The Diabetic Retinopathy Clinical Research Network Intravitreous AntiVEGF

The Diabetic Retinopathy Clinical Research Network Intravitreous Anti-VEGF Treatment for Prevention of Vision Threatening Diabetic Retinopathy in Eyes at High Risk Investigator Training Slides 2. 0 [Protocol version 1. 0] 1

Background Ø Eyes with severe NPDR are at high risk for DR worsening and subsequent VA loss • 52% develop PDR over 1 year • 60% develop PDR with HRC over next 5 years 2
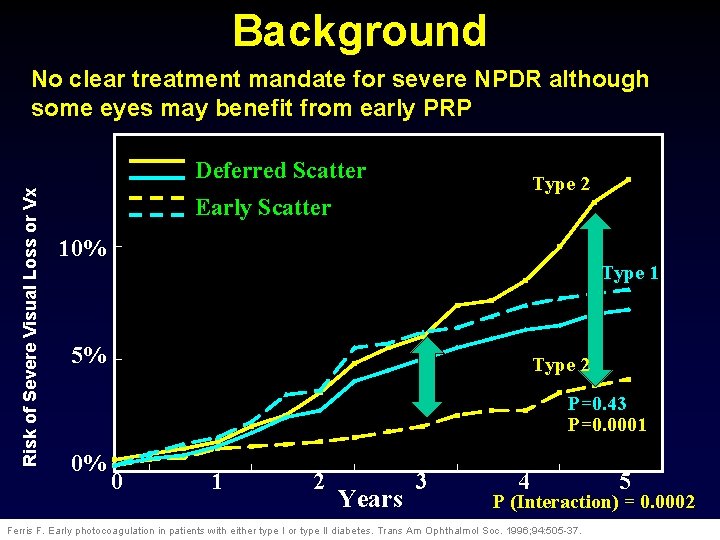
Background No clear treatment mandate for severe NPDR although some eyes may benefit from early PRP Risk of Severe Visual Loss or Vx Deferred Scatter Type 2 Early Scatter 10% Type 1 5% Type 2 P=0. 43 P=0. 0001 0% 0 1 2 Years 3 4 5 P (Interaction) = 0. 0002 Ferris F. Early photocoagulation in patients with either type I or type II diabetes. Trans Am Ophthalmol Soc. 1996; 94: 505 -37.
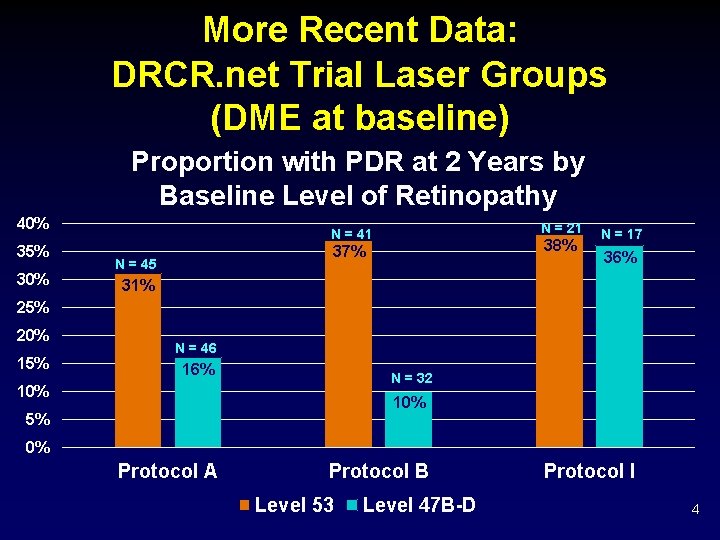
More Recent Data: DRCR. net Trial Laser Groups (DME at baseline) Proportion with PDR at 2 Years by Baseline Level of Retinopathy 40% 35% 30% N = 21 N = 41 38% 37% N = 45 N = 17 36% 31% 25% 20% 15% N = 46 16% N = 32 10% 5% 0% Protocol A Protocol B Level 53 Level 47 B-D Protocol I 4
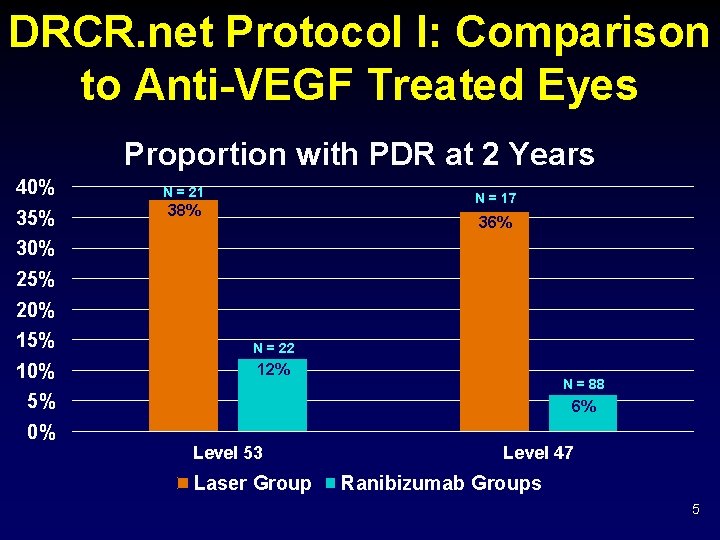
DRCR. net Protocol I: Comparison to Anti-VEGF Treated Eyes Proportion with PDR at 2 Years 40% 35% N = 21 N = 17 38% 36% 30% 25% 20% 15% N = 22 10% 12% N = 88 5% 6% 0% Level 53 Laser Group Level 47 Ranibizumab Groups 5
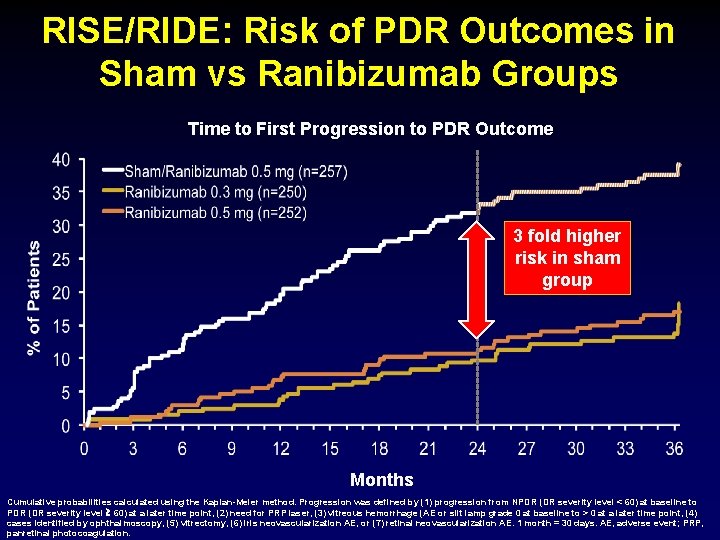
RISE/RIDE: Risk of PDR Outcomes in Sham vs Ranibizumab Groups Time to First Progression to PDR Outcome 3 fold higher risk in sham group Months Cumulative probabilities calculated using the Kaplan-Meier method. Progression was defined by (1) progression from NPDR (DR severity level < 60) at baseline to PDR (DR severity level 60) at a later time point, (2) need for PRP laser, (3) vitreous hemorrhage (AE or slit lamp grade 0 at baseline to > 0 at a later time point, (4) cases identified by ophthalmoscopy, (5) vitrectomy, (6) iris neovascularization AE, or (7) retinal neovascularization AE. 1 month = 30 days. AE, adverse event; PRP, panretinal photocoagulation.
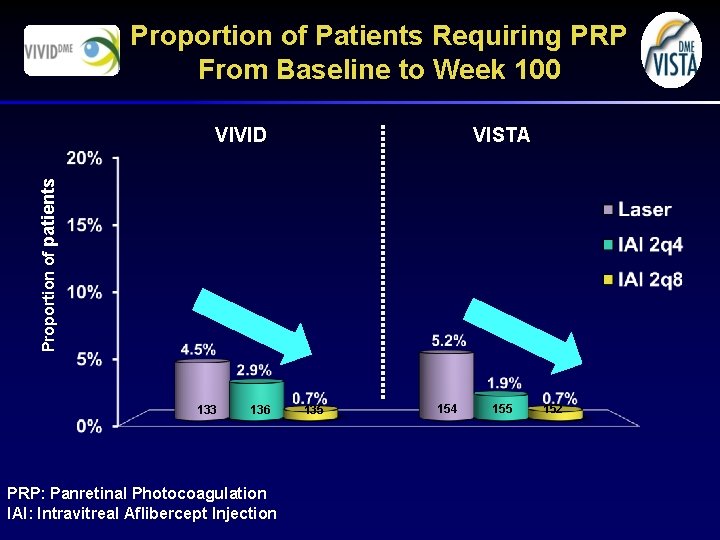
Proportion of Patients Requiring PRP From Baseline to Week 100 VISTA Proportion of patients VIVID 133 136 PRP: Panretinal Photocoagulation IAI: Intravitreal Aflibercept Injection 135 154 155 152

DME Development Ø Eyes with severe NPDR and no CI-DME at baseline are also at risk for developing DME requiring anti-VEGF treatment • 15% in ETDRS developed CI-DME on photos by 2 years Ø DRCR. net Protocol R included eyes with non-CI DME and any level of retinopathy and 14% developed CI-DME on OCT or required treatment by 1 year 8

Primary Objective To determine safety and efficacy of prompt anti-VEGF versus observation in eyes presenting with severe NPDR and no CI-DME for prevention of vision threatening outcomes Observation (sham injections) Intravitreous anti-VEGF Primary outcome: Proportion of eyes that develop PDR/PDR-related outcomes or center-involved DME causing visual acuity loss at 2 years 9

Follow-Up and Treatment Overview Ø Total duration: 4 years • Primary outcome: 2 years for anatomic outcome – if anatomic benefit through 2 years, continue follow-up through 4 years to determine if VA benefit too Ø Visits at 1, 2, and 4 months; every 4 months thereafter Ø Injections (intravitreous or sham) required at each of the above visits through 2 years Ø Thereafter, evaluate at each visit for retreatment: • If eye is “Mild NPDR” or better, defer injection • If “Moderate NPDR” or worse, injection is required 10

Composite Primary Outcome: Part 1 – PDR Ø Development of NV within the 7 modified ETDRS fields on fundus photography or FA, confirmed by Reading Center Ø NVI, NVA, or NVG on clinical exam Ø Traction retinal detachment, vitreous hemorrhage, or pre-retinal hemorrhage presumed to be from PDR, documented on fundus photography or FA Ø PRP, anti-VEGF, or vitrectomy for PDR, images should be obtained prior to treatment 11

Composite Primary Outcome: Part 2 – DME Ø Center-involved DME on clinical exam with ≥ 10% increase in central subfield thickness from baseline and visual acuity loss, defined as: • 1) at least 10 letter VA loss at a single visit, or • 2) 5 to 9 letter VA loss at 2 -consecutive visits, presumed to be from DME Ø Treatment for DME performed without meeting above criteria (protocol deviation) Note: An eye will be considered to have met the primary outcome if any one of the above PDR or DME criteria are met 12

Outcome Estimates Ø Anti-VEGF group • Based on Protocol I and RIDE/RISE data, we estimate ~ 15% of eyes in this study that receive the study anti-VEGF regimen will develop PDR/DME outcome. Ø Observation (Sham) group • Based on available data from Protocols A, B, I, we estimate ~ 30% of eyes in this study that receive no treatment will develop PDR/DME outcome. SAMPLE SIZE 386 eyes (193 per group) 13

Long-Term Objectives Ø If there is a clinically important difference identified among the treatment groups for the primary outcome at 2 years, the study will also evaluate whether increased chance of prevention of PDR/DME with anti -VEGF at 2 years results in long-term beneficial visual outcomes at 4 years. 14

Rationale Ø The application of anti-VEGF therapy earlier in the course of disease could help to reduce future potential treatment burden in patients, at the same time resulting in similar or better long-term visual acuity outcomes. Ø If this study demonstrates that anti-VEGF treatment is effective and safe in the setting of severe NPDR, a new strategy to prevent visionthreatening complications will be available for patients. 15

Major Inclusion/Exclusion Criteria in Study Eye Ø Severe NPDR (ETDRS level 53) according to investigator 4 -2 -1 rule o Severe hemorrhages in at least 4 quadrants, or o Definite venous beading in at least 2 quadrants, or o Moderate IRMA in at least 1 quadrant Ø VA letter score 20/25 or better Ø No CI-DME using standard OCT thresholds Ø No history of DME/DR treatment in prior 12 months and <4 prior injections at any time Ø No prior PRP 16
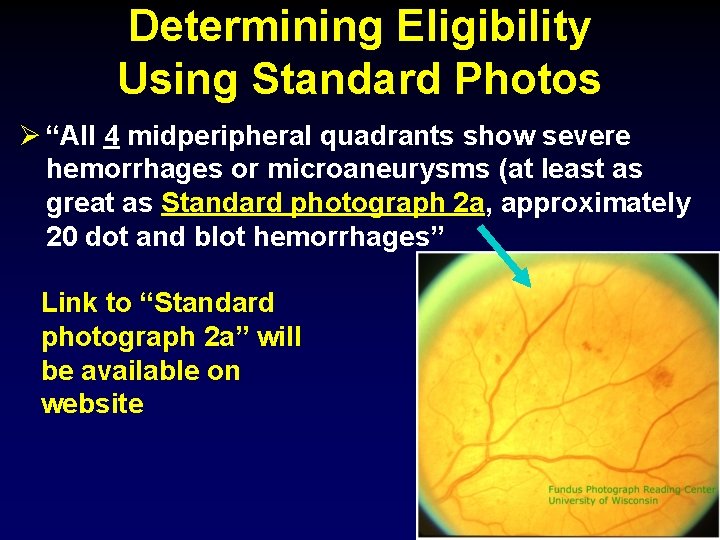
Determining Eligibility Using Standard Photos Ø “All 4 midperipheral quadrants show severe hemorrhages or microaneurysms (at least as great as Standard photograph 2 a, approximately 20 dot and blot hemorrhages” Link to “Standard photograph 2 a” will be available on website 17
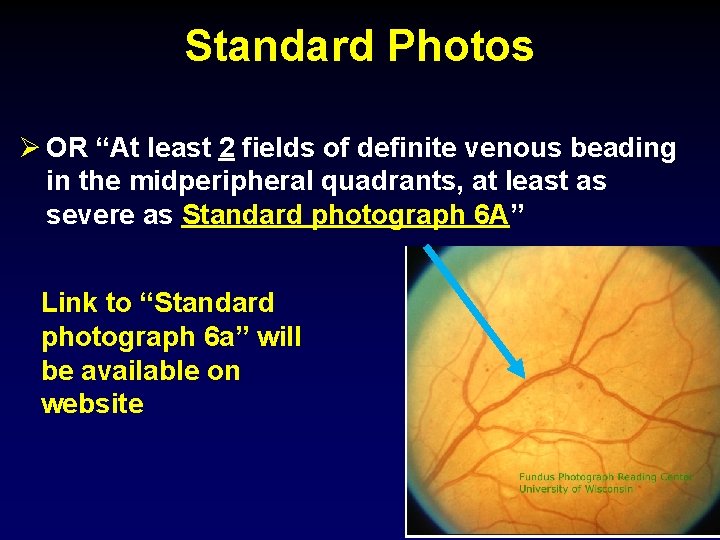
Standard Photos Ø OR “At least 2 fields of definite venous beading in the midperipheral quadrants, at least as severe as Standard photograph 6 A” Link to “Standard photograph 6 a” will be available on website 18

Standard Photos Ø OR “At least 1 field of moderate intraretinal microvascular abnormalities (IRMA) in the midperipheral quadrants, at least as severe as Standard photograph 8 A” Link to “Standard photograph 8 a” will be available on website 19

Website Tools NPDR definition provided Links to standard photos 20

DR Level Confirmation Ø At Screening Visit, investigator must confirm eye has severe NPDR on photos and no PDR within the 7 -modified ETDRS fields on FA or clinical exam Ø The FA and photos must be uploaded immediately for Reading Center grading Ø The Reading Center will confirm eligibility prior to randomization • Expected turnaround within 1 week Ø If eligible, the Randomization Visit must occur within 35 days of Screening Visit 21

Use of Wide-Field Imaging for FA Ø UWF color photos will not be permitted Ø For FA, sites should use OPTOS if available at baseline • Presence of NV outside of the 7 -modified ETDRS fields will NOT be an exclusion. Ø If a new OPTOS machine is obtained during follow-up, FA images should then be taken for ALL participants going forward • Peripheral NV outside the 7 modified ETDRS fields will not meet the primary outcome and generally should not be treated unless high risk Ø Note: Heidelberg UWF device not permitted at this time 22

Randomization Reminder Ø Before submitting the Randomization Visit, the investigator MUST • Confirm eligibility • Confirm patient’s willingness to accept either assignment and to complete all treatment/follow-up • Be available to perform the injection (intravitreous or sham) THAT DAY Ø Educate patient with a thorough ICF process so that they understand: • Time commitment • Treatment requirements 23
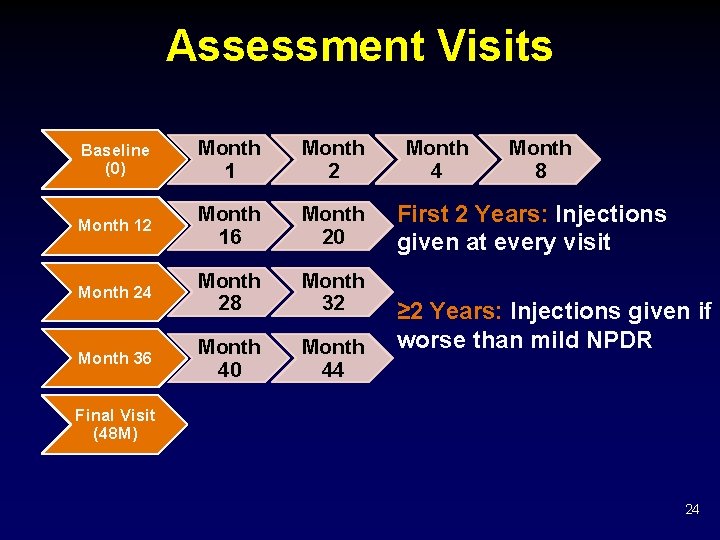
Assessment Visits Baseline (0) Month 1 Month 2 Month 16 Month 20 Month 24 Month 28 Month 32 Month 36 Month 40 Month 44 Month 8 First 2 Years: Injections given at every visit ≥ 2 Years: Injections given if worse than mild NPDR Final Visit (48 M) 24

When are photos/FA required? Ø At 4 -month visit and annually • Reading Center will perform a masked assessment of whether primary endpoint has been met Ø If initiating PDR or DME treatment and primary endpoint not previously confirmed by RC at one of the time points above • Note: Images will not be sent as soon as early NV detected • There is concern with unmasked investigators detecting NV earlier in the sham group than in the anti -VEGF group, this approach is intended to minimize such potential bias Ø To document TRD, VH, or PRH for primary endpoint 25

Intravitreous Injection Procedure Ø Two individuals must confirm the study eye and drug number against the printout or website Ø Mark the eye for injection Ø Apply topical anesthetic • Subconjunctival anesthetic may only be given if topical anesthetic is not sufficient to minimize discomfort Ø Place the lid speculum Ø Apply povidone iodine directly over and surrounding the injection site • DRCR. net injections must NOT be given without the use of povidone iodine in any circumstance Ø Pre- and post-injection topical antibiotics should NOT be used (prior discussion with Protocol Chair or her designate will be required prior to use) 26

Endophthalmitis Rates by Antibiotic Use 24, 052* Intravitreal Injections (2, 596 eyes) 9 Cases of Endophthalmitis 3 (0. 02%) Without Topical Antibiotics 6 (0. 06%) With Topical Antibiotics *Excluding injections given without povidone iodine (13 injections in 2 eyes) P = 0. 19 27
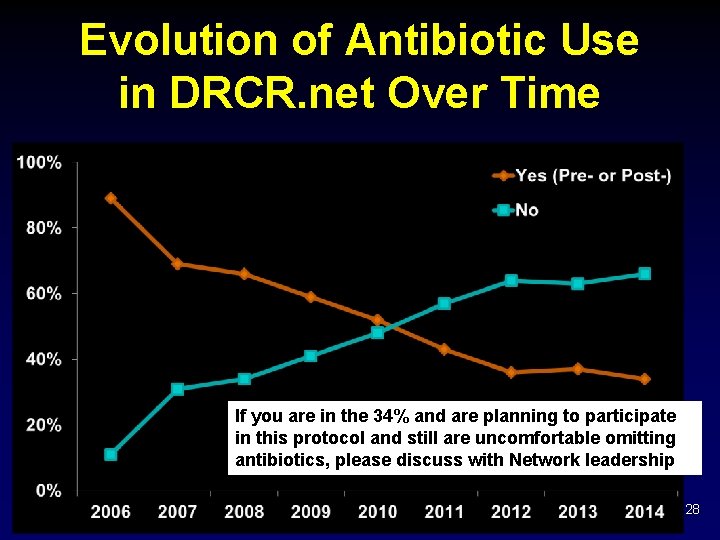
Evolution of Antibiotic Use in DRCR. net Over Time If you are in the 34% and are planning to participate in this protocol and still are uncomfortable omitting antibiotics, please discuss with Network leadership 28

Povidone-Iodine Use 24, 065 Intravitreal Injections (2, 598 eyes) e n di S U M b T u e d e s 13 injections (2 eyes) without Povidone-Iodine (protocol violation) v o P n o id o I e 100% of eyes developed endophthalmitis 29

Sham Injection Procedure Ø Same procedure as intravitreous injection, including: • • Confirming/marking the study eye Apply topical anesthetic (subconj should not be used) Place the lid speculum Apply povidone iodine directly over and surrounding the injection site (allowing sufficient time for the povidone iodine to dry) o Sham injections must NOT be given without the use of povidone iodine in any circumstance Ø A syringe without a needle will be used, with the hub pressed against the conjunctival surface to 30 simulate the force of an actual injection

Successful Sham Masking Ø In DRCR. net Protocol I, participants with 1 study eye (N = 423) Participant Response to type of injections Sham Group Ranibizumab Groups IVT Group Always Real 72% 88 -90% 55% Sometimes real /sometimes sham 18% 7 -12% 44% Always Sham 10% 0 -4% 1% Ø The majority receiving sham thought they were receiving real injections 31

Bilateral Injections Ø 2 study injections • Perform all required injection procedures on the right eye first before initiating any pre-injection prep of the left eye. • Study drug for the left eye should not be in the room before completing all right eye injection procedures. Ø One non-study injection • Perform all required injection procedures on the study eye before initiating any pre-injection prep of the non-study eye. • Study drug for the non-study eye should not be in the room before completing all study eye injection procedures. 32

PDR/DME Treatment During Follow-Up Ø It is expected that many eyes will require PDR or DME treatment at some point during follow-up • ~15% to 30% in the first 2 years are estimated to meet PDR/DME endpoint Ø Standardizing the criteria to treat and the treatment itself will allow us to better evaluate long-term visual acuity outcomes for the two treatment strategies (prevention vs. observe and treat) 33

PDR Treatment Criteria Ø Treatment for PDR must not be given unless: 1. The eye has high-risk characteristics: o NVD greater than standard photograph 10 A (1/4 to 1/3 disc area) or o Any NVD with pre-retinal or vitreous hemorrhage or o NVE greater than ½ disc area with pre-retinal or vitreous hemorrhage 2. The eye has VH requiring treatment that is presumed to be from PDR 34

PDR Treatment Criteria Ø If high-risk criteria not met, RC confirmation of the primary endpoint (NV within 7 -modified fields) should be obtained prior to initiating treatment whenever possible. Ø Treatment for NVE outside of the 7 modified fields without the presence of pre-retinal or vitreous hemorrhage is discouraged. • If the investigator believes treatment for peripheral NV is necessary, protocol chair review is required. 35
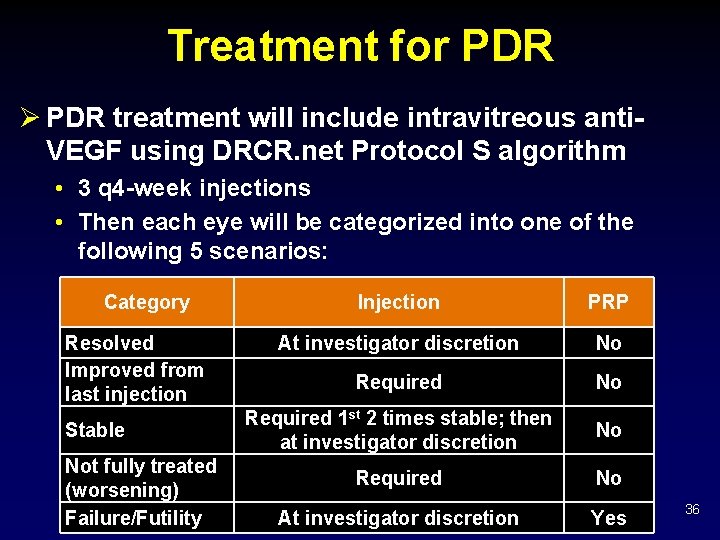
Treatment for PDR Ø PDR treatment will include intravitreous anti. VEGF using DRCR. net Protocol S algorithm • 3 q 4 -week injections • Then each eye will be categorized into one of the following 5 scenarios: Category Resolved Improved from last injection Stable Not fully treated (worsening) Failure/Futility Injection PRP At investigator discretion No Required 1 st 2 times stable; then at investigator discretion No Required No At investigator discretion Yes 36

DME Criteria and Treatment Ø Treatment for CI-DME must not be given until the primary endpoint for DME has been met: Ø CI-DME on clinical exam with ≥ 10% increase in central subfield thickness from baseline and: • 1) at least 10 letter VA loss at a single visit, or • 2) 5 to 9 letter VA loss at 2 consecutive visits. Ø Once the above endpoint has been met, must use DRCR. net Anti-VEGF Regimen for DME: • Continue q 4 w injections as long as there is improvement or worsening • No injection if stable after 2 consecutive injections and either “success” or >24 w from initial injection • Resume injection if worsen after withholding injection 37
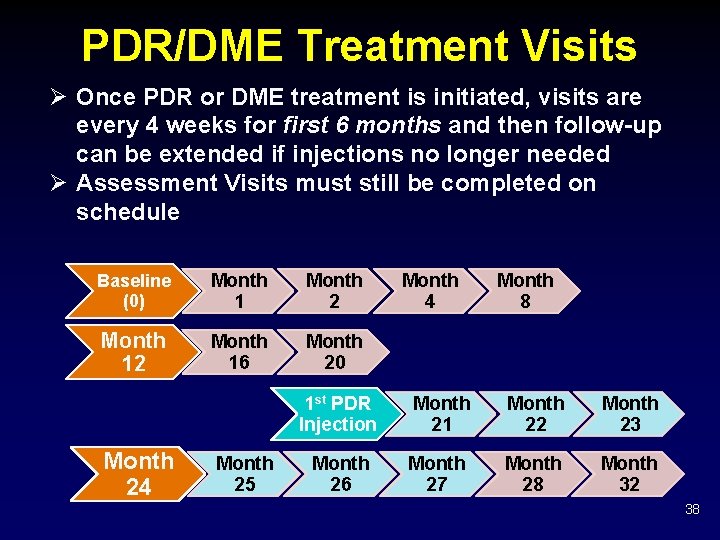
PDR/DME Treatment Visits Ø Once PDR or DME treatment is initiated, visits are every 4 weeks for first 6 months and then follow-up can be extended if injections no longer needed Ø Assessment Visits must still be completed on schedule Baseline (0) Month 1 Month 2 Month 16 Month 20 Month 24 Month 25 Month 4 Month 8 1 st PDR Injection Month 21 Month 22 Month 23 Month 26 Month 27 Month 28 Month 32 38

DRCR. net Website Ø Like all DRCR. net trials, the website will help guide you through follow-up, including: • Assessing eligibility (standard photos provided) • Assessing primary outcome (reminders when imaging is needed) • Criteria to initiate treatment PDR or DME • Retreatment criteria once initiated • Visit schedule 39

Complete the Visit Form Ø A treatment message will display for each indication (prevention, PDR, DME) Ø The investigator must make a treatment determination based on all messages Ø A second individual should confirm that the treatment planned is not contrary to the messages An injection of aflibercept in the left eye must be given at this visit. An injection of Aflibercept should not be given for PDR at this visit since criteria to initiate anti-VEGF injections for PDR have not been met. An injection of Aflibercept should not be given in the left eye for DME at this visit since criteria to initiate anti-VEGF injections for DME have not been met. 40

Complete the Visit Form Ø You will then indicate whether an injection is planned AND the indication Ø If PDR or DME is entered as an indication for the first time, the eye will have met that outcome and the retreatment protocol for PDR or DME will be initiated It is extremely important that these questions are answered accurately 41

Treatment Message Questions Ø Retreatment calculation depends on correct data entry Ø Prior missed visits/missing data could also impact the calculations Ø If at any time, you do not believe the message is correct or you wish to deviate, CONTACT US! An injection of Aflibercept should not be given for PDR at this visit since criteria to initiate anti-VEGF injections for PDR have not been met. An injection of Aflibercept should not be given in the left eye for DME at this visit since criteria to initiate anti-VEGF injections for DME have not been met. 42

The Diabetic Retinopathy Clinical Research Network Only YOU can prevent vision loss! 43
- Slides: 43