The Digestive System Mouthbite chew swallow Pharynx and
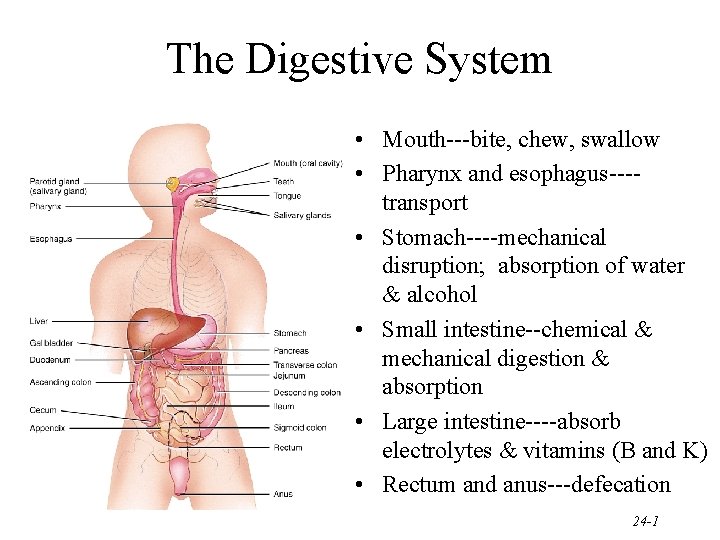
The Digestive System • Mouth---bite, chew, swallow • Pharynx and esophagus---transport • Stomach----mechanical disruption; absorption of water & alcohol • Small intestine--chemical & mechanical digestion & absorption • Large intestine----absorb electrolytes & vitamins (B and K) • Rectum and anus---defecation 24 -1

Types of Digestion • Mechanical – mouth, stomach, SI, LI • Chemical – mouth, stomach, SI 24 -2
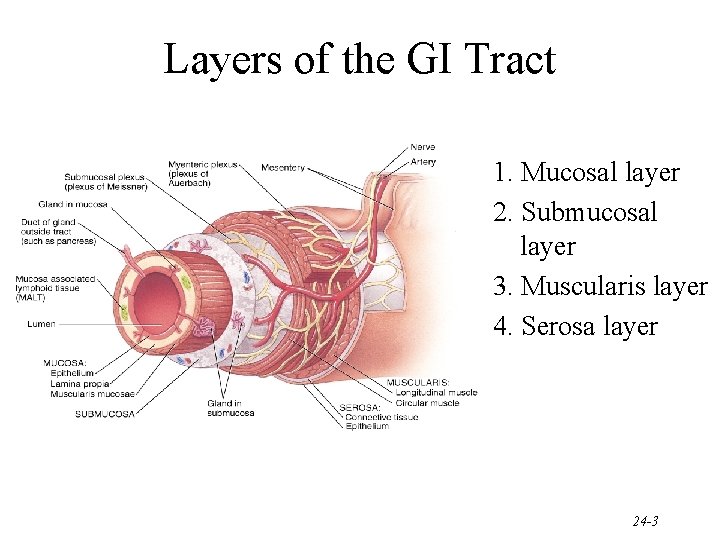
Layers of the GI Tract 1. Mucosal layer 2. Submucosal layer 3. Muscularis layer 4. Serosa layer 24 -3
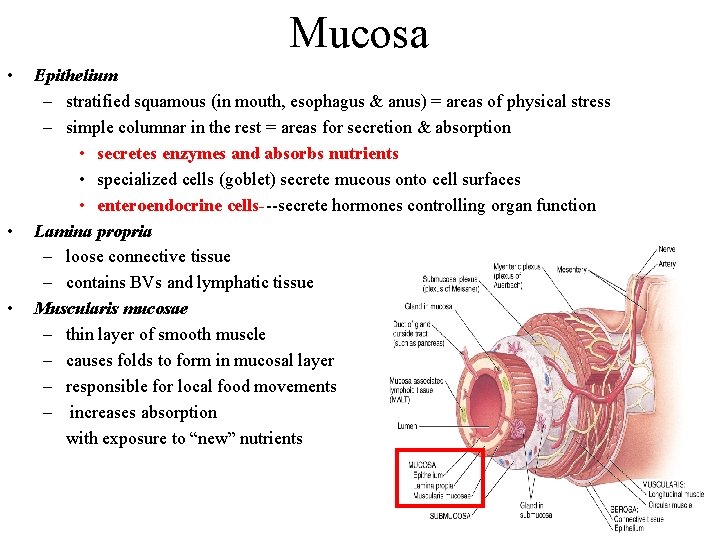
Mucosa • • • Epithelium – stratified squamous (in mouth, esophagus & anus) = areas of physical stress – simple columnar in the rest = areas for secretion & absorption • secretes enzymes and absorbs nutrients • specialized cells (goblet) secrete mucous onto cell surfaces • enteroendocrine cells---secrete hormones controlling organ function Lamina propria – loose connective tissue – contains BVs and lymphatic tissue Muscularis mucosae – thin layer of smooth muscle – causes folds to form in mucosal layer – responsible for local food movements – increases absorption with exposure to “new” nutrients 24 -4
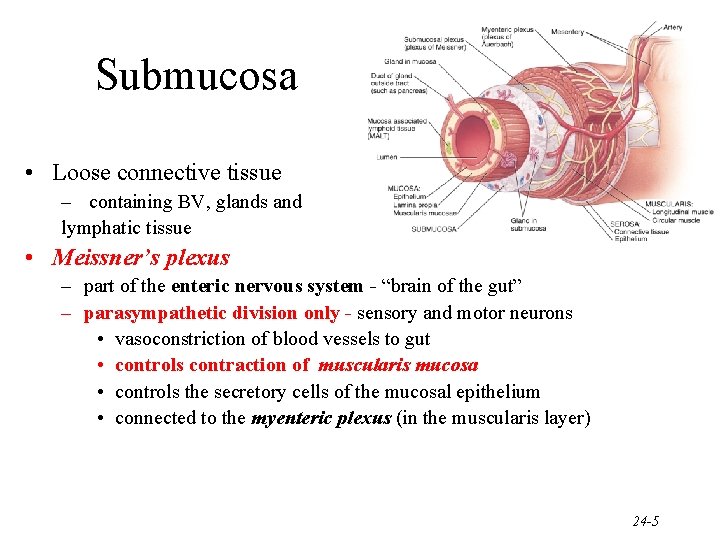
Submucosa • Loose connective tissue – containing BV, glands and lymphatic tissue • Meissner’s plexus – part of the enteric nervous system - “brain of the gut” – parasympathetic division only - sensory and motor neurons • vasoconstriction of blood vessels to gut • controls contraction of muscularis mucosa • controls the secretory cells of the mucosal epithelium • connected to the myenteric plexus (in the muscularis layer) 24 -5
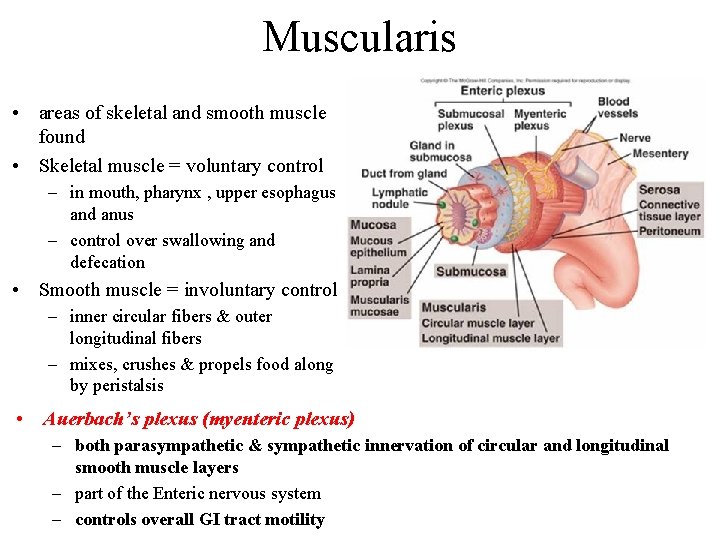
Muscularis • areas of skeletal and smooth muscle found • Skeletal muscle = voluntary control – in mouth, pharynx , upper esophagus and anus – control over swallowing and defecation • Smooth muscle = involuntary control – inner circular fibers & outer longitudinal fibers – mixes, crushes & propels food along by peristalsis • Auerbach’s plexus (myenteric plexus) – both parasympathetic & sympathetic innervation of circular and longitudinal smooth muscle layers – part of the Enteric nervous system – controls overall GI tract motility
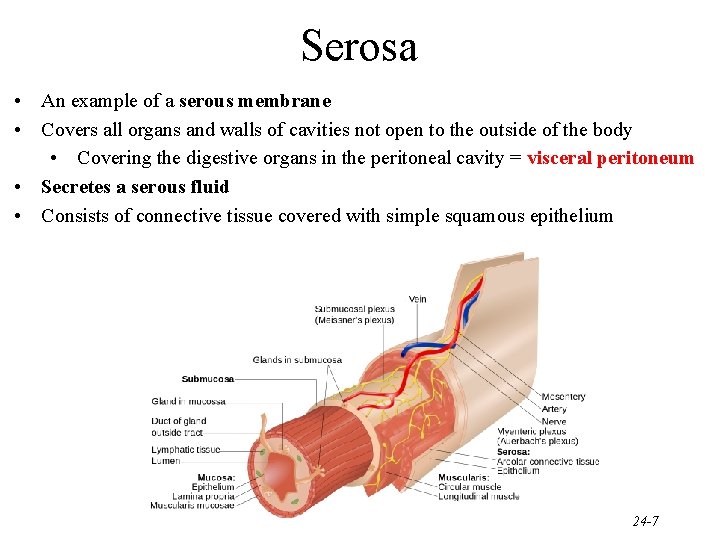
Serosa • An example of a serous membrane • Covers all organs and walls of cavities not open to the outside of the body • Covering the digestive organs in the peritoneal cavity = visceral peritoneum • Secretes a serous fluid • Consists of connective tissue covered with simple squamous epithelium 24 -7
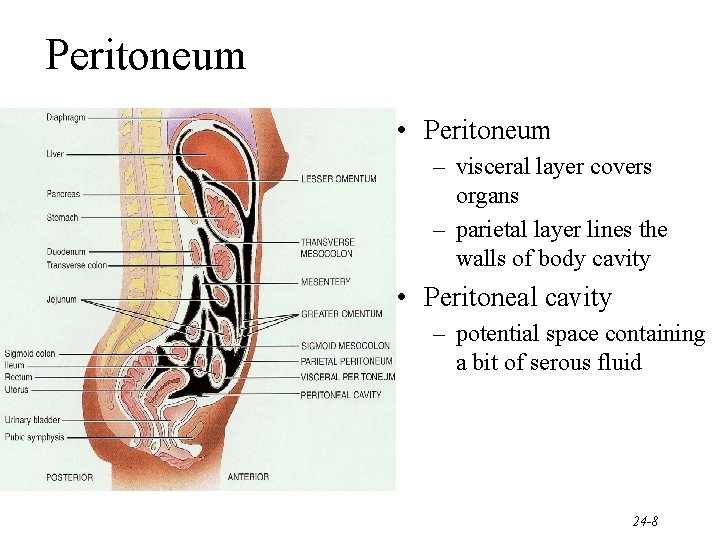
Peritoneum • Peritoneum – visceral layer covers organs – parietal layer lines the walls of body cavity • Peritoneal cavity – potential space containing a bit of serous fluid 24 -8
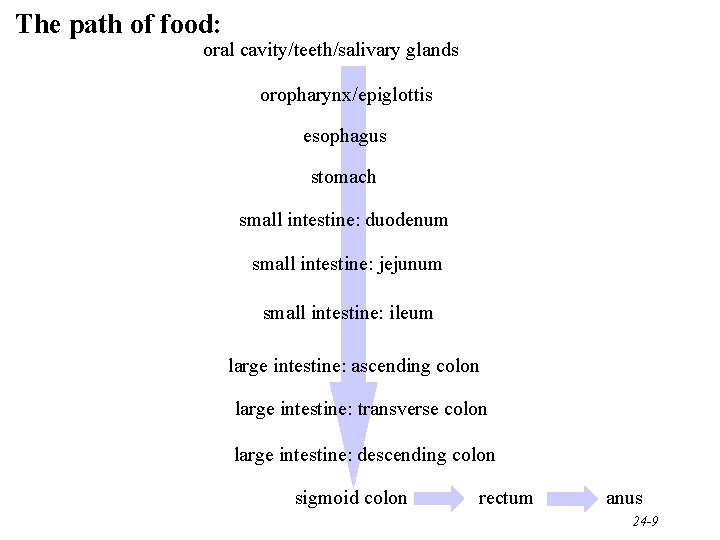
The path of food: oral cavity/teeth/salivary glands oropharynx/epiglottis esophagus stomach small intestine: duodenum small intestine: jejunum small intestine: ileum large intestine: ascending colon large intestine: transverse colon large intestine: descending colon sigmoid colon rectum anus 24 -9
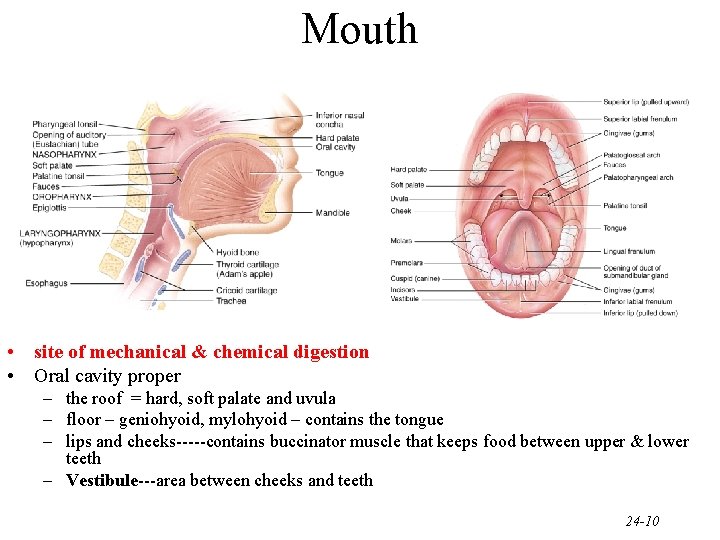
Mouth • site of mechanical & chemical digestion • Oral cavity proper – the roof = hard, soft palate and uvula – floor – geniohyoid, mylohyoid – contains the tongue – lips and cheeks-----contains buccinator muscle that keeps food between upper & lower teeth – Vestibule---area between cheeks and teeth 24 -10
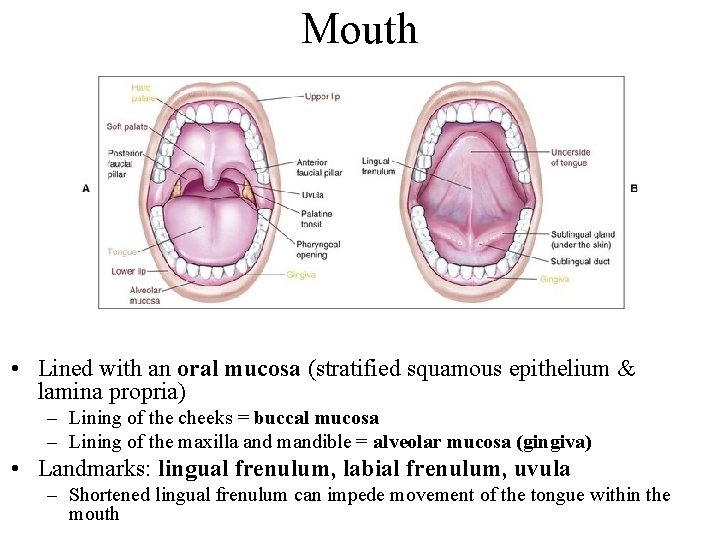
Mouth • Lined with an oral mucosa (stratified squamous epithelium & lamina propria) – Lining of the cheeks = buccal mucosa – Lining of the maxilla and mandible = alveolar mucosa (gingiva) • Landmarks: lingual frenulum, labial frenulum, uvula – Shortened lingual frenulum can impede movement of the tongue within the mouth
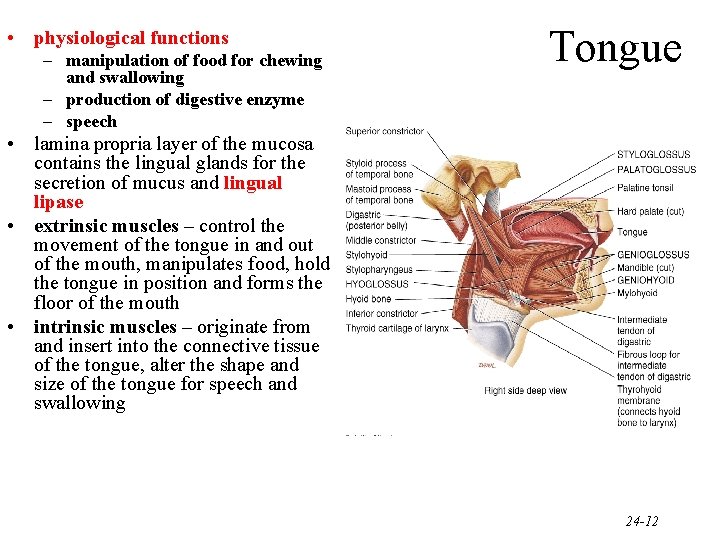
• physiological functions – manipulation of food for chewing and swallowing – production of digestive enzyme – speech Tongue • lamina propria layer of the mucosa contains the lingual glands for the secretion of mucus and lingual lipase • extrinsic muscles – control the movement of the tongue in and out of the mouth, manipulates food, hold the tongue in position and forms the floor of the mouth • intrinsic muscles – originate from and insert into the connective tissue of the tongue, alter the shape and size of the tongue for speech and swallowing 24 -12
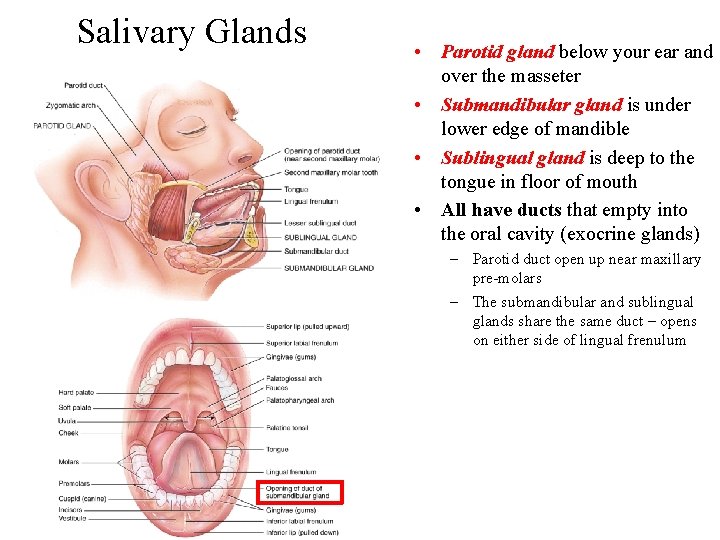
Salivary Glands • Parotid gland below your ear and over the masseter • Submandibular gland is under lower edge of mandible • Sublingual gland is deep to the tongue in floor of mouth • All have ducts that empty into the oral cavity (exocrine glands) – Parotid duct open up near maxillary pre-molars – The submandibular and sublingual glands share the same duct – opens on either side of lingual frenulum
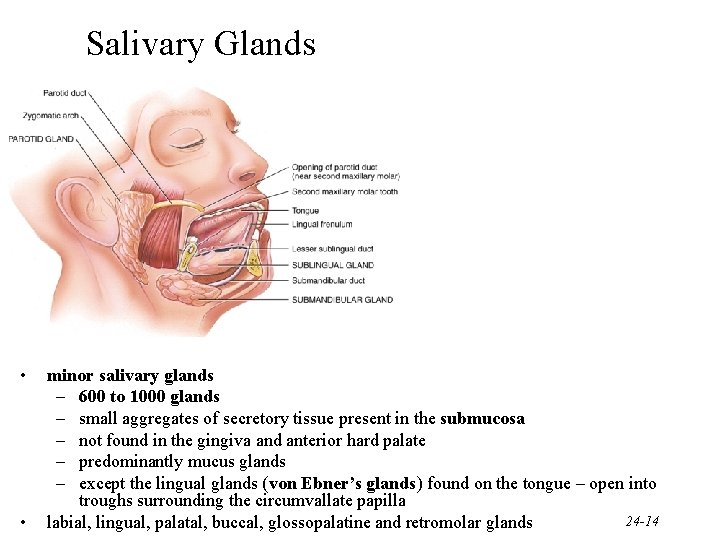
Salivary Glands • • minor salivary glands – 600 to 1000 glands – small aggregates of secretory tissue present in the submucosa – not found in the gingiva and anterior hard palate – predominantly mucus glands – except the lingual glands (von Ebner’s glands) found on the tongue – open into troughs surrounding the circumvallate papilla 24 -14 labial, lingual, palatal, buccal, glossopalatine and retromolar glands
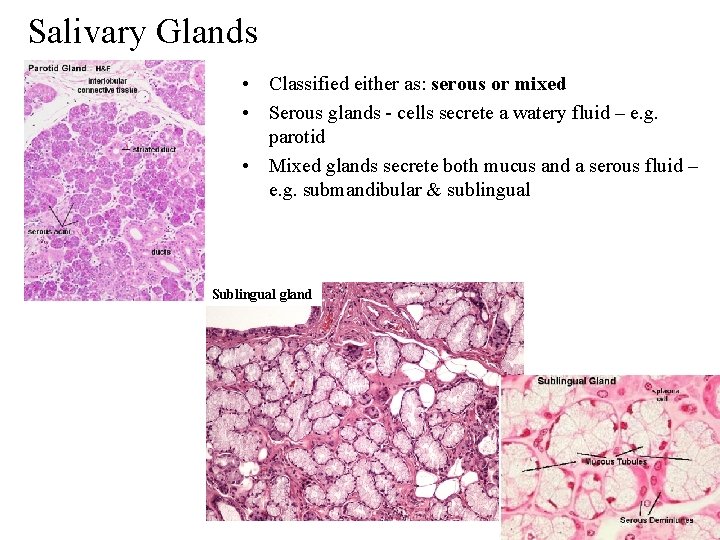
Salivary Glands • Classified either as: serous or mixed • Serous glands - cells secrete a watery fluid – e. g. parotid • Mixed glands secrete both mucus and a serous fluid – e. g. submandibular & sublingual Sublingual gland

Saliva • • Components: 1. water 2. enzymes: amylase, lipase, lyzozyme 3. mucins, mucus – composition can vary from gland to gland – parotid gland: watery fluid rich in amylase, proline-rich proteins and glycoproteins – submandibular gland also contains higher levels of mucins • 4. multiple electrolytes: sodium, postassium, chloride, calcium, magnesium • 5. glucose, amino acids, urea, uric acid and lipids • 6. secretory Igs – Ig. G and Ig. M and Ig. A • 7. growth factors & hormones: EGF, insulin
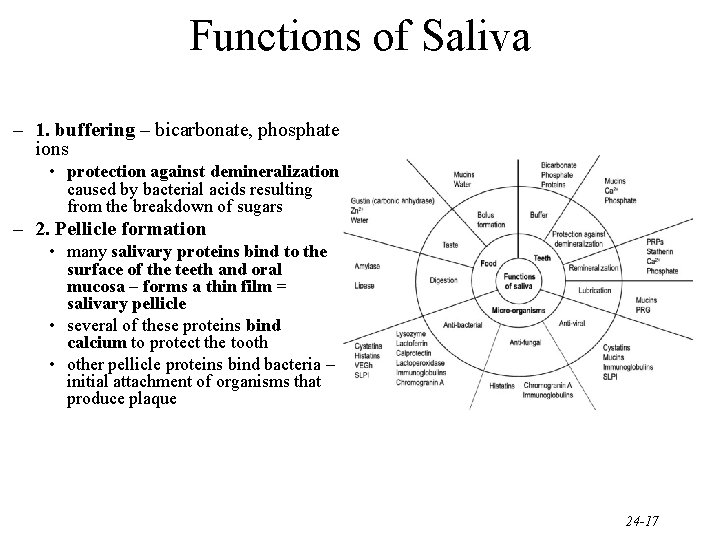
Functions of Saliva – 1. buffering – bicarbonate, phosphate ions • protection against demineralization caused by bacterial acids resulting from the breakdown of sugars – 2. Pellicle formation • many salivary proteins bind to the surface of the teeth and oral mucosa – forms a thin film = salivary pellicle • several of these proteins bind calcium to protect the tooth • other pellicle proteins bind bacteria – initial attachment of organisms that produce plaque 24 -17

Functions of Saliva – 3. maintenance of tooth integrity • saliva is saturated with calcium and phosphate ions • at the tooth surface the high concentration of calcium and phosphate results in maturation of the enamel – increases surface hardness • re-mineralization of lesions upon caries can also be induced by saliva – enhanced by fluoride in the saliva • repair to large areas of enamel breakdown is not possible – 4. antimicrobial action • barrier function provided by mucins • saliva also contains a spectrum of proteins with antimicrobial activity – histatins, lysozyme, lactoferrin and peroxidase • also the presence of antibodies – Ig. A is the major salivary Ig (results in agglutination of microbes and prevents their adherence to oral tissues) 24 -18

Functions of Saliva – 5. tissue repair • variety of growth factors are present in saliva • many promote tissue growth and differentiation – 6. digestion • wets food for swallowing – produces the bolus • chemical digestion via amylase and lipase – 7. taste • solubilizes food substances – allows binding to taste receptors located in taste buds 24 -19

Salivation • controlled by the ANS • parasympathetic system provides a constant supply of saliva to keep the mucus membranes moist and to lubricate the food • Increased salivation – parasympathetic system – sight, smell, sounds, memory of food, tongue stimulation---rock in mouth – stimulation of taste receptors are conveyed to the cerebral cortex to the salivatory nuclei in brainstem- returning impulses via the parasymp system travel via CN 7 & 9 • Decreased salivation – sympathetic system – dry mouth when you are afraid – also inhibits salivation during dehydration 24 -20

Mumps • Myxovirus that attacks the parotid gland • Symptoms – inflammation and enlargement of the parotid – fever, malaise & sour throat (especially swallowing sour foods) – swelling on one or both sides • Sterility rarely possible in males with testicular involvement (only one side involved) • Vaccine available since 1967 24 -21

Digestion in the Mouth • Mechanical digestion = mastication or chewing • breaks food into pieces • mixes food with saliva so it forms a bolus • Chemical digestion – salivary amylase • begins starch digestion at p. H of 6. 5 or 7. 0 found in mouth • when bolus & enzyme hit the p. H 2. 5 gastric juices hydrolysis ceases – lingual lipase • secreted by glands in lamina propria of tongue • begins breakdown of long and medium-chain triglycerides into a free fatty acids and a diglyceride 24 -22
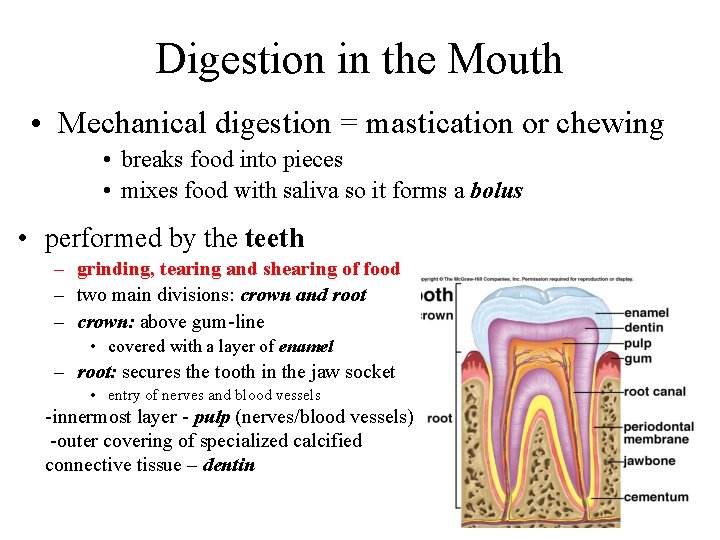
Digestion in the Mouth • Mechanical digestion = mastication or chewing • breaks food into pieces • mixes food with saliva so it forms a bolus • performed by the teeth – grinding, tearing and shearing of food – two main divisions: crown and root – crown: above gum-line • covered with a layer of enamel – root: secures the tooth in the jaw socket • entry of nerves and blood vessels -innermost layer - pulp (nerves/blood vessels) -outer covering of specialized calcified connective tissue – dentin 24 -23

Pharynx • Funnel-shaped tube extending from internal nares to the esophagus (posteriorly) and larynx (anteriorly) • Skeletal muscle lined by mucous membrane • Deglutition or swallowing is facilitated by saliva and mucus – starts when bolus is pushed into the oropharynx – sensory nerves send signals to deglutition center in brainstem (medulla oblongata) 24 -24
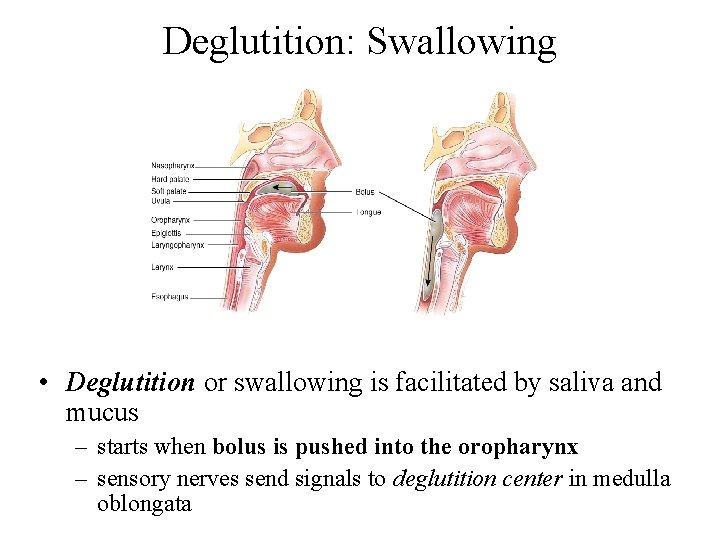
Deglutition: Swallowing • Deglutition or swallowing is facilitated by saliva and mucus – starts when bolus is pushed into the oropharynx – sensory nerves send signals to deglutition center in medulla oblongata
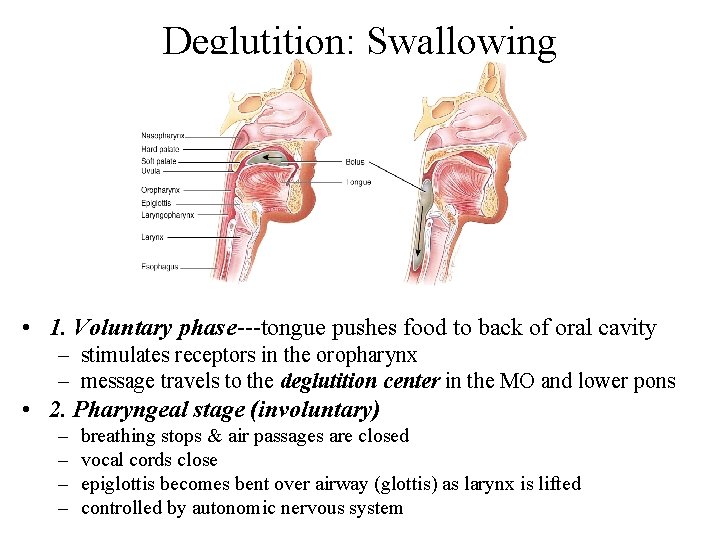
Deglutition: Swallowing • 1. Voluntary phase---tongue pushes food to back of oral cavity – stimulates receptors in the oropharynx – message travels to the deglutition center in the MO and lower pons • 2. Pharyngeal stage (involuntary) – – breathing stops & air passages are closed vocal cords close epiglottis becomes bent over airway (glottis) as larynx is lifted controlled by autonomic nervous system
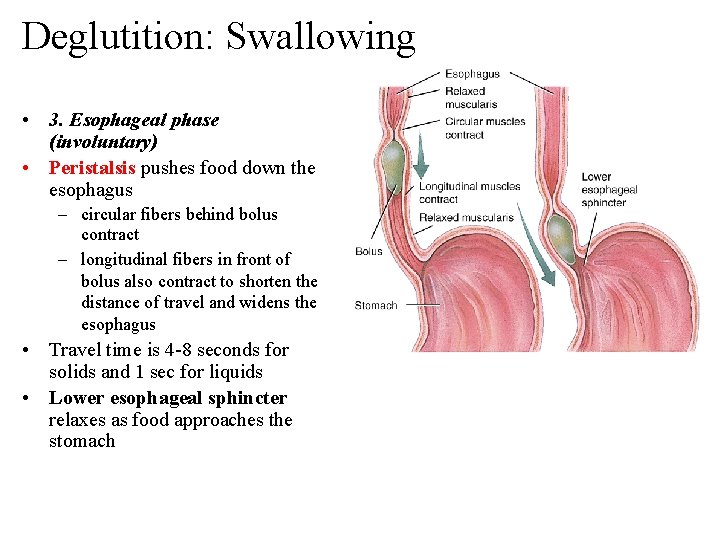
Deglutition: Swallowing • 3. Esophageal phase (involuntary) • Peristalsis pushes food down the esophagus – circular fibers behind bolus contract – longitudinal fibers in front of bolus also contract to shorten the distance of travel and widens the esophagus • Travel time is 4 -8 seconds for solids and 1 sec for liquids • Lower esophageal sphincter relaxes as food approaches the stomach
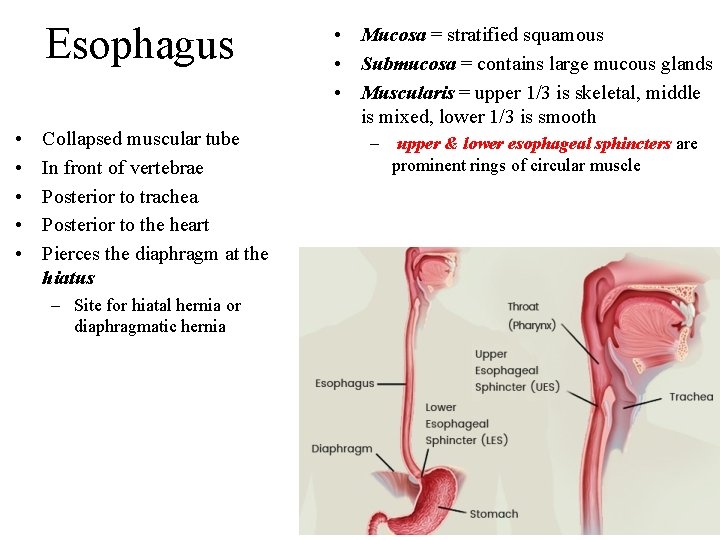
Esophagus • • • Collapsed muscular tube In front of vertebrae Posterior to trachea Posterior to the heart Pierces the diaphragm at the hiatus – Site for hiatal hernia or diaphragmatic hernia • Mucosa = stratified squamous • Submucosa = contains large mucous glands • Muscularis = upper 1/3 is skeletal, middle is mixed, lower 1/3 is smooth – upper & lower esophageal sphincters are prominent rings of circular muscle

Gastroesophageal Reflex Disease • If lower esophageal sphincter fails to open – distension of esophagus feels like chest pain or heart attack • If lower esophageal sphincter fails to close – stomach acids enter esophagus & cause heartburn (GERD) – for a weak sphincter---don't eat a large meal and lay down in front of TV – smoking and alcohol make the sphincter relax worsening the situation • Control the symptoms by avoiding – coffee, chocolate, tomatoes, fatty foods, onions & mint – take Tagamet HB or Pepcid AC 60 minutes before eating – neutralize existing stomach acids with Tums

Stomach--Chemical Digestion • Protein digestion begins – HCl denatures (unfolds) protein molecules – HCl transforms pepsinogen into pepsin that breaks peptides bonds between certain amino acids • Fat digestion continues – gastric lipase splits the triglycerides in milk fat • most effective at p. H 5 to 6 (infant stomach) • HCl kills microbes in food • Mucous cells protect stomach walls from being digested – 1 -3 mm thick layer of mucous 24 -30
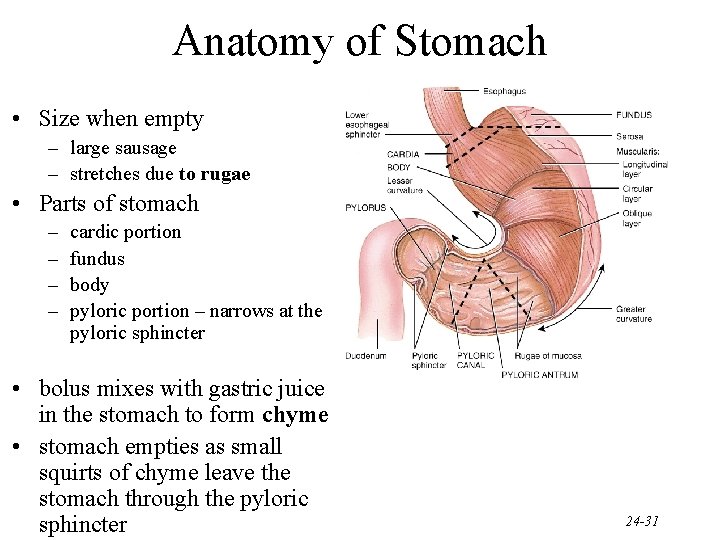
Anatomy of Stomach • Size when empty – large sausage – stretches due to rugae • Parts of stomach – – cardic portion fundus body pyloric portion – narrows at the pyloric sphincter • bolus mixes with gastric juice in the stomach to form chyme • stomach empties as small squirts of chyme leave the stomach through the pyloric sphincter 24 -31
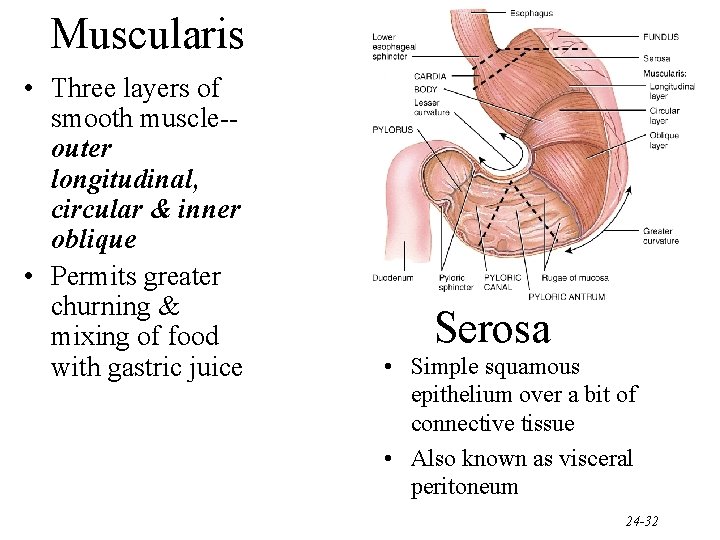
Muscularis • Three layers of smooth muscle-outer longitudinal, circular & inner oblique • Permits greater churning & mixing of food with gastric juice Serosa • Simple squamous epithelium over a bit of connective tissue • Also known as visceral peritoneum 24 -32
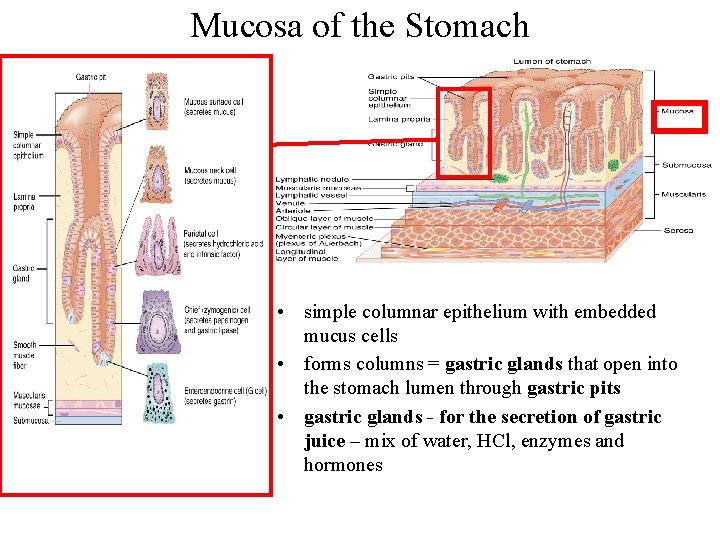
Mucosa of the Stomach • simple columnar epithelium with embedded mucus cells • forms columns = gastric glands that open into the stomach lumen through gastric pits • gastric glands - for the secretion of gastric juice – mix of water, HCl, enzymes and hormones

Histology of the Stomach - Mucosa • • • food can remain in the fundus of the stomach for up to one hour before being mixed with gastric juice during this time – salivary amylase and lipase continue their digestion after being mixed with gastric juice – these enzymes become inactivated 24 -34
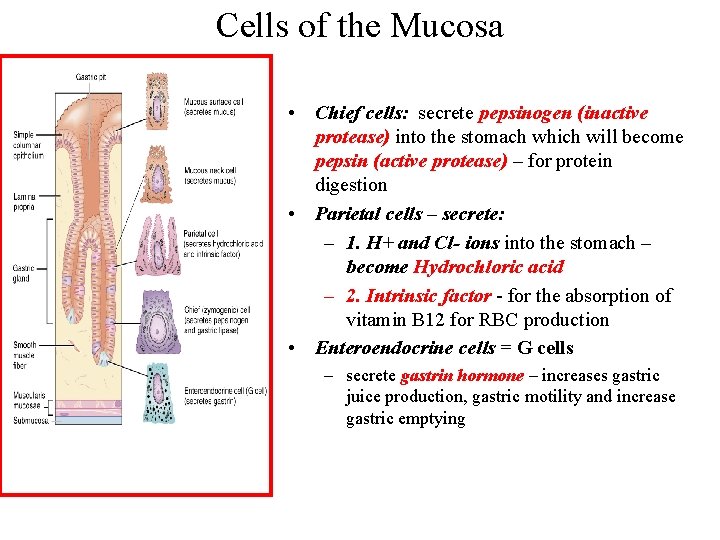
Cells of the Mucosa • Chief cells: secrete pepsinogen (inactive protease) into the stomach which will become pepsin (active protease) – for protein digestion • Parietal cells – secrete: – 1. H+ and Cl- ions into the stomach – become Hydrochloric acid – 2. Intrinsic factor - for the absorption of vitamin B 12 for RBC production • Enteroendocrine cells = G cells – secrete gastrin hormone – increases gastric juice production, gastric motility and increase gastric emptying
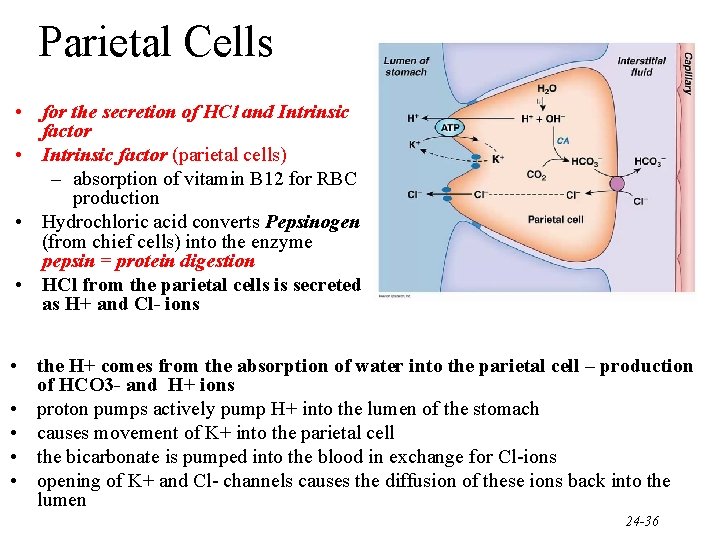
Parietal Cells • for the secretion of HCl and Intrinsic factor • Intrinsic factor (parietal cells) – absorption of vitamin B 12 for RBC production • Hydrochloric acid converts Pepsinogen (from chief cells) into the enzyme pepsin = protein digestion • HCl from the parietal cells is secreted as H+ and Cl- ions • the H+ comes from the absorption of water into the parietal cell – production of HCO 3 - and H+ ions • proton pumps actively pump H+ into the lumen of the stomach • causes movement of K+ into the parietal cell • the bicarbonate is pumped into the blood in exchange for Cl-ions • opening of K+ and Cl- channels causes the diffusion of these ions back into the lumen 24 -36
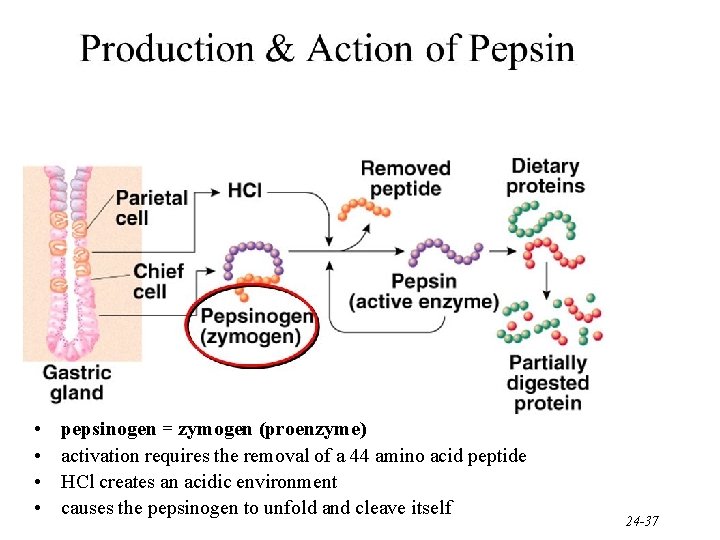
• • pepsinogen = zymogen (proenzyme) activation requires the removal of a 44 amino acid peptide HCl creates an acidic environment causes the pepsinogen to unfold and cleave itself 24 -37

Gastric Mucosa Secretions • Parietal cells: HCl and Intrinsic Factor • Chief cells: pepsin and gastric lipase – pepsin – breaks down proteins into smaller peptides • most efficient at breaking the peptide bonds at the Nterminus end of phenylalanine, tyrosine and tryptophan – gastric lipase – like lingual lipase it removes one fatty acid to create a free fatty acid and a diglyceride • lingual and gastric lipases are known as acidic lipases • they do not require bile to function 24 -38

Absorption of Nutrients by the Stomach • • Water especially if it is cold Electrolytes Some drugs (especially aspirin) & alcohol Gastric mucosal cells contain alcohol dehydrogenase that converts some alcohol to acetaldehyde – more of this enzyme found in males than females – 5 different forms of ADH – some more efficient then others 24 -39

Gastric phase of digestion • starts once food reaches the stomach • stretching of the stomach begins this phase • neural and hormonal regulation to promote gastric secretion and motility 24 -40

Gastric phase of digestion: Neural Regulation • distension of the stomach stimulates stretch mechanoreceptors – stimulates production of gastric juices • chemoreceptors also detect elevated p. H (from bolus) – adds to the stimulation • impulses travel via the parasympathetic neurons of the Meissner’s plexus and the Auerbach’s plexus to the cells of the mucosa – stimulates the flow of gastric juice, causes waves of peristalsis to mix the food with the juice and move food into the SI • chemoreceptors monitor p. H of the stomach chyme as juice is being made – as the p. H of the stomach chyme decreases (becomes more acidic) –creates a negative feedback loop • as the food leaves the stomach and the stretching of the wall lessens – this inhibits this path
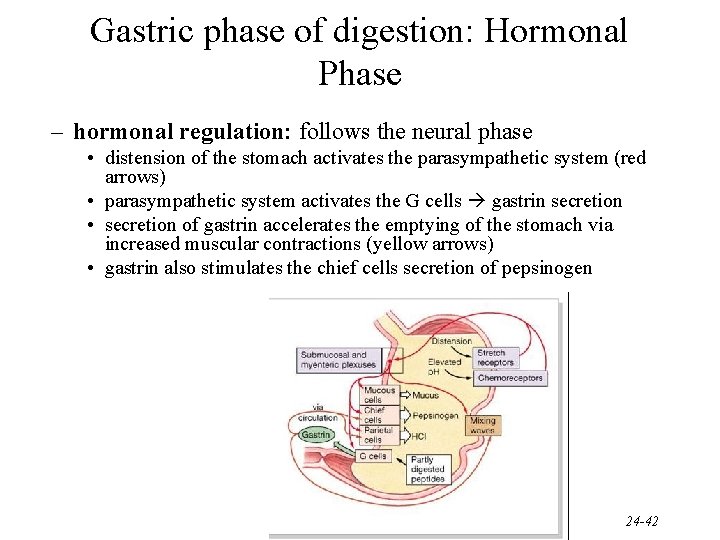
Gastric phase of digestion: Hormonal Phase – hormonal regulation: follows the neural phase • distension of the stomach activates the parasympathetic system (red arrows) • parasympathetic system activates the G cells gastrin secretion • secretion of gastrin accelerates the emptying of the stomach via increased muscular contractions (yellow arrows) • gastrin also stimulates the chief cells secretion of pepsinogen 24 -42
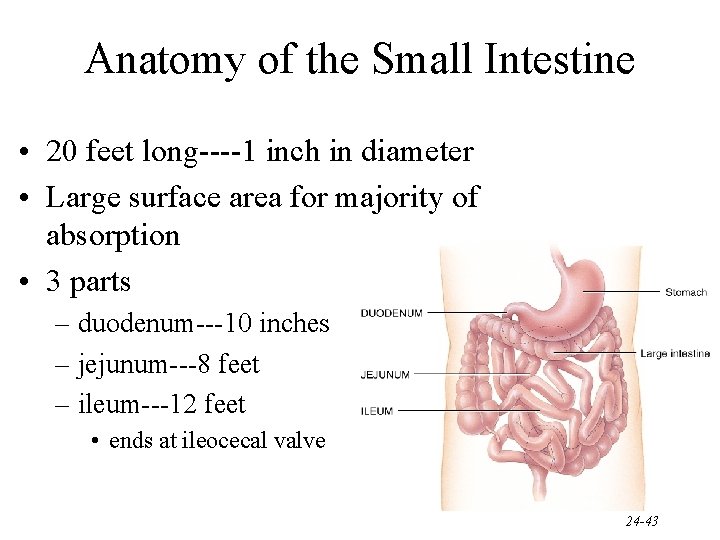
Anatomy of the Small Intestine • 20 feet long----1 inch in diameter • Large surface area for majority of absorption • 3 parts – duodenum---10 inches – jejunum---8 feet – ileum---12 feet • ends at ileocecal valve 24 -43
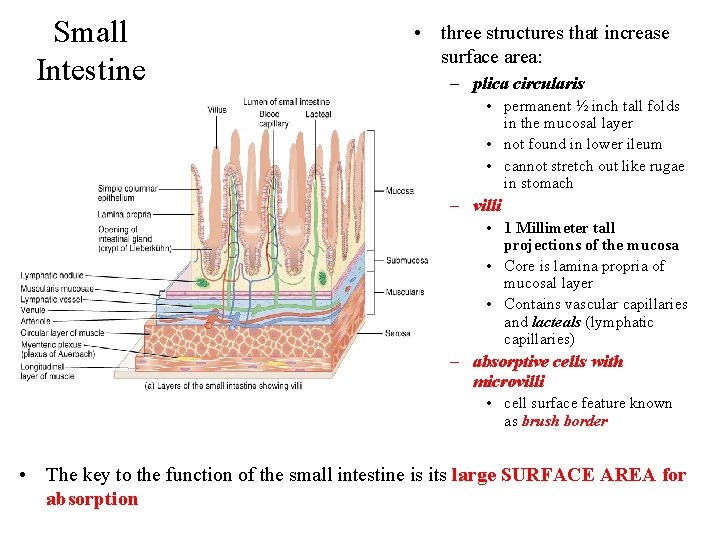
Small Intestine • three structures that increase surface area: – plica circularis • permanent ½ inch tall folds in the mucosal layer • not found in lower ileum • cannot stretch out like rugae in stomach – villi • 1 Millimeter tall projections of the mucosa • Core is lamina propria of mucosal layer • Contains vascular capillaries and lacteals (lymphatic capillaries) – absorptive cells with microvilli • cell surface feature known as brush border • The key to the function of the small intestine is its large SURFACE AREA for absorption
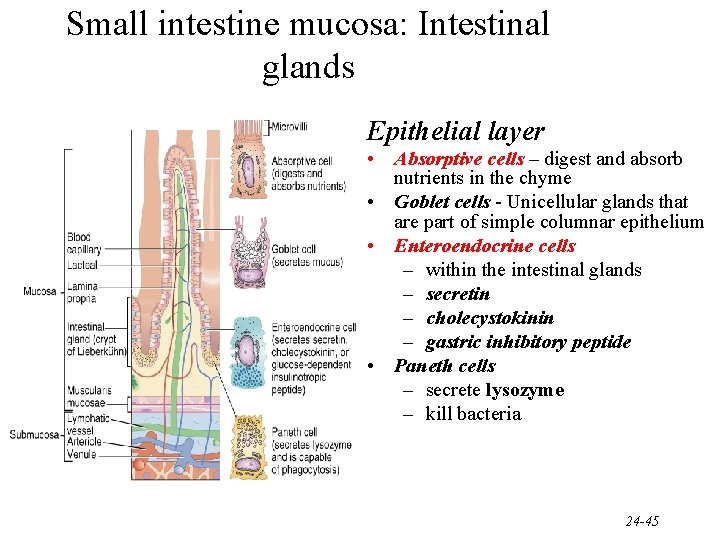
Small intestine mucosa: Intestinal glands Epithelial layer • Absorptive cells – digest and absorb nutrients in the chyme • Goblet cells - Unicellular glands that are part of simple columnar epithelium • Enteroendocrine cells – within the intestinal glands – secretin – cholecystokinin – gastric inhibitory peptide • Paneth cells – secrete lysozyme – kill bacteria 24 -45

SI mucos: the Lymphatic System • lamina propria of the SI contains areolar connective tissue • plus an abundance of mucosa-associated lymphatic tissue – MALT – solitary lymphatic nodules in the distal part of the ileum – groups of nodes in the ileum – Peyer’s patches 24 -46

Intestinal glands: Absorptive cells • for the production of brush-border enzymes (“intestinal juice”) • 1 to 2 liters per day • BB enzymes are made and inserted into the microvilli of the absorptive cells • enzymatic digestion by these enzymes occurs externally on these microvilli rather than in the lumen of the SI • BB enzymes: enzymes for the digestion of carbohydrates, proteins and nucleic acids • as the older cells of the villus are sloughed off and die – burst open and release more enzymes that digest more food in the chyme

Small Intestine: Chemical Digestion -protein and carbohydrate digestion via synthesis of the brush border enzymes by the intestinal glands -enterokinase -maltase, sucrase, lactase, a-dextrinase = small carbohydrates and disaccharides -aminopeptidase, dipeptidase = small peptides and dipeptides into amino acids -phosphatases and nucleosidases = nucleotides into nucleosides -resulting monosaccharides, amino acids and nucleotides are internalized by the absorptive cell -SO carbohydrate and protein digestion stops in the interior of the absorptive cell
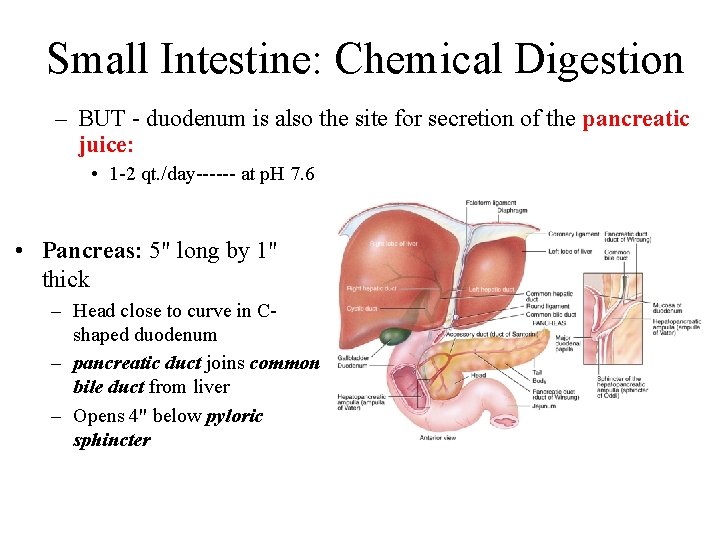
Small Intestine: Chemical Digestion – BUT - duodenum is also the site for secretion of the pancreatic juice: • 1 -2 qt. /day------ at p. H 7. 6 • Pancreas: 5" long by 1" thick – Head close to curve in Cshaped duodenum – pancreatic duct joins common bile duct from liver – Opens 4" below pyloric sphincter
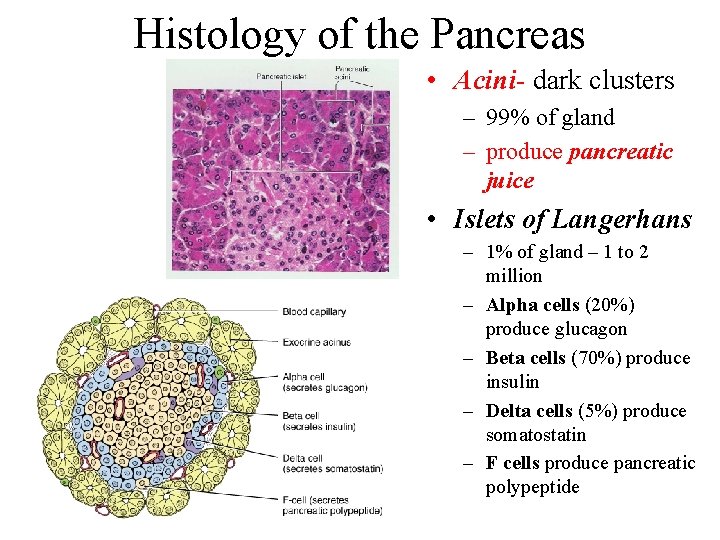
Histology of the Pancreas • Acini- dark clusters – 99% of gland – produce pancreatic juice • Islets of Langerhans – 1% of gland – 1 to 2 million – Alpha cells (20%) produce glucagon – Beta cells (70%) produce insulin – Delta cells (5%) produce somatostatin – F cells produce pancreatic polypeptide

Composition and Functions of Pancreatic Juice • these enzymes act before the BB enzymes • Contains water, enzymes & sodium bicarbonate • Digestive enzymes – pancreatic amylase = larger carbs into smaller disaccharides – pancreatic lipase = triglycerides – ribonuclease &deoxyribonuclease = digests nucleic acids into nucleotides – four proteases: trypsin, chymotrypsin, elastase, carboxypeptidase • these proteases are made in the pancreas as inactive forms – eg. trypsinogen, chymotrypsinogen, proelastase, procarboxypeptidase • trypsinogen converted to trypsin by the brush border enzyme enterokinase • activated trypsin then converts other three proteases into their active forms
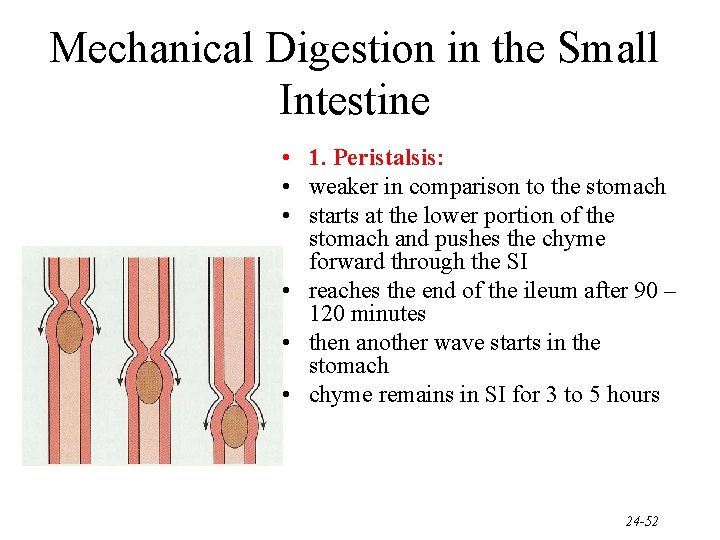
Mechanical Digestion in the Small Intestine • 1. Peristalsis: • weaker in comparison to the stomach • starts at the lower portion of the stomach and pushes the chyme forward through the SI • reaches the end of the ileum after 90 – 120 minutes • then another wave starts in the stomach • chyme remains in SI for 3 to 5 hours 24 -52

Mechanical Digestion in the Small Intestine • 2. Segmentation: • local mixing of chyme with “digestive juices” in the SI • does NOT push the food through the tract • just moves chyme back and forth in a segment • specific segments are defined by the smooth muscle layers • most rapid in the duodenum and slows at it reaches the ileum
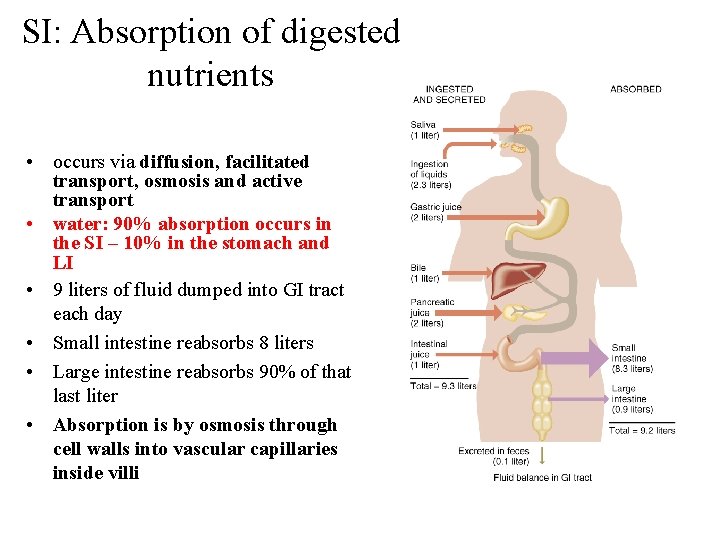
SI: Absorption of digested nutrients • occurs via diffusion, facilitated transport, osmosis and active transport • water: 90% absorption occurs in the SI – 10% in the stomach and LI • 9 liters of fluid dumped into GI tract each day • Small intestine reabsorbs 8 liters • Large intestine reabsorbs 90% of that last liter • Absorption is by osmosis through cell walls into vascular capillaries inside villi
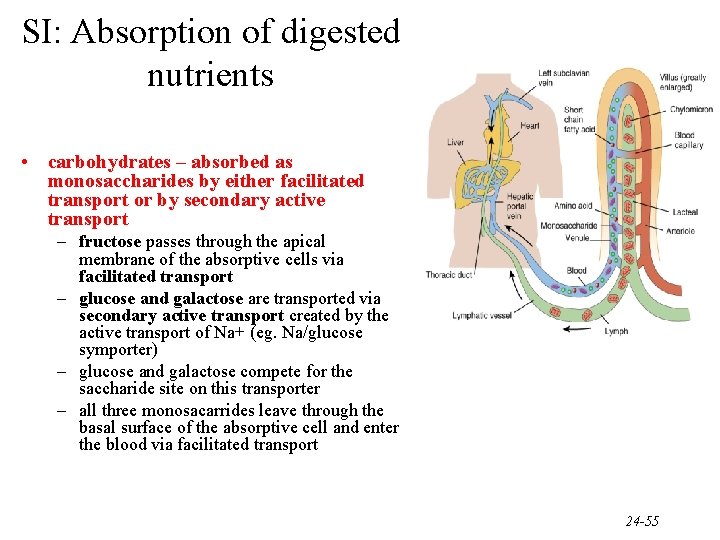
SI: Absorption of digested nutrients • carbohydrates – absorbed as monosaccharides by either facilitated transport or by secondary active transport – fructose passes through the apical membrane of the absorptive cells via facilitated transport – glucose and galactose are transported via secondary active transport created by the active transport of Na+ (eg. Na/glucose symporter) – glucose and galactose compete for the saccharide site on this transporter – all three monosacarrides leave through the basal surface of the absorptive cell and enter the blood via facilitated transport 24 -55
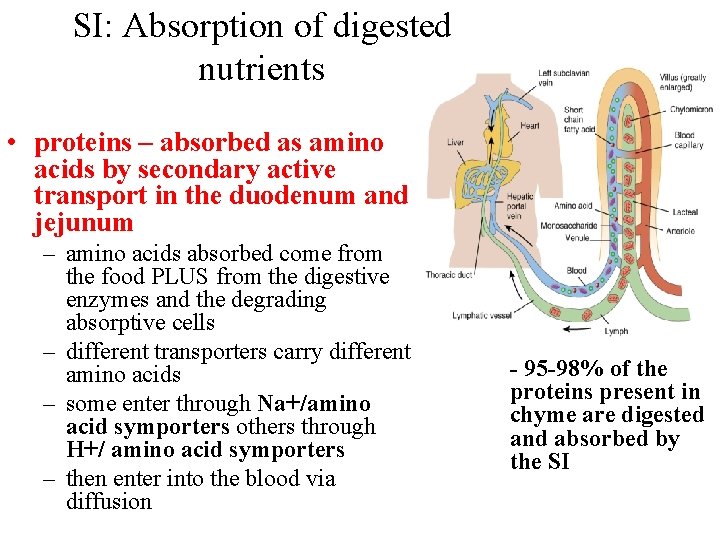
SI: Absorption of digested nutrients • proteins – absorbed as amino acids by secondary active transport in the duodenum and jejunum – amino acids absorbed come from the food PLUS from the digestive enzymes and the degrading absorptive cells – different transporters carry different amino acids – some enter through Na+/amino acid symporters others through H+/ amino acid symporters – then enter into the blood via diffusion - 95 -98% of the proteins present in chyme are digested and absorbed by the SI

SI: Absorption of digested nutrients • fats – absorbed via simple diffusion – 95% absorbed in the small intestine – bile induces emulsification - results in breakdown of a fat into 2 fatty acids + a monoglyceride (one fatty acid + glycerol) – the fatty acids are either short-chain or long chain – short chain fatty acids and cholesterol move into absorptive cell via simple diffusion – long chain fatty acids and monoglycerides require combination with bile in the form of a micelle Fat globule Bile salts Fat droplets coated with bile salts Epithelium of small intestine Epithelium of lacteal Micelles made up of fatty acids, monoglycerides, and bile salts Lacteal
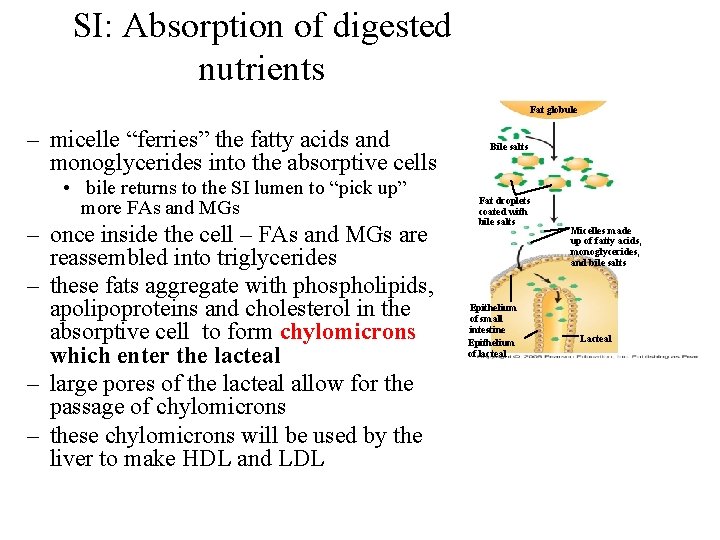
SI: Absorption of digested nutrients Fat globule – micelle “ferries” the fatty acids and monoglycerides into the absorptive cells • bile returns to the SI lumen to “pick up” more FAs and MGs – once inside the cell – FAs and MGs are reassembled into triglycerides – these fats aggregate with phospholipids, apolipoproteins and cholesterol in the absorptive cell to form chylomicrons which enter the lacteal – large pores of the lacteal allow for the passage of chylomicrons – these chylomicrons will be used by the liver to make HDL and LDL Bile salts Fat droplets coated with bile salts Epithelium of small intestine Epithelium of lacteal Micelles made up of fatty acids, monoglycerides, and bile salts Lacteal

Fat Processing – nascent (new) chylomicrons enter the blood at the subclavian veins – removed from the blood as they pass through the liver – liver expresses lipoprotein lipase (LPL) – breaks down the chylomicron into fatty acids, monoglycerides and cholesterol – cholesterol is used to make bile – cholesterol, triglycerides and apoplipoproteins are assembled into HDL or VLDL • VLDL breaks down into LDL (by LPL enzyme) – adipose cells are also capable of taking up chylomicrons and breaking them down via the LPL enzyme 24 -59

Absorption in the SI • Blood that enters the SI villi is rich in oxygen, poor in nutrients • Blood that exits the villi is poor in oxygen and rich in nutrients • BUT: venous blood may also be contaminated with toxins • SO: blood from SI flows into the liver via the hepatic portal vein – to be filtered prior to emptying via the hepatic vein into the inferior vena cava 24 -60
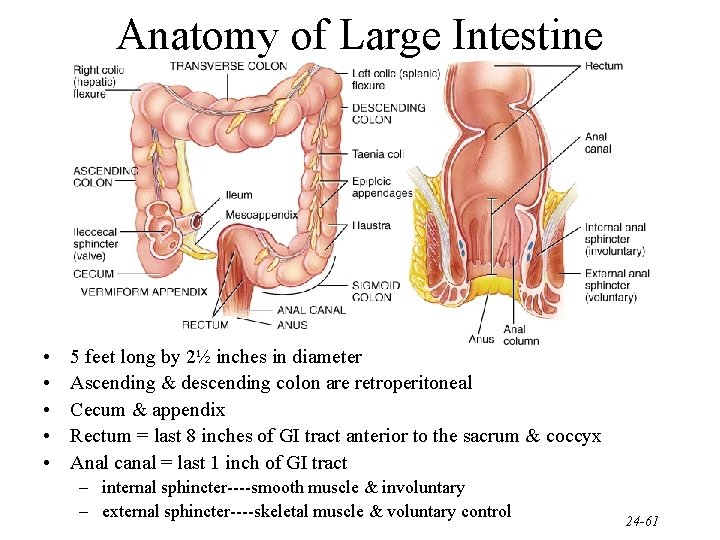
Anatomy of Large Intestine • • • 5 feet long by 2½ inches in diameter Ascending & descending colon are retroperitoneal Cecum & appendix Rectum = last 8 inches of GI tract anterior to the sacrum & coccyx Anal canal = last 1 inch of GI tract – internal sphincter----smooth muscle & involuntary – external sphincter----skeletal muscle & voluntary control 24 -61
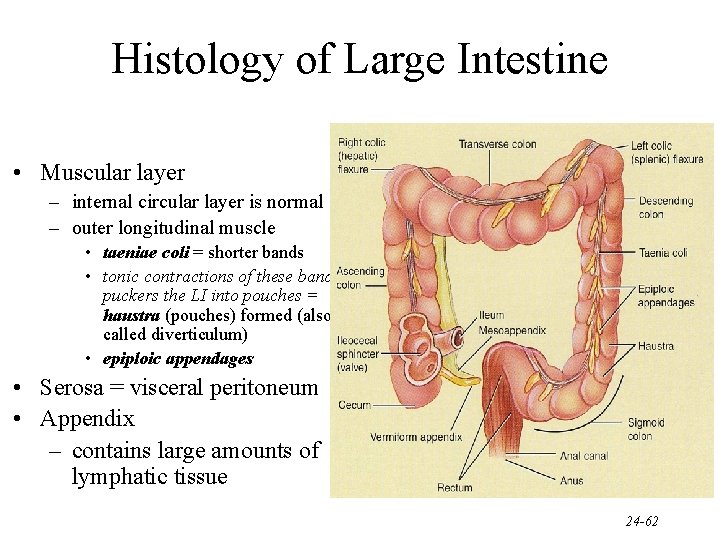
Histology of Large Intestine • Muscular layer – internal circular layer is normal – outer longitudinal muscle • taeniae coli = shorter bands • tonic contractions of these bands puckers the LI into pouches = haustra (pouches) formed (also called diverticulum) • epiploic appendages • Serosa = visceral peritoneum • Appendix – contains large amounts of lymphatic tissue 24 -62
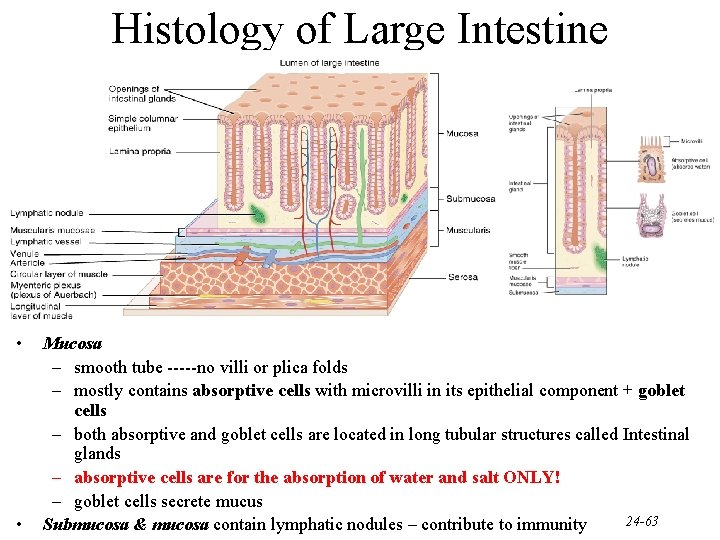
Histology of Large Intestine • • Mucosa – smooth tube -----no villi or plica folds – mostly contains absorptive cells with microvilli in its epithelial component + goblet cells – both absorptive and goblet cells are located in long tubular structures called Intestinal glands – absorptive cells are for the absorption of water and salt ONLY! – goblet cells secrete mucus 24 -63 Submucosa & mucosa contain lymphatic nodules – contribute to immunity

Mechanical Digestion in Large Intestine • Smooth muscle of muscularis = mechanical digestion • Peristaltic waves (3 to 12 contractions/minute) – haustral churning----relaxed pouches are filled by muscular contractions in the haustra below it – gastroilial reflex = when stomach is full, gastrin hormone relaxes ileocecal sphincter so small intestine will empty and make room for new chyme • Also intensifies the peristaltic waves in the ileum and the older chyme then enters the caecum – gastrocolic reflex = when stomach fills, a strong peristaltic wave moves contents of transverse colon into rectum

Chemical Digestion in Large Intestine • No enzymes are secreted only mucous – by the goblet cells in the intestinal glands • BUT - chyme is aacted upon by the action of bacteria – bacterial based chemical digestion NOT human-based • Bacteria ferment: – undigested carbohydrates - carbon dioxide & methane gas – undigested proteins - simpler substances (indoles, skatoles, hydrogen sulfide)----odor – turn bilirubin into simpler substances that produce color of feces • Bacteria also produce vitamin K and B in colon

Absorption & Feces Formation in the Large Intestine • food has now been in the GI tract for 3 to 10 hours • solid or semisolid form in the LI due to water reabsorption = feces – 90% of all water absorption takes place in the SI – last 10% in the LI • feces = water, salts, sloughed-off epithelial cells, bacteria, products of bacterial decomposition, unabsorbed and undigested materials • the LI is very important in maintaining water balance – Excess water in feces = diarrhea – Insufficient water in feces = constipation • also absorbs some electrolytes = Na+ and Cl • can also absorb some vitamins

Fiber • feces also contains materials undigestible by human enzymes = Fiber • Three types of fiber: • 1. dietary fiber - indigestible plant carbohydrates (cellulose, lignin and pectin) • 2. soluble fiber – dissolves in water (beans, barley, broccoli, prunes, apples and citrus) – forms a gel that slows the passage of materials through the colon – helps to lower blood cholesterol – binds to bile salts to prevent their reabsorption – eliminated through feces – liver must make more bile – so it gets the cholesterol component of bile from LDL in the blood – lowers LDL levels – also acted upon by bacteria carbon dioxide and methane gas • 3. insoluble fiber – woody or structural parts of the plant (skins of fruits and vegetables, coatings around bran and corn) – passes though the colon relatively unchanged
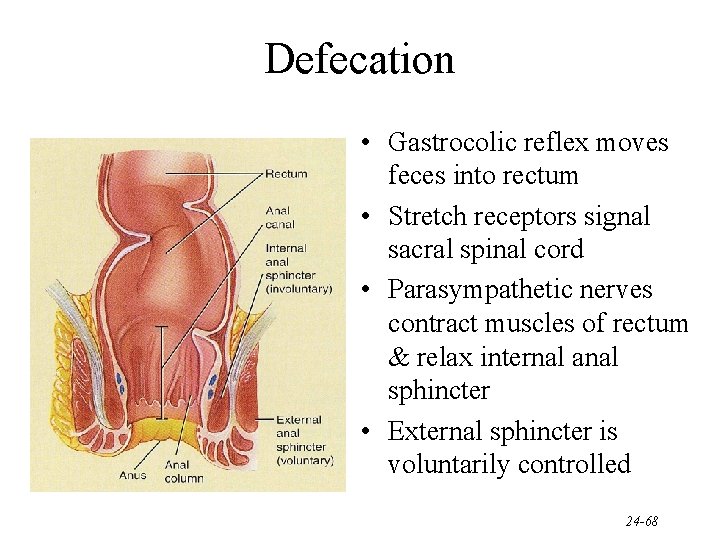
Defecation • Gastrocolic reflex moves feces into rectum • Stretch receptors signal sacral spinal cord • Parasympathetic nerves contract muscles of rectum & relax internal anal sphincter • External sphincter is voluntarily controlled 24 -68

Digestive Hormones • stomach: – gastrin – by the G cells of the stomach lining • stimulates production of gastric juice and encourages emptying of the stomach • also relaxes the sphincter between the ileum and cecum (ileocecal) • small intestine: – gastric inhibitory peptide/enterogastrone – antagonist to gastrin • inhibits emptying of the stomach

Digestive Hormones • small intestine: – CCK/cholecystikinin: by the enteroendocrine cells of the SI (presence of fatty acids) • CCK stimulates the release of pancreatic juice and bile (synthesis and increased gallbladder contraction) • also slows the emptying of the stomach • decreases gastric juice production – secretin: by the enteroendocrine cells of the SI • secretin stimulates the release of bicarbonate from the pancreas – neutralizes chime • decreases gastric juice production • decreases gastrin production and release • increases pepsinogen • role in water regulation – activates the release of ADH from posterior pituitary
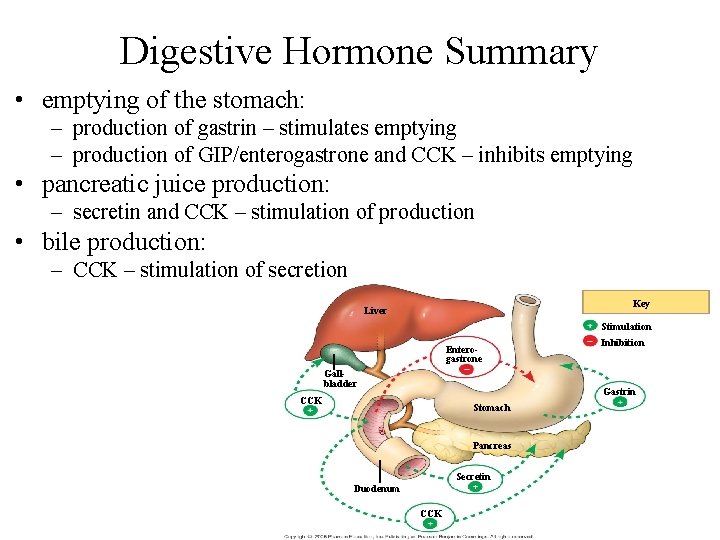
Digestive Hormone Summary • emptying of the stomach: – production of gastrin – stimulates emptying – production of GIP/enterogastrone and CCK – inhibits emptying • pancreatic juice production: – secretin and CCK – stimulation of production • bile production: – CCK – stimulation of secretion Key Liver Stimulation Enterogastrone Gallbladder Inhibition Gastrin CCK Stomach Pancreas Secretin Duodenum CCK
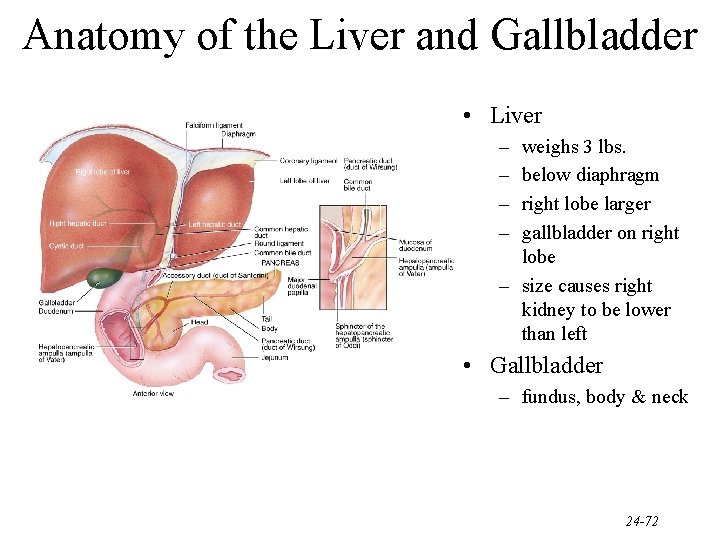
Anatomy of the Liver and Gallbladder • Liver – – weighs 3 lbs. below diaphragm right lobe larger gallbladder on right lobe – size causes right kidney to be lower than left • Gallbladder – fundus, body & neck 24 -72
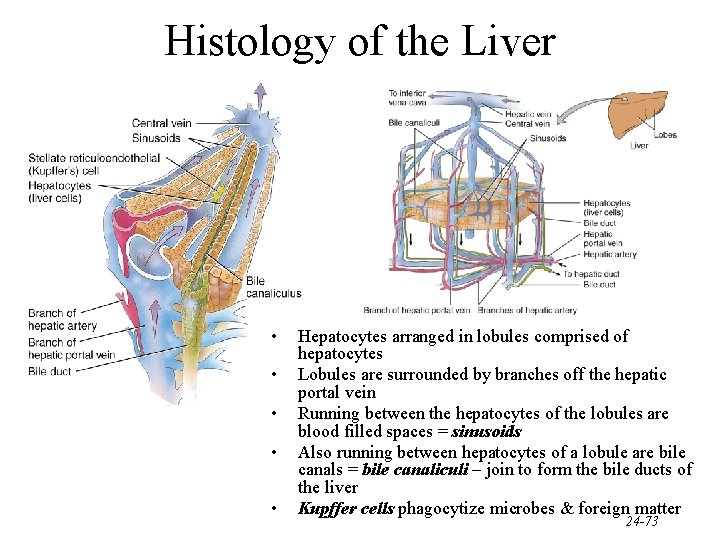
Histology of the Liver • • • Hepatocytes arranged in lobules comprised of hepatocytes Lobules are surrounded by branches off the hepatic portal vein Running between the hepatocytes of the lobules are blood filled spaces = sinusoids Also running between hepatocytes of a lobule are bile canals = bile canaliculi – join to form the bile ducts of the liver Kupffer cells phagocytize microbes & foreign matter 24 -73
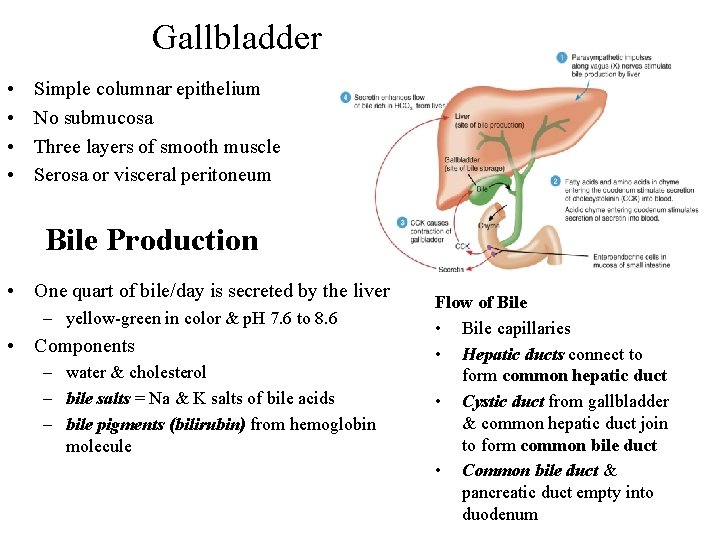
Gallbladder • • Simple columnar epithelium No submucosa Three layers of smooth muscle Serosa or visceral peritoneum Bile Production • One quart of bile/day is secreted by the liver – yellow-green in color & p. H 7. 6 to 8. 6 • Components – water & cholesterol – bile salts = Na & K salts of bile acids – bile pigments (bilirubin) from hemoglobin molecule Flow of Bile • Bile capillaries • Hepatic ducts connect to form common hepatic duct • Cystic duct from gallbladder & common hepatic duct join to form common bile duct • Common bile duct & pancreatic duct empty into duodenum 24 -74

Bile functions • emulsification – breakdown of fats into fatty acids (long or short chain) + monoglycerides • make the long-chain fatty acids and monoglycerides (which are large) more soluble in the watery environment of the chyme • bile salts surround the long-chain fatty acids and form tiny spheres called micelles – amphipathetic nature of bile salts – hydrophobic portion interacts with the fatty acids • micelles are absorbed into the absorptive cell – the long-chain fatty acids and monoglycerides then separate from the bile and move into the absorptive cells cytoplasm – leaving the micelles behind (move back into the chyme) – micelles act as a lipid “ferry” – also solubilize other large hydrophobic molecules like the fat-soluble vitamins (A, D, E, K) and cholesterol 24 -75

Liver Functions--Carbohydrate Metabolism • Turn amino acids into glucose (gluconeogenesis) – Alanine and glutamine • Turn triglycerides into glucose Liver Functions--Protein Metabolism – Turns glycerol into glucose (gluconeogenesis) – Turns odd number FAs into glucose (gluconeogenesis) • Turn excess glucose into glycogen & store • Deamination = removes NH 2 in the liver (amine group) from amino acids • Turn glycogen back into glucose as needed • Converts resulting toxic ammonia (NH 3) into urea for excretion by the Liver Functions --Lipid kidney Metabolism • Synthesizes plasma proteins utilized in the clotting mechanism and • Synthesize cholesterol - Synthesize immune system lipoproteins----HDL and LDL (used to transport fatty acids in bloodstream) • Convert one amino acid into another • Stores some fat • Breaks down some fatty acids for 24 -76 energy production (ATP)

Other Liver Functions • Detoxifies the blood by removing or altering drugs & hormones (thyroid & estrogen) • Releases bile salts help digestion by emulsification • Stores fat soluble vitamins-----A, B 12, D, E, K • Stores iron and copper • Phagocytizes worn out blood cells & bacteria • Activates vitamin D (the skin can also do this with 1 hr of sunlight a week) 24 -77

Chemical Digestion of Carbohydrates • Mouth---salivary amylase – inactivated in the stomach by the low p. H • Esophagus & stomach--nothing happens • Duodenum – secretion of pancreatic juice (amylase) – synthesis of the brush border enzymes (maltase, sucrase & lactase) act on disaccharides • produces monosaccharides-fructose, glucose & galactose • lactose intolerance (no enzyme; bacteria ferment sugar)--gas & diarrhea Digestion of Proteins • Stomach – HCl denatures or unfolds proteins – secretion of pepsinogen and activation by HCl - pepsin turns proteins into peptides • Pancreas – secretion of pancreatic juice which contains trypsin, chymotrypsin etc… • Intestines – synthesis of brush border enzymes-----aminopeptidase or dipeptidase------split off amino acid at amino end of molecule 24 -78

Digestion of Lipids • Mouth----lingual lipase • Small intestine – emulsification by bile – pancreatic lipase within the pancreatic juice---splits into 2 fatty acids + a monoglyceride – no lipid-digesting enzymes made by the brush border Digestion of Nucleic Acids • Pancreatic juice contains 2 nucleases – ribonuclease which digests RNA – deoxyribonuclease which digests DNA • Nucleotides produced are further digested by brush border enzymes (nucleosideases and phosphatases) – break the nucleotide into pentose, phosphate & nitrogenous bases • Absorbed by active transport 24 -79
- Slides: 79