The Management of Tibial Plafond Fractures James Reidy

The Management of Tibial Plafond Fractures James Reidy Bart's Teaching Oct 2012

Background • 1911 Destot – French Radiologist • Pestle • Domed or vaulted ceiling • 1959 Jergesen – ORIF impossible

Pilon Timeline 1969 Ruedi and Allgower – 84 consecutive pilon #s treated with ORIF – 4 principles • Restoration of fibular length with plating • Anatomical reconstruction of the articular surface of the tibia • Cancellous autograft for metaphyseal Tibial defects • Plating of the anteromedial tibia to prevent varus – 74% good or excellent results at 4 years 1976 Heim and Nasser – 128 pilon #s – ORIF with same technique – 90% “good functional results” (85% return to athletic activity)
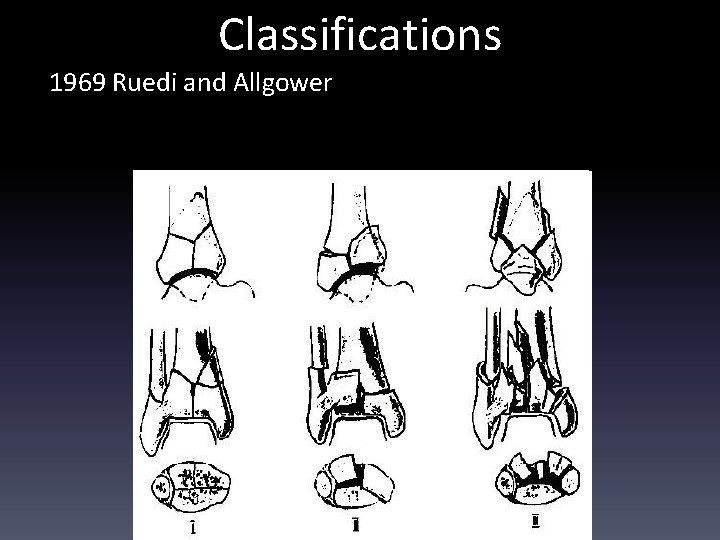
Classifications 1969 Ruedi and Allgower

Classifications 1969 Kellam • Type A: Low energy rotational - Valgus • Type B: High energy axial load - Varus
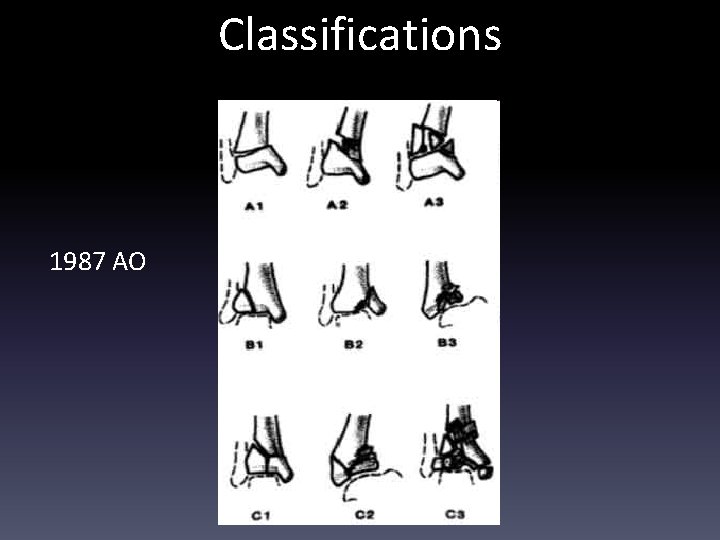
Classifications 1987 AO
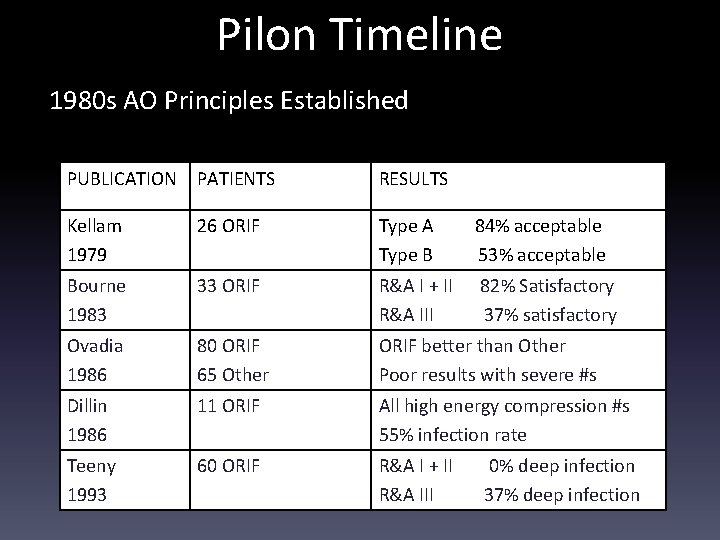
Pilon Timeline 1980 s AO Principles Established PUBLICATION PATIENTS RESULTS Kellam 1979 26 ORIF Type A Type B 84% acceptable 53% acceptable Bourne 1983 33 ORIF R&A I + II R&A III 82% Satisfactory 37% satisfactory Ovadia 1986 80 ORIF 65 Other ORIF better than Other Poor results with severe #s Dillin 1986 11 ORIF All high energy compression #s 55% infection rate Teeny 1993 60 ORIF R&A I + II R&A III 0% deep infection 37% deep infection

Pilon Timeline 1990 s Staged Management – Early operation through traumatised soft tissues inadvisable – Temporary spanning ex fix • Stabilise to protect soft tissues • Restores length and may reduce articular fragments by ligamentotaxis – Strict elevation – Definitive fixation when soft tissues settled • Healing of skin blisters • Skin wrinkling • Typically 7 to 21 days
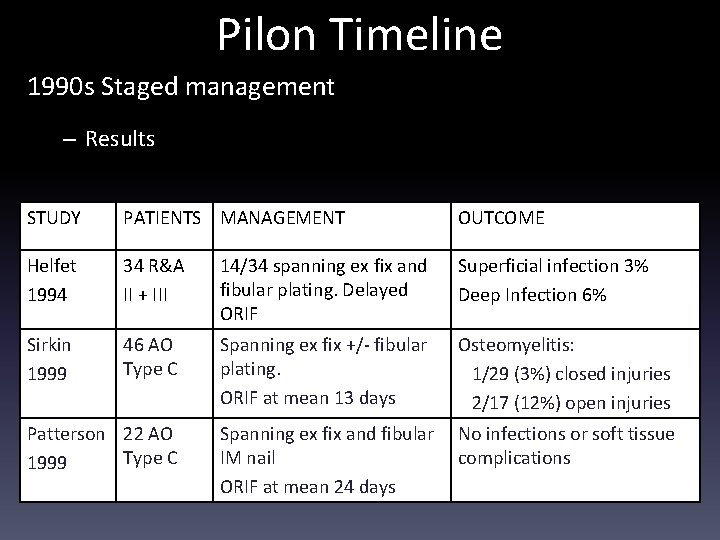
Pilon Timeline 1990 s Staged management – Results STUDY PATIENTS MANAGEMENT OUTCOME Helfet 1994 34 R&A II + III 14/34 spanning ex fix and fibular plating. Delayed ORIF Superficial infection 3% Deep Infection 6% Sirkin 1999 46 AO Type C Spanning ex fix +/- fibular plating. ORIF at mean 13 days Osteomyelitis: 1/29 (3%) closed injuries 2/17 (12%) open injuries Spanning ex fix and fibular IM nail ORIF at mean 24 days No infections or soft tissue complications Patterson 22 AO Type C 1999
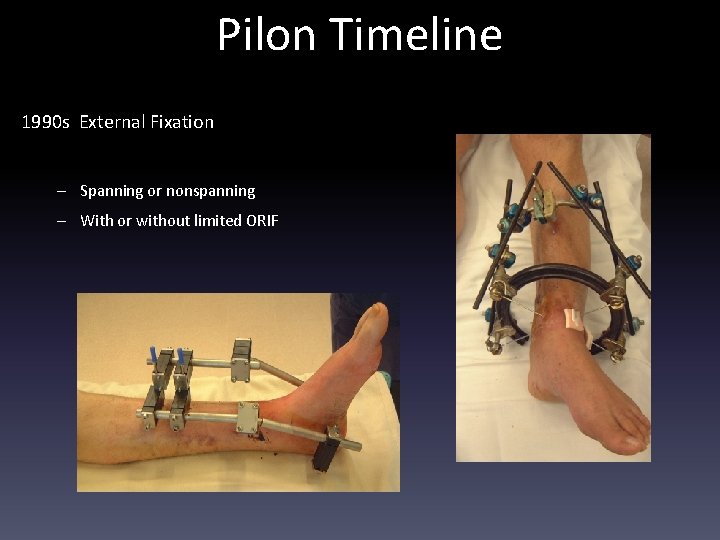
Pilon Timeline 1990 s External Fixation – Spanning or nonspanning – With or without limited ORIF
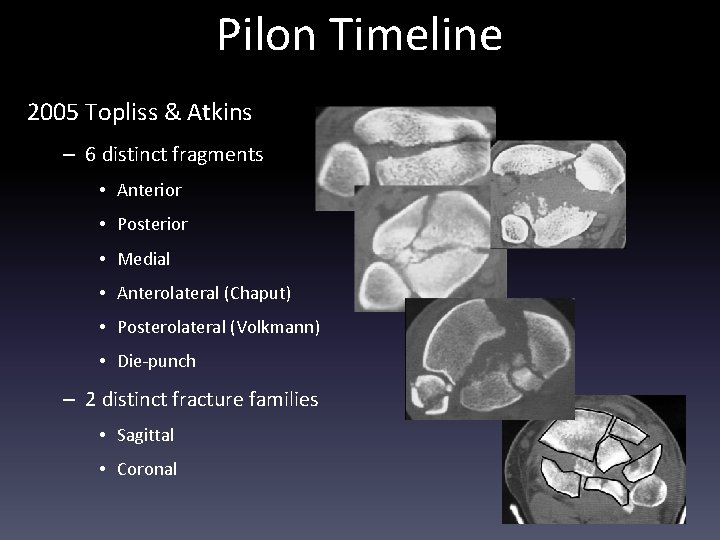
Pilon Timeline 2005 Topliss & Atkins – 6 distinct fragments • Anterior • Posterior • Medial • Anterolateral (Chaput) • Posterolateral (Volkmann) • Die-punch – 2 distinct fracture families • Sagittal • Coronal
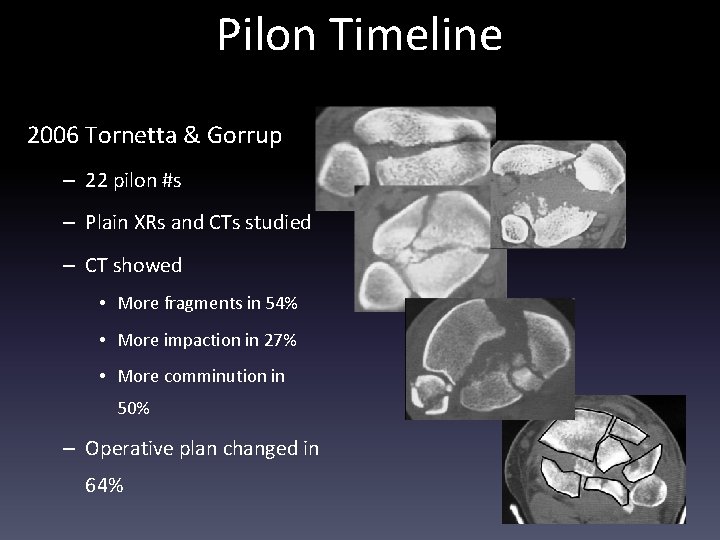
Pilon Timeline 2006 Tornetta & Gorrup – 22 pilon #s – Plain XRs and CTs studied – CT showed • More fragments in 54% • More impaction in 27% • More comminution in 50% – Operative plan changed in 64%
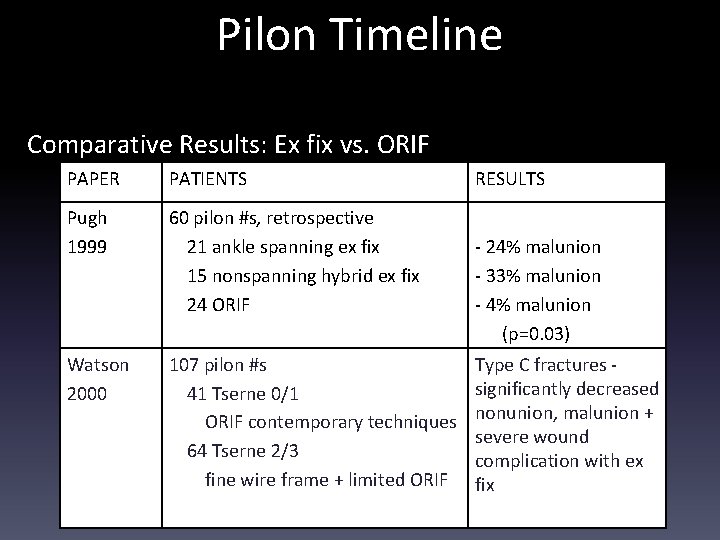
Pilon Timeline Comparative Results: Ex fix vs. ORIF PAPER PATIENTS Pugh 1999 60 pilon #s, retrospective 21 ankle spanning ex fix 15 nonspanning hybrid ex fix 24 ORIF Watson 2000 107 pilon #s 41 Tserne 0/1 ORIF contemporary techniques 64 Tserne 2/3 fine wire frame + limited ORIF RESULTS - 24% malunion - 33% malunion - 4% malunion (p=0. 03) Type C fractures significantly decreased nonunion, malunion + severe wound complication with ex fix
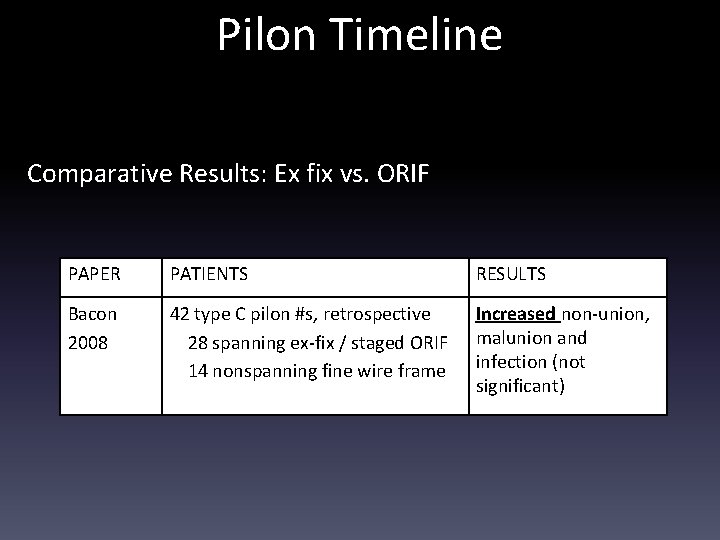
Pilon Timeline Comparative Results: Ex fix vs. ORIF PAPER PATIENTS RESULTS Bacon 2008 42 type C pilon #s, retrospective 28 spanning ex-fix / staged ORIF 14 nonspanning fine wire frame Increased non-union, malunion and infection (not significant)
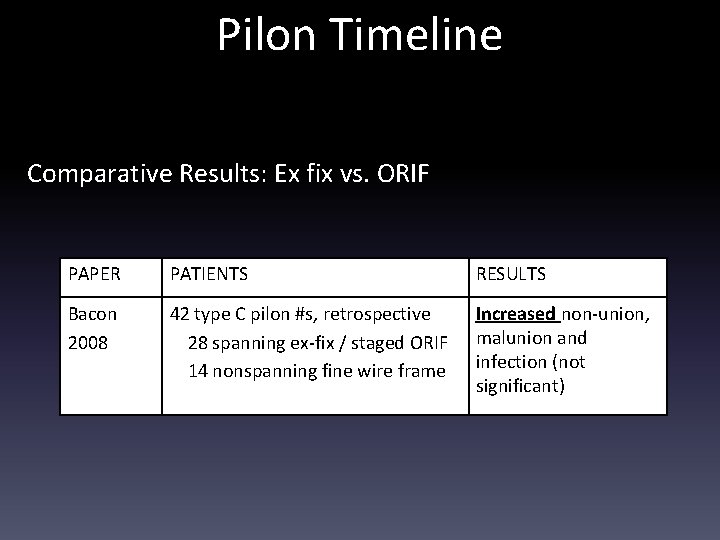
Pilon Timeline Comparative Results: Ex fix vs. ORIF PAPER PATIENTS RESULTS Bacon 2008 42 type C pilon #s, retrospective 28 spanning ex-fix / staged ORIF 14 nonspanning fine wire frame Increased non-union, malunion and infection (not significant)

The evidence is Clear! • Staged Procedure • ORIF marginally better than frame • Conroy et al, 32 GA 3 B, 11 43 C • Deep infection/amputation rates 6%

Present • Less invasive “biological” techniques – Small, direct approaches to fracture sites for reduction – Percutaneous screw fixation of articular block – Metadiaphyseal fixation • • low profile plates – Medial, anterolateral, posterior – Buttress, bridge, compression, locking and nonlocking hybrid or fine wire non-spanning external fixators

Exam Answer • Surgeon independent factors (type C 3) 1. Two or more medical comorbidities 2. $25000 USD or less annually( Mr. Achans monthly interest Return? ) 3. Lack of high school diploma 4. Married 5. Initial ex-fix treatment

Exam • After resolution of soft tissue injury including plastics intervention • Generally takes 10 days to 3 weeks • Supine with bump under the knee and tourniquet

Fibula or not • Can aid in length restoration and rotation • If done early – adds to soft tissue trauma • If not done well – can impede tibial reduction • Has higher risk of wound breakdown • Therefore delayed fibula fixation should be considered.
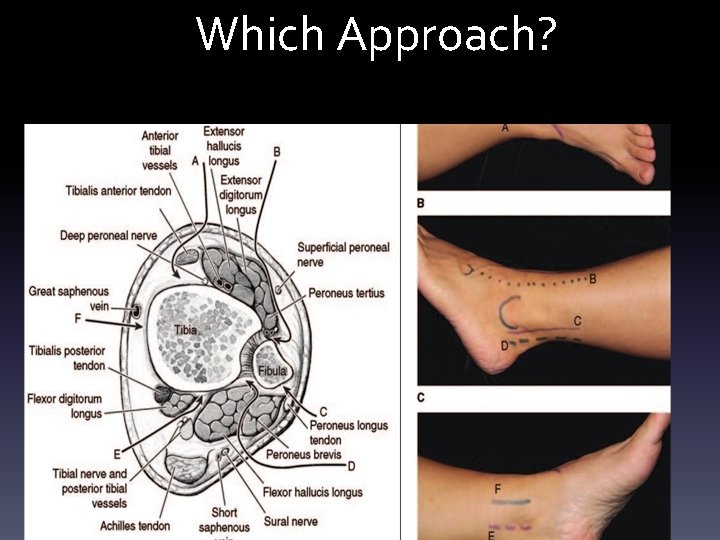
Which Approach?

Which philosophy? • Locked Plates • MIPO • Fine wire fixators • Combination

Wound care • No proven role for NPWT • Serial examination of soft tissues and ongoing surveillance of pin sites paramount

Outcome Summary • Outcomes in high energy fractures generally poor • Patient factors important • Avoidance of treatment complications essential • Staged protocol best • Which strategy?

Thanks • Please Direct all questions to Mr Amin.
- Slides: 25