The Incidence Correlates and Impact of Nuisance Bleeding

The Incidence, Correlates and Impact of “Nuisance” Bleeding in patients undergoing Intracoronary Drug-Eluting Stent Implantation Ron Waksman, MD Washington Hospital Center

DISCLOSURES Ron Waksman, MD Consulting Fees – Abbott Vascular, Biotronik, Medtronic Cardio. Vascular, Inc, Boston Scientific Corporation Grants/Contracted Research – Abbott Vascular, Biotronik, Boston Scientific Corporation, The Medicines Company, Glaxo. Smith. Kline, Schering-Plough, sanofi-aventis U. S. LLC

Background I • Studies assessing the efficacy and safety of prolonged dual anti-platelet therapy have reported bleeding events using the Thrombolysis in Myocardial Infarction (TIMI) and Global Use of Strategies to Open Coronary Arteries (GUSTO) bleeding criteria. • These definitions were established in the context of fibrinolytic therapy and may be less applicable in the current era of mechanical revascularization and prolonged dual anti-platelet therapy. • Most studies focus on major or severe bleeding and do not report mild bleeding events.

Define Nuisance Bleeding • Dictionary: an obnoxious or annoying person, thing, condition, practice, etc • In reality nuisance bleeding is bleeding that happens to somebody else. But it involves these skin ecchymoses and kinds of things that patients complain about. • In our center 10% of the patients who suffered a nuisance bleed stopped taking their medication. • There is increasing awareness that even nuisance bleeding complications are enough for some patients to stop therapy, especially since the benefits of antiplatelet therapy may not be readily apparent. Roy P, Waksman R, American Journal of Cardiology 2008

Background II • Superficial or “nuisance” bleeding is commonly encountered in patients taking dual anti-platelet therapy and may be the cause of premature clopidogrel cessation in some patients. • Early clopidogrel withdrawal post DES implantation is detrimental to prognosis and may be potentially avoided in patients with “nuisance” bleeding with better education and follow-up.

Objectives • To report the incidence of “nuisance” bleeding using a newly proposed bleeding classification in an unselected patient population undergoing intracoronary DES implantation at a single medical center. • To detect correlates for nuisance bleeding and its impact on clinical events. • Furthermore, to attempt to report the impact such bleeding events had on clopidogrel compliance

Methods: Study design and patient population • Single-center, observational study at the WHC. • The study cohort consisted of 2948 unselected patients who underwent successful DES implantation. • All bleeding events were recorded using a newly proposed bleeding classification. • Compliance with both aspirin and clopidogrel therapy following a bleeding event was recorded. • All patients gave written consent for the PCI procedure and the study was conducted under local Institutional Review Board approval.

Methods: Study design and patient population • The study endpoint was bleeding classified as alarming, internal, and superficial or “nuisance”. • Alarming bleeding was defined as bleeding which was intracranial, life-threatening, and required blood transfusion. • Internal bleeding included hematoma, epistaxis, mouth and vaginal bleeding, melena, eye bleed, hematuria and hematemesis. • “Nuisance” bleeding included easy bruising, bleeding from small cuts, petechia, and ecchymosis. • Interruption to aspirin and clopidogrel therapy at the time of bleeding was assessed as a dichotomous variable.
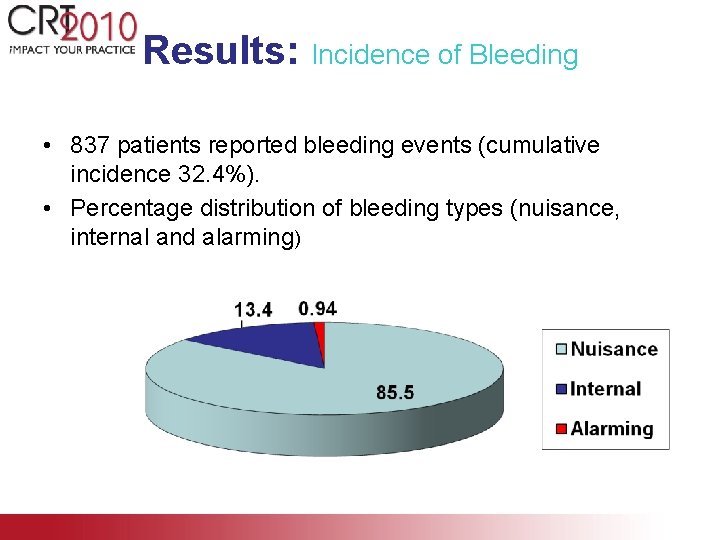
Results: Incidence of Bleeding • 837 patients reported bleeding events (cumulative incidence 32. 4%). • Percentage distribution of bleeding types (nuisance, internal and alarming)
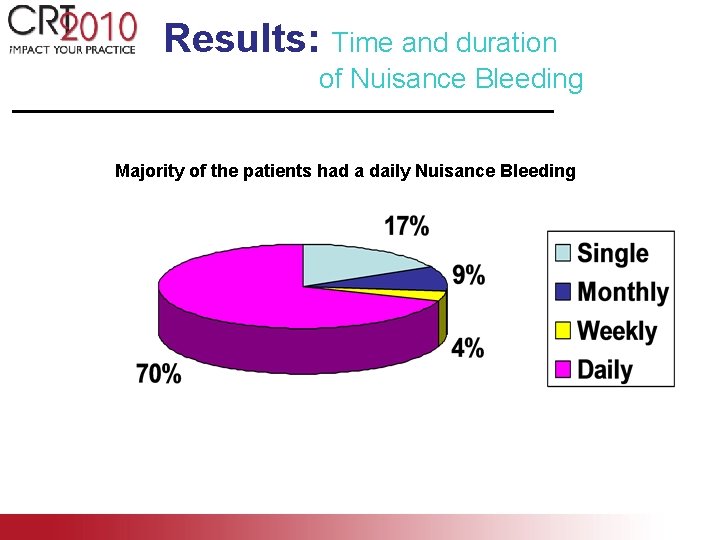
Results: Time and duration of Nuisance Bleeding Majority of the patients had a daily Nuisance Bleeding
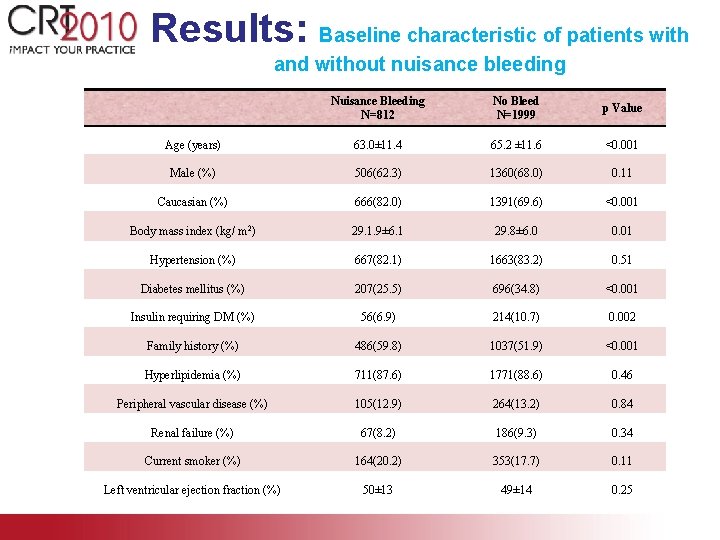
Results: Baseline characteristic of patients with and without nuisance bleeding Nuisance Bleeding N=812 No Bleed N=1999 p Value Age (years) 63. 0± 11. 4 65. 2 ± 11. 6 <0. 001 Male (%) 506(62. 3) 1360(68. 0) 0. 11 Caucasian (%) 666(82. 0) 1391(69. 6) <0. 001 Body mass index (kg/ m 2) 29. 1. 9± 6. 1 29. 8± 6. 0 0. 01 Hypertension (%) 667(82. 1) 1663(83. 2) 0. 51 Diabetes mellitus (%) 207(25. 5) 696(34. 8) <0. 001 Insulin requiring DM (%) 56(6. 9) 214(10. 7) 0. 002 Family history (%) 486(59. 8) 1037(51. 9) <0. 001 Hyperlipidemia (%) 711(87. 6) 1771(88. 6) 0. 46 Peripheral vascular disease (%) 105(12. 9) 264(13. 2) 0. 84 Renal failure (%) 67(8. 2) 186(9. 3) 0. 34 Current smoker (%) 164(20. 2) 353(17. 7) 0. 11 Left ventricular ejection fraction (%) 50± 13 49± 14 0. 25
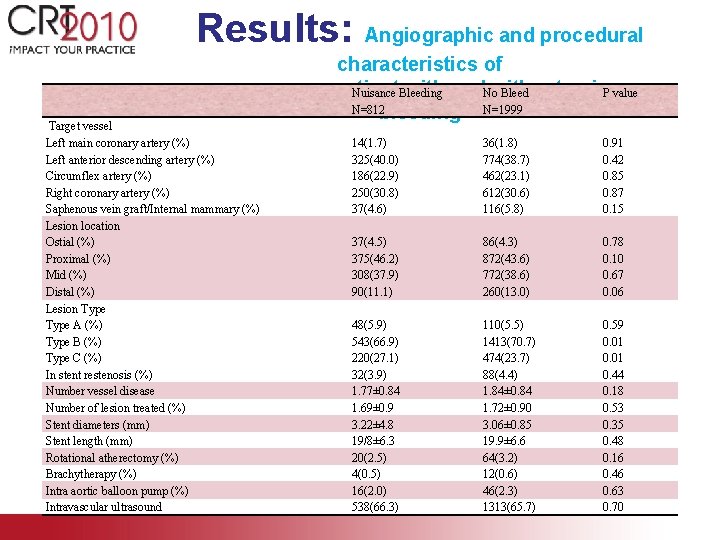
Results: Angiographic and procedural Target vessel Left main coronary artery (%) Left anterior descending artery (%) Circumflex artery (%) Right coronary artery (%) Saphenous vein graft/Internal mammary (%) Lesion location Ostial (%) Proximal (%) Mid (%) Distal (%) Lesion Type A (%) Type B (%) Type C (%) In stent restenosis (%) Number vessel disease Number of lesion treated (%) Stent diameters (mm) Stent length (mm) Rotational atherectomy (%) Brachytherapy (%) Intra aortic balloon pump (%) Intravascular ultrasound characteristics of patient with and. Nowithout nuisance Nuisance Bleeding Bleed P value N=812 bleeding N=1999 14(1. 7) 325(40. 0) 186(22. 9) 250(30. 8) 37(4. 6) 36(1. 8) 774(38. 7) 462(23. 1) 612(30. 6) 116(5. 8) 0. 91 0. 42 0. 85 0. 87 0. 15 37(4. 5) 375(46. 2) 308(37. 9) 90(11. 1) 86(4. 3) 872(43. 6) 772(38. 6) 260(13. 0) 0. 78 0. 10 0. 67 0. 06 48(5. 9) 543(66. 9) 220(27. 1) 32(3. 9) 1. 77± 0. 84 1. 69± 0. 9 3. 22± 4. 8 19/8± 6. 3 20(2. 5) 4(0. 5) 16(2. 0) 538(66. 3) 110(5. 5) 1413(70. 7) 474(23. 7) 88(4. 4) 1. 84± 0. 84 1. 72± 0. 90 3. 06± 0. 85 19. 9± 6. 6 64(3. 2) 12(0. 6) 46(2. 3) 1313(65. 7) 0. 59 0. 01 0. 44 0. 18 0. 53 0. 35 0. 48 0. 16 0. 46 0. 63 0. 70
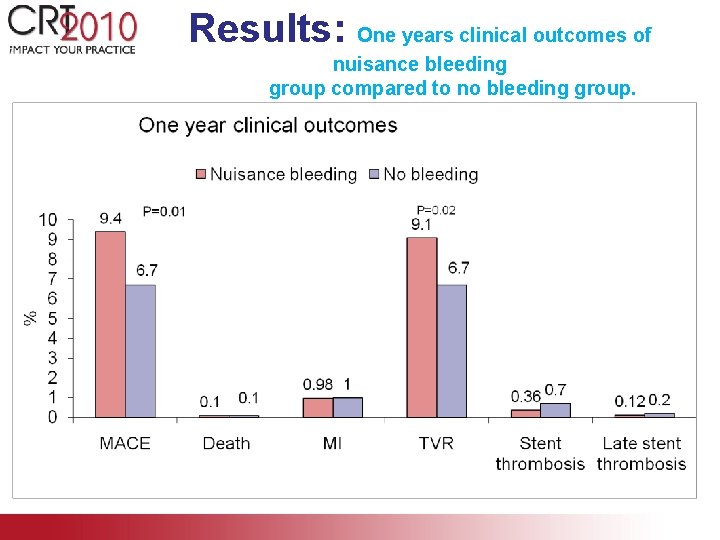
Results: One years clinical outcomes of nuisance bleeding group compared to no bleeding group.
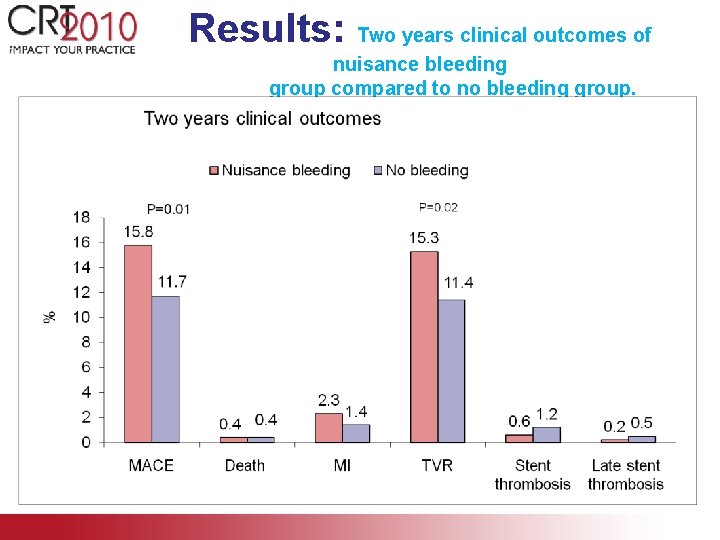
Results: Two years clinical outcomes of nuisance bleeding group compared to no bleeding group.
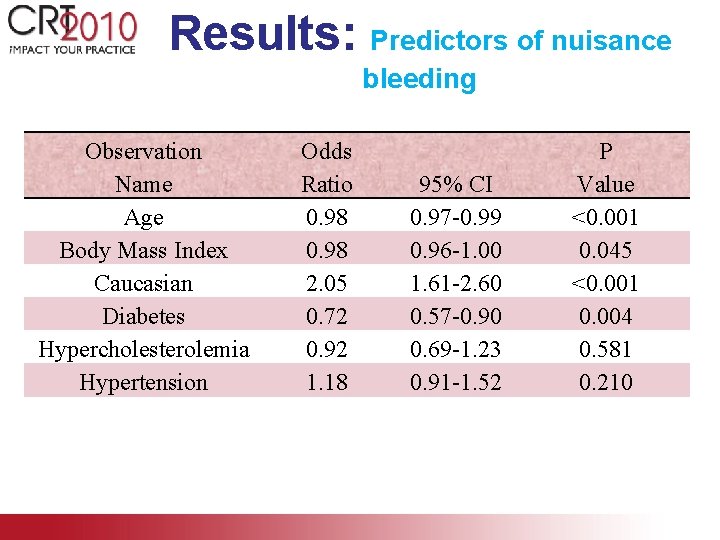
Results: Predictors of nuisance bleeding Observation Name Age Body Mass Index Caucasian Diabetes Hypercholesterolemia Hypertension Odds Ratio 0. 98 2. 05 0. 72 0. 92 1. 18 95% CI 0. 97 -0. 99 0. 96 -1. 00 1. 61 -2. 60 0. 57 -0. 90 0. 69 -1. 23 0. 91 -1. 52 P Value <0. 001 0. 045 <0. 001 0. 004 0. 581 0. 210
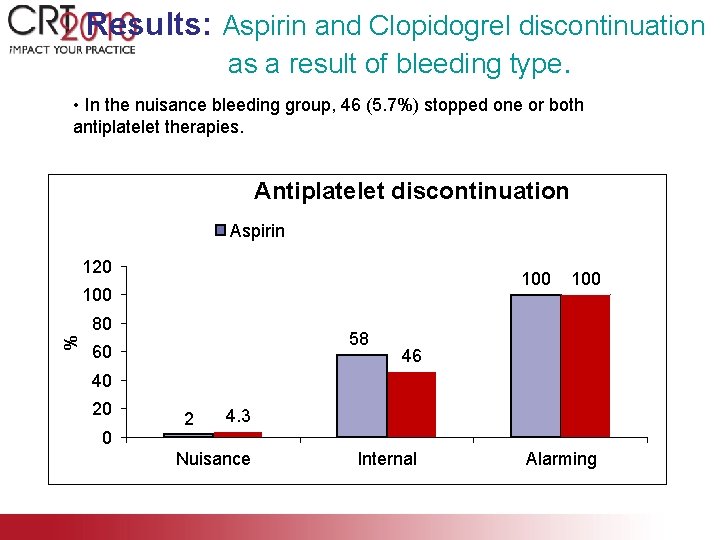
Results: Aspirin and Clopidogrel discontinuation as a result of bleeding type. • In the nuisance bleeding group, 46 (5. 7%) stopped one or both antiplatelet therapies. Antiplatelet discontinuation Aspirin 120 100 % 80 58 60 100 46 40 20 0 2 4. 3 Nuisance Internal Alarming
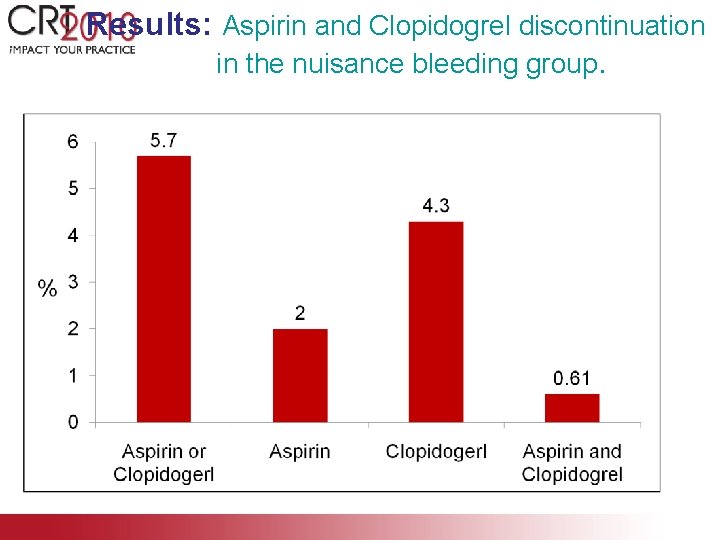
Results: Aspirin and Clopidogrel discontinuation in the nuisance bleeding group.
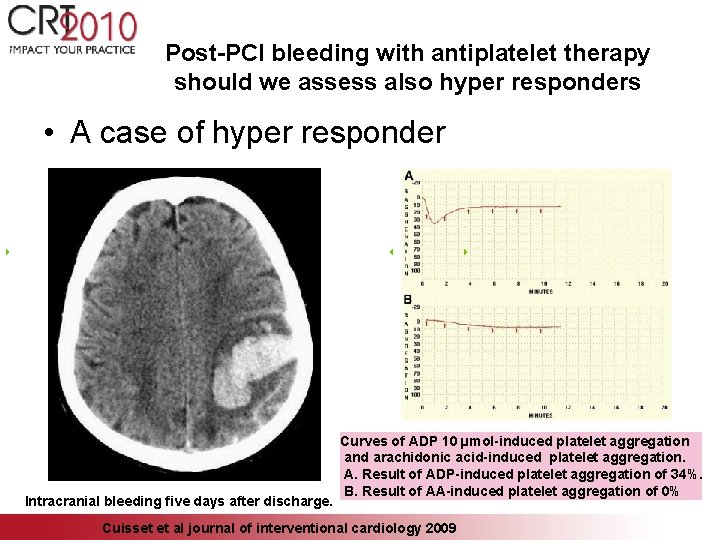
Post-PCI bleeding with antiplatelet therapy should we assess also hyper responders • A case of hyper responder Intracranial bleeding five days after discharge. Curves of ADP 10 µmol-induced platelet aggregation and arachidonic acid-induced platelet aggregation. A. Result of ADP-induced platelet aggregation of 34%. B. Result of AA-induced platelet aggregation of 0% Cuisset et al journal of interventional cardiology 2009
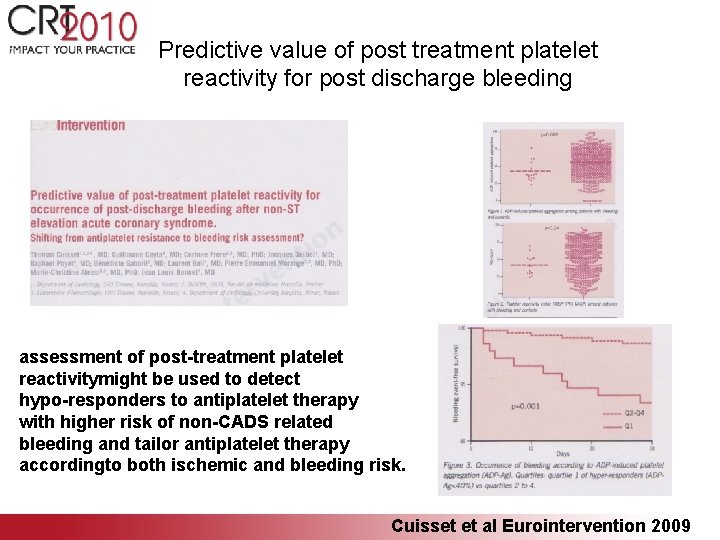
Predictive value of post treatment platelet reactivity for post discharge bleeding assessment of post-treatment platelet reactivitymight be used to detect hypo-responders to antiplatelet therapy with higher risk of non-CADS related bleeding and tailor antiplatelet therapy accordingto both ischemic and bleeding risk. Cuisset et al Eurointervention 2009

Conclusions • Nuisance bleeding is common in patients taking dual antiplatelet therapy post PCI with drug eluting stents and results with cessation of antiplatelet therapy. • Greater education and follow-up in this patient subset may lead to improved compliance with clopidogrel therapy. • Platelet reactivity studies should be considered once the criteria for Nuisance Bleeding are defined
- Slides: 20