The Placenta and Fetal Membranes Fetal Tissues of

The Placenta and Fetal Membranes

Fetal Tissues of the Fetal-Maternal Communication System The extravillous and villous traphoblasts Placental arm The fetal membranes (the amnion-chorion leave) Paracrine arm Human placenta : hemochorioendothelial type
Discoid Placenta in Humans
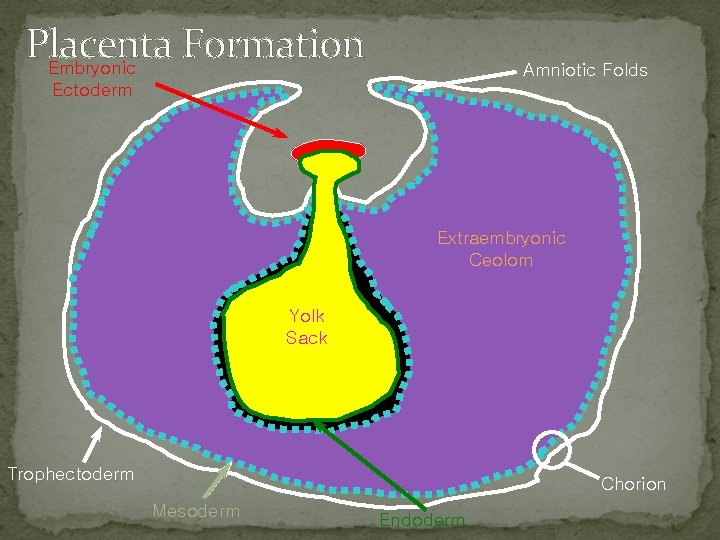
Placenta Formation Embryonic Amniotic Folds Ectoderm Extraembryonic Ceolom Yolk Sack Trophectoderm Chorion Mesoderm Endoderm

Placental Membranes Yolk Sack In birds to nourish embryo In mammal atrophies but source of blood cells and primordial germ cells Amnion Non-vascular, fluid filled Fluid produced by fetus Protective cushion Ruptures at birth (not breaking of water)

Placental Membranes (cont. ) Allantois Blood vessels Fuses with chorion Allantochorion or chorioallantois Brings blood vessels to chorion Chorion Outermost membrane Attachment to mother
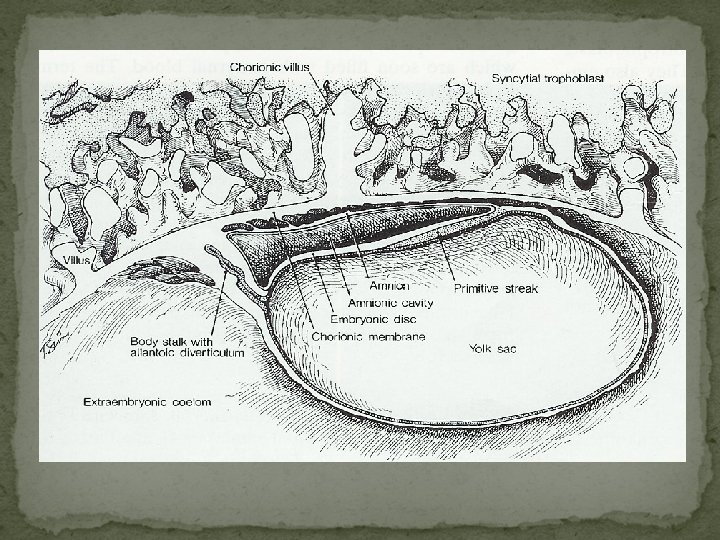
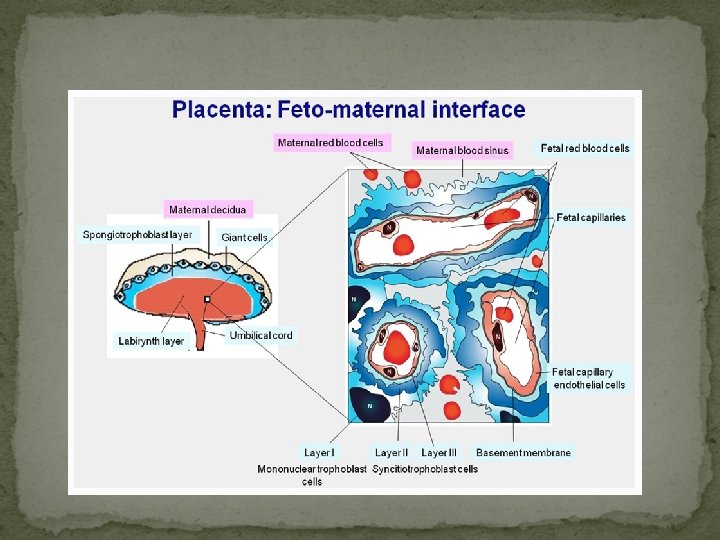
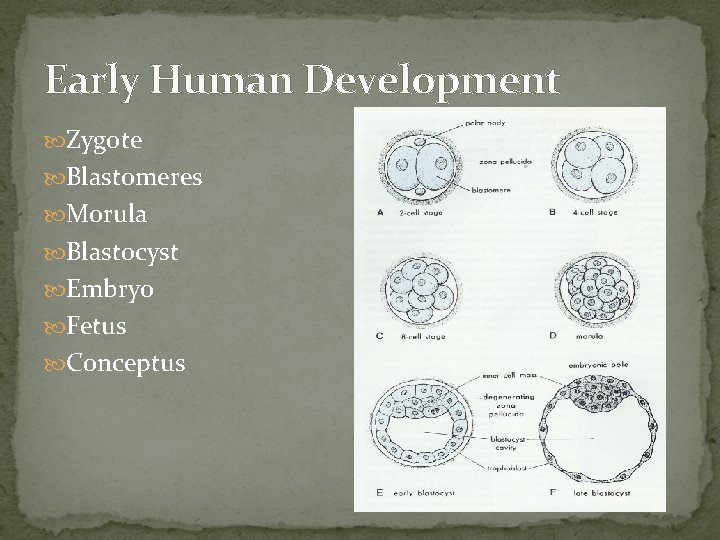
Early Human Development Zygote Blastomeres Morula Blastocyst Embryo Fetus Conceptus
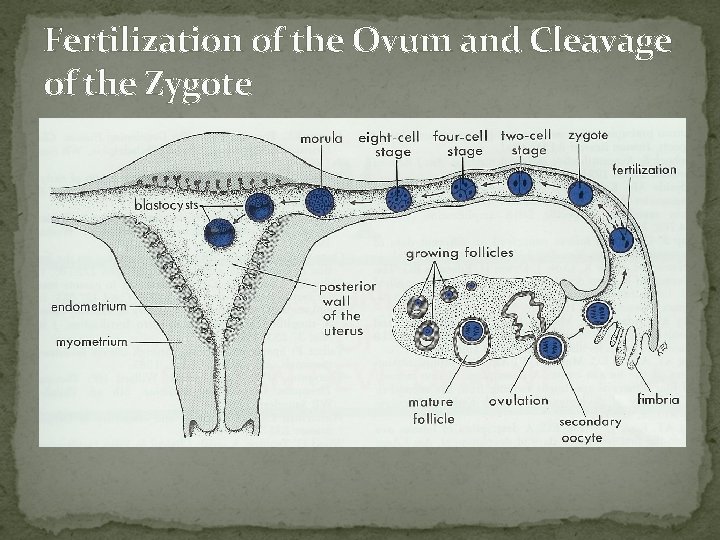
Fertilization of the Ovum and Cleavage of the Zygote Moore, fig 3 -5
58 -cell blastocyst 107 -cell blastocyst Fig 5 -1
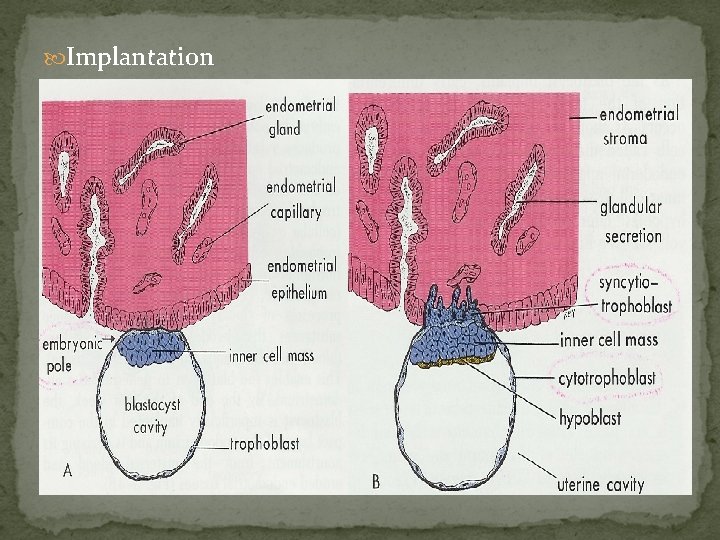
Implantation Moore, fig 3 -4

Biology of trophoblast Trophoblast is the most variable in structure, function and development invasiveness provides for attatchment of blastocyst to decidua of uterine cavity nutrition of the conceptus function as endocrine organ in human pregnancy essential to maternal physiological adaptations & maintenance of pregnancy
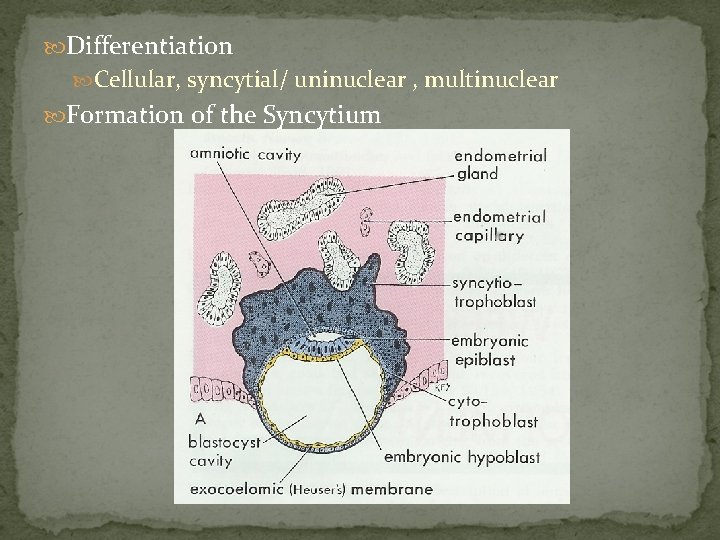
Differentiation Cellular, syncytial/ uninuclear , multinuclear Formation of the Syncytium

Cytotrophoblasts are the cellular progenitors of the syncytiotrophoblast Cytotrophoblast Syncytiotrophoblast Morphologically uninuclear cells multinuclear giant cells cell boders well demarcated lacking single, distinct multiple & diverse present absent germinal cell cytotrophoblast nucleus miotic figure Origin

after apposition & adherence, intrusion of cytotrophoblast between endometrial epithelial cells this process is facilitated by degradation of the extracellula matrix of endometrium /decidua catalyzed by urokinase-type plasminogen activator urokinase plasminogen activator receptor multiple metalloproteinase These functions of cytotrophoblasts invading the endometrium are indistinguishable from those of metastasizing malignant cells

Immunological Acceptance of the Conceptus Previous Theories antigenic immaturity of the embryo-fetus diminished immunological responsiveness of the pregnant woman Decidua : immunologically privileged tissue site The acceptance and the survival of conceptus in the maternal uterus must be attributed to immunological peculiarity of the trophoblasts, not the decidua

Current Status of Research Expression of the HLA system in trophoblast unique set of lymphocytes > may provide explanation for immunological acceptance of the conceptus trophoblast HLA expression (monomorphic HLA-G class I) uterine large granular lymphocyte (LGL)

Immunocompetency of the Trophoblasts Many researchers focused on the expression of the major histocompatibility complex (MHC) antigens in trophoblast MHC class II antigens are absent from trophoblasts at all stages of gestation

Trophoblast HLA Class I Expression Normal implantation is dependent upon controlled trophoblast invasion of maternal endometrium/decidua and the spiral arteries a mechanism for permitting and then for limitting trophoblast invasion Such a system involves the uterine large granular lymphocytes(LGSs) and the unique expression of specific nomomeric HLA class I antigens in the trophoblasts

HLA-I Gene Expression HLA genes the products of multiple genetic loci of the MHC within short arm of chromosome 6 17 class I genes have been identified three classical genes A, B, C => major class I(a) transplantation antigens three other class I(b) genes E, F, G => class I HLA antigen HLA-G gene

Uterine Large Granular Lymphocyte (LGL) Believed to be lymphoid and of bone marrow origin and natural killer cell lineage. Present in large numbers only at the midluteal phase of the cycle-at the expected time of implantation in the human endometrium. Near the end of luteal phase of nonfertile ovulatory cycles, the nuclei of LGLs begin to disintegrate. With blastocyst implantation, these cells persist in the decidua during the early weeks of pregnancy. speculated that LGLs are involved in the regulation of trophoblast invasion.

HLA-G Expression in Human Trophoblasts HLA-G antigen identified only in extravillous cytotrophoblast in decidua basails and chorion laeve not present in villous trophoblast, either in syncytium or in cytotrophoblasts. expressed in cytotrophoblast that are contiguous with maternal tissue (decidual cell) It is hopothesized that HLA-G is immunologically permissive of antigen mismatch between mother and fetus.

HLA Expression in the Human Embryo as gestation progresses, cells from inner cell mass of blastocyst gradually develop both class I and II HLA antigen these tissuee are not in direct contact with maternal tissue or blood

Implantation and Integrin Switching Apposition, adherence, then intrusion and invasion of the endometrium/decidua by cytotrophoblast(implantation) appears to be dependent upon trophoblast elaboration of specific proteinases degrade selected extracellular matrix proteins of the endometrium/decidua coordinated and alternating process referred to as "integrin switching“ facilitates migration and then attachment of trophoblasts in the decidua

Integrin one of four families of cell adhesion molecules (CAMs) cell-surface receptors that mediate the adhesion of cells to extracellular matrix proteins

Trophoblast Attachment in Decidua: Oncofetal Fibronectin onf. FN(oncofetal fibronectin) unique glycopeptide of the trophouteronectin molecule trophouteronectin or trophoblast glue formed by extravillous trophoblast, including those of chorion laeve Function a critical role for migration and attachment of the trophoblasts to maternal decidua facilitates separation of extraembryonic tissues from the uterus at delivery

Embryonic and Placental Development Early Blastocyst Trophoblast h. CG Grow & expand
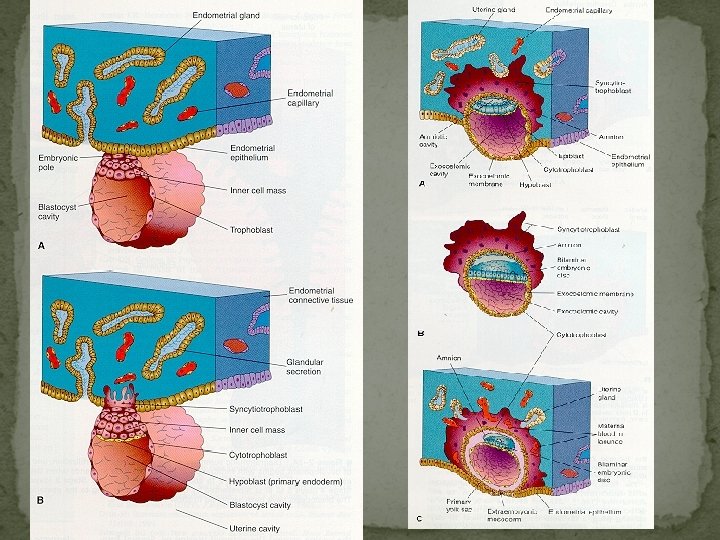
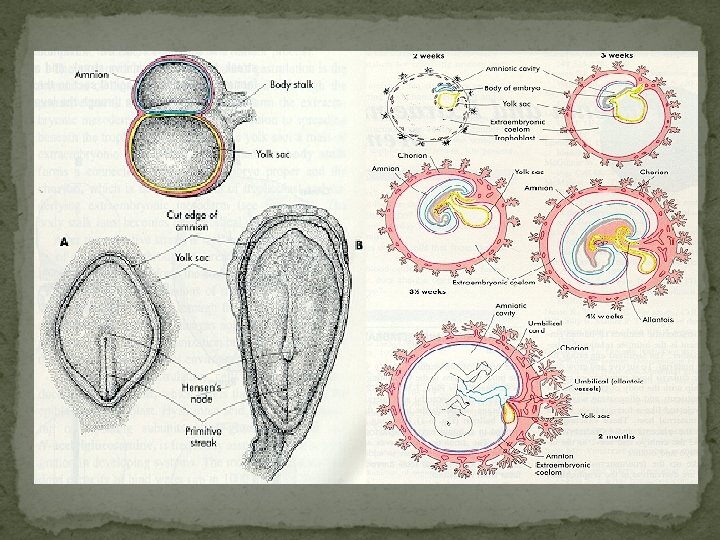
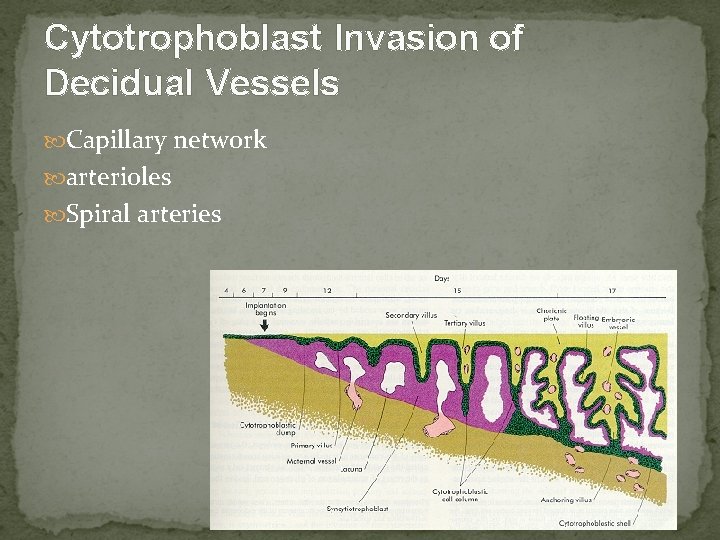
Cytotrophoblast Invasion of Decidual Vessels Capillary network arterioles Spiral arteries
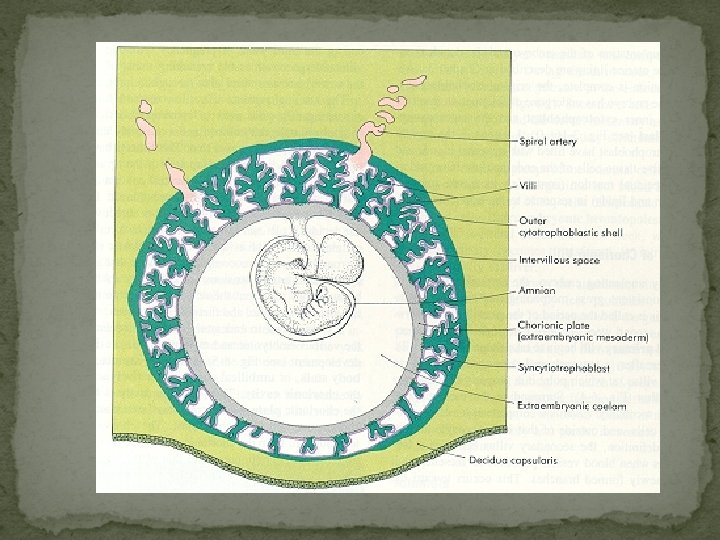
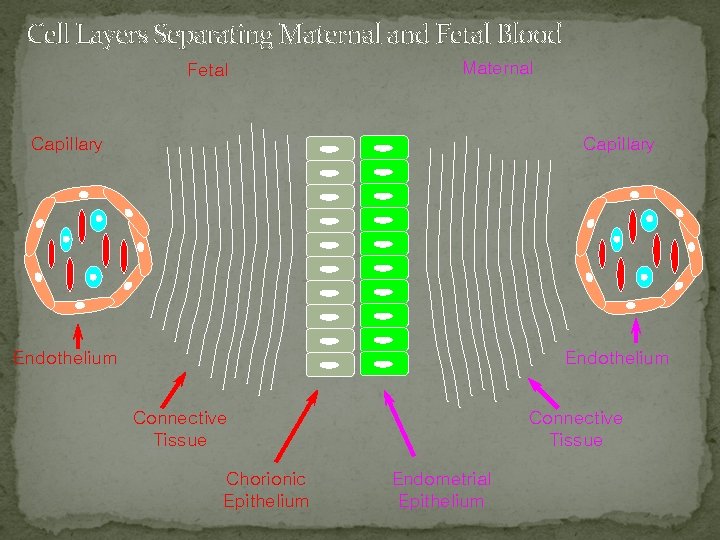
Cell Layers Separating Maternal and Fetal Blood Fetal Maternal Capillary Endothelium Connective Tissue Chorionic Epithelium Connective Tissue Endometrial Epithelium

Histological Classification Tissues syndesmochorial endothelialchorial Maternal endothelium + conn. tissue + epithelium + + + - - - Fetal epithelium + conn. tissue + endothelium + + + *ruminant dog cat human rat rabbit Species epithelialchorial pig horse ruminant hemochorial endothelial

Several curious features trophoblasts in the vessels lumen do not appear to replicate these cells are not readily dislodged by flow of blood these cytotrophoblast appear to migrate against arterial flow and pressure no obvious adhesion of these cells one to the other invasion of maternal vascular tissue bt trophoblasts involves only the decidual spiral arteries, not the veins
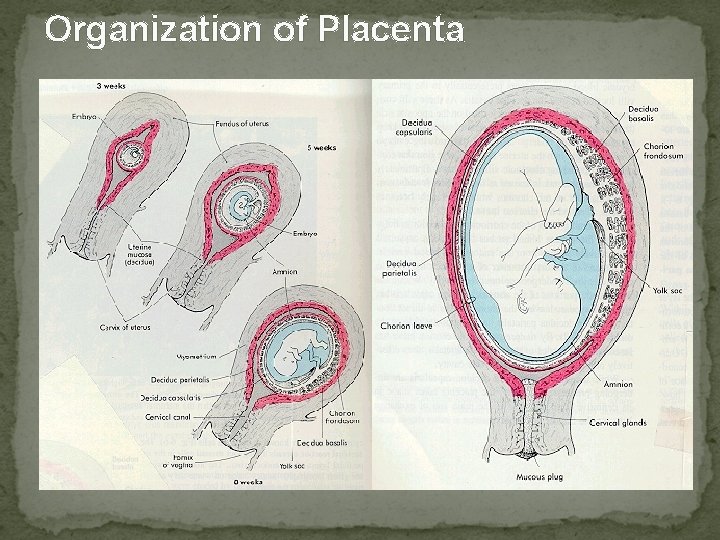
Organization of Placenta

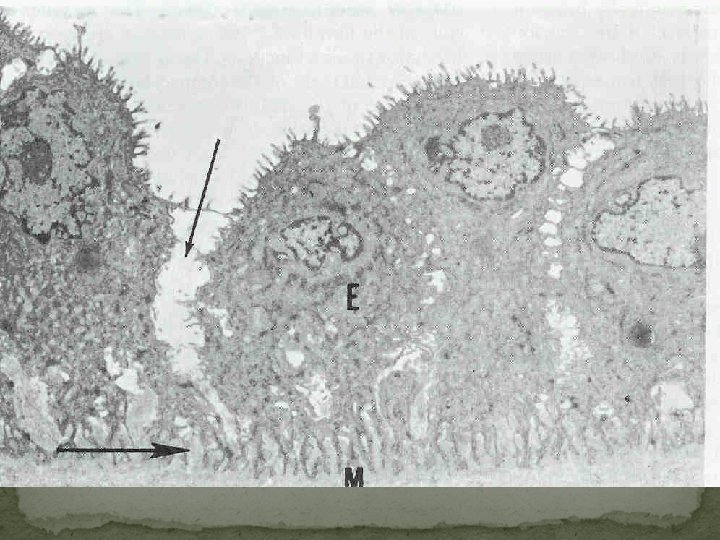
Trophoblast Ultrastructure Prominent microvilli of the syncytial surface (brush border) pinocytotic vacuoles and vesicles absorptive and secretory placental function

Chorionic Villi 12 th day Primary villi proliferation of cytotrophoblast extend into syncytiotrophoblast Secondary villi mesenchymal cord, derived from cytotrophoblast, invade solid trophoblast column Tertiary villi after angiogenesis occurs from the mesenchymal cores in situ 17 th day에 fetal blood vessels are functional & placental circulation이 establish됨.
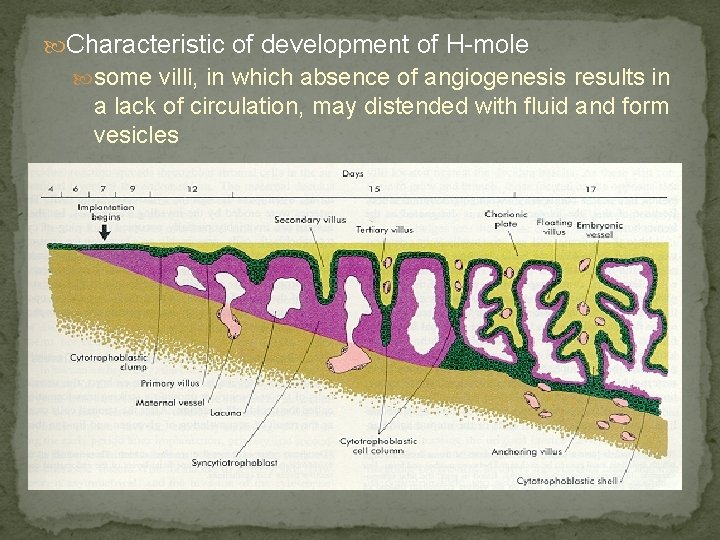
Characteristic of development of H-mole some villi, in which absence of angiogenesis results in a lack of circulation, may distended with fluid and form vesicles

Placental Cotyledons Certain villi of the chorion frondosum extend from chorionic plate to the decidua and serve as anchoring villi Each of the main stem villi(truncal) and their ramifications (rami) constitute a placental cotyledon (lobe) For each cotyledon, a 1: 1: 1 ratio of artery to vein to cotyledon
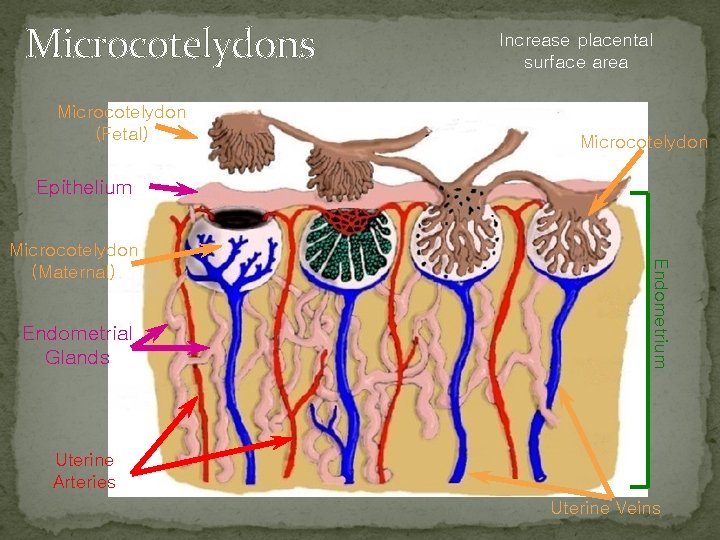
Microcotelydons Microcotelydon (Fetal) Increase placental surface area Microcotelydon Epithelium Endometrial Glands Endometrium Microcotelydon (Maternal) Uterine Arteries Uterine Veins

Breaks in the Placental " Barrier“ Numerous findings of passage of cells between mother and fetus in both directions ex) erythroblastosis fetalis A few fetal blood cells are found in the mother's blood Fetal leukocytes may replicate in the mother and leukocyte s bearing a Y chromosome have been identified in women for up to 5 years after giving birth to a son
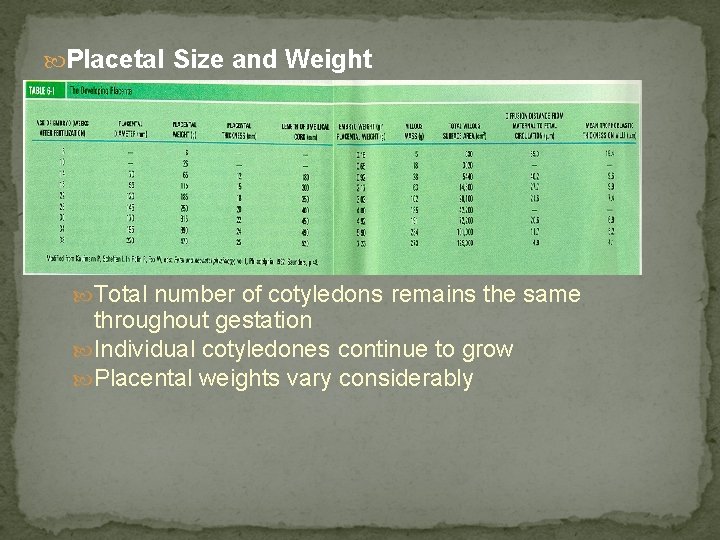
Placetal Size and Weight Total number of cotyledons remains the same throughout gestation Individual cotyledones continue to grow Placental weights vary considerably

Placental Aging As villi continue to branch and terminal ramifications become more numerous and smaller > volume and prominence of cytotrophoblasts decrease As syncytium thins and forms knots > vessels become more prominent and lie closer to the surface The stroma of the villi in early pregnancy branching connective ts. cells are seperated by abundant loose intercellular matrix later stroma becomes denser, and the cells more spindly and more closely packed

Histologic changes that accompany placental growth and aging are suggestive of increase in the efficiency of transport to and exchange to meet increasing fetal metabolic requirements decrease in thickness of the syncytium partial reduction of cytotropholastic cell decrease in the stroma increase in the number of capillaries and approximation of these vessels to the syncytial surface By 4 months the apparent continuity of the cytotrophoblast is broken the syncytium forms knots on the more numerous, smaller villi

At term Covering of villi may be focally reduced to a thin layer of syncytium with minimal connective tissue Fetal capillaries seem to abut the tropohoblast Villous stroma, Hofbauer cells, and cytotrophoblasts are markedly reduced villi appear filled with thin-walled capillaries Other changes suggestive of a decrease in the efficiency for placental exchange thickening of the basement membrane of trophoblast capillaries obliteration of certain fetal vessels fibrin deposition on the surface of villi in basal and chorionic plates as well as elsewhere in the intervillous space
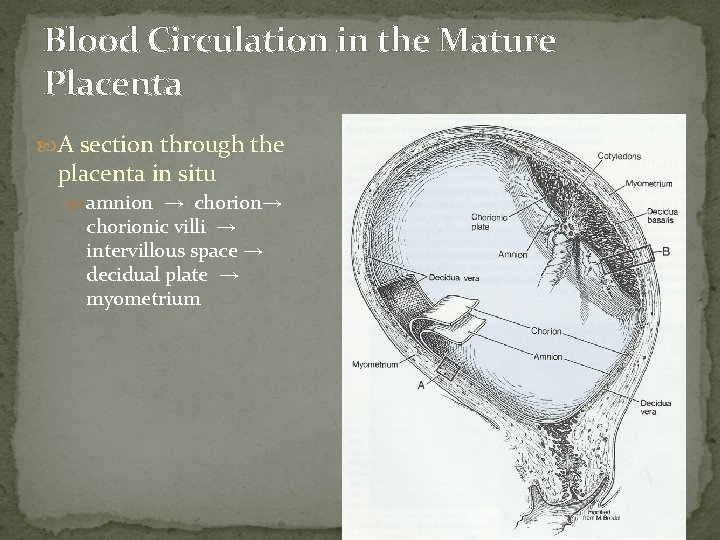
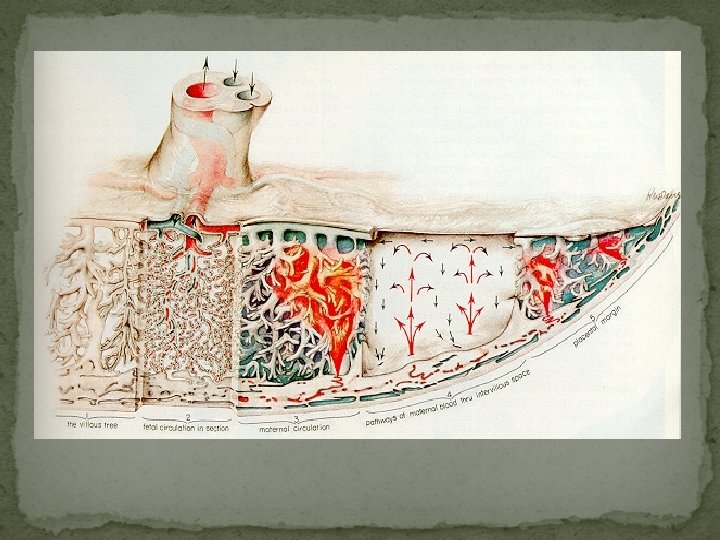
Blood Circulation in the Mature Placenta A section through the placenta in situ amnion → chorionic villi → intervillous space → decidual plate → myometrium
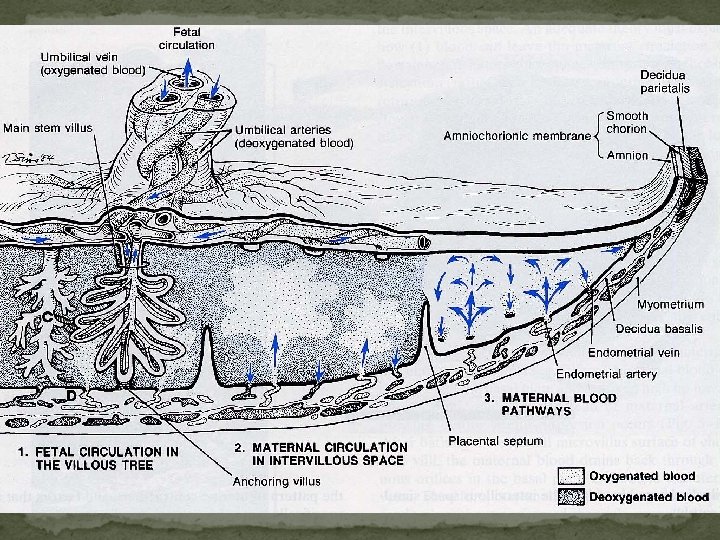

Fetal Circulation 2 umbilical arteries deoxygenated, or "venous-like" blood flows to the placenta 1 umbilical vein with a significantly higher oxygen content Hyrtl anastomosis Two umbilical a. separate at the chorionic plate to supply branches to the cotyledons

Maternal Circulation Intervillous space -> chorionic plate -> vein Spiral a. , vein Ut. Contraction vein Intervillous space Ramsey's concept

The principle factors regulating the flow of blood in the intervillous space arterial blood pressure intrauterine pressure pattern of uterine contraction factors that act specifically upon the arteriolar walls

The Amnion Innermost fetal membrane and is contiguous with amnionic fluid Avascular structure Provide almost all of the tensile strength of the fetal membranes protect against rupture or tearing

Structure single layer of cuboidal epithelial cells basement membrane acellular compact layer fibroblast-like mesenchymal cells zona spongiosa Missing element of human amnion smooth muscle cell, nerves, lymphatics, blood vessels
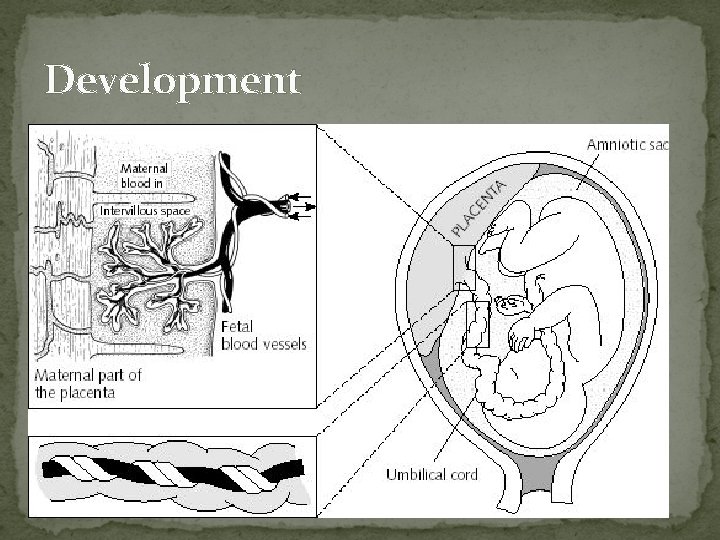
Development
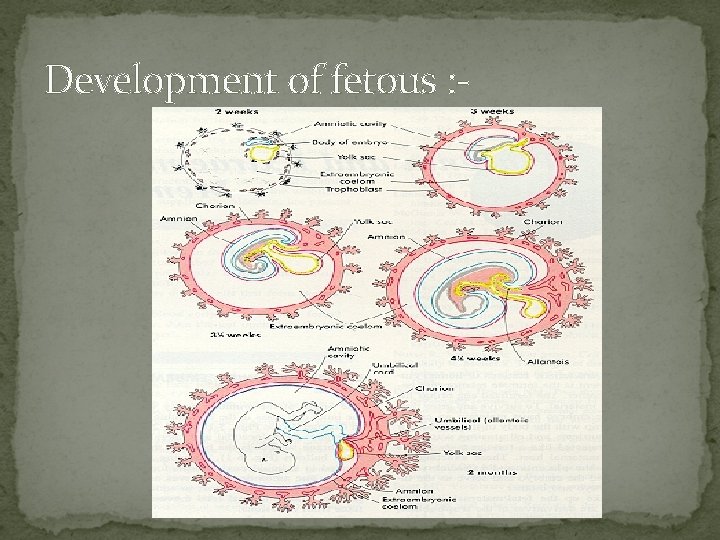
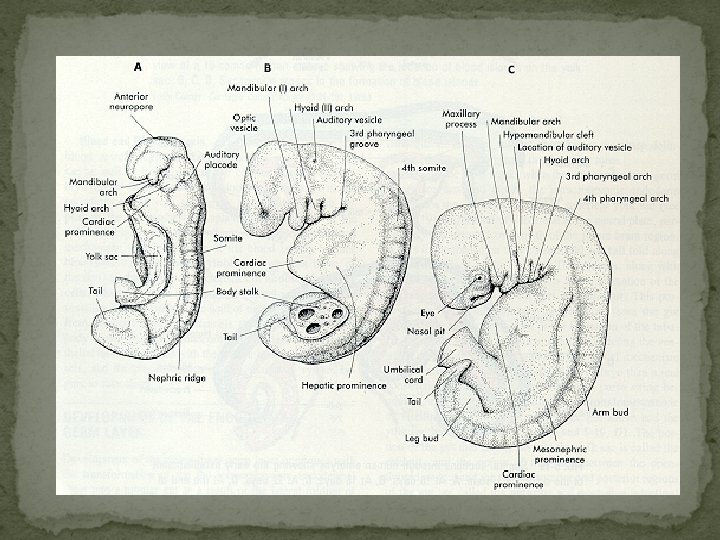
Development of fetous : -

Amnion Cell Histogenesis Amnion epithelial cells derived from fetal ectoderm (embryonic disc) active metabolically; synthesis of tissue inhibitos of metalloproteinase-1 Amnion mesenchymal cells derived from the embryonic mesoderm synthesis of interstitial collagens that make up the compact layer of the amnion highly capable of synthesizing cytokines - IL-6, IL-8, MCP-1 increased in response to bacterial toxin and IL-1

Anatomy Reflected amnion Placental amnion Umbilical amnion

Tensile Strength decidua and chorion laeve are quite elastic and can expand to twice normal size during pregnancy Amnion provides the major strength of the membrane Tensile strength of amnion resides almost exclusively in the compact layer composed of cross-linked interstial collagens I, III, and lesser amounts of V and VI

Metabolic Functions solute and water transport to maintain amnionic fluid homeostasis produces a variety of bioactive compounds vasoactive peptides, growth factors, cytokines Amnionic Fluid normally clear fluid that collects within the amnionic cavity increases in quantity as pregnancy advances until near term, when it normally decreases Average volume of about 1, 000 m. L is found at term
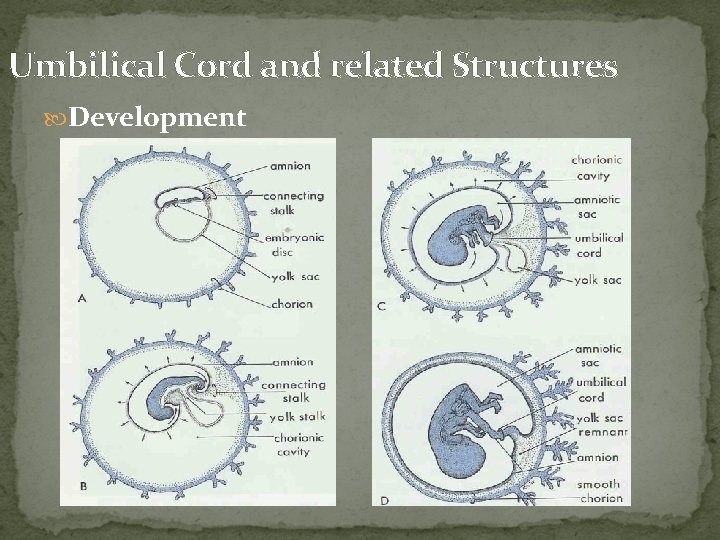
Umbilical Cord and related Structures Development

Structure and Function Umbilical cord, or funis fetal umbilicus -fetal surface of the placenta diameter: 0. 8 - 2. 0 cm average length: 55 cm (usual length: 30 - 100 cm) nodulation , false knot Extracellular matrix: Wharton's jelly
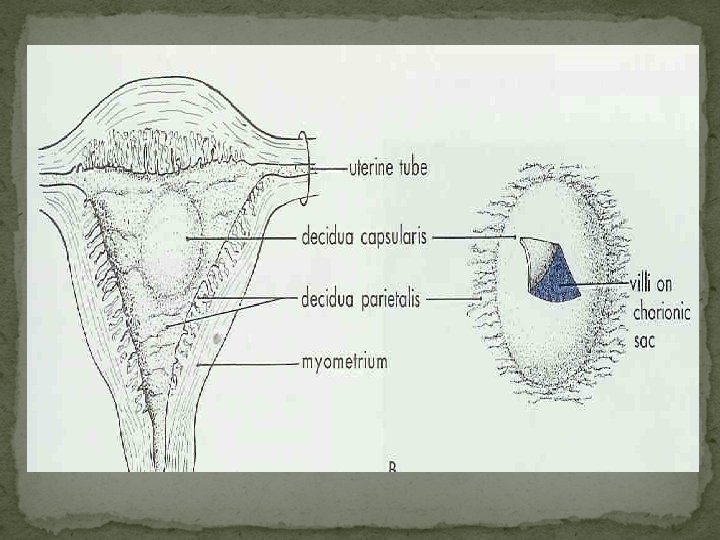
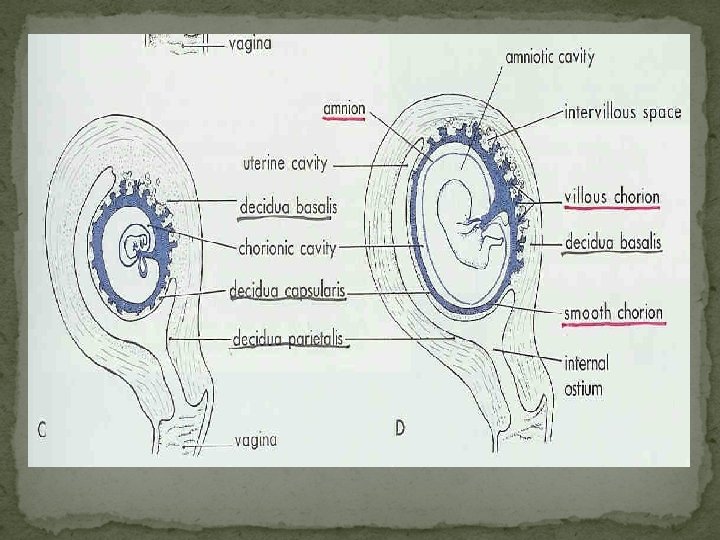
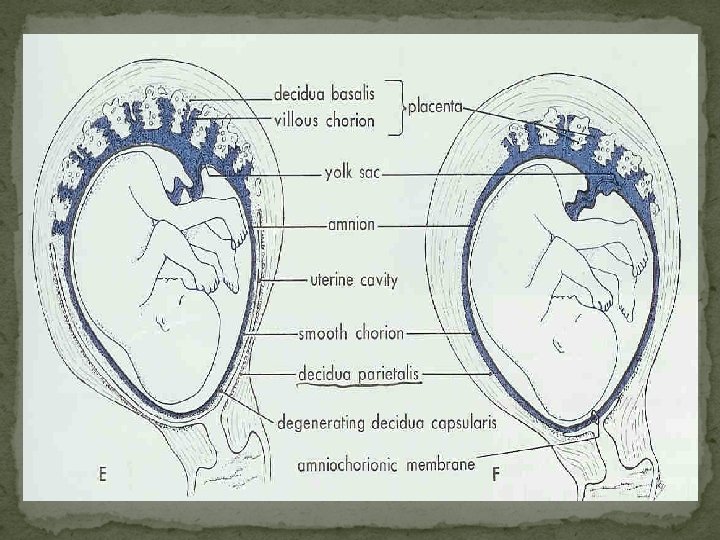

Important!!!! In all cases, fetal and maternal blood does not mix.
- Slides: 69