The Personal Medical Home and Maternity Care Brooks

The Personal Medical Home and Maternity Care Brooks Flood, DO, Brandy Deffenbacher, MD, Annamarie Meeuwsen, MD, Suzanne Gomez, MD, and Jay H. Lee, MD University of Colorado Family Medicine Residency (UCFMR)


Objectives • Describe the Patient Centered Medical Home (PCMH) • Describe the “current state” of maternity care at the UCFMR • Discuss the PCMH curriculum • Describe how residents use practicebased learning to assess change

PCMH • Future of Family Medicine 2004 o Described “New Model” of Care § Evidence Based § EMR’s § Asynchronous Communication § Office design § § o • Advanced scheduling Group Visits Described Medical Home P 4 2006 o How do we put these concepts into residency training?

P 4 • Preparing the Personal Physician for Practice • CU Goals: o Make a better doctor for today’s and tomorrow's needs o Revamp Curriculum o “Intentionalize” Internship o Create a PCMH

PCMH • Prepare PGY 2 residents to be effective participants in a practice that is a patient centered medical home by: o More consistent presence in clinic o More cohesive teams o Group visits o Community integration o Health behavior change counseling o New roles and relationships

Schedules n Prior to PCMH n Rotations dictated clinic days n No clinic days during certain rotations n Each month focused on specialty training n “training to be surgeon, internist, ob/gyn”
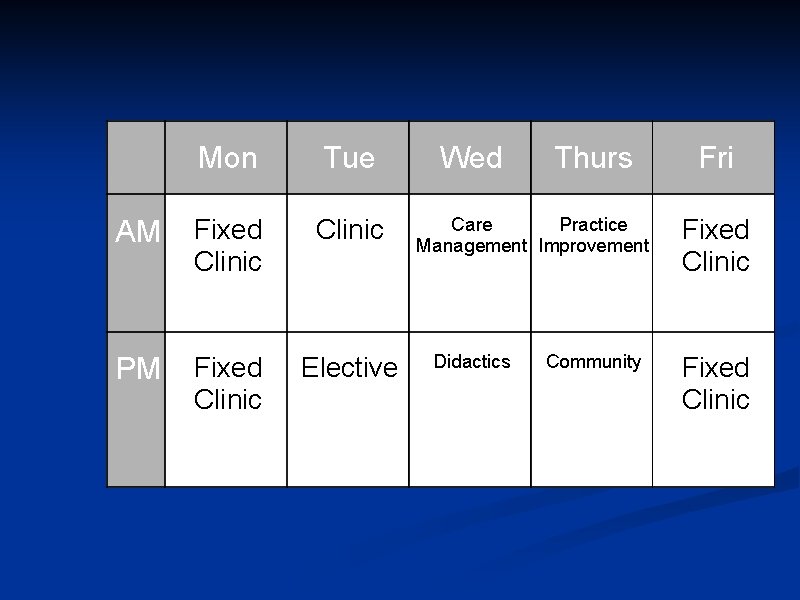

Mon Tue AM Fixed Clinic PM Fixed Clinic Elective Wed Thurs Care Practice Management Improvement Didactics Community Fri Fixed Clinic

PCMH Research Question n How does working in a PCMH residency affect our maternity care, especially in terms of continuity of care?

Methods Suzy Gomez

Study Method n Retrospective chart review

Definition of Continuity and PCP • Continuity Requirement for Residency Review Committee (RRC) • • Prenatal, and postnatal Primary Care Provider • Provider who saw the patient the most times

University of Colorado Family Medicine Residency n University Track Academics and Research n 6 Residents n n Denver Health Track Underserved n 2 Residents n

AF Williams • Continuity clinic for the residents of the UH track • Part of the University of Colorado Hospital system

Lowry • Continuity clinic for residents of the DH track • Part of the Denver Health and Hospitals system (eight community health centers)

Inclusion Criteria • Receiving prenatal care from August 2008 to Feb 2009 • Delivered before Feb 1, 2009 • Prior to PCMH • AFW included all OB patients • Lowry data included OB patients seen by a resident

Exclusion Criteria o Two or less prenatal visits o Non-prenatal visits o Ultrasounds o Acute sick visits

Data Collection • Lowry • • AF • Data gathered in central log from each OB patient seen by a resident Williams Obtained of all OB patients from medical records

Data Collection § EMR search § Age, Gravity, Parity § LMP & EDC § Insurance § Number of providers § Number of prenatal visits

Continuity • Modified • MMCI modified continuity index = (1 - P/V)/(1 - 1/V) • P = # of providers who saw the patient • V = # of visits J Fam Pract 1987; 24: 165 -8.

Results Brandy Deffenbacher

Questions • Is there a relationship between age and continuity? • Do primigravidas or multigravidas have better continuity? • Do non-resident providers have better continuity? • Do insured patients have better continuity?
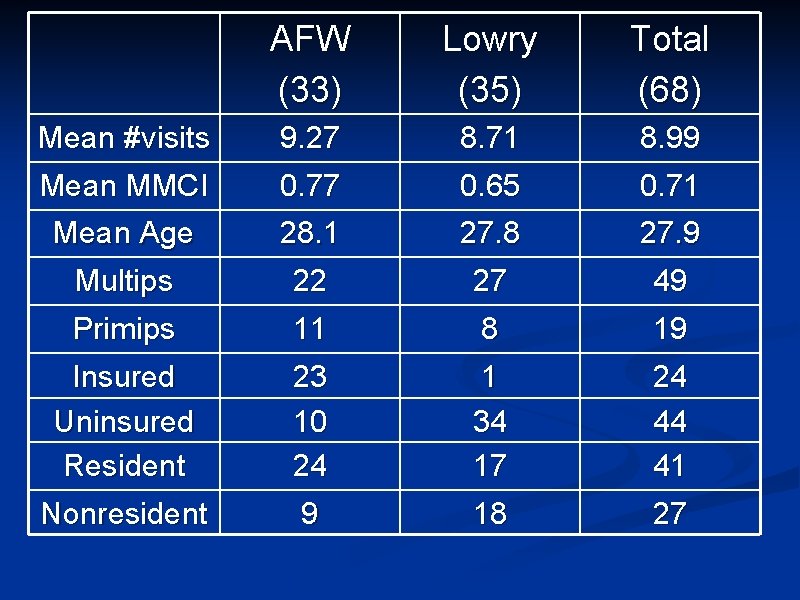
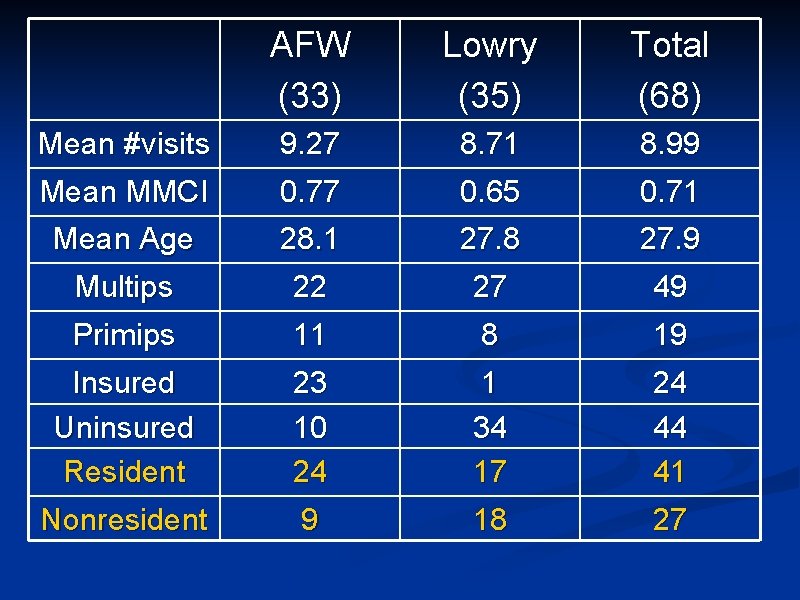
AFW (33) Lowry (35) Total (68) Mean #visits Mean MMCI 9. 27 0. 77 8. 71 0. 65 8. 99 0. 71 Mean Age Multips 28. 1 22 27. 8 27 27. 9 49 Primips 11 8 19 Insured Uninsured Resident 23 10 24 1 34 17 24 44 41 Nonresident 9 18 27
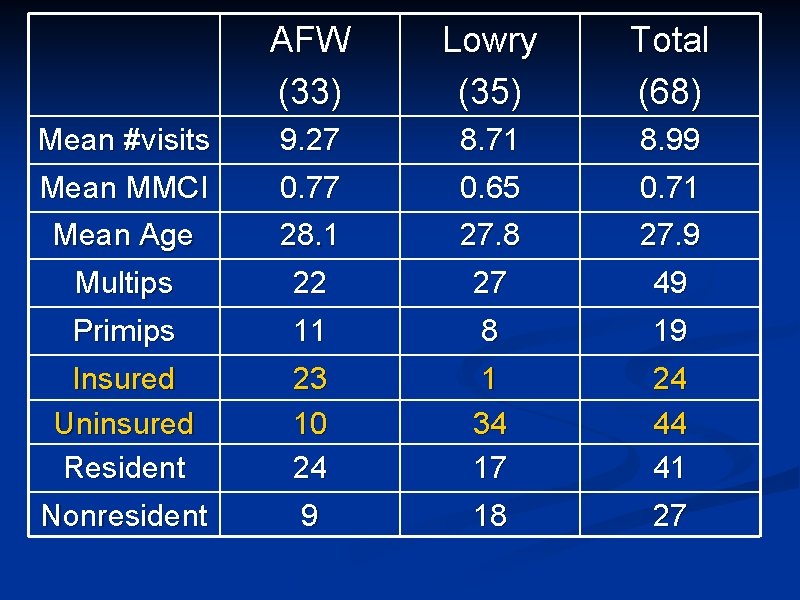
AFW (33) Lowry (35) Total (68) Mean #visits Mean MMCI 9. 27 0. 77 8. 71 0. 65 8. 99 0. 71 Mean Age Multips 28. 1 22 27. 8 27 27. 9 49 Primips 11 8 19 Insured Uninsured Resident 23 10 24 1 34 17 24 44 41 Nonresident 9 18 27

Age and Continuity • Is there a relationship between age and continuity?
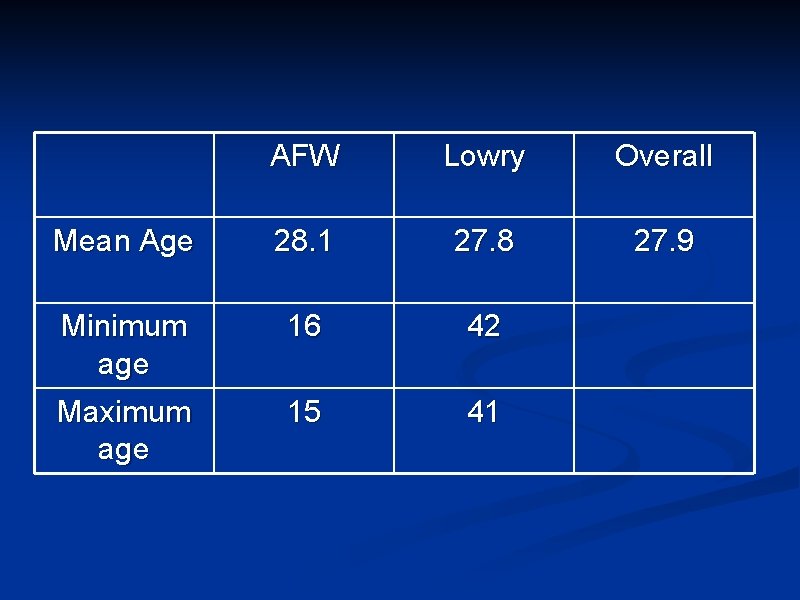
AFW Lowry Overall Mean Age 28. 1 27. 8 27. 9 Minimum age 16 42 Maximum age 15 41

Age and Continuity • AFW • • Lowry • • Spearman correlation=0. 64 Overall • • Spearman correlation=0. 45 Spearman correlation=0. 97 No correlation between age and continuity

Multip vs Primip • Do multigravidas or primigravidas have better continuity?
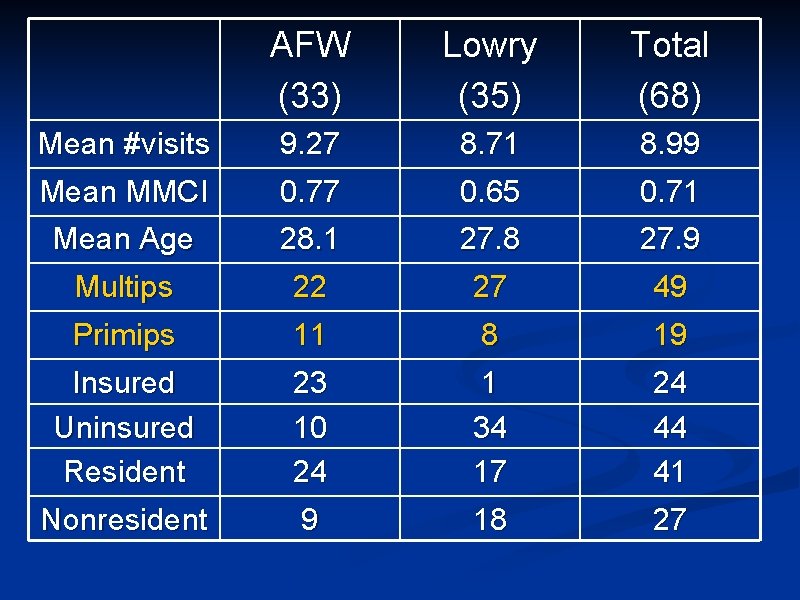
AFW (33) Lowry (35) Total (68) Mean #visits Mean MMCI 9. 27 0. 77 8. 71 0. 65 8. 99 0. 71 Mean Age Multips 28. 1 22 27. 8 27 27. 9 49 Primips 11 8 19 Insured Uninsured Resident 23 10 24 1 34 17 24 44 41 Nonresident 9 18 27

Multip vs Primip • AFW • • Multips median MMCI: 0. 80 (IQ range 0. 69 -0. 89) Primips median MMCI: 0. 85 (IQ range 0. 75 -0. 92) P*=0. 31 Lowry • • • Multips median MMCI: 0. 67 (IQ range 0. 55 -0. 83) Primips median MMCI: 0. 71 (IQ range 0. 67 -0. 74) P*= 0. 62 *Wilcoxon Rank-Sum test (used for non-normally distributed data)

Multip vs Primip • Overall • Multips median MMCI: 0. 75 (IQ range 0. 60 -0. 83) • Primips median MMCI: 0. 75 (IQ range 0. 70 -0. 89) • P*=0. 21 • No difference in continuity * Wilcoxon Rank-Sum test

Nonresident vs Resident PCP • Do non-resident providers have better continuity?
AFW (33) Lowry (35) Total (68) Mean #visits Mean MMCI 9. 27 0. 77 8. 71 0. 65 8. 99 0. 71 Mean Age Multips 28. 1 22 27. 8 27 27. 9 49 Primips 11 8 19 Insured Uninsured Resident 23 10 24 1 34 17 24 44 41 Nonresident 9 18 27
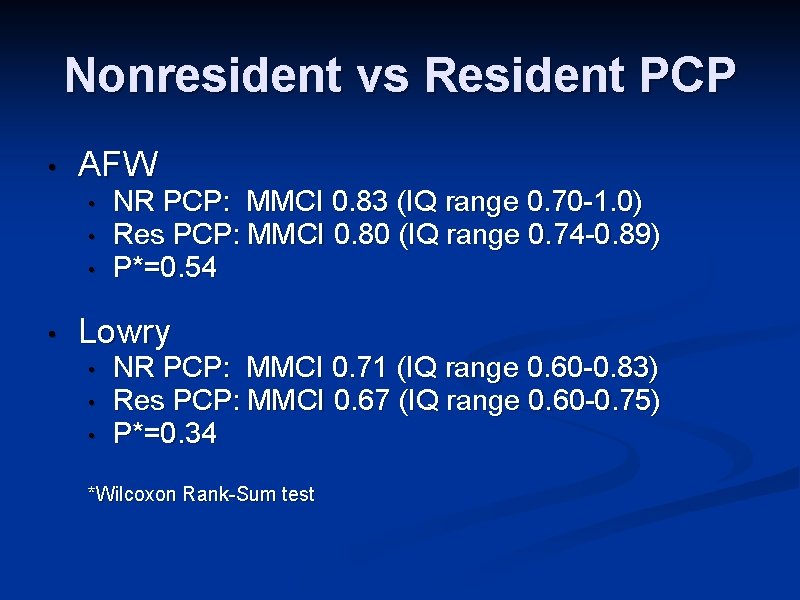

Nonresident vs Resident PCP • AFW • • NR PCP: MMCI 0. 83 (IQ range 0. 70 -1. 0) Res PCP: MMCI 0. 80 (IQ range 0. 74 -0. 89) P*=0. 54 Lowry • • • NR PCP: MMCI 0. 71 (IQ range 0. 60 -0. 83) Res PCP: MMCI 0. 67 (IQ range 0. 60 -0. 75) P*=0. 34 *Wilcoxon Rank-Sum test

Nonresident vs Resident PCP • Overall • NR PCP: MMCI 0. 71 (IQ range 0. 60 -0. 85) • Res PCP: MMCI 0. 75 (IQ range 0. 67 -0. 86) • P*=0. 88 • No difference *Wilcoxon rank-sum test

Level of Resident Training • Is there a difference in continuity between residents in different years of postgraduate training?
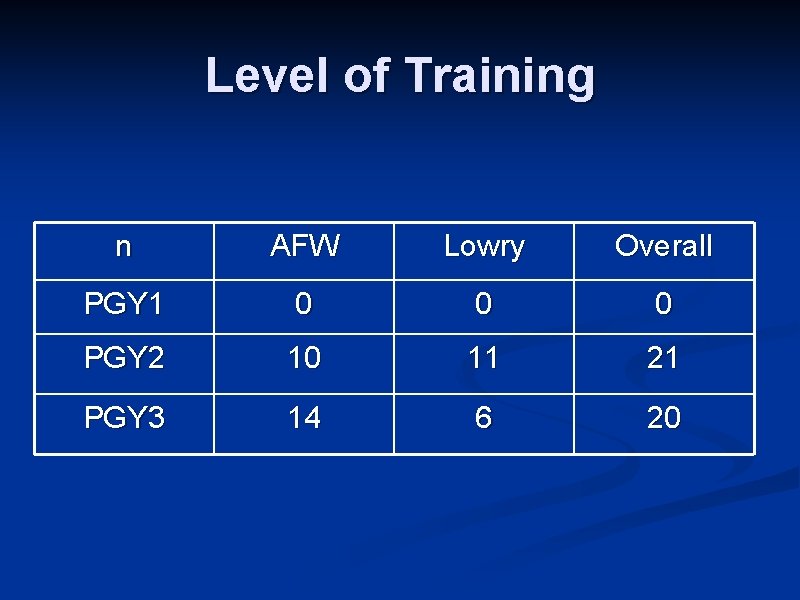
Level of Training n AFW Lowry Overall PGY 1 0 0 0 PGY 2 10 11 21 PGY 3 14 6 20

Level of Training • Overall: • • • No data for PGY 1 PGY 2 median MMCI: 0. 67 (0. 67 -0. 80) PGY 3 median MMCI: 0. 78 (0. 71 -0. 89) P*= 0. 08 No difference *Wilcoxon rank-sum test

Insured vs Uninsured • Do insured patients have better continuity?
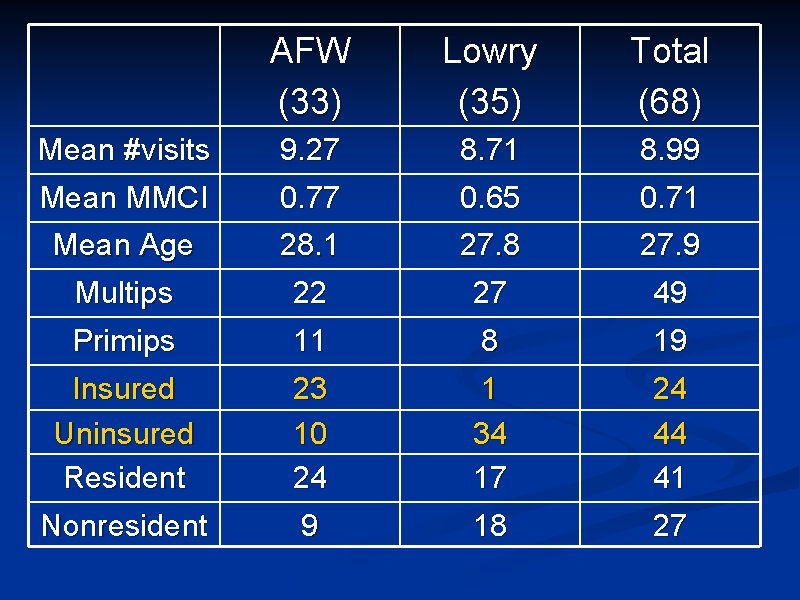
AFW (33) Lowry (35) Total (68) Mean #visits Mean MMCI 9. 27 0. 77 8. 71 0. 65 8. 99 0. 71 Mean Age Multips 28. 1 22 27. 8 27 27. 9 49 Primips 11 8 19 Insured Uninsured Resident 23 10 24 1 34 17 24 44 41 Nonresident 9 18 27
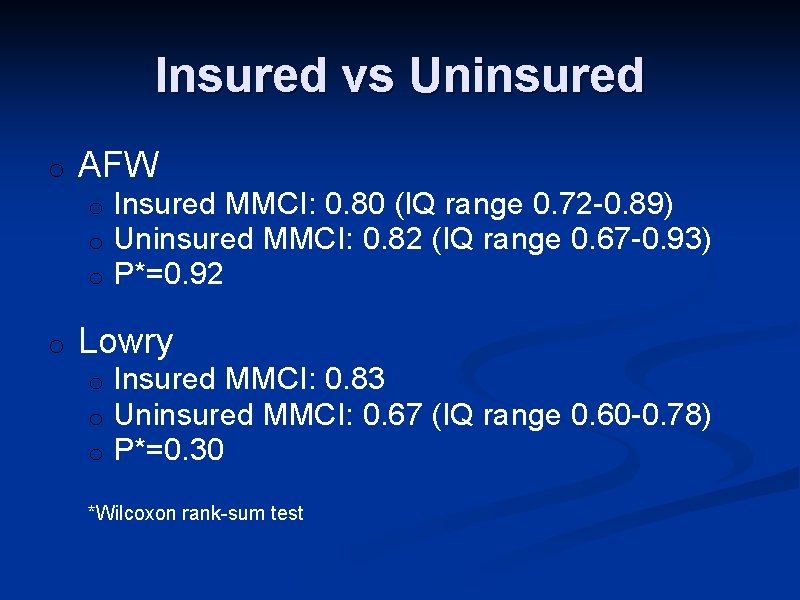
Insured vs Uninsured o AFW o o Insured MMCI: 0. 80 (IQ range 0. 72 -0. 89) Uninsured MMCI: 0. 82 (IQ range 0. 67 -0. 93) P*=0. 92 Lowry o o o Insured MMCI: 0. 83 Uninsured MMCI: 0. 67 (IQ range 0. 60 -0. 78) P*=0. 30 *Wilcoxon rank-sum test

Insured vs Uninsured o Overall o Insured MMCI: 0. 82 (IQ range 0. 74 - 0. 89) o Uninsured 0. 83) o P*= 0. 001 *Wilcoxon rank-sum test MMCI: 0. 70 (IQ range 0. 60 -

DISCUSSION Brooks Flood

Outline n How this evolved n Flaws n What we learned n Future plans for continued study

How this idea started

n The minimum requirements for a continuity patient (program requirements IV. A. 5. b. 3. c)

What the idea evolved into: n How to provide better continuity in the care of our patients

n Our new goal focused on how our new PCMH curriculum changes our OB continuity

n Upon doing the study we came upon difficulties and realized flaws in our design

Definitions of continuity differed n RRC definition of continuity was more lenient n MMCI more strictly defined

Other variables that affected our data n Lowry and AFW collected data differently n Patients were excluded if not seen more than twice during the antenatal period

The MMCI numbers we came up with are actually better than we anticipated

Why our results may be different than what we expected: n Retrospective study design n Artificial designation of PCP n Inconsistent methods of collection n Poor handwriting on some charts n Providers having the same initials

What we’ve learned

Poor communication = Poor continuity

Future Directions

In the future n Focus on improved clinic communication n Predictable presence in clinic n Collect nine more months of data while in PCMH

Thank you!

Acknowledgements Rachel Everhart Jay Lee
- Slides: 59