The Gut Microbiome and Treatment Response in Schizophrenia
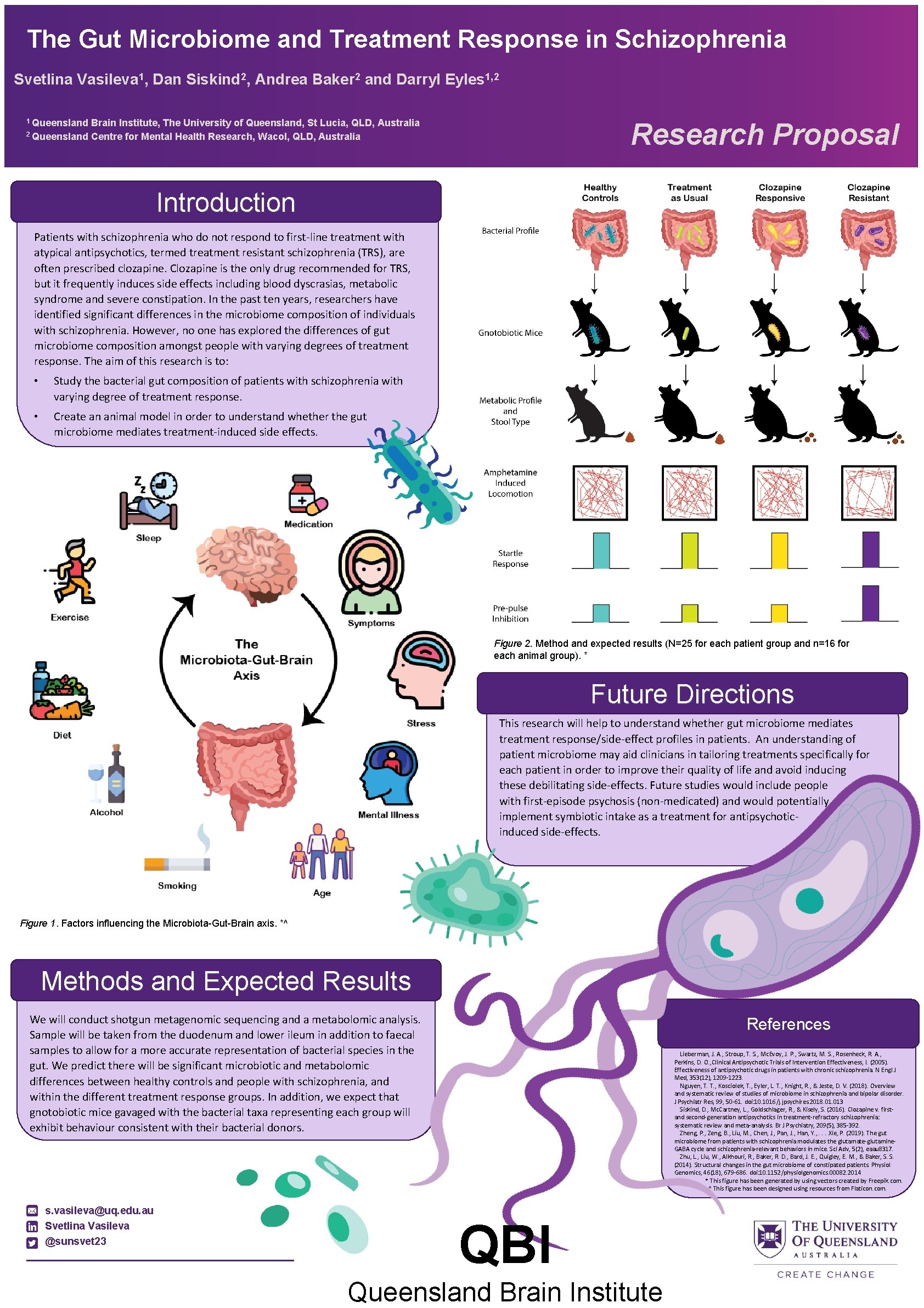
The Gut Microbiome and Treatment Response in Schizophrenia Svetlina Vasileva 1, Dan Siskind 2, Andrea Baker 2 and Darryl Eyles 1, 2 1 Queensland Brain Institute, The University of Queensland, St Lucia, QLD, Australia 2 Queensland Centre for Mental Health Research, Wacol, QLD, Australia Research Proposal Introduction Patients with schizophrenia who do not respond to first-line treatment with atypical antipsychotics, termed treatment resistant schizophrenia (TRS), are often prescribed clozapine. Clozapine is the only drug recommended for TRS, but it frequently induces side effects including blood dyscrasias, metabolic syndrome and severe constipation. In the past ten years, researchers have identified significant differences in the microbiome composition of individuals with schizophrenia. However, no one has explored the differences of gut microbiome composition amongst people with varying degrees of treatment response. The aim of this research is to: • Study the bacterial gut composition of patients with schizophrenia with varying degree of treatment response. • Create an animal model in order to understand whether the gut microbiome mediates treatment-induced side effects. Figure 2. Method and expected results (N=25 for each patient group and n=16 for each animal group). * Future Directions This research will help to understand whether gut microbiome mediates treatment response/side-effect profiles in patients. An understanding of patient microbiome may aid clinicians in tailoring treatments specifically for each patient in order to improve their quality of life and avoid inducing these debilitating side-effects. Future studies would include people with first-episode psychosis (non-medicated) and would potentially implement symbiotic intake as a treatment for antipsychoticinduced side-effects. Figure 1. Factors influencing the Microbiota-Gut-Brain axis. *^ Methods and Expected Results We will conduct shotgun metagenomic sequencing and a metabolomic analysis. Sample will be taken from the duodenum and lower ileum in addition to faecal samples to allow for a more accurate representation of bacterial species in the gut. We predict there will be significant microbiotic and metabolomic differences between healthy controls and people with schizophrenia, and within the different treatment response groups. In addition, we expect that gnotobiotic mice gavaged with the bacterial taxa representing each group will exhibit behaviour consistent with their bacterial donors. s. vasileva@uq. edu. au Svetlina Vasileva @sunsvet 23 References Lieberman, J. A. , Stroup, T. S. , Mc. Evoy, J. P. , Swartz, M. S. , Rosenheck, R. A. , Perkins, D. O. , Clinical Antipsychotic Trials of Intervention Effectiveness, I. (2005). Effectiveness of antipsychotic drugs in patients with chronic schizophrenia. N Engl J Med, 353(12), 1209 -1223. Nguyen, T. T. , Kosciolek, T. , Eyler, L. T. , Knight, R. , & Jeste, D. V. (2018). Overview and systematic review of studies of microbiome in schizophrenia and bipolar disorder. J Psychiatr Res, 99, 50 -61. doi: 10. 1016/j. jpsychires. 2018. 013 Siskind, D. , Mc. Cartney, L. , Goldschlager, R. , & Kisely, S. (2016). Clozapine v. firstand second-generation antipsychotics in treatment-refractory schizophrenia: systematic review and meta-analysis. Br J Psychiatry, 209(5), 385 -392. Zheng, P. , Zeng, B. , Liu, M. , Chen, J. , Pan, J. , Han, Y. , . . . Xie, P. (2019). The gut microbiome from patients with schizophrenia modulates the glutamate-glutamine. GABA cycle and schizophrenia-relevant behaviors in mice. Sci Adv, 5(2), eaau 8317. Zhu, L. , Liu, W. , Alkhouri, R. , Baker, R. D. , Bard, J. E. , Quigley, E. M. , & Baker, S. S. (2014). Structural changes in the gut microbiome of constipated patients. Physiol Genomics, 46(18), 679 -686. doi: 10. 1152/physiolgenomics. 00082. 2014 * This figure has been generated by using vectors created by Freepik. com. ^ This figure has been designed using resources from Flaticon. com. QBI Queensland Brain Institute
- Slides: 1