The Pathology of Liver Biliary System Part1 Is

The Pathology of Liver & Biliary System Part-1 Is life worth living? It depends on the liver! 1

This is liver ! • If individual hepatocytes are destroyed but the architecture of the lobule is not destroyed, the remaining hepatocytes will totally regenerate the liver parenchyma. – The Greek titan Prometheus had his liver devoured each day by a monster bird (simurg), but it always grew right back. 2

• Belongs to RE & Digestive system. • Hemopoietic organ before birth. • 1500 g, (2. 5% of body weight) right hypochondrium, wedge shape • end-stage cirrhotic 700 g liver, • an alcoholic 7000 g liver • Center of metabolic homeostasis. • Portal and Hepatic blood supply. • Micro-architecture – Lobules / Acini. 3
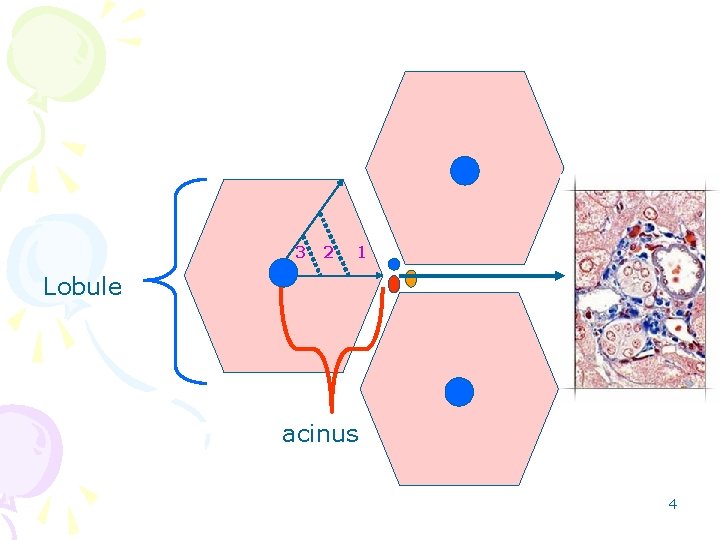
3 2 1 Lobule acinus 4

• Zones of a lobulus: – Zone 1 is the hepatocytes near the portal areas, – Zone 2 is the hepatocytes midway between the portal areas and central veins, – Zone 3 is the hepatocytes around the central veins. 5
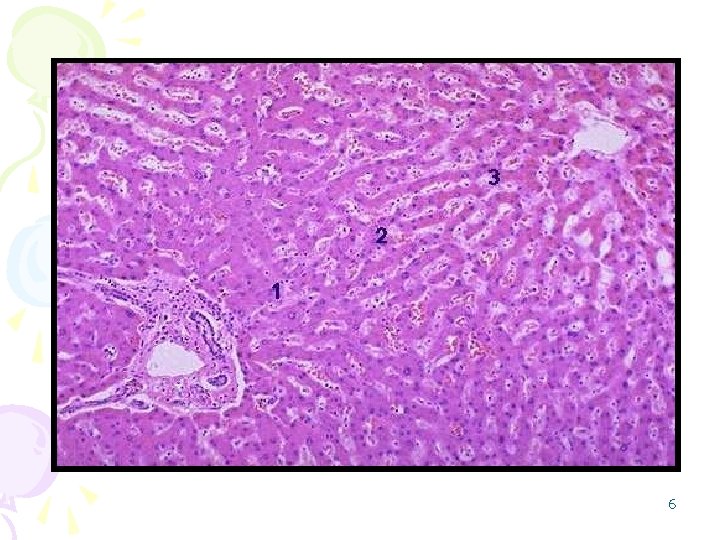
6

Functions • Metabolism – Carbohydrate, Fat & Protein • Secretory – Bile, Bile acids, salts & pigments • Excretory – Bilirubin, drugs, toxins • Synthesis – Albumin, coagulation factors • Storage – Vitamins, carbohydrates etc. • Detoxification – Toxins, ammonia, etc. 7
Disorders • Acute Liver Disorder: – Viral, Drug, Gall stones, alcohol toxicity. • Chronic Liver Disease: – Chronic hepatitis, Cirrhosis, viral, alcohol, – Autoimmune hepatitis. • Congenital Disorders: – Haemochromatosis, – Wilsons, – 1 AT deficiency • Tumors: – Benign: Adenoma, angioma, Nodular hyperplasia – Malignant: Hepatocellular carcinoma, Cholangiocarcinoma, Hepatoblastoma, Angiosarcoma. • Cysts: – Simple, – Hydatid. 8

Pathogenesis of clinical features Jaundice Impaired conjugation or obstruction. Dark urine Conjugated hyperbiluribinemia Pale stools Biliary obstruction Edema Low albumin – low oncotic pressure Steatorrhoea Bile obstruction Pruritis Bile obstruction Bile salt in blood. Ascites Portal hypertension, low albumin Bleeding Coagulation factor synthesis Hematemesis Esophageal varices (+hemorrhoids) Encephalopathy Toxic nitrogen products – gut bacteria Fetor hepaticus Musty odor (mercaptans by gut bacteria) 9

Circulatory Disorders • Liver Infarction • Portal Vein Obstruction and Thrombosis • Passive Congestion and Centrilobular Necrosis • Peliosis Hepatis • Hepatic Vein Thrombosis (Budd. Chiari Syndrome) • Veno-Occlusive Disease 10
Liver Infarction • Liver infarcts are rare (double blood supply) • Cause is thrombosis or compression of an intrahepatic branch of the hepatic artery by – – embolism, neoplasia, polyarteritis nodosa, sepsis. • Zahn infarct: Occlusion of an intrahepatic branch of the portal vein (does not cause ischemic infarction) sharply demarcated area of red-blue discoloration infarct of Zahn (old terminology). – In this condition, there is no necrosis, only marked stasis in distended sinusoids, with secondary hepatocellular atrophy. 11
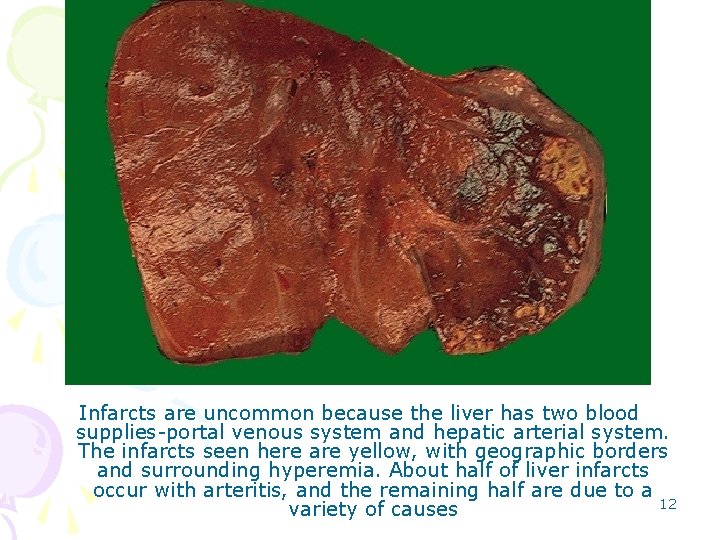
Infarcts are uncommon because the liver has two blood supplies-portal venous system and hepatic arterial system. The infarcts seen here are yellow, with geographic borders and surrounding hyperemia. About half of liver infarcts occur with arteritis, and the remaining half are due to a 12 variety of causes
• Portal Vein Obstruction and Thrombosis Extrahepatic causes of portal vein obstruction include: – (1) massive enlargement of hilar lymph nodes owing to metastatic abdominal cancer; – (2) phlebitis resulting from peritoneal sepsis (e. g. , acute diverticulitis or appendicitis); – (3) splenic vein thrombosis secondary to pancreatitis; – (4) post-surgical thrombosis following upper abdominal procedures. The most common intrahepatic cause: – Cirrhosis of the liver. 13

• Banti’s syndrome: – splenomegaly, – hypersplenism, – portal hypertension • Postulated causes: – – – – neonatal omphalitis, dehydration, sepsis, umbilical vein catheterization, hypercoagulable myeloproliferative disorders, biliary tract surgery, peritonitis, exposure to arsenicals. 14

Passive Congestion • Acute and chronic passive congestion of the liver usually reflects cardiac decompensation most commonly rightsided failure • Liver: – slightly enlarged, – tense, – cyanotic, with rounded edges. • On cut section, – there is an excessive ooze of blood, – centrilobular areas are soft, – surrounded by paler, fatty liver substance in the portal areas (the “nutmeg liver”). 15
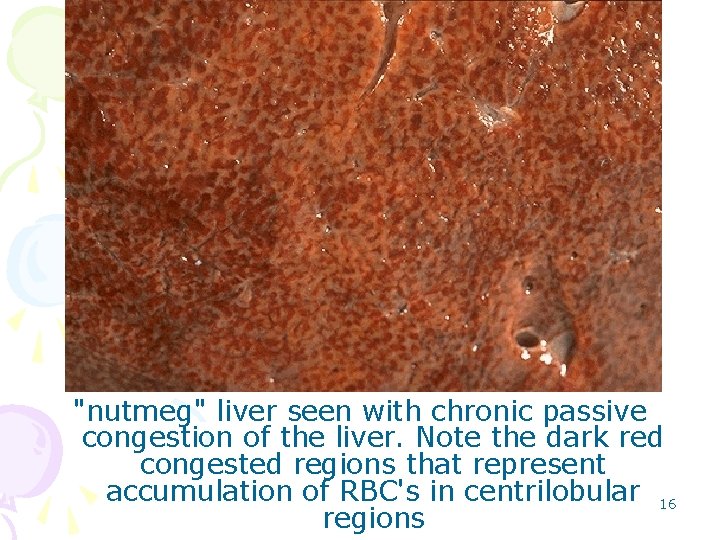
"nutmeg" liver seen with chronic passive congestion of the liver. Note the dark red congested regions that represent accumulation of RBC's in centrilobular 16 regions

• Nutmeg: Fruit of nutmeg tree Myristica fragrans. This tree grows in the Molucca Islands and elsewhere in Indonesia 17
18

Centrilobular Necrosis • Left-sided cardiac failure or shock hepatic hypoperfusion and hypoxia ischemic necrosis of hepatocytes in the central region of the lobule (Centrilobular necrosis) macroscopically as a slight depression of necrotic lobular centers. • Microscopy: – sharp demarcation of viable and necrotic hepatocytes moving from portal tract to the centrilobular region. – The necrosis is coagulative, – there is no inflammation. 19
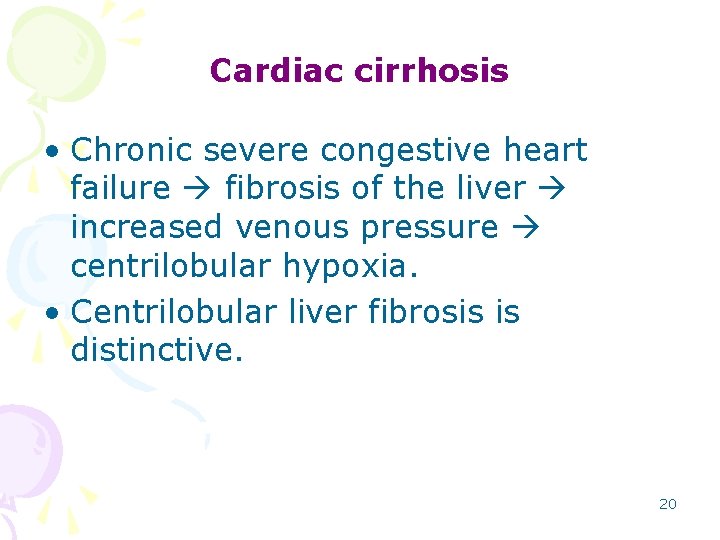
Cardiac cirrhosis • Chronic severe congestive heart failure fibrosis of the liver increased venous pressure centrilobular hypoxia. • Centrilobular liver fibrosis is distinctive. 20
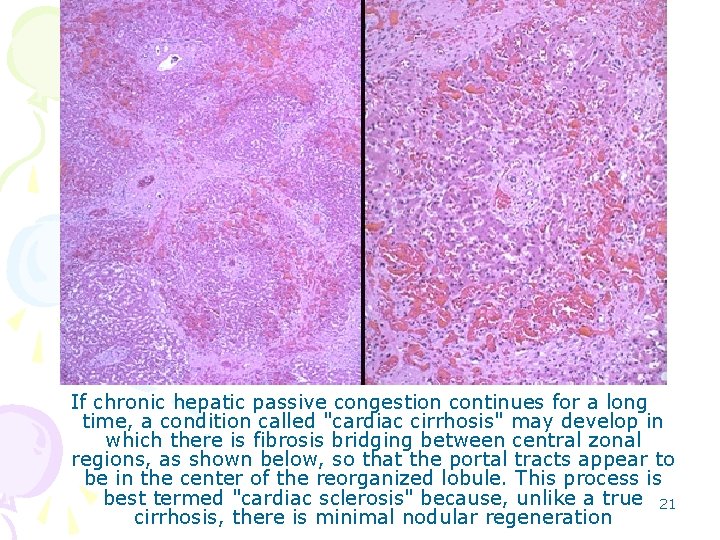
If chronic hepatic passive congestion continues for a long time, a condition called "cardiac cirrhosis" may develop in which there is fibrosis bridging between central zonal regions, as shown below, so that the portal tracts appear to be in the center of the reorganized lobule. This process is best termed "cardiac sclerosis" because, unlike a true 21 cirrhosis, there is minimal nodular regeneration

Peliosis Hepatis • Sinusoidal dilation • Although peliosis may be associated with hepatomegaly and even hepatic failure, it is more commonly a lesion found incidentally. • Etiology: – Drugs • anabolic steroids • oral contraceptives • danazol. 22
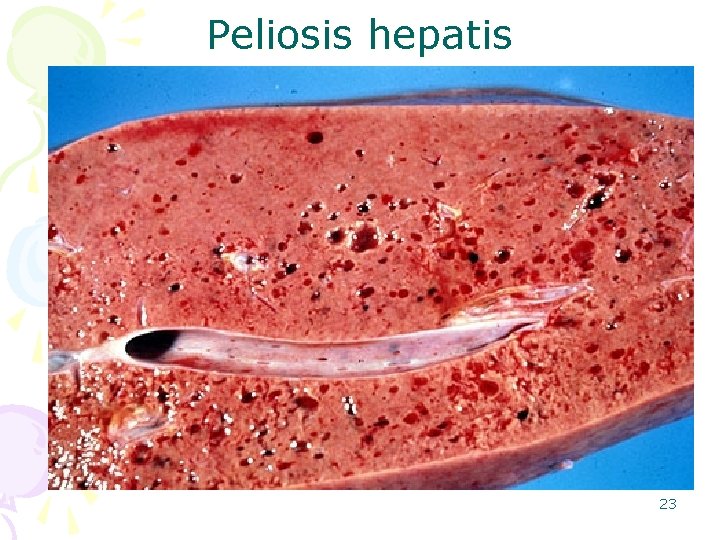
Peliosis hepatis 23
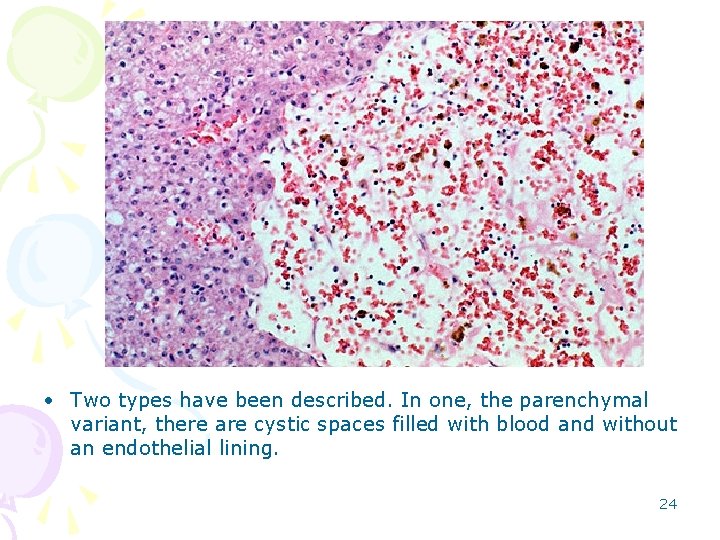
• Two types have been described. In one, the parenchymal variant, there are cystic spaces filled with blood and without an endothelial lining. 24
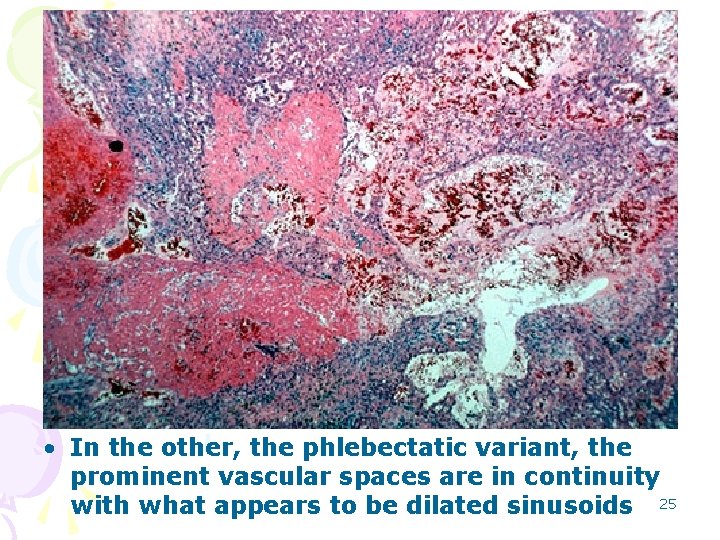
• In the other, the phlebectatic variant, the prominent vascular spaces are in continuity with what appears to be dilated sinusoids 25

Hepatic vein thrombosis ("Budd-Chiari") • Common causes: – polycythemia vera – hypercoagulable blood – invasion of the hepatic veins by hepatocellular carcinoma. • Complications: – ascites, – venous infarction. 26

Portal Hypertension • Increased resistance to portal blood flow • prehepatic, intrahepatic, and posthepatic causes. Prehepatic portal hypertension • Obstructive thrombosis and narrowing of the portal vein before it ramifies within the liver • massive splenomegaly shunts excessive blood into the splenic vein, which drains into the portal vein. 27

Intrahepatic portal hypertension • cirrhosis, • schistosomiasis • veno-occlusive disease • massive fatty change • diffuse fibrosing granulomatous disease, (sarcoidosis, miliary tuberculosis) • diseases affecting the portal microcirculation. 28

Posthepatic portal hypertension • severe right-sided heart failure, • constrictive pericarditis, • hepatic vein outflow obstruction. 29

Consequences of Portal hypertension • Ascites, • The formation of portosystemic venous shunts, • Congestive splenomegaly, • Hepatic encephalopathy. 30

Jaundice (icterus) increased bilirubin in the bloodstream • Hemolytic jaundice – – – too much bilirubin being produced Hemolytic anemias Intravascular hemolysis Extravascular hemolysis • Big hematomas • GI bleeding • Red infarcts Ineffective erytopoiesis Thalassemias Megaloblastic anemias • Hepatocellular jaundice – – – liver fails to uptake and/or conjugate bilirubin Newborns Hypoperfusion Bad alcoholism Genetic deficiency of bilirubin UGT activity (Crigler-Najhar syndrome) Gilbert Syndrome (mixedetiology) Diffuse hepatocellular disease (e. g. Viral or drug-induced hepatitis, cirrhosis) !!! The serum unconjugated bilirubin will be elevated!!!31

• Cholestatic jaundice – liver doesn't send bilirubin to the right place – Problems with the liver cells • drugs (estrogen, anabolic steroids) • Dubin-Johnson (pigmented) disease • Rotor (non-pigmented) disease • Byler's disease • benign familial recurrent intrahepatic cholestasis • hepatitis, cirrhosis, alcoholism – Problems with the bile ducts in the liver • • • Biliary cirrhosis Biliary atresia Alagille's syndrome – Problems with the bile ducts beyond the liver • Gallstones • Cancer (biliary, pancreatic, ampullary) • Iatrogenic (i. e. , the surgeon nicked the common bile duct). !!!The serum conjugated bilirubin will be elevated!!! 32

Post Hepatic (Obstructive) jaundice • Stone, tumor – Conjugated/Direct, High colored urine, Pre Hepatic (Acholuric) jaundice • Hemolytic – Unconjugated/Indirect, pale urine Hepatocellular jaundice • Viral, alcohol, toxins, drugs – Unconjugated : Liver damage – Conjugated: Swelling, canalicular obstruction 33
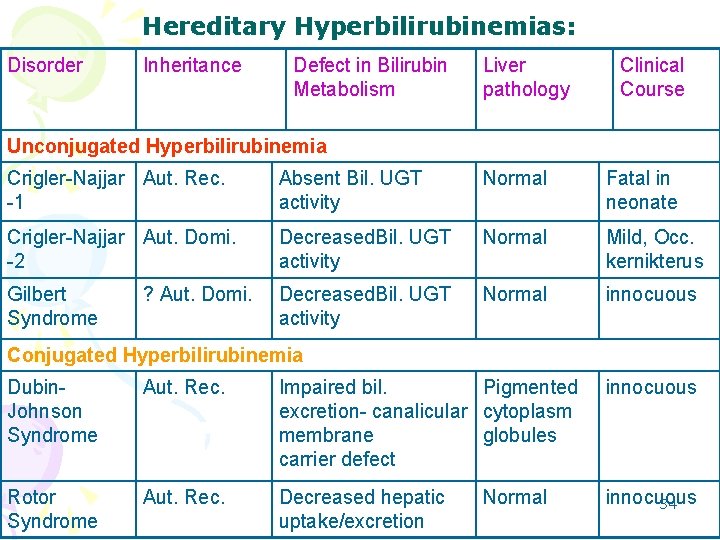
Hereditary Hyperbilirubinemias: Disorder Inheritance Defect in Bilirubin Metabolism Liver pathology Clinical Course Unconjugated Hyperbilirubinemia Crigler-Najjar Aut. Rec. -1 Absent Bil. UGT activity Normal Fatal in neonate Crigler-Najjar Aut. Domi. -2 Decreased. Bil. UGT activity Normal Mild, Occ. kernikterus Gilbert Syndrome Decreased. Bil. UGT activity Normal innocuous ? Aut. Domi. Conjugated Hyperbilirubinemia Dubin. Johnson Syndrome Aut. Rec. Impaired bil. Pigmented excretion- canalicular cytoplasm membrane globules carrier defect innocuous Rotor Syndrome Aut. Rec. Decreased hepatic uptake/excretion innocuous 34 Normal

Cholestasis • Hepatocellular dysfunction or intra or extrahepatic biliary obstruction may also present with jaundance. • Characteristic finding: elevated serum Alkaline phosphatase. • Elevated plasma bile acids results with pruritis. • Skin Xanthomas (focal accumulation of cholesterol) • Malabsorbtion of fat soluble vitamins due to reduced bile flow. 35

Byler Disease: • Progressive intrahepatic cholestasis • Aut. Rec. • This inherited condition results from impairment of bile salts or phospholipid secretion. Making correct diagnosis of the cause of jaundence and cholestatsis is urgent! 36
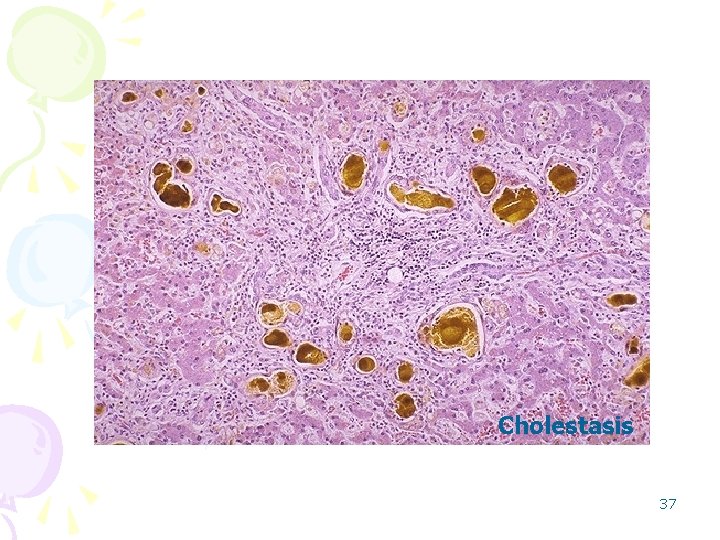
Cholestasis 37
38

Before specific disease processes are discussed general aspects of liver disease and definitions of general morphologic patterns of hepatic injury are reviewed! 39

Clinical Findings in Hepatic Failure • jaundice • hypoalbuminemia – ascites – edema • hypocholesterolemia • coagulopathy (diminished hepatic synthesis of factors II, V, VII, IX, and X). • hyperammonemia – fetor hepaticus • palmar erythema, • spider angiomas, • gynecomastia & testicular atrophy, • enlargement of the parotid glands (in longstanding liver failure). 40

Responses to injurious events Necrosis • Ischemic necrosis: – Poorly stained mummified hepatocytes remain (coagulative necrosis). • Apoptosis (Councilman or acidophyl bodies): • in toxic or immunologically mediated necrosis, • isolated hepatocytes round up to form shrunken, pyknotic, and intensely eosinophilic. 41
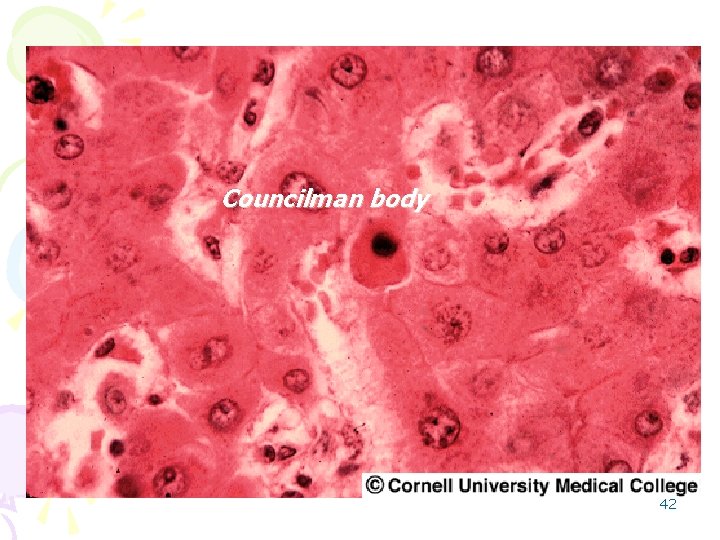
Councilman body 42

• Focal necrosis : Necrosis may be limited to scattered cells within the hepatic lobules • Zonal necrosis : Necrosis may involve particular regions of the lobule • Submassive necrosis : Necrosis may entire lobules • Massive necrosis : Necrosis may involve the whole liver 43

Focal necrosis • viral hepatitis. Zonal Necrosis • Centrilobular necrosis (3) – ischemic injury – drugs – toxic chemical reactions. • Midzonal necrosis (2) – yellow fever. • Periportal necrosis (1) – phosphorus poisoning – eclampsia. Massive necrosis – severe chemical – drug toxicity – viral hepatitis. Geographic necrosis – typhoid fever, – tularemia, – brucellosis, – herpesvirus, – adenovirus. Abscesses: with disseminated candidal or bacterial infection. 44
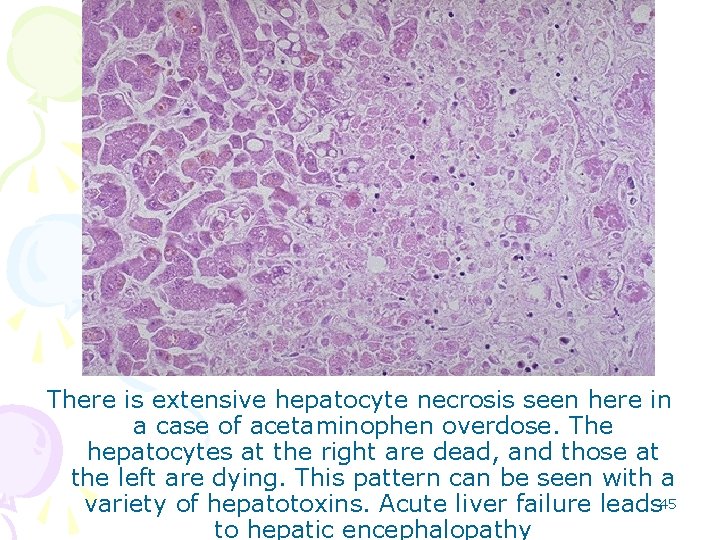
There is extensive hepatocyte necrosis seen here in a case of acetaminophen overdose. The hepatocytes at the right are dead, and those at the left are dying. This pattern can be seen with a variety of hepatotoxins. Acute liver failure leads 45 to hepatic encephalopathy

Hepatic injury Degeneration • Ballooning degeneration: – swollen, edematous appearance clumped cytoplasm – large, clear spaces • Cholestasis: – retained biliary material – diffuse foamy swollen appearance to the hepatocyte (Foamy degeneration) • Accumulation of specific substances in viable hepatocytes: iron, copper, viral particles. • Steatosis: Accumulation of fat droplets within the hepatocytes. (steatosis may be either microvesicular or macrovesicular) 46

Inflammation • Hepatitis – influx of acute or chronic inflammatory cells into the liver • Inflammation may be secondary to – hepatocellular necrosis, – lymphocytic attack of viable antigenexpressing liver cells. • Granulomatous reactions – foreign bodies, – organisms, – drugs. 47
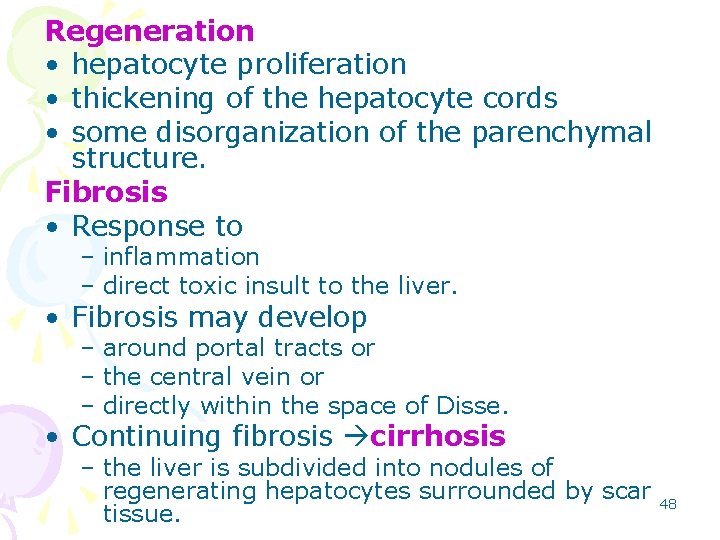
Regeneration • hepatocyte proliferation • thickening of the hepatocyte cords • some disorganization of the parenchymal structure. Fibrosis • Response to – inflammation – direct toxic insult to the liver. • Fibrosis may develop – around portal tracts or – the central vein or – directly within the space of Disse. • Continuing fibrosis cirrhosis – the liver is subdivided into nodules of regenerating hepatocytes surrounded by scar 48 tissue.

CIRRHOSIS • Disruption of the normal liver architecture by fibrous scars which have resulted from loss of liver cells • nodules of "regenerative" liver cells, which represent successful regeneration of the illperfused remaining hepatocytes. • Largely the result of : – – – alcohol abuse, viral hepatitis, chronic hepatitis, biliary disease, iron overload. 49

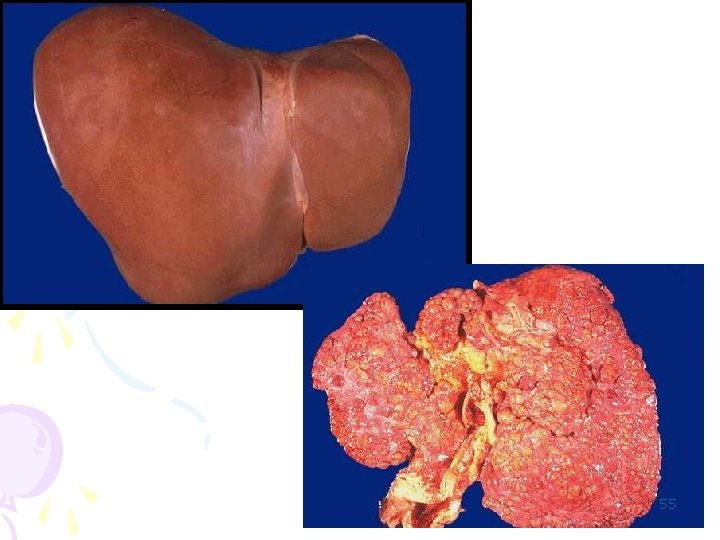
CIRRHOSIS; It is common end result of many chronic liver disorders. Diffuse disorder of liver characterised by: u Complete loss of normal architecture, u Replaced by extensive fibrosis with, u Regenerating parenchymal nodules. 50

Etiology of Cirrhosis • • • Alcoholic liver disease 60 -70% Viral hepatitis 10% Biliary disease 5 -10% Primary hemochromatosis 5% Cryptogenic (unknown origin) cirrhosis 10 -15% • Wilson’s, 1 AT deficiency rare 51

Pathogenesis: • Diffuse liver injury leading to necrosis. – (Alcohol, virus, drugs, toxins, genetic etc. ) • • • Chronic inflammation & healing (hepatitis). Bridging fibrosis – loss of architecture. Regeneration nodules. Obstruction to blood flow & shunts. Portal hypertension spleen, varices Liver failure debilitation, jaundice, ascites, edema, bleeding. • Hormone imbalance testes atrophy gynecomastia. 52

• Fibrosis – delicate bands – disruption of parenchymal architecture of the entire liver by interconnecting fibrous scars. • Parenchymal nodules – created by regeneration of hepatocytes. • The nodules – micronodules (less than 3 mm in diameter) – macronodules (3 mm to several centimeters in diameter). Cirrhotic deaths • (1) progressive liver failure, • (2) a complication related to portal hypertension • (3) the development of hepatocellular carcinoma. 53
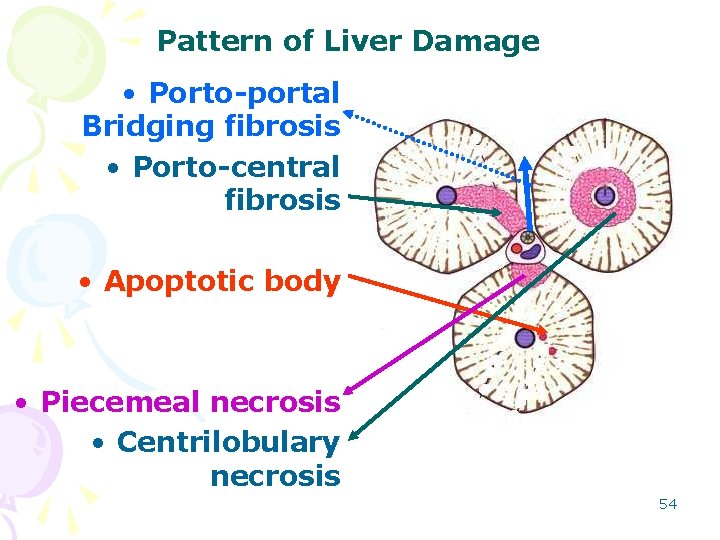
Pattern of Liver Damage • Porto-portal Bridging fibrosis • Porto-central fibrosis • Apoptotic body • Piecemeal necrosis • Centrilobulary necrosis 54
55
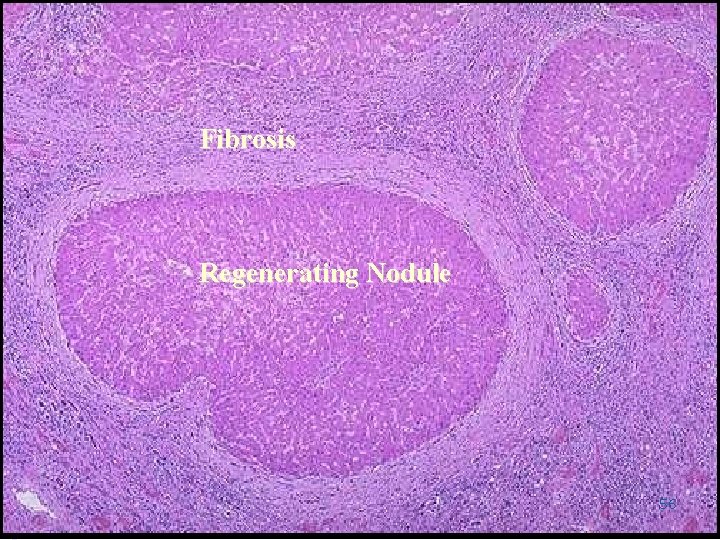
Fibrosis Regenerating Nodule 56

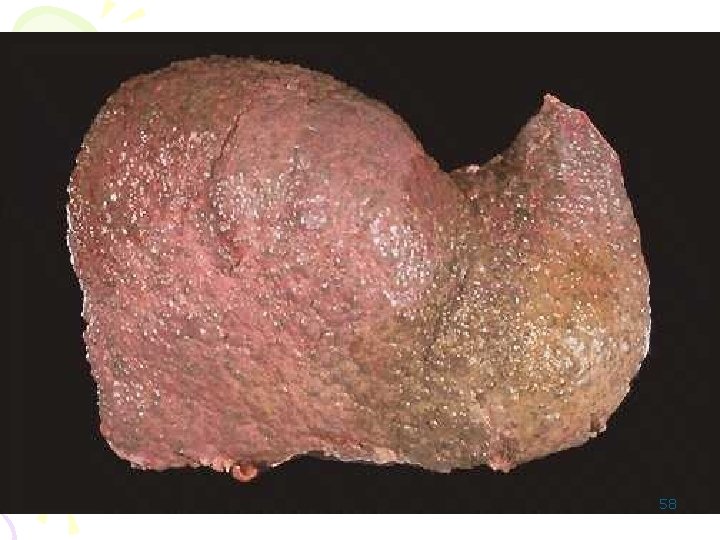
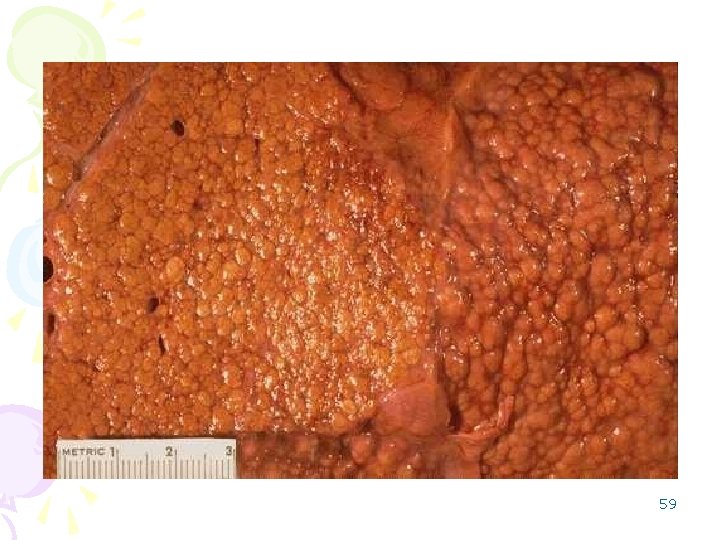
Micronodular cirrhosis • Most of the nodules are smaller than 0. 3 cm, • the fibrous-scar bands are relatively thin. • Etiology: – alcoholism, – hemochromatosis, – primary-autoimmune biliary cirrhosis, – biliary infection/obstruction. 57
58
59

Macronodular cirrhosis • Most of the nodules are larger than 0. 3 cm, • the fibrous-scar bands are relatively thin. • Etiology: – chronic hepatitis, – Wilson's disease, – galactosemia, Ø -1 antitrypsin deficiency – alcoholic's micronodular liver (after a few years). 60
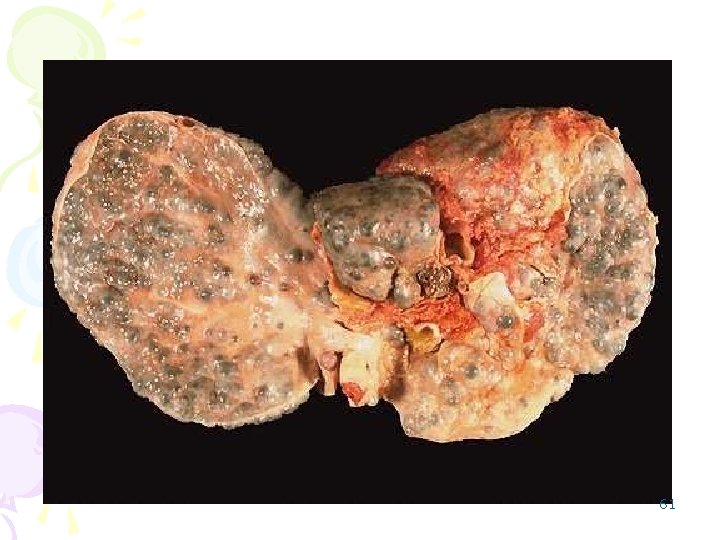
61
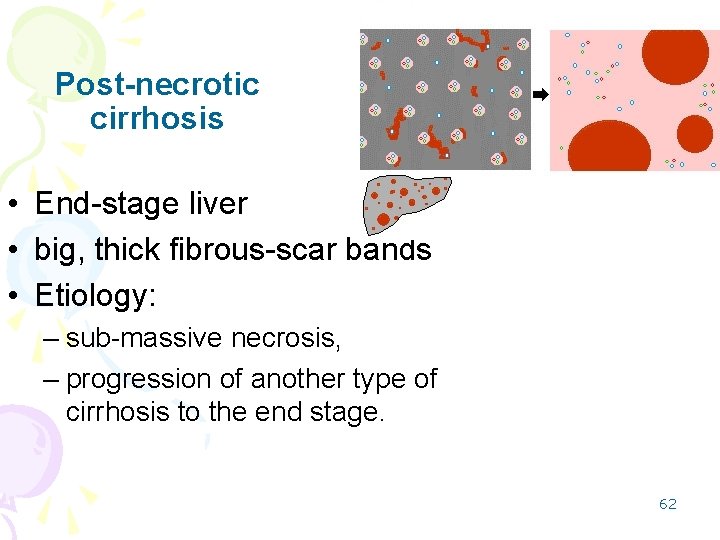
Post-necrotic cirrhosis • End-stage liver • big, thick fibrous-scar bands • Etiology: – sub-massive necrosis, – progression of another type of cirrhosis to the end stage. 62

Portal hypertension in cirrhosis: • increased resistance to portal flow at the level of the sinusoids • compression of central veins by perivenular fibrosis • expansile parenchymal nodules. 63

• Major clinical consequences: – (1) ascites, – (2) the formation of portosystemic venous shunts, – (3) congestive splenomegaly, – (4) hepatic encephalopathy. 64

1. Ascites • Excess fluid in the peritoneal cavity, • contain a scant number of mesothelial cells and mononuclear leukocytes, • neutrophils suggests secondary infection, • cells point to possible disseminated intra-abdominal cancer. 65
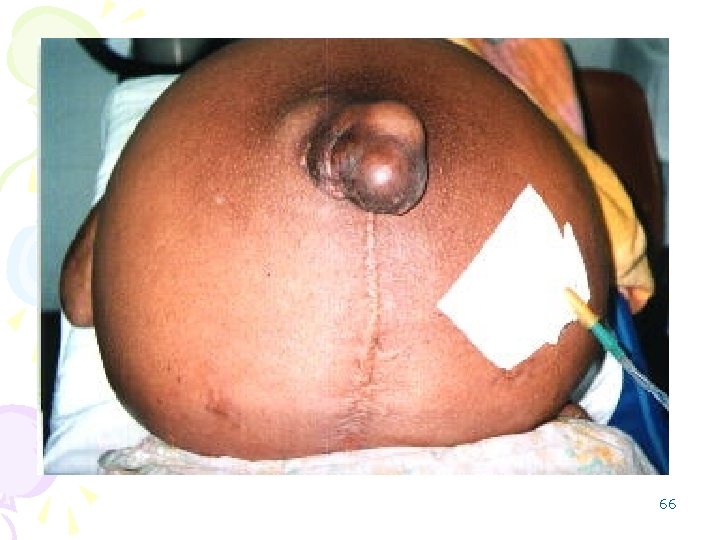
66

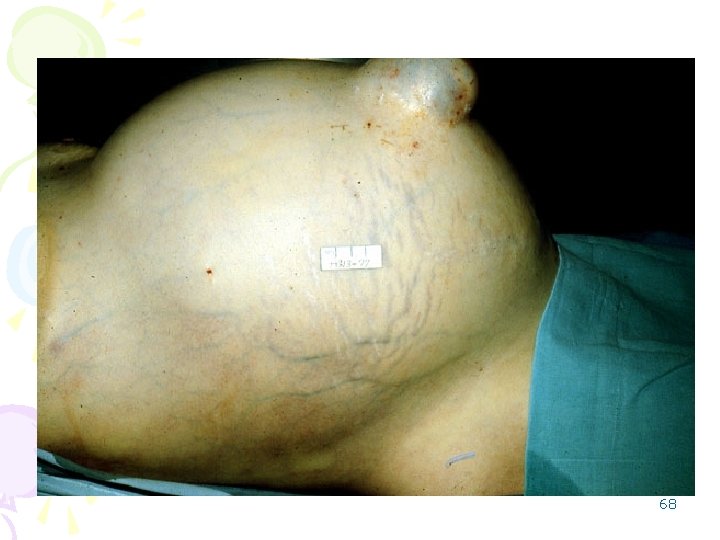
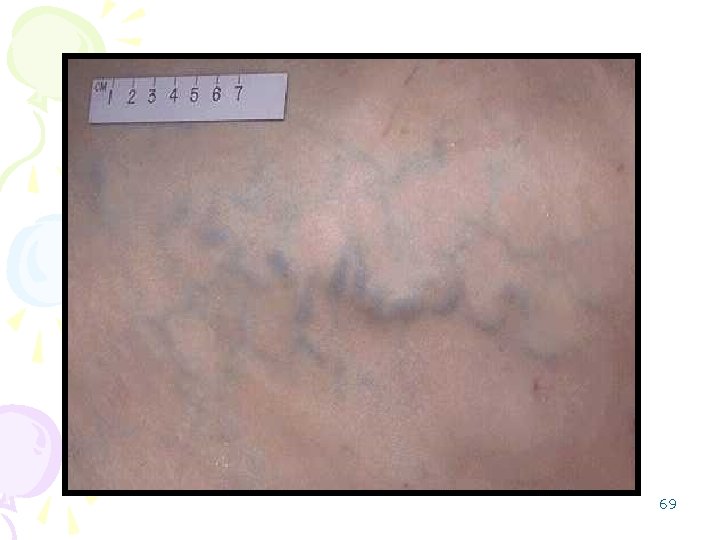
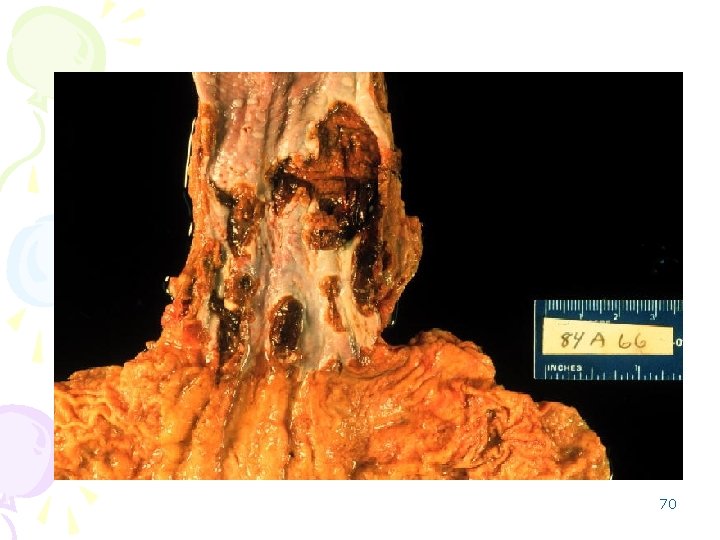
2. Portosystemic Shunts • Varices: – rectum (hemorrhoids), – cardioesophageal junction (esophagogastric varices), – retroperitoneum, – falciform ligament of the liver (periumbilical and abdominal wall collaterals). • abdominal wall collaterals appear as dilated subcutaneous veins extending from the umbilicus toward the rib margins (caput medusae); they are an important clinical hallmark of portal 67 hypertension.
68
69
70

3. Splenomegaly • Long-standing congestion congestive splenomegaly. • Massive splenomegaly hypersplenism hematologic abnormalities – Thrombocytopenia 71

4. Hepatic encephalopathy • Complication of acute and chronic liver failure. • Monitoring the hepatic encephalopathy by measuring blood ammonia. • Disturbances in consciousness, – ranging from subtle behavioral abnormalities to marked confusion • stupor to deep coma and death. • Morphologic changes in the brain: – edema, – astrocytic reaction. 72
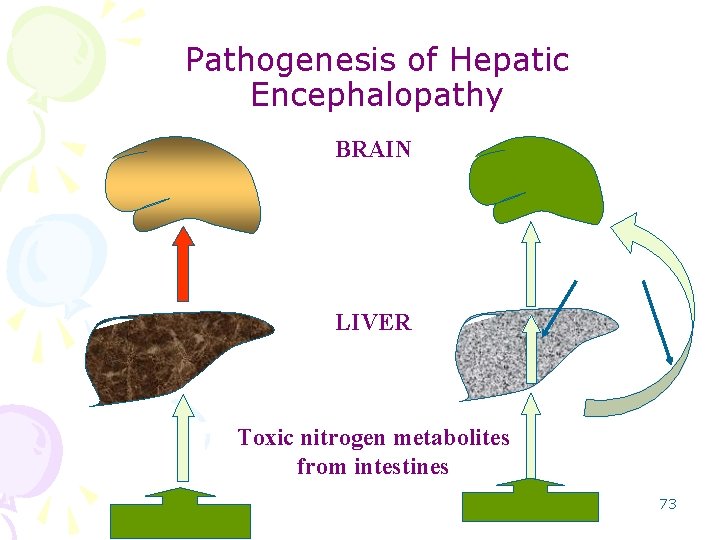
Pathogenesis of Hepatic Encephalopathy BRAIN LIVER Toxic nitrogen metabolites from intestines 73

Hepatorenal Syndrome • Renal failure in patients with severe liver disease. • Acute fulminant or advanced chronic hepatic disease circulatory collapse acute tubular necrosis renal failure. 74

The Pathology of Liver & Biliary System Part-2 75

PRIMARY NEOPLASMS of the LIVER • Tumor-like developments: – Nodular Hyperplasia • Benign tumors – Adenoma • Malignant tumors – Hepatocellular carcinoma – Cholangiocarcinoma – Hepatoblastoma 76

Benign Tumors Nodular Hyperplasias • Solitary or multiple benign hepatocellular nodules • in the absence of cirrhosis • well-demarcated but poorly encapsulated nodule • roughly spherical nodules of plump hepatocytes surrounded by rims of atrophic cells • no fibrosis. 77

Hepatic Adenomas • hepatocytes or bile duct epithelial cells, • More common in young women – who have used oral contraceptives and regress on discontinuance of use, • pale, yellow-tan, and frequently bilestained nodules, • composed of sheets and cords of cells – portal tracts are absent • have a tendency to rupture – particularly during pregnancy (under estrogenic stimulation), causing severe intraperitoneal hemorrhage. 78
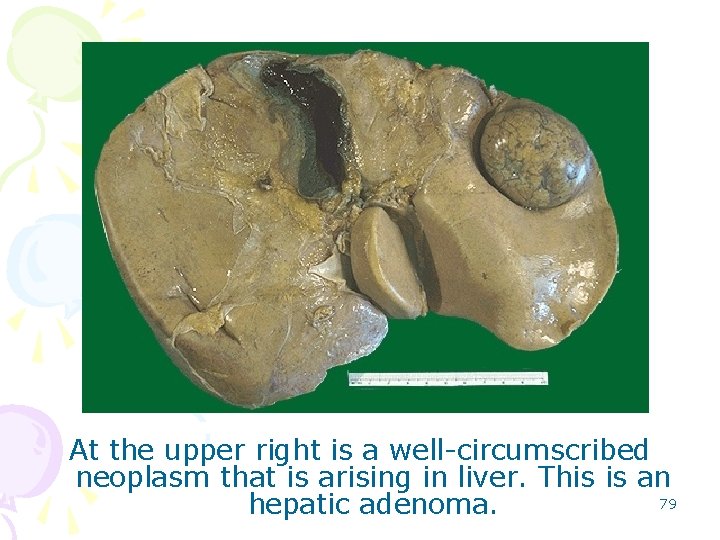
At the upper right is a well-circumscribed neoplasm that is arising in liver. This is an 79 hepatic adenoma.

• The cut surface of the liver reveals the hepatic adenoma. Note how well circumscribed it is. The remaining liver is a pale yellow brown because of fatty change from chronic alcoholism. 80
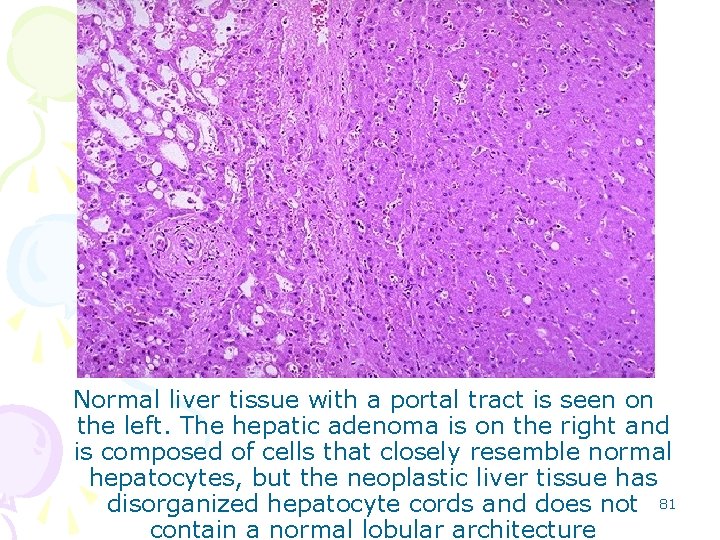
Normal liver tissue with a portal tract is seen on the left. The hepatic adenoma is on the right and is composed of cells that closely resemble normal hepatocytes, but the neoplastic liver tissue has disorganized hepatocyte cords and does not 81 contain a normal lobular architecture

Primary Malignancies of the Liver • Hepatocellular carcinoma • Cholangiocarcinoma 82

Hepatocellular carcinoma • Etiology: – hepatitis B and/or C viruses – cirrhotic liver – iron overload – aflatoxin – thorotrast – anabolic steroids 83
Grossly • single mass or multicentric • better-differentiated tumor greener (hepatocytes want to make bile). • Hepatocellular carcinomas, unlike most carcinomas, have a great propensity to invade veins. ****The four carcinomas which invade veins in preference to lymphatics: • • 1. Follicular carcinoma of the thyroid 2. Hepatocellular carcinoma 3. Renal cell carcinoma 4. Yolk sac carcinoma. 84
Histology Ø may look like nearly-normal liver, Ø or be wildly anaplastic, Ø bile production by the tumor cells (pathognomonic), Ø Mallory's hyaline (not really pathognomonic), Ø -1 antitrypsin inside cells, Ø stainable hepatitis B virus proteins, Ø stainable -fetoprotein (serum marker for hepatocellular carcinoma). 85
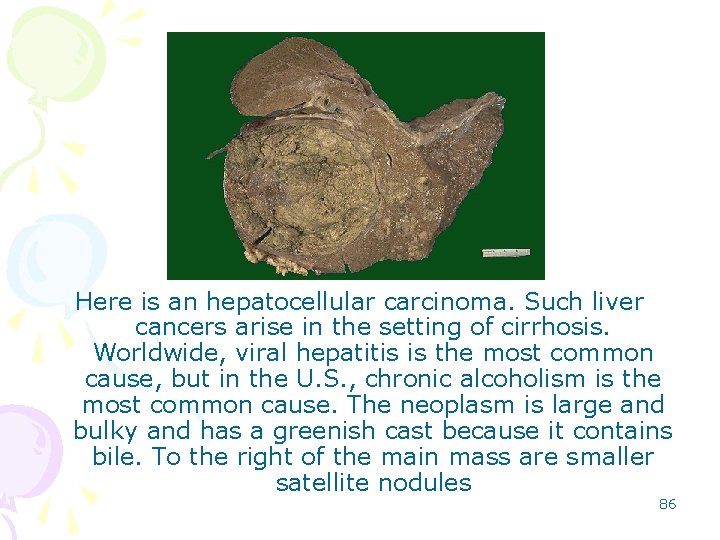
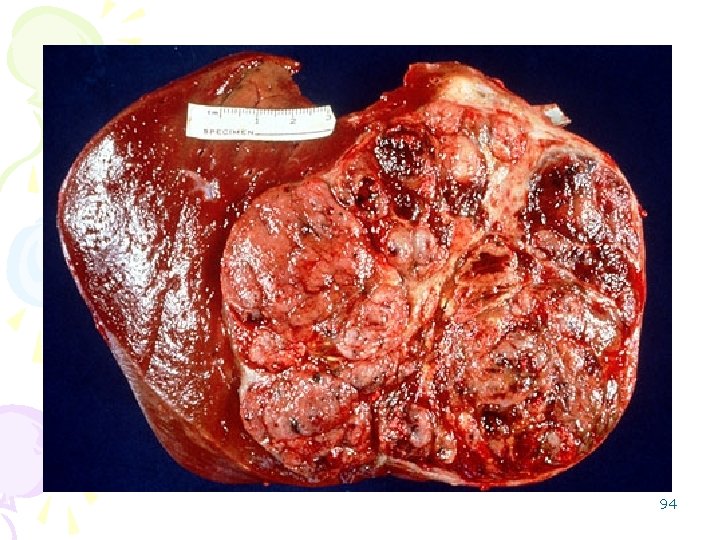
Here is an hepatocellular carcinoma. Such liver cancers arise in the setting of cirrhosis. Worldwide, viral hepatitis is the most common cause, but in the U. S. , chronic alcoholism is the most common cause. The neoplasm is large and bulky and has a greenish cast because it contains bile. To the right of the main mass are smaller satellite nodules 86
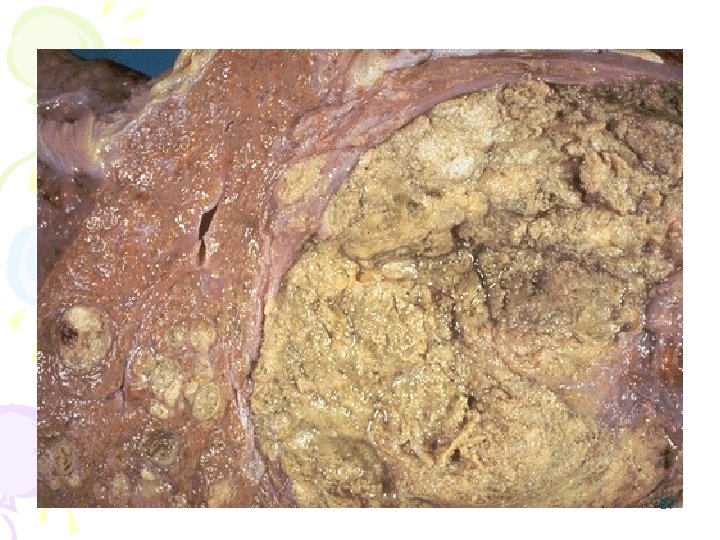
87
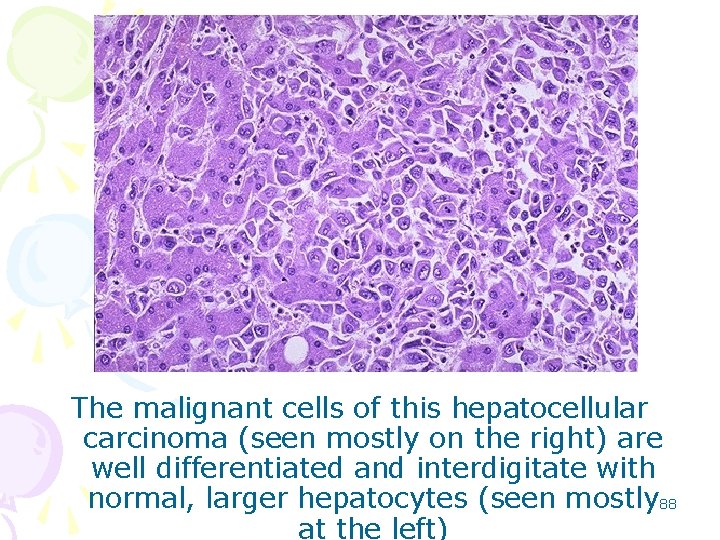
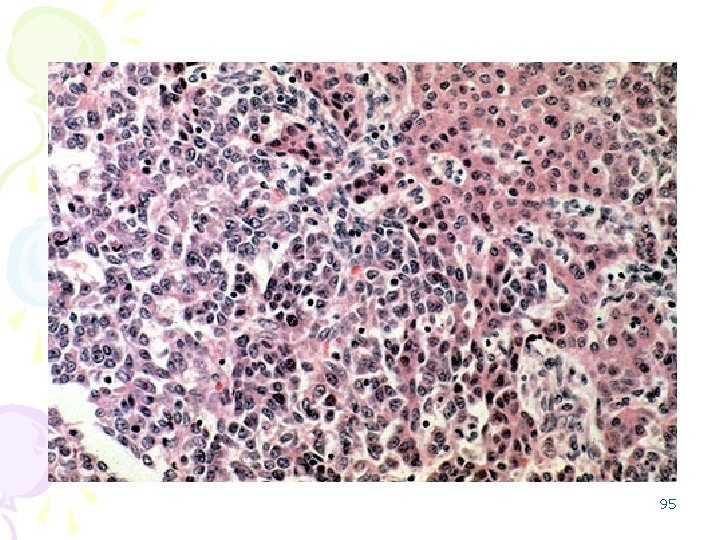
The malignant cells of this hepatocellular carcinoma (seen mostly on the right) are well differentiated and interdigitate with normal, larger hepatocytes (seen mostly 88 at the left)
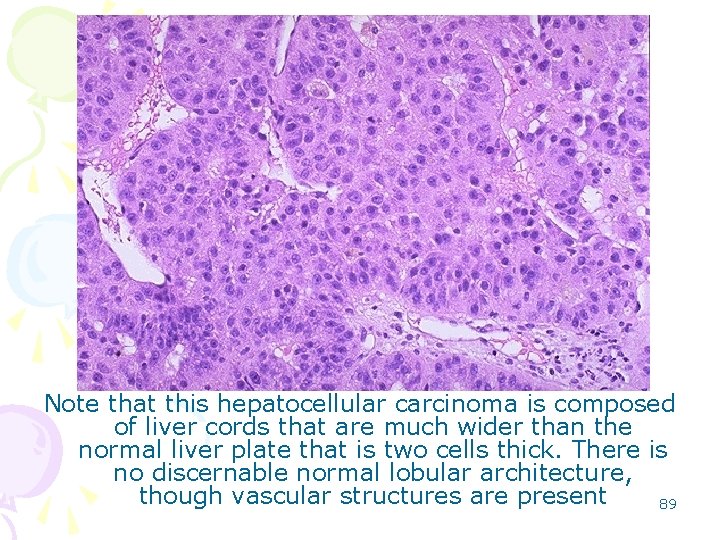
Note that this hepatocellular carcinoma is composed of liver cords that are much wider than the normal liver plate that is two cells thick. There is no discernable normal lobular architecture, though vascular structures are present 89
Cholangiocellular carcinoma • occur within the liver, or as a mix with hepatocellular carcinoma. • desmoplastic adenocarcinoma, • often mucin-positive. • The cells do not secrete bile. • The risk factors for this lesion are – (1) thorotrast exposure, – (2) liver fluke infestation, – (3) idiopathic sclerosing cholangitis, – (4) Caroli's disease. 90

• A Cholangiocarcinoma is: – (1) a unifocal (usually large) mass; – (2) multifocal, widely distributed nodules of variable size; – (3) a diffusely infiltrative cancer, permeating widely and sometimes involving the entire liver. • Cholangiocarcinomas are rarely bile stained because differentiated bile duct epithelium does not synthesize pigmented bile. • Microscopy: Cholangiocarcinomas resemble adenocarcinomas • often markedly desmoplastic, • Metastases: – Hematogenous metastases to the lungs, bones (mainly vertebrae), adrenals, brain. 91

The carcinoma at the left has a glandular appearance that is most consistent with a cholangiocarcinoma. A liver cancer may have both hepatocellular as well as cholangiolar differentiation. Cholangiocarcinomas do not make bile, but the cells do make mucin, and they can be almost impossible to distinguish from metastatic adenocarcinoma on biopsy or fine needle 92 aspirate

Hepatoblastoma Ø Hepatoblastoma is the most common primary malignant hepatic tumor in children Ø -fetoprotein is high, Ø FSH/LH often high. 93
94
95

Mesenchymal neoplasms of Liver: 1. mesenchymal hamartoma is an uncommon lesion of childhood, usually diagnosed in the first two years of life. There is progressive painless abdominal enlargement; radiographic studies reveal a large mass with multiple cysts. There is a striking male predominance. The tumor is large (up to 21 cm) and solitary. It is composed of a gelatinous mesenchyme and cysts or poorly formed cystic spaces filled with clear fluid 96
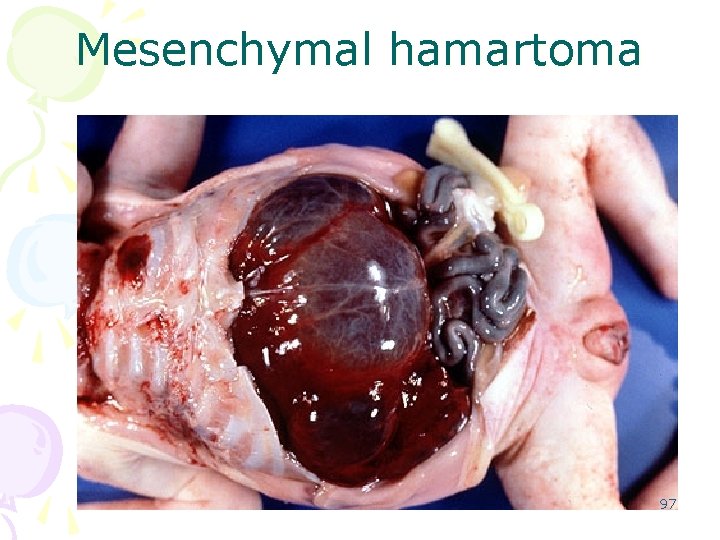
Mesenchymal hamartoma 97

2 -Infantile hemangioendothelioma • one of the more common childhood hepatic tumors • follow a benign course and usually spontaneously involute • discovered within the first six months of life • other organs such as skin, lung, lymph nodes, and bone may be involved 98
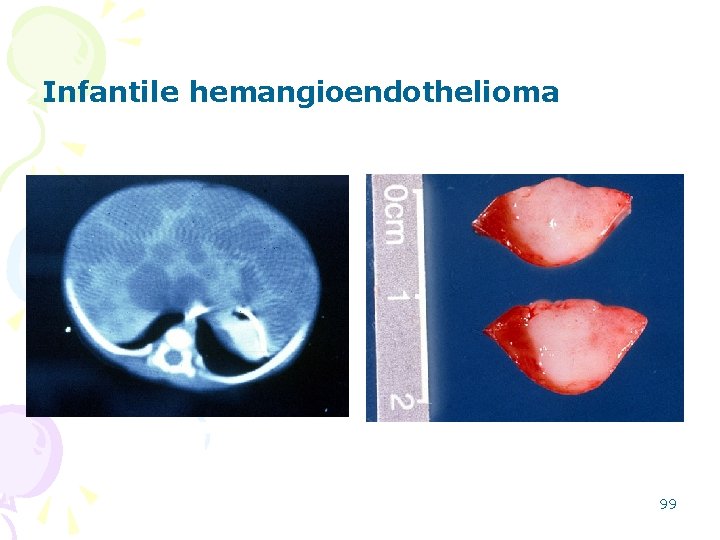
Infantile hemangioendothelioma 99

3 -Hemangiomas • common incidental findings, being present in over 1% of autopsies. • Most are totally asymptomatic. The 15% of individuals with these lesions who have symptoms present with the effects of a mass compressing adjacent structures. • Almost all of these patients have giant hemangiomas, defined as being more than 10 cm in diameter • more common in women. 100 • 10% are multiple

Hemangioma 101
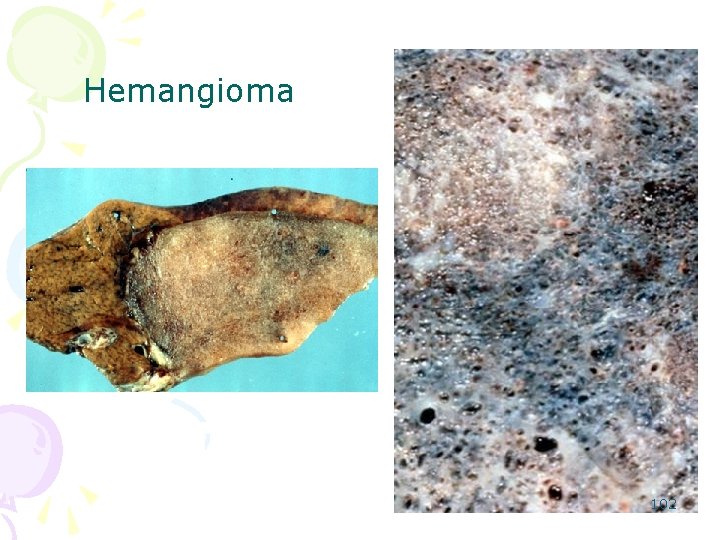
Hemangioma 102
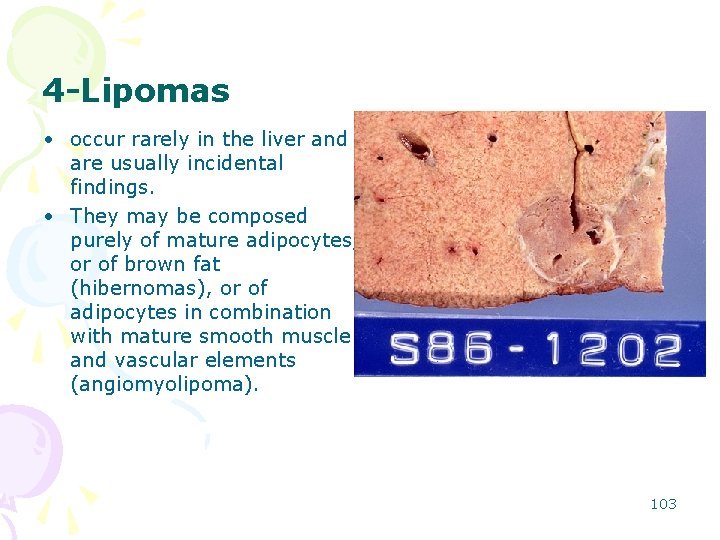
4 -Lipomas • occur rarely in the liver and are usually incidental findings. • They may be composed purely of mature adipocytes, or of brown fat (hibernomas), or of adipocytes in combination with mature smooth muscle and vascular elements (angiomyolipoma). 103
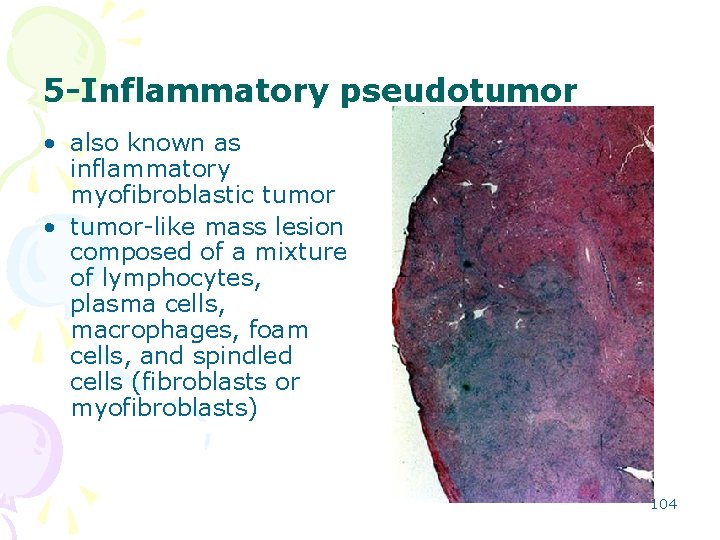
5 -Inflammatory pseudotumor • also known as inflammatory myofibroblastic tumor • tumor-like mass lesion composed of a mixture of lymphocytes, plasma cells, macrophages, foam cells, and spindled cells (fibroblasts or myofibroblasts) 104

5 -Miscellaneous benign tumors include lymphangiomas, leiomyomas, fibromas, and myxomas • They occur quite rare 105

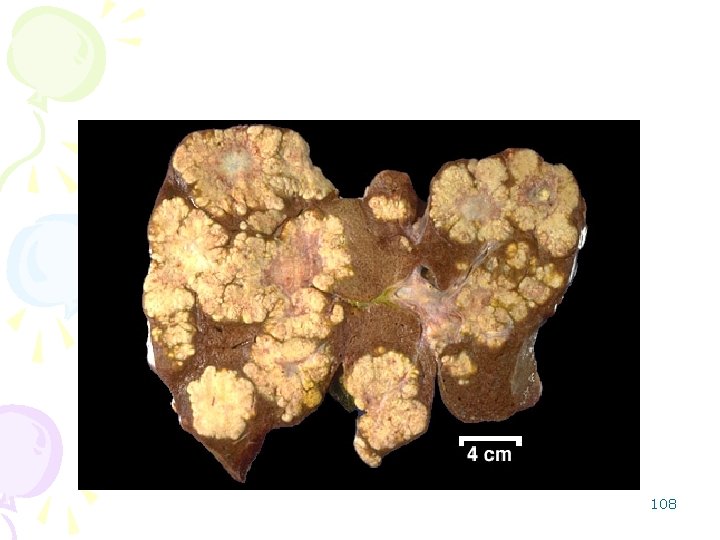
Metastatic Tumors • Multiple nodular hepatomegaly • Massive/diffuse icterus • More common than primary neoplasia: – breast, – lung, – colon, – leukemias and lymphomas. 106

Note the numerous mass lesions that are of variable size. Some of the larger ones demonstrate central necrosis. The masses are metastases to the liver. The obstruction from such masses generally elevates alkaline phosphatase, but not all bile ducts are obstructed, so hyperbilirubinemia is typically not present. Also, the transaminases are usually not greatly elevated 107
108
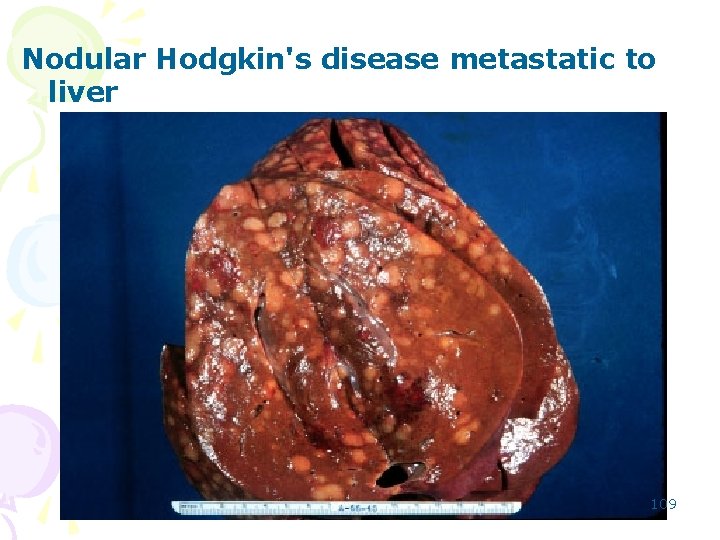
Nodular Hodgkin's disease metastatic to liver 109
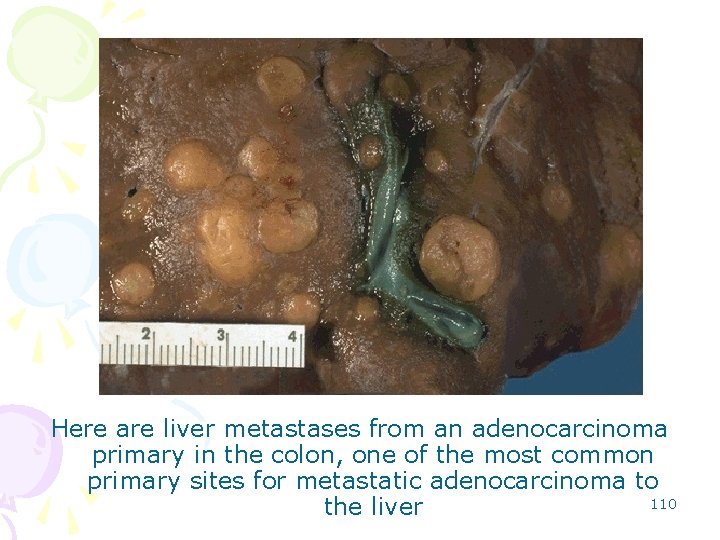
Here are liver metastases from an adenocarcinoma primary in the colon, one of the most common primary sites for metastatic adenocarcinoma to 110 the liver
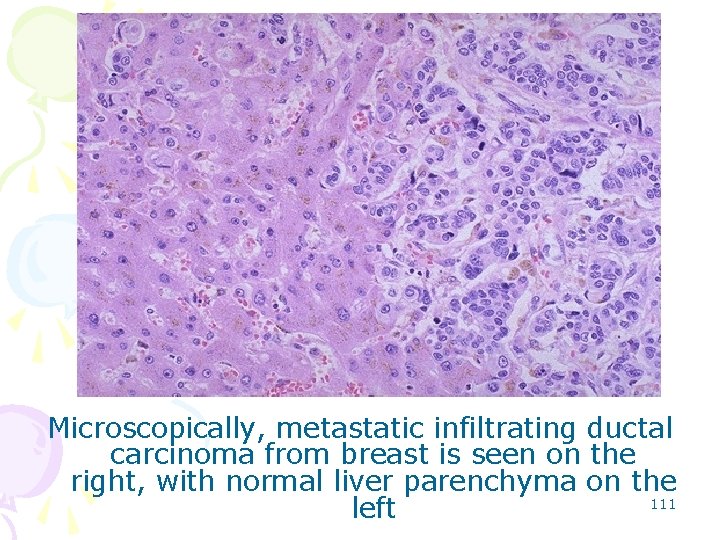
Microscopically, metastatic infiltrating ductal carcinoma from breast is seen on the right, with normal liver parenchyma on the 111 left

Biliary Tract Pathology 112
113

Gallstones • Cholesterol stones: – pure or contaminated with calcium, oxalate, and/or bilirubin – result from bile becoming super-saturated with cholesterol – yellow and various in size • some large barrel-shape casts of the gallbladder. 114
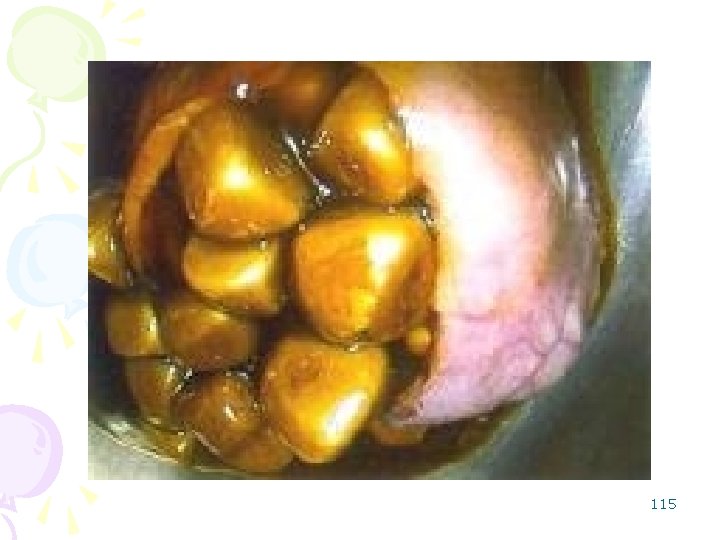
115

• Bilirubin stones ("mulberry stones"; "pigment stones") – calcium bilirubinate – bile becoming super-saturated with unconjugated bilirubin, • when there is hemolysis (sickle cell, hemoglobin C, spherocytosis, autoimmune Coombs-positive anemia, thalassemias). 116
Complications • Obstructions: – the cystic duct causing pain ("biliary colic") inviting cholecystitis or mucocele formation; – the common bile duct –> causing pain ("biliary colic") inviting ascending cholangitis; – the pancreatic duct causing pancreatitis. • Erosion: – through the wall of the gallbladder and the duodenum, – then passing along and getting hung up at the ileocecal valve ("gallstone ileus") • Cancer of the gallbladder. 117

Acute cholecystitis • Inflammation of the gallbladder, usually containing gallstones, usually with infection. • Etiology: • E. coli, • Enterococci, • clostridia , • salmonella (typhoid is carried in the gallbladder). 118

Macroscopy: – Red, swollen, and tense. – pus on the inside (even an "empyema"), – fibrin all over the outside, – even gangrene of the wall. – There almost always gallstones. Microscopy: – Hypertrophy and hyperplasia of the smooth muscle – "Rokitansky-Aschoff sinuses“: • pseudo-diverticula where the mucosa has pooched into or through the muscularis propria. can be seen in normal gallbladders, too. 119

• Cholesterolosis (strawberry gallbladder): – – maybe 5% of autopsies. Little clusters of cholesterol-laden macrophages just under the epithelium, looking like strawberry seeds. • Inflammatory polyps: benign; on the gallbladder wall. • Mucocele (hydrops): – filled with mucus instead of bile, – its cystic duct has become obstructed. – The gallbladder won't visualize on x-ray. • Benign tumors: rare. 120

Carcinoma of the gallbladder – Adenocarcinomas are most common. Risk factors include: – gallstones – chronic carrying of typhoid or paratyphoid bacteria increases the risk by about fifty times 121
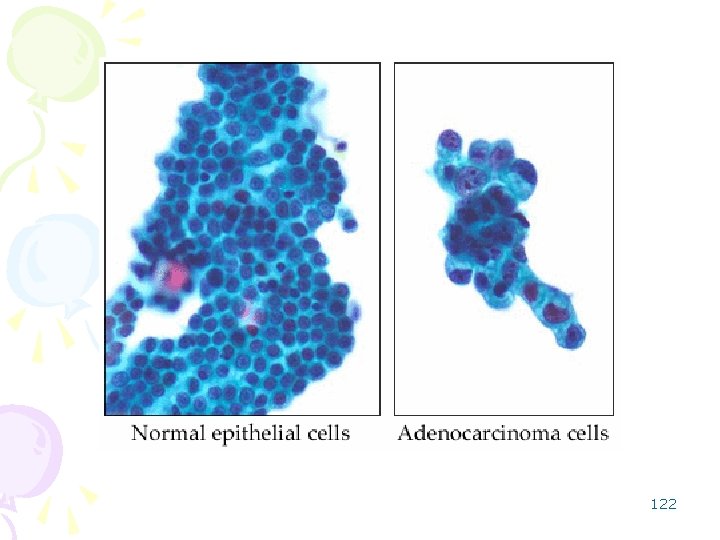
122

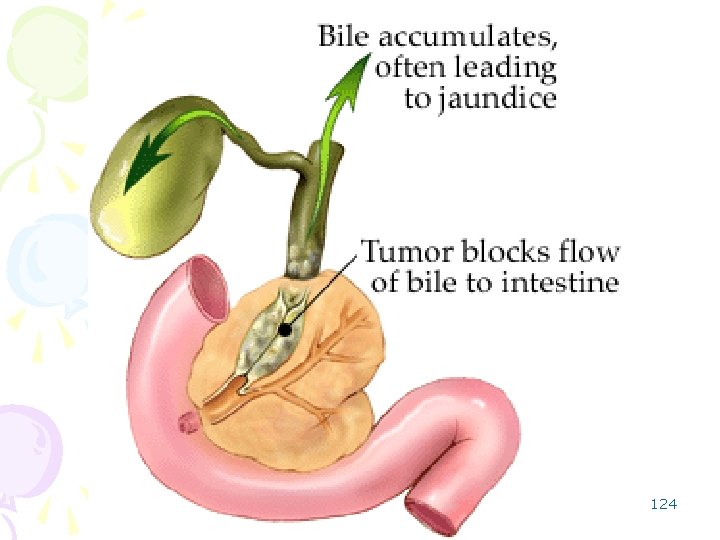
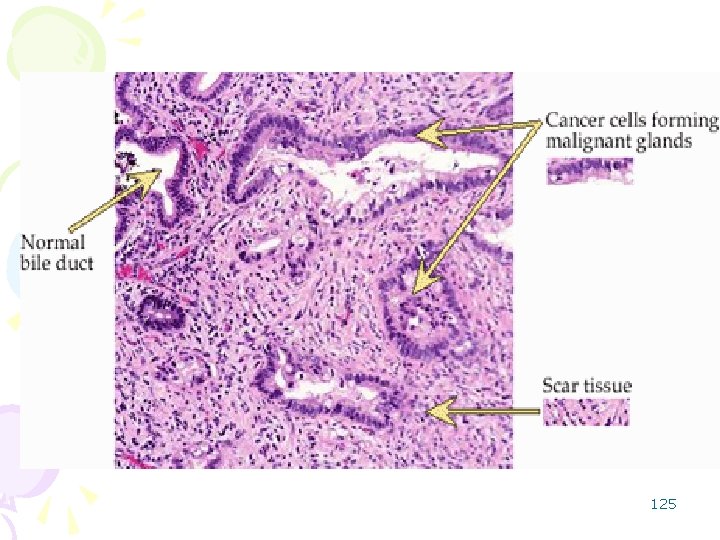
Carcinoma of the bile ducts • Adenocarcinoma is most common and produce obstructive jaundice • Carcinoma of the extrahepatic and intrahepatic bile ducts is slightly more common in males, and patients usually present in their 50's. Risk factors include: • History of Primary Sclerosing Cholangitis • Congenital abnormalities (abnormalities one is born with) of the bile ducts -- these include choledochal cysts (dilation of the common bile duct) and Caroli's disease (dilation of the intrahepatic bile ducts • Benign tumors of the bile ducts • Hepatobiliary parasitic infection • Toxic exposures -- thorium dioxide (Thorotrast), used as a contrast dye in radiologic procedures between 1930 -1950, has been shown to promote cancers in the liver and bile ducts. • ulcerative colitis 123
124
125

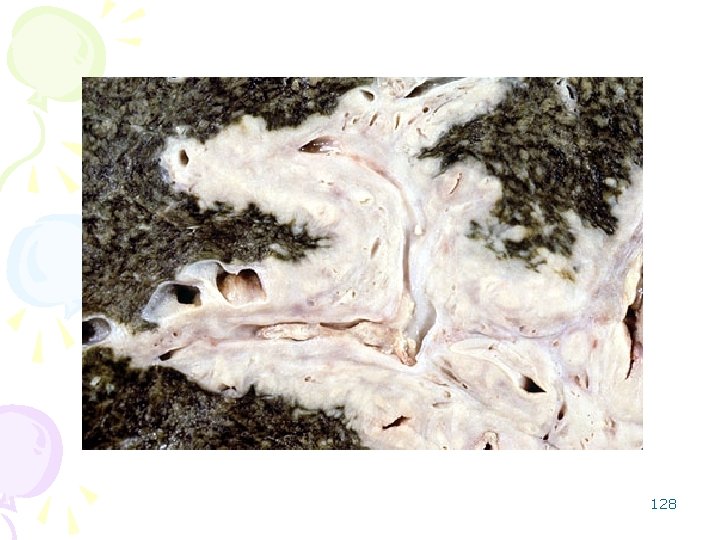
• Common sites : – ampulla of Vater, – junction of the hepatic and common ducts. • Cancer of the ampulla tend to be mucin-producing. • Intrahepatic Cholangiocarcinoma: Klatskin tumor • Cancers arising elsewhere from among the bile ducts tend to be desmoplastic. • Itching – makes these patients particularly miserable. 126
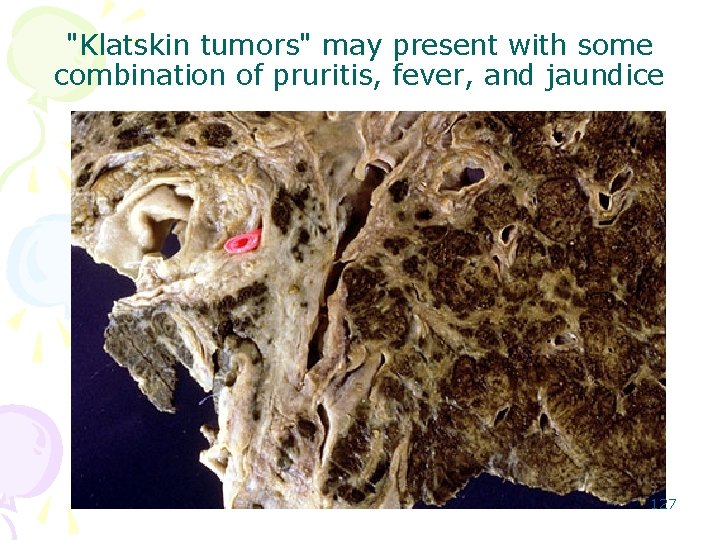
"Klatskin tumors" may present with some combination of pruritis, fever, and jaundice 127
128

Biliary Tract Diseases Secondary Biliary Cirrhosis • Prolonged obstruction profound alteration of the liver • Causes: – gallstone in the common bile duct; – biliary atresia, – malignancies of the biliary tree – malignancies of the head of the pancreas, – strictures resulting from previous surgical procedures. 129

Gross • Periportal fibrosis • secondary biliary cirrhosis. • The liver • – hard, with a finely • granular appearance. • – extraordinary yellowgreen pigmentation (Cholestasis). • • Marked icteric discoloration of body tissues and fluids. Microscopy Distended bile ducts containing bile, Inflammation, Edema in portal tracts Degeneration of hepatocytes, and the formation of bile lakes, Ascending bacterial infection neutrophilic infiltration of bile ducts cholangitic abscesses. 130

Primary Biliary Cirrhosis • Fatal cholestatic liver • Antimitochondrial autoantibodies disease. – in more than 90% of – Chronic, patients. – Progressive. • Female-to-male 6: 1. – Destruction of intrahepatic bile ducts, • Age of onset is between 20 and 80 – portal inflammation, years, – Scarring. – with the peak Eventual incidence between 40 development of and 50 years. cirrhosis and liver 131 failure.

• Four histologic stages: • • 1. The florid duct lesion – (granulomatous destruction of interlobular bile ducts) • 2. Ductular proliferation with periportal hepatitis • 3. Scarring, with bridging necrosis and septal fibrosis • 4. Cirrhosis Extrahepatic manifestations associated with PBC include: – the sicca complex of dry eyes and mouth (Sjögren’s syndrome), – scleroderma, – thyroiditis, – rheumatoid arthritis, – Raynaud’s phenomenon, – membranous glomerulonephritis, – celiac disease. 132

Primary sclerosing cholangitis (PSC) • Inflammation (fibrosing cholangitis of bile ducts): – lymphocytic infiltrate, – obliterative fibrosis (“onionskin fibrosis”) , – segmental dilatation: irregular strictures and dilatations of affected bile ducts, – progressive atrophy of the bile duct epithelium, – obliteration of the lumen • Commonly seen in association with inflammatory bowel disease (Ulcerative Colitis). 133

Anomalies of the Biliary Tree • Altered architecture of the intrahepatic biliary tree. • Von Meyenburg Complexes: bile duct microhamartomas • Polycystic Liver Disease: multiple diffuse cystic lesions (scattered few to hundreds). • Congenital Hepatic Fibrosis: portal tracts are enlarged by irregular and broad bands of collagenous tissue, forming septae and dividing the liver into irregular islands. • Caroli’s Disease: larger ducts of the intrahepatic biliary tree are segmentally dilated (cystic; may contain inspissated bile). 134
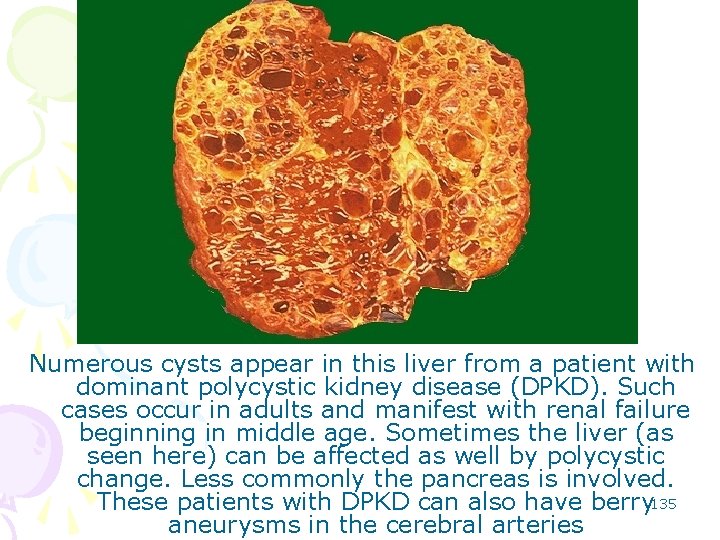
Numerous cysts appear in this liver from a patient with dominant polycystic kidney disease (DPKD). Such cases occur in adults and manifest with renal failure beginning in middle age. Sometimes the liver (as seen here) can be affected as well by polycystic change. Less commonly the pancreas is involved. These patients with DPKD can also have berry 135 aneurysms in the cerebral arteries
- Slides: 135