The Nervous System Nursing Care of Patients with























































- Slides: 64

The Nervous System Nursing Care of Patients with Central Nervous System Disorders

Meningitis �Pathophysiology �Infection / Inflammation of Brain & Spinal Cord �Viral- flu-like s/s, last 1 -2 wks �Bacterial- may begin as URI, enters blood and invade CNS, causes meninges to become inflamed and ICP to increase. May cause vessel occulsion and necrosis of brain, may affect cranial nerves.

Signs & Symptoms �Severe Headache �Fever �Photophobia �Petechial Rash �Nuchal Rigidity �Positive Kernig’s and Brudzinski’s Signs �Nausea and Vomiting �Encephalopathy

Kernig’s & Brudzinski’s

Complications �Seizures �Cranial Nerve Damage �Occasional Permanent Neurological Deficits �Dx with Lumbar puncture and C&S

Therapeutic Interventions Antibiotics Antipyretics Cooling Blanket PRN Dark, Quiet Environment Monitor VS, neuro cks Monitor for s/s of >ICP and seizure activity Analgesics Corticosteroids Antiemetics Isolation if Contagious

Encephalitis �Pathophysiology �Inflammation of Brain Tissue- affects cerebrum, brainstem and cerebellum �May cause Nerve Damage, Edema, Necrosis �IICP �May be viral , bacterial, parasitic, or vaccines

Signs & Symptoms Headache Fever Nausea and Vomiting Nuchal Rigidity Confusion Decreased LOC and mental status change are s/s of >ICP Seizures Photophobia Ataxia Tremors Coma Death

Complications �Cognitive Disabilities �Personality Changes �Ongoing Seizures �Blindness �Dx: CT, EEG, LP

Therapeutic Interventions Analgesics Anticonvulsants Antipyretics Corticosteroids Antivirals Sedatives Neurological Assessment Symptomatic Care

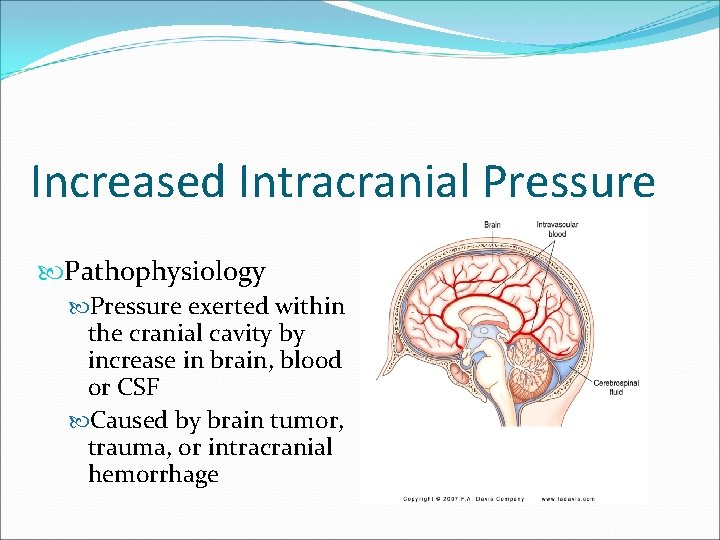
Increased Intracranial Pressure Pathophysiology Pressure exerted within the cranial cavity by increase in brain, blood or CSF Caused by brain tumor, trauma, or intracranial hemorrhage

Signs & Symptoms �Restlessness >Confusion > coma �Irritability �Decrease in LOC- earliest s/s �Hyperventilation �Pupil Changes �Cushing’s Response- late s/s

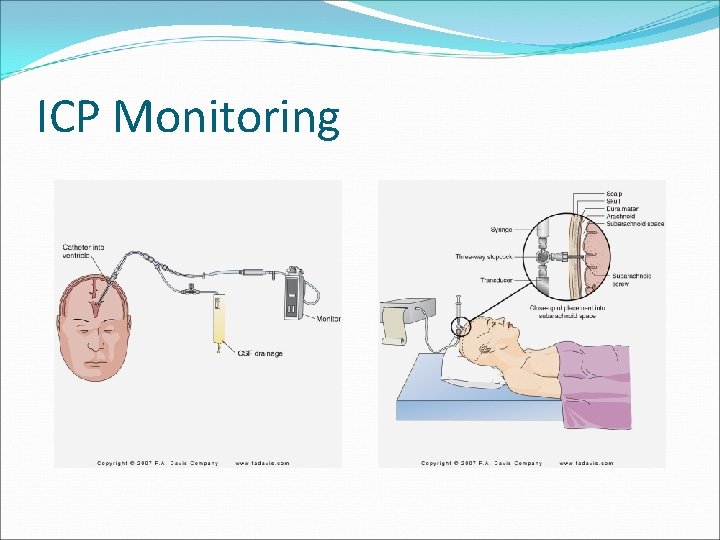
ICP Monitoring �External Ventricular Drain- catheter into the ventricle allows CSF drainage and monitor ICP �Subarachnoid Bolt-easy to place, but easily occluded. �Intraparenchymal Monitor- placed directly into brain tissue, most accurate but does not drain CSF and can become occluded

ICP Monitoring

Nursing Diagnoses: CNS Infections �Pain �Hyperthermia �Disturbed Thought Processes �Self Care Deficit �Impaired Physical Mobility �Risk for Injury: Seizures

Headaches �Tension-persistent contraction of scalp and facial muscles causing tenderness and HA. �Result of stress and sustained muscle contraction of head/neck. �May be r/t premenstrual syndrome, anxiety, emotional distress, and depression �Use relaxation exercises, massage affected muscles, rest, heat, non-narcotic analgesics

Migraines �Caused by cerebral vasoconstriction followed by vasodilation �May have aura, throbbing, pounding pain usually on one side of head, exacerbated by noise and light �Triggers may include specific foods, noise, bright light, alcohol and stress �Tx: quiet, dark environment, cold compress, medications (Imitrex, Zomig, Ergot)

Cluster Headaches �Occurs in clusters during time span of days to weeks. Caused by anxiety, stress, and vascular disturbances, worse with use of alcohol. �Usually begins suddenly, same time of night, unilateral, throbbing, severe pain �Tx: quiet dark environment. Cold compress, meds. NSAIDs and antidepressants

Nursing Care for Headaches �Assessment �WHAT’S UP? (Where, how, Aggravating, timing, severity, other s/s, pt perception) �Patient Education �Keep HA Diary �Record Triggers, Timing, Symptoms �Teach Relaxation and Stress Reduction �Teach : Medications

Seizures �Sudden, abnormal, and excessive electrical discharges from the brain that can change motor or autonomic function, consciousness, or sensation.

Classification �Partial (Simple) �Begin on One Side of Cerbral Cortex �Generalized (complex) �Both Hemispheres Involved �Both may have aura (visual, auditory, olfactory disturbance)

Signs & Symptoms cont’d Partial Seizures (Simple) begin on 1 side of brain Automatisms- dream like state Maintain Consciousness Usually < 1 Minute Paresthesias- numbness, tingling Visual Disturbances Generalized (Complex Partial) both hemispheres involved Lose Consciousness, 2 – 15 minutes Two types

Signs & Symptoms cont’d �Generalized Seizures �Absence (Petit Mal) � Staring �Tonic Clonic � May Have Aura � Usually Lose Consciousness � Rigidity Followed by Muscle Contraction and Relaxation � Incontinence � Postictal Period Dx: EEG, look for underlying cause Tx: anticonvulsants, surgical resection

Emergency Care: Seizure �Pad Side Rails �Prevent Injury �Maintain an open Airway �Do Not Restrain �Turn on Side to Prevent Aspiration �Suction PRN �Observe and Document

Status Epilepticus � 30 Minutes of Seizure Activity �Therapeutic Interventions �Ensure Airway and Oxygenation �Administer IV Diazepam �Teach patient – sudden withdrawal of anticonvulsants can lead to status epilepticus

Traumatic Brain Injury Trauma Hemorrhage Contusion- bruising Laceration Most common cause is MVA, falls, assault, sports-related injury Think immobilize if trauma Can Cause Cerebral Edema Hyperemia Hydrocephalus Brain Herniation Death

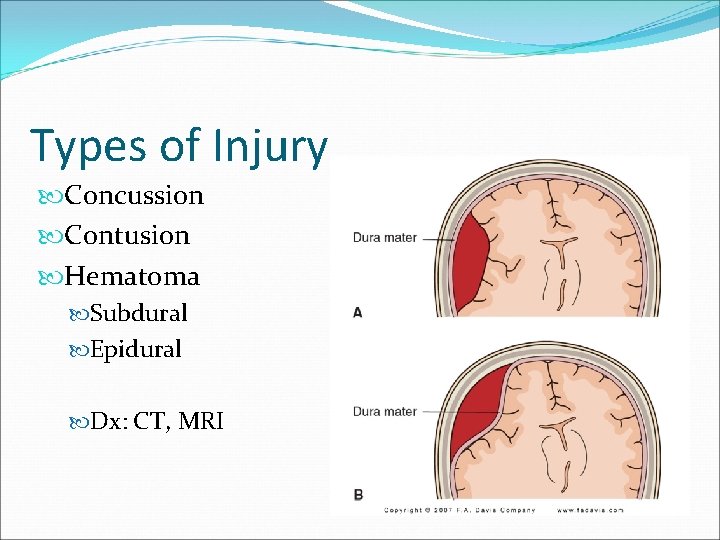
Types of Injury Concussion Contusion Hematoma Subdural Epidural Dx: CT, MRI

Therapeutic Interventions �Surgical Removal of Hematoma �Control IICP �ICP Monitoring �Osmotic Diuretic- mannitol �Mechanical Hyperventilation �Therapeutic Coma

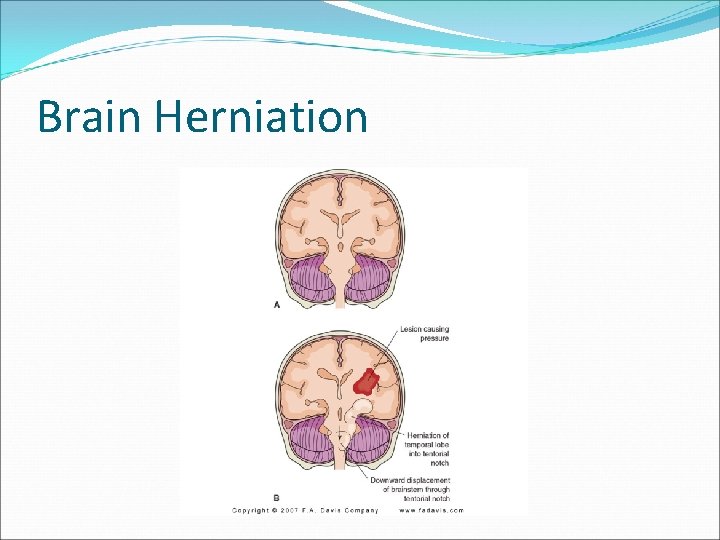
Complications of TBI �Brain Herniation �Diabetes Insipidus �Acute Hydrocephalus �Labile Vital Signs �Posttraumatic Syndrome �Cognitive and Personality Changes

Brain Herniation

Nursing Diagnoses �Ineffective Cerebral Tissue Perfusion- monitor VS, GCS, implement measures to prevent ICP �Ineffective Airway Clearance- Monitor airway and BS, Limit suction, >HOB 30, turn pt freq to mobilize secretions �Ineffective Breathing Pattern- monitor Bs, resp rate, O 2 sat, ABG’s

Brain Tumor �Pathophysiology �Neoplastic growth of the Brain or Meninges �Primary or secondary (Metastatic) �Compress or Infiltrate Brain Tissue �Cause IICP �Begin with vague s/s HA, visual changes, seizures, motor and sensory changes �Dx: MRI, CT, angiogram �Tx: Radiation, Chemo, surgery, symptom control

Complications/ Nursing Dx Seizures, HA Aphasia Memory Impairment Cognitive Changes Ataxia, lethargy Coma, then death Disturbed thought process Self-care deficit Pain Impaired physical mobility Risk for injury

Intracranial Surgery �Indicated for Hematomas, tumor, trauma, malformation, and seizures �Craniotomy- surgical opening in the skull � Craniectomy- removal of part of cranial bone � Crainoplasty- repair of bone or replacement with prosthesis

Preoperative Care �Lab work-up and anesthesia evaluation �Patient Education helps control anxiety �ICU visit �Surgery may last 2 hrs for biopsy to 12 hrs or longer for procedure

Postoperative Care �Nursing Diagnoses �Risk for Ineffective Cerebral Tissue Perfusion �Risk for Infection �Body Image Disturbance �Deficient Knowledge

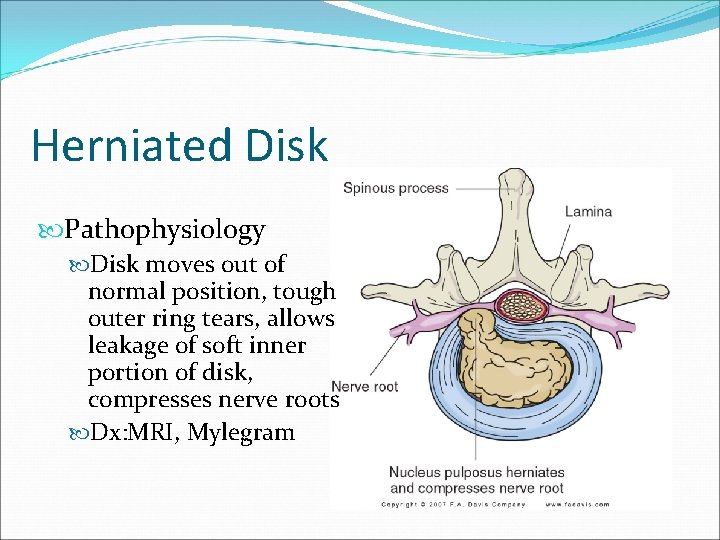
Herniated Disk Pathophysiology Disk moves out of normal position, tough outer ring tears, allows leakage of soft inner portion of disk, compresses nerve roots Dx: MRI, Mylegram

Signs & Symptoms �Pain �Muscle Spasm �Numbness or Tingling of Extremity �Weakness �Atrophy

Therapeutic Interventions �Rest �Physical Therapy �Traction- seperates the verebral bodies and allow disk to return to normal position �Muscle Relaxants �NSAIDS, Analgesics �Epidural Anesthetic/Steroid �Surgery- diskectomy, spinal fusion Complications are hemorrhage, nerve damage, reherniation

Pre / Postoperative Care �Preop- teach log rolling, routine teaching �Postop- Monitor exts (color, warmth, pulses), pain, monitor surgical site, I & O �Nursing Diagnoses �Pain �Risk for Impaired Urinary Elimination �Risk for Impaired Physical Mobility

Spinal Cord Injury �Pathophysiology �Damage to Nerve Fibers, interferes with communication Between Brain and Body. If suspected, avoid flexion or rotation of the spine �Damage may be cause by bruising, tearing, cut, edema, or bleeding into the spinal cords. Most common are MVA, Falls, sports injury and assault �Dx: x-ray, CT, MRI

Signs & Symptoms �Cervical Injury �Paralysis, may be quadriplegia �Paresthesias �Impaired Respiration �Loss of Bladder and Bowel Control �C 3 or Above Fatal- muscles for breathing are paralyzed �When assessing motor/sensory function, no sensation/movement in all 4 exts, C 4 -C 8 damaged.

Signs & Symptoms continued �Thoracic/Lumbar Injury �Paraplegia- paralyzed from waist down �Altered Bowel and Bladder Control �Cord below the injury stops functioning completely, urine and feces retention

Spinal Shock �SNS Disruption ( Spinal Neurogenic Shock) cord stops functioning below injury �Vasodilation- SNS disrupted, dilation of blood vessels allows more blood flow �Hypotension �Bradycardia �Hypothermia- cooled blood circulates, unable to maintain body temp �Urine and Feces Retention

Complications of Spinal Cord Injury �Infection �DVT �Orthostatic Hypotension �Skin Breakdown �Renal Complications �Depression and Substance Abuse �Autonomic Dysreflexia- life-threatening

Spinal Cord Injury

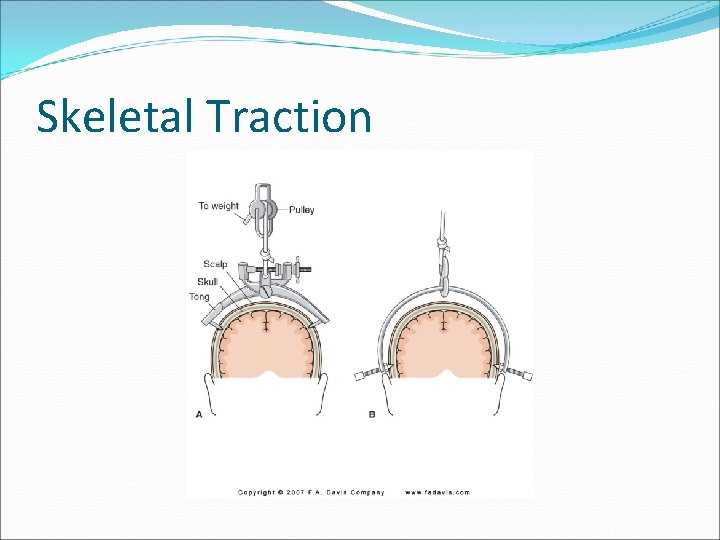
Emergency Management �Respiratory-mechanical ventilation, trach �Gastrointestinal- TPN, feeding not started till BS returns �Genitourinary- Foley �Immobilization- skeletal traction (Crutchfield, Gardner-Wells, Halo)

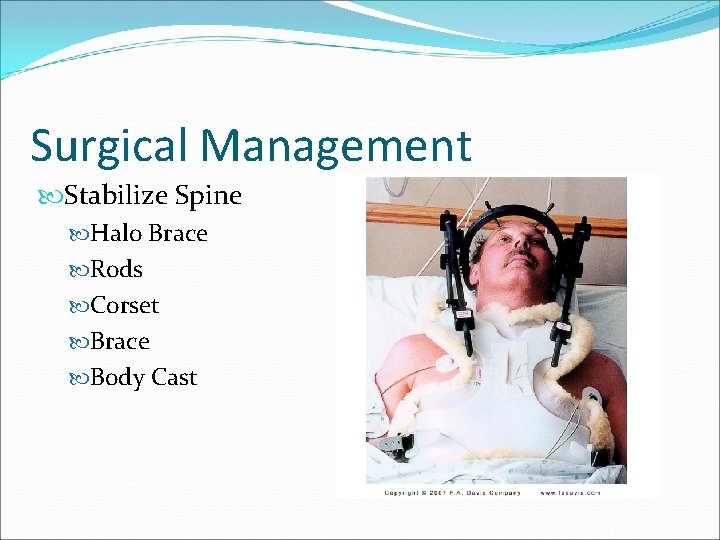
Surgical Management Stabilize Spine Halo Brace Rods Corset Brace Body Cast

Skeletal Traction

Nursing Diagnoses �Impaired Gas Exchange �Ineffective Airway Clearance �Risk for Autonomic Dysreflexia �Total Urinary Incontinence/ Skin Integrity �Constipation �Impaired Physical Mobility �Self-Care deficit �Anxiety �Risk for Sexual Dysfuntion

Dementia �Not a disease, but a s/s of a number of different disorders �Huntington’s Disease �Parkinson’s Disease �Alzheimer’s Disease �Vascular Dementia �Chronic Alcoholism �Medications

Signs & Symptoms �Recent Memory Affected First �Remote Memory Affected Later �Forget How to Perform Simple Tasks �Wandering �Aphasia �Behavioral Problems �Total Dependence �Dx: MRI, CT, for underlying cause, Depression screening, medication review

Therapeutic Interventions Medications Delay Progression �Cholinesterase Inhibitors �NMDA Agonist �End of Life Decision Making �Nursing Diagnosis �Risk for Injury �Disturbed Thought processes �Imbalanced nutrition

Delirium �Temporary mental disturbance with rapid or gradual onset, must be treated promptly �Underlying Cause Must be Corrected �Pain �Hypoxia �Response to medications �Illness, electrolyte imbalance

Parkinson’s Disease �Chronic, degenerative disorder affects basal ganglia and < production of dopamine and excess of Acetylcholine. Loss of dopamine impairs semiautomatic movements because it transmits impulses. �Etiology is unknown, may be genetic.

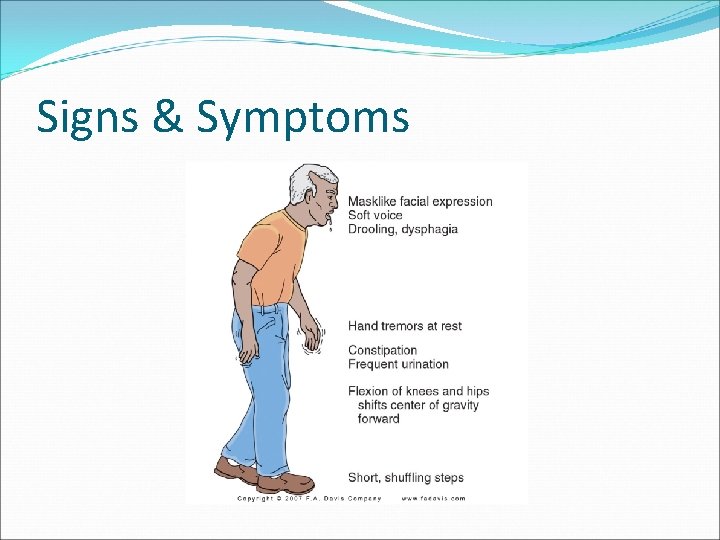
Signs & Symptoms �Muscular Rigidity, posture changes �Bradykinesia �Pill-Rolling Tremor �Difficulty Initiating Movement �Shuffling and Freezing Gait �Dx: Hx/physical exam

Signs & Symptoms

Therapeutic Interventions �Antiparkinson drugs �Anticholinergic Agents �Pallidotomy �Nursing Diagnosis �Impaired physical mobility �Self-care deficit �Risk for injury

Huntington’s Disease

Signs & Symptoms Progressive, genetic, degenerative disease of the brain Dementia Personality Changes Inappropriate Behavior Paranoia Violence Choreiform Movements Dysphagia Depression Death Dx: Family hx, CT, MRI, genetic testing Tx: antipsychotics, antidepressant

Alzheimer’s Disease S/S Progressive, degenerative disease Stage 2 with loss of mental Progressive Memory Loss functioning Irritability Dx: H/P, MRI, autopsy Depression Stage 1 Aphasia Forgetfulness Sleep Disruption Last 2 -4 yrs Decreased interest in Hallucinations Seizures activities

Signs & Symptoms cont’d �Stage 3 - Constant supervision required �Complete Dependency �Bowel and Bladder Control Lost �Emotional Control Lost �Inability to Recognize Significant Others �Death

Therapeutic Interventions �Cholinesterase Inhibitors (Aricept, Exelon) �NMDA Antagonists (Namenda, Axura) �Antidepressants �Antipsychotics �Antianxiety Agents

Nursing Diagnoses: The Patient with Dementia �Self-care deficit �Risk for Injury �Imbalanced Nutrition �Disturbed Thought Processes �Caregiver Role Strain