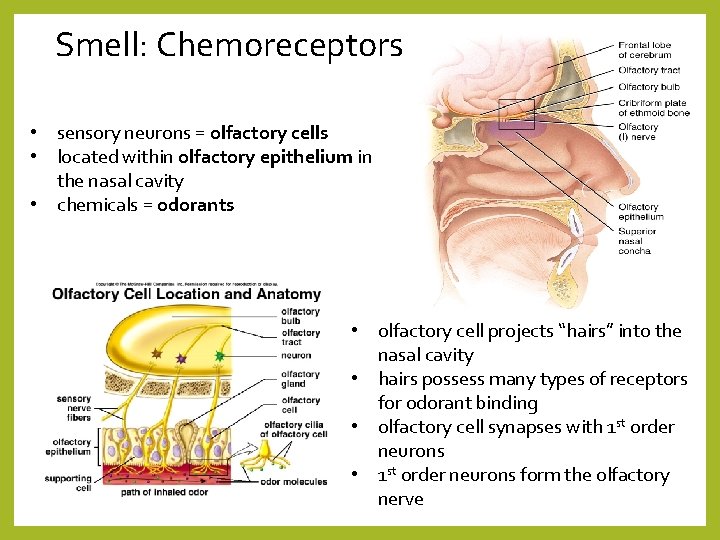
Smell: Chemoreceptors • sensory neurons = olfactory cells • located within olfactory epithelium in the nasal cavity • chemicals = odorants • olfactory cell projects “hairs” into the nasal cavity • hairs possess many types of receptors for odorant binding • olfactory cell synapses with 1 st order neurons • 1 st order neurons form the olfactory nerve

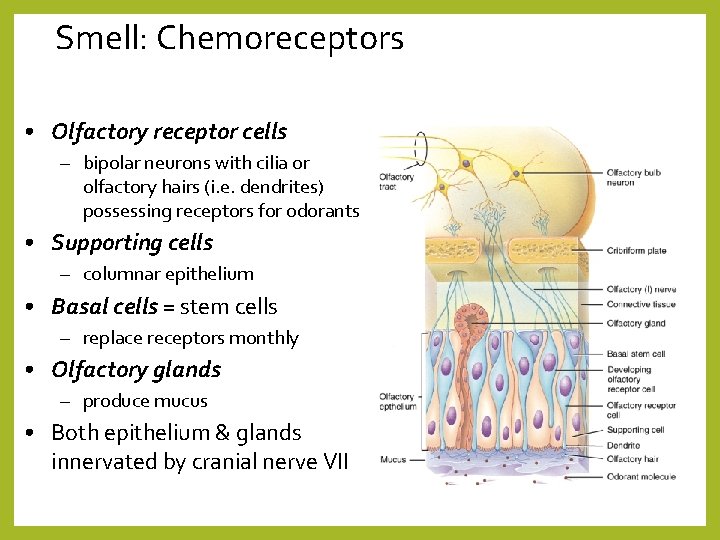
Smell: Chemoreceptors • Olfactory receptor cells – bipolar neurons with cilia or olfactory hairs (i. e. dendrites) possessing receptors for odorants • Supporting cells – columnar epithelium • Basal cells = stem cells – replace receptors monthly • Olfactory glands – produce mucus • Both epithelium & glands innervated by cranial nerve VII

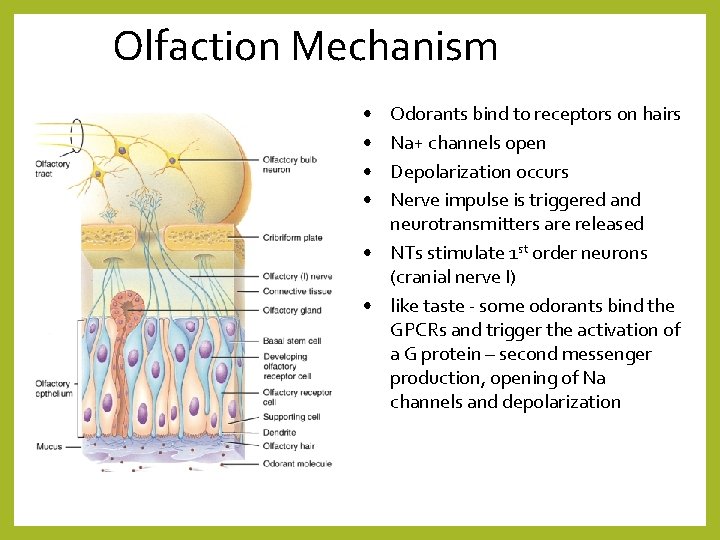
Olfaction Mechanism • • Odorants bind to receptors on hairs Na+ channels open Depolarization occurs Nerve impulse is triggered and neurotransmitters are released • NTs stimulate 1 st order neurons (cranial nerve I) • like taste - some odorants bind the GPCRs and trigger the activation of a G protein – second messenger production, opening of Na channels and depolarization

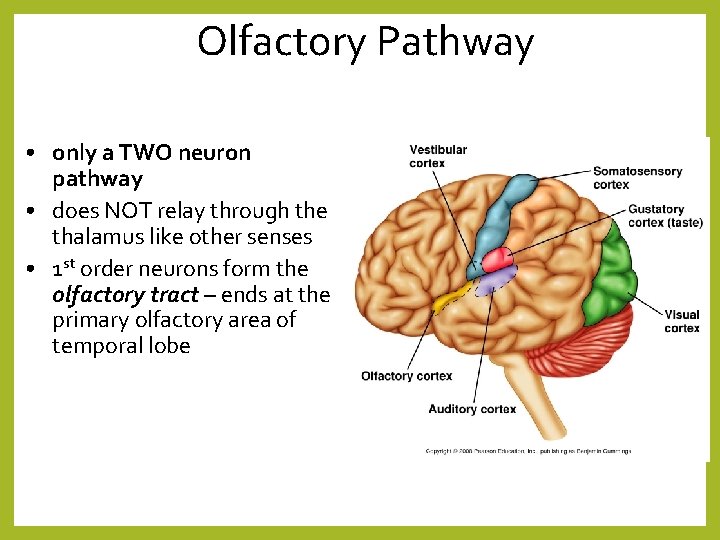
Olfactory Pathway • only a TWO neuron pathway • does NOT relay through the thalamus like other senses • 1 st order neurons form the olfactory tract – ends at the primary olfactory area of temporal lobe

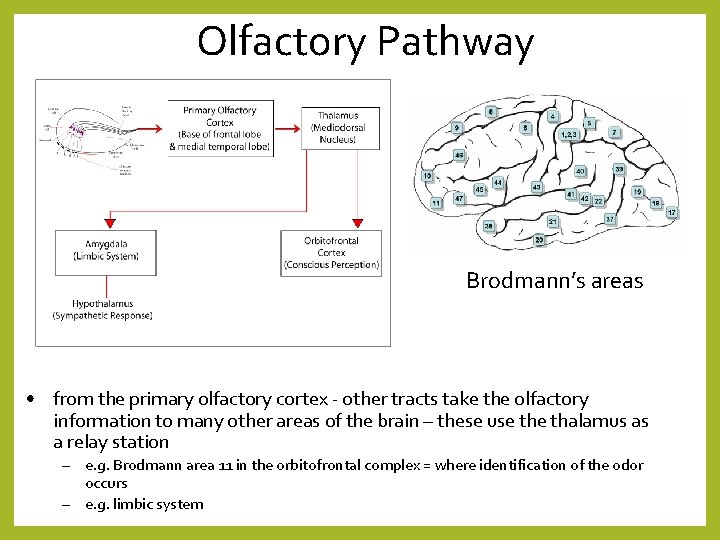
Olfactory Pathway Brodmann’s areas • from the primary olfactory cortex - other tracts take the olfactory information to many other areas of the brain – these use thalamus as a relay station – e. g. Brodmann area 11 in the orbitofrontal complex = where identification of the odor occurs – e. g. limbic system

Adaptation & Odor Thresholds • Olfactory adaptation is rapid – 50% in 1 second – complete in 1 minute • Low threshold – only a few odorant molecules need to be present • hyperosmia – keener sense of smell then others – seen in women (time of ovulation) – opposite is hyposmia –reduction in the sense of smell

NEXT CLASS Vision & Hearing

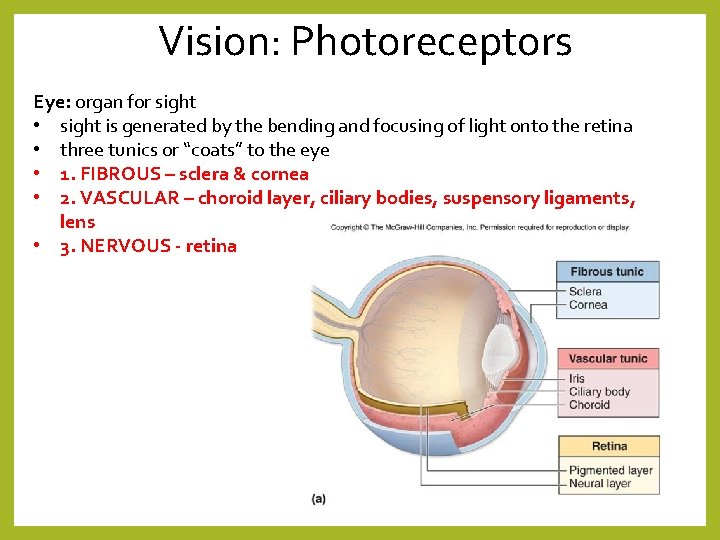
Vision: Photoreceptors Eye: organ for sight • sight is generated by the bending and focusing of light onto the retina • three tunics or “coats” to the eye • 1. FIBROUS – sclera & cornea • 2. VASCULAR – choroid layer, ciliary bodies, suspensory ligaments, lens • 3. NERVOUS - retina


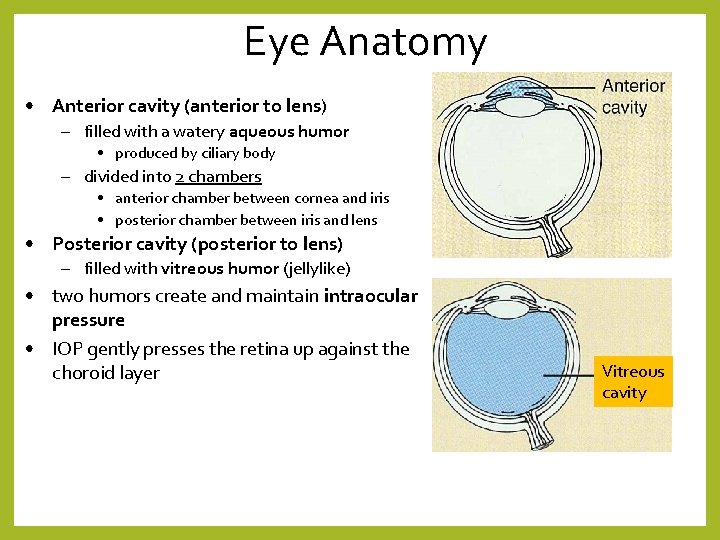
Eye Anatomy • Anterior cavity (anterior to lens) – filled with a watery aqueous humor • produced by ciliary body – divided into 2 chambers • anterior chamber between cornea and iris • posterior chamber between iris and lens • Posterior cavity (posterior to lens) – filled with vitreous humor (jellylike) • two humors create and maintain intraocular pressure • IOP gently presses the retina up against the choroid layer Vitreous cavity

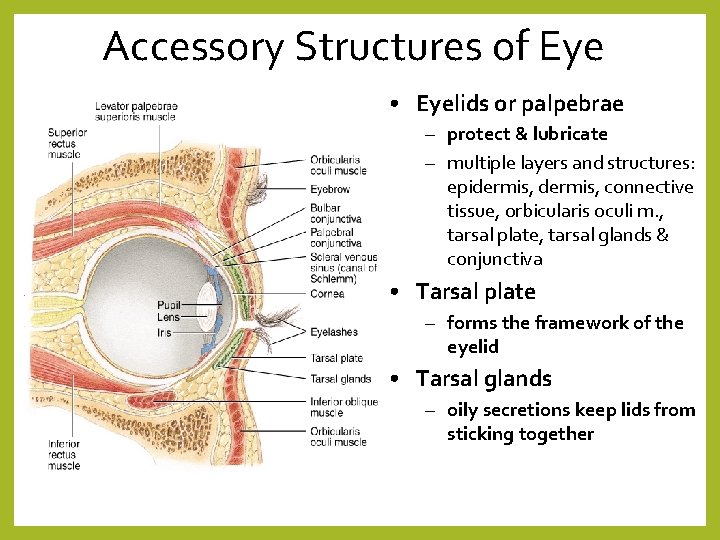
Accessory Structures of Eye • Eyelids or palpebrae – protect & lubricate – multiple layers and structures: epidermis, connective tissue, orbicularis oculi m. , tarsal plate, tarsal glands & conjunctiva • Tarsal plate – forms the framework of the eyelid • Tarsal glands – oily secretions keep lids from sticking together

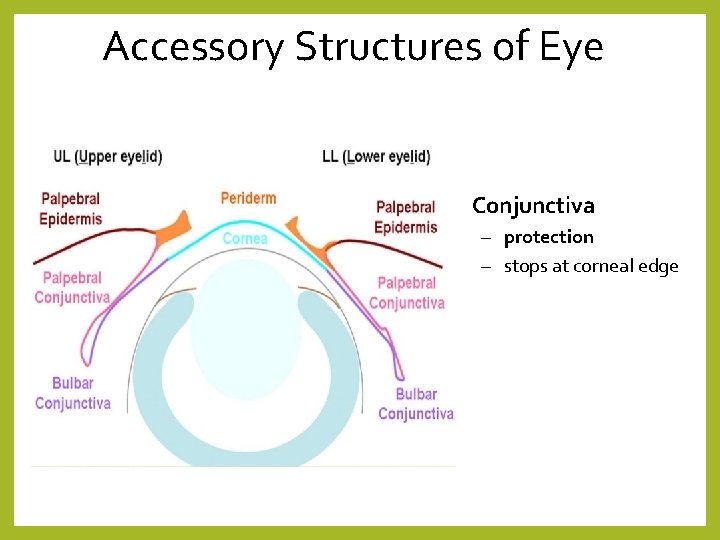
Accessory Structures of Eye • Conjunctiva – protection – stops at corneal edge

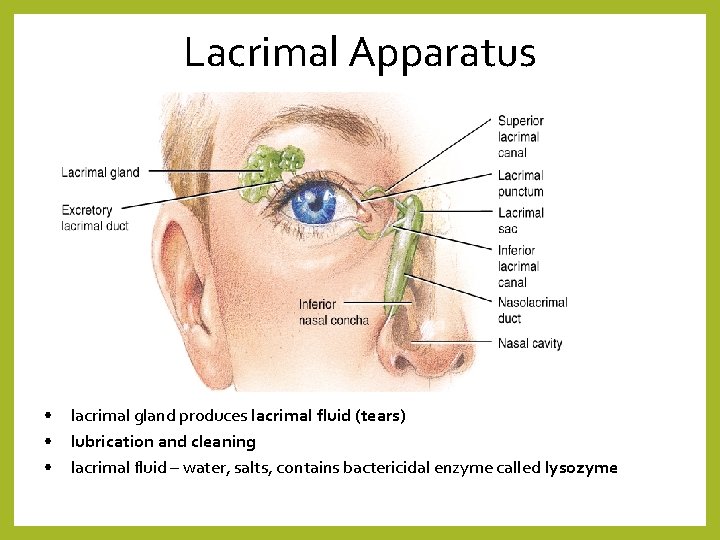
Lacrimal Apparatus • • • lacrimal gland produces lacrimal fluid (tears) lubrication and cleaning lacrimal fluid – water, salts, contains bactericidal enzyme called lysozyme

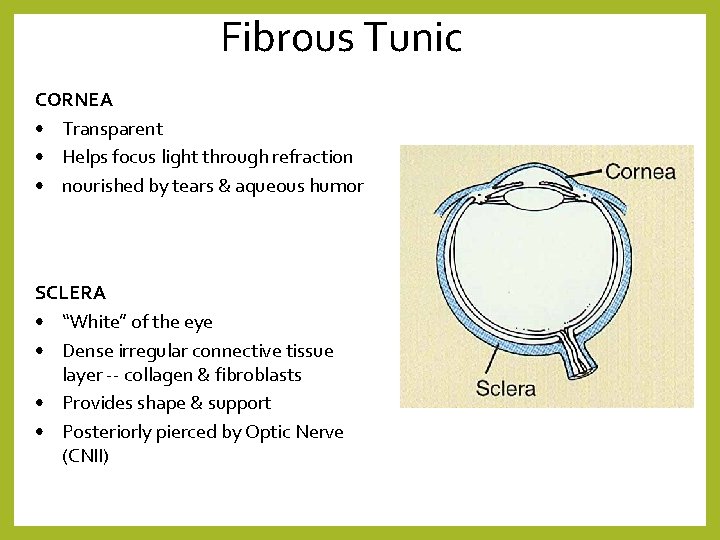
Fibrous Tunic CORNEA • Transparent • Helps focus light through refraction • nourished by tears & aqueous humor SCLERA • “White” of the eye • Dense irregular connective tissue layer -- collagen & fibroblasts • Provides shape & support • Posteriorly pierced by Optic Nerve (CNII)

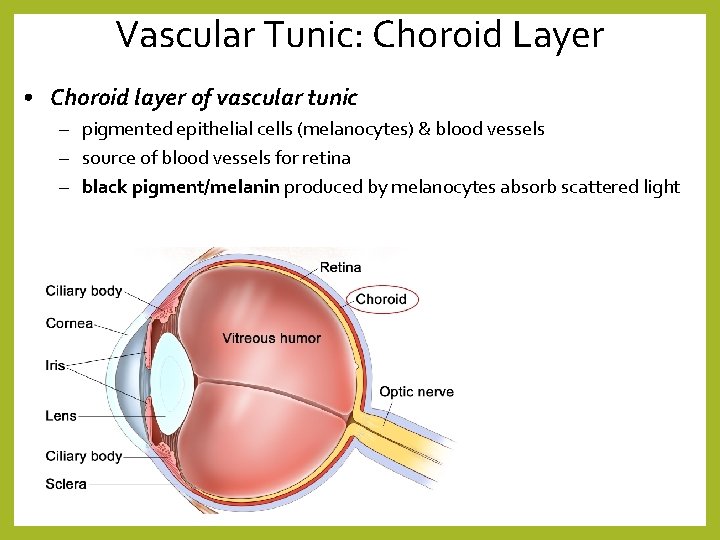
Vascular Tunic: Choroid Layer • Choroid layer of vascular tunic – pigmented epithelial cells (melanocytes) & blood vessels – source of blood vessels for retina – black pigment/melanin produced by melanocytes absorb scattered light

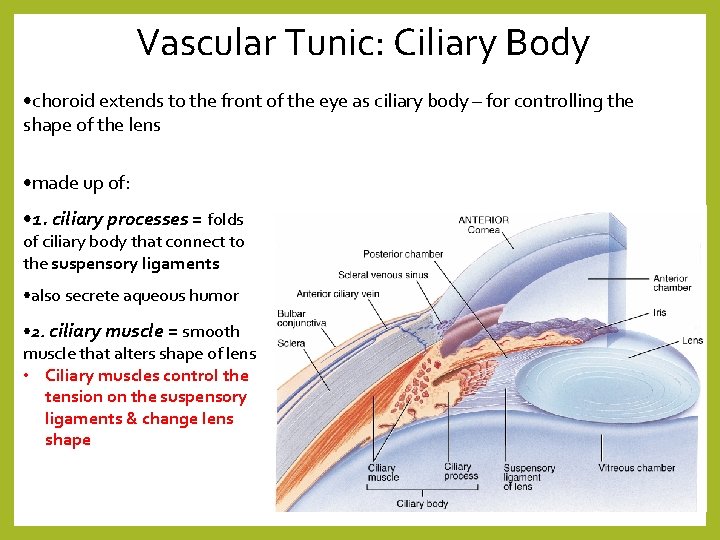
Vascular Tunic: Ciliary Body • choroid extends to the front of the eye as ciliary body – for controlling the shape of the lens • made up of: • 1. ciliary processes = folds of ciliary body that connect to the suspensory ligaments • also secrete aqueous humor • 2. ciliary muscle = smooth muscle that alters shape of lens • Ciliary muscles control the tension on the suspensory ligaments & change lens shape

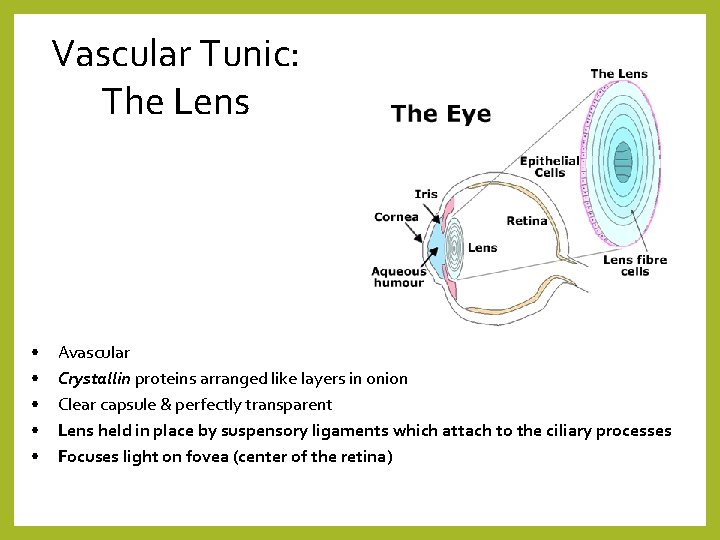
Vascular Tunic: The Lens • • • Avascular Crystallin proteins arranged like layers in onion Clear capsule & perfectly transparent Lens held in place by suspensory ligaments which attach to the ciliary processes Focuses light on fovea (center of the retina)

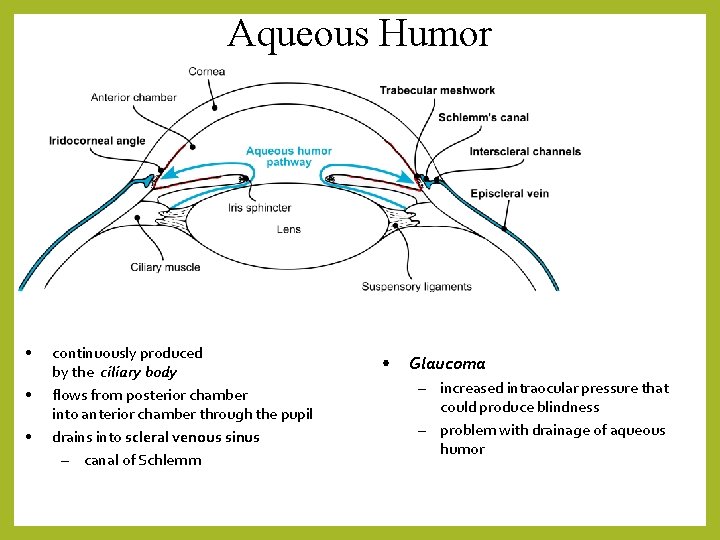
Aqueous Humor • • • continuously produced by the ciliary body flows from posterior chamber into anterior chamber through the pupil drains into scleral venous sinus – canal of Schlemm • Glaucoma – increased intraocular pressure that could produce blindness – problem with drainage of aqueous humor

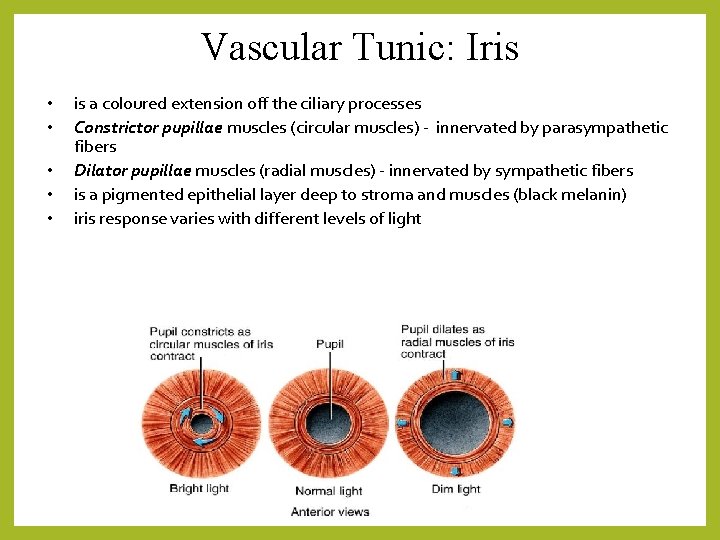
Vascular Tunic: Iris • • • is a coloured extension off the ciliary processes Constrictor pupillae muscles (circular muscles) - innervated by parasympathetic fibers Dilator pupillae muscles (radial muscles) - innervated by sympathetic fibers is a pigmented epithelial layer deep to stroma and muscles (black melanin) iris response varies with different levels of light

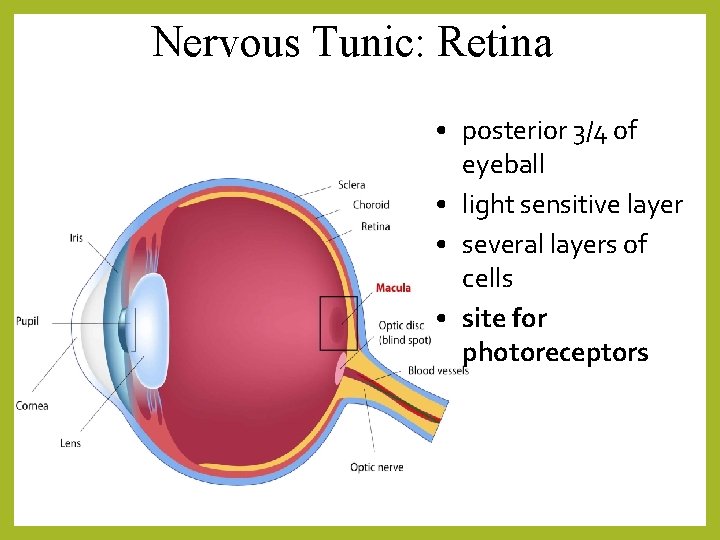
Nervous Tunic: Retina • posterior 3/4 of eyeball • light sensitive layer • several layers of cells • site for photoreceptors

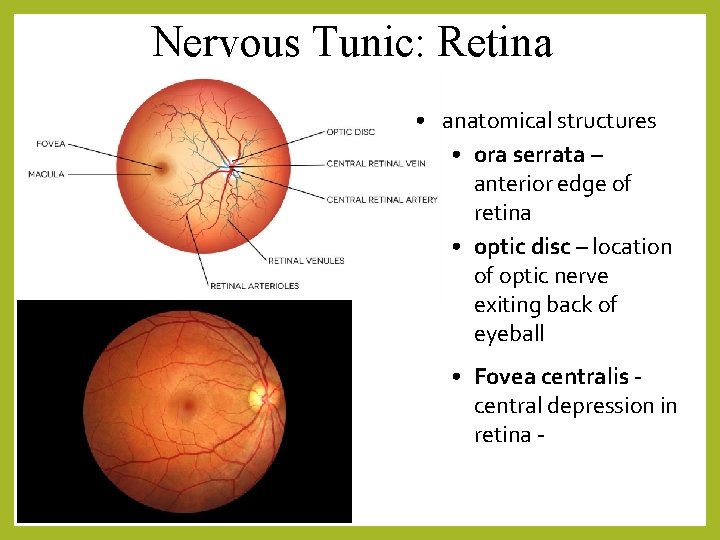
Nervous Tunic: Retina • anatomical structures • ora serrata – anterior edge of retina • optic disc – location of optic nerve exiting back of eyeball • Fovea centralis central depression in retina -

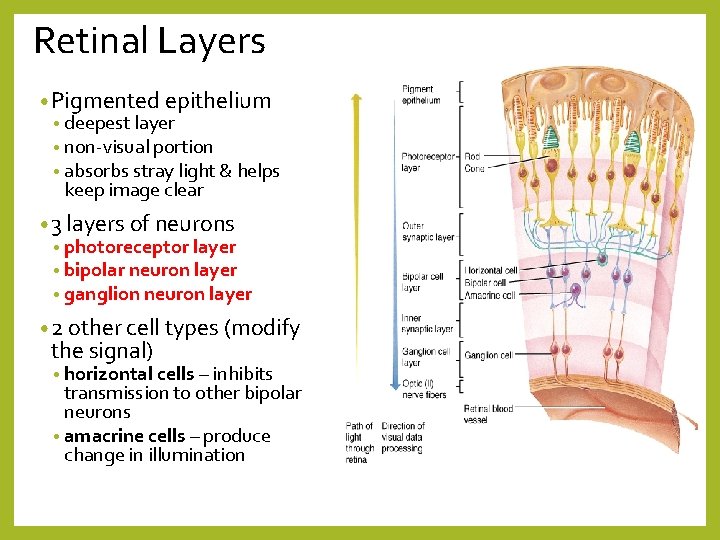
Retinal Layers • Pigmented epithelium • deepest layer • non-visual portion • absorbs stray light & helps keep image clear • 3 layers of neurons • photoreceptor layer • bipolar neuron layer • ganglion neuron layer • 2 other cell types (modify the signal) • horizontal cells – inhibits transmission to other bipolar neurons • amacrine cells – produce change in illumination

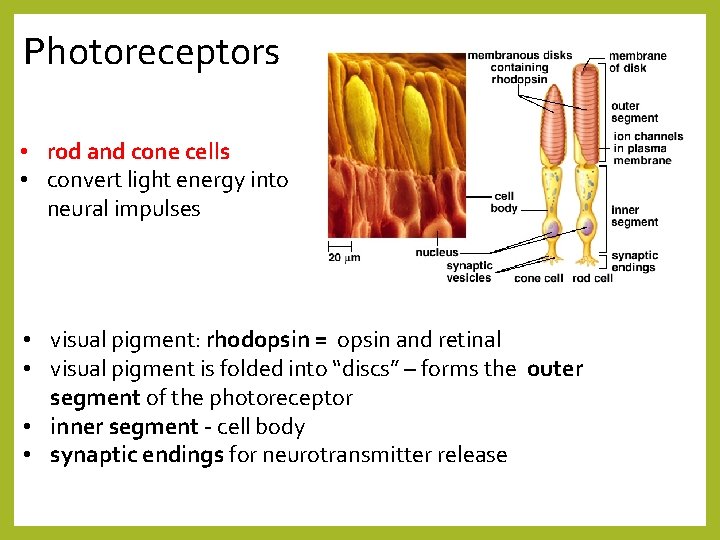
Photoreceptors • rod and cone cells • convert light energy into neural impulses • visual pigment: rhodopsin = opsin and retinal • visual pigment is folded into “discs” – forms the outer segment of the photoreceptor • inner segment - cell body • synaptic endings for neurotransmitter release

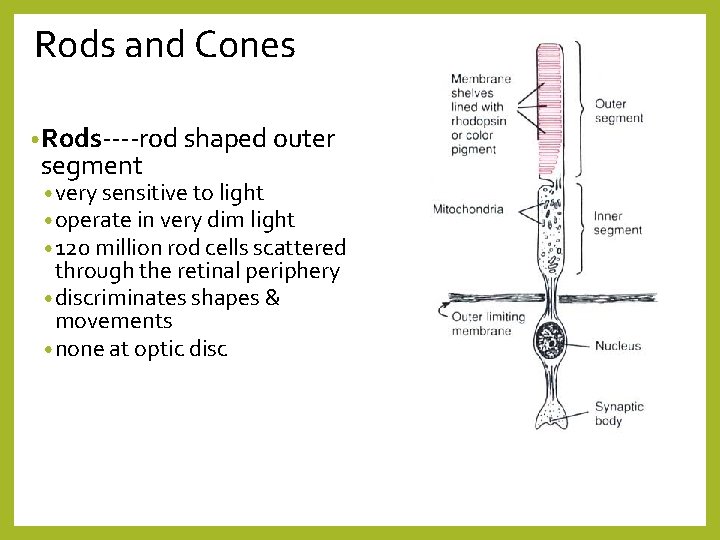
Rods and Cones • Rods----rod shaped outer segment • very sensitive to light • operate in very dim light • 120 million rod cells scattered through the retinal periphery • discriminates shapes & movements • none at optic disc

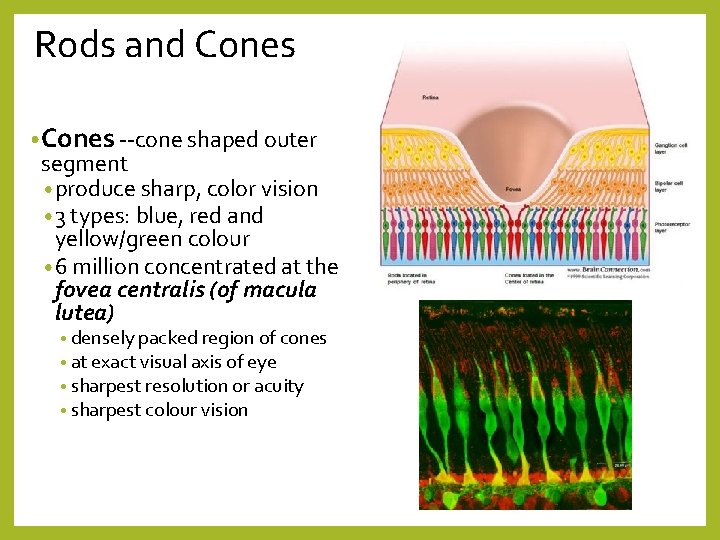
Rods and Cones • Cones --cone shaped outer segment • produce sharp, color vision • 3 types: blue, red and yellow/green colour • 6 million concentrated at the fovea centralis (of macula lutea) • densely packed region of cones • at exact visual axis of eye • sharpest resolution or acuity • sharpest colour vision

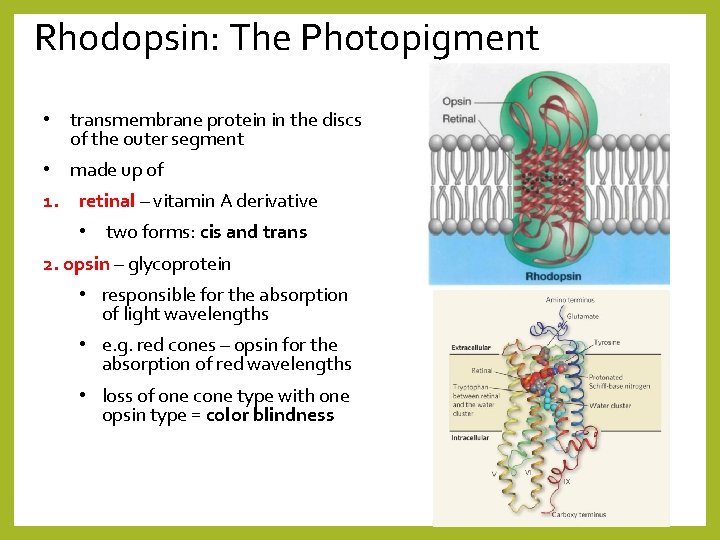
Rhodopsin: The Photopigment • transmembrane protein in the discs of the outer segment • made up of 1. retinal – vitamin A derivative • two forms: cis and trans 2. opsin – glycoprotein • responsible for the absorption of light wavelengths • e. g. red cones – opsin for the absorption of red wavelengths • loss of one cone type with one opsin type = color blindness

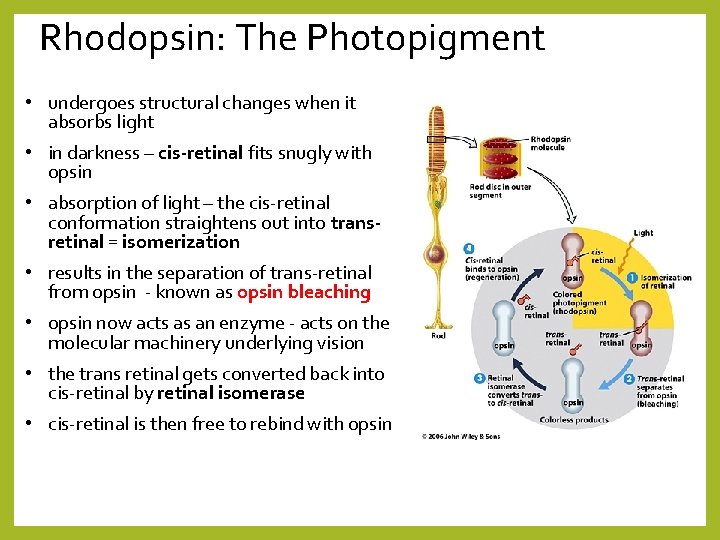
Rhodopsin: The Photopigment • undergoes structural changes when it absorbs light • in darkness – cis-retinal fits snugly with opsin • absorption of light – the cis-retinal conformation straightens out into transretinal = isomerization • results in the separation of trans-retinal from opsin - known as opsin bleaching • opsin now acts as an enzyme - acts on the molecular machinery underlying vision • the trans retinal gets converted back into cis-retinal by retinal isomerase • cis-retinal is then free to rebind with opsin

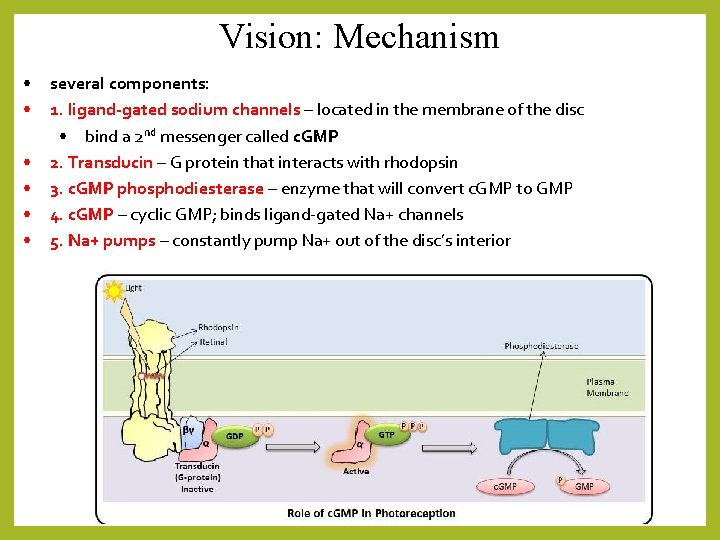
Vision: Mechanism • • • several components: 1. ligand-gated sodium channels – located in the membrane of the disc • bind a 2 nd messenger called c. GMP 2. Transducin – G protein that interacts with rhodopsin 3. c. GMP phosphodiesterase – enzyme that will convert c. GMP to GMP 4. c. GMP – cyclic GMP; binds ligand-gated Na+ channels 5. Na+ pumps – constantly pump Na+ out of the disc’s interior

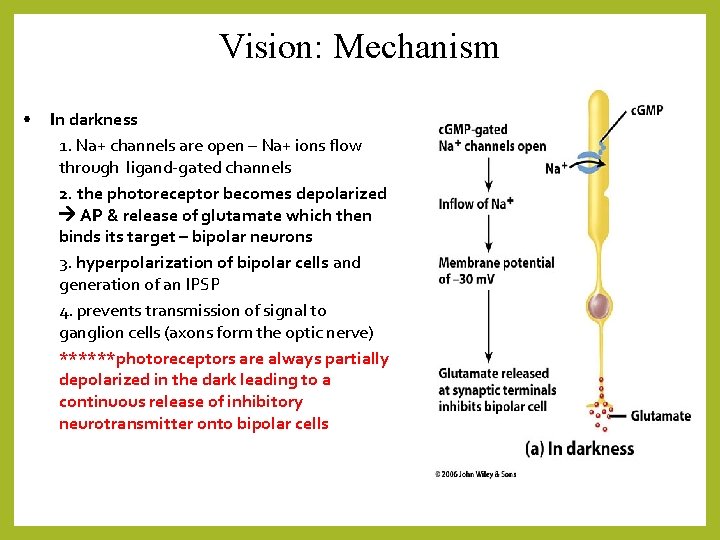
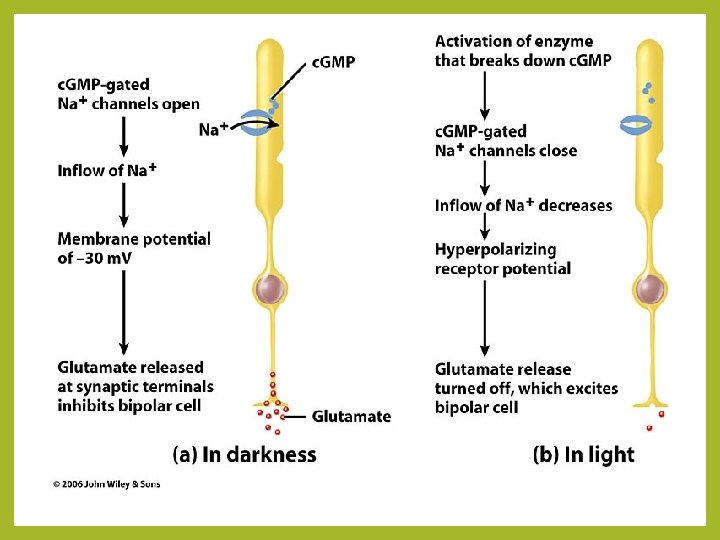
Vision: Mechanism • In darkness 1. Na+ channels are open – Na+ ions flow through ligand-gated channels 2. the photoreceptor becomes depolarized AP & release of glutamate which then binds its target – bipolar neurons 3. hyperpolarization of bipolar cells and generation of an IPSP 4. prevents transmission of signal to ganglion cells (axons form the optic nerve) ******photoreceptors are always partially depolarized in the dark leading to a continuous release of inhibitory neurotransmitter onto bipolar cells

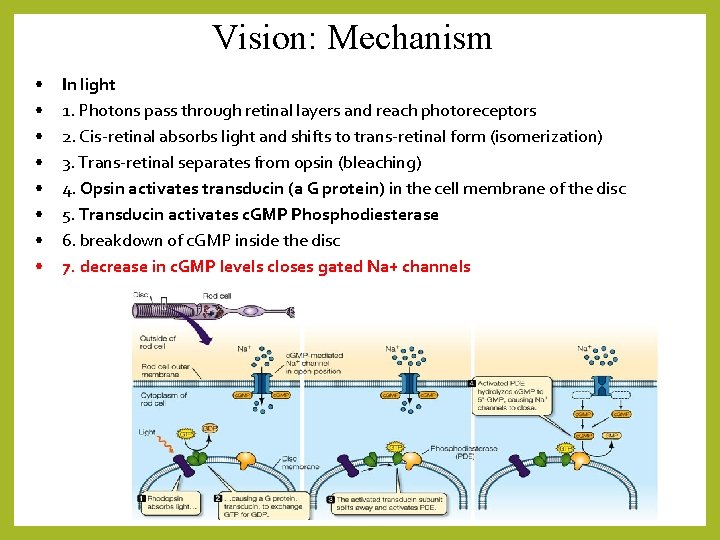
Vision: Mechanism • • In light 1. Photons pass through retinal layers and reach photoreceptors 2. Cis-retinal absorbs light and shifts to trans-retinal form (isomerization) 3. Trans-retinal separates from opsin (bleaching) 4. Opsin activates transducin (a G protein) in the cell membrane of the disc 5. Transducin activates c. GMP Phosphodiesterase 6. breakdown of c. GMP inside the disc 7. decrease in c. GMP levels closes gated Na+ channels

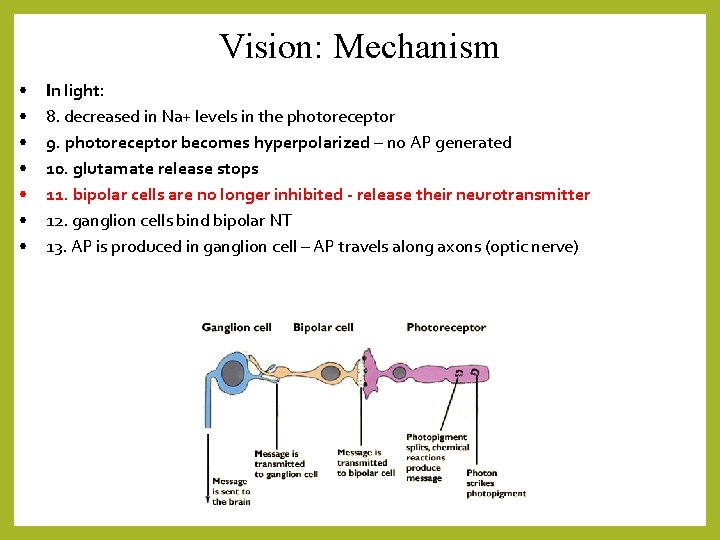
Vision: Mechanism • • In light: 8. decreased in Na+ levels in the photoreceptor 9. photoreceptor becomes hyperpolarized – no AP generated 10. glutamate release stops 11. bipolar cells are no longer inhibited - release their neurotransmitter 12. ganglion cells bind bipolar NT 13. AP is produced in ganglion cell – AP travels along axons (optic nerve)

Vision: Mechanism • once light is removed: • 1. Retinal isomerase shifts trans-retinal back to cis-retinal form • 2. Cis-retinal rebinds with opsin (regeneration) • 3. Transducin is deactivated and Na+ channels are reopened • 4. Na+ begins to flow back into photoreceptor


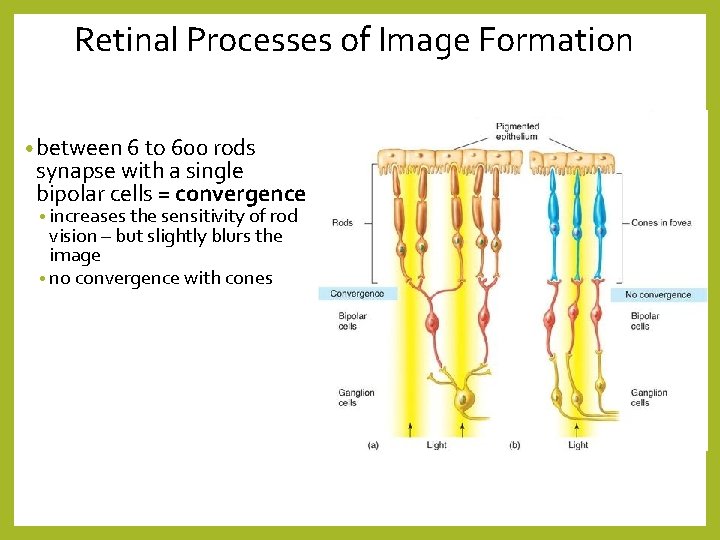
Retinal Processes of Image Formation • between 6 to 600 rods synapse with a single bipolar cells = convergence • increases the sensitivity of rod vision – but slightly blurs the image • no convergence with cones

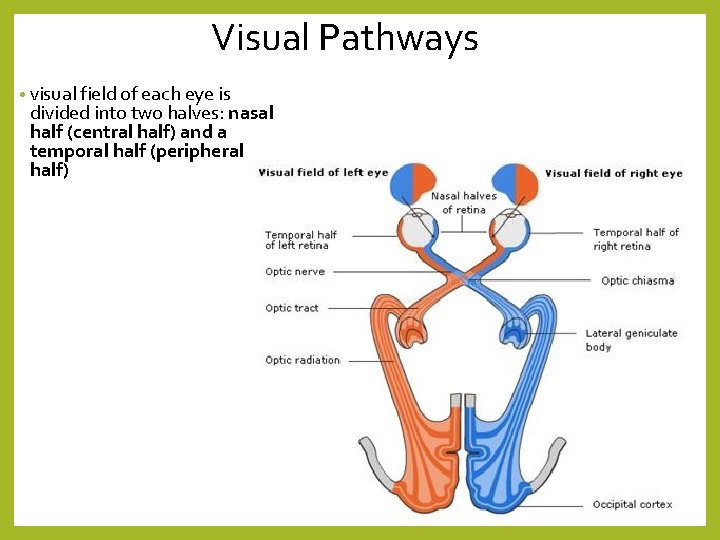
Visual Pathways • visual field of each eye is divided into two halves: nasal half (central half) and a temporal half (peripheral half)

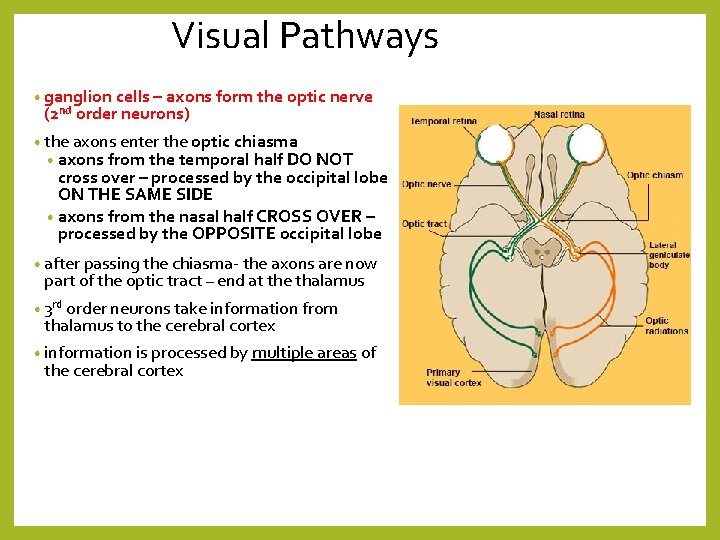
Visual Pathways • ganglion cells – axons form the optic nerve (2 nd order neurons) • the axons enter the optic chiasma • axons from the temporal half DO NOT cross over – processed by the occipital lobe ON THE SAME SIDE • axons from the nasal half CROSS OVER – processed by the OPPOSITE occipital lobe • after passing the chiasma- the axons are now part of the optic tract – end at the thalamus • 3 rd order neurons take information from thalamus to the cerebral cortex • information is processed by multiple areas of the cerebral cortex

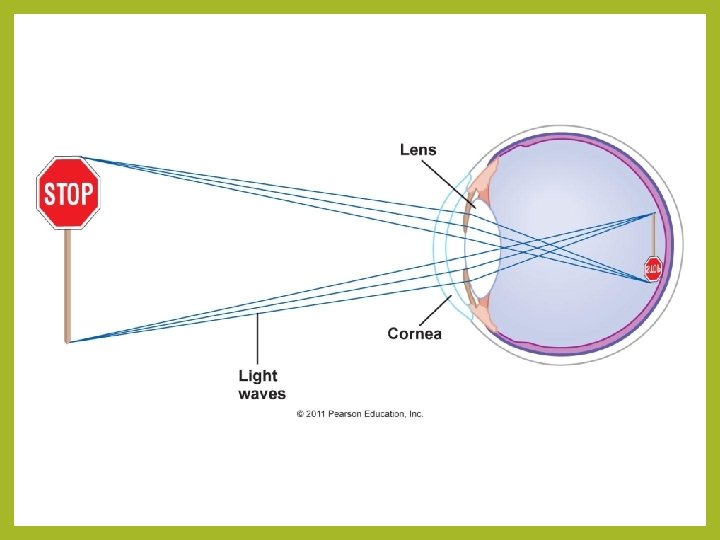
Major Processes of Image Formation • Refraction of light – by cornea & lens – light rays must fall upon the retina • Accommodation of the lens – changing shape of lens so that light is focused • Constriction of the pupil – less light enters the eye

Definition of Refraction • Bending of light as it passes from one substance (air) into a 2 nd substance with a different density(cornea) • In the eye, light is refracted by the anterior & posterior surfaces of the cornea and the lens

Refraction by the Cornea & Lens • Image focused on retina is inverted & reversed from left to right • Brain learns to work with that information • objects at a distance - 75% of Refraction is done by cornea -- rest is done by the lens • light rays from > 20’ are nearly parallel and only need to be bent enough to focus on retina • objects close up - light rays from < 6’ are more divergent & need more refraction – extra process needed to get additional bending of light is called accommodation – done by the lens

Accommodation & the Lens • • Convex lens refracts light rays towards each other Lens of eye is convex on both surfaces View a distant object – use the cornea and a flat lens – lens is nearly flat by pulling of suspensory ligaments – relaxation by ciliary muscles View a close object – use the cornea and a round lens – ciliary muscle contracts & decreases the pull of the suspensory ligaments on the lens – elastic lens thickens as the tension is removed from it – increase in curvature of lens is called accommodation

• Emmetropic eye (normal) – can refract light from 20 ft away • Myopia (nearsighted) – eyeball is too long from front to back – glasses concave • Hypermetropic (farsighted) – eyeball is too short – glasses convex (cokebottle) • Astigmatism – corneal surface wavy – parts of image out of focus

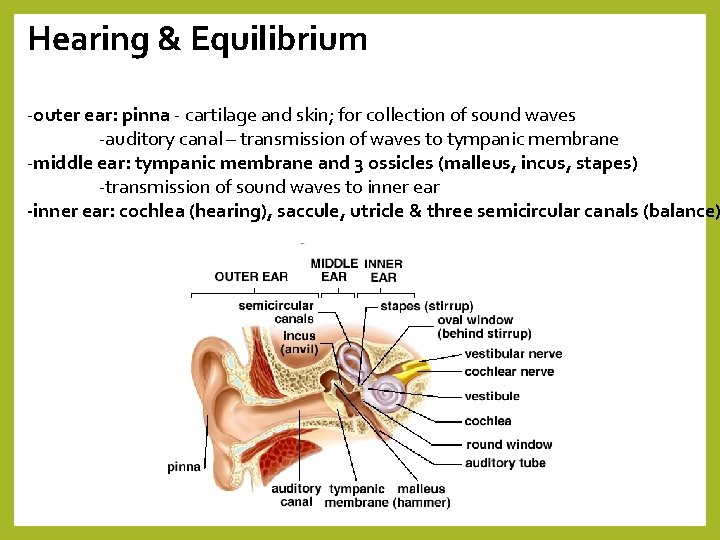
Hearing & Equilibrium -outer ear: pinna - cartilage and skin; for collection of sound waves -auditory canal – transmission of waves to tympanic membrane -middle ear: tympanic membrane and 3 ossicles (malleus, incus, stapes) -transmission of sound waves to inner ear -inner ear: cochlea (hearing), saccule, utricle & three semicircular canals (balance)

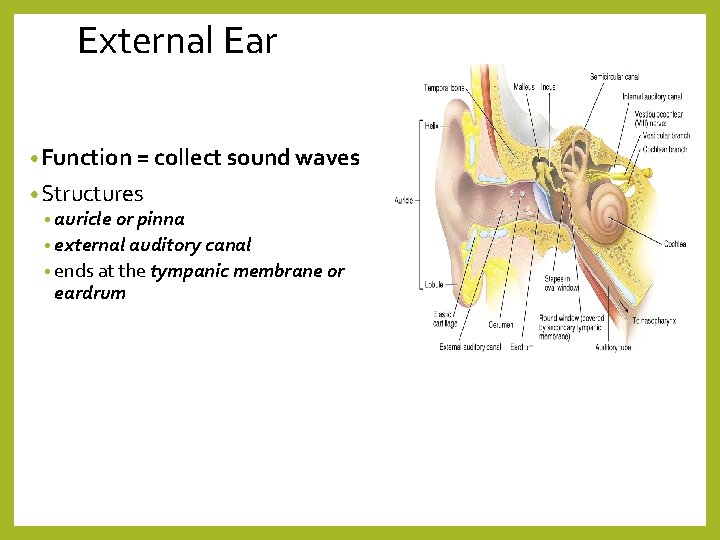
External Ear • Function = collect sound waves • Structures • auricle or pinna • external auditory canal • ends at the tympanic membrane or eardrum

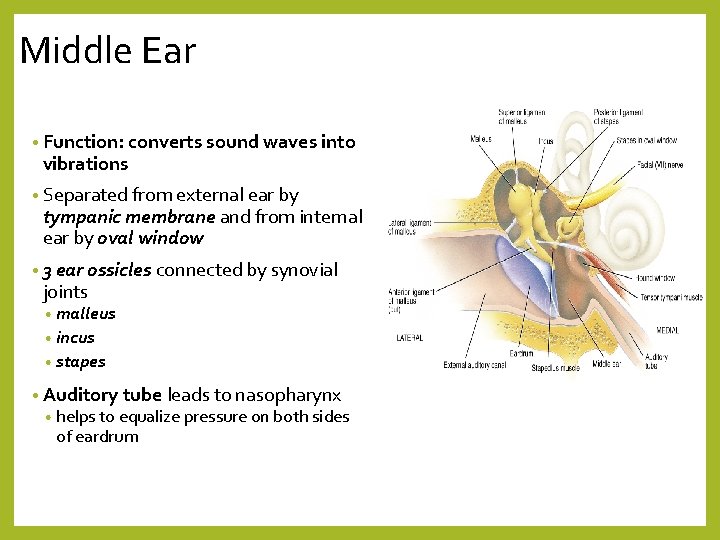
Middle Ear • Function: converts sound waves into vibrations • Separated from external ear by tympanic membrane and from internal ear by oval window • 3 ear ossicles connected by synovial joints • malleus • incus • stapes • Auditory tube leads to nasopharynx • helps to equalize pressure on both sides of eardrum

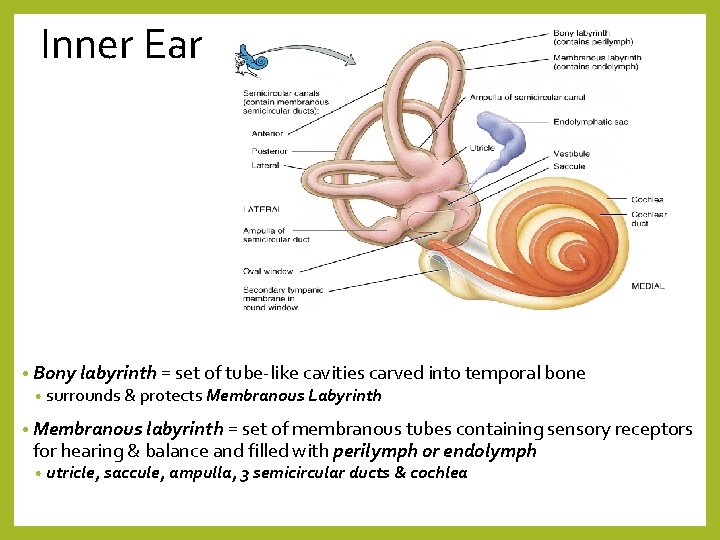
Inner Ear • Bony labyrinth = set of tube-like cavities carved into temporal bone • surrounds & protects Membranous Labyrinth • Membranous labyrinth = set of membranous tubes containing sensory receptors for hearing & balance and filled with perilymph or endolymph • utricle, saccule, ampulla, 3 semicircular ducts & cochlea

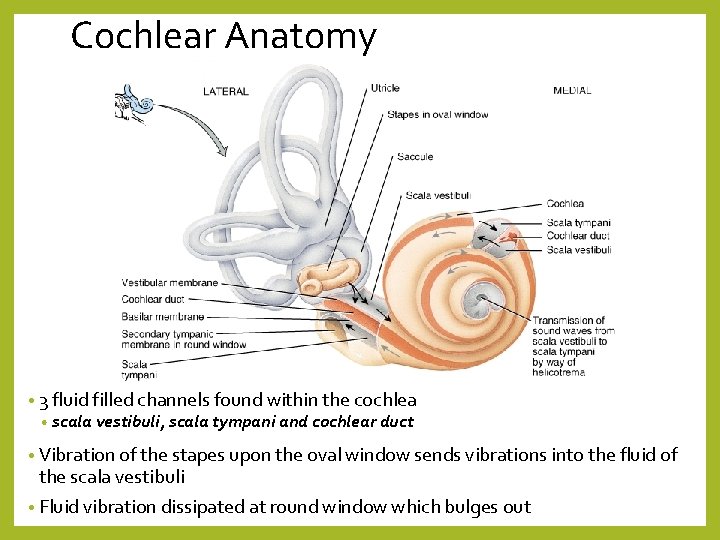
Cochlear Anatomy • 3 fluid filled channels found within the cochlea • scala vestibuli, scala tympani and cochlear duct • Vibration of the stapes upon the oval window sends vibrations into the fluid of the scala vestibuli • Fluid vibration dissipated at round window which bulges out

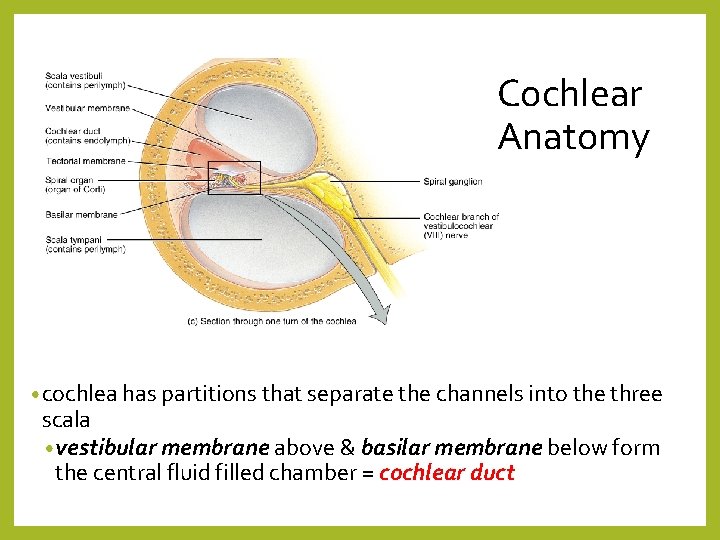
Cochlear Anatomy • cochlea has partitions that separate the channels into the three scala • vestibular membrane above & basilar membrane below form the central fluid filled chamber = cochlear duct

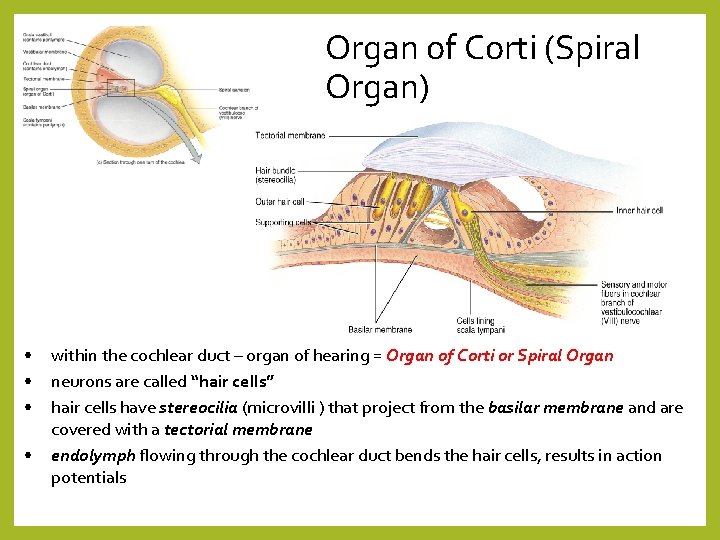
Organ of Corti (Spiral Organ) • • within the cochlear duct – organ of hearing = Organ of Corti or Spiral Organ neurons are called “hair cells” hair cells have stereocilia (microvilli ) that project from the basilar membrane and are covered with a tectorial membrane endolymph flowing through the cochlear duct bends the hair cells, results in action potentials

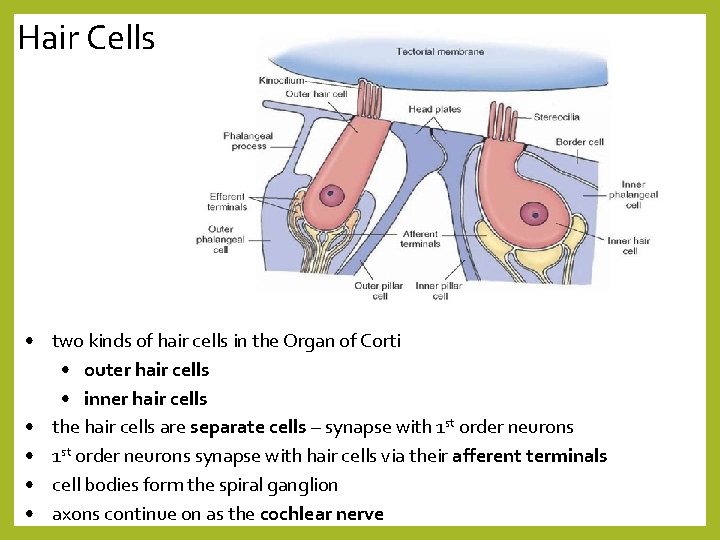
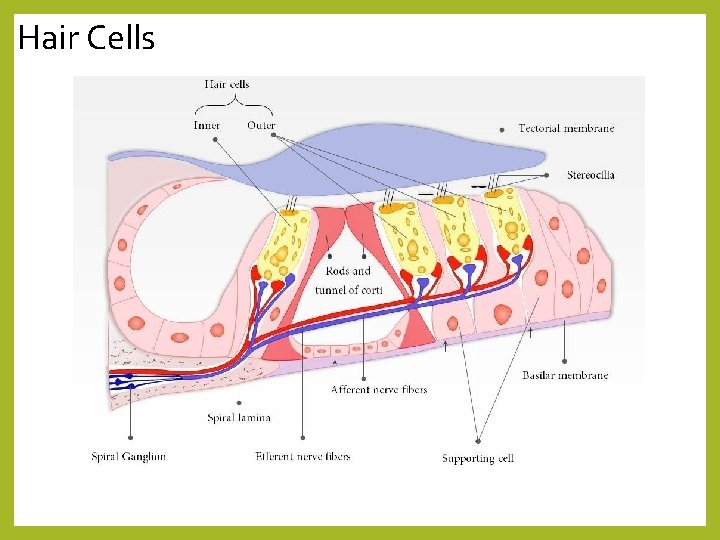
Hair Cells • two kinds of hair cells in the Organ of Corti • outer hair cells • inner hair cells • the hair cells are separate cells – synapse with 1 st order neurons • 1 st order neurons synapse with hair cells via their afferent terminals • cell bodies form the spiral ganglion • axons continue on as the cochlear nerve

Hair Cells

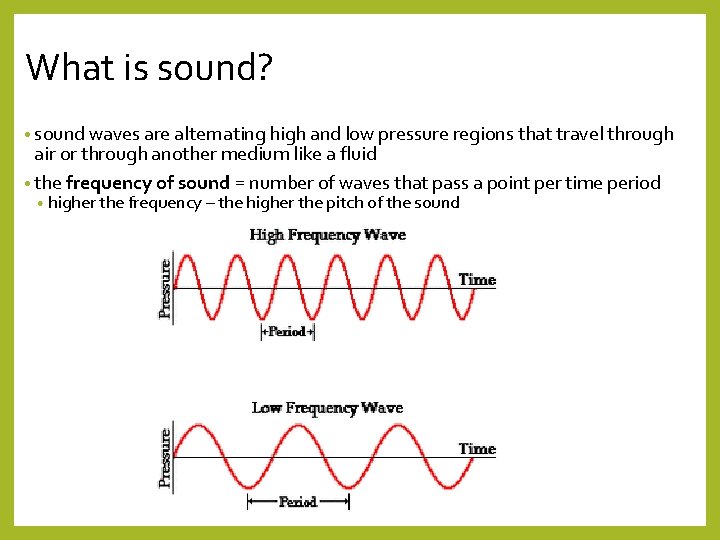
What is sound? • sound waves are alternating high and low pressure regions that travel through air or through another medium like a fluid • the frequency of sound = number of waves that pass a point per time period • higher the frequency – the higher the pitch of the sound

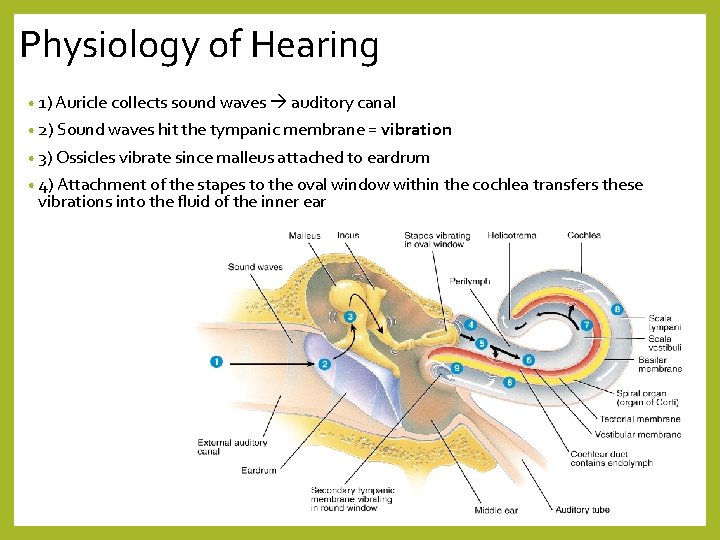
Physiology of Hearing • 1) Auricle collects sound waves auditory canal • 2) Sound waves hit the tympanic membrane = vibration • 3) Ossicles vibrate since malleus attached to eardrum • 4) Attachment of the stapes to the oval window within the cochlea transfers these vibrations into the fluid of the inner ear

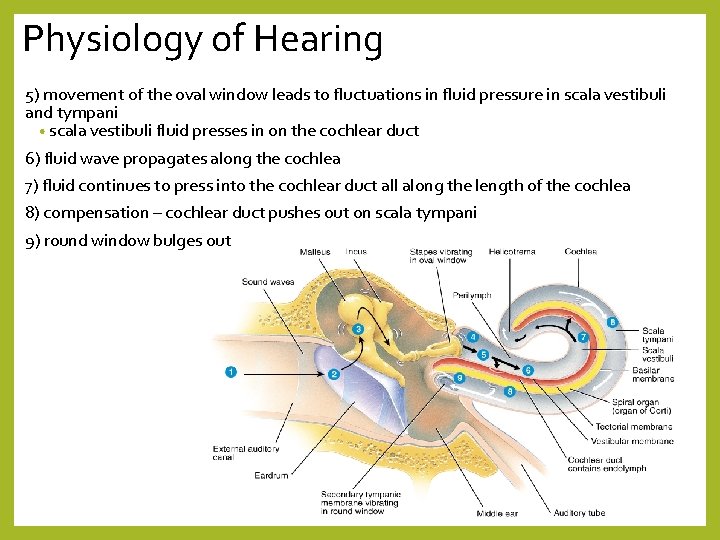
Physiology of Hearing 5) movement of the oval window leads to fluctuations in fluid pressure in scala vestibuli and tympani • scala vestibuli fluid presses in on the cochlear duct 6) fluid wave propagates along the cochlea 7) fluid continues to press into the cochlear duct all along the length of the cochlea 8) compensation – cochlear duct pushes out on scala tympani 9) round window bulges out

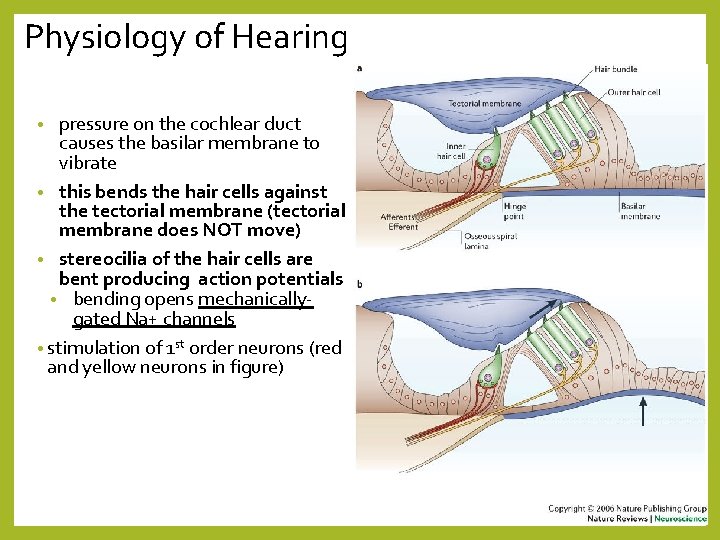
Physiology of Hearing pressure on the cochlear duct causes the basilar membrane to vibrate • this bends the hair cells against the tectorial membrane (tectorial membrane does NOT move) • stereocilia of the hair cells are bent producing action potentials • bending opens mechanicallygated Na+ channels • stimulation of 1 st order neurons (red and yellow neurons in figure) •

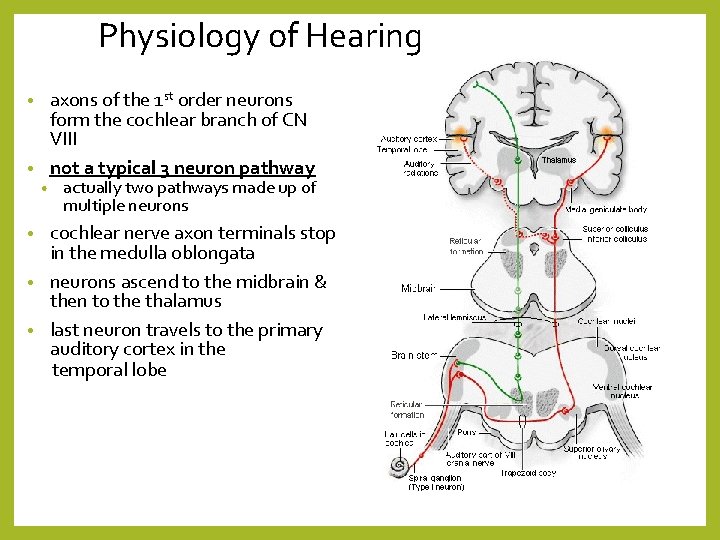
Physiology of Hearing axons of the 1 st order neurons form the cochlear branch of CN VIII • not a typical 3 neuron pathway • • actually two pathways made up of multiple neurons cochlear nerve axon terminals stop in the medulla oblongata • neurons ascend to the midbrain & then to the thalamus • last neuron travels to the primary auditory cortex in the temporal lobe •

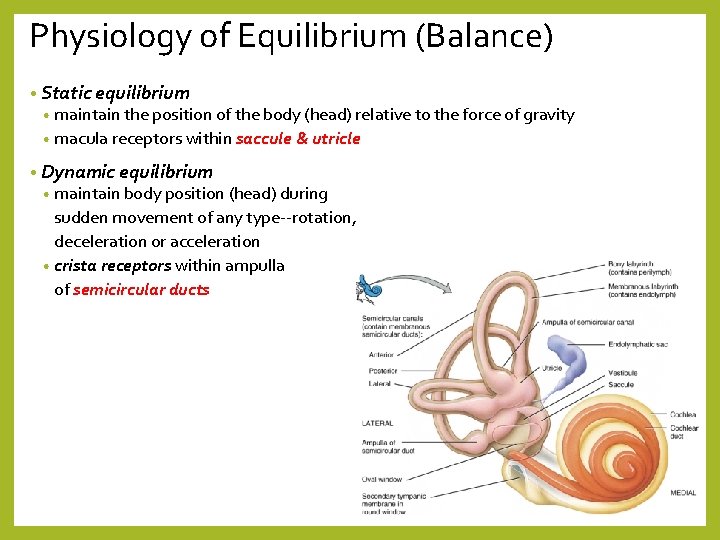
Physiology of Equilibrium (Balance) • Static equilibrium • maintain the position of the body (head) relative to the force of gravity • macula receptors within saccule & utricle • Dynamic equilibrium • maintain body position (head) during sudden movement of any type--rotation, deceleration or acceleration • crista receptors within ampulla of semicircular ducts

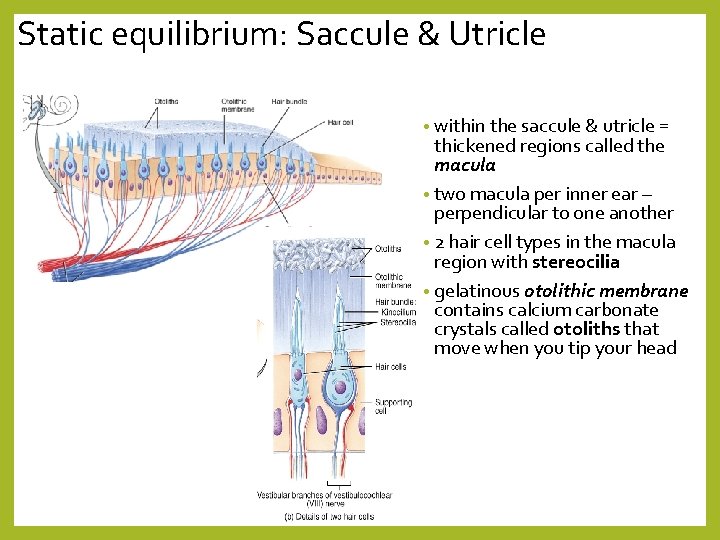
Static equilibrium: Saccule & Utricle • within the saccule & utricle = thickened regions called the macula • two macula per inner ear – perpendicular to one another • 2 hair cell types in the macula region with stereocilia • gelatinous otolithic membrane contains calcium carbonate crystals called otoliths that move when you tip your head

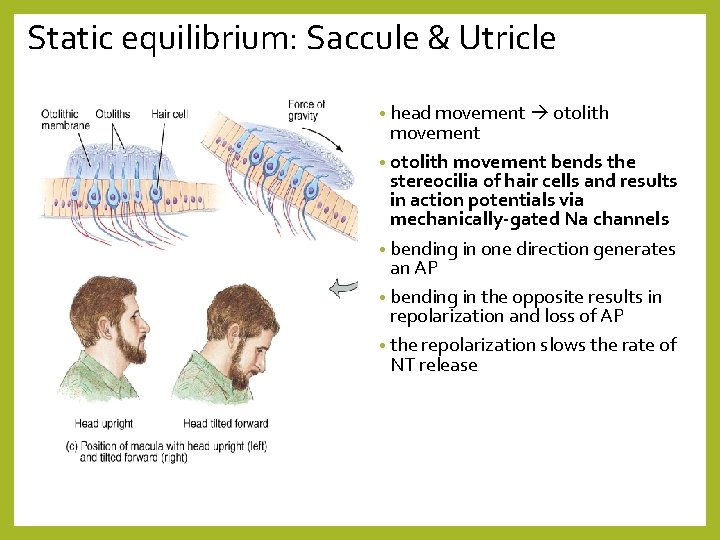
Static equilibrium: Saccule & Utricle • head movement otolith movement • otolith movement bends the stereocilia of hair cells and results in action potentials via mechanically-gated Na channels • bending in one direction generates an AP • bending in the opposite results in repolarization and loss of AP • the repolarization slows the rate of NT release

Static equilibrium: Saccule & Utricle • hair cells synapse with first order neurons – axons form the vestibular nerve/branch of cranial nerve VIII • depolarization -> faster NT release and faster nerve impulses through VIII • repolarization -> slower NT release and slower nerve impulse through VIII

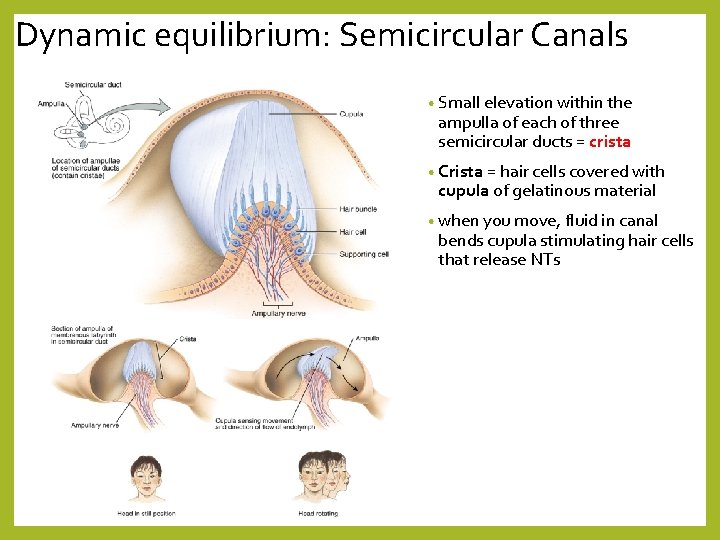
Dynamic equilibrium: Semicircular Canals • Small elevation within the ampulla of each of three semicircular ducts = crista • Crista = hair cells covered with cupula of gelatinous material • when you move, fluid in canal bends cupula stimulating hair cells that release NTs

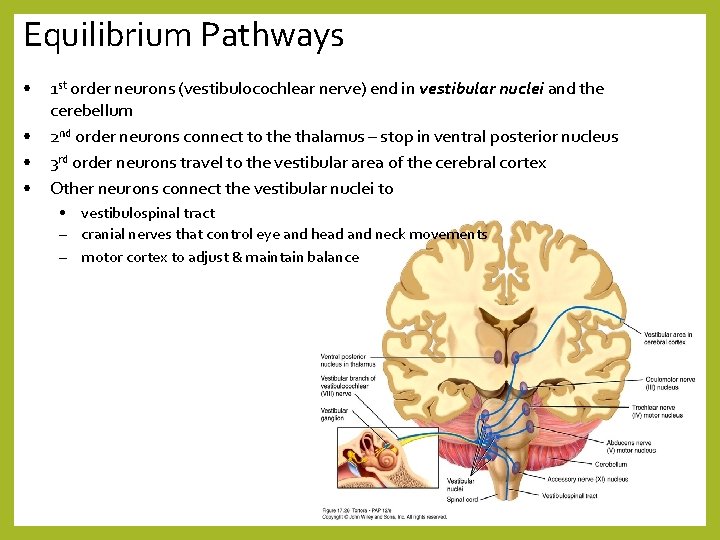
Equilibrium Pathways • • 1 st order neurons (vestibulocochlear nerve) end in vestibular nuclei and the cerebellum 2 nd order neurons connect to the thalamus – stop in ventral posterior nucleus 3 rd order neurons travel to the vestibular area of the cerebral cortex Other neurons connect the vestibular nuclei to • vestibulospinal tract – cranial nerves that control eye and head and neck movements – motor cortex to adjust & maintain balance