The Enablers Project Yin Li Special Projects Coordinator

The Enablers Project Yin Li – Special Projects Coordinator Anne Harley – Aged and Palliative Care Coordinator
Diagnosis Results Day 1 Day 2 Day 5 • Came in ready to implement our Integrated Care Project • Not enough consultation • Too many assumptions • Too process driven, not person centred • No focus on culture or intrinsic motivators Measuresconsultation were not indicative of a ‘value add’and fortheir our target • Planned with General Practices audience external providers • Additional measures for patient and provider experience • Investigate activities to promote culture change and team building based on lessons learnt from Collaboratives model

Rationale for Change Patients in South Western Sydney with chronic conditions experience fragmented care contributed in part by: • Recording and sharing of inaccurate and unreliable patient data; • Ineffective communication between members of their care team; and • Care planning that is not person-centred

Overarching Aims & Objectives • To improve the care and experience of our patients with chronic conditions through improved care planning within general practice that is person-centred and through improved communication between their care team members. Specifically to: • Improve the accuracy and completeness of patient data • Improve information sharing via secure messaging and use of My Health Record • Increase practice team capacity to prepare person-centred care plans

Mission Statement • South Western Sydney has high chronic disease incidence and prevalence when compared with NSW. It is folly to think that people with chronic diseases are able to receive optimal care from isolated health care professionals. Joined up, person-centred integrated care is data driven and reliant upon effective communication and care planning. As a foundational step towards integrated care, SWSPHN wishes to work with general practice and primary health providers to develop quality primary care data, seamless communication practices and coordinated care planning to positively influence health outcomes for our community members and reduce health care professional burden.
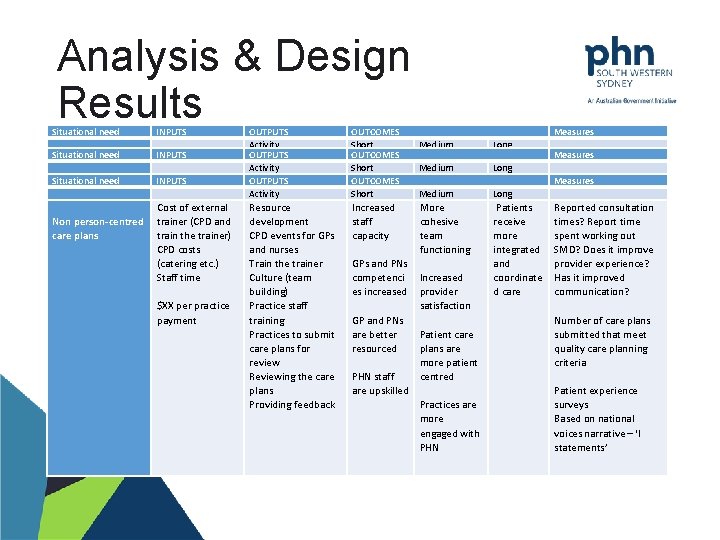
Analysis & Design Results Situational need Situationaland need Recording sharing of inaccurate and Situational need data Ineffectivepatient unreliable communication between members Non person-centred of their care team care plans INPUTS QIPC program Staff time INPUTS Buying SMD licenses Cost external Staff of time trainer (CPD and train the trainer) CPD costs (catering etc. ) Staff time $XX per practice payment OUTPUTS Activity OUTPUTS 4/12 Benchmarking Activity reports OUTPUTS Internalspecific staff Disease Activity training reports Resource CAT training Providing/installing Goal development SMDsetting licenses Regular 6/52 CPD events Practicefollow-up stafffor GPs Culture and nurses training in SMD Train usagethe trainer Culture Practice(team staff building) training in MHR Practice usage staff training Engaging with allied Practices to submit health/specialist care plans for Culture – bringing review GPs and their Reviewing the care providers together plans to build trust Providing feedback OUTCOMES Short OUTCOMES Data quality Short will improve OUTCOMES Increase Short SMD usage Increased (sending and staff receiving) capacity Increase GPs PNs MHRand usage competenci (uploading es SHSincreased and viewing) GP and PNs are better resourced PHN staff are upskilled Measures Medium Recall reminder Medium systems Improved improve Medium communicati More Information on between that shared is cohesive GPs isand more accurate team external and reliable functioning providers Increased provider satisfaction Patient care plans are more patient centred Practices are more engaged with PHN Long Patients Long receive Patients more Long receive integrated Patients and more coordinated receive integrated care more and integrated coordinate and d coordinate d care Measures % data quality improvement for Measures Number of recording of secure risk factors, messages sent/received coded diagnoses, Reported consultation medications etc. number over time – can measure times? Report time of messages viewed? ? ? spent working Provider views out SMD? Does it improve provider Reductionexperience? in faxes and Has it improved letters sent/received – communication? can measure number of letters printed? Number of care plans submitted that meet Improved provider quality care experience planning criteria Patient experience surveys Based on national voices narrative – ‘I statements’

Action Plan with Timescales Action When Consult with practices that participated in pilot project ASAP Consult with potential practices for the Enablers Wave 2 ASAP Bring GPs and their referrers together to build trust and co-design ASAP Create tools to support culture and team building ASAP Create patient experience and provider experience measurement tools ASAP
- Slides: 7