THE INSIDE STORY OF BLOOD TRANSFUSION DR MOHAMED

THE INSIDE STORY OF BLOOD TRANSFUSION DR. MOHAMED BILAL DELVI ASSISTANT PROFESSOR DEPT OF ANAESTHESIA COLLEGE OF MEDICINE KSU. Done by : 428 surgery team 1

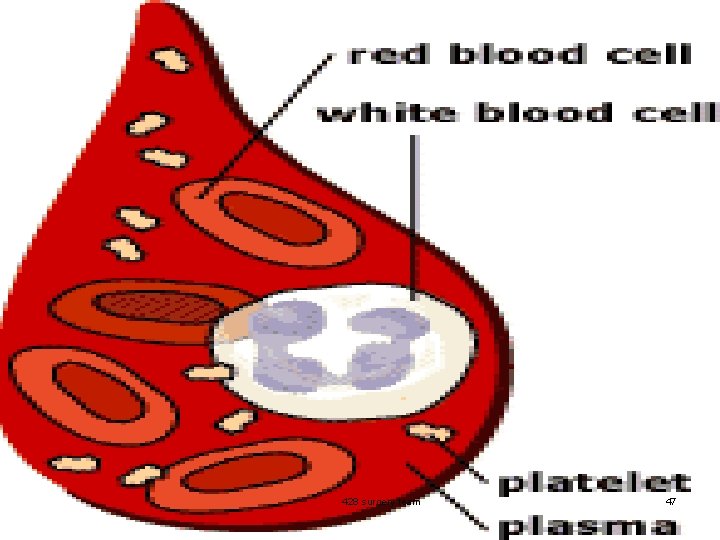
What is blood? n A highly specialised circulating tissue which has several types of cells suspended in a liquid medium called plasma. n Origins from Greek ‘haima’ n Blood is a life sustaining fluid 428 surgery team 2

n Blood is an amazing fluid! n Keeps us warm n Provides nutrients for cells, tissues and organs n Removes waste products from various sites 428 surgery team 3

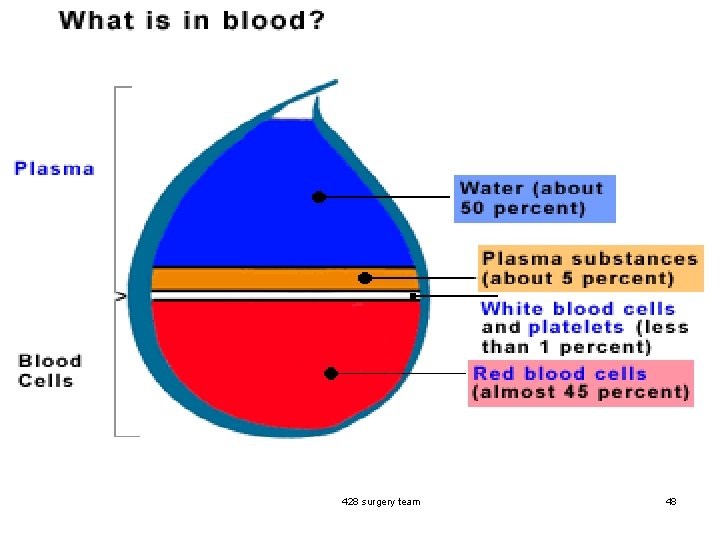
Blood Composition n Plasma: 55%. (50% water + 5% plasma substance) n Formed elements: 45%. n - RBC: live in circulation for 120 days. (near 45%) n - WBC: their life in circulation extends from months to years. n - Platelets: their life in circulation is 6 -10 days. WBC + platelets less than 1% 428 surgery team 4

Blood components n Blood Products: n Whole Blood n Packed red cells RBC. n Platelets concentrate. n White cell concentrate. n Plasma Products: n Fresh Frozen Plasma FFP. n Frozen plasma n Cryoprecipitate. n Albumin containing solution. n Human Immunoglobulins. n Prothrombin complex concentrate. n Factor VIII concentrates. 428 surgery team 5
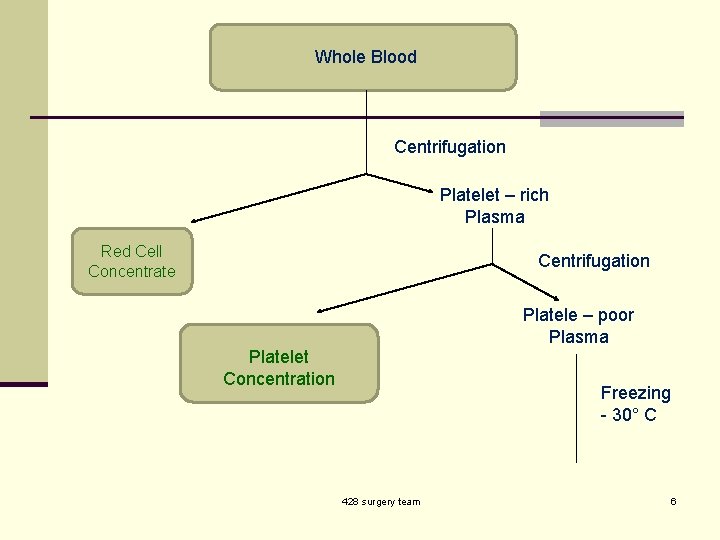
Whole Blood Centrifugation Platelet – rich Plasma Red Cell Concentrate Centrifugation Platele – poor Plasma Platelet Concentration Freezing - 30° C 428 surgery team 6
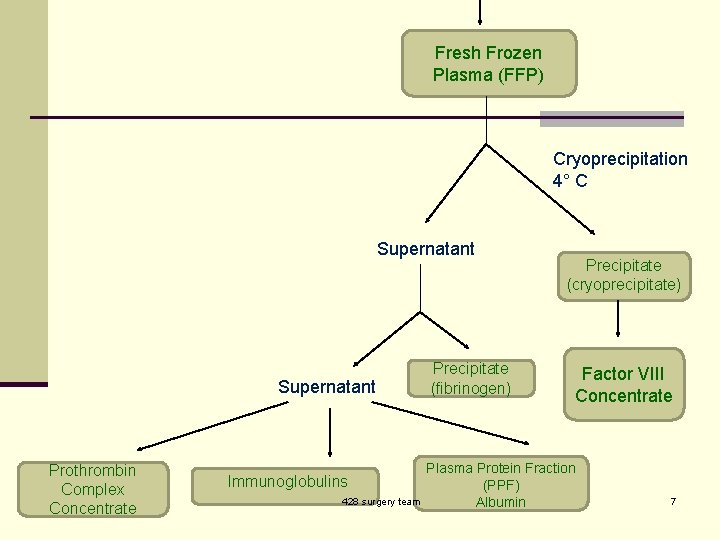
Fresh Frozen Plasma (FFP) Cryoprecipitation 4° C Supernatant Prothrombin Complex Concentrate Immunoglobulins 428 surgery team Precipitate (fibrinogen) Precipitate (cryoprecipitate) Factor VIII Concentrate Plasma Protein Fraction (PPF) Albumin 7

Packed Red Blood Cells n One unit contains 300 ml. n Out of this, 70% are RBC. n Indicated in: n - Acute blood loss, n - Chronic anemias. n Shelf life 42 days at 4 C 428 surgery team 8

Platelet Concentrate n One unit contains 50 x 109 platelets. n Usually 5 -6 units are given as one pool. n Indicated in: n - Bleeding due to platelet deficiency. n - Bleeding due to platelet dysfunction. n Shelf life 5 day at 22 C 428 surgery team 9

WBC Concentrate n Difficult to get sufficient quantities. n Half life is only 8 hours. n Rarely indicated because most patients respond to antibiotics and do not need white blood cells. n Nonhemolytic transfusion reactions are common. 428 surgery team 10

Plasma Products n 1. Fresh frozen plasma (FFP): n Stored at – 30° C. n Shelf life 1 year. n Rich in all components of plasma. n Indicated in: n - Disseminated intravascular coagulation (DIC). n - Liver failure. n - Warfarin overdose. n - Massive RBC transfusions. 428 surgery team 11

2 - Cryoprecipitate n Prepared from FFP after thawing it to 4° C. n When refrozen, the shelf life is 3 to 6 months. n Rich in factors VIII, XIII and VWF (Von Willebrand factor). n 3 - Factor VIII concentrate: n Prepared by fractionation of cryoprecipitate. n Large numbers of cryoprecipitate are required. n Indicated in hemophilia. Type A 428 surgery team 12

4 - prothrombin complex concentrate: n Contains factors II, VII, IX, and X. n Indicated in hemophilia B. n 5 - Human immunoglobulins: n Nonspecific immunoglobulins are used in: n n n n n - Congenital immunodeficiencies. - Acquired immunodeficiencies. - Idiopathic thrombocytopenia purpura (ITP). Specific immunoglobulins are used in: - Hepatitis B. - Herpes zoster. - Rubella. - Rabies. - Tetanus. 428 surgery team - Measles. 13

6 - Albumin containing solutions: n Used as plasma expander in severe hemorrhage while waiting for blood. n Also used to maintain plasma albumin levels in: n - Liver failure. n - Malnutrition. n - Protein losing states. 428 surgery team 14

Blood Types: n O Rh-positive n O Rh-negative n A Rh-positive n A Rh-negative n B Rh-positive n B Rh-negative n AB Rh-positive n AB Rh-negative 38% 7% universal donor 34% 6% 9% 2% 3% universal recipient 1% 428 surgery team 15
INDICATIONS FOR BLOOD TRANSFUSION n Massive blood loss – acute blood loss. n Different types of anaemia – chronic anemias. n Haemophilia & other clotting factor deficiency – chronic deficiency of any blood component. n Cancer patients n For surgeries 428 surgery team 16

HISTORICAL ASPECTS * 15 th century- unsuccessful attempts. n 1666 - dog to dog transfusion ( ﺑﻌﺾ ﺍﻟﺸﺒﺎﺏ ﻗﺎﻟﻮﺍ ﺟﺎ ﻋﻠﻴﻬﺎ ﺳﺆﺎﻝ ) n 1667 -animal to human n 1818 - human to human n 1901 - major breakthrough- discovery of A, B, O groups. 428 surgery team 17

HISTORICAL ASPECTS n 1907 - cross matching n 1914 - anticoagulant discovered n 1936 - first blood bank n 1939/40 - Rh factor discovery n 1950 - plastic blood containers. 428 surgery team 18
DOG TO DOG TRANSFUSION 428 surgery team 19
SHEEP TO HUMAN TRANSFUSION 428 surgery team 20
HUMAN TO HUMAN TRANSFUSION 428 surgery team 21

Theoretical Yield of components n 1 unit of blood theoretically gives n 1 unit FFP n 1 unit PRBC’s n 1 single donor unit cryoprecipitate, single donor unit platelets n Plasma for Ig and albumin 428 surgery team 22

BLOOD GROUP SYSTEMS n ABO System Most studied & important n Rh system from clinical point of view. n Lewis n Kell n Duffy 428 surgery team 23

BLOOD GROUP SYSTEMS n MNSs n Lutheran n P n Ii n kid 428 surgery team 24
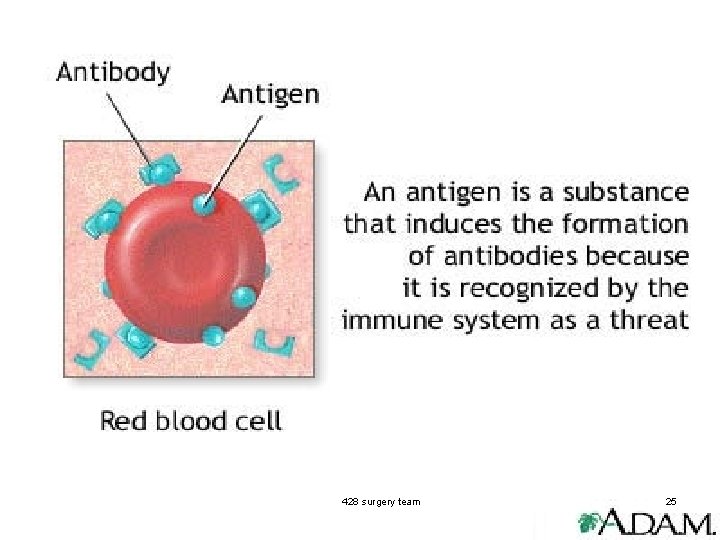
428 surgery team 25
DIFFERENT BLOOD GROUPS 428 surgery team 26
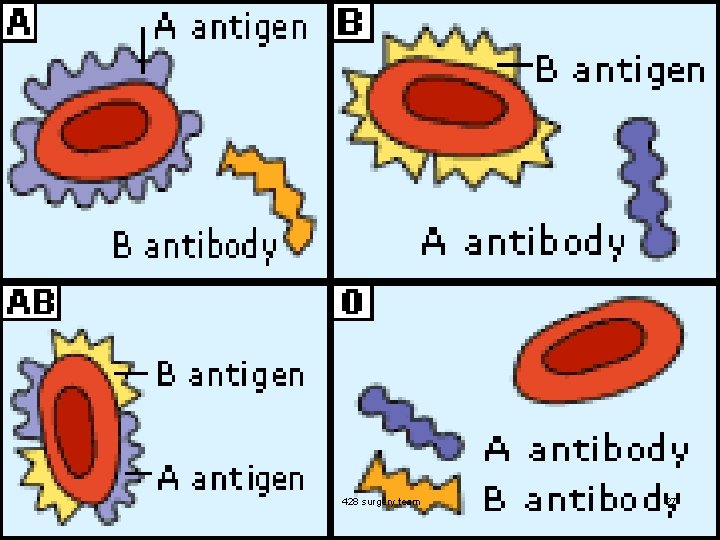
428 surgery team 27
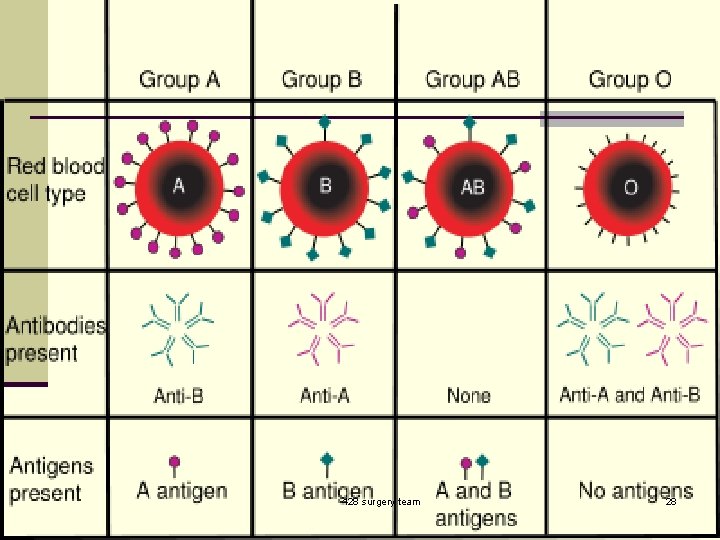
428 surgery team 28
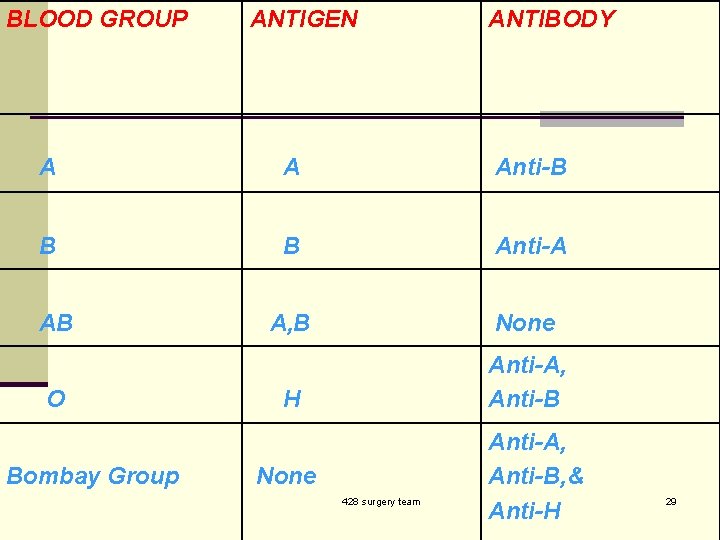
BLOOD GROUP ANTIGEN ANTIBODY A A Anti-B B B Anti-A A, B None H Anti-A, Anti-B AB O Bombay Group None 428 surgery team Anti-A, Anti-B, & Anti-H 29

RHESUS MONKEYS 428 surgery team 30
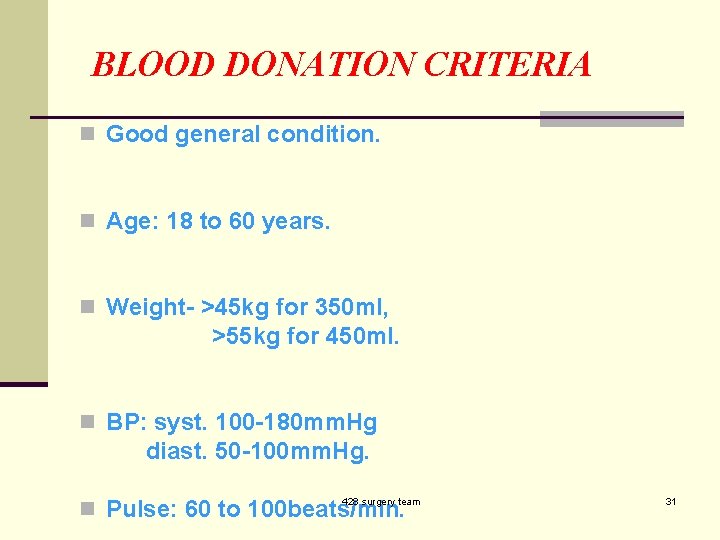
BLOOD DONATION CRITERIA n Good general condition. n Age: 18 to 60 years. n Weight- >45 kg for 350 ml, >55 kg for 450 ml. n BP: syst. 100 -180 mm. Hg diast. 50 -100 mm. Hg. n Pulse: 60 to 100 beats/min. 428 surgery team 31

BLOOD DONATION CRITERIA n Temp. >37. 5 deg. C n Hb. >12. 5 gm% n Jaundice n Malaria n High risk behaviour n Pregnancy 428 surgery team 32

BLOOD DONATION CRITERIA n Surgeries n Last blood donation n Tattooing n Chronic diseases n Last blood transfusion 428 surgery team 33

428 surgery team 34

INSTRUCTIONS TO DONOR AFTER DONATION n More fluids than usual. n Do not remain hungry. n Do not smoke for 1 hour. n Remove bandage after 6 hours. n If bleeding from puncture site, apply pressure. surgery team n If feeling faint/dizzy, lie 428 down. 35

MISCONCEPTIONS/ REASONS FOR NOT DONATING BLOOD n Fear of contracting some disease n I do not have enough blood/ I will become weak. n I am too old n I am too busy. 428 surgery team 36

REASONS TO DONATE BLOOD n New blood formation. n Regular health check up. n Blood investigations done. n Satisfaction of noble work. 428 surgery team 37

TESTS DONE IN BLOOD BANK n Blood grouping & Rh typing n Cross matching n Tests for irregular antibodies n HBs. Ag test & Anti-HBc n HCV test n HIV test (HIV 1 & HIV 2) n Test for syphilis n Test for malaria 428 surgery team 38

428 surgery team 39
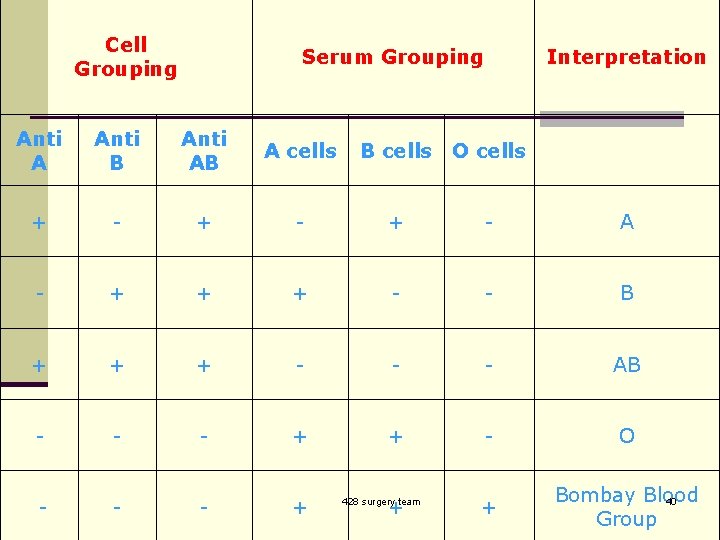
Cell Grouping Serum Grouping Interpretation Anti A Anti B Anti AB A cells + - + - A - + + + - - B + + + - - - AB - - - + + - O - - - + + + Bombay Blood 40 Group B cells O cells 428 surgery team
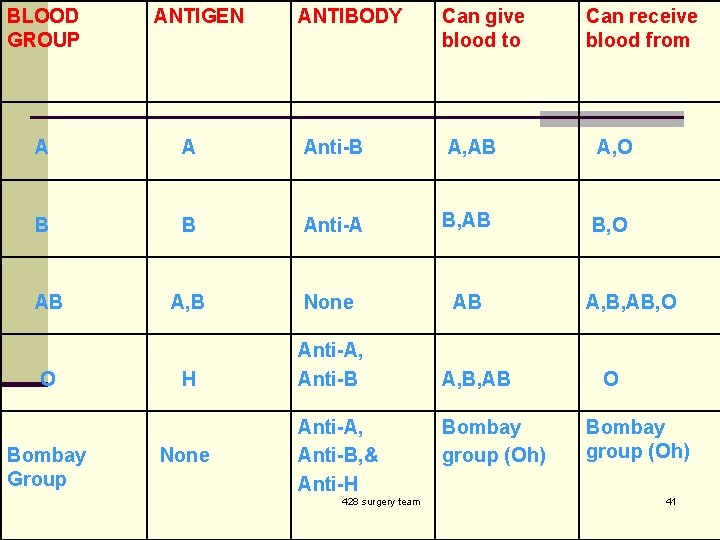
BLOOD GROUP ANTIGEN ANTIBODY Can give blood to Can receive blood from A A Anti-B A, AB A, O B B Anti-A B, AB B, O A, B None AB H Anti-A, Anti-B AB O Bombay Group None Anti-A, Anti-B, & Anti-H 428 surgery team A, B, AB Bombay group (Oh) A, B, AB, O O Bombay group (Oh) 41
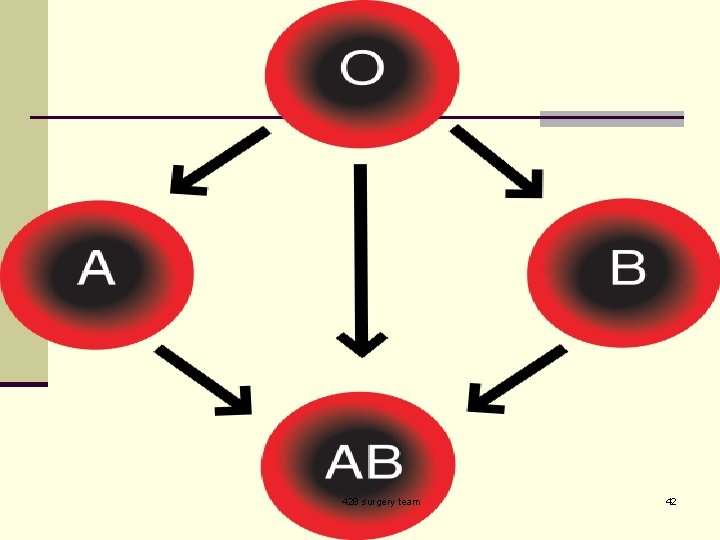
428 surgery team 42

Screening tests on donors’ blood: - Hepatitis B surface antigen (HBs. Ag). - Hepatitis B core antibody (anti-HBc). - Hepatitis C virus antibody (anti-HCV). - HIV-1 and HIV-2 antibody (anti-HIV-1 and anti-HIV-2). - HTLV-I and HTLV-II antibody (anti-HTLV-I and anti. HTLV-II). -Serologic test for syphilis. Prerequisites: -Take samples for full blood count (FBC), serum iron or ferritin B, and folate levels. - Cross match. - Choose the appropriate blood group in emergency. - Appropriate IV access. 428 surgery team 43
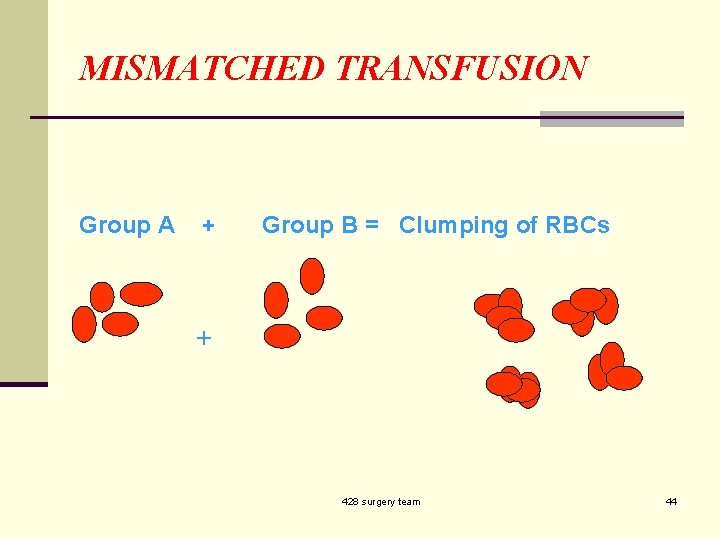
MISMATCHED TRANSFUSION Group A + Group B = Clumping of RBCs + 428 surgery team 44

AUTOLOGOUS DONATION n Self help is the best help. n Planned gynaecological, orthopedic, plastic general surgeries n Individuals with rare blood groups/ irregular antibodies/ infectious disease positive. 428 surgery team 45

AUTOLOGOUS DONATION Advantages n Safest blood. n Easy availability n No risk of TTDs n Best option in patients with irregular antibodies, rare blood groups, infectious disease positive. n Blood scarcity can be reduced to some extent. 428 surgery team 46
428 surgery team 47
428 surgery team 48
Blood Transfusion: A. Autologous: - Blood donor and transfusion recipient are the same in order to avoid blood borne diseases or infections. Four types: 1. Preoperative donations: - Donating the patient’s own blood before surgery. - The blood bank draws the patient’s blood and stores it until he/she needs it during or after surgery. - Only for elective surgery. 2. Preoperative hemodilution: - Immediately before surgery, some of the patient’s blood is taken and replace with IV fluids, i. e. normal saline. - Only for elective surgeries. 428 surgery team 49

3. Perioperative (intraoperative) collection: - Recycling the patient’s blood during surgery. - Blood lost during surgery is filtered, and put back into the patient’s body during surgery. - Can be done in emergency and elective surgeries. 4. Postoperative collection: - Recycling the patient’s blood after surgery. - Blood lost after surgery is collected, filtered and returned to the patient’s body. - Can be done in emergency and elective surgeries. 428 surgery team 50

B. Allogenic: Blood transfused to someone other than the donor. Practical tips: Give one unit over 4 hours. Use blood warmer if patient is hypothermic. Give 40 mg IV frusemide in between each unit. If possible, give transfusions early in the day. Check hemoglobin 24 -48 hours after transfusion. 428 surgery team 51

Complications of Transfusion: Transfusion reaction. Transmission of infections. Hyperkalemia. Hypocalcemia. Thrombocytopenia. Depletion of clotting factors. Transfusion reaction: Fever. Urticarial rash. Agitation. Chest or abdominal pain. Hypotension. Wheezing. Severe back pain. 428 surgery team 52

Management of transfusion reaction: Stop transfusion. Return the remaining blood to lab. Give 100 mg of hydrocortisone and 10 mg chlorpheniramine IV. Recheck the cross matches. Monitor vital signs. Monitor urine output. Inform your senior colleague. 428 surgery team 53
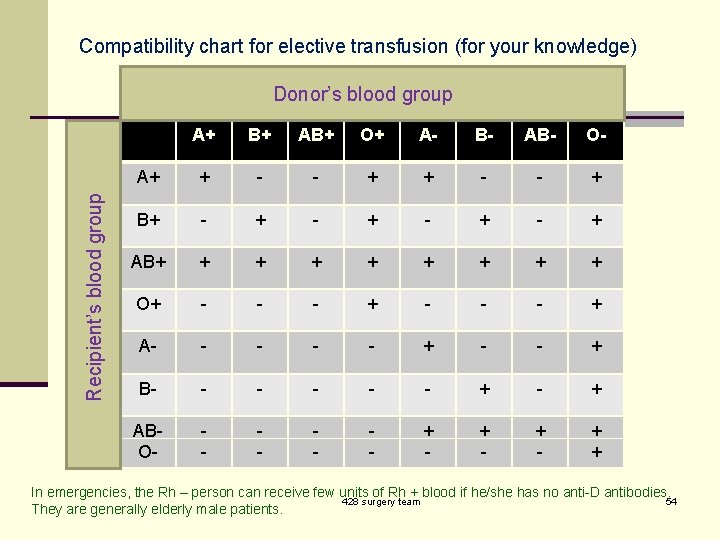
Compatibility chart for elective transfusion (for your knowledge) Recipient’s blood group Donor’s blood group A+ B+ AB+ O+ A- B- AB- O- A+ + - - + B+ - + - + AB+ + + + + O+ - - - + A- - - + B- - - + - + ABO- - - + - + + In emergencies, the Rh – person can receive few units of Rh + blood if he/she has no anti-D antibodies. 428 surgery team 54 They are generally elderly male patients.
BLOOD COMPONENTS n Blood separated into different parts. 1) Packed red cells 2) Platelets 3) Fresh frozen plasma 4) Cryoprecipitate 5) Granulocytes 6) Factor IX conc. 7) Factor VIII conc. 428 surgery team 55

COMPONENTS Advantages n Overload avoided. n Better patient management. n Greater shelf life than whole blood. n Blood shortage can be overcome. 428 surgery team 56
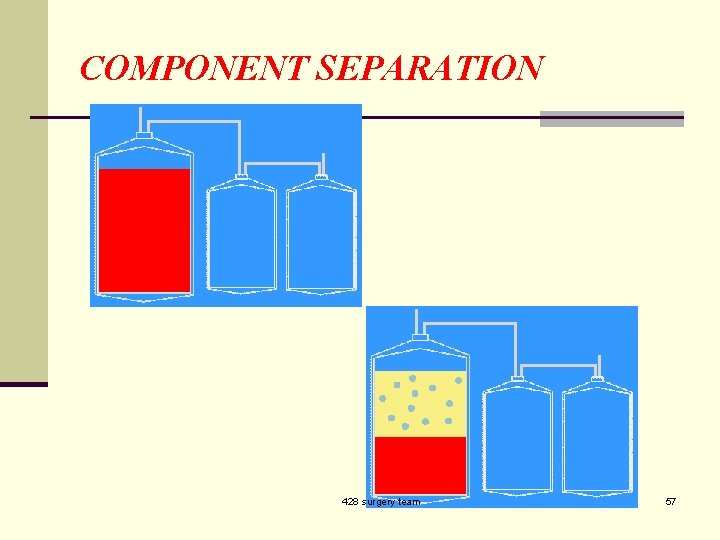
COMPONENT SEPARATION 428 surgery team 57
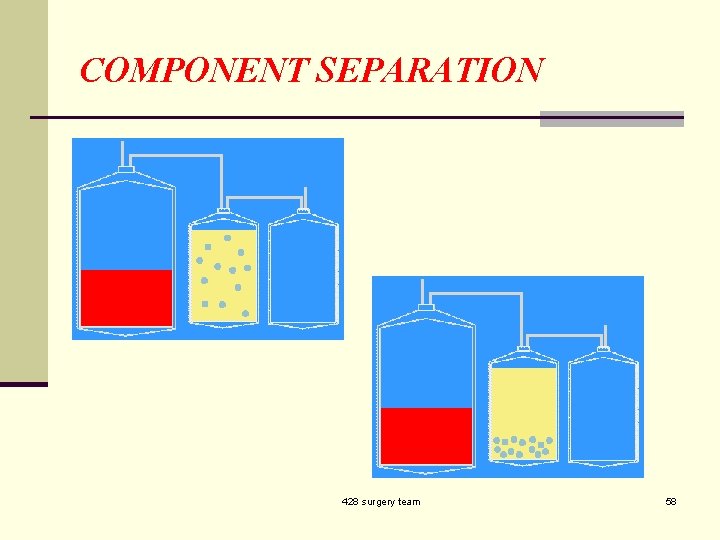
COMPONENT SEPARATION 428 surgery team 58
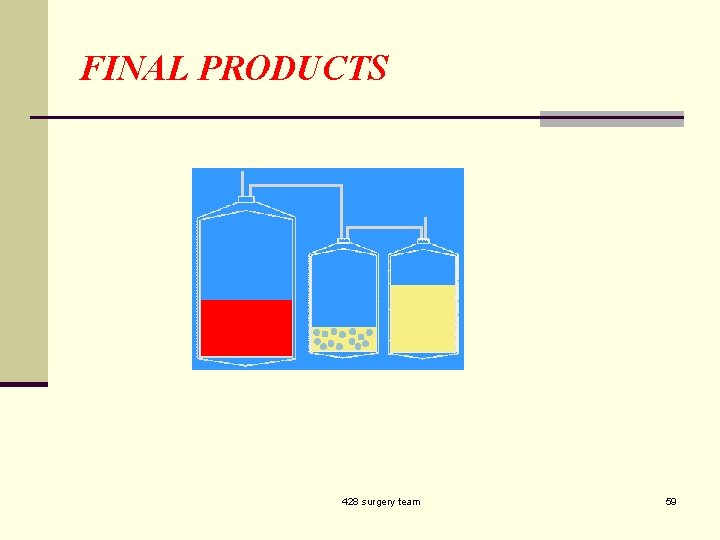
FINAL PRODUCTS 428 surgery team 59
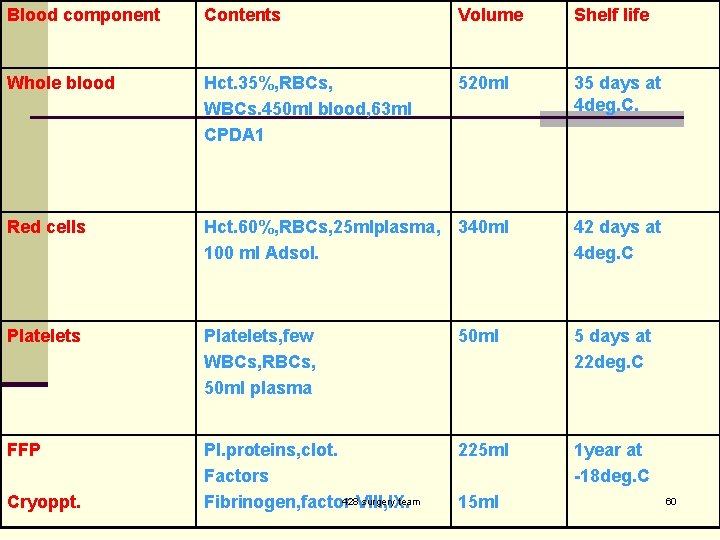
Blood component Contents Volume Shelf life Whole blood Hct. 35%, RBCs, WBCs. 450 ml blood, 63 ml CPDA 1 520 ml 35 days at 4 deg. C. Red cells Hct. 60%, RBCs, 25 mlplasma, 340 ml 100 ml Adsol. 42 days at 4 deg. C Platelets, few WBCs, RBCs, 50 ml plasma 50 ml 5 days at 22 deg. C FFP Pl. proteins, clot. Factors 428 VIII, IX. surgery team Fibrinogen, factor 225 ml 1 year at -18 deg. C Cryoppt. 15 ml 60
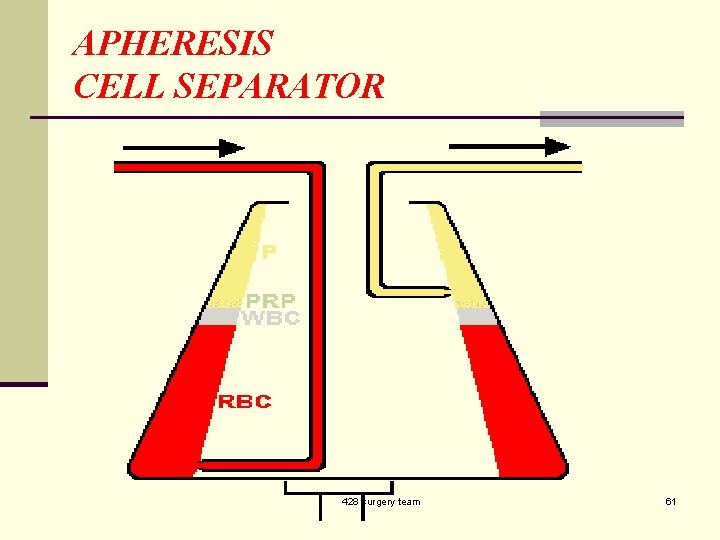
APHERESIS CELL SEPARATOR 428 surgery team 61

APHERESIS n Plasmapheresis: plasma is removed. n Plateletapheresis: platelets are removed. n Leukapheresis: leucocytes are removed. 428 surgery team 62

The rational use of blood and blood products 428 surgery team 63

BLOOD LOSS- Signs, Symptoms and Indication for Transfusion Volume Lost Clinical signs m. L % of Total Blood Volume 500 10 None; 1000 20 tachycardia 1500 30 drop in BP 2000 40 shock Preparation of choice No transfusion or crystalloid solution or colloids or RBC if necesssary crystalloid solution plus colloids plus RBC or blood if available 428 surgery team 64
RED CELLS TRANFUSION-Indication(1) 1. Whole blood • acute hypovolemia (hemorrhagic shock) • massive transfusion • exchange transfusion in infants for hemolytic anemia of the newborn 428 surgery team 65

Packed red cells n 150 -200 mls. of red cells with plasma removed n Haemoglobin 20 g/ 100 ml, PCV 55 -75 n Expected rise in Hb with 1 unit of red cells is approximately 1 g/d. L 428 surgery team 66
Indications for Packed Cells n Massive blood loss n Anaemia of chronic disease n Haemoglobinopathies n Perioperative period to maintain Hb> 7 g/d. L n No need for transfusion with Hb >10 428 surgery team 67

Platelets n 150 -400 x 109 /L n Platelet units can be either n n Single donor units Apheresis units n 1 single donor unit contains 55 x 109 n 1 apheresis unit contains 240 x 109 428 surgery team 68

Platelets n Stored at room temperature n Constantly agitated n Only last for 5 days n 1 dose of platelets should raise patient’s counts by 30 x 109 after 1 hour n Infused in 15 mins 428 surgery team 69

Indications for platelet transfusion n BLEEDING due to thrombocytopaenia n Due to platelet dysfunction n Prevention of spontaneous bleeding with counts < 20 428 surgery team 70
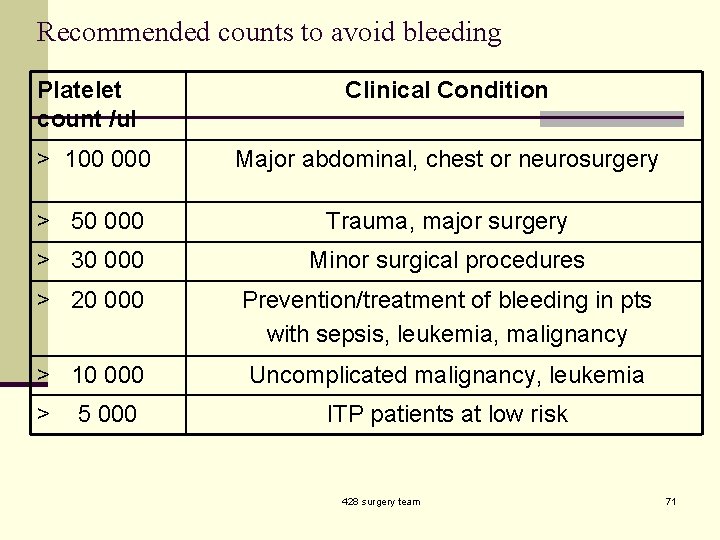
Recommended counts to avoid bleeding Platelet count /ul Clinical Condition > 100 000 Major abdominal, chest or neurosurgery > 50 000 Trauma, major surgery > 30 000 Minor surgical procedures > 20 000 Prevention/treatment of bleeding in pts with sepsis, leukemia, malignancy > 10 000 Uncomplicated malignancy, leukemia > 5 000 ITP patients at low risk 428 surgery team 71

FFP n Fresh Frozen Plasma collected from single donor units or by apheresis n Frozen within 8 hours of collection n -18 o to -30 o C n Can last for a year 428 surgery team 72

FFP n 1 unit is 250 ml n Contains all plasma proteins n Indications: n Correction of bleeding due to excess warfarin, Vitamin K deficiency, liver disease n DIC, dilutional coagulopathy n Inherited factor XI deficiency n TTP 428 surgery team 73

FFP n Dose: 15 mls/kg about 3 -5 units n FFP and INR <2 n Give at 1 ml/kg per hour in likely fluid overload patients n Given within 24 hours of thawing n Requesting FFP 428 surgery team 74

Frozen Plasma frozen within 24 hours of collection n Maintains level of plasma proteins except factor VIII n Same indications as FFP 428 surgery team 75

Cryoprecipitate n FFP thawed at 4 o. C and centrifuged n Cryoprecipitate is the by-product n Contains Fibrinogen, Factor VIII, Factor XIII, von Willebrand’s Factor 428 surgery team 76

Cryoprecipitate n No longer indicated for Hemophilia* n Source of Fibrinogen in acquired coagulopathies as in DIC; platelet dysfunction in uremia n Indicated for bleeding in v. WD, Factor XIII deficiency 428 surgery team 77

Cryoprecipitate n Infused as quickly as possible n Give within 6 hours of thawing n 10 -15 mls; usually 10 units pooled n 10 bags contain approx. 2 gm of fibrinogen and should raise fibrinogen level to 70 mg/d. L 428 surgery team 78

Almost there!!!!!!! 428 surgery team 79

Appropriateness of transfusion n May be life-saving n May have acute or delayed complications n Puts patient at risk unnecessarily n ‘ The transfusion of safe blood products to treat any condition leading to significant morbidity or mortality, that cannot be managed by any other means’. 428 surgery team 80

Inappropriateness of transfusion n Giving blood products for conditions that can otherwise be treated e. g. anaemia n Using blood products when other fluids work just as well n Blood is often unnecessarily given to raise a patient’s haemoglobin level before surgery or to allow earlier discharge from hospital. These are rarely valid reasons for transfusion. 428 surgery team 81

Inappropriateness of Transfusion n Patients’ transfusion requirements can often be minimized by good anaesthetic and surgical management. n Blood not needed exposes patient unnecessarily n Blood is an expensive, scarce resource. Unnecessary transfusions may cause a shortage of blood products for patients in real need. 428 surgery team 82

428 surgery team 83

Problems faced n Too few donors n Lack of equipment n Insufficient products n Insufficient reagent n Infectious disease testing 428 surgery team 84

Recommendations n Increase public awareness about need for blood and hence the number of voluntary donors n Continue to encourage relatives to donate for patients* n Increase the number of mobile clinics n Extend the opening hours for blood collecting 428 surgery team 85

Recommendations n Management of stocks of blood and blood products n Maintenance and replacement of equipment n On-going training of Haematology Lab Staff n Better management of reagents for- infectious disease testing, antigens etc. n Improved record keeping n Move to electronic record keeping 428 surgery team 86

Recommendations n View to reduce the need for allogeneic transfusions n Autologous transfusions n Blood saving devices in OR (operating room) n Acute normovolemic haemodilution n Oxygen carrying compounds 428 surgery team 87
428 surgery team 88

Bibliography n Uptodate. com n British Transfusion guidelines 2007 n Clinical use of blood, WHO n MJA: Tuckfield et al. , Reduction of inappropriate use of blood products n n n by prospective monitoring of blood forms Transfusion practice: Palo et al. , Population based audit of fresh frozen plasma transfusion practices Vox Sanguinis: Titlestead et al. , Monitoring transfusion practices at two university hospitals Transfusion: Schramm et al. , Influencing blood usage in Germany Transfusion: Healy et al. , Effect of Fresh Frozen Plasma on Prothrombin Time in patients with mild coagulation abnormalities Transfusion: Sullivan et al. , Blood collection and transfusion in the USA in 2001 Transfusion: Triulzi, The art of plasma transfusion therapy 428 surgery team 89

428 surgery team 90
- Slides: 90