The Impact of Return of Unsolicited Results on























- Slides: 29

The Impact of Return of Unsolicited Results on Health Care Providers (HCPs) in e. MERGE III: Preliminary Findings June 21, 2019 Ingrid A. Holm, MD, MPH On behalf of the HCP R 01 Team

HCP Core group NHGRI R 01 • • • Ingrid Holm – BCH Jill Madden – BCH Melanie Myers – CCHMC Janet Williams – Geisinger Kathy Leppig – KP/UW Georgia Wiesner – Vanderbilt Ellen Clayton – Vanderbilt Kyle Brothers – Louisville Sonja Ziniel – Survey methodologist Subcontracts to 9 clinical sites

Background Little is known concerning the views, concerns, and challenges for HCP regarding the desirability, utility, actionability, and meaning of incorporating results of genome sequencing (targeted sequencing of disease gene panels, WES, WGS) into clinical care HCP surveys were not part of the plan at most sites

Significance • The e. MERGE III Network is one of the first in which unsolicited genomic results will be returned to HCPs on a large scale. • We will leverage this unique opportunity to study the impact of genomic results disclosure in a real world setting, including the HCPs’ perceptions of their role and responsibilities, their actions and barriers to actions.

Aims 1. Survey participant’s HCPs (primary care +/- subspecialists) one month after receiving an unsolicited positive GS result. 2. Conduct in-depth qualitative interviews at four representative e. MERGE sites: • Within 6 months after a HCP receives a positive result, assess 1) actions taken in response to the result and 2) ELSI of receiving the result on HCPs. • In HCPs at sites where negative results are reported, assess whether HCPs took any actions in response to this information. 3. Identify approaches to returning unsolicited GS results that overcome barriers to HCPs acting on genomic results, and that facilitate interactions between HCPs and patients in the return and follow-up of the results. HCP data will be integrated with data collected by the Outcomes Workgroup and the Participant Survey Subgroup correlating the HCP self-reported data with impact on health service utilization, medical outcomes, and participant self-reported data.

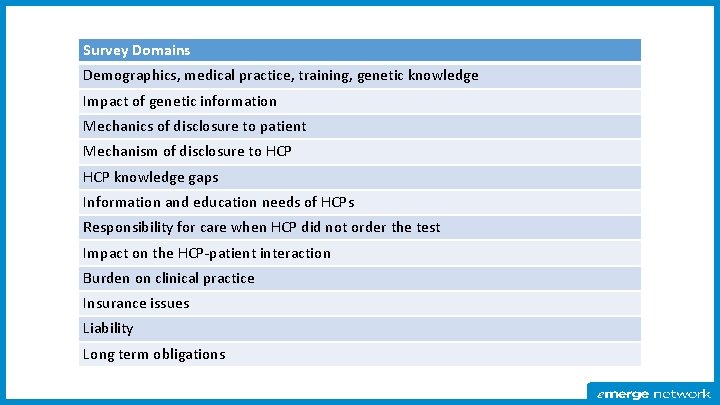
Survey Domains Demographics, medical practice, training, genetic knowledge Impact of genetic information Mechanics of disclosure to patient Mechanism of disclosure to HCP knowledge gaps Information and education needs of HCPs Responsibility for care when HCP did not order the test Impact on the HCP-patient interaction Burden on clinical practice Insurance issues Liability Long term obligations

Enrollment to date Emails invitations sent Email surveys completed Email response rate 306 115 38% Mailed invitations sent Mailed surveys completed Mail response rate 136 11 8% Total invitations sent Total surveys completed Total response rate 442 126 29%

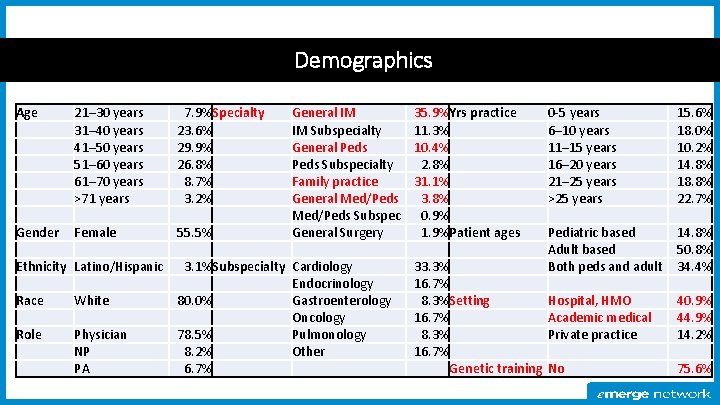
Demographics Age 21– 30 years 31– 40 years 41– 50 years 51– 60 years 61– 70 years >71 years 7. 9%Specialty 23. 6% 29. 9% 26. 8% 8. 7% 3. 2% Gender Female 55. 5% Ethnicity Latino/Hispanic Race White Role Physician NP PA General IM IM Subspecialty General Peds Subspecialty Family practice General Med/Peds Subspec General Surgery 3. 1%Subspecialty Cardiology Endocrinology 80. 0% Gastroenterology Oncology 78. 5% Pulmonology 8. 2% Other 6. 7% 35. 9%Yrs practice 11. 3% 10. 4% 2. 8% 31. 1% 3. 8% 0. 9% 1. 9%Patient ages 33. 3% 16. 7% 8. 3%Setting 16. 7% 8. 3% 16. 7% Genetic training 0 -5 years 6– 10 years 11– 15 years 16– 20 years 21– 25 years >25 years 15. 6% 18. 0% 10. 2% 14. 8% 18. 8% 22. 7% Pediatric based Adult based Both peds and adult 14. 8% 50. 8% 34. 4% Hospital, HMO Academic medical Private practice 40. 9% 44. 9% 14. 2% No 75. 6%

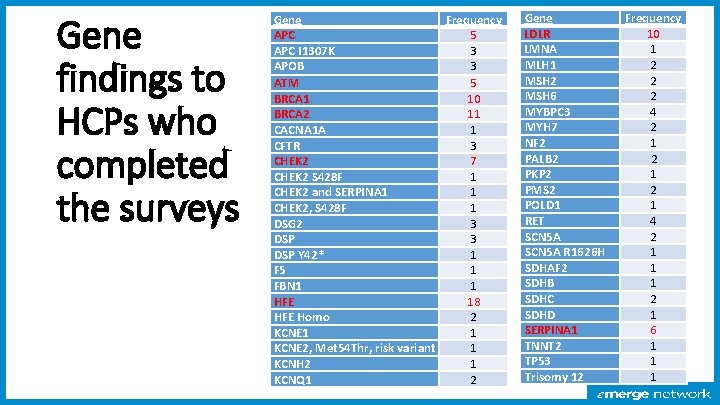
Gene findings to HCPs who completed the surveys Gene Frequency APC 5 APC I 1307 K 3 APOB 3 ATM 5 BRCA 1 10 BRCA 2 11 CACNA 1 A 1 CFTR 3 CHEK 2 7 CHEK 2 S 428 F 1 CHEK 2 and SERPINA 1 1 CHEK 2, S 428 F 1 DSG 2 3 DSP Y 42* 1 F 5 1 FBN 1 1 HFE 18 HFE Homo 2 KCNE 1 1 KCNE 2, Met 54 Thr, risk variant 1 KCNH 2 1 KCNQ 1 2 Gene LDLR LMNA MLH 1 MSH 2 MSH 6 MYBPC 3 MYH 7 NF 2 PALB 2 PKP 2 PMS 2 POLD 1 RET SCN 5 A R 1626 H SDHAF 2 SDHB SDHC SDHD SERPINA 1 TNNT 2 TP 53 Trisomy 12 Frequency 10 1 2 2 2 4 2 1 2 1 4 2 1 1 1 2 1 6 1 1 1

“Initial reactions to receiving the unsolicited genomic result Strongly Somewhat Strongly for this patient” Positive Negative Surprised Ambivalent disagree 11. 1% 50. 0% 12. 8% 40. 6% disagree 8. 6% 20. 8% 20. 5% 20. 3% agree 46. 9% 15. 3% 42. 3% 30. 4% “To what extent do you agree with the following statements about receiving this …result? ” The result was informative The result was confusing The result was helpful The result was useless Strongly disagree 10. 7% 38. 8% 9. 8% 56. 0% Somewhat disagree 11. 9% 26. 2% 18. 3% 26. 7% Somewhat agree 41. 7% 5. 0% 26. 8% 5. 3% Strongly agree 35. 7% 30. 0% 45. 1% 12. 0% agree 33. 3% 13. 9% 24. 4% 8. 7%

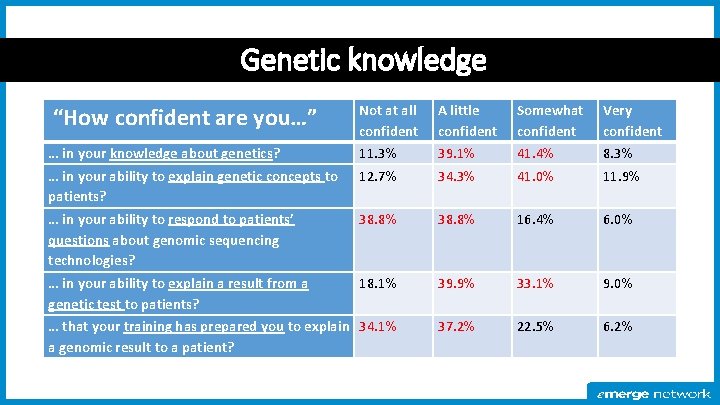
Genetic knowledge Not at all confident A little confident Somewhat confident Very confident … in your knowledge about genetics? … in your ability to explain genetic concepts to patients? 11. 3% 12. 7% 39. 1% 34. 3% 41. 4% 41. 0% 8. 3% 11. 9% … in your ability to respond to patients’ questions about genomic sequencing technologies? 38. 8% 16. 4% 6. 0% … in your ability to explain a result from a genetic test to patients? 18. 1% 39. 9% 33. 1% 9. 0% … that your training has prepared you to explain 34. 1% a genomic result to a patient? 37. 2% 22. 5% 6. 2% “How confident are you…”

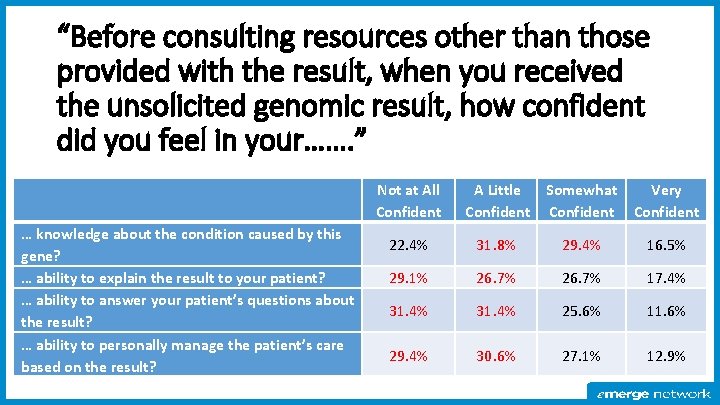
“Before consulting resources other than those provided with the result, when you received the unsolicited genomic result, how confident did you feel in your……. ” Not at All Confident … knowledge about the condition caused by this gene? … ability to explain the result to your patient? … ability to answer your patient’s questions about the result? … ability to personally manage the patient’s care based on the result? A Little Somewhat Confident Very Confident 22. 4% 31. 8% 29. 4% 16. 5% 29. 1% 26. 7% 17. 4% 31. 4% 25. 6% 11. 6% 29. 4% 30. 6% 27. 1% 12. 9%

“Which of the following actions did you perform to gather any additional information after receiving the unsolicited genomic result? ” Yes Learned more information about the condition Learned more information about this specific variant Reviewed the patient's personal medical history for symptoms of the condition Reviewed the patient's family history for this condition No Not sure 55. 9% 40. 5% 3. 6% 45. 2% 50. 0% 4. 8% 75. 0% 23. 8% 1. 2% 70. 2% 26. 2% 3. 6%

“How similar or different was receiving this unsolicited genomic result for this patient compared to receiving other unsolicited results, such as a CBC ordered by another physician? ” Very different Somewhat similar Very similar 40. 7% 42. 0% 9. 9% 7. 4%

Discussions with patient • 72. 9% had discussed the result with their patient • 62. 9% contacted the patient to discuss the result • Of those who did not… • 39. 1% plan to speak to patient • 52. 2% defer speaking to patient to allow another provider whom the patient sees to contact patient

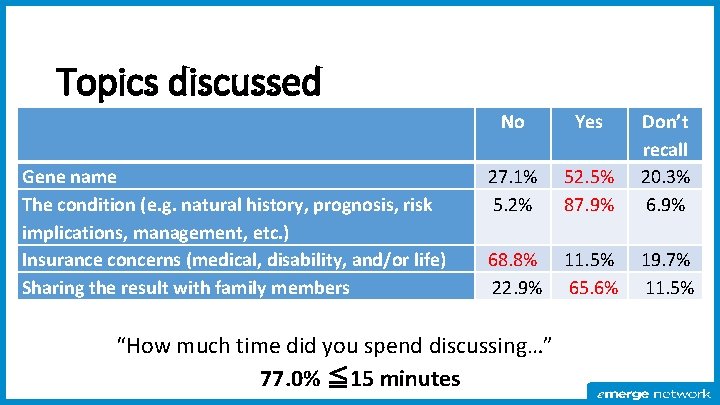
Topics discussed Gene name The condition (e. g. natural history, prognosis, risk implications, management, etc. ) Insurance concerns (medical, disability, and/or life) Sharing the result with family members No Yes 27. 1% 5. 2% 52. 5% 87. 9% Don’t recall 20. 3% 6. 9% 68. 8% 22. 9% 11. 5% 65. 6% 19. 7% 11. 5% “How much time did you spend discussing…” 77. 0% ≦ 15 minutes

• “Did you refer your patient to a subspecialist/s? ” 55. 7% Yes • “Which subspecialists did you refer your/the patient to? ” • 41. 2% Genetics • 14. 7% Cardiology • 11. 8% Oncology • 32. 3% Other Actions taken • “Did you order additional test/s on your/the patient? ” 19. 7% Yes • “Which of the following additional tests did you order on the patient? ” • 75. 0% Blood work or urine test • 25. 0% Colonoscopy • 8. 3% X-rays • 8. 3% ECG/EKG • 8. 3% MRI/CT scan • 8. 3% Mammogram • “Did you recommend family members undergo testing? ” 42. 6% Yes

Implications for patient’s current care Strongly Somewhat Strongly disagree 8. 3% 7. 1% 32. 1% 46. 4% The unsolicited genomic result is important to this patient's healthcare The unsolicited genomic result might lead to 33. 3% 34. 5% patient harm through unnecessary follow-up Responding to the unsolicited genomic result 32. 1% 23. 8% was a burden to me “In what ways did you find the unsolicited genomic result useful? ” 51. 1% Planned future disease surveillance or screening 32. 2% Identified at-risk family members 25. 6% Informed disease prevention 21. 1% Supported the management of patient’s care already underway 16. 7% Changed current management of patient’s care 14. 4% I did not find the unsolicited genomic result useful 21. 4% 3. 6% 33. 3% 7. 1%

”What type of information would you have liked to receive with result? ” • 71. 1% Explanation of the result • 67. 8% Recommendation(s) for patient management Information to receive with result • 61. 1% Information on long-term implications of the result on the patient • 58. 9% Recommendation(s) for patient referral • 56. 7% Contact information for referral to genetic counselors and/or medical geneticist “How would you liked to receive this additional information? ” • 66. 7% Through the EHR • 25. 6% A letter with the result or after the result was received • 12. 2% By email • 2. 2% By phone

Thinking about the future What effect do you believe receiving unsolicited genomic results will have… Increase greatly …on your workload? 19. 5% …on the difficulties getting reimbursed for medical 15. 8% care related to managing the results? Increase somewhat No Decrease effect somewhat Decrease greatly Don’t know 57. 8% 29. 9% 17. 2% 1. 6% 25. 2% 0. 8% 0. 0% 0. 8% 3. 9% 27. 6% I would like to receive unsolicited genomic results…. . . that could affect the patient’s health in the future even if there is no medical intervention. …indicating that a patient is NOT at risk for developing a condition (a. k. a. negative results). …even if there is an unclear association between the genetic finding and disease. Strongly Disagree 8. 6% Somewhat Disagree Agree 10. 9% 48. 4% Strongly Agree 32. 0% 7. 0% 14. 1% 42. 2% 36. 7% 25. 8% 25. 0% 32. 0% 17. 2%

Comments from HCPs

Receiving unsolicited results I want ownership of the result by the investigators who ordered it. There should be autonomic consult already in the computer and placed so that the unknowing physician is not burdened with dealing with something that is out of their knowledge base or expertise. (Patient: male, 67 years old, BRCA 2, hereditary breast ovarian cancer syndrome (HBOC) condition type; Provider: Not main provider)

I am excited about the idea of introducing genetic testing for patients when there is a clear and actionable response to testing. However, I have always been weary about ordering testing for patients ('unsolicited' to use your terminology) when the ordering provider is not responsible for following up the testing themselves. I think the accountability must be there. If testing is performed and a primary is responsible for reviewing with the family who never ordered the test I think that would make many of us uncomfortable. As an example, Genesight testing is not uncommon at our practice. For most patients it is not the clear response families are hoping for, they often pay out of pocket (possibly hundreds of dollars), and it may or may not affect treatment, not to mention the cost overall to the healthcare system. I think testing can be very helpful, but providers should be responsible for explaining to a patient why a test should or should not be performed, the benefits, the potential costs, and what we would do with it. Patients overall love testing as I see it, but when they realize it is costly, often low yield, and may or likely won't change management they tend to realize its not always worth it. Thanks for your time! (Patient: male, 15 years old, LDLR, familial hypercholesterolemia condition type; Provider: PCP)

The genetics staff needs to make more effort to contact patients in a way that is convenient to patients. I had one patient complaint quite a bit about how he was contacted (messages left to call genetics right away and when he did, no one was there). Genetics staff should take the lead in explaining the result and refer back to the PCP once this conversation has occurred with recommendations for the PCP about next steps, just like any other consultant would do. Genetics is a broad field. a PCP might know a lot about one disorder but not much about another, depending on how rare one might be. It would be best if the genetics team where more clinically oriented and act as clinical consultants like any other specialty. (Patient: male, 68 years old, HFE, hemochromatosis condition type; Provider: PCP)

Relevancy of unsolicited results I received a genetic result on a 76 yo patient. The likelihood that he would develop an inherited disease at the age of 76 is vanishingly small. Nonetheless, after discussion, we pursued further work up. An incidental finding will require further follow up. I find this aggravating in that the result is of no practical use and yet creates more work for me and more interventions for the patient. (Patient: male, 76 years old, SDHC, hereditary paraganglioma/pheochromocytoma syndrome condition type; Provider: Not main provider) information on how their mental health was considered prior to enrollment in study. Was this really the best time in her life to get this information (Patient: female, 14 years old, BRCA 1, hereditary breast and ovarian cancer syndrome condition type; Provider: Not main provider)

The result was absolutely useless for this patient. She is an 85 year old frail individual with dementia and multiple medical problems, She would have no understanding of this condition and did not benefit at all from finding this out. She has lived 85 years without any evidence of any problems related to having this genetic variant. Finding it out now was beyond ridiculous. I did call her daughter took it well and she ahs a medical background so the discussion was very easy, fortunately. I discussed that she and her sister may want to discuss this further. the patient has at least two grandchildren that I am aware of that are young. I discussed with her daughter about perhaps discussing further with their pediatricians. The daughter does think that she and her two children have been enrolled in mycode. I am actually not sure how this patient got enrolled. I do not think she is capable of giving informed consent herself. Daughter may have agreed to it but in our conversation she does not recall. (Patient: female, 85 years old, TP 53, Li-Fraumeni syndrome condition type; Provider: PCP)

Benefits I can see that there may be long term benefits to genetic testing but we are not there yet. Right now the work is greater than the benefit to the patient (Patient: female, 20 years old, HFE, hemochromatosis condition type; Provider: Not main provider)

Summary HCPs are not particularly confident in their genetics knowledge and ability to communicate genetics results to their patients Initial reactions to receiving results were generally positive, HCPs generally found the results useful HCP perceive unsolicited genomic results as different than other unsolicited results Familial implications – about 65% discussed familial implications and about ½ recommended family testing Despite concerns about increased burden on their practice, most HCPs would like to receive results that could impact their patients care, as well as negative results.

Thank you!