The National Optimum Lung Cancer Pathway David Baldwin

The National Optimum Lung Cancer Pathway David Baldwin Consultant Respiratory Physician Nottingham University Hospitals Hon. Professor, School of Medicine, University of Nottingham Chair, CEG for Lung Cancer, NHSE

Objectives • Key features of NOLCP • Selected detail of pathways and supplements • Discuss implementation

Pathway development: A National Consultation

Lung Cancer Commissioning Guidance • Guidance for commissioners of specialised and non-specialised services • Including: – Priorities for healthcare improvement – What to commission – What to measure • • Approved by the Programme of Care Board (NHSE) 2015 Approved by the Clinical Panel (NHSE) 2016 Updated for 2017/18 – signed-off NHSE August 2017 Sent to Alliances for implementation Available at: https: //www. roycastle. org/how-we-help/lung-cancerinformation/information-for-healthcare-professionals/commissioning-guidance

Nationally agreed pathways Requested by Clinical Panel NHSE Oct 15 Draft by 8 clinicians Modified by CRG Consultation with all networks and professional bodies (supported by CRUK) • Draft updated following comments • Finalised by CRG • Sent to stakeholders for endorsement • • • Update vs. 2. 0 June 2017 • Signed off by NHSE August 2017 Jan 16 June 17

Pathways developed • Standard – current practice • Optimal pathway (previously termed “aspirational” • Triage • Curative intent • Direct to CT • Update 2017 – release ? May

Detail of Optimal Pathway
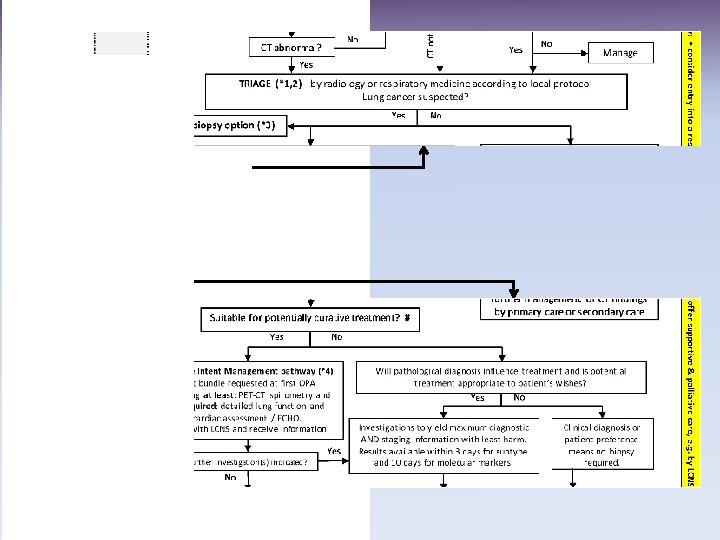
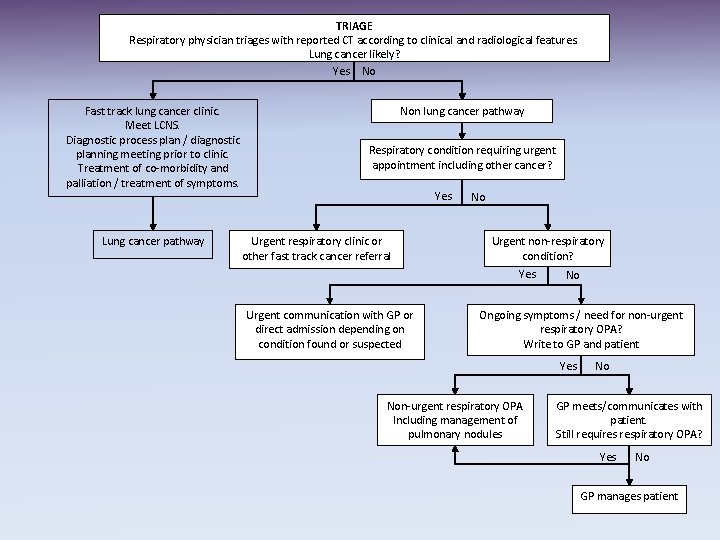
TRIAGE Respiratory physician triages with reported CT according to clinical and radiological features. Lung cancer likely? Yes No Fast track lung cancer clinic. Meet LCNS. Diagnostic process plan / diagnostic planning meeting prior to clinic. Treatment of co-morbidity and palliation / treatment of symptoms. Lung cancer pathway Non lung cancer pathway Respiratory condition requiring urgent appointment including other cancer? Yes Urgent respiratory clinic or other fast track cancer referral No Urgent non-respiratory condition? Yes Urgent communication with GP or direct admission depending on condition found or suspected No Ongoing symptoms / need for non-urgent respiratory OPA? Write to GP and patient Yes Non-urgent respiratory OPA Including management of pulmonary nodules No GP meets/communicates with patient. Still requires respiratory OPA? Yes No GP manages patient
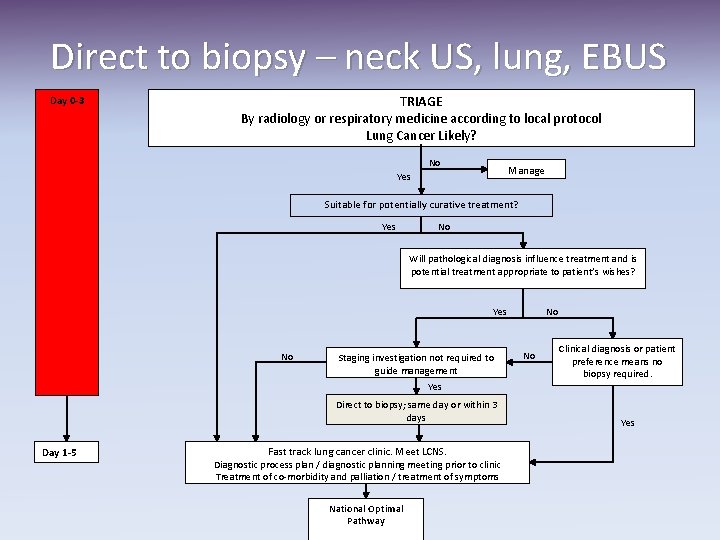
Direct to biopsy – neck US, lung, EBUS Day 0 -3 TRIAGE By radiology or respiratory medicine according to local protocol Lung Cancer Likely? No Manage Yes Suitable for potentially curative treatment? Yes No Will pathological diagnosis influence treatment and is potential treatment appropriate to patient’s wishes? No Yes No Staging investigation not required to guide management No Clinical diagnosis or patient preference means no biopsy required. Yes Direct to biopsy; same day or within 3 days Day 1 -5 Fast track lung cancer clinic. Meet LCNS. Diagnostic process plan / diagnostic planning meeting prior to clinic Treatment of co-morbidity and palliation / treatment of symptoms National Optimal Pathway Yes
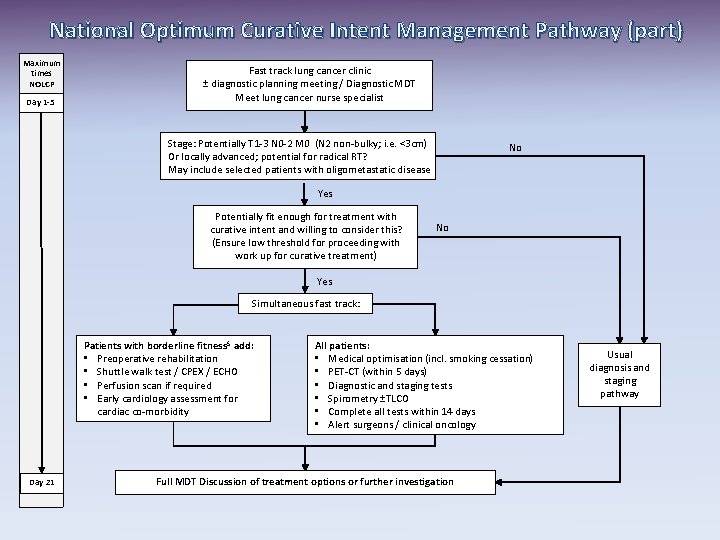
National Optimum Curative Intent Management Pathway (part) Maximum times NOLCP Day 1 -5 Fast track lung cancer clinic ± diagnostic planning meeting / Diagnostic MDT Meet lung cancer nurse specialist Stage: Potentially T 1 -3 N 0 -2 M 0 (N 2 non-bulky; i. e. <3 cm) Or locally advanced; potential for radical RT? May include selected patients with oligometastatic disease No Yes Potentially fit enough for treatment with curative intent and willing to consider this? (Ensure low threshold for proceeding with work up for curative treatment) No Yes Simultaneous fast track: Patients with borderline fitness$ add: • Preoperative rehabilitation • Shuttle walk test / CPEX / ECHO • Perfusion scan if required • Early cardiology assessment for cardiac co-morbidity Day 21 All patients: • Medical optimisation (incl. smoking cessation) • PET-CT (within 5 days) • Diagnostic and staging tests • Spirometry ±TLCO • Complete all tests within 14 days • Alert surgeons / clinical oncology Full MDT Discussion of treatment options or further investigation Usual diagnosis and staging pathway
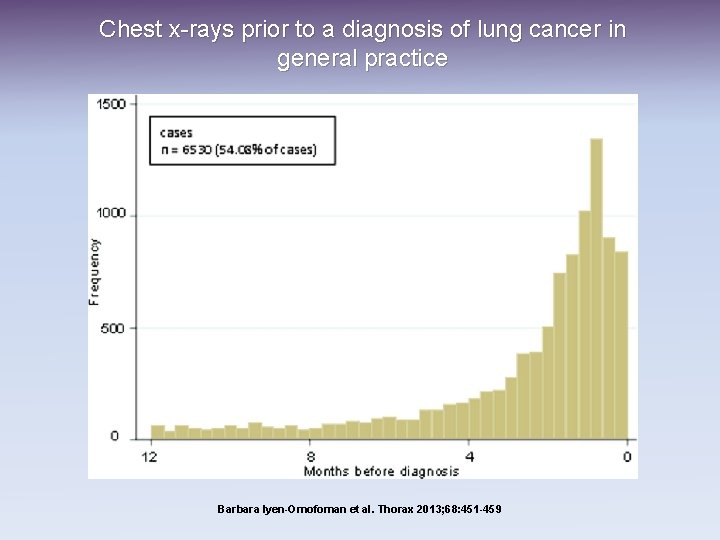
Chest x-rays prior to a diagnosis of lung cancer in general practice Barbara Iyen-Omofoman et al. Thorax 2013; 68: 451 -459
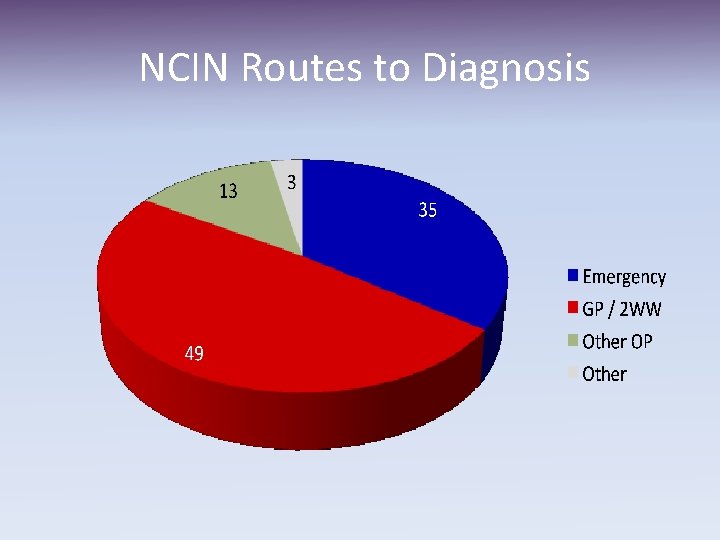
NCIN Routes to Diagnosis
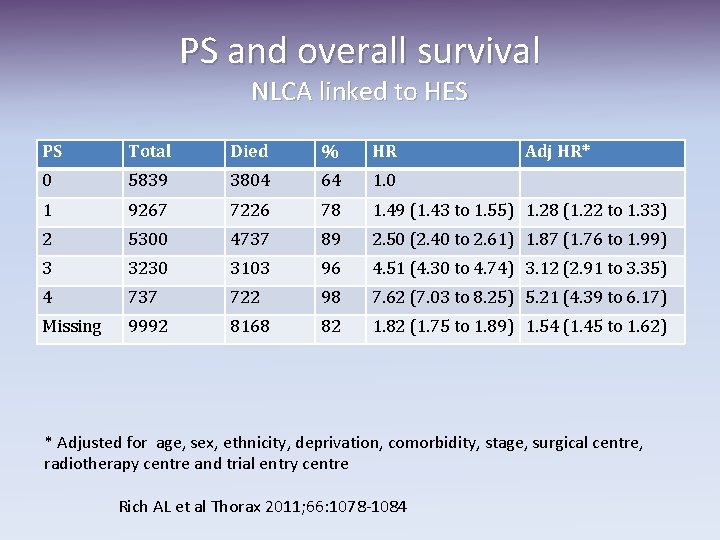
PS and overall survival NLCA linked to HES PS Total Died % HR Adj HR* 0 5839 3804 64 1. 0 1 9267 7226 78 1. 49 (1. 43 to 1. 55) 1. 28 (1. 22 to 1. 33) 2 5300 4737 89 2. 50 (2. 40 to 2. 61) 1. 87 (1. 76 to 1. 99) 3 3230 3103 96 4. 51 (4. 30 to 4. 74) 3. 12 (2. 91 to 3. 35) 4 737 722 98 7. 62 (7. 03 to 8. 25) 5. 21 (4. 39 to 6. 17) Missing 9992 8168 82 1. 82 (1. 75 to 1. 89) 1. 54 (1. 45 to 1. 62) * Adjusted for age, sex, ethnicity, deprivation, comorbidity, stage, surgical centre, radiotherapy centre and trial entry centre Rich AL et al Thorax 2011; 66: 1078 -1084

8 Dec 2015
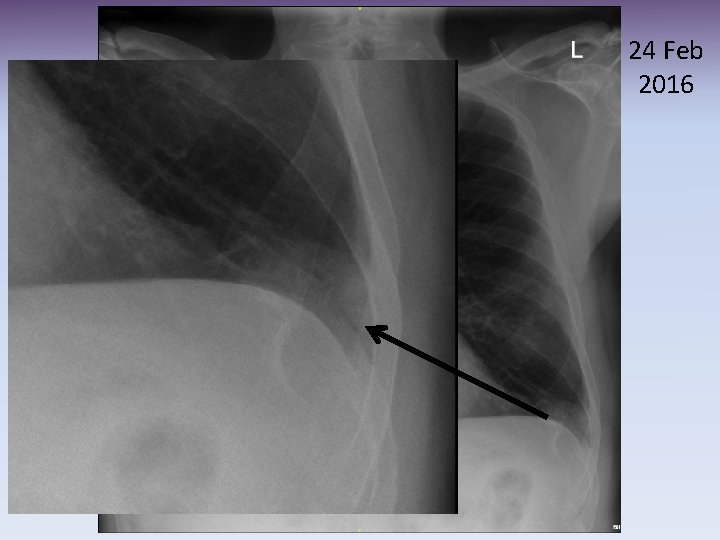
24 Feb 2016
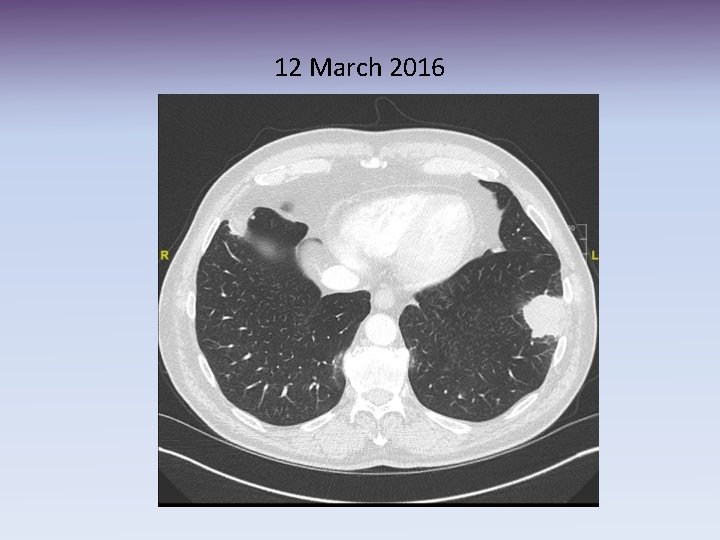
12 March 2016

National Optimum Lung Cancer Pathway

Implementation • All elements working now at some hospitals – Liverpool – Nottingham – Manchester and London • Successful bids for Alliance Transformation funding • Toolkit in preparation https: //www. roycastle. org/how-we-help/lung-cancerinformation/information-for-healthcareprofessionals/commissioning-guidance

The Future • Implementation of Service Guidance and NOLCP – Supported by CRUK, RCF, NHSE, Alliances • Big, challenging ideas are needed for big, challenging problems

Thanks Roy Castle Lung Cancer Foundation Members of CRG: Diana Borthwick Julie Hendry David Gilligan Andrew Bates Neil Bayman Anand Devaraj Sue Maughan Amelia Randle Yvonne Summers Andrew Wilcock Michele Mc. Mahon Martin Grange John White Denis Talbot Sanjay Popat Paul Cane David Baldwin Sam Janes Robert Rintoul Yvtis Dudzevicius Imran Hussain Sion Barnard Doug West Stakeholders (for comments) Ian Woolhouse, Martin Ledson, Paul Beckett, Sadia Anwar, Mick Peake, Mat Callister, Robert Rintoul. Ruth Bridgeman, Louise Wilson
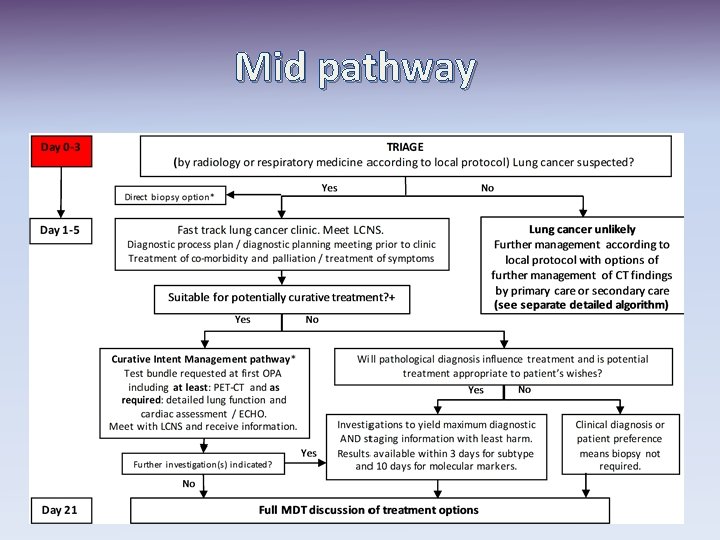
Mid pathway
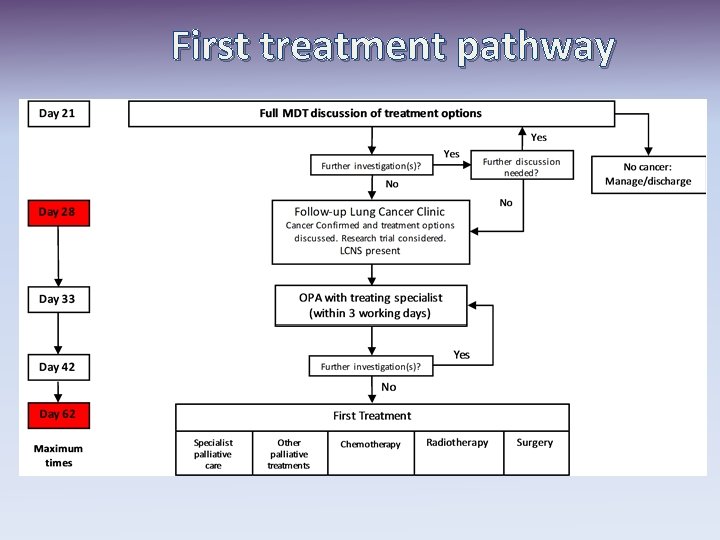
First treatment pathway
- Slides: 23