The hierarchy of research methods Eileen K Hutton




































- Slides: 53

The hierarchy of research methods Eileen K. Hutton RM Ph. D Mc. Master University Hamilton, Canada

Systematic reviews and meta-analysis

Evidence based practice “Integration of research evidence with clinical expertise and patient values” * * From Sackett et al. Evidenced Based Medicine, 2000

Evidence based practice “Integration of research evidence with clinical expertise and patient values” * * From Sackett et al. Evidenced Based Medicine, 2000

Research • Single original research studies are the building blocks of clinical knowledge • Systematic reviews bring together and assess all relevant studies • Meta-analyses give single estimate of efficacy and effectiveness

Research • Single original research studies are the building blocks of clinical knowledge • Systematic reviews bring together and assess all relevant studies • Meta-analyses give single estimate of efficacy and effectiveness

Research • Single original research studies are the building blocks of clinical knowledge • Systematic reviews bring together and assess all relevant studies • Meta-analyses give single estimate of efficacy and effectiveness

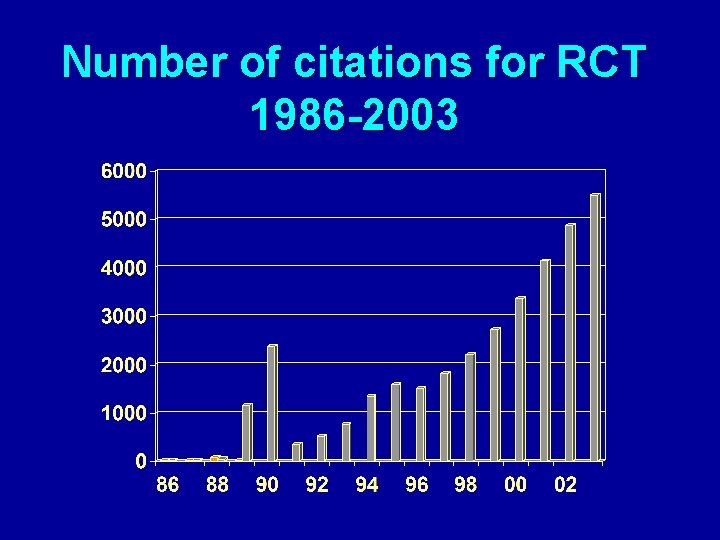
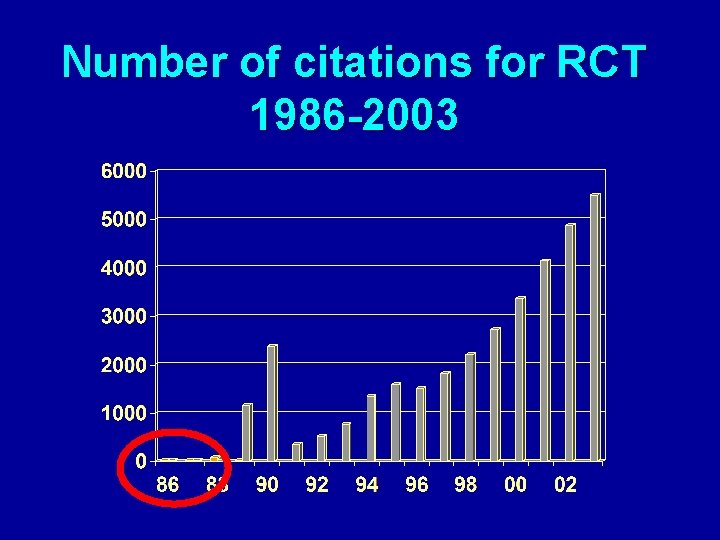
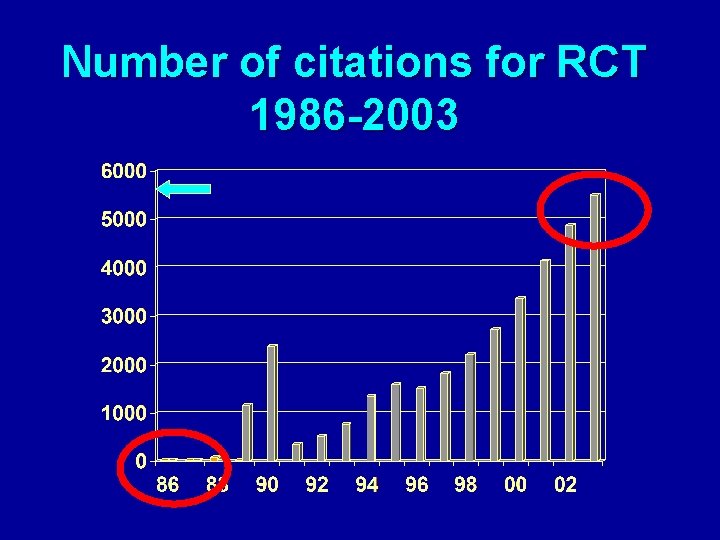
Number of citations for RCT 1986 -2003

Number of citations for RCT 1986 -2003

Number of citations for RCT 1986 -2003

“Systematic reviews - the critical links in the great chain of evidence” - 1998, Mulrow C. Cook D. Davidoff F.

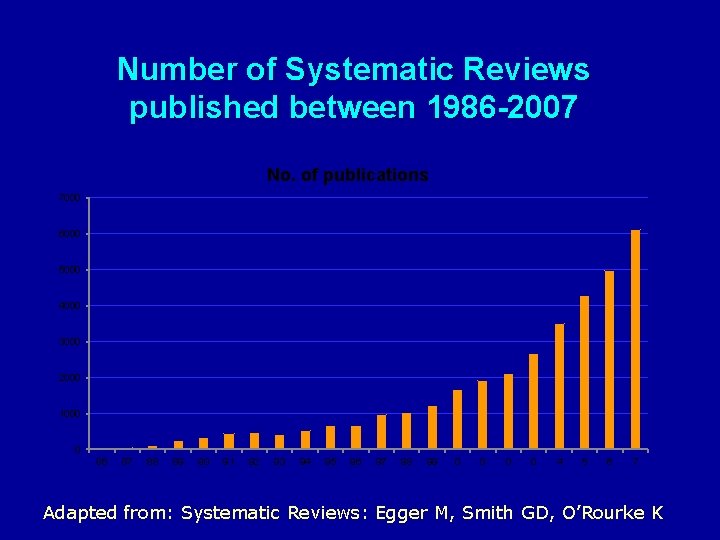
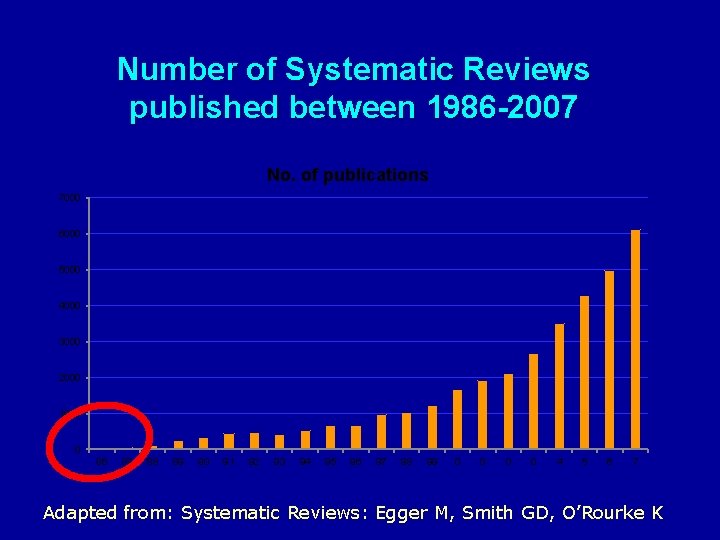
Number of Systematic Reviews published between 1986 -2007 No. of publications 7000 6000 5000 4000 3000 2000 1000 0 86 87 88 89 90 91 92 93 94 95 96 97 98 99 0 0 4 5 6 7 Adapted from: Systematic Reviews: Egger M, Smith GD, O’Rourke K

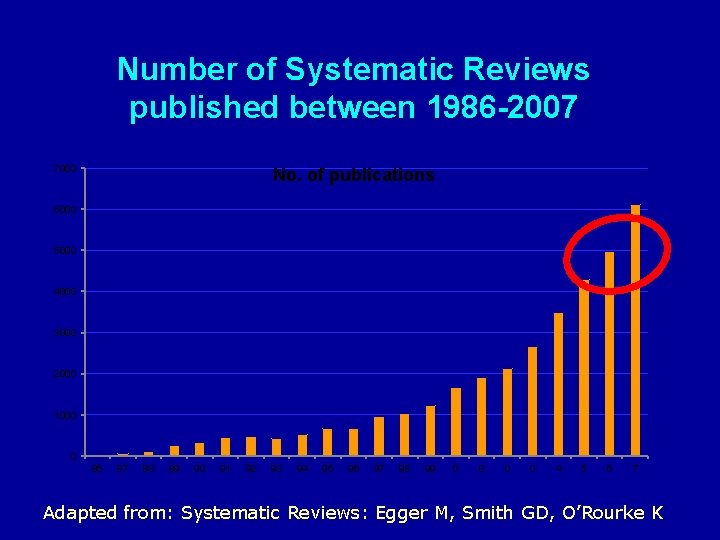
Number of Systematic Reviews published between 1986 -2007 No. of publications 7000 6000 5000 4000 3000 2000 1000 0 86 87 88 89 90 91 92 93 94 95 96 97 98 99 0 0 4 5 6 7 Adapted from: Systematic Reviews: Egger M, Smith GD, O’Rourke K

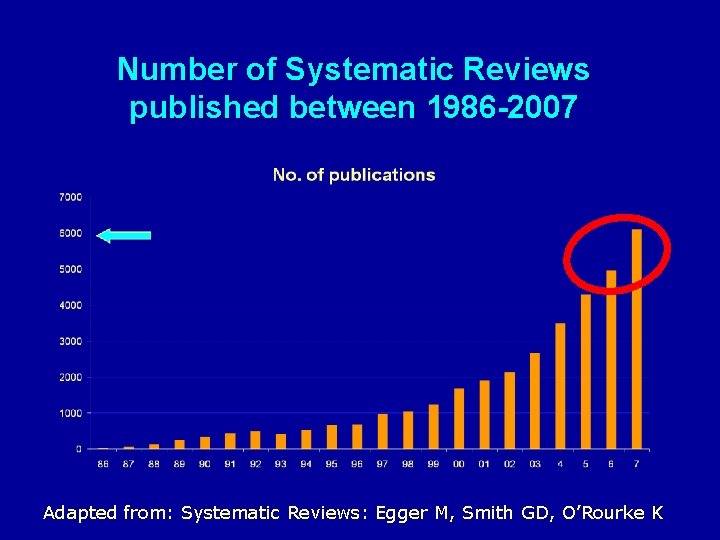
Number of Systematic Reviews published between 1986 -2007 7000 No. of publications 6000 5000 4000 3000 2000 1000 0 86 87 88 89 90 91 92 93 94 95 96 97 98 99 0 0 4 5 6 7 Adapted from: Systematic Reviews: Egger M, Smith GD, O’Rourke K

Number of Systematic Reviews published between 1986 -2007 Adapted from: Systematic Reviews: Egger M, Smith GD, O’Rourke K

Timing of umbilical cord clamping in term infants

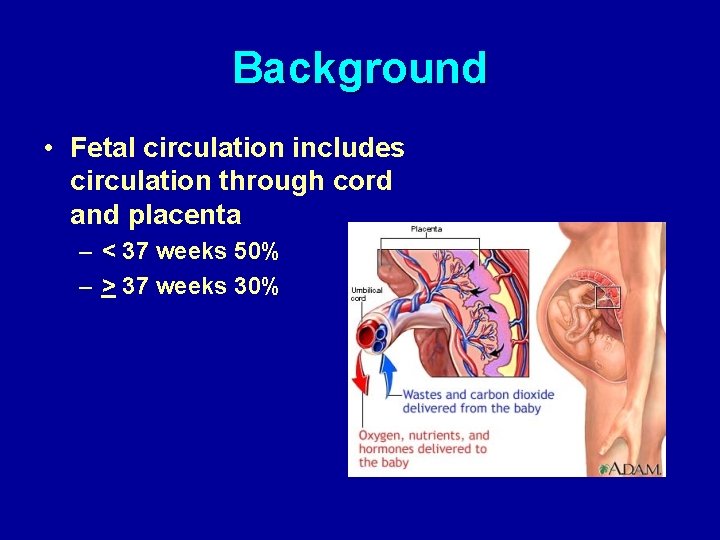
Background • Fetal circulation includes circulation through cord and placenta – < 37 weeks 50% – > 37 weeks 30%

Background • What happens at birth? – Without intervention, a significant amount placental circulation infant – Clamping of cord interrupts this “placental transfusion”

Question • Is this important to neonatal wellbeing?

“Another thing very injurious to the child is the tying and cutting of the navel string too soon, which should always be left till the child has not only repeatedly breathed, but till all pulsation in the cord ceases. ”

“Another thing very injurious to the child is the tying and cutting of the navel string too soon, which should always be left till the child has not only repeatedly breathed, but till all pulsation in the cord ceases. ” Erasmus Darwin 1801

Delayed cord clamping • Increased: – Oxygen perfusion – Hbg; hct; iron stores • Less anaemia fewer transfusions • Better cardiopulmonary adaptation – Higher blood pressure – Decreased RDS • Improved breast feeding success • Decreased risk of maternal-fetal transfusion

Early cord clamping • Allows for : – active management of 3 rd stage decreasing maternal blood loss – immediate resuscitation • Avoids: – – – Hypothermia Polycythemia Hyperviscosity Hypervolemia Hyperbilirubinemia • Increases cord blood collection

Delayed Cord Clamping - Term • Systematic Review and Metaanalysis • March 2007 Hutton EK. Hassan E. JAMA 2007; 297: 1241 -1252

Objective • To compare potential benefits and harms of late vs early cord clamping in term infants

Data sources • Electronic search of 6 databases: ØCochrane trials registers (2) ØCochrane library, ØMEDLINE ØEMBASE ØCINHAL • Hand search of references

Inclusion • Controlled trials • Term pregnancy (≥ 37 weeks) • Reported original data ØAt least one outcome of interest

Exclusion • Studies involving only preterm or low birth weight infants

Data extraction • Standardised extraction forms developed • Authors independently Øassessed eligibility of identified studies ØExtracted data

Analysis • Revman version 4. 2 used • Double data entry • Mean and SD for continuous variables converted to WMD • Harmful effects reported as RR of adverse event

Search Results 37 studies found 15 included 22 excluded 8 RCT 7 nonrandomised

Systematic Review and Metaanalysis • 15 Controlled trials • 1912 infants ØLate n = 1001 ØEarly n = 911

Definitions • Majority defined “early” : Ø“immediate” or within 10 seconds ØOne study within 60 seconds

Definitions • Shortest time in “late” group: Ø 2 minutes ØMost trials 3 minutes or after cord pulsation cessation

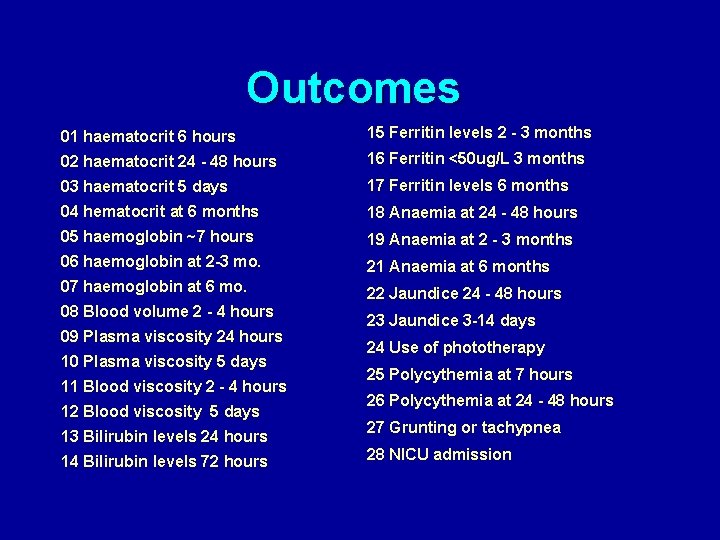
Outcomes 01 haematocrit 6 hours 15 Ferritin levels 2 - 3 months 02 haematocrit 24 - 48 hours 16 Ferritin <50 ug/L 3 months 03 haematocrit 5 days 17 Ferritin levels 6 months 04 hematocrit at 6 months 18 Anaemia at 24 - 48 hours 05 haemoglobin ~7 hours 19 Anaemia at 2 - 3 months 06 haemoglobin at 2 -3 mo. 21 Anaemia at 6 months 07 haemoglobin at 6 mo. 22 Jaundice 24 - 48 hours 08 Blood volume 2 - 4 hours 09 Plasma viscosity 24 hours 10 Plasma viscosity 5 days 11 Blood viscosity 2 - 4 hours 12 Blood viscosity 5 days 13 Bilirubin levels 24 hours 14 Bilirubin levels 72 hours 23 Jaundice 3 -14 days 24 Use of phototherapy 25 Polycythemia at 7 hours 26 Polycythemia at 24 - 48 hours 27 Grunting or tachypnea 28 NICU admission

Findings 01 haematocrit 6 hours 15 Ferritin levels 2 - 3 months 02 haematocrit 24 - 48 hours 16 Ferritin <50 ug/L 3 months 03 haematocrit 5 days 17 Ferritin levels 6 months 04 hematocrit at 6 months 18 Anaemia at 24 - 48 hours 05 haemoglobin ~7 hours 19 Anaemia at 2 - 3 months 06 haemoglobin at 2 -3 mo. 21 Anaemia at 6 months 07 haemoglobin at 6 mo. 22 Jaundice 24 - 48 hours 08 Blood volume 2 - 4 hours 09 Plasma viscosity 24 hours 10 Plasma viscosity 5 days 11 Blood viscosity 2 - 4 hours 12 Blood viscosity 5 days 13 Bilirubin levels 24 hours 14 Bilirubin levels 72 hours 23 Jaundice 3 -14 days 24 Use of phototherapy 25 Polycythemia at 7 hours 26 Polycythemia at 24 - 48 hours 27 Grunting or tachypnea 28 NICU admission

Findings • Delaying clamping at least 2 minutes: ØImproved short & long term hematological and iron status ØNo significant impact on bilirubin, plasma viscosity in first week ØIncreases in polycythemia ØNo increase in rates of NICU or phototherapy

Results - Physiological parameters Blood volume at 2 - 4 hours – (n = 60) – WMD 9. 07 m. L/kg – 95% CI (5. 81, 12. 32)

Results - Physiological parameters Blood viscosity at 2 - 4 hours (n=90): WMD 1. 39; 95% CI (1. 19, 1. 59) Blood viscosity at 5 days (n=90): WMD 0. 94; 95% CI (0. 72, 1. 16)

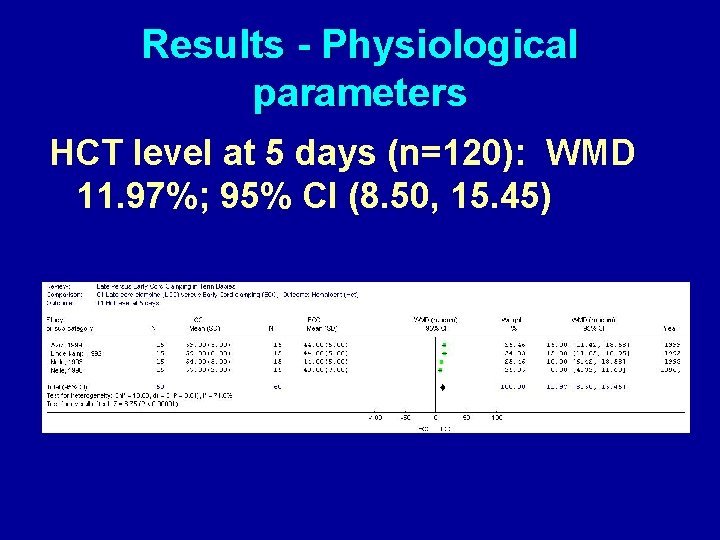
Results - Physiological parameters HCT level at 5 days (n=120): WMD 11. 97%; 95% CI (8. 50, 15. 45)

Results - Physiological parameters Hbg at 7 hours (n=354): WMD 0. 60 g/d. L; 95% CI (0. 11, 1. 09) • No difference at 2 - 3 or at 6 months

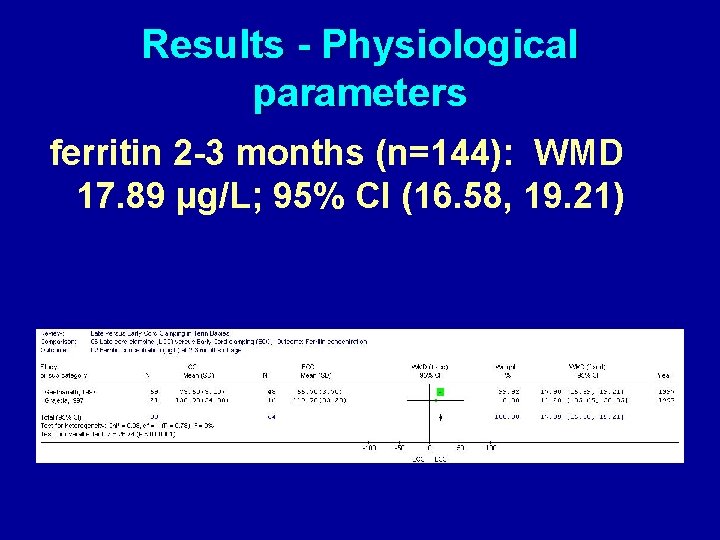
Results - Physiological parameters ferritin 2 -3 months (n=144): WMD 17. 89 µg/L; 95% CI (16. 58, 19. 21)

Results - Physiological parameters Ferritin <50 µg/L at 3 months: RR, 0. 67; 95%CI, (0. 47 to 0. 96) Ferritin 6 months (n=315): WMD 11. 80 µg/L; 95% CI (4. 07, 19. 53) Stored iron at 6 months (n=315): WMD, 19. 90 mg; 95% CI (7. 67, 32. 13)

Results – clinical outcomes Risk of anaemia 2 -3 months (n=119): RR 0. 53; 95% CI (0. 40, 0. 70)

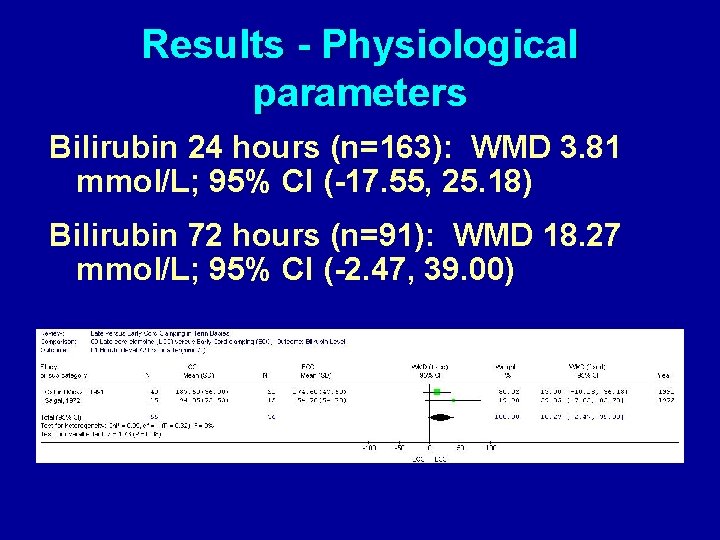
Results - Physiological parameters Bilirubin 24 hours (n=163): WMD 3. 81 mmol/L; 95% CI (-17. 55, 25. 18) Bilirubin 72 hours (n=91): WMD 18. 27 mmol/L; 95% CI (-2. 47, 39. 00)

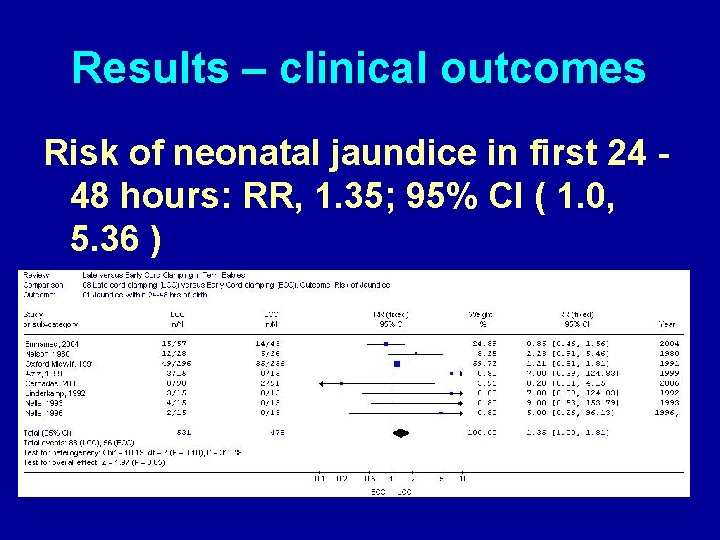
Results – clinical outcomes Risk of neonatal jaundice in first 24 48 hours: RR, 1. 35; 95% CI ( 1. 0, 5. 36 )

Results – clinical outcomes Jaundice at 3 – 14 days (n=332): RR, 1. 27; 95%CI (0. 76 – 2. 10)

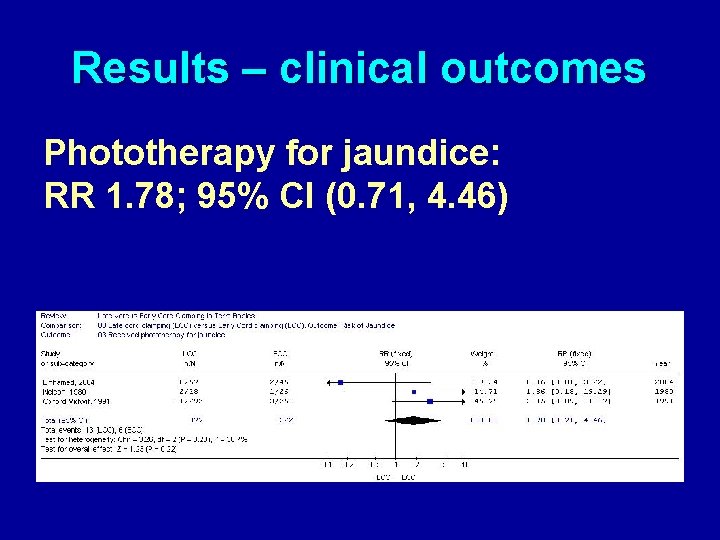
Results – clinical outcomes Phototherapy for jaundice: RR 1. 78; 95% CI (0. 71, 4. 46)

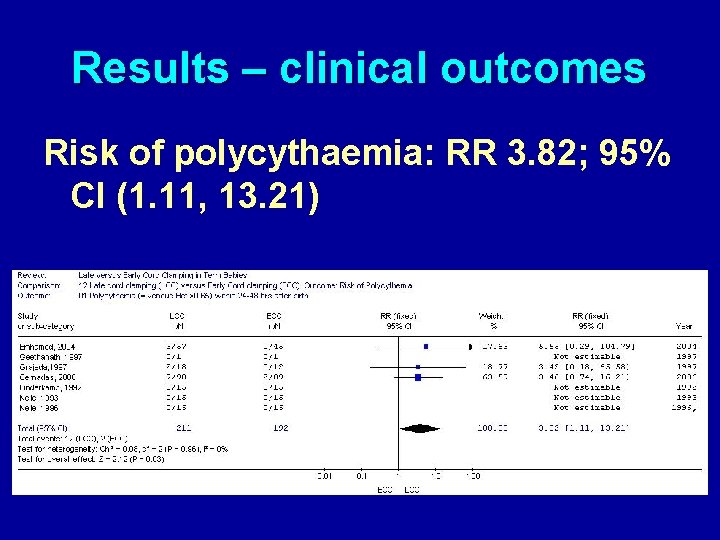
Results – clinical outcomes Risk of polycythaemia: RR 3. 82; 95% CI (1. 11, 13. 21)

Authors’ conclusions “We believe that this meta-analysis supports incorporating into clinical practice a minimum delay of 2 minutes before clamping the umbilical cord in all full-term newborns. ” Hutton EK, Hassan ES. JAMA 2007; 297: 1241 -52

Delayed cord clamping – Term Authors conclusions: • A minimum of 2 minutes in cord clamping is beneficial to the term newborn • Benefit extends into infancy as far as 6 months • Increase in polycythemia appears to be benign

Clamp early or clamp late? • For term infants, improved outcomes with delay of at least 2 minutes
