The endocrine system Pituitary gland Anterior lobe Posterior

The endocrine system

Pituitary gland ü ü Anterior lobe Posterior lobe Endocrine abnormalities Local mass effect

Hyperpituarism Caused by adenomas: ü Growth hormone ü Adrenocorticotropic hormone ü Prolactin ü Rare – thyroid stimulating hormone, gonadortropin ü 25% adenomas – non-functional (causes HYPOpituarism by compression) ü Microadenomas, macroadenomas (10 mm) ü Nuclear atypia is NOT sign of malignancy ü Ultrastructurally – secretory granules

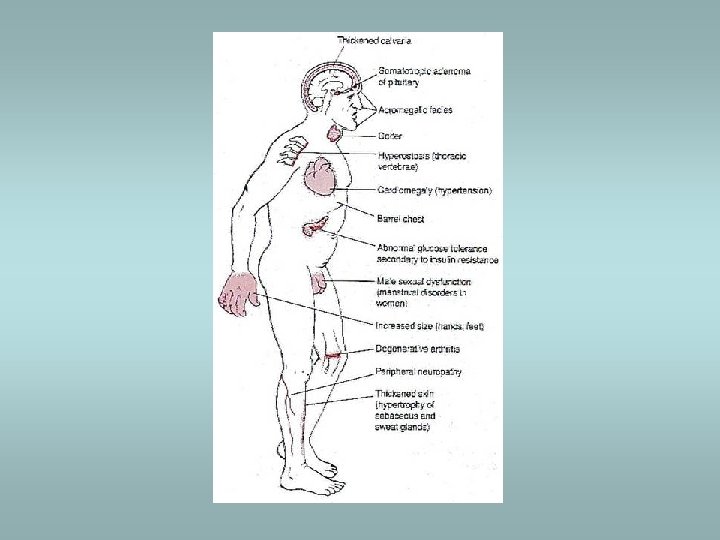
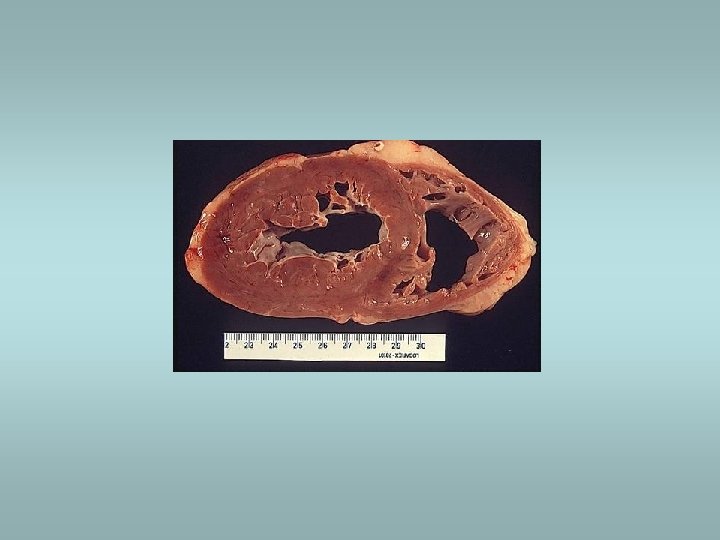
Somatotropic adenomas ü Acromegaly – in adults ü Gigantism – prior to closure of epiphyses ü Granulated, eosinophilic cells – eosinophilic adenoma

Prolactinomas ü Hypogonadism ü Galactorrhea ü Granulated acidophilic or chromophobic cells – chromophobic adenoma

Corticotroph tumors ü Cushing’s syndrome ü Basophilic cells – basophilic adenoma

Hypopituarism Caused by 1) hypothalamic lesions: ü Craniopharyngioma ü Glioma ü Germinoma 2) pituitary lesions: ü Nonsecretory adenomas ü Sheehan’s syndrome ü Empty sella syndrome Clinically – variable ü Hypogonadotropism ü Hypothyroidism, etc.

Hypothalamic lesions – craniopharyngioma ü Benign cystic tumor ü Calcifications ü Squamous epithelial cells and reticular stroma

Nonsecretory chromophobe pituitary adenoma ü Mass effect (visual problems, headache) ü Chromophobic or oncocytic forms exists

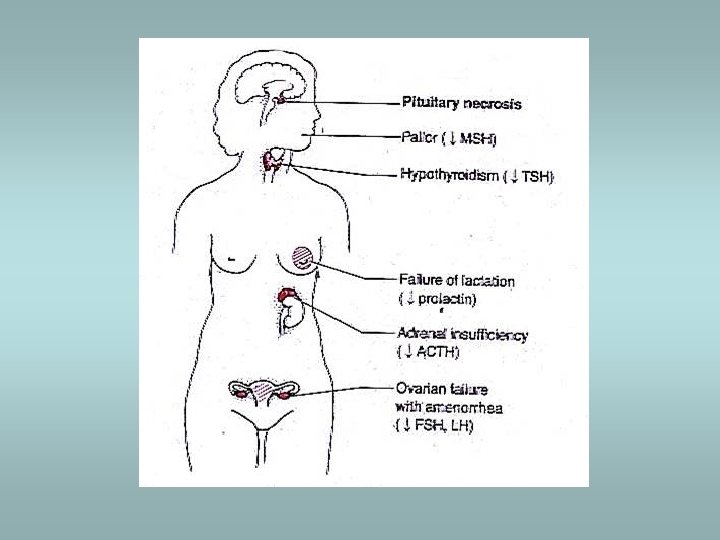
Sheehan’s syndrome ü ü ü Associated with obstetric haemorrhage or shock Caused by infarction of anterior pituitary Gonadal failure – inability to lactate ACTH, TSH deficiency Healing of necrosis – fibrous tissue

Posterior pituitary syndrome ü Excess or deficiency of antidiuretic hormone – ADH ü Caused by suprasellar/hypothalamic lesions

Posterior pituitary syndrome Excess of ADH ü Abnormal resorption of water, hyponatremia and inability to excrete diluted urine Caused by ectopic ADH secretion: ü Non-endocrine neoplasms (small cell carcinoma of the lung) ü Non-neoplastic pulmonary diseases (TBC, pneumonia) ü Primary CNS lesions (infarcts, meningitis, haemorrhage)

Posterior pituitary syndrome ADH deficiency (Diabetes insipidus) Inability to concentrate urine: ü Polyuria ü Polydipsia ü Hypernatremia

Thyroid gland ü Hyperthyroidism ü Hypothyroidism ü Goitre – focal, diffuse

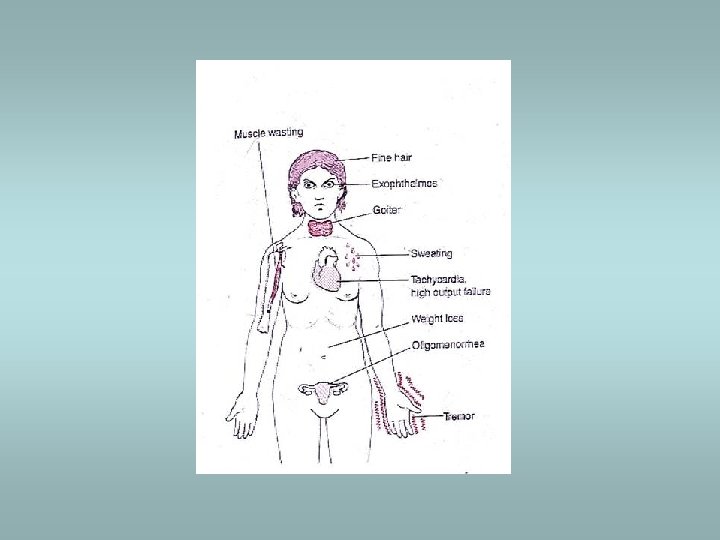
Hyperthyroidism (thyrotoxicosis) ü Increased levels of triodothyronine (T 3), thyroxine (T 4) ü Clinically: wide-eyed gaze, tachycardia, palpitations, nervouseness, weight loss (increased appetite), moist hand, tremor, peripheral vasodilatation ü Associated with diffuse hyperplasia (Graves’ disease) or with toxic multinodular goitre or toxic adenoma ü May be associated with struma ovarii (teratoma)!!

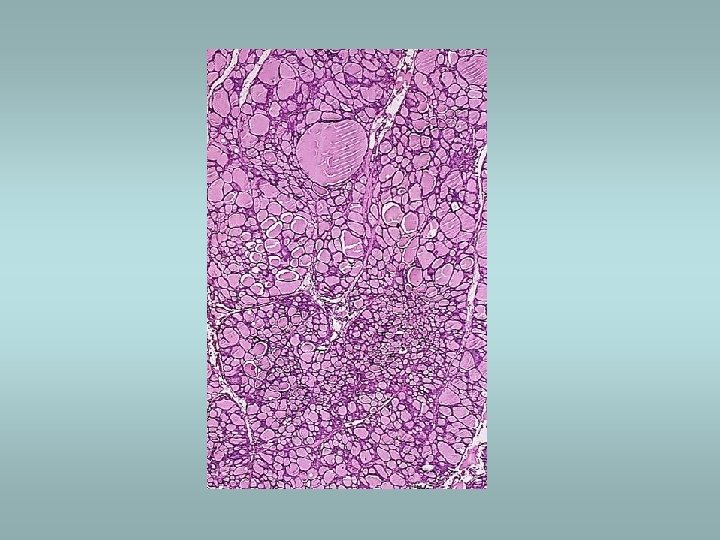
Graves’ disease ü Autoimmune process ü Presence of thyroid stimulating antibody (TSAb) and thyrotropin binding inhibitor immunoglobulin (TBII) ü Associated with other autoimmune diseases ü Presence of hyperplasia of fo. Ilicular epithelium , depletion of colloid and lymphoid aggregates

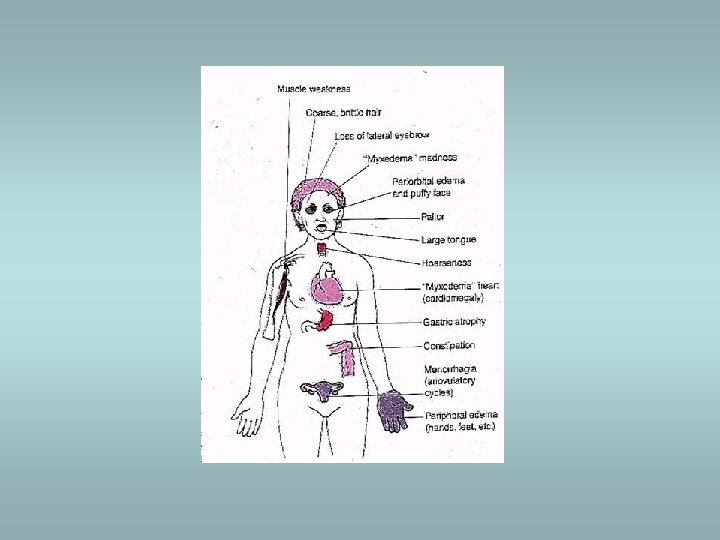
Hypothyroidism Cretinism (during infancy) ü Endemic form ü Sporadic form ü Physical an mental retardation Myxoedema (in adults) Slowing of physical and mental activity, fatigue and apathy Signs - periorbital oedema, coarsening of skin, cardiomegaly, accumulation of mucopolysaccharides in dermis Various causes - idiopathic primary, inflammation – Hashimoto thyroiditis, etc.

Thyroiditis ü ü ü Hashimoto’s thyroiditis De Quervain’s thyroiditis Riedel’s fibrosing thyroiditis Lymphocytic thyroiditis Infectious thyroiditis

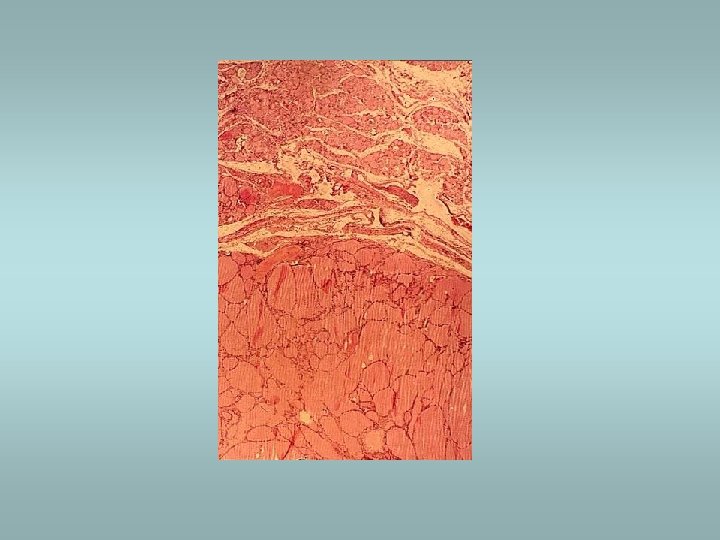
Hashimoto’s thyroiditis ü Autoimmune disorder ü Female predominance ü Defect in suppressor T cells, production of autoantibodies ü Associated with other autoimmune disease (SLE, Sjögren sy, rheumatoid arthritis…) ü Microscopically – dense lymphocytic infiltrate, germinal centers, abundant eosinophilic oncocytes (Hürtle cells)

De Quervain’s subacute granulomatous thyroiditis ü Also known as giant cell thyroiditis ü Probably viral etiology ü Destruction of follicles, neutrophil infiltrate, multinucleate giant cells ü Recovery in 6 -8 weeks

Subacute lymphocytic thyroiditis ü Nonspecific lymphoid infiltration ü Without germinal centre ü In women in postpartum period

Riedel’s fibrosing thyroiditis ü Thyroid replaced by fibrous tissue ü Fibrous tissue extends and penetrate into the surrounding neck structures ü May be mistaken for infiltrating neoplasm

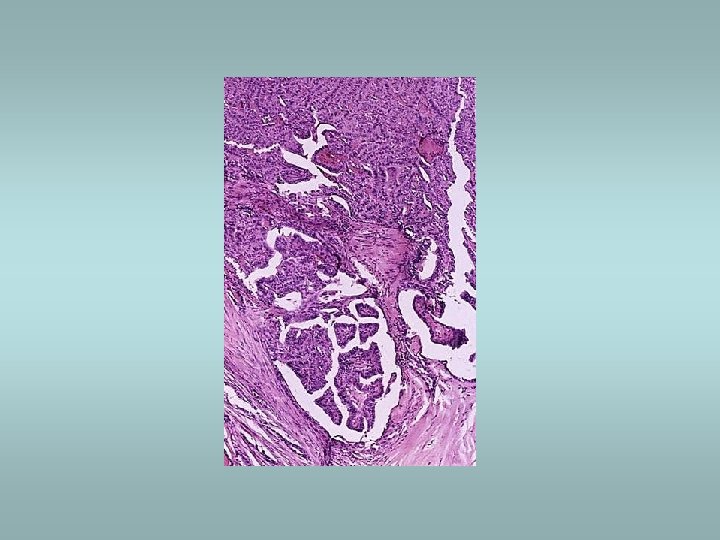
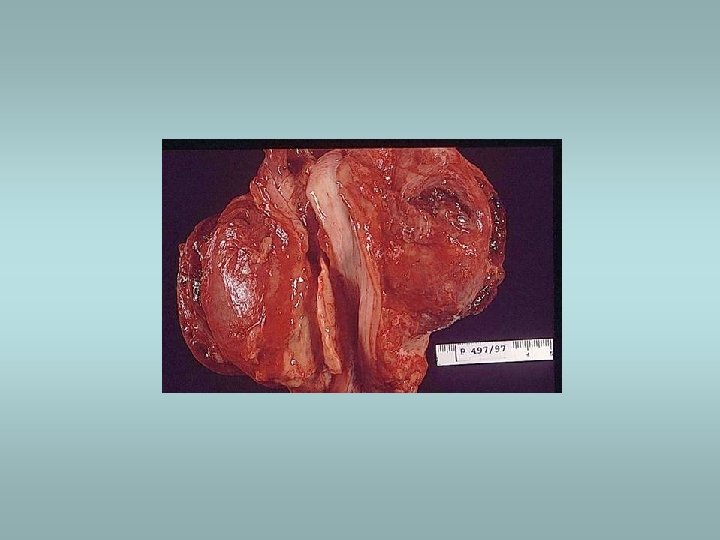
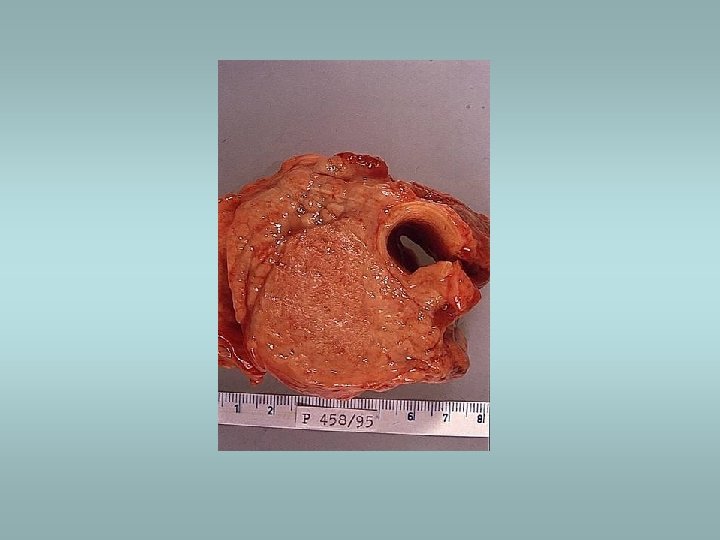
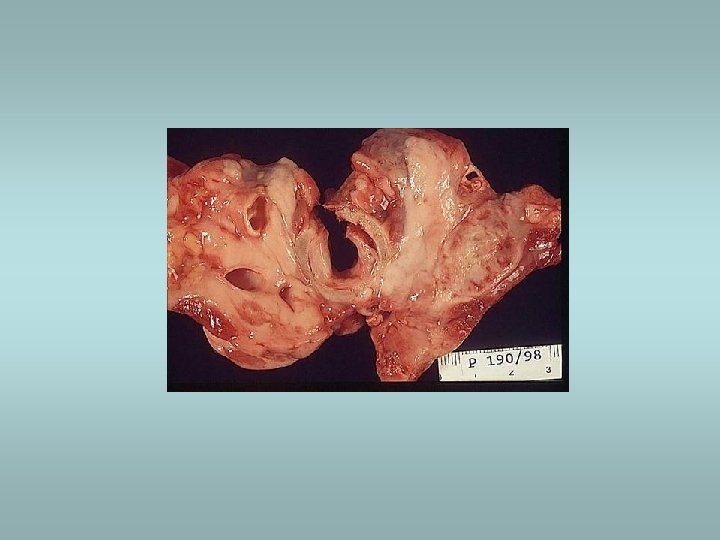
Tumors Benign – adenomas ü Well demarcated ü Fibrosis ü Haemorrhage ü Calcifications ü Hürtle cell adenoma - oncocytic ü Usually „cold“ Malignant - carcinomas ü See transparency


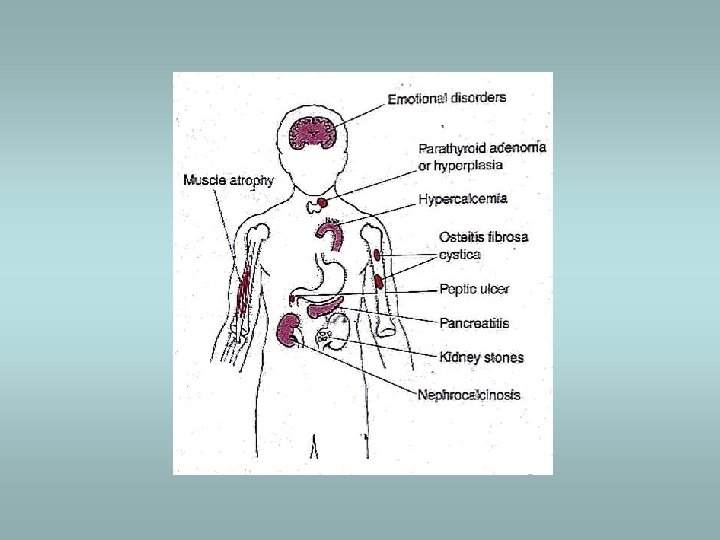
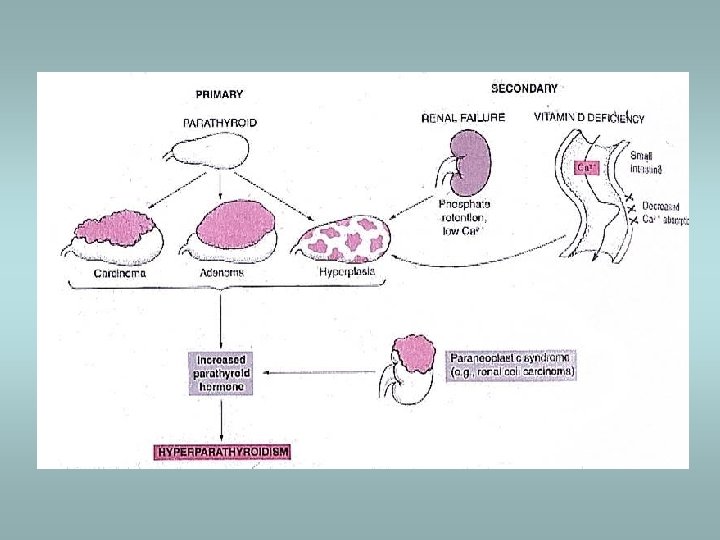
Parathyroid gland Primary hyperparathyroidism ü Hypersecretion of parathormone ü Caused by adenoma (80%), hyperplasia (15%), carcinoma (5%) ü Bone resorption, hypercalcemia – osteoporosis, muscle weaknes, nephrolithiasis, ulcers, pancreatitis, headache, depression Secondary hyperparathyroidism ü In patients with renal failure ü Compensatory hypersecretion of parathormone (reaction to phosphate retention and hypocalcemia)

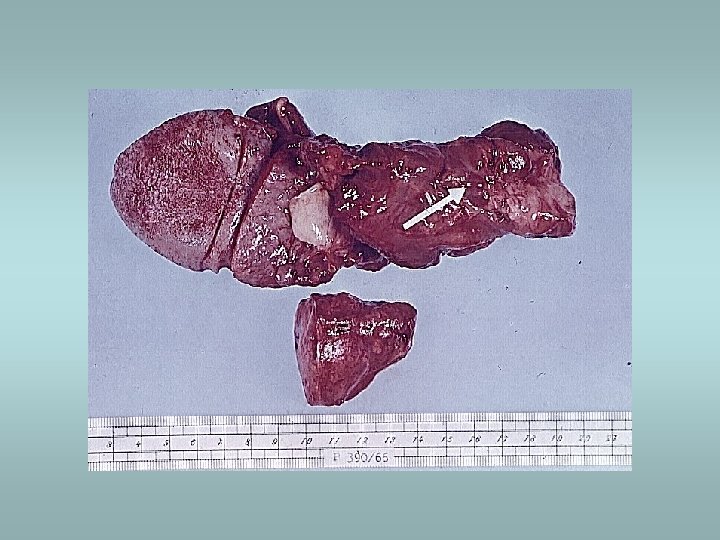
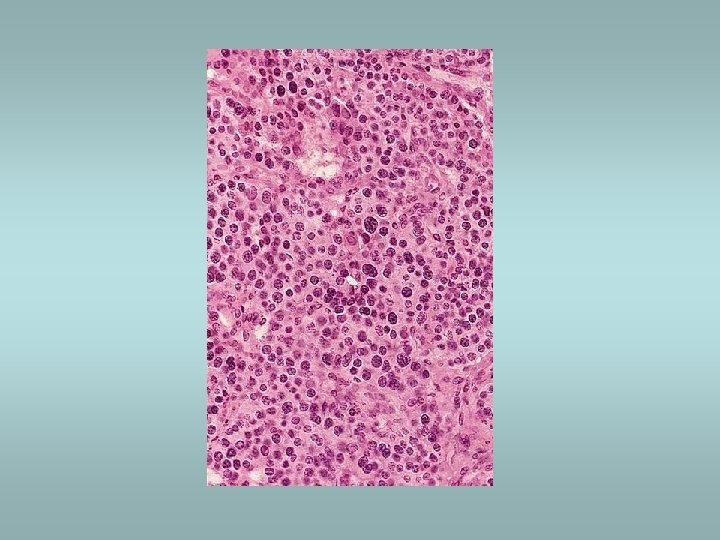
Parathyroid gland - tumors Adenoma ü Solitary, encapsulated – compression of adjacent gland ü No stromal fat ü Composed predominatly of chief cells ü Part of MEN I, MEN II Carcinoma ü Rare ü Invasion, metastases Hyperplasia ü All glands ü Fat cells interspersed

Hypoparathyroidism, pseudohypoparathyroidism Hypoparathyroidism ü Multiple etiology (surgical removal, autoimunne destruction, congenital…) ü Tetany, neuromuscular excitability, paraesthesiae psychosis Pseudohypoparathyroidism ü Rare ü Abnormality PTH receptors, loss of responsiveness, hypocalcemia ü Compensatory parathyroid hyperfunction

Adrenal cortex - hyperfunction Three syndromes: ü Cushing’s syndrome ü Hyperaldosteronism ü Adrenogenital syndromes

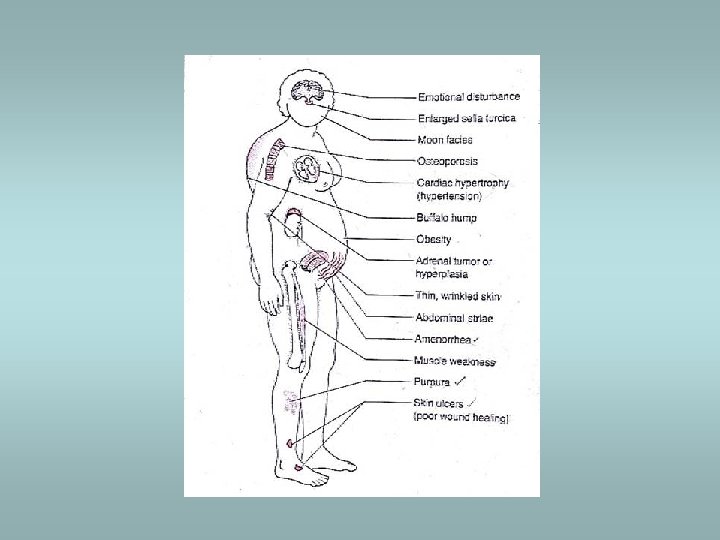
Cushing’s syndrome Causes: ü Administration of exogenous glucocorticoids – most common ü Pituitary hypersecretion of ACTH (Cushing’s disease) – adenoma ü Ectopic ACTH secretion – small cell carcinoma !! Histology: ü Crooke’s hyaline changes within pituitary basophils Clinically: ü Central obesity, moon facies, fatigability, hirsutism, hypertension, osteoporosis, cutaneous striae

Hyperaldosteronism Conn’s syndrome: ü Adenoma/hyperplasia ü Excessive production of aldosterone – low plasma renin, sodium retention, hypertension, loss of potassium, muscular weakness, cardiac arrhytmias, metabolic alkalosis, tetany Secondary: ü Reduced glomerular perfusion (fail in blood volume) – activation of renin angiotensin system – stimulation of aldosterone secretion ü Most common

Adrenogenital syndromes ü Variable manifestation (virilization, pubertax praecox, hermaphroditism, pseudohermaphroditism) ü Autosomal recessive trait ü Most often – deficiency of 21 -hydroxylase - virilization

Hypofunction of adrenal cortex ü Adrenal crisis ü Addison’s disease ü Secondary insufficiency

Primary acute adrenocortical insufficiency ü Rapid withdrawal of steroids ü Massive destruction of steroids – Waterhouse. Friderichsen syndrome: • • • During septic meningococcal infection Massive hemorrhage Hypotension Shock DIC

Addison’s disease (chronic adrenocortical insufficiency) ü ü Autoimunne Infection (TBC, fungi, etc. ) Metastatic cancer (lung, stomach, etc. ) Clinically: • • Anorexia Weakness Cutaneous hyperpigmentation ACTH elevation (in primary insufficiency) Secondary insufficiency ü decreased production of ACTH, absence of hyperpigmentation, normal aldosterone levels

Adrenal medulla Phaeochromocytoma ü Catecholamine production – hypertension ü 85% in medulla (extra-adrenal tumors designated paragangliomas) ü Sporadic (90%) or associated with familial syndromes (MEN, von Hippel-Lindau, von Recklinghausen) ü Histologically – pleomorphism, mitotic activity - however there are no reliable histological predictors of malignancy!! ü Only criterion of malignancy – metastasis Other tumors – neuroblastoma, ganglioneuroma

Multiple Endocrine Neoplasia MEN I (Wermer’s syndrome) ü Parathyroid (hyperplasia, adenoma) ü Pancreas (islet cell tumors) ü Pituitary (adenoma) MEN II (Sipple’s syndrome) ü Medullary thyroid carcinoma ü Phaeochromocytoma ü Parathyroid adenoma/hyperplasia MEN III ü MEN II and neuroma/ganglioneuroma All MENs – autosomal dominant trait

- Slides: 56