The Personality Disorders By Dr Diyar Hussein Tahir

The Personality Disorders By Dr. Diyar Hussein Tahir M. B. Ch. B. -F. I. C. M. S. Psych. Department of psychiatry, College of Medicine, Hawler Medical University. 1

What is Personality? It is the enduring patterns of thinking, feeling and behaviour which makes one individual distinguishable from another. So personality is stable – or at least relatively stable, i. e. we do not change dramatically from week to week. Jekyll-and-Hyde personality changes are, thankfully, extremely rare. 2

General Determinants of Personality: 1 - Genetic factor. 2 - Neuropsychological factors. 3 - Family Environment. 4 - Social Factors. 3

General characteristics of personality traits or elements: 1. Present since teenage years. 2. Consistent overtime. 3. Recognized by friends and relatives. 4. Stable in different situations. 4

Questions to ask when assessing personality: v v v Do you make friends easily? Can you sustain relationships? Are you usually happy, miserable, worrying? Are you very tidy, punctual, exciting? Do you ever lose control or behave violently? How do you react to frustration? Do you stand up for yourself ? Have you talked about the future & what you wish for it? Are you able to express feelings? How do you respond to difficult situations? Do you behave impulsively? Are you prone to mood swings? 5

The Five-Factor Model of Personality: Character + Temperament 1 - Neuroticism Ø Ø Ø Calm – Worrying Even tempered – Temperamental Self satisfied – Self dissatisfied Comfortable – Self conscious Unemotional – Emotional Hardy – Vulnerable 2 - Extraversion Ø Ø Ø Reserved – Affectionate Loner – Joiner Quiet – Talkative Passive – Active Serious – Fun loving Unfeeling – Passionate 3 - Openness to Experience Ø Ø Ø Down to earth – Imaginative Uncreative – Creative Conventional – Original Prefer routine – Prefer variety 6 Uncurious – Curious Conservative – Liberal 4 - Agreeableness Ø Ø Ø Callous – Soft hearted Suspicious – Trusting Stingy – Generous Antagonistic – compliant Critical – Easygoing Irritable – Good natured 5 - Conscientiousness Ø Ø Ø Negligent – Conscientious Lazy – Hardworking Disorganized –Well organized Late – Punctual Aimless – Ambitious Quitting – Persevering

Abnormal Personalities Definitions: The personality that characterized by deeply ingrained maladaptive patterns of behaviour which are recognizable from adolescence & continue onto adult life. The abnormality may be in the balance of personality elements, their quality or expression, or in its total aspect. The person &/or society suffer as a result. …So: Everyone has a collection of personality traits but if these traits lead to a personal distress or to problems in the social or occupational functioning, the person may have a personality disorder. 7

General diagnostic criteria for PD according to DSM-IV-TR: A. An enduring pattern of inner experience and behavior that deviates markedly from the expectations of the individual's culture. This pattern is manifested in two (or more) of the following areas: 1 - Cognition (i. e. ways of perceiving & interpreting self, other people, & events) 2 -Affectivity(i. e. range, intensity, liability, & appropriateness of emotional response) 3 - Interpersonal functioning 4 - Impulse control B. The enduring pattern is inflexible and pervasive across a broad range of personal & social situations. C. The enduring pattern leads to clinically significant distress or impairment in social, occupational, or other important areas of functioning. D. The pattern is stable and of long duration, and its onset can be traced back at least to adolescence or early adulthood. E. The enduring pattern is not better accounted for as a manifestation or consequence of another mental disorder. F. The enduring pattern is not due to the direct physiological effects of a substance (as a drug of abuse, a medication) or a general medical condition as head trauma

The general characteristics of PD: 1 - PD are remarkably stable and “orderly” i. e. predictable and unmalleable, so the term “disorder” is somewhat misleading. 2 - They tend to be rigid & inflexible, show a restricted range of traits with a dominant single trait. 3 -They have low grade chronic problems with no insight, and often no enough pain to seek help themselves; therefore they often forced to treatment, but difficult to be assessed. 4 -While PD have unhappiness and often other clinical disorders, they are not likely to feel conflicted about their traits, i. e. they are egosyntonic rather than egodystonic 5 -PD (Axis-II ) can co-exist with many Axis-I disorders. Mostly with substance use, mood, anxiety, and eating disorders. 6 -An individual can have more than one PD diagnosis. 9

The DSM multi-axial approach to diagnosing ; where all factors in a person’s life affect the mental health. Axis I: Clinical Syndromes; e. g. MDD, schizophrenia, …etc. Axis II: Developmental ( as autism, mental retardation) &Personality Disorders Axis III: Physical Conditions which play a role in the development, continuance, or exacerbation of Axis I and II Disorders, as brain injury or HIV/AIDS. Axis IV: Severity of Psychosocial Stressors; events in a person’s life, such as death of a loved one, starting a new job, college, unemployment, and even marriage Axis V: Highest Level of Functioning (Global Assessment of Relational Functioning; GARF Scale), by rating the person’s level of functioning at the present time & the highest level within the past year, to understand how the above four axes are affecting & the changes that could be expected to occur. 10

Historical perspective - Roots in the Freudian psychoanalysis: Narcissism, Masochism, etc. - Karl Abraham – first theorist to focus on PD Freud’s famous couch 11

Prevalence n n 10 -13% of the population. Prevalence is higher among people with other mental disorders 60% of inpatient psychiatric patients. Most people with PD never come to the attention of mental health professionals 12
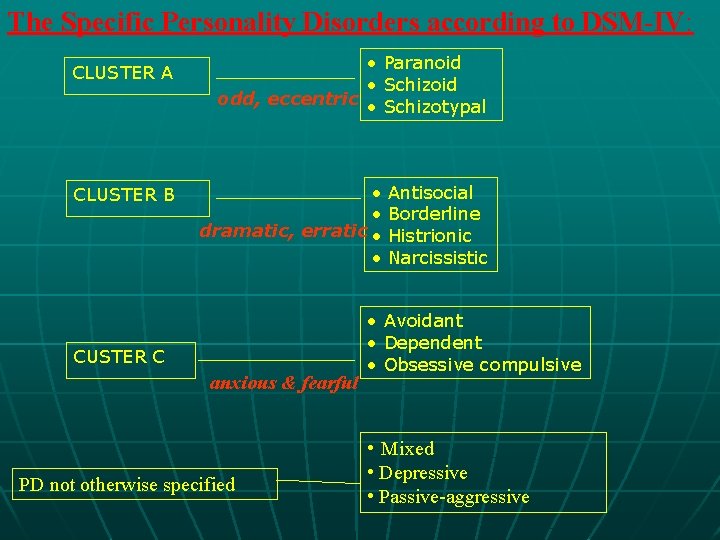
The Specific Personality Disorders according to DSM-IV: CLUSTER A CLUSTER B • Paranoid • Schizoid odd, eccentric • Schizotypal • • dramatic, erratic • • CUSTER C anxious & fearful PD not otherwise specified Antisocial Borderline Histrionic Narcissistic • Avoidant • Dependent • Obsessive compulsive • Mixed • Depressive • Passive-aggressive

The Specific Personality Disorders according to DSM-IV: A-Cluster A (odd & eccentric) PD: 1 -Paranoid Personality Disorder Feature: - Highly suspicious & preoccupied with distrust toward others but no delusions or hallucinations - Often hostile, irritable, argumentative & envious. - No confidants; the surrounding people have sinister motives - Sense of exploitation. - Sensitivity to any feeling for insult, & develop grudges Prevalence: * 0. 5 – 2. 5% in the general population. 14

2 -Schizoid Personality Disorder Features: ……aloof - Keep a distance from social relationships (withdrawn & reserved). - Few interests & pleasures in life, & takes pleasure in few activities. - Lacks close friends aside from relatives - Emotional coldness, detachment or flattened affect with Little interest in sexual experiences. - Chooses solitary activities - Indifferent to praise or criticism but they do not secretly wish for popularity. Prevalence: (<1%) 15

3 -Schizotypal Personality Disorder: Features: -Eccentric , odd thinking, behaviour & appearance. - Speaks in unusual vague & circumstantial ways. - Ideas of reference (incorrect interpretations) - Unconventional beliefs as having extrasensory abilities, or excessive magical thinking as about superstition or telepathy - Suspiciousness and paranoid ideation - Inappropriate or constricted affect. - Lack of close friends - Excessive social anxieties & Problems with close personal relationships. Prevalence: 3% of the general population 16

B-Cluster B (dramatic , emotional, or erratic) PD: 1 -Antisocial Personality Disorder (APD): Diagnostic criteria (DSM-IV) or features of APD : A. There is a pervasive pattern of disregard for and violation of the rights of others occurring since age 15 years, as indicated by three (or more) of the following: 1) failure to conform to social norms with respect to lawful behaviours as indicated by repeatedly performing acts that are grounds for arrest 2) deceitfulness, as indicated by repeated lying, use of aliases, or conning others for personal profit or pleasure. 3) impulsivity or failure to plan ahead. 17

4) irritability and aggressiveness, as indicated by repeated physical fights or assaults 5) reckless disregard for safety of self or others 6) consistent irresponsibility, as indicated by repeated failure to sustain consistent work behaviour or honour financial obligations 7) lack of remorse (regret), as indicated by being indifferent to or rationalising having hurt, mistreated, or stolen from another B. The individual is at least age 18 years. C. There is evidence of Conduct Disorder with onset before age 15 y. D. The occurrence of antisocial behavior is not exclusively during the course of Schizophrenia or a Manic Episode. 18
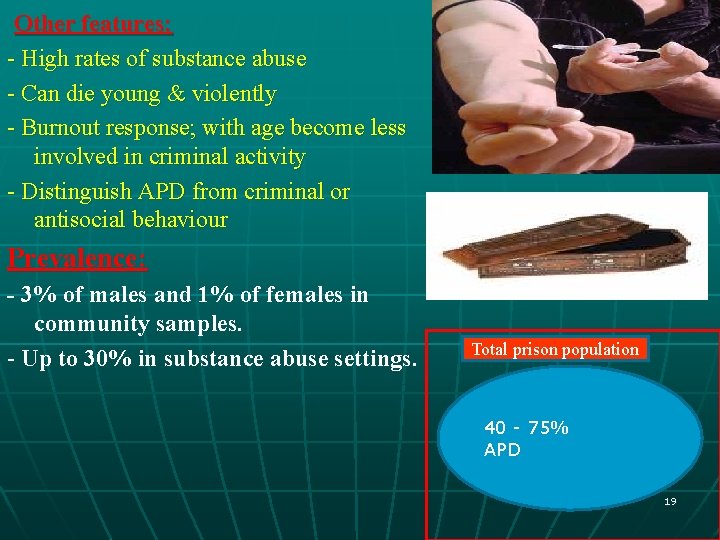
Other features: - High rates of substance abuse - Can die young & violently - Burnout response; with age become less involved in criminal activity - Distinguish APD from criminal or antisocial behaviour Prevalence: - 3% of males and 1% of females in community samples. - Up to 30% in substance abuse settings. Total prison population 40 - 75% APD 19

Etiology of APD - Family and parenting factors: disruptive family life, harsh & inconsistent discipline & lack of monitoring - Genetics: concordance rates for criminality are 51% for MZ twins & 21% for DZ. - Regarding punishment: it increase the frequency of the punished behaviour, rather than decrease it (defiance/opposition). Superego SE Ego Id Id Neurotic Sociopath 20

2 -Borderline PD: Features: - feelings of emptiness & boredom. -fragile identity with poor self-image - unpredictable, impulsive, argumentative, irritable with bouts of anger when their expectations are not met. Anger may directed toward themselves (self-mutilating behaviour). Suicide threats & action may happen - A fear of rejection and loss. - Rapidly changing mood & behaviour with intense unstable relationships - Brief psychotic episodes may occur. - Splitting: divide persons into those who like & those who hate them. - Turning against the self (self hate is prominent). - In their thirties or forties usually gain more stability Prevalence: - 75% are female - 2% of the general population. - 90% have other psychiatric diagnosis, & 40% have two. 21

3 -Histrionic Personality Disorder: Features : ( prevalence: 2%-3% of the general population) - Wants to be the center of attention, & often interrupt others to be the center of conversation - Rapidly shifting, & shallow but excessive expression of emotion. - very seductive; “life of the party” , but difficulty in relationships, & may be frigid sexually. - Shows self-dramatization, & exaggerate illnesses & friendships. - Suggestible, i. e. easily influenced by others or circumstances. - Consider relationships to be more intimate than they actually are. - Common defenses include repression, regression, identification, somatization, conversion, dissociation, denial, & externalization. 22

4 -Narcissistic Personality Disorder Features: ( Prevalence: 1% of the general population) - Inflated sense of their own importance with boastfulness. - Believes that they should associate with high-status people ( or institutions) as they perceive themselves to be. - Unable to see that others may not appreciate them, but hyper-sensitive to criticism - Offer help or facilities to others but to exploit them in the future. - lack of empathy & litigious in the quarrels. - Grandiosity, egocentricity, vengeful, but low self-esteem 23

C- Cluster C (anxious & fearful) PD: 1 -Avoidant Personality Disorder Features: - Extreme sensitivity to criticism and disapproval, so avoid situations in which criticism may be given otherwise feel anxious & get tachycardia, sweating, flushing…etc. due to chronic feeling of inadequacy. - Consider themselves to be socially incompetent or personally unappealing, and avoid social interaction for fear of being ridiculed or humiliated. - Inhibited, introverted with low self-esteem. - Shy and restrained. - Avoidance of intimacy. - Only involved if sure of praise. Prevalence: 0. 5%-1% of the general population 24

2 -Dependant PD: Features: - Pervasive psychological dependence on other people. - Has difficulty making everyday decisions without an excessive amount of advice, direction and reassurance from others. - Low opinion of their own abilities with fear of disapproval. - Fears of being alone & being unable to cope. - Not uncommon for such a patient to be living with a controlling, domineering, or overprotective person. 25

3 -Obsessive-compulsive PD: Features: - Inflexibility, stubbornness and desire for perfection - Tend to stress perfectionism above all else, and feel anxious when they perceive that things aren't "right". - A sense of their being only one way to do things - Failure to appreciate creative solutions. -Over-meticulous attention to the system & details - Failure to get things done as a result of excessive attention to detail. - A tendency to check and re-check, but absence of obsessional thoughts and compulsive behaviours Prevalence: 1% of the general population 26

D- PD not otherwise specified: Do not meet full criteria for any specific PD, however diagnostic criteria of PD are present , e. g. is the presence of features of more than one specific PD that do not meet the full criteria for anyone PD ("mixed PD"), but that together cause clinically significant distress or social or occupational impairment. This category can also be used when the clinician judges that a specific PD that is not included in the classification of PD is appropriate, e. g. depressive PD and passive-aggressive PD Diagnostic criteria of depressive personality disorder: A. A pervasive pattern of depressive cognitions and behaviors beginning by early adulthood & indicated by presence of most of the following: (1) usual mood is dominated by dejection, gloominess, joylessness, unhappiness (2) self-concept centers around beliefs of inadequacy, worthlessness, & low self esteem (3) is critical. blaming, and derogatory toward self (4) is brooding and given to worry (5) is negativistic, critical, and judgmental toward others (6) is pessimistic (7) is prone to feeling guilty or remorseful B. Does not occur exclusively during Major Depressive Episodes 27 & is not better accounted for by Dysthymic Disorder.

Passive aggressive PD: Features: - Outwardly compliant but inwardly hostile, which may alternate with regret. - Procrastinates with negative attitudes but passive resistance. - Sullen & argumentative. -Inefficient but expresses envy & resentment toward those apparently more fortunate. -May ask for help but then does not comply with the physician’s advice. 28
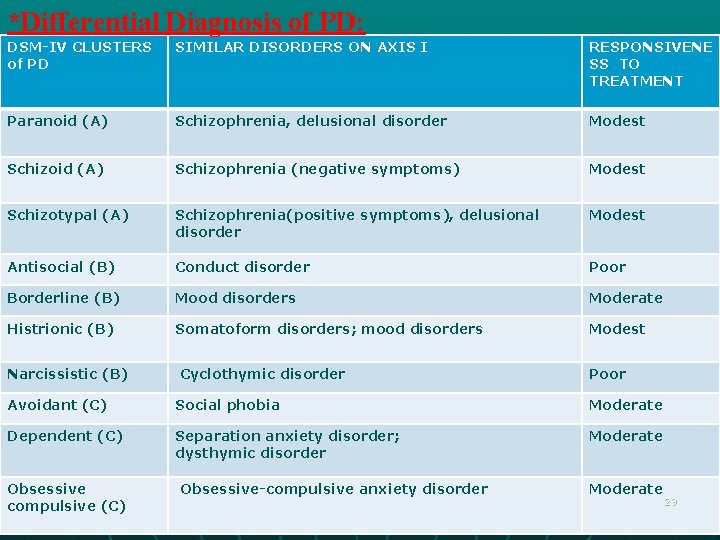
*Differential Diagnosis of PD: DSM-IV CLUSTERS of PD SIMILAR DISORDERS ON AXIS I RESPONSIVENE SS TO TREATMENT Paranoid (A) Schizophrenia, delusional disorder Modest Schizoid (A) Schizophrenia (negative symptoms) Modest Schizotypal (A) Schizophrenia(positive symptoms), delusional disorder Modest Antisocial (B) Conduct disorder Poor Borderline (B) Mood disorders Moderate Histrionic (B) Somatoform disorders; mood disorders Modest Narcissistic (B) Cyclothymic disorder Poor Avoidant (C) Social phobia Moderate Dependent (C) Separation anxiety disorder; dysthymic disorder Moderate Obsessive compulsive (C) Obsessive-compulsive anxiety disorder Moderate 29

*Management of PD: PD have no insight & lack awareness that they are the cause of their own relationship problems, so they rarely seek psychological help unless compelled by others. General principles in the management: • Be Respectful with a non-judgmental attitude. • Acknowledge affect (emotion). • Be aware of the counter transference. • Set realistic expectations. • Set limits and provide consistent structure. • Maintain professional boundaries. • Label the maladaptive behaviors of the patient. • Seek consultation from a psychiatrist. Medication: pharmacological treatment has no proven usefulness in PD. Antipsychotics, antidepressants & antianxiety drugs can however be used when there is psychotic, depressive or anxiety features or disorders. But: - Sever behavioural dyscontrol as sometimes seen in APD & BPD may respond to carbamazipine - Impulsivity……. . SSRI - Affective Dysregulation………SSRI, Mood Stabilizers. 30 i. e. Medication choice based more on the target symptom & less on diagnosis.

Psychotherapy: Individual, group & family psychotherapies, & self-help groups may benefit patients with PD. Those based on: -Psychodynamic therapy -Cognitive behavioural therapy (CBT), especially dialectical behavioural therapy ( a systematic CBT, focuses on motivational issues and seeks to balance skill development with a supportive context) - The resolution of many problems faced by PD patients requires the development of new copping mechanisms & better social skills. • Treatment of Cluster A disorders is most difficult • Treatment of the Cluster C disorders seems most promising • For Borderline PD: CBT, esp. dialectical behavior therapy, shows promise through : – Building tolerance for distress and negative affect without being self-destructive – Decrease self-harm behaviors (suicide, mutilation, substance abuse), – Decrease behaviors that interfere with therapy (missing sessions, lying) – Learn to regulate emotion and improve interpersonal skills • In APD: -Difficulty establishing therapeutic alliance, & treatment approaches are not very successful , & more success occur with prevention and early intervention - Need to focus on specific behaviours, as anger management 31

THANK YOU 32
- Slides: 32