The Hepatobiliary Cystoadenoma and Cystadenocarcinoma Study for Kras
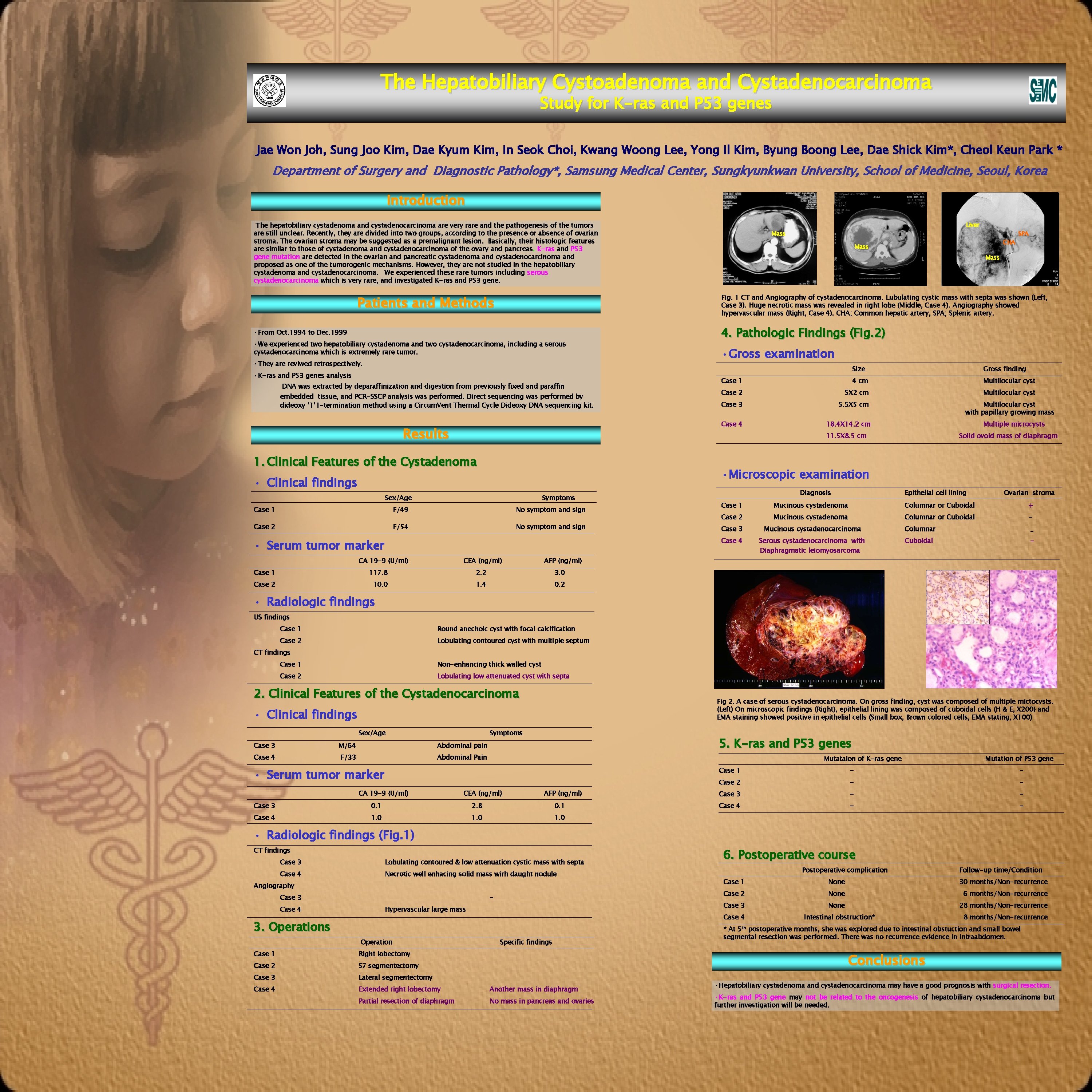
The Hepatobiliary Cystoadenoma and Cystadenocarcinoma Study for K-ras and P 53 genes Jae Won Joh, Sung Joo Kim, Dae Kyum Kim, In Seok Choi, Kwang Woong Lee, Yong Il Kim, Byung Boong Lee, Dae Shick Kim*, Cheol Keun Park * Department of Surgery and Diagnostic Pathology*, Samsung Medical Center, Sungkyunkwan University, School of Medicine, Seoul, Korea Introduction The hepatobiliary cystadenoma and cystadenocarcinoma are very rare and the pathogenesis of the tumors are still unclear. Recently, they are divided into two groups, according to the presence or absence of ovarian stroma. The ovarian stroma may be suggested as a premalignant lesion. Basically, their histologic features are similar to those of cystadenoma and cystadenocarcinoma of the ovary and pancreas. K-ras and P 53 gene mutation are detected in the ovarian and pancreatic cystadenoma and cystadenocarcinoma and proposed as one of the tumorogenic mechanisms. However, they are not studied in the hepatobiliary cystadenoma and cystadenocarcinoma. We experienced these rare tumors including serous cystadenocarcinoma which is very rare, and investigated K-ras and P 53 gene. Mass CHA Mass SPA Mass Fig. 1 CT and Angiography of cystadenocarcinoma. Lubulating cystic mass with septa was shown (Left, Case 3). Huge necrotic mass was revealed in right lobe (Middle, Case 4). Angiography showed hypervascular mass (Right, Case 4). CHA; Common hepatic artery, SPA; Splenic artery. Patients and Methods • From Oct. 1994 to Dec. 1999 • We experienced two hepatobiliary cystadenoma and two cystadenocarcinoma, including a serous cystadenocarcinoma which is extremely rare tumor. • They are reviwed retrospectively. • K-ras and P 53 genes analysis DNA was extracted by deparaffinization and digestion from previously fixed and paraffin embedded tissue, and PCR-SSCP analysis was performed. Direct sequencing was performed by dideoxy ‘ 1’ 1 -termination method using a Circum. Vent Thermal Cycle Dideoxy DNA sequencing kit. 4. Pathologic Findings (Fig. 2) • Gross examination Size Gross finding Case 1 4 cm Multilocular cyst Case 2 5 X 2 cm Multilocular cyst Case 3 5. 5 X 5 cm Case 4 Results Multilocular cyst with papillary growing mass 18. 4 X 14. 2 cm Multiple microcysts 11. 5 X 8. 5 cm 1. Clinical Features of the Cystadenoma Solid ovoid mass of diaphragm • Microscopic examination • Clinical findings Sex/Age Symptoms Case 1 F/49 No symptom and sign Case 2 F/54 No symptom and sign • Serum tumor marker CA 19 -9 (U/ml) Liver CEA (ng/ml) Diagnosis Epithelial cell lining Ovarian stroma Case 1 Mucinous cystadenoma Columnar or Cuboidal + Case 2 Mucinous cystadenoma Columnar or Cuboidal - Case 3 Mucinous cystadenocarcinoma Columnar _ Case 4 Serous cystadenocarcinoma with Diaphragmatic leiomyosarcoma Cuboidal - AFP (ng/ml) Case 1 117. 8 2. 2 3. 0 Case 2 10. 0 1. 4 0. 2 • Radiologic findings US findings Case 1 Round anechoic cyst with focal calcification Case 2 Lobulating contoured cyst with multiple septum CT findings Case 1 Non-enhancing thick walled cyst Case 2 Lobulating low attenuated cyst with septa 2. Clinical Features of the Cystadenocarcinoma Fig 2. A case of serous cystadenocarcinoma. On gross finding, cyst was composed of multiple mictocysts. (Left) On microscopic findings (Right), epithelial lining was composed of cuboidal cells (H & E, X 200) and EMA staining showed positive in epithelial cells (Small box, Brown colored cells, EMA stating, X 100) • Clinical findings Sex/Age Symptoms Case 3 M/64 Abdominal pain Case 4 F/33 Abdominal Pain 5. K-ras and P 53 genes Mutataion of K-ras gene • Serum tumor marker CA 19 -9 (U/ml) CEA (ng/ml) AFP (ng/ml) Case 3 0. 1 2. 8 0. 1 Case 4 1. 0 Mutation of P 53 gene Case 1 - - Case 2 - - Case 3 - - Case 4 - - • Radiologic findings (Fig. 1) CT findings Case 3 Lobulating contoured & low attenuation cystic mass with septa Case 4 Necrotic well enhacing solid mass wirh daught nodule Angiography Case 3 Case 4 Hypervascular large mass Postoperative complication Specific findings Case 1 Right lobectomy Case 2 S 7 segmentectomy Case 3 Lateral segmentectomy Case 4 Extended right lobectomy Another mass in diaphragm Partial resection of diaphragm No mass in pancreas and ovaries Follow-up time/Condition Case 1 None 30 months/Non-recurrence Case 2 None 6 months/Non-recurrence Case 3 None 28 months/Non-recurrence Case 4 3. Operations Operation 6. Postoperative course Intestinal obstruction* 8 months/Non-recurrence * At 5 th postoperative months, she was explored due to intestinal obstuction and small bowel segmental resection was performed. There was no recurrence evidence in intraabdomen. Conclusions • Hepatobiliary cystadenoma and cystadenocarcinoma may have a good prognosis with surgical resection. • K-ras and P 53 gene may not be related to the oncogenesis of hepatobiliary cystadenocarcinoma but further investigation will be needed.
- Slides: 1