The Neonatal Airway and Neonatal Intubation Matthew L

The Neonatal Airway and Neonatal Intubation Matthew L. Paden, MD Pediatric Critical Care Fellow Emory University Children’s Healthcare of Atlanta

Goals of Presentation Ø Recognize differences between neonatal and adult airway Ø Review neonatal intubation technique and equipment Ø Review common mistakes and complications of intubation Ø Examine syndromes commonly associated with difficult neonatal airways

Why do we care? Ø Prompt intubation of a distressed neonate can be life-saving l Increasingly premature population Ø Residents are getting less training at this l l RRC limitation of intensive care training (1994) Revision of NRP protocols (2000)

Why do we care? Ø Database of all neonatal intubations at UCSD from 1992 -2002 l Ø 9190 attempts recorded What did they find? l Successful intubation on each attempt • PGY 1 33%, PGY 2 40%, PGY 3 40% l Total intubations attempted during residency • 1994 – 38(+/- 19), 2002 – 12(+/- 6) l Total intubations successful during residency • 1994 – 24(+/- 14), 2002 – 4(+/-2) Ø Conclusion l “Pediatric trainees are currently provided inadequate experience to allow development of proficiency at neonatal intubation. ” NN Finer, et al. Neonatal Intubation: Success of Pediatric Trainees. J Peds 2005; 146: 638 -41.
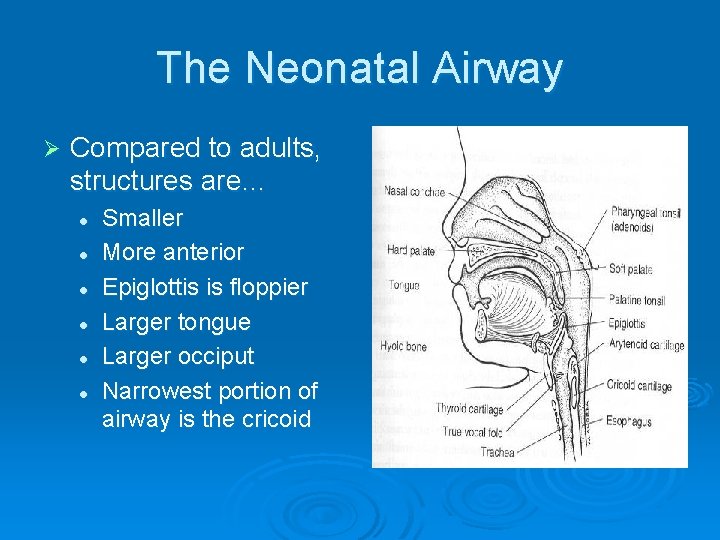
The Neonatal Airway Ø Compared to adults, structures are… l l l Smaller More anterior Epiglottis is floppier Larger tongue Larger occiput Narrowest portion of airway is the cricoid
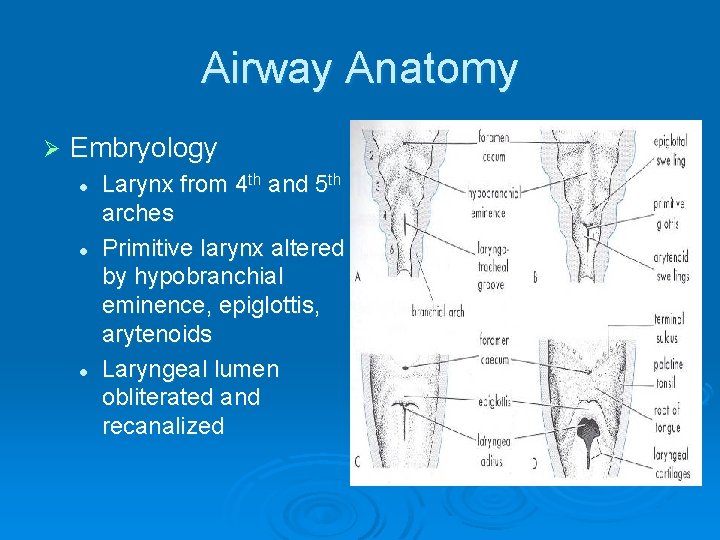
Airway Anatomy Ø Embryology l l l Larynx from 4 th and 5 th arches Primitive larynx altered by hypobranchial eminence, epiglottis, arytenoids Laryngeal lumen obliterated and recanalized

Indications for Intubation Ø In delivery room l l Cardiorespiratory instability Meconium during birth, with a depressed infant Prematurity requiring need for surfactant therapy Congenital malformations

Indications for Intubation Ø In NICU l l Unable to protect airway Hypercarbic respiratory failure Hypoxic respiratory failure Therapeutic indication

What do you need? Monitors - Cardiac and pulse oximetry Suction - Yankauer or catheter Machine - Laryngoscope, ventilator or bag/mask Airway - Endotracheal tube Intravenous - Peripheral or central line Drugs -Sedation/analgesia/paralysis/atropine

Laryngoscope Blades Straight blades are placed under the epiglottis and used to lift anteriorly to expose the cords. Ø Curved blades are placed in the valecula and lifted anteriorly to expose the cords. Ø Miller Macintosh Wisconsin

Endotracheal Tubes Ø Endotracheal tubes are divided by the size of their internal diameter Ø For neonates endotracheal tube size roughly corresponds to 1/10 th of gestational age rounded down to the nearest size. l For example • A 36 week premie would get a 3. 5 ETT • A 28 week premie would get a 2. 5 ETT

Intubation Procedure Ø Proper positioning l Equipment • • l Bed and patient at comfortable height Suction and meconium aspirator readily available Endotracheal tubes not under warmer All equipment tested and working just prior to use Patient • • Shoulder roll Head in sniffing position l Too much hyperextension can make visualization difficult

Intubation Procedure Ø Pre-oxygenate with 100% bag valve mask ventilation l Contraindicated in known congenital diaphragmatic hernia Ø Apply monitors Ø Give drugs l l Remember minimum atropine dose Ensure ability to bag/mask ventilate before paralysis
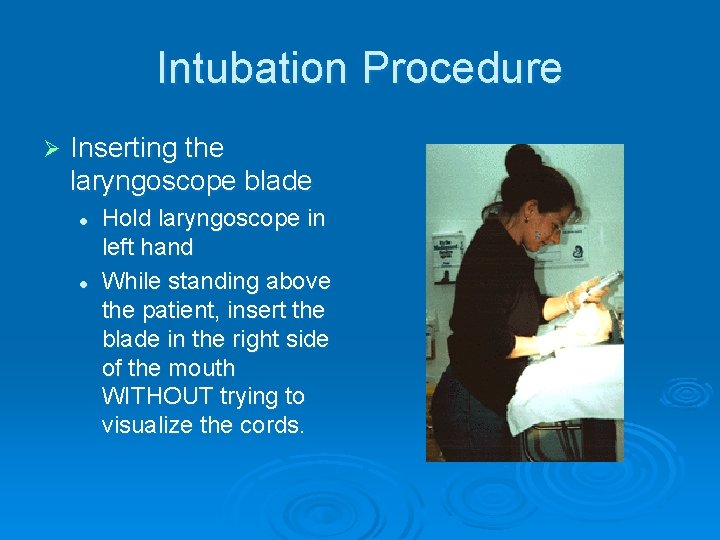
Intubation Procedure Ø Inserting the laryngoscope blade l l Hold laryngoscope in left hand While standing above the patient, insert the blade in the right side of the mouth WITHOUT trying to visualize the cords.

Intubation Procedure Take a step back Ø Lower your head to the level of the label Ø Slowly advance laryngoscope until you visualize the epiglottis Ø Use straight or curved blade appropriately Ø
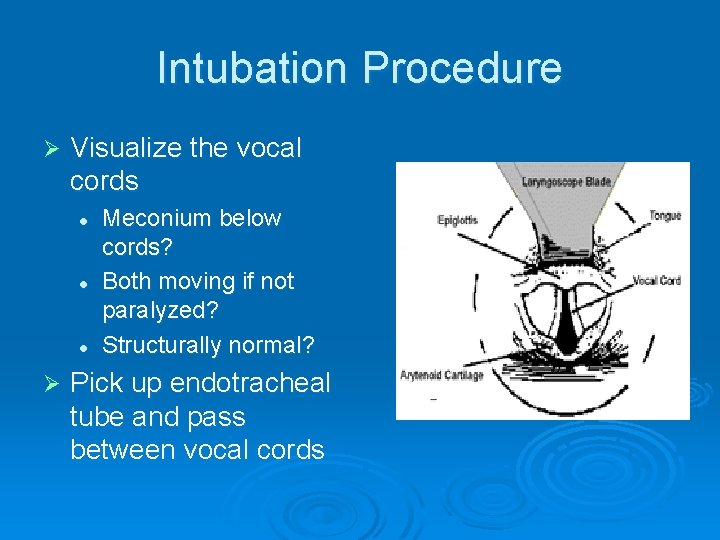
Intubation Procedure Ø Visualize the vocal cords l l l Ø Meconium below cords? Both moving if not paralyzed? Structurally normal? Pick up endotracheal tube and pass between vocal cords

Assessing Endotracheal Tube Placement Ø Direct visualization Ø End tidal CO 2 monitoring Ø Chest rise Ø Auscultation Ø ETT vapor l Less reliable Ø Chest X-ray
Intubation Procedure Ø Secure endotracheal tube to lip with tape l Do not let go of tube until secure Ø Reassess that endotracheal tube is still in place. Ø Assess the neonate – l Improving? More pink? Heart rate increasing? Ø Continue resuscitation – proceed to B and C….

Common Problems Ø Esophageal Intubation l Blade placed too deep, cords not visualized Ø Tongue obscures visualization l l l Sweep tongue to one side with blade More anterior lift Tape on blade Ø Cannot see cords l Head is hyper-extended - reposition

Common Problems Ø Cannot intubate l l Most neonates can be bag valve mask ventilated easily Call early for anesthesiology assistance • “Bag ventilating with oxygen can prolong life for a long time, repeatedly attempting and failing intubation will not. ” l Surgical airway

Difficult Neonatal Airways Ø Must always be prepared for something abnormal Ø Increasing awareness of problems beforehand because of neonatal ultrasound Ø “Things you can see” versus “Things you may find”

Difficult Neonatal Airways Ø Congenital malformations l l “Things you can see” Predictable from looking at the patient • • • Cleft lip and palate Pierre Robin syndrome Treacher Collins syndrome Goldenhar syndrome Apert and Crouzon Syndrome
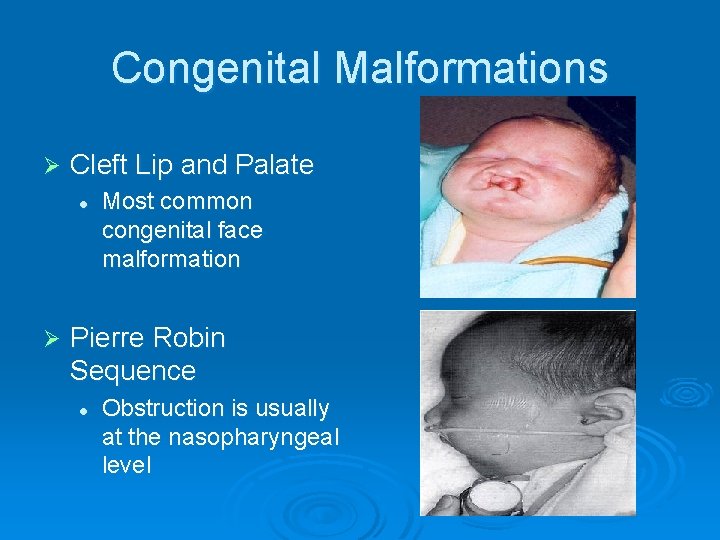
Congenital Malformations Ø Cleft Lip and Palate l Ø Most common congenital face malformation Pierre Robin Sequence l Obstruction is usually at the nasopharyngeal level
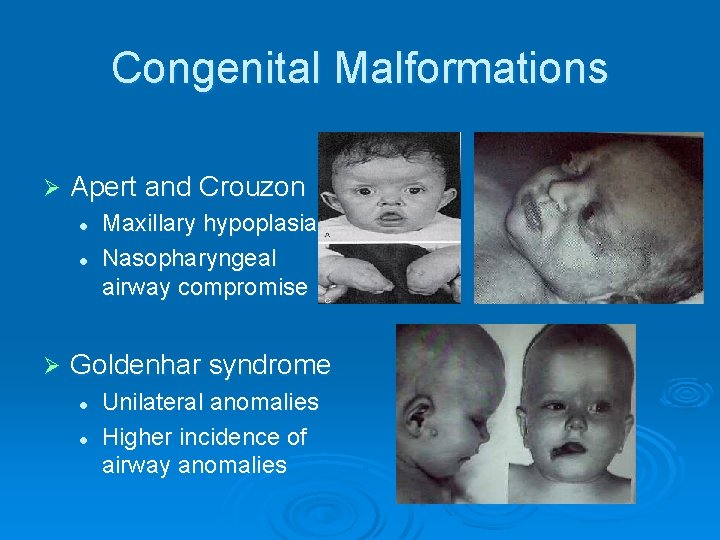
Congenital Malformations Ø Apert and Crouzon l l Ø Maxillary hypoplasia Nasopharyngeal airway compromise Goldenhar syndrome l l Unilateral anomalies Higher incidence of airway anomalies
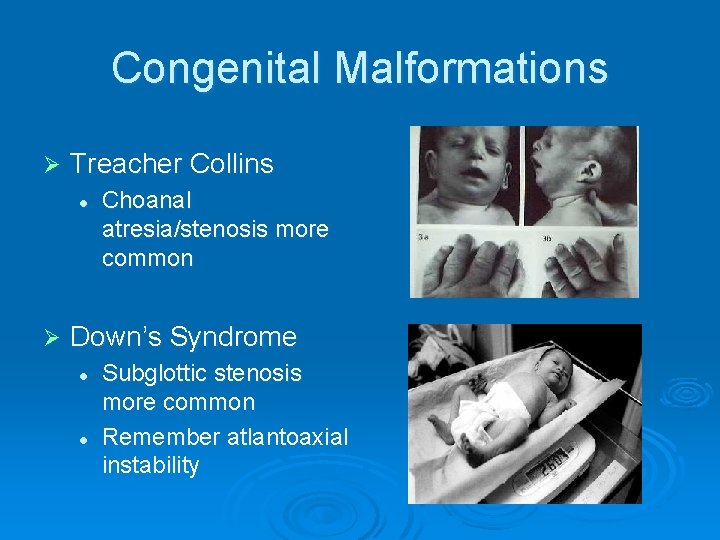
Congenital Malformations Ø Treacher Collins l Ø Choanal atresia/stenosis more common Down’s Syndrome l l Subglottic stenosis more common Remember atlantoaxial instability
Difficult Neonatal Airways Ø Congenital Malformations l “Things you may find” • Laryngomalacia • Hemangioma or Lymphangioma • Tracheal web • Laryngeal atresia • Subglotic stenosis
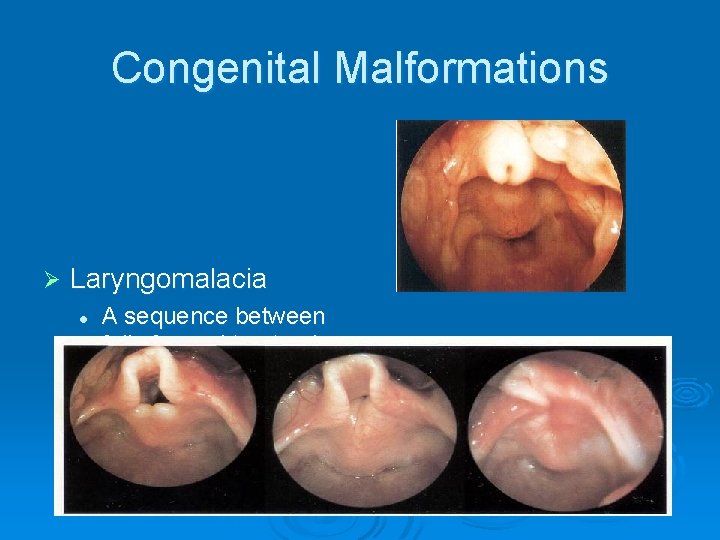
Congenital Malformations Ø Laryngomalacia l A sequence between fully formed to atresia
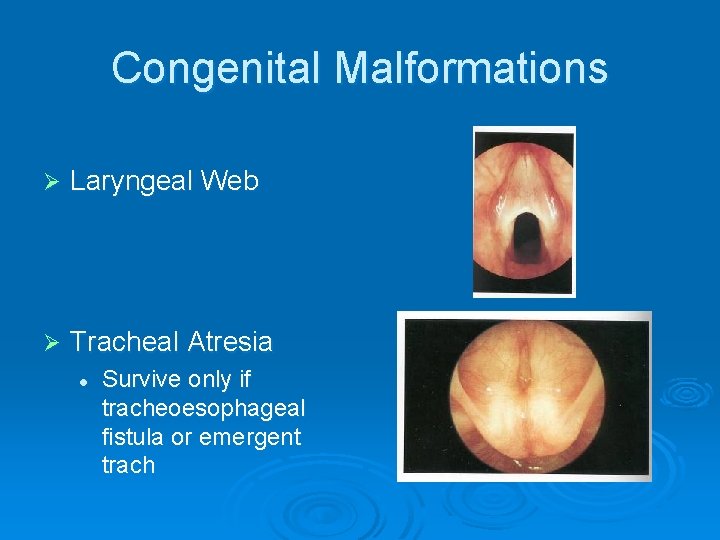
Congenital Malformations Ø Laryngeal Web Ø Tracheal Atresia l Survive only if tracheoesophageal fistula or emergent trach
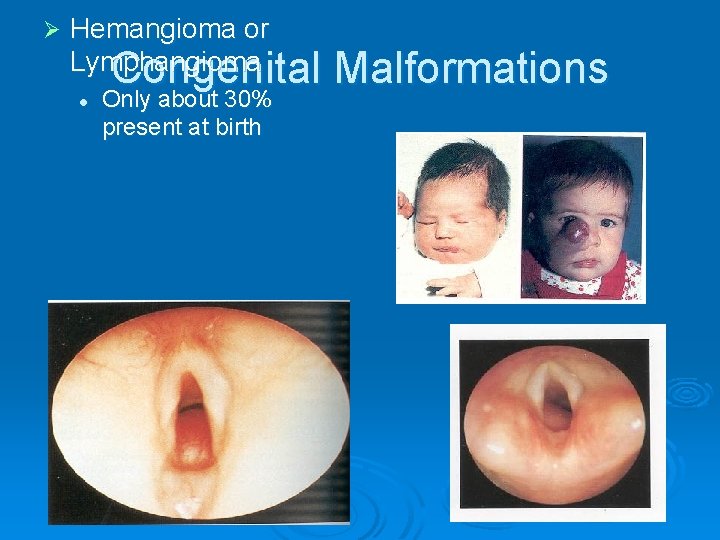
Ø Hemangioma or Lymphangioma Congenital l Only about 30% present at birth Malformations
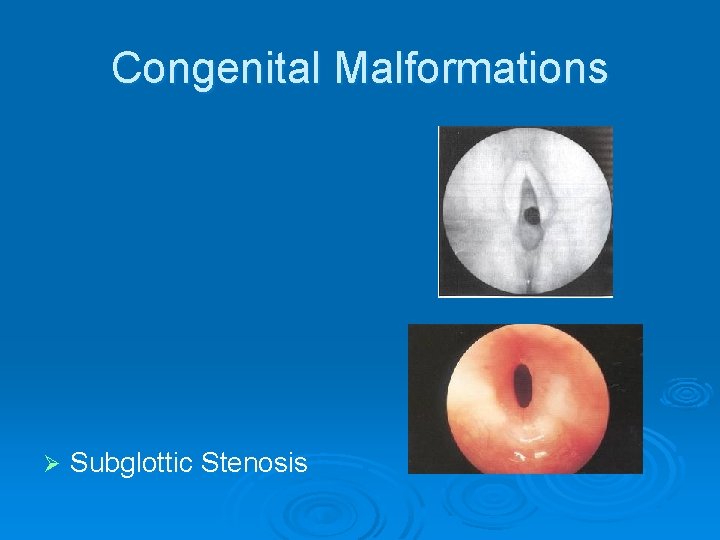
Congenital Malformations Ø Subglottic Stenosis

In Review Proper positioning is critical for successful neonatal intubation Ø Call for help early if unable to intubate or for any congenital anomalies Ø l Ø Continue to provide oxygen with bag valve mask ventilation Practice makes perfect l It is estimated that you need to perform at least 90 intubations to be able to intubate successfully on the first or second attempt at least 80% of the time

Ø QUESTIONS?
- Slides: 32