The Management of Alzheimers Disease Laurel Coleman MD




















- Slides: 27

The Management of Alzheimer’s Disease Laurel Coleman, MD Maine Medical Center Portland, Maine

Management of Alzheimer’s Disease Manage cognitive symptoms Manage BPSD Support patient/family Increased quality of life for patient and family

Pharmacologic Options for AD • Cognitive enhancers ─ 2 classes • Cholinesterase inhibitors (Ch. EIs) • NMDA-receptor antagonist ─ Do not cure the disease or reverse cognitive impairment ─ Can improve cognition and functional ability ─ Reduce the rate of decline 9 -12 months (Ch. EIs) ─ Delay in nursing home placement was 17 -21 months (Ch. EIs)

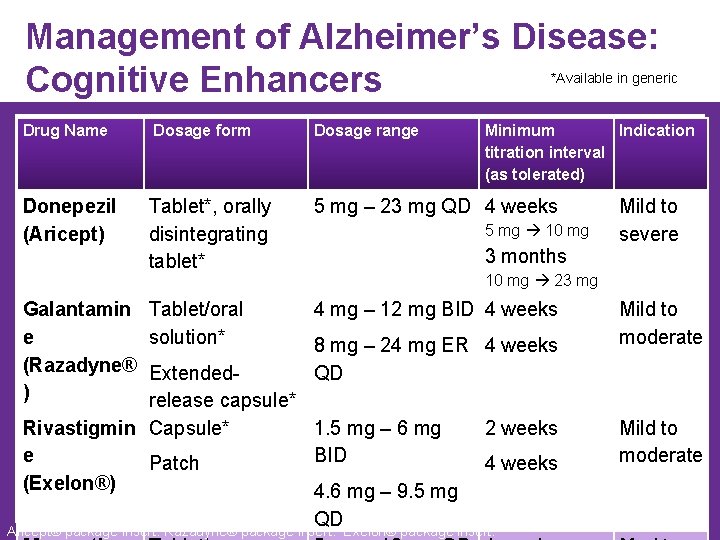
Management of Alzheimer’s Disease: Cognitive Enhancers *Available in generic Drug Name Dosage form Dosage range Donepezil (Aricept) Tablet*, orally disintegrating tablet* 5 mg – 23 mg QD 4 weeks Tablet/oral solution* 4 mg – 12 mg BID 4 weeks Galantamin e (Razadyne® ) Minimum Indication titration interval (as tolerated) 5 mg 10 mg 3 months Mild to severe 10 mg 23 mg 8 mg – 24 mg ER 4 weeks QD Extendedrelease capsule* Rivastigmin Capsule* 1. 5 mg – 6 mg e BID Patch (Exelon®) 4. 6 mg – 9. 5 mg QD 2 weeks 4 weeks Aricept® package insert. Razadyne® package insert. Exelon® package insert. Mild to moderate

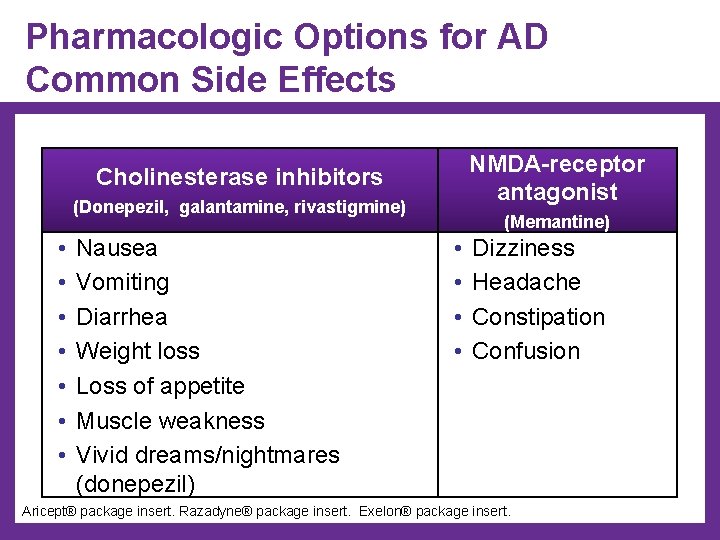
Pharmacologic Options for AD Common Side Effects NMDA-receptor antagonist Cholinesterase inhibitors (Donepezil, galantamine, rivastigmine) • • Nausea Vomiting Diarrhea Weight loss Loss of appetite Muscle weakness Vivid dreams/nightmares (donepezil) (Memantine) • • Dizziness Headache Constipation Confusion Aricept® package insert. Razadyne® package insert. Exelon® package insert.

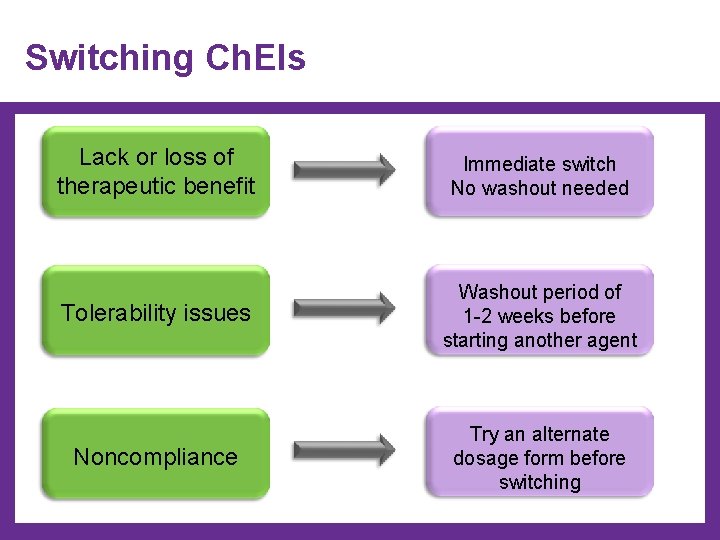
Switching Ch. EIs Lack or loss of therapeutic benefit Immediate switch No washout needed Tolerability issues Washout period of 1 -2 weeks before starting another agent Noncompliance Try an alternate dosage form before switching

Discontinuation of Therapy • Data for optimal duration of treatment as disease progresses is limited ─ ─ • Consider discontinuation in the following situations: ─ ─ ─ 1. 2. Modest cognitive and functional benefits associated with continued therapy with (donepezil) in moderate to severe AD 1 Discontinuation associated with adverse behavioral changes and reduced participation in activites 2 Inability to tolerate multiple Ch. EIs No improvement or greater than expected decline after one or more therapeutic trials End-stage dementia Howard et al. New Engl J Med. 2012; 366: 893 -903. Daiello et al. Am J Geriatr Pharmacother. 2009; 7: 74 -83.

Impact of Coexisting Medical Conditions 2. 4 conditions/pt HTN 82% DM 39% CAD 21% CHF 14% Stroke 10% Cognitive Impairment Prevalence of coexisting conditions in PWD Schubert CC, et al. J Am Geriatr Soc. 2006; 54(1): 104– 109.

Impact of Coexisting Medical Conditions • PWD in primary care average 5. 1 medications/pt 1 ─ 50% take ≥ 1 anticholinergic medications • Medications with anticholinergic activity ─ Impairs cognition acutely (delerium) and chronically 2 • Anticholinergic burden ─ Interfere with therapeutic effect of Ch. EIs 3 1. Schubert CC, et al. J Am Geriatr Soc. 2006; 54(1): 104– 109. 2. Campbell N, et al. Clin Interv Aging. 2009; 4: 225– 233. 3. Lu C, Tune LE. Am J Geriatr Psychiatry. 2003; 11(4): 458– 461.

Behavioral and Psychological Symptoms of Dementia (BPSD) • • Apathy Depressive symptoms Anxiety Agitation/irritability/ aggression • Psychotic symptoms ─ Delusions ─ Hallucinations Tampi et al. Clinical Geriatrics. 2011; 19: 41 -46. • • • Disinhibition Euphoria Loss of appetite Sleep disturbances Stereotyped behaviors (eg, pacing, wandering, rummaging, picking

Managing BPSD • Identify triggers ─ Observe symptom timing and frequency ─ Look for environmental triggers, eg noise, lighting ─ Investigate potentially treatable causes, eg pain • Make adjustments ─ Address medical causes ─ Adapt environment ─ Adapt caregiving • Modify as needed

Managing BPSD Nonpharmacological Interventions • • Use the “ 3 Rs”—repeat, reassure, redirect Simplify the environment, task, routine Anticipate unmet needs Allow adequate rest between stimulating events • Use cues • Encourage physical activity • Other interventions

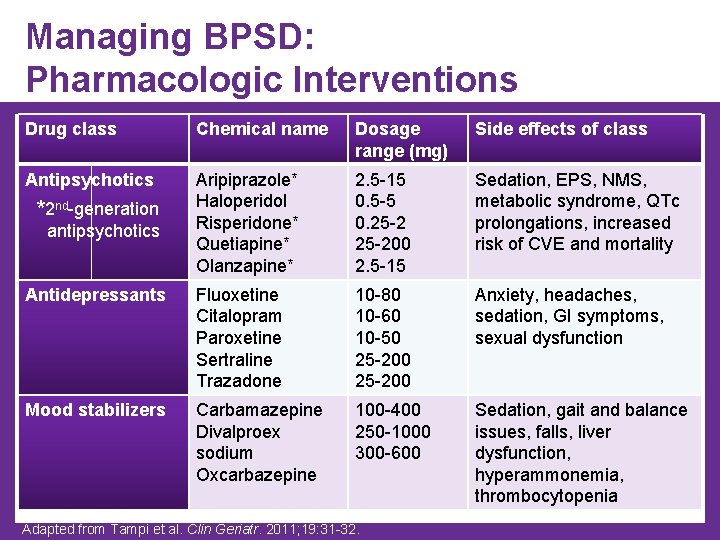
Managing BPSD: Pharmacologic Interventions Drug class Chemical name Dosage range (mg) Side effects of class Antipsychotics Aripiprazole* Haloperidol Risperidone* Quetiapine* Olanzapine* 2. 5 -15 0. 5 -5 0. 25 -200 2. 5 -15 Sedation, EPS, NMS, metabolic syndrome, QTc prolongations, increased risk of CVE and mortality Antidepressants Fluoxetine Citalopram Paroxetine Sertraline Trazadone 10 -80 10 -60 10 -50 25 -200 Anxiety, headaches, sedation, GI symptoms, sexual dysfunction Mood stabilizers Carbamazepine Divalproex sodium Oxcarbazepine 100 -400 250 -1000 300 -600 Sedation, gait and balance issues, falls, liver dysfunction, hyperammonemia, thrombocytopenia *2 nd-generation antipsychotics Adapted from Tampi et al. Clin Geriatr. 2011; 19: 31 -32.

Alzheimer’s Disease Education of Patient and Family

Education of Patient and Family • Safety issues: ─ ─ ─ Home environment Driving Medication adherence Financial exploitation Elder abuse • Address future needs: financial planning, advanced directives, power of attorney

Education of Patient and Family Medications • Define treatment success ─ Symptomatic benefit in • Cognition • Physical function and ADLs • Behavior ─ Increases time to nursing home placement • Discuss length of therapy ─ Adequate trial is 6 months Cummings JL. Am J Geriatr Psychiatry. 2003; 11(2): 131– 145. Doody RS, et al. Arch Neurol. 2001; 58(3): 427– 433.

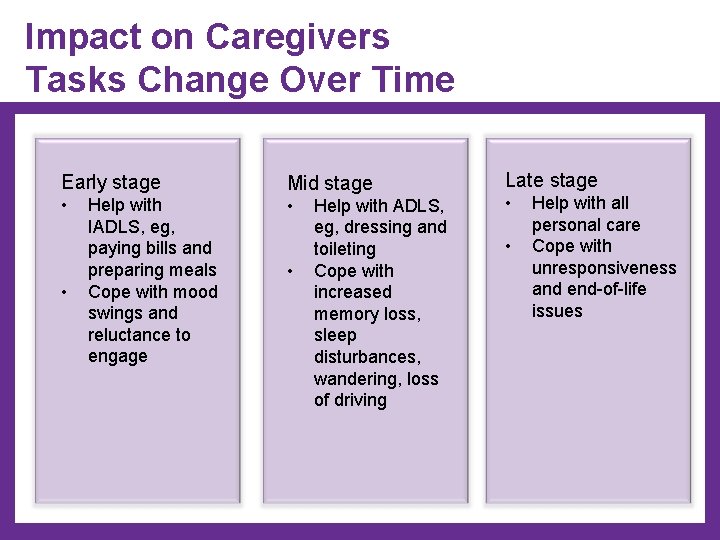
Impact on Caregivers Tasks Change Over Time Early stage Mid stage • • • Help with IADLS, eg, paying bills and preparing meals Cope with mood swings and reluctance to engage • Help with ADLS, eg, dressing and toileting Cope with increased memory loss, sleep disturbances, wandering, loss of driving Late stage • • Help with all personal care Cope with unresponsiveness and end-of-life issues

Education of Patient and Family Alzheimer’s Association • 24/7 Nationwide Helpline ─ ─ • www. alz. org ─ • 800. 272. 3900 Information and referral in 170 languages Current reliable information for healthcare professionals, people with dementia, family members and caregivers 300 local offices ─ ─ ─ Information and referral Support groups Care consultation Safety services Education, local conferences

Clinical Trials • >120 clinical studies in the US are recruiting participants ─ • Slow recruitment is a barrier to discovering new treatments Alzheimer’s Association Trial. Match™ ─ ─ Connect potential participants with appropriate clinical studies Access via phone or online Confidential Free

Understanding prevention research • Much evidence comes from large epidemiological studies that show associations, not proof • Study results apply to populations, not individuals • Large randomized studies for many prevention strategies unlikely ─ Cost prohibitive

Prevention Factors with a consistent association • • Heart-head connection Preventative drug treatments Physical exercise Diet Social connections Intellectual activity Head trauma prevention

Prevention Factors with a consistent association Increased risk of AD Decreased risk of AD • • Conjugated equine estrogen with progesterone* Diabetes Depression Smoking *Moderate evidence, all other factors had low evidence Physical activity Mediterranean diet Cognitive engagement

The Future of Alzheimer’s Disease • Earlier recognition ─ Dependent on reliable biomarkers • New medications ─ Current medications only address symptoms ─ New medications in development • Disease-modifying therapy • Combination disease-modifying and symptomatic therapy • Prevention

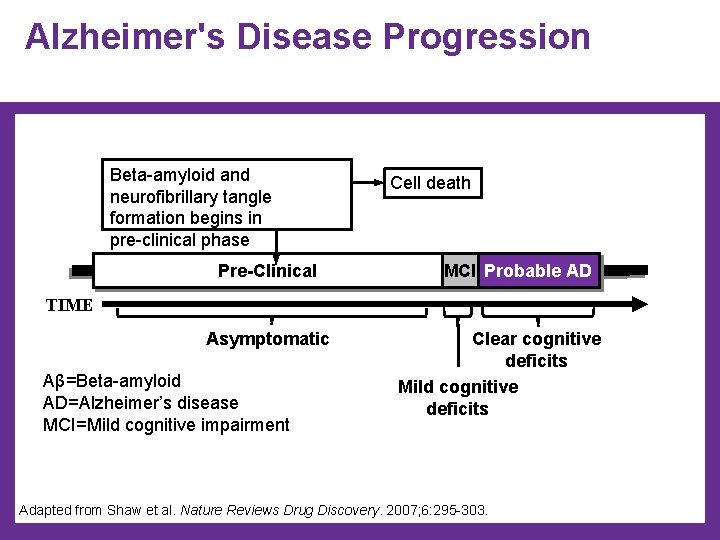
Alzheimer's Disease Progression Beta-amyloid and neurofibrillary tangle formation begins in pre-clinical phase Pre-Clinical Cell death MCI Probable AD TIME Asymptomatic Aβ=Beta-amyloid AD=Alzheimer’s disease MCI=Mild cognitive impairment Clear cognitive deficits Mild cognitive deficits Adapted from Shaw et al. Nature Reviews Drug Discovery. 2007; 6: 295 -303.

Targets for Future Therapies • A ─ -secretase inhibitors ─ Monoclonal antibodies • Tau protein • Inflammation • Insulin resistance

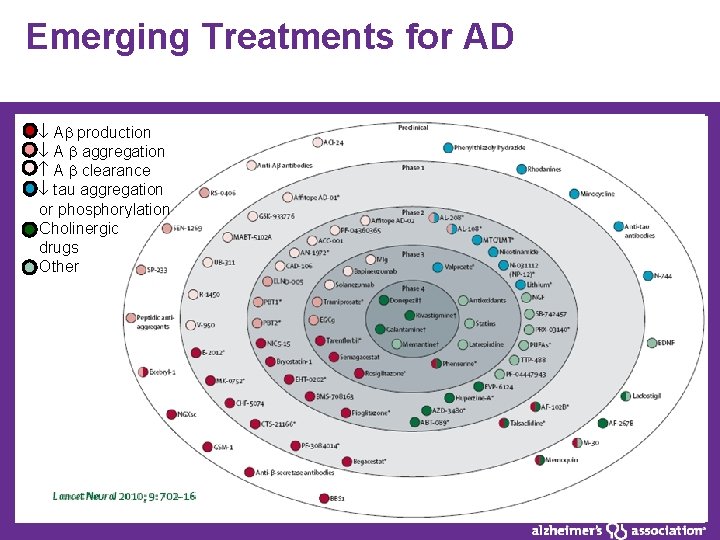
Emerging Treatments for AD A production A aggregation A clearance tau aggregation or phosphorylation Cholinergic drugs Other

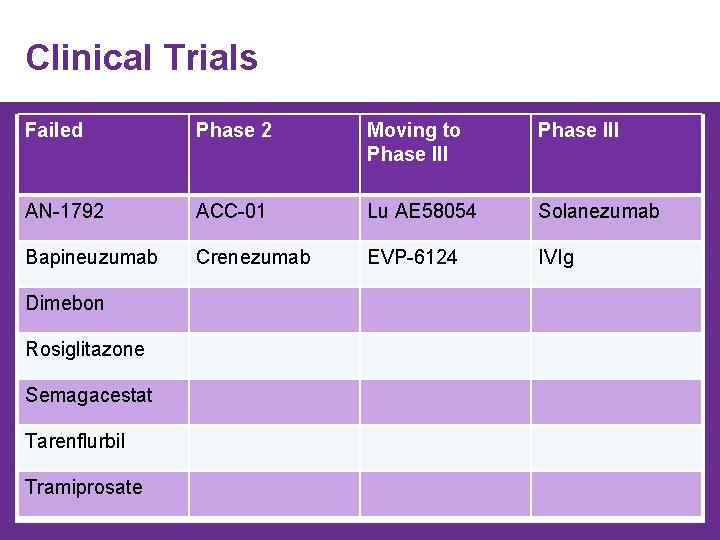
Clinical Trials Failed Phase 2 Moving to Phase III AN-1792 ACC-01 Lu AE 58054 Solanezumab Bapineuzumab Crenezumab EVP-6124 IVIg Dimebon Rosiglitazone Semagacestat Tarenflurbil Tramiprosate