The Metabolic Syndrome International Diabetes Federation IDF consensus

The Metabolic Syndrome: International Diabetes Federation (IDF) consensus definition Paul Zimmet & George Alberti Co-Chairmen

METABOLIC SYNDROME A cluster of risk factors for diabetes and cardiovascular disease

The Metabolic Syndrome (“Deadly Quartet”) A cluster of risk factors for diabetes and cardiovascular disease consisting of: • Central (abdominal) obesity • Diabetes, IFG and IGT • Hypertension • Dyslipidaemia

International Diabetes Federation (IDF) consensus definition In 2004, the IDF held an expert workshop to examine how the currently available definitions for the Metabolic Syndrome could be improved and developed with the aim of reaching a consensus for the introduction of a new and unifying definition.

THE ORIGINS • 1920 s • 1940 s/50 s – Vague • 1967 – Avogaro & Crepaldi • 1988 - Reaven

Kylin 1923 Description Kylin E: Studien ϋber das Hypertonie-Hyperglykämie – Hyperurika miesyndrome 1923

Crepaldi 1965 Description “seems to suggest a peculiar syndrome including hyperlipemia, obesity and diabetes. The development of ischaemic heart disease … and hypertension is often found in these patients. ” Avogaro & Crepaldi, 1965

The 2000 WHO Working Group attempt to describe & define the Metabolic Syndrome was an initiative to create interest and debate – it was never meant to be the final answer.
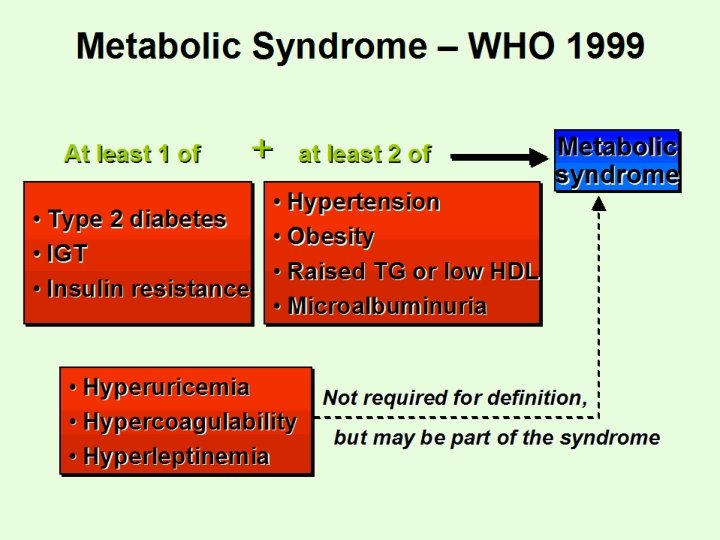
Metabolic Syndrome – WHO 1999 At least 1 of + at least 2 of • Hypertension • Type 2 diabetes • Obesity • IGT • Raised TG or low HDL • Insulin resistance • Microalbuminuria Metabolic syndrome • Hyperuricemia Not required for definition, • Hypercoagulability but may be part of the syndrome • Hyperleptinemia
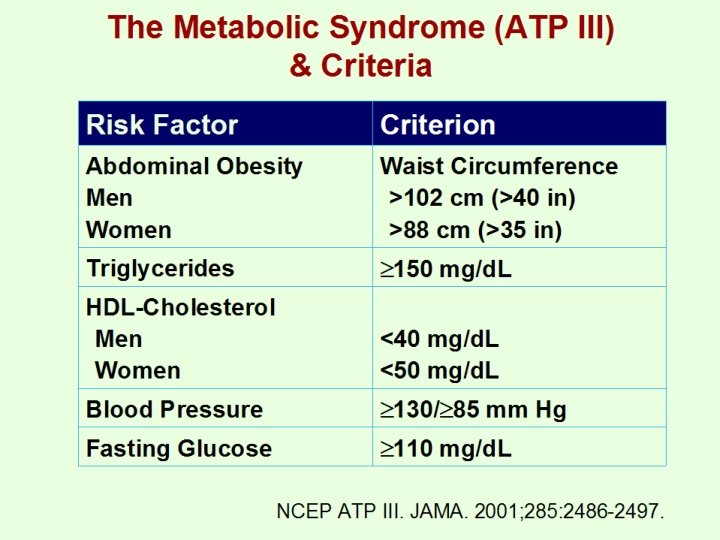
The Metabolic Syndrome (ATP III) & Criteria Risk Factor Criterion Abdominal Obesity Men Women Waist Circumference >102 cm (>40 in) >88 cm (>35 in) Triglycerides 150 mg/d. L HDL-Cholesterol Men Women <40 mg/d. L <50 mg/d. L Blood Pressure 130/ 85 mm Hg Fasting Glucose 110 mg/d. L NCEP ATP III. JAMA. 2001; 285: 2486 -2497.

EGIR Definition of Metabolic Syndrome: 1999 • • • Insulin resistance + 2 or more of: Central obesity (94 cm -M; 80 cm - F) TG >2. 9 m. M OR HDL <1. 0 Hypertension (> 140/90) FPG > 6. 1 m. M
The Metabolic Syndrome in Australia; Different Prevalences for Different Criteria
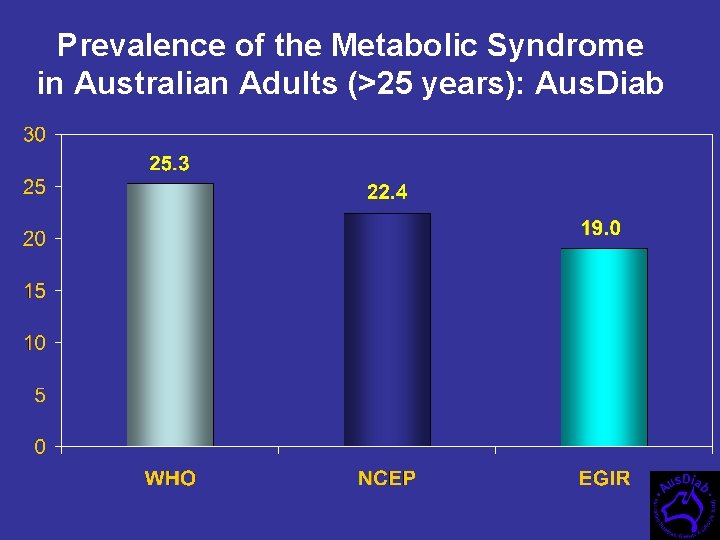
Prevalence of the Metabolic Syndrome in Australian Adults (>25 years): Aus. Diab
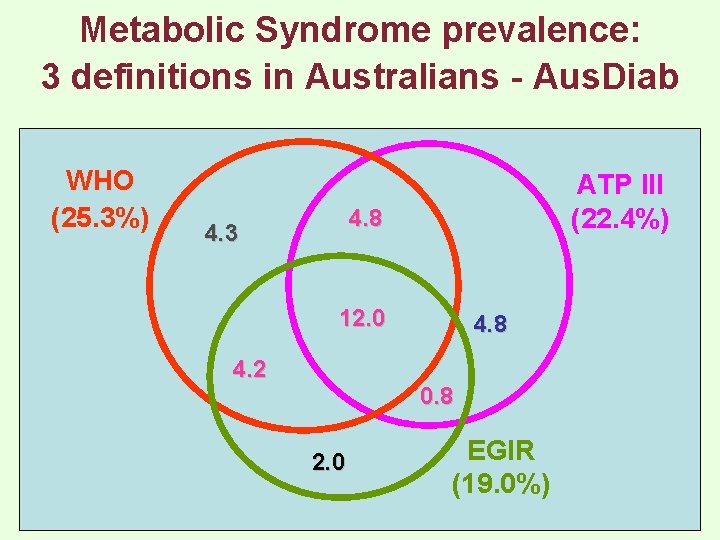
Metabolic Syndrome prevalence: 3 definitions in Australians - Aus. Diab WHO (25. 3%) ATP III (22. 4%) 4. 8 4. 3 12. 0 4. 2 4. 8 0. 8 2. 0 EGIR (19. 0%)

RESULT Confusion!!!

“Consensus Means That A Lot Of People Say Collectively What No One Believes Individually”. Abba Eban
Central obesity: a driving force for cardiovascular disease & diabetes Front Back “Balzac” by Rodin

Developing A New Definition of the Metabolic Syndrome: IDF Objectives Needs: • To identify individuals at high risk of developing cardiovascular disease (and diabetes) • To be useful for clinicians • To be useful for international comparisons

International Diabetes Federation (IDF) Consensus Definition 2005 The new IDF definition focusses on abdominal obesity rather than insulin resistance
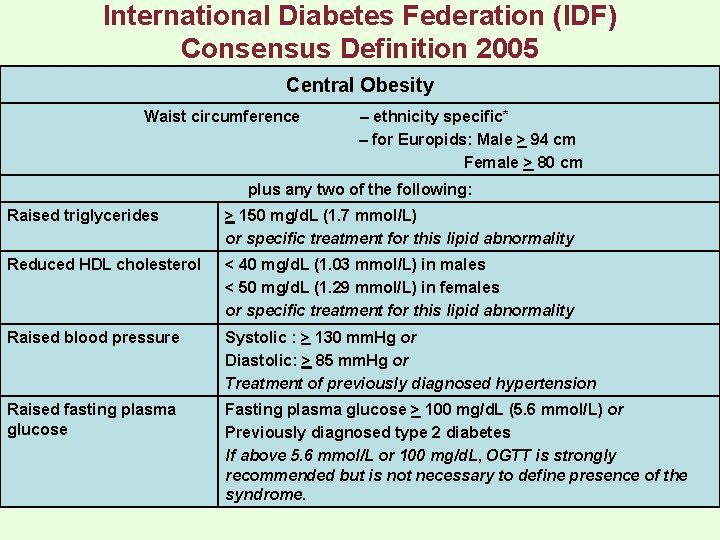
International Diabetes Federation (IDF) Consensus Definition 2005 Central Obesity Waist circumference – ethnicity specific* – for Europids: Male > 94 cm Female > 80 cm plus any two of the following: Raised triglycerides > 150 mg/d. L (1. 7 mmol/L) or specific treatment for this lipid abnormality Reduced HDL cholesterol < 40 mg/d. L (1. 03 mmol/L) in males < 50 mg/d. L (1. 29 mmol/L) in females or specific treatment for this lipid abnormality Raised blood pressure Systolic : > 130 mm. Hg or Diastolic: > 85 mm. Hg or Treatment of previously diagnosed hypertension Raised fasting plasma glucose Fasting plasma glucose > 100 mg/d. L (5. 6 mmol/L) or Previously diagnosed type 2 diabetes If above 5. 6 mmol/L or 100 mg/d. L, OGTT is strongly recommended but is not necessary to define presence of the syndrome.
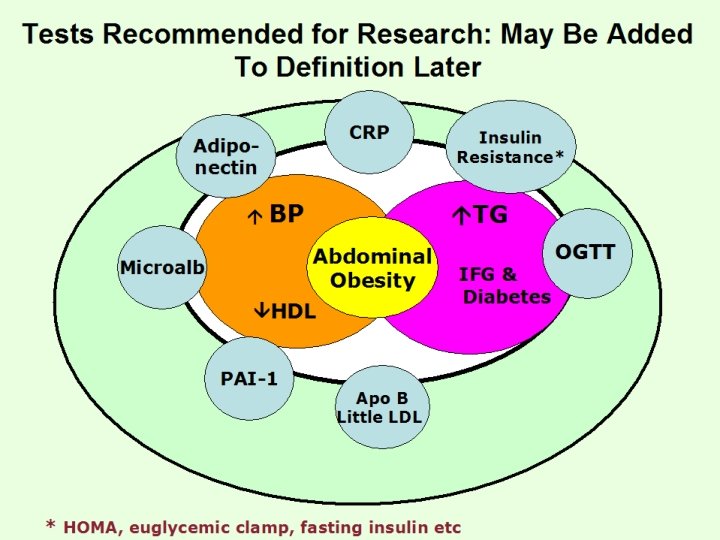
Tests Recommended for Research: May Be Added To Definition Later CRP Adiponectin BP TG Abdominal Obesity Microalb HDL PAI-1 Insulin Resistance* IFG & Diabetes Apo B Little LDL * HOMA, euglycemic clamp, fasting insulin etc OGTT
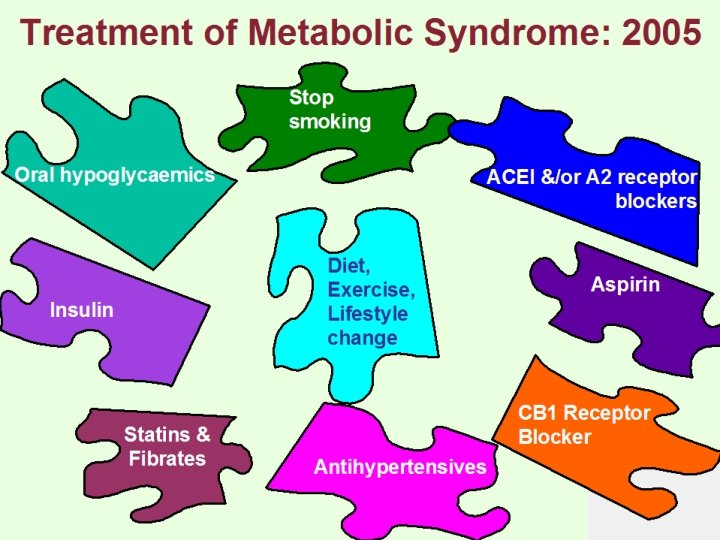
Treatment of Metabolic Syndrome: 2005 Stop smoking Oral hypoglycaemics ACEI &/or A 2 receptor blockers Diet, Exercise, Lifestyle change Insulin Statins & Fibrates Aspirin CB 1 Receptor Blocker Antihypertensives

Recommendations for treatment Primary management for the Metabolic Syndrome is healthy lifestyle promotion. This includes: • moderate calorie restriction (to achieve a 5 -10% loss of body weight in the first year) • moderate increases in physical activity • change dietary composition to reduce saturated fat and total intake, increase fibre and, if appropriate, reduce salt intake.

Management of the Metabolic Syndrome • Appropriate & aggressive therapy is essential for reducing patient risk of cardiovascular disease • Lifestyle measures should be the first action • Pharmacotherapy should have beneficial effects on – – Glucose intolerance/diabetes Obesity Hypertension Dyslipidaemia • Ideally, treatment should address all of the components of the syndrome and not the individual components

Summary: new IDF definition for the Metabolic Syndrome The new IDF definition addresses both clinical and research needs: • provides a simple entry point for primary care physicians to diagnose the Metabolic Syndrome • providing an accessible, diagnostic tool suitable for worldwide use, taking into account ethnic differences • establishing a comprehensive ‘platinum standard’ list of additional criteria that should be included in epidemiological studies and other research into the Metabolic Syndrome
- Slides: 25