The Diabetic Retinopathy Clinical Research Network Protocol I

The Diabetic Retinopathy Clinical Research Network Protocol I: Clinical Applications Supported through a cooperative agreement from the National Eye Institute and the National Institute of Diabetes and Digestive and Kidney Diseases, National Institutes of Health, Department of Health and Human Services EY 14231, EY 14229, EY 018817 1

Diabetic Macular Edema Treatment Ø Focal/Grid Photocoagulation • ~25 years following ETDRS Ø Intravitreal Steroids • ~10 years Ø Anti-VEGF Agents • Late stage studies ~15 months
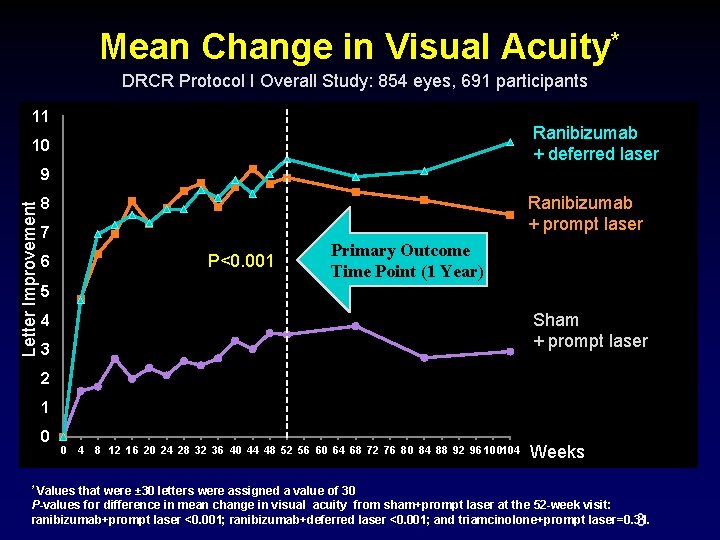
Mean Change in Visual Acuity* DRCR Protocol I Overall Study: 854 eyes, 691 participants 11 Ranibizumab + deferred laser 10 Letter Improvement 9 Ranibizumab + prompt laser 8 7 P<0. 001 6 Primary Outcome Time Point (1 Year) 5 Sham + prompt laser 4 3 2 1 0 0 * Values 4 8 12 16 20 24 28 32 36 40 44 48 52 56 60 64 68 72 76 80 84 88 92 96 100104 Weeks that were ± 30 letters were assigned a value of 30 P-values for difference in mean change in visual acuity from sham+prompt laser at the 52 -week visit: ranibizumab+prompt laser <0. 001; ranibizumab+deferred laser <0. 001; and triamcinolone+prompt laser=0. 31. 3

Background Ø Protocol I demonstrated that ranibizumab (with prompt or deferred focal/grid laser) resulted in superior visual acuity outcomes compared with laser alone through 2 years Ø The treatment regimen for ranibizumab (with prompt or deferred laser ) was very detailed and facilitated by a real-time web -based system 4

Purpose of this Presentation To discuss clinical applications that might provide clinicians with: • a simplified approach to retreatment • in accord with the general opinion of the DRCR. net investigators, and is • based on the Protocol I retreatment algorithm 5
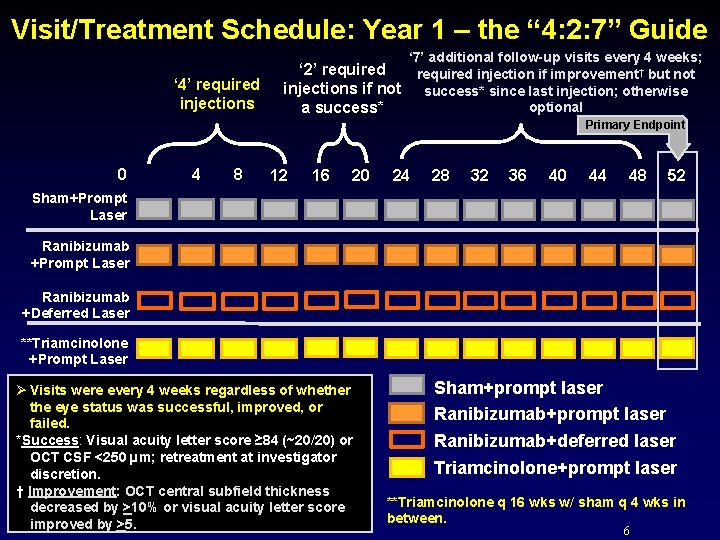
Visit/Treatment Schedule: Year 1 – the “ 4: 2: 7” Guide ‘ 7’ additional follow-up visits every 4 weeks; ‘ 4’ required injections ‘ 2’ required injection if improvement† but not injections if not success* since last injection; otherwise optional a success* Primary Endpoint 0 4 8 12 16 20 24 28 32 36 40 44 48 52 Sham+Prompt Laser Ranibizumab +Deferred Laser **Triamcinolone +Prompt Laser Ø Visits were every 4 weeks regardless of whether the eye status was successful, improved, or failed. *Success: Visual acuity letter score ≥ 84 (~20/20) or OCT CSF <250 µm; retreatment at investigator discretion. † Improvement: OCT central subfield thickness decreased by >10% or visual acuity letter score improved by >5. Sham+prompt laser Ranibizumab+deferred laser Triamcinolone+prompt laser **Triamcinolone q 16 wks w/ sham q 4 wks in between. 6
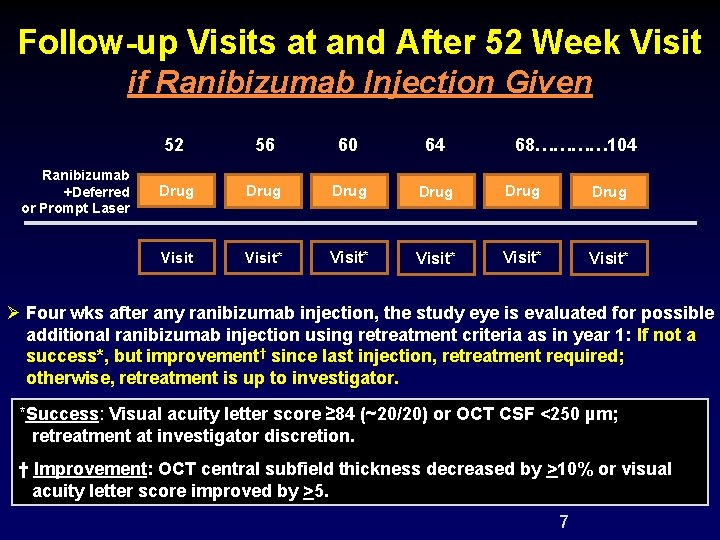
Follow-up Visits at and After 52 Week Visit if Ranibizumab Injection Given Ranibizumab +Deferred or Prompt Laser 52 56 60 64 68………… 104 Drug Drug Visit* Visit* Ø Four wks after any ranibizumab injection, the study eye is evaluated for possible additional ranibizumab injection using retreatment criteria as in year 1: If not a success*, but improvement† since last injection, retreatment required; otherwise, retreatment is up to investigator. *Success: Visual acuity letter score ≥ 84 (~20/20) or OCT CSF <250 µm; retreatment at investigator discretion. † Improvement: OCT central subfield thickness decreased by >10% or visual acuity letter score improved by >5. 7

Follow-up Visits at and After 52 Week Visit if Ranibizumab Not Given (4 to 8 to 16 Weeks) 52 Ranibizumab +deferred No Drug or Prompt Laser Visit 56 60 No Drug Visit 64 68………………. …… 84 No Drug Skip Visit No Drug Skip 16 wks Visit Ø If a ranibizumab injection is not given at the current and previous 2 visits (e. g. week 60 above), the next follow-up visit is in 8 weeks. Ø If at the next 8 week interval visit the injection is deferred again, the next follow-up visit is in 16 weeks; visits continue every 16 weeks unless a ranibizumab injection is given, at which point the visit 8 schedule goes back to 4 week intervals.
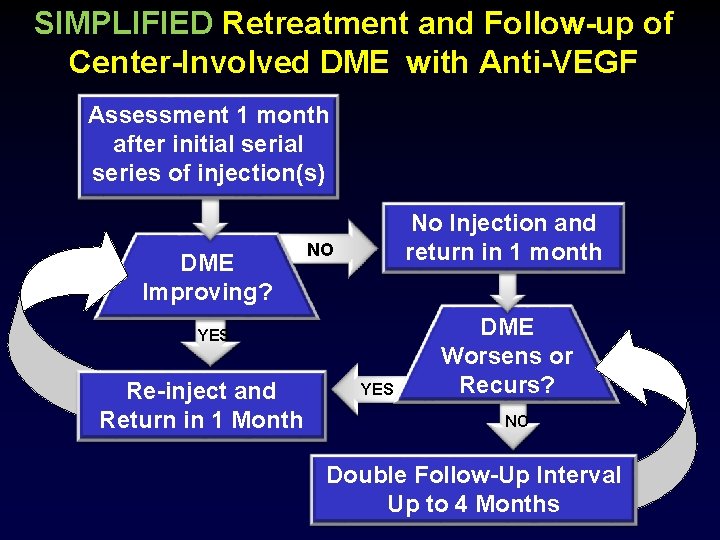
SIMPLIFIED Retreatment and Follow-up of Center-Involved DME with Anti-VEGF Assessment 1 month after initial series of injection(s) DME Improving? No Injection and return in 1 month NO YES Re-inject and Return in 1 Month YES DME Worsens or Recurs? NO Double Follow-Up Interval Up to 4 Months

Anti-VEGF Treatment Concepts Ø For which eyes with DME should anti-VEGF therapy be considered? Clinical Practice Considerations DRCR. net Study Patients could be enrolled if they had edema involving the center of the macula defined as central subfield thickness ≥ 250µm and vision impairment defined as Snellan equivalent of 20/32 to 20/320. 10

Anti-VEGF Treatment Concepts Ø For which eyes with DME should anti-VEGF therapy be considered? Clinical Practice Considerations Patients with edema involving the center of the macula DRCR. net Study Patients could be enrolled if they had edema involving the center of the macula defined as central subfield thickness ≥ 250µm and vision impairment defined as Snellan equivalent of 20/32 to 20/320. 11

Anti-VEGF Treatment Concepts Ø What follow-up interval could be considered after initiating therapy? Clinical Practice Considerations DRCR. net Study 4 required injections at 4 weekly intervals, followed by 2 injections at next 4 -weekly intervals unless edema resolved or vision improved to 20/20 or better † “Improvement” in the DRCR. net study was defined as “increase of at least 5 letters (approximately 1 line) in visual acuity or at least a 10% reduction in the central 12 subfield thickness on OCT since the last injection.

Anti-VEGF Treatment Concepts Ø What follow-up interval could be considered after initiating therapy? Clinical Practice Considerations DRCR. net Study Several serial monthly injections until vision and edema are no longer improving† or can no longer improve 4 required injections at 4 weekly intervals, followed by 2 injections at next 4 -weekly intervals unless edema resolved or vision improved to 20/20 or better (e. g. vision 20/20 or better, or edema resolved) † “Improvement” in the DRCR. net study was defined as “increase of at least 5 letters (approximately 1 line) in visual acuity or at least a 10% reduction in the central 13 subfield thickness on OCT since the last injection.

Anti-VEGF Treatment Concepts Ø What treatment is employed when the DME no longer is improving? Clinical Practice Considerations DRCR. net Study If no improvement from prior injection, decision to re-inject was at investigator discretion. Injections were recommended if there still was edema to treat. 14

Anti-VEGF Treatment Concepts Ø What treatment is employed when the DME no longer is improving? Clinical Practice Considerations DRCR. net Study Focal/grid laser can be added if it not previously used and injections would continue. Injections may be withheld, but resumed if the edema worsens. If no improvement from prior injection, decision to re-inject was at investigator discretion. Injections were recommended if there still was edema to treat. 15

Anti-VEGF Treatment Concepts Ø When should treatment be resumed after it has not been given? Clinical Practice Considerations DRCR. net Study Re-injection was at the investigator’s discretion if edema recurred or worsened, but was recommended if there was edema to treat; follow-up then returned to 4 week intervals once injections resumed 16

Anti-VEGF Treatment Concepts Ø When should treatment be resumed after it has not been given? Clinical Practice Considerations DRCR. net Study Re-injection was at the Injections may be reinvestigator’s discretion if sumed if edema recurs edema recurred or worsened, or worsens; follow-up but was recommended if there was edema to treat; then returns to monthly intervals until follow-up then returned to 4 week intervals once injection is not given injections resumed 17

Anti-VEGF Treatment Concepts Ø What follow-up is employed when the DME does not recur or worsen after an injection is not given? Clinical Practice Considerations DRCR. net Study Starting with the second year of treatment, if an injection was withheld at 3 consecutive 4 weekly visits, follow-up interval was extended to 8 weeks, and then again to 16 weeks if treatment still not warranted 18

Anti-VEGF Treatment Concepts Ø What follow-up is employed when the DME does not recur or worsen after an injection is not given? Clinical Practice Considerations DRCR. net Study If injection was not given and edema does not recur, follow-up may be doubled (up to 4 months or longer). Starting with the second year of treatment, if an injection was withheld at 3 consecutive 4 weekly visits, follow-up interval was extended to 8 weeks, and then again to 16 weeks if treatment still not warranted 19

Anti-VEGF Treatment Concepts Ø When should focal/grid laser treatment be added? Clinical Practice Considerations DRCR. net Study Randomized treatment groups included either prompt (within 310 days) or deferred (at least 24 weeks) focal/grid laser. If deferred, laser only could be added if edema was still present after 24 weeks and there was no improvement from two prior consecutive injections 20

Anti-VEGF Treatment Concepts Ø When should focal/grid laser treatment be added? Clinical Practice Considerations DRCR. net Study Randomized treatment groups Focal/grid laser may included either prompt (within 3 be given initially or 10 days) or deferred (at least 24 deferred. If deferred, weeks) focal/grid laser. If laser may be added deferred, laser only could be at any time if edema added if edema was still present is no longer improv- after 24 weeks and there was no ing after an injection. improvement from two prior consecutive injections 21

Anti-VEGF Treatment Concepts Ø When should focal/grid laser be repeated after initiation? Clinical Practice Considerations DRCR. net Study Once initiated, focal/grid was re-applied if 1) edema was present, 2) eye did not have “complete” laser, and 3) it had been at least 13 weeks since last laser 22

Anti-VEGF Treatment Concepts Ø When should focal/grid laser be repeated after initiation? Clinical Practice Considerations Focal/grid laser generally should be repeated at any time that edema persists or is not improving while giving anti-VEGF therapy (as long as it is believed that additional laser may be of benefit) DRCR. net Study Once initiated, focal/grid was re-applied if 1) edema was present, 2) eye did not have “complete” laser, and 3) it had been at least 13 weeks since last laser 23

Summary Ø Given that duplication of the treatment approach used within the DRCR. net trial with its elaborate infrastructure may not be practical in all clinical settings Ø This presentation provides guidelines based on DRCR. net investigators’ opinion for a simplified retreatment approach when using intravitreal ranibizumab to treat center-involved DME with vision impairment Ø However, it is unknown whether these or other modifications to the DRCR. net protocol would result in better, same or worse outcomes 24
- Slides: 24