The Lymphatic System And Body Defenses The Lymphatic

The Lymphatic System And Body Defenses

The Lymphatic System • Lymphatic vessels • Lymphoid tissues and organs • Lymphatic system functions – Transport fluids back to the blood – Play essential roles in body defense and resistance to disease

How Lymph Moves • One way system toward the heart • No pump • Milking action of skeletal muscle • Peristalsis in vessel walls

Lymphatic Pathways

Lymphatic Ducts • Lymph is delivered into one of two large ducts – Right lymphatic duct drains the right upper arm and the right side of the head and thorax – Thoracic duct arises from the cisterna chyli and drains the rest of the body • Each empties lymph into venous circulation at the junction of the internal jugular and subclavian veins on its own side of the body
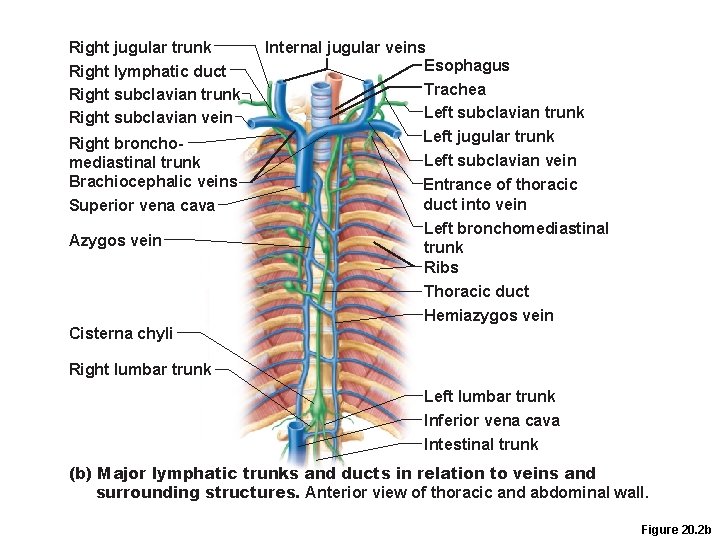
Right jugular trunk Right lymphatic duct Right subclavian trunk Right subclavian vein Right bronchomediastinal trunk Brachiocephalic veins Superior vena cava Azygos vein Internal jugular veins Esophagus Trachea Left subclavian trunk Left jugular trunk Left subclavian vein Entrance of thoracic duct into vein Left bronchomediastinal trunk Ribs Thoracic duct Hemiazygos vein Cisterna chyli Right lumbar trunk Left lumbar trunk Inferior vena cava Intestinal trunk (b) Major lymphatic trunks and ducts in relation to veins and surrounding structures. Anterior view of thoracic and abdominal wall. Figure 20. 2 b
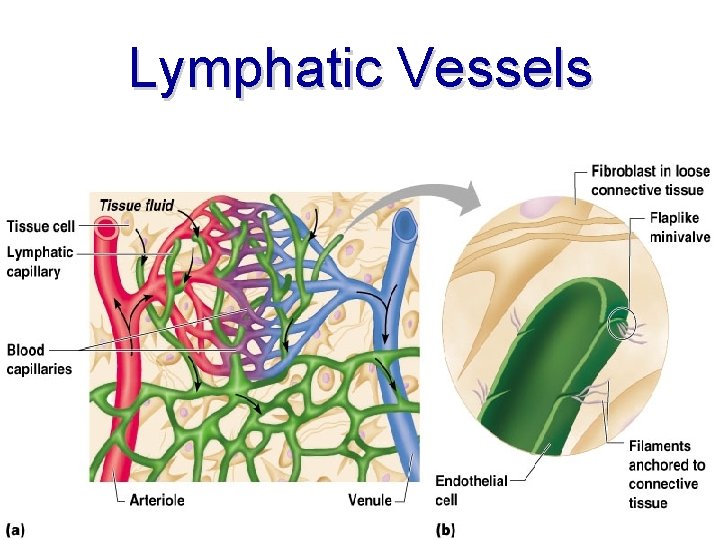
Lymphatic Vessels

Lymphatic Vessels • • Collects lymph from lymph capillaries Carries lymph to and away from lymph nodes Returns fluid to circulatory veins near the heart Lymph Functions: absorption of dietary fats, delivers fats to bloodstream, collection of excess interstitial fluids, delivers excess fluids to bloodstream, delivers foreign particles to lymph nodes

Lymphatic Capillaries • Similar to blood capillaries, except – Very permeable (take up cell debris, pathogens, and cancer cells) – Endothelial cells overlap to form one-way minivalves • Absent from bones, teeth, bone marrow and the CNS • Lacteals: specialized lymph capillaries present in intestinal mucosa – Absorb digested fat and deliver fatty lymph (chyle) to the blood
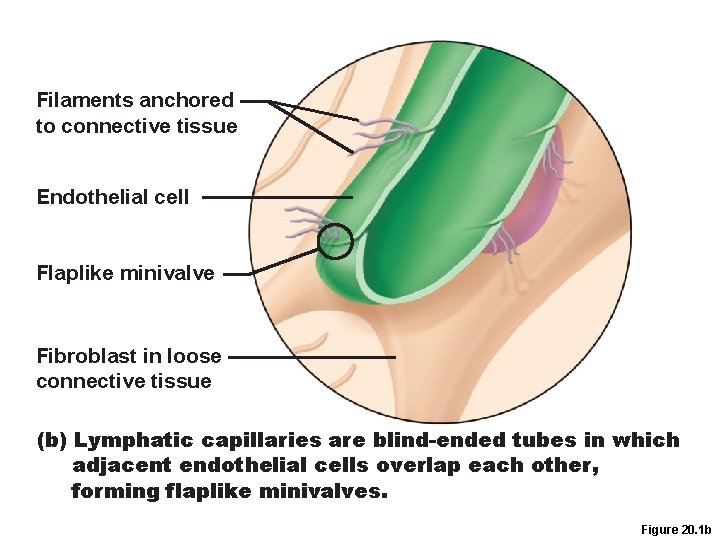
Filaments anchored to connective tissue Endothelial cell Flaplike minivalve Fibroblast in loose connective tissue (b) Lymphatic capillaries are blind-ended tubes in which adjacent endothelial cells overlap each other, forming flaplike minivalves. Figure 20. 1 b

Lymph • Materials returned to the blood – Water – Blood cells – Proteins • Harmful materials that enter lymph vessels – Bacteria – Viruses – Cancer cells – Cell debris

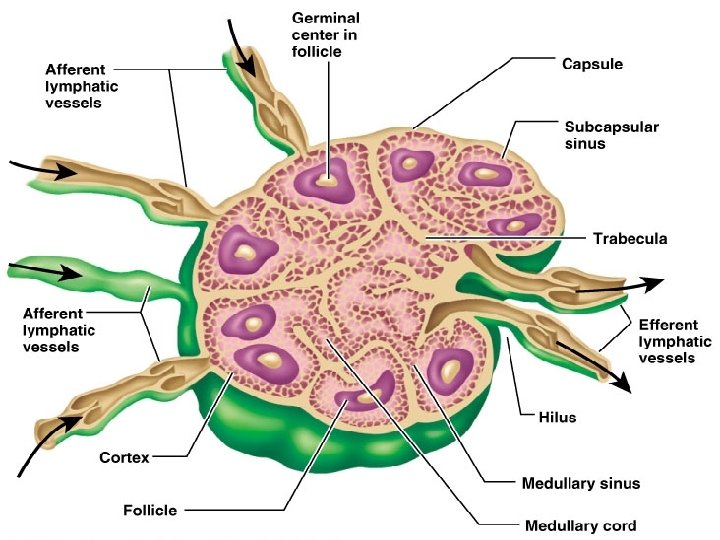
Lymph Nodes • Filter lymph before it is returned to the blood • Defense cells within lymph nodes – Macrophages – Lymphocytes • Most are kidney-shaped, less than 1 inch long • Cortex: collections of lymphocytes • Medulla: phagocytic macrophages
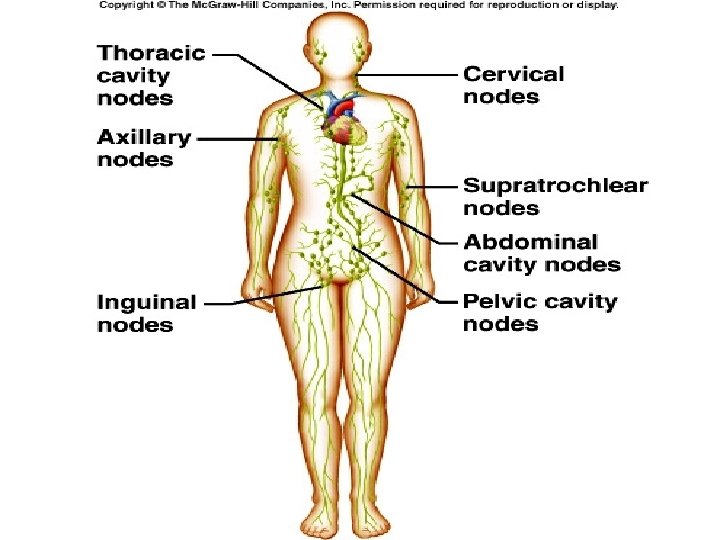

Other Lymphoid Organs • : Spleen, Thymus, Tonsils, Peyer’s patches • Spleen: Filters blood, Destroys worn out blood cells, Forms blood cells in the fetus, Acts as a blood reservoir. • Thymus: Located low in the throat, overlying the heart, Functions at peak levels only during childhood, Produces hormones (like thymosin) to program lymphocytes. Maturation of T-Cells • Tonsils: Trap and remove bacteria and other foreign materials, Tonsillitis is caused by congestion with bacteria • Peyer’s Patches: Capture and destroy bacteria in the intestine
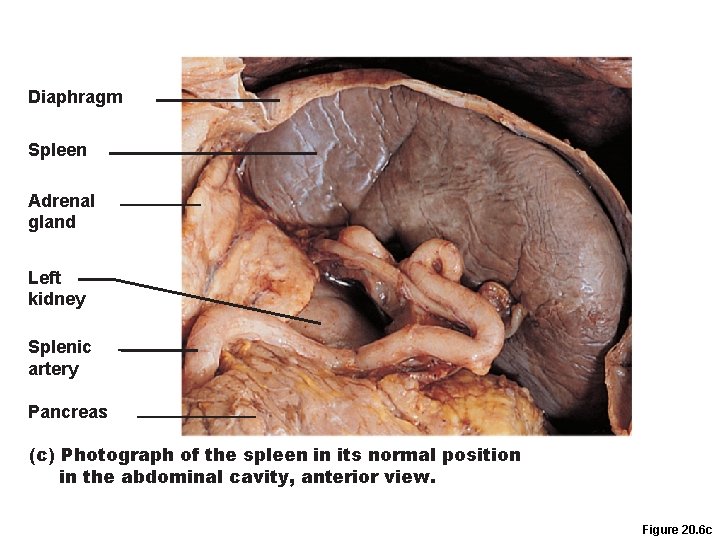
Diaphragm Spleen Adrenal gland Left kidney Splenic artery Pancreas (c) Photograph of the spleen in its normal position in the abdominal cavity, anterior view. Figure 20. 6 c

Immunity • Resistance to disease • Immune system has two intrinsic systems – Innate (nonspecific) defense system – Adaptive (specific) defense system
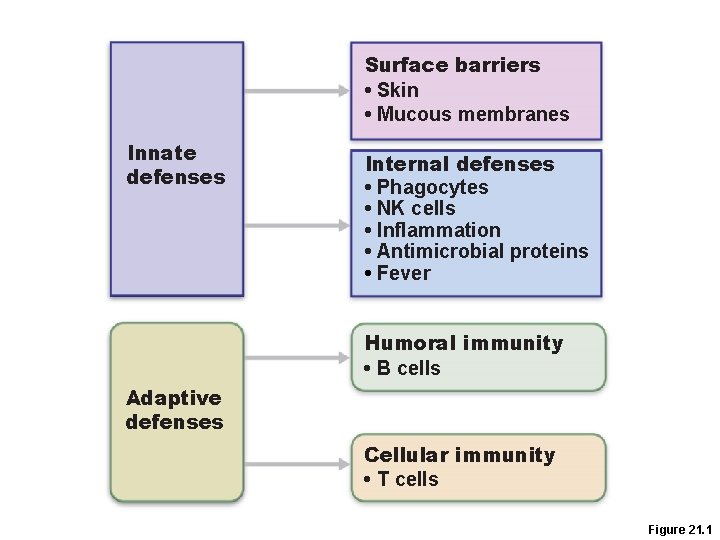
Surface barriers • Skin • Mucous membranes Innate defenses Internal defenses • Phagocytes • NK cells • Inflammation • Antimicrobial proteins • Fever Humoral immunity • B cells Adaptive defenses Cellular immunity • T cells Figure 21. 1

Lets Play Defense • The body has two defense systems foreign materials – Nonspecific defense system • Mechanisms protect against a variety of invaders, Responds immediately to protect body from foreign materials • Specific defense is required for each type of invader, Also known as the immune system

Nonspecific Body Defenses • The skin: • Stomach mucosa • Saliva and lacrimal fluid contain lysozyme • Mucus

Defensive Cells • Natural Killer Cells: lyse or kill viral infected cells and cancer cells. Tend to be non-specific in their chemical use of perforins. • Macrophages: Free or Fixed (microglial) • Neutrophils: phagocytic levels rise and fall • Dendritic Cells: Carry foreign bodies to lymph nodes • How Phagocytosis works: – Opsonization helps them adhere – Engulf via phagocytosis – Destroy with lysosomal enzymes
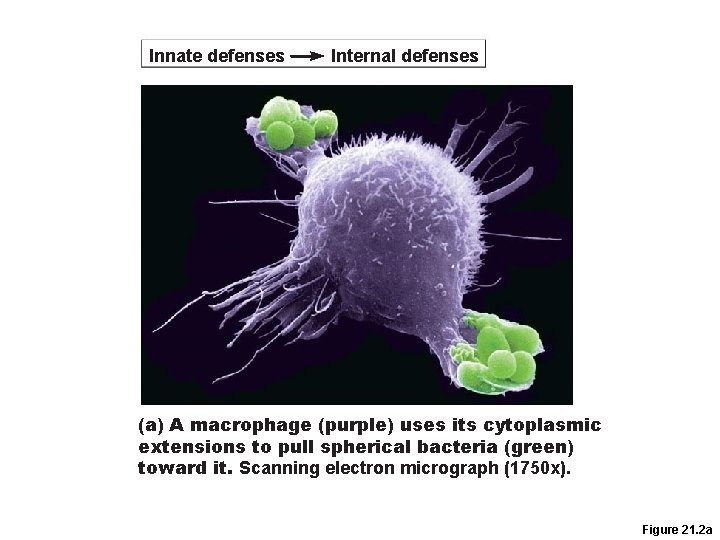
Innate defenses Internal defenses (a) A macrophage (purple) uses its cytoplasmic extensions to pull spherical bacteria (green) toward it. Scanning electron micrograph (1750 x). Figure 21. 2 a
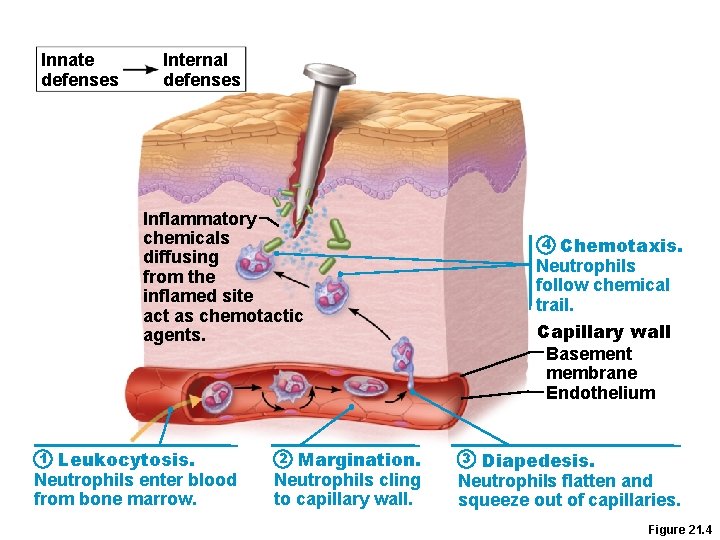
Innate defenses Internal defenses Inflammatory chemicals diffusing from the inflamed site act as chemotactic agents. Leukocytosis. Neutrophils enter blood from bone marrow. 1 Margination. Neutrophils cling to capillary wall. 2 Chemotaxis. Neutrophils follow chemical trail. 4 Capillary wall Basement membrane Endothelium Diapedesis. Neutrophils flatten and squeeze out of capillaries. 3 Figure 21. 4

Chemical Defense: • interferons- are proteins that are secreted by viral infected cells that bond to healthy cells and prevent virus from bonding. • Complement- 20 proteins that when activated can punch holes in infected cells literally blowing them up. • Collectins- are proteins that recognize foreign structure or sugar arrangement and stick
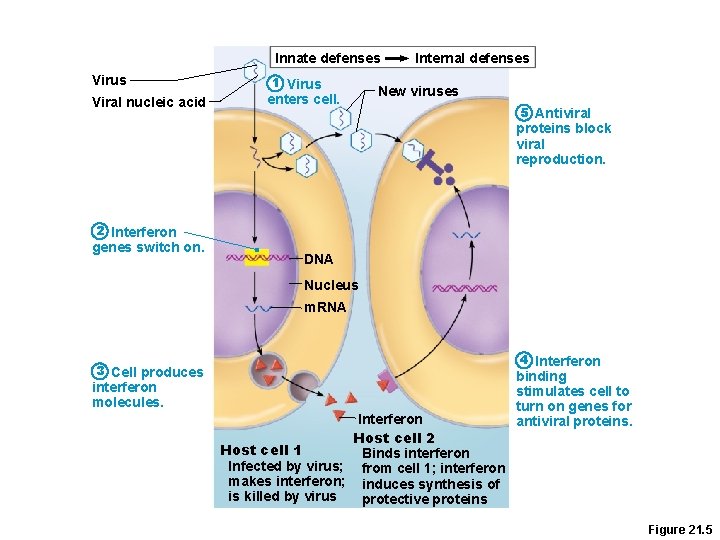
Innate defenses Virus Viral nucleic acid 1 Virus enters cell. Internal defenses New viruses 5 Antiviral proteins block viral reproduction. 2 Interferon genes switch on. DNA Nucleus m. RNA 4 Interferon 3 Cell produces interferon molecules. Interferon Host cell 2 Host cell 1 Binds interferon Infected by virus; from cell 1; interferon makes interferon; induces synthesis of is killed by virus protective proteins binding stimulates cell to turn on genes for antiviral proteins. Figure 21. 5
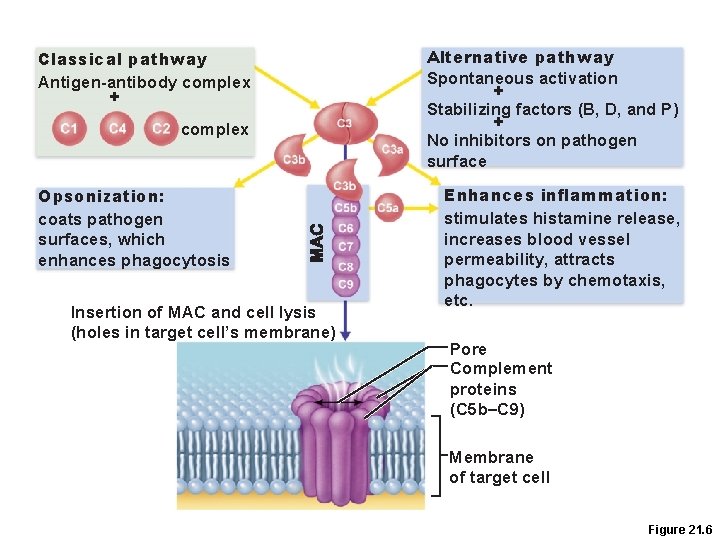
Classical pathway Antigen-antibody complex + complex Opsonization: coats pathogen surfaces, which enhances phagocytosis Insertion of MAC and cell lysis (holes in target cell’s membrane) Alternative pathway Spontaneous activation + Stabilizing factors (B, D, and P) + No inhibitors on pathogen surface Enhances inflammation: stimulates histamine release, increases blood vessel permeability, attracts phagocytes by chemotaxis, etc. Pore Complement proteins (C 5 b–C 9) Membrane of target cell Figure 21. 6

Cont. . • Fever: – Caused by pyrogens released from macrophages – High temperatures inhibit the release of iron and zinc from liver and spleen needed by bacteria – Fever also increases the speed of tissue repair • Inflammatory response. – chemical signals of the inflamatory response is histamine. basophils and mast cells – triggers both dilation and increased permeability of nearby capillaries.
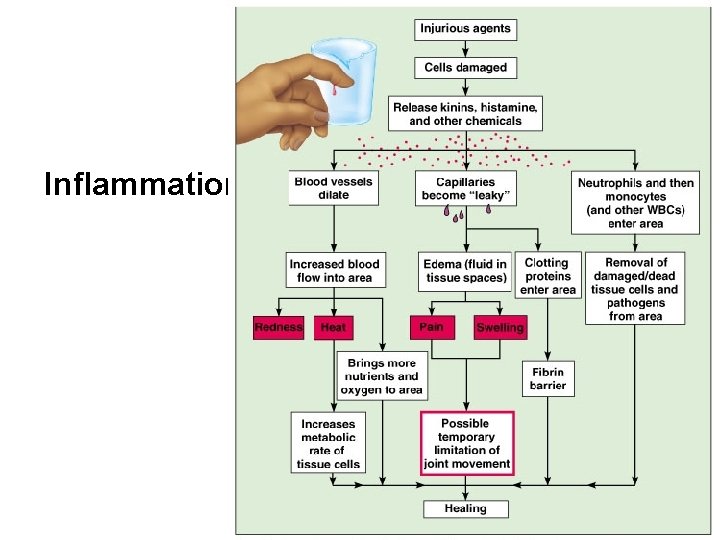
Inflammation

Immunity (Specific) • • • Antigen specific----Pathogen? Systemic Has memory Distinguish self from non-self Humoral immunity: Antibody-mediated. – B-cells • Cellular immunity: Cell-mediated immunity, – T-cells

Cont……. • Allergies: haptens or incomplete antigens) are not antigenic alone, but link up with our own proteins • The immune system may recognize and respond to a protein-hapten combination • Ex. Poison Ivy, Detergents, Pollen • Cells: Lymphocytes- Originate from hemocytoblasts in the red bone marrow and B lymphocytes become immunocompetent in the bone marrow T lymphocytes become immunocompetent in the thymus.

Antigen Receptor Diversity • Lymphocytes make up to a billion different types of antigen receptors – Coded for by ~25, 000 genes – Gene segments are shuffled by somatic recombination • Genes determine which foreign substances the immune system will recognize and resist

Cont… • Each antigen has a particular molecular shape and stimulates certain B cells to secrete antibodies that interact specifically with it • B and T cells recognize specific antigens through their plasma membrane-bound antigen receptors • single T or B lymphocyte bears about 100, 000 receptors for antigen, all with exactly the same specificity • Although it encounters a large repertoire of B cells and T cells, a microorganism interacts only with lymphocytes bearing receptors specific for its various antigenic molecules

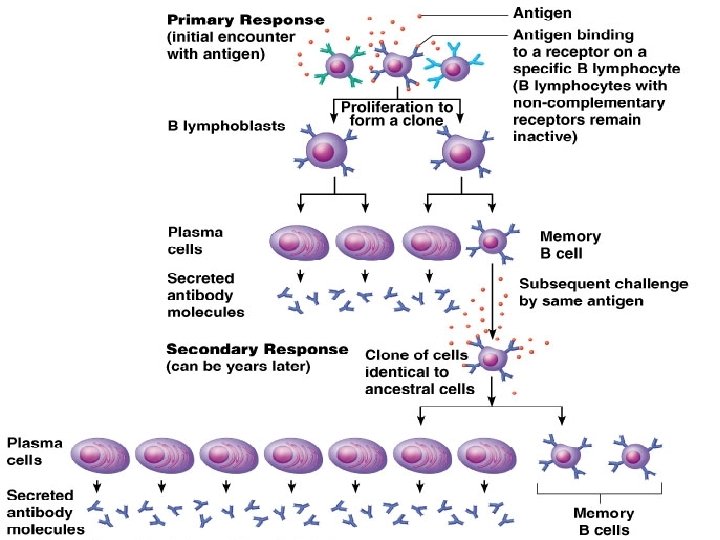
B - Cells • Plasma cells – secrete about 2, 000 antibody molecules per second over the cell’s 4 - to 5 -day life span • Memory cells • Clonal selection • This 1 st encounter is called the Primary Immune Response

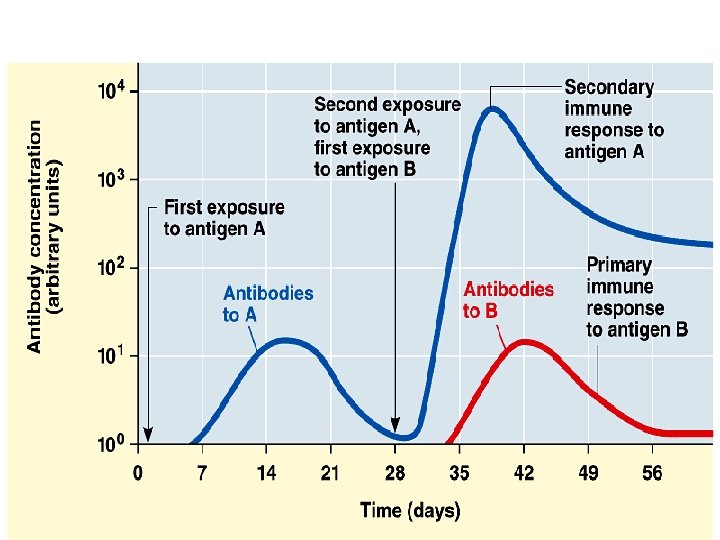
Cont… • Secondary immune response— stronger then the 1 st • response is faster (only 2 to 7 days), of greater magnitude, and more prolonged • immunological memory—the basis of the vaccine

Cell Mediated Immunity • B cells and T cells mature in the bone marrow and thymus, their antigen receptors are tested for potential self-reactivity • failures of self-tolerance can lead to autoimmune diseases • T cells do have a crucial interaction with one important group of native molecules whereas BCells do not • cell surface glycoproteins encoded by a family of genes called the major histocompatibility complex (MHC) mark body cells as self

Cont… • Class I MHC molecules- found on almost all nucleated cells • Class II MHC molecules macrophages, B cells, activated T cells, and those inside thymus • numerous possible alleles for each class I and class II MHC gene it is unlikely that any two people, except identical twins, will have exactly the same set of MHC molecules---Think transplant • MHC Molecules are antigen presenters • 2 main types of T cells, and each responds to one class of MCH molecule. – Cytotoxic T cells (TC) class I MHC molecules. – Helper T cells (TH) class II MCH molecules
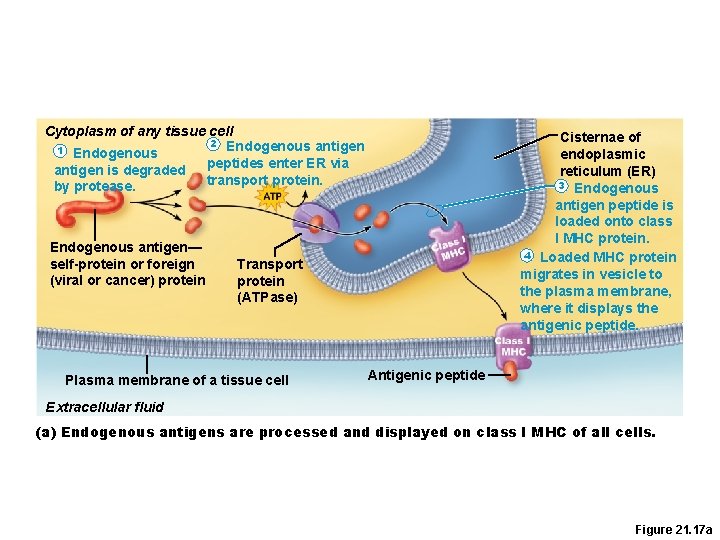
Cytoplasm of any tissue cell 2 Endogenous antigen 1 Endogenous peptides enter ER via antigen is degraded transport protein. by protease. Endogenous antigen— self-protein or foreign (viral or cancer) protein Cisternae of endoplasmic reticulum (ER) 3 Endogenous antigen peptide is loaded onto class I MHC protein. 4 Loaded MHC protein migrates in vesicle to the plasma membrane, where it displays the antigenic peptide. Transport protein (ATPase) Plasma membrane of a tissue cell Antigenic peptide Extracellular fluid (a) Endogenous antigens are processed and displayed on class I MHC of all cells. Figure 21. 17 a
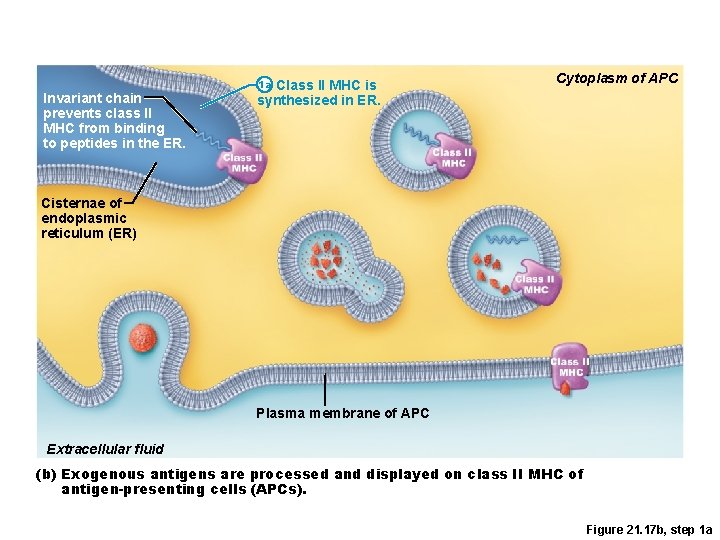
Invariant chain prevents class II MHC from binding to peptides in the ER. 1 a Class II MHC is synthesized in ER. Cytoplasm of APC Cisternae of endoplasmic reticulum (ER) Plasma membrane of APC Extracellular fluid (b) Exogenous antigens are processed and displayed on class II MHC of antigen-presenting cells (APCs). Figure 21. 17 b, step 1 a
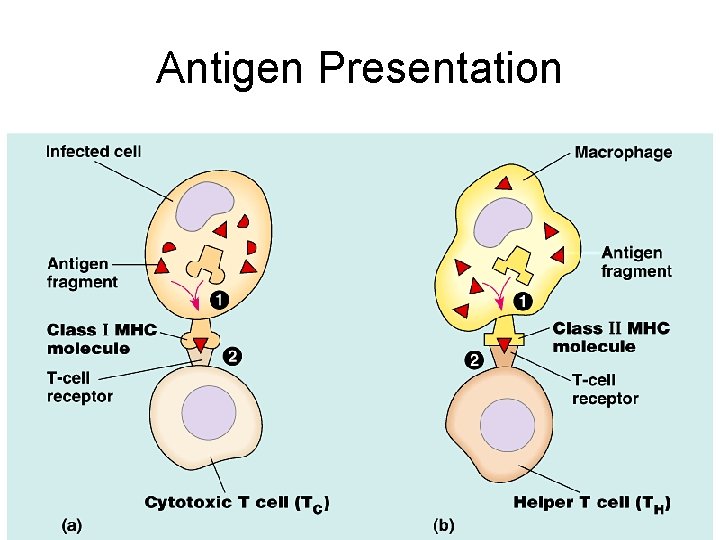
Antigen Presentation
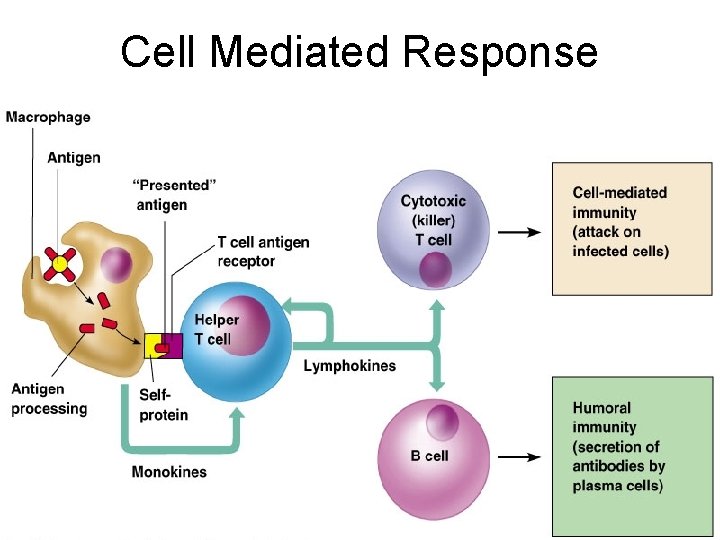
Cell Mediated Response
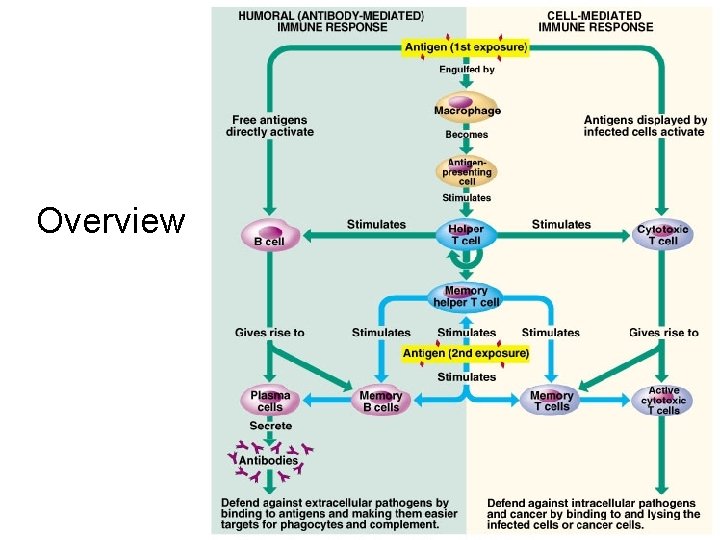
Overview
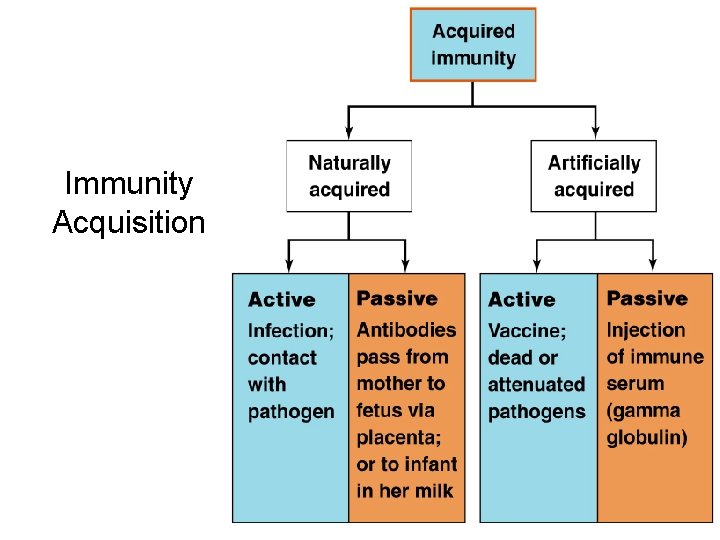
Immunity Acquisition

Antibodies • Y shaped proteins that are completely specific and have many uses for immunity and science. Also known as immunoglobulin (Igs) • secreted by B cells (plasma cells) • Carried in blood plasma • Capable of binding specifically to an antigen • 5 main types made of 4 amino acids chains linked by di-sulfide bonds.
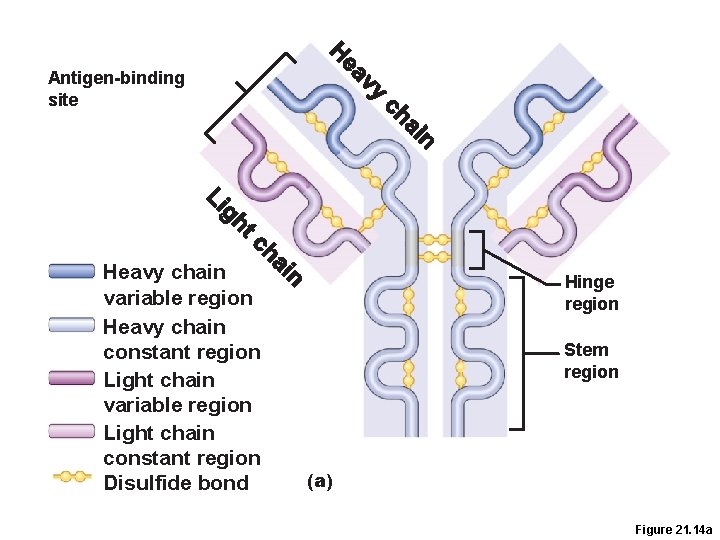
Antigen-binding site Heavy chain variable region Heavy chain constant region Light chain variable region Light chain constant region Disulfide bond Hinge region Stem region (a) Figure 21. 14 a
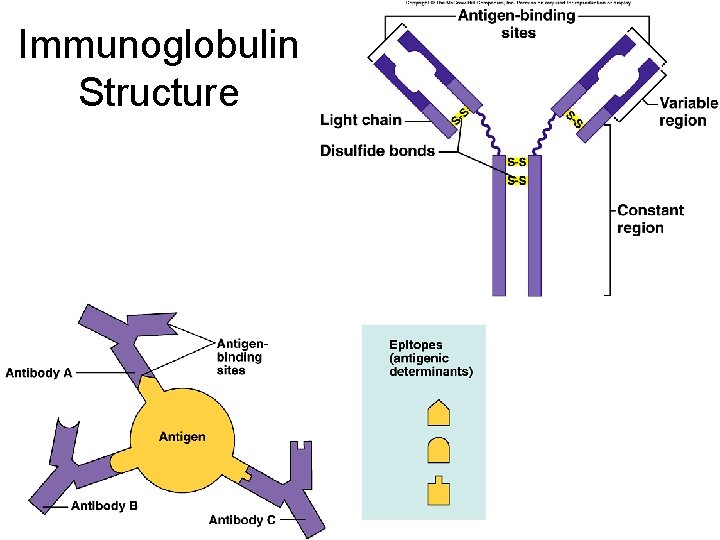
Immunoglobulin Structure

Types • Ig. G – activates complement – defends against bacteria, viruses, and toxins • Ig. A – defends against bacteria and viruses • Ig. M – reacts with naturally occurring antigens on RBCs following certain blood transfusions – activates complement • Ig. D – plays a role in B cell activation • Ig. E – promotes inflammation and allergic reactions

Review
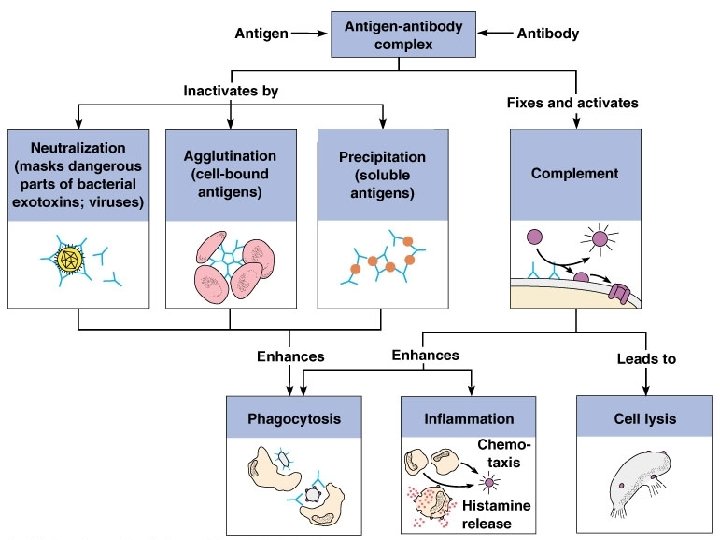
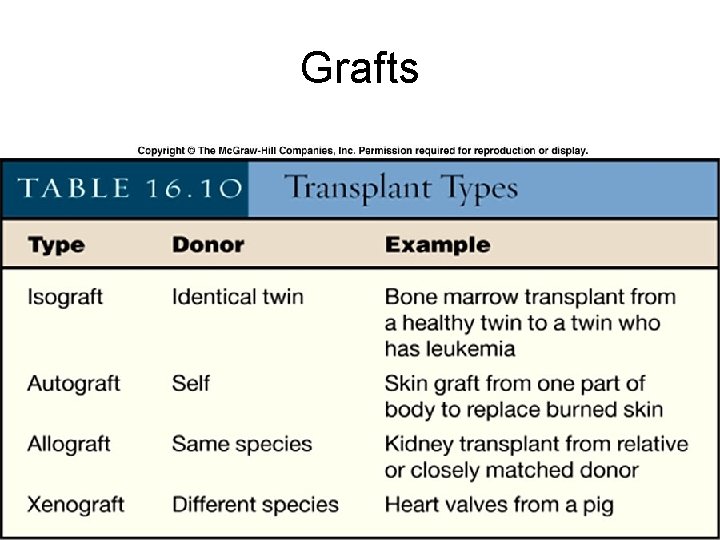
Grafts

Autoimmunity • The immune system does not distinguish between self and nonself • The body produces antibodies and sensitized T lymphocytes that attack its own tissues
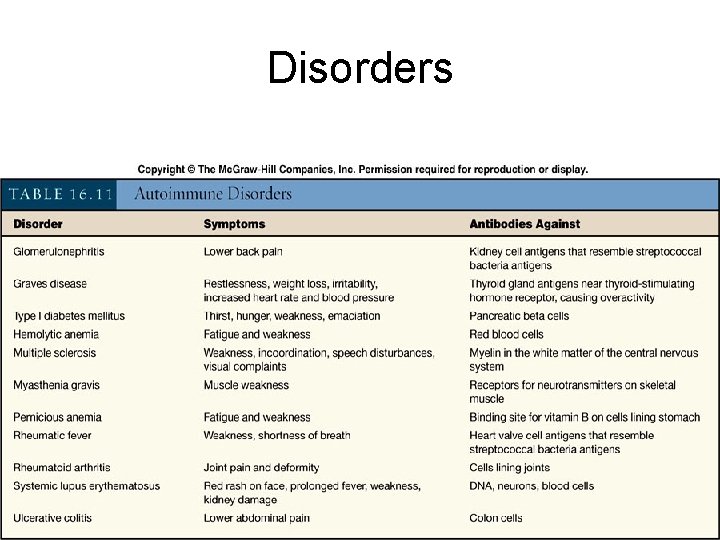
Disorders

Allergic Reactions • Type I: immediate-reaction allergy, hives, hay fever, asthma, eczema, gastric disturbances, anaphylactic shock- penicillin, or stings • Type II: antibody-dependent cytotoxic reaction – takes 1 -3 hours to develop – transfusion reaction • Type III: immune-complex reaction – antibody complexes cannot be cleared from body – damage of body tissues • Type IV – delayed-reaction allergy
- Slides: 54